Drivers of Under-Five Stunting Trend in 14 Low- and Middle-Income Countries since the Turn of the Millennium: A Multilevel Pooled Analysis of 50 Demographic and Health Surveys
Abstract
1. Introduction
2. Materials and Methods
2.1. Data Source
2.2. Variables
2.3. Statistical Analysis
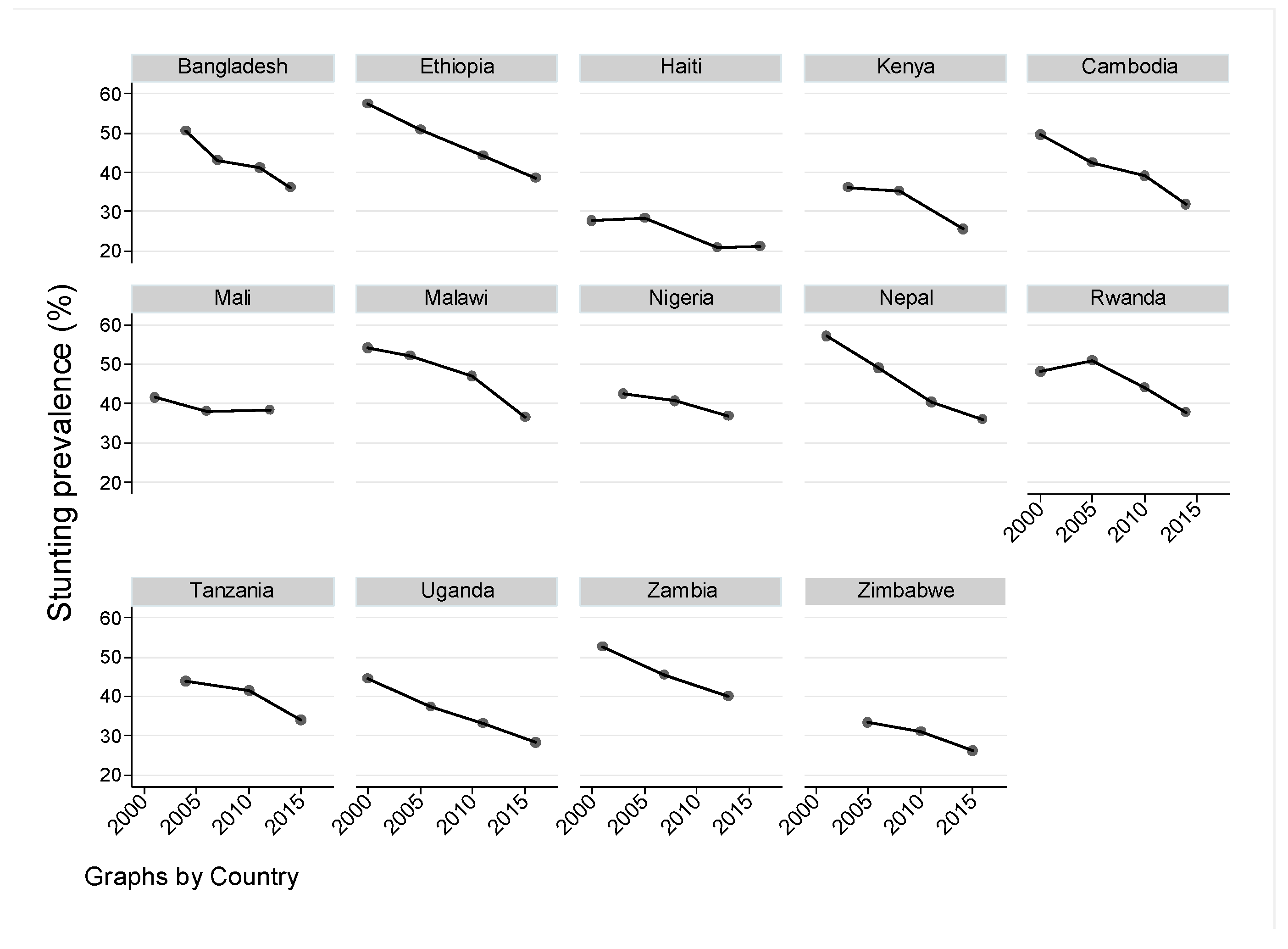
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- United Nations Children’s Fund (UNICEF); World Health Organization (WHO); International Bank for Reconstruction and Development; The World Bank. Levels and Trends in Child Malnutrition: Key Findings of the 2019 Edition of the Joint Child Malnutrition Estimates; WHO: Geneva, Switzerland, 2019. [Google Scholar]
- Black, R.E.; Allen, L.H.; Bhutta, Z.A.; Caulfield, L.E.; De Onis, M.; Ezzati, M.; Mathers, C.; Rivera, J. Maternal and child undernutrition: Global and regional exposures and health consequences. Lancet 2008, 371, 243–260. [Google Scholar] [CrossRef]
- Sudfeld, C.R.; McCoy, D.C.; Danaei, G.; Fink, G.; Ezzati, M.; Andrews, K.G.; Fawzi, W.W. Linear Growth and Child Development in Low- and Middle-Income Countries: A Meta-Analysis. Pediatrics 2015, 135, 1266–1275. [Google Scholar] [CrossRef] [PubMed]
- Guerrant, R.L.; Deboer, M.D.; Moore, S.R.; Scharf, R.J.; Lima, A.A.M. The impoverished gut—A triple burden of diarrhoea, stunting and chronic disease. Nat. Rev. Gastroenterol. Hepatol. 2013, 10, 220–229. [Google Scholar] [CrossRef] [PubMed]
- Addo, O.Y.; Stein, A.D.; Fall, C.H.D.; Gigante, D.P.; Guntupalli, A.M.; Horta, B.L.; Kuzawa, C.W.; Lee, N.; Norris, S.A.; Osmond, C.; et al. Parental childhood growth and offspring birthweight: Pooled analyses from four birth cohorts in low and middle income countries. Am. J. Hum. Biol. 2015, 27, 99–105. [Google Scholar] [CrossRef]
- Leroy, J.L.; Frongillo, E.A. Perspective: What Does Stunting Really Mean? A Critical Review of the Evidence. Adv. Nutr. 2019, 10, 196–204. [Google Scholar] [CrossRef]
- De Onis, M.; Dewey, K.G.; Borghi, E.; Onyango, A.W.; Blössner, M.; Daelmans, B.; Piwoz, E.; Branca, F. The World Health Organization’s global target for reducing childhood stunting by 2025: Rationale and proposed actions. Matern. Child Nutr. 2013, 9, 6–26. [Google Scholar] [CrossRef]
- Danaei, G.; Andrews, K.G.; Sudfeld, C.R.; Fink, G.; McCoy, D.C.; Peet, E.; Sania, A.; Fawzi, M.C.S.; Ezzati, M.; Fawzi, W.W. Risk Factors for Childhood Stunting in 137 Developing Countries: A Comparative Risk Assessment Analysis at Global, Regional, and Country Levels. PLoS Med. 2016, 13, e1002164. [Google Scholar] [CrossRef]
- Torlesse, H.; Cronin, A.A.; Sebayang, S.K.; Nandy, R. Determinants of stunting in Indonesian children: Evidence from a cross-sectional survey indicate a prominent role for the water, sanitation and hygiene sector in stunting reduction. BMC Public Health 2016, 16, 669. [Google Scholar] [CrossRef]
- Tiwari, R.; Ausman, L.M.; Agho, K.E. Determinants of stunting and severe stunting among under-fives: Evidence from the 2011 Nepal Demographic and Health Survey. BMC Pediatr. 2014, 14, 239. [Google Scholar] [CrossRef]
- Semali, I.A.; Tengia-Kessy, A.; Mmbaga, E.J.; Leyna, G. Prevalence and determinants of stunting in under-five children in central Tanzania: Remaining threats to achieving Millennium Development Goal 4. BMC Public Health 2015, 15, 1153. [Google Scholar] [CrossRef]
- Khan, S.; Zaheer, S.; Safdar, N.F. Determinants of stunting, underweight and wasting among children <5 years of age: Evidence from 2012–2013 Pakistan demographic and health survey. BMC Public Health 2019, 19, 358. [Google Scholar]
- Chirande, L.; Charwe, D.; Mbwana, H.; Victor, R.; Kimboka, S.; Issaka, A.I.; Baines, S.K.; Dibley, M.J.; Agho, K.E. Determinants of stunting and severe stunting among under-fives in Tanzania: Evidence from the 2010 cross-sectional household survey. BMC Pediatr. 2015, 15, 165. [Google Scholar] [CrossRef] [PubMed]
- Aguayo, V.M.; Nair, R.; Badgaiyan, N.; Krishna, V. Determinants of stunting and poor linear growth in children under 2 years of age in India: An in-depth analysis of Maharashtra’s comprehensive nutrition survey. Matern. Child Nutr. 2016, 12, 121–140. [Google Scholar] [CrossRef] [PubMed]
- Huicho, L.; Huayanay-Espinoza, C.A.; Herrera-Perez, E.; Segura, E.R.; De Guzman, J.N.; Rivera-Ch, M.; Barros, A.J. Factors behind the success story of under-five stunting in Peru: A district ecological multilevel analysis. BMC Pediatr. 2017, 17, 29. [Google Scholar] [CrossRef]
- Masibo, P.K.; Makoka, D. Trends and determinants of undernutrition among young Kenyan children: Kenya Demographic and Health Survey; 1993, 1998, 2003 and 2008–2009. Public Health Nutr. 2012, 15, 1715–1727. [Google Scholar] [CrossRef]
- Zanello, G.; Srinivasan, C.S.; Shankar, B. What Explains Cambodia’s Success in Reducing Child Stunting-2000-2014? PLoS ONE 2016, 11, e0162668. [Google Scholar] [CrossRef]
- Headey, D.; Hoddinott, J.; Park, S. Drivers of nutritional change in four South Asian countries: A dynamic observational analysis. Matern. Child Nutr. 2016, 12, 210–218. [Google Scholar] [CrossRef]
- Headey, D.; Hoddinott, J.; Ali, D.; Tesfaye, R.; Dereje, M. The Other Asian Enigma: Explaining the Rapid Reduction of Undernutrition in Bangladesh. World Dev. 2015, 66, 749–761. [Google Scholar] [CrossRef]
- Headey, D.; Hoddinott, J.; Park, S. Accounting for nutritional changes in six success stories: A regression-decomposition approach. Glob. Food Secur. 2017, 13, 12–20. [Google Scholar] [CrossRef]
- Headey, D.D. Developmental Drivers of Nutritional Change: A Cross-Country Analysis. World Dev. 2013, 42, 76–88. [Google Scholar] [CrossRef]
- Milman, A.; Frongillo, E.A.; De Onis, M.; Hwang, J.-Y. Differential Improvement among Countries in Child Stunting Is Associated with Long-Term Development and Specific Interventions. J. Nutr. 2005, 135, 1415–1422. [Google Scholar] [CrossRef] [PubMed]
- Vollmer, S.; Harttgen, K.; Subramanyam, M.A.; Finlay, J.; Klasen, S.; Subramanian, S.V. Association between economic growth and early childhood undernutrition: Evidence from 121 Demographic and Health Surveys from 36 low-income and middle-income countries. Lancet Glob. Health 2014, 2, e225–e234. [Google Scholar] [CrossRef]
- Smith, L.C.; Haddad, L. How Potent Is Economic Growth in Reducing Undernutrition? What Are the Pathways of Impact? New Cross-Country Evidence. Econ. Dev. Cult. Chang. 2003, 51, 55–76. [Google Scholar] [CrossRef]
- Smith, L.C.; Haddad, L. Reducing Child Undernutrition: Past Drivers and Priorities for the Post-MDG Era. World Dev. 2015, 68, 180–204. [Google Scholar] [CrossRef]
- Corsi, D.J.; Neuman, M.; Finlay, J.E.; Subramanian, S. Demographic and health surveys: A profile. Int. J. Epidemiol. 2012, 41, 1602–1613. [Google Scholar] [CrossRef]
- WHO. WHO Child Growth Standards: Length/Height-for-Age, Weight-for-Age, Weight-for-Length, Weight-for-Height and Body Mass Index-for-Age: Methods and Development; World Health Organization, Department of Nutrition for Health and Development: Geneva, Switzerland, 2006. [Google Scholar]
- United Nation’s Children’s Fund (UNICEF). Strategy for Improved Nutrition of Children and Women in Developing Countries; Policy Review Paper; UNICEF: New York, NY, USA, 1990. [Google Scholar]
- Black, R.E.; Victora, C.G.; Walker, S.P.; Bhutta, Z.A.; Christian, P.; De Onis, M.; Ezzati, M.; Grantham-McGregor, S.; Katz, J.; Martorell, R.; et al. Maternal and child undernutrition and overweight in low-income and middle-income countries. Lancet 2013, 382, 427–451. [Google Scholar] [CrossRef]
- Croft, T.N.; Marshall, A.M.J.; Allen, C.K. Guide to DHS Statistics; ICF: Rockville, MD, USA, 2018. [Google Scholar]
- Fairbrother, M. Two Multilevel Modeling Techniques for Analyzing Comparative Longitudinal Survey Datasets. Political Sci. Res. Methods 2014, 2, 119–140. [Google Scholar] [CrossRef]
- McNeish, D.; Kelley, K. Fixed effects models versus mixed effects models for clustered data: Reviewing the approaches, disentangling the differences, and making recommendations. Psychol. Methods 2019, 24, 20–35. [Google Scholar] [CrossRef]
- Carlson, G.J.; Kordas, K.; Murray-Kolb, L.E. Associations between women’s autonomy and child nutritional status: A review of the literature. Matern. Child Nutr. 2015, 11, 452–482. [Google Scholar] [CrossRef]
- Lauer, J.M.; Duggan, C.P.; Ausman, L.M.; Griffiths, J.K.; Webb, P.; Bashaasha, B.; Agaba, E.; Turyashemererwa, F.M.; Ghosh, S. Unsafe Drinking Water Is Associated with Environmental Enteric Dysfunction and Poor Growth Outcomes in Young Children in Rural Southwestern Uganda. Am. J. Trop. Med. Hyg. 2018, 99, 1606–1612. [Google Scholar] [CrossRef]
- Lin, A.; Arnold, B.F.; Afreen, S.; Goto, R.; Huda, T.M.N.; Haque, R.; Raqib, R.; Unicomb, L.; Ahmed, T.; Colford, J.M.; et al. Household environmental conditions are associated with enteropathy and impaired growth in rural Bangladesh. Am. J. Trop. Med. Hyg. 2013, 89, 130–137. [Google Scholar] [CrossRef] [PubMed]
- Christian, P.; Lee, S.E.; Angel, M.D.; Adair, L.S.; Arifeen, S.E.; Ashorn, P.; Barros, F.C.; Fall, C.H.D.; Fawzi, W.W.; Hao, W.; et al. Risk of childhood undernutrition related to small-for-gestational age and preterm birth in low- and middle-income countries. Int. J. Epidemiol. 2013, 42, 1340–1355. [Google Scholar] [CrossRef] [PubMed]
- Ruel, M.T.; Menon, P. Child feeding practices are associated with child nutritional status in Latin America: Innovative uses of the demographic and health surveys. J. Nutr. 2002, 132, 1180–1187. [Google Scholar] [CrossRef] [PubMed]
- Arimond, M.; Ruel, M.T. Dietary diversity is associated with child nutritional status: Evidence from 11 demographic and health surveys. J. Nutr. 2004, 134, 2579–2585. [Google Scholar] [CrossRef] [PubMed]
- Krasevec, J.; An, X.; Kumapley, R.; Bégin, F.; Frongillo, E.A. Diet quality and risk of stunting among infants and young children in low- and middle-income countries. Matern. Child Nutr. 2017, 13, e12430. [Google Scholar] [CrossRef] [PubMed]
- Harding, K.L.; Aguayo, V.M.; Webb, P. Birthweight and feeding practices are associated with child growth outcomes in South Asia. Matern. Child Nutr. 2018, 14, e12650. [Google Scholar] [CrossRef] [PubMed]
- Darapheak, C.; Takano, T.; Kizuki, M.; Nakamura, K.; Seino, K. Consumption of animal source foods and dietary diversity reduce stunting in children in Cambodia. Int. Arch. Med. 2013, 6, 29. [Google Scholar] [CrossRef]
- Headey, D.; Hirvonen, K.; Hoddinott, J. Animal Sourced Foods and Child Stunting. Am. J. Agric. Econ. 2018, 100, 1302–1319. [Google Scholar] [CrossRef]
- Shapiro, M.J.; Downs, S.M.; Swartz, H.J.; Parker, M.; Quelhas, D.; Kreis, K.; Kraemer, K.; West, K.P.; Fanzo, J. A Systematic Review Investigating the Relation Between Animal-Source Food Consumption and Stunting in Children Aged 6-60 Months in Low and Middle-Income Countries. Adv. Nutr. 2019, 10, 827–847. [Google Scholar] [CrossRef]
- Simondon, K.B.; Simondon, F.; Costes, R.; Delaunay, V.; Diallo, A. Breast-feeding is associated with improved growth in length, but not weight, in rural Senegalese toddlers. Am. J. Clin. Nutr. 2001, 73, 959–967. [Google Scholar] [CrossRef]
- Habicht, J.P. The Association between Prolonged Breastfeeding and Poor Growth. In Short and Long Term Effects of Breast Feeding on Child Health. Advances in Experimental Medicine and Biology; Koletzko, B., Michaelsen, K.F., Hernell, O., Eds.; Springer: Boston, MA, USA, 2002; Volume 478. [Google Scholar]
- Marquis, G.S.; Habicht, J.P.; Lanata, C.F.; Black, R.; Rasmussen, K.M.; Black, R.E. Association of breastfeeding and stunting in Peruvian toddlers: An example of reverse causality. Int. J. Epidemiol. 1997, 26, 349–356. [Google Scholar] [CrossRef] [PubMed]
- Boerma, T.; Mathers, C.; AbouZahr, C.; Chatterji, S.; Hogan, D.; Stevens, G. Health in 2015: From MDGs, Millennium Development Goals to SDGs, Sustainable Development Goals; World Health Organization (WHO): Geneva, Switzerland, 2015. [Google Scholar]
| Variables | Definition |
|---|---|
| Outcome | |
| Stunting | Height/length-for-age z score value 2.0 SD below the median based on the WHO 2006 Child Growth Standards. |
| Distal Determinants | |
| Gini coefficient | A coefficient calculated from the DHS household wealth index score indicating the level of concentration of wealth among households in a country. Possible values range from 0 (being an equal distribution) to 1 (a totally unequal distribution) with higher values indicating more unequal distribution with a lower proportion of households controlling more of the wealth in the country. |
| Total fertility rate | The average number of births women (15–49 years) would have by the time they reach age 50 years based on the current age-specific fertility rate during the 3 years preceding the survey (excluding 1–36 months before the survey). |
| Urbanization | Percentage of total population living in urban areas. |
| Female primary education coverage | Percentage of women (15–49 years) who attended any level of primary education. |
| Male secondary education coverage | Percentage of men (15–49 years) who attended any level of secondary education. |
| Women decision making power | Percentage of currently married women (15–49 years) who usually make final decisions (alone or jointly with their husband) about their own healthcare, large household purchases, and visits to family or relatives. |
| Women work opportunity | Percentage of women (15–49 years) who worked in the past 7 days (including women who did not work in the past 7 days, but who are regularly employed and were absent from work for leave, illness, vacation, or any other reason) or worked in the past 12 months, but not currently. |
| Intermediate Health and Related Service Determinants | |
| Improved sanitation facility coverage | Percentage of total households with improved sanitation following the WHO/UNICEF Joint Monitoring Programme (JMP) for Water Supply, Sanitation and Hygiene. |
| Improved drinking water sources coverage | Percentage of total households with improved drinking water source following the WHO/UNICEF Joint Monitoring Programme (JMP) for Water Supply, Sanitation and Hygiene. |
| Antenatal care follow-up with ≥4 visits coverage | Percentage of women with a live birth in the 5 years preceding the survey who received ≥ 4 antenatal care visits for the most recent birth. |
| Delivery at health facility coverage | Percentage of live births to interviewed women in the 5 years preceding the survey delivered in a health facility. |
| Iron supplementation during pregnancy coverage | Percentage of women with a birth in the 5 years preceding the survey who took iron tablets or syrup (given or bought) during the pregnancy for the most recent live birth. |
| Children with all 8 basic vaccinations coverage | Percentage of living children (12–35 months) who received BCG, 3 doses of DPT-containing vaccine, 3 doses of polio vaccine (excluding polio vaccine given at birth), and 1 dose of MCV at any time, according to vaccination card or mother’s report. |
| Proximal Determinants | |
| Initiation of breastfeeding in ≤1 day | Percentage of last-born children who were born in the 2 years preceding the survey put to the breast within one day of birth. |
| Median duration of exclusive breastfeeding | Median duration (in months) of exclusive breastfeeding among children born in the past three years. |
| Complementary feeding between ages 6–9 months | Percentage of children (6–8 months) who were both breastfed and received complementary food (solid or semi-solid foods) in the 24 h preceding the interview. |
| Prevalence of reported low birthweight | Percentage of live births to interviewed women in the 5 years preceding the survey where the mother’s estimated baby’s size at time of birth as smaller than average. |
| Prevalence of acute respiratory infection (ARI) | Percentage of living children (0–59 months) with symptoms of ARI at any time in the 2 weeks preceding the survey. |
| Prevalence of diarrhea | Percentage of living children (0–59 months) with diarrhea at any time in the 2 weeks preceding the survey. |
| Characteristics | Statistics | |
|---|---|---|
| Surveys, n | 50 | |
| Countries, n | 14 | |
| Surveys per country, n | ||
| 3 rounds | 6 | |
| 4 rounds | 8 | |
| Countries with survey years | ||
| Bangladesh | 2004, 2007, 2011, 2014 | |
| Cambodia | 2000, 2005, 2010, 2014 | |
| Ethiopia | 2000, 2005, 2011,2016 | |
| Haiti | 2000, 2005, 2012, 2016 | |
| Kenya | 2003, 2008, 2014 | |
| Malawi | 2000, 2004, 2010, 2015 | |
| Mali | 2001, 2006, 2012 | |
| Nepal | 2001, 2006, 2011, 2016 | |
| Nigeria | 2003, 2008, 2013 | |
| Rwanda | 2000, 2005, 2010, 2014 | |
| Tanzania | 2004, 2010, 2015 | |
| Uganda | 2000, 2006, 2011, 2016 | |
| Zambia | 2001, 2007, 2013 | |
| Zimbabwe | 2005, 2010, 2015 | |
| Total sample size, n | 322,320 | |
| Children per survey, mean (range) | 6457 (2070–24,505) | |
| Child age (months), mean (SD) | 28.6 (17.2) | |
| Child sex (female), % | 49.8 | |
| Maternal age (years), mean (SD) | 28.7 (6.86) | |
| Variables | Average Annualized Rate of Change | |
|---|---|---|
| Beta (95% CI) | p | |
| Stunting prevalence in under-five children (%) | −1.04 (−1.24, −0.84) | <0.001 |
| Gini coefficient | −0.01 (−0.02, −0.01) | <0.001 |
| Total fertility rate (average number of births per women) | −0.07 (−0.09, −0.05) | <0.001 |
| Urbanization (%) | 0.61 (0.21, 1.00) | 0.003 |
| Female primary education (%) | 0.21 (−0.49, 0.91) | 0.560 |
| Male secondary education (%) | 0.13 (−0.05, 0.30) | 0.163 |
| Women’s decision-making power (%) | 2.31 (1.36, 3.26) | <0.001 |
| Women working (%) | −0.30 (−0.84, 0.25) | 0.286 |
| Improved sanitation facilities (%) | 1.87 (1.02, 2.72) | <0.001 |
| Improved drinking water sources (%) | 1.25 (0.66, 1.84) | <0.001 |
| Antenatal care follow-up with ≥4 visits (%) | 1.13 (0.53, 1.72) | <0.001 |
| Delivery at health facility (%) | 1.82 (1.17, 2.47) | <0.001 |
| Iron supplementation during pregnancy (%) | 0.39 (−2.59, 3.37) | 0.798 |
| Children with all 8 basic vaccinations (%) | 1.18 (0.98, 1.38) | <0.001 |
| Initiation of breastfeeding in ≤1 day (%) | 1.00 (0.66, 1.33) | <0.001 |
| Median duration of exclusive breastfeeding (months) | 0.08 (0.04, 0.12) | <0.001 |
| Complementary feeding between ages 6–9 months (%) | 0.32 (−0.21, 0.86) | 0.239 |
| Prevalence of reported low birthweight (%) | −0.18 (−0.58, 0.23) | 0.392 |
| Prevalence of acute respiratory illness (%) | −1.00 (−1.14, −0.86) | <0.001 |
| Prevalence of diarrhea (%) | −0.47 (−0.69, −0.26) | <0.001 |
| Indicators | Stunting | |
|---|---|---|
| Beta (95% CI) | p | |
| Distal determinants | ||
| Gini coefficient (SD) | 1.10 (0.29, 1.91) | 0.008 |
| Total fertility rate (SD) | 0.39 (−0.78, 1.56) | 0.513 |
| Urbanization (10%) | −0.67 (−1.21, −0.14) | 0.013 |
| Women primary education (10%) | −1.12 (−2.42, 0.18) | 0.092 |
| Male secondary education (10%) | −1.95 (−5.47, 1.56) | 0.275 |
| Women’s decision making (10%) | −0.36 (−0.69, −0.02) | 0.040 |
| Women’s working (10%) | −0.72 (−2.58, 1.15) | 0.450 |
| Intermediate service related determinants | ||
| Improved sanitation facilities (10%) | −1.40 (−2.17, −0.62) | <0.001 |
| Improved drinking water sources (10%) | −1.48 (−2.45, −0.52) | 0.003 |
| Antenatal care follow-up with ≥4 visits (10%) | 0.38 (−0.46, 1.23) | 0.377 |
| Delivery at health facility (10%) | 0.08 (−1.20, 1.36) | 0.907 |
| Iron supplementation during pregnancy (10%) | 0.21 (−0.14, 0.56) | 0.240 |
| Children with all 8 basic vaccinations (10%) | −1.74 (−2.53, −0.94) | <0.001 |
| Proximal determinants | ||
| Initiation of breastfeeding in ≤1 day (10%) | −1.17 (−1.62, −0.73) | <0.001 |
| Median duration of exclusive breastfeeding (SD) | 0.18 (−0.32, 0.68) | 0.473 |
| Complementary feeding b/n age 6–9 months (10%) | 0.75 (−0.53, 2.03) | 0.250 |
| Prevalence of reported low birthweight (10%) | 3.91 (2.40, 5.43) | <0.001 |
| Prevalence of acute respiratory illness (10%) | 1.28 (−1.40, 3.96) | 0.349 |
| Prevalence of diarrhea (10%) | −2.73 (−6.12, 0.65) | 0.113 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Argaw, A.; Hanley-Cook, G.; De Cock, N.; Kolsteren, P.; Huybregts, L.; Lachat, C. Drivers of Under-Five Stunting Trend in 14 Low- and Middle-Income Countries since the Turn of the Millennium: A Multilevel Pooled Analysis of 50 Demographic and Health Surveys. Nutrients 2019, 11, 2485. https://doi.org/10.3390/nu11102485
Argaw A, Hanley-Cook G, De Cock N, Kolsteren P, Huybregts L, Lachat C. Drivers of Under-Five Stunting Trend in 14 Low- and Middle-Income Countries since the Turn of the Millennium: A Multilevel Pooled Analysis of 50 Demographic and Health Surveys. Nutrients. 2019; 11(10):2485. https://doi.org/10.3390/nu11102485
Chicago/Turabian StyleArgaw, Alemayehu, Giles Hanley-Cook, Nathalie De Cock, Patrick Kolsteren, Lieven Huybregts, and Carl Lachat. 2019. "Drivers of Under-Five Stunting Trend in 14 Low- and Middle-Income Countries since the Turn of the Millennium: A Multilevel Pooled Analysis of 50 Demographic and Health Surveys" Nutrients 11, no. 10: 2485. https://doi.org/10.3390/nu11102485
APA StyleArgaw, A., Hanley-Cook, G., De Cock, N., Kolsteren, P., Huybregts, L., & Lachat, C. (2019). Drivers of Under-Five Stunting Trend in 14 Low- and Middle-Income Countries since the Turn of the Millennium: A Multilevel Pooled Analysis of 50 Demographic and Health Surveys. Nutrients, 11(10), 2485. https://doi.org/10.3390/nu11102485





