Exploring Views of Healthcare Professionals, Researchers, and People Living with and beyond Colorectal Cancer on a Healthy-Eating and Active Lifestyle Resource
Abstract
:1. Introduction
2. Materials and Methods
2.1. Population and Recruitment
2.1.1. Survivors of Colorectal Cancer
2.1.2. Professionals
2.1.3. Consent
2.1.4. Focus Groups
2.1.5. Telephone Interviews
2.2. Data Analysis
3. Results
3.1. General Feedback
3.2. Identified Themes Based on Focus Group Discussions and Telephone Interviews
3.2.1. Understanding the Behavior Change Concept
3.2.2. Contradictions in Fiber and Wholegrains Consumption
3.2.3. Malnutrition after CRC
3.2.4. Overwhelmed by Information
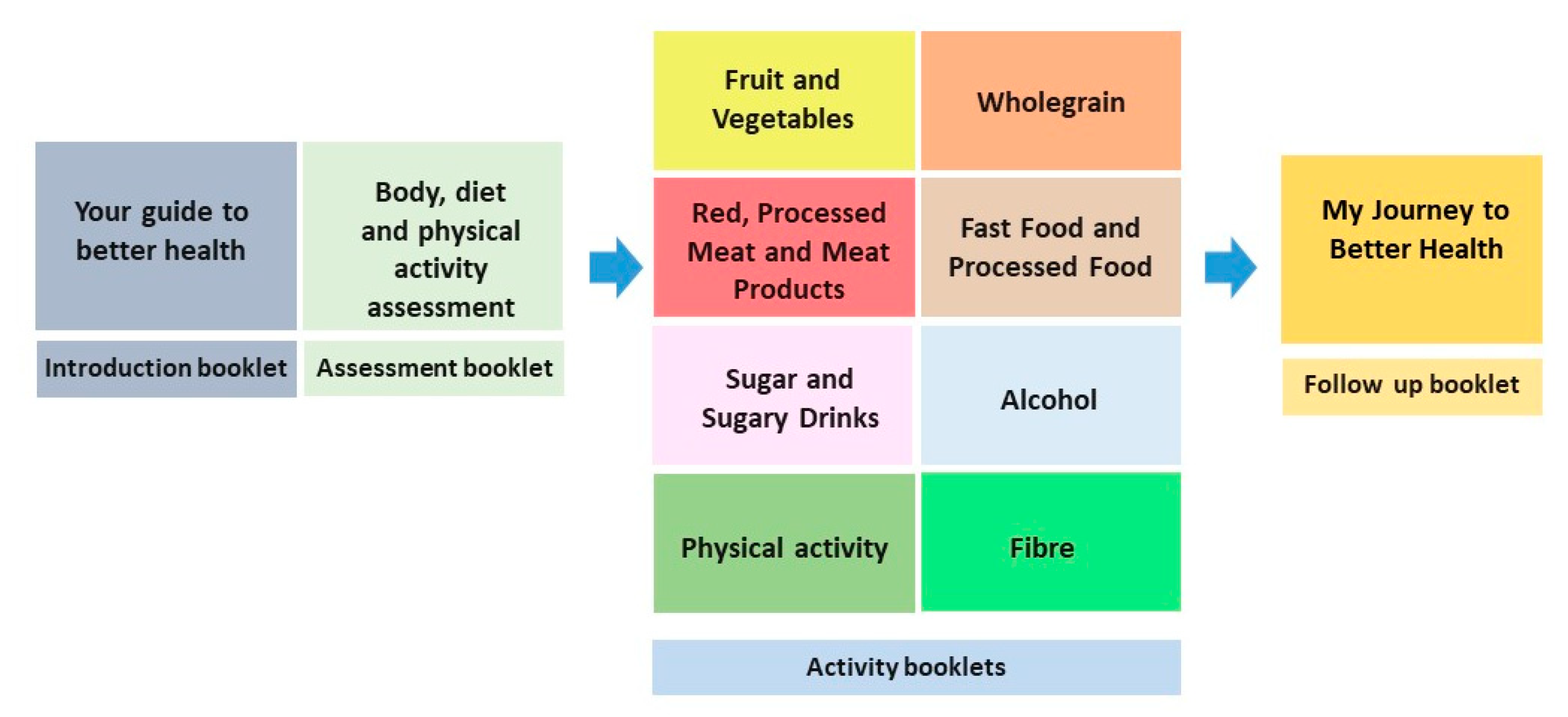
3.2.5. Resource Content
3.2.6. WCRF/AICR Guidelines on Prevention
3.2.7. Final Thoughts
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
Appendix B
Appendix C
References
- Arnold, M.; Sierra, M.S.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global patterns and trends in colorectal cancer incidence and mortality. Gut 2017, 66, 683–691. [Google Scholar] [CrossRef] [PubMed]
- Smittenaar, C.; Petersen, K.; Stewart, K.; Moitt, N. Cancer incidence and mortality projections in the UK until 2035. Br. J. Cancer 2016, 115, 1147. [Google Scholar] [CrossRef] [PubMed]
- Cancer Resarch UK. Bowel Cancer Statistics. Available online: https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/bowel-cancer#heading-Zero (accessed on 15 June 2019).
- Maddams, J.; Utley, M.; Møller, H. Projections of cancer prevalence in the United Kingdom, 2010–2040. Br. J. Cancer 2012, 107, 1195–1202. [Google Scholar] [CrossRef] [PubMed]
- Cuthbert, C.A.; Hemmelgarn, B.R.; Xu, Y.; Cheung, W.Y. The effect of comorbidities on outcomes in colorectal cancer survivors: A population-based cohort study. J. Cancer Surviv. 2018, 12, 733–743. [Google Scholar] [CrossRef]
- Johnson, C.B.; Davis, M.K.; Law, A.; Sulpher, J. Shared Risk Factors for Cardiovascular Disease and Cancer: Implications for Preventive Health and Clinical Care in Oncology Patients. Can. J. Cardiol. 2016, 32, 900–907. [Google Scholar] [CrossRef]
- Jabaaij, L.; van den Akker, M.; Schellevis, F.G. Excess of health care use in general practice and of comorbid chronic conditions in cancer patients compared to controls. BMC Fam. Pract. 2012, 13, 60. [Google Scholar] [CrossRef]
- Vergnaud, A.C.; Romaguera, D.; Peeters, P.H.; van Gils, C.H.; Chan, D.S.; Romieu, I.; Freisling, H.; Ferrari, P.; Clavel-Chapelon, F.; Fagherazzi, G.; et al. Adherence to the World Cancer Research Fund/American Institute for Cancer Research guidelines and risk of death in Europe: Results from the European Prospective Investigation into Nutrition and Cancer cohort study. Am. J. Clin. Nutr. 2013, 97, 1107–1120. [Google Scholar] [CrossRef]
- Van Blarigan, E.L.; Fuchs, C.S.; Niedzwiecki, D.; Zhang, S.; Saltz, L.B.; Mayer, R.J.; Mowat, R.B.; Whittom, R.; Hantel, A.; Benson, A.; et al. Association of survival with adherence to the American Cancer Society Nutrition and Physical Activity Guidelines for Cancer Survivors after colon cancer diagnosis: The CALGB 89803/Alliance trial. JAMA Oncol. 2018, 4, 783–790. [Google Scholar] [CrossRef]
- Demark-Wahnefried, W.; Aziz, N.M.; Rowland, J.H.; Pinto, B.M. Riding the crest of the teachable moment: Promoting long-term health after the diagnosis of cancer. J. Clin. Oncol. 2005, 23, 5814–5830. [Google Scholar] [CrossRef]
- National Cance Research Institute. The UK Top Living with and Beyond Cancer Research Priorities 2018. Available online: https://www.ncri.org.uk/lwbc/ (accessed on 25 July 2019).
- Hawkins, N.A.; Berkowitz, Z.; Rodriguez, J.L. Awareness of Dietary and Alcohol Guidelines among Colorectal Cancer Survivors. Am. J. Prev. Med. 2015, 49 (Suppl. 5), S509–S517. [Google Scholar] [CrossRef]
- Demark-Wahnefried, W.; Rogers, L.Q.; Alfano, C.M.; Thomson, C.A.; Courneya, K.S.; Meyerhardt, J.A.; Stout, N.L.; Kvale, E.; Ganzer, H.; Ligibel, J.A. Practical clinical interventions for diet, physical activity, and weight control in cancer survivors. CA Cancer J. Clin. 2015, 65, 167–189. [Google Scholar] [CrossRef] [PubMed]
- Demark-Wahnefried, W.; Clipp, E.C.; McBride, C.; Lobach, D.F.; Lipkus, I.; Peterson, B.; Clutter Snyder, D.; Sloane, R.; Arbanas, J.; Kraus, W.E. Design of FRESH START: A randomized trial of exercise and diet among cancer survivors. Med. Sci. Sports Exerc. 2003, 35, 415–424. [Google Scholar] [CrossRef] [PubMed]
- Beeken, R.J.; Croker, H.; Heinrich, M.; Smith, L.; Williams, K.; Hackshaw, A.; Hines, J.; Machesney, M.; Krishnaswamy, M.; Cavanagh, S.; et al. Study protocol for a randomised controlled trial of brief, habit-based, lifestyle advice for cancer survivors: Exploring behavioural outcomes for the Advancing Survivorship Cancer Outcomes Trial (ASCOT). BMJ Open 2016, 6, e011646. [Google Scholar] [CrossRef] [PubMed]
- Gordon, L.G.; Patrao, T.; Kularatna, S.; Hawkes, A.L. A telephone-delivered multiple health behaviour change intervention for colorectal cancer survivors: Making the case for cost-effective healthcare. Eur. J. Cancer Care 2015, 24, 854–861. [Google Scholar] [CrossRef] [PubMed]
- Palmer, N.R.; Bartholomew, L.K.; McCurdy, S.A.; Basen-Engquist, K.M.; Naik, A.D. Transitioning from active treatment: Colorectal cancer survivors’ health promotion goals. Palliat Support Care 2013, 11, 101–109. [Google Scholar] [CrossRef] [PubMed]
- Burden, S.; Sremanakova, J.; Jones, D.; Todd, C. Dietary interventions in cancer survivors. Proc. Nutr. Soc. 2018. [Google Scholar] [CrossRef] [PubMed]
- Aubrey, V.; Hon, Y.; Shaw, C.; Burden, S. Healthy eating interventions in adults living with and beyond colorectal cancer: A systematic review. J. Hum. Nutr. Diet. 2019, 32, 501–511. [Google Scholar] [CrossRef]
- Burden, S.; Gibson, D.J.; Todd, C.; Gratton, E.K.; Pilling, M.; Lal, S. Dietary interventions for adult cancer survivors (Protocol). Cochrane Database Syst. Rev. 2014. [Google Scholar] [CrossRef]
- Demark-Wahnefried, W.; Clipp, E.C.; Lipkus, I.M.; Lobach, D.; Snyder, D.C.; Sloane, R.; Peterson, B.; Macri, J.M.; Rock, C.L.; McBride, C.M.; et al. Main outcomes of the FRESH START trial: A sequentially tailored, diet and exercise mailed print intervention among breast and prostate cancer survivors. J. Clin. Oncol. 2007, 25, 2709–2718. [Google Scholar] [CrossRef]
- Pierce, J.P.; Natarajan, L.; Caan, B.J.; Parker, B.A.; Greenberg, E.R.; Flatt, S.W.; Rock, C.L.; Kealey, S.; Al-Delaimy, W.K.; Bardwell, W.A.; et al. Influence of a diet very high in vegetables, fruit, and fiber and low in fat on prognosis following treatment for breast cancer: The Women’s Healthy Eating and Living (WHEL) randomized trial. JAMA 2007, 298, 289–298. [Google Scholar] [CrossRef]
- Burden, S.T.; Stamataki, Z.; Hill, J.; Molasiotis, A.; Todd, C. An exploration of food and the lived experience of individuals after treatment for colorectal cancer using a phenomenological approach. J. Hum. Nutr. Diet. 2016, 29, 137–145. [Google Scholar] [CrossRef] [PubMed]
- Wright, S.J.; Gibson, D.; Eden, M.; Lal, S.; Todd, C.; Ness, A.; Burden, S. What are colorectal cancer survivors’ preferences for dietary advice? A best-worst discrete choice experiment. J. Cancer Surviv. 2017, 11, 782–790. [Google Scholar] [CrossRef] [PubMed]
- World Cancer Research Fund/American Institute for Cancer Research. Continuous Update Project Expert Report 2018. Diet, Nutrition, Physical Activity and Colorectal Cancer 2018. Available online: https://www.wcrf.org/sites/default/files/Colorectal-cancer-report.pdf (accessed on 2 June 2019).
- Weber, M.; Belala, N.; Clemson, L.; Boulton, E.; Hawley-Hague, H.; Becker, C.; Schwenk, M. Feasibility and Effectiveness of Intervention Programmes Integrating Functional Exercise into Daily Life of Older Adults: A Systematic Review. Gerontology 2018, 64, 172–187. [Google Scholar] [CrossRef] [PubMed]
- Schwarzer, R. The Health Action Process Approach (HAPA). Available online: http://www.hapa-model.de/ (accessed on 5 February 2019).
- Bandura, A. Self-Efficacy: The Exercise of Control; W H Freeman/Times Books/; Henry Holt Co.: New York, NY, USA, 1997. [Google Scholar]
- Ritchie, J.L.S. Qualitative Data Analysis for Applied Policy Research; Analysing Qualitative Data; Taylor Francis: London, UK, 1994; pp. 173–194. [Google Scholar]
- Krok-Schoen, J.L.; Palmer-Wackerly, A.L.; Dailey, P.M.; Wojno, J.C.; Krieger, J.L. Age Differences in Cancer Treatment Decision Making and Social Support. J. Aging Health 2017, 29, 187–205. [Google Scholar] [CrossRef]
- Niu, C.; Eng, L.; Qiu, X.; Shen, X.; Espin-Garcia, O.; Song, Y.; Pringle, D.; Mahler, M.; Halytskyy, O.; Charow, R.; et al. Lifestyle Behaviors in Elderly Cancer Survivors: A Comparison with Middle-Age Cancer Survivors. J. Oncol. Pract. 2015, 11, e450–e459. [Google Scholar] [CrossRef]
- McCreadie, C.; Tinker, A. The acceptability of assistive technology to older people. Ageing Soc. 2005, 25, 91–110. [Google Scholar] [CrossRef]

| General Characteristics n = 19 | |
|---|---|
| Age | 62 (SD 11.5) |
| Gender | |
| Female | 11 (58%) |
| Male | 8 (42%) |
| Ethnicity | White British |
| n = 13 * | |
| Marital status | |
| Married | 8 (61.5%) |
| Single | 3 (23.1%) |
| Divorced | 2 (15.4%) |
| Education level | |
| Degree | 5 (38.5%) |
| Higher education diploma | 4 (30.8%) |
| A level/GCSE | 3 (23.1%) |
| No formal education | 1 (7.6%) |
| Location of surgery | |
| Colon | 7 (53.8%) |
| Colon and rectum | 6 (46.2%) |
| Stoma | |
| Yes | 4 (30.8%) |
| No | 9 (69.2%) |
| Smoking status | |
| Active | 1 (7.7%) |
| Past | 2 (15.4%) |
| Never | 10 (76.9%) |
| Theme | People after Bowel Cancer | Professionals |
|---|---|---|
| Structure | ||
| Organization and explanation of tasks | “Structure clear and helpful” “Similar format in each booklet and familiarity when you open a new book” (Eva, 52). | “The structure is really nice, you explain the WCRF recommendation and then give them the guide and how they can plan their goals” (Dietitian 2). |
| Lay out | ||
| Font | “I really like the font and it’s big enough to read” (George 69). | Not reported |
| Layout | “I thought it is very attractive, colorful, easy to read, not too much text and appropriate language. It is a good product” (Rose, 65). | “I really like you have the rainbow there to write down the names of fruit and vegetables” (Occupational therapist). |
| Content | ||
| Background information | “It’s good for educational purposes as people have to change their lifestyle you know after operation” (Paul, 71). | “I like it, it is reasonable language and fairly straightforward” (Dietitian 4). |
| Portions guide | “I found very relevant and useful the portions in red meat booklet, as vegetarian it was useful for me to find out about protein” (Jane,41). | “I like the portion sizes. Everyone knows they should eat 5 a day but they do not know how much to eat” (Dietitian 3). |
| Healthy tips and swaps | “Useful to get you think about what you can swap” (Jason, 66). | “They have plenty of choices there and different ways to eat” (Researcher 1). |
| Setting goals and planning | “I like it. You can put in what you want to do and back track your goal with your diary” (Emma, 44). | “I love the way to plan the goals, very smart and easy. Patient can discover by reading the booklet, what they want to do and how” (Research nurse). |
| Body assessment | “I thought it is very important to have body assessment as I gained quite a lot of weight during my chemo” (Jane, 41). | Not reported |
| Daily activities and exercise | “Really like exercise booklet, would like to try the exercise and meal alternatives particularly. I would use booklet to improve my lifestyle” (Julia, 71). | “I think your pictures are excellent and the descriptions of the exercises explain the exercises well. I like the exercise record at the back and tips on how to sneak exercises into your routine” (Physiotherapist). |
| Using the booklets | “I am already using your booklets. I almost wish I could start in hospital and do changes in my diet” (Sofia, 74). | Not reported |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sremanakova, J.; Jones, D.; Cooke, R.; Burden, S. Exploring Views of Healthcare Professionals, Researchers, and People Living with and beyond Colorectal Cancer on a Healthy-Eating and Active Lifestyle Resource. Nutrients 2019, 11, 2482. https://doi.org/10.3390/nu11102482
Sremanakova J, Jones D, Cooke R, Burden S. Exploring Views of Healthcare Professionals, Researchers, and People Living with and beyond Colorectal Cancer on a Healthy-Eating and Active Lifestyle Resource. Nutrients. 2019; 11(10):2482. https://doi.org/10.3390/nu11102482
Chicago/Turabian StyleSremanakova, Jana, Debra Jones, Richard Cooke, and Sorrel Burden. 2019. "Exploring Views of Healthcare Professionals, Researchers, and People Living with and beyond Colorectal Cancer on a Healthy-Eating and Active Lifestyle Resource" Nutrients 11, no. 10: 2482. https://doi.org/10.3390/nu11102482
APA StyleSremanakova, J., Jones, D., Cooke, R., & Burden, S. (2019). Exploring Views of Healthcare Professionals, Researchers, and People Living with and beyond Colorectal Cancer on a Healthy-Eating and Active Lifestyle Resource. Nutrients, 11(10), 2482. https://doi.org/10.3390/nu11102482







