Diuretics, Ca-Antagonists, and Angiotensin-Converting Enzyme Inhibitors Affect Zinc Status in Hypertensive Patients on Monotherapy: A Randomized Trial
Abstract
:1. Introduction
2. Materials and Methods
2.1. Study Patients
2.2. Study Design
2.3. Anthropometry
2.4. Blood Pressure Measurement
2.5. Collection of Blood Samples
2.6. Collection of Urine Samples
2.7. Collection of Hair Samples
2.8. Mineral Determination
2.9. Biochemical Measurements
2.10. Statistical Analysis
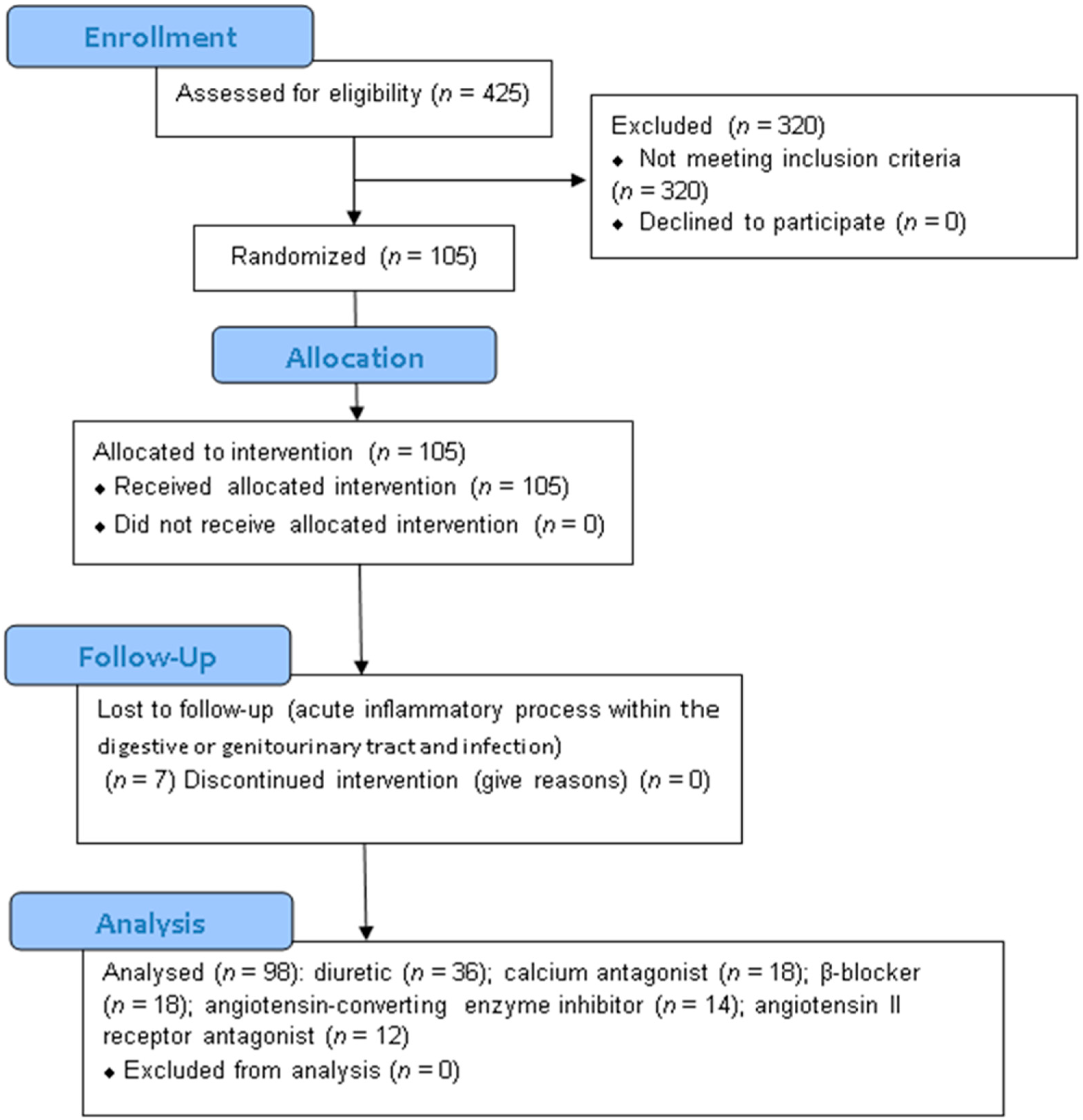
2.11. Randomization
3. Results
3.1. Blood Pressure Measurements
3.2. Mineral Measurements
3.3. Biochemical Measurements
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Wester, P.O. Urinary zinc excretion during treatment with different diuretics. Acta Med. Scand. 1980, 208, 209–212. [Google Scholar] [CrossRef] [PubMed]
- Khedun, S.M.; Naicker, T.; Maharaj, B. Zinc, hydrochlorothiazide and sexual dysfunction. Cent. Afr. J. Med. 1995, 41, 312–315. [Google Scholar] [PubMed]
- Rubio-Luengo, M.A.; Maldonado-Martín, A.; Gil-Extremera, B.; González-Gómez, L.; Luna del Castillo, J.D. Variations in magnesium and zinc in hypertensive patients receiving different treatments. Am. J. Hypertens. 1995, 8, 689–695. [Google Scholar] [CrossRef]
- Baykal, Y.; Yilmaz, M.I.; Celik, T.; Gok, F.; Rehber, H.; Akay, C.; Kocar, I.H. Effects of antihypertensive agents, alpha receptor blockers, beta blockers, angiotensin-converting enzyme inhibitors, angiotensin receptor blockers and calcium channel blockers, on oxidative stress. J. Hypertens. 2003, 21, 1207–1211. [Google Scholar] [CrossRef] [PubMed]
- Abu-Hamdan, D.K.; Desai, H.; Sondheimer, J.; Felicetta, J.; Mahajan, S.; Mcdonald, F. Taste acuity and zinc metabolism in captopril-treated hypertensive male patients. AJH 1988, 1, 303–308. [Google Scholar] [CrossRef]
- Golik, A.; Modai, D.; Averbukh, Z.; Sheffy, M.; Shamis, A.; Cohen, N.; Shaked, U.; Dolev, E. Zinc metabolism in patients treated with captopril versus enalapril. Metabolism 1990, 39, 665–667. [Google Scholar] [CrossRef]
- Golik, A.; Zaidenstein, R.; Dishi, V.; Blatt, A.; Cohen, N.; Cotter, G.; Berman, S.; Weissgarten, J. Effects of captopril and enalapril on zinc metabolism in hypertensive patients. J. Am. Coll. Nutr. 1998, 17, 75–78. [Google Scholar] [CrossRef] [PubMed]
- Tubek, S. Urinary zinc excretion is normalized in primary arterial hypertension after perindopril treatment. Biol. Trace Elem. Res. 2006, 114, 127–134. [Google Scholar] [CrossRef]
- Koren-Michowitz, M.; Dishy, V.; Zaidenstein, R.; Yona, O.; Berman, S.; Weissgarten, J.; Golik, A. The effect of losartan and losartan/hydrochlorothiazide fixed-combination on magnesium, zinc, and nitric oxide metabolism in hypertensive patients: A prospective open-label study. Am. J. Hypertens. 2005, 18, 358–363. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Braun, L.A.; Rosenfeldt, F. Pharmaco-nutrient interactions—A systematic review of zinc and antihypertensive therapy. Int. J. Clin. Pract. 2013, 67, 717–725. [Google Scholar] [CrossRef] [PubMed]
- Suliburska, J.; Bogdanski, P.; Szulińska, M.; Pupek-Musialik, D. The influence of antihypertensive drugs on mineral status in hypertensive patients. Eur. Rev. Med. Pharmacol. Sci. 2014, 18, 58–65. [Google Scholar] [PubMed]
- Suliburska, J.; Bogdański, P.; Pupek-Musialik, D.; Krejpcio, Z. Dietary intake and serum and hair concentrations of minerals and their relationship with serum lipids and glucose levels in hypertensive and obese patients with insulin resistance. Biol. Trace Elem. Res. 2011, 139, 137–150. [Google Scholar] [CrossRef] [PubMed]
- Marcinek, K.; Suliburska, J.; Krejpcio, Z.; Bogdański, P. Evaluation of mineral status hypertensive patients undergoing pharmacotherapy. Rocz. Panstw. Zakl. Hig. 2015, 66, 61–67. [Google Scholar] [PubMed]
- Ahmad, A.; Singhal, U.; Hossain, M.M.; Islam, N.; Rizvi, I. The role of the endogenous antioxidant enzymes and malondialdehyde in essential hypertension. J. Clin. Diagn. Res. 2013, 7, 987–990. [Google Scholar] [CrossRef] [PubMed]
- Moinuddin, G.; Inamdar, M.N.; Kulkarni, K.S.; Kulkarni, C. Modulation of haemodynamics, endogeneous antioxidant enzymes, and pathophysiological changes by selective inhibition of angiotensin II type 1 receptors in pressureoverload rats. Cardiovasc. J. Afr. 2013, 24, 58–65. [Google Scholar] [CrossRef] [PubMed]
- Zuo, X.L.; Chen, J.M.; Zhou, X.; Li, X.Z.; Mei, G.Y. Levels of selenium, zinc, copper, and antioxidant enzyme activity in patients with leukemia. Biol. Trace Elem. Res. 2006, 114, 41–54. [Google Scholar] [CrossRef]
- Davis, C.D.; Milne, D.B.; Nielsen, F.H. Changes in dietary zinc and copper affect zinc-status indicators of postmenopausal women, notably, extracellular superoxide dismutase and amyloid precursor proteins. Am. J. Clin. Nutr. 2000, 71, 781–788. [Google Scholar] [CrossRef] [PubMed]
- Mainous, A.G., III; Weinberg, E.D.; Diaz, V.A.; Johnson, S.P.; Hulihan, M.M.; Grant, A.M. Calcium channel blocker use and serum ferritin in adults with hypertension. BioMetals 2012, 25, 563–568. [Google Scholar] [CrossRef] [PubMed]
- Mancia, G.; Fagard, R.; Narkiewicz, K.; Redon, J.; Zanchetti, A.; Bohm, M.; Christiaens, T.; Cifkova, R.; De Backer, G.; Dominiczak, A.; et al. 2013 ESH/ESC Guidelines for the management of arterial hypertension. J. Hypertens. 2013, 31, 1281–1357. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- WHO. Waist Circumference and Waist-Hip Ratio: Report of a WHO Expert Consultation; WHO: Geneva, Switzerland, 2008. [Google Scholar]
- Tremblay, A.J.; Morrissette, H.; Gagné, J.-M.; Bergeron, J.; Gagné, C.; Couture, P. Validation of the Friedewald formula for the determination of low-density lipoprotein cholesterol compared with beta-quantification in a large population. Clin. Biochem. 2004, 37, 785–790. [Google Scholar] [CrossRef] [PubMed]
- Singh, R.B.; Niaz, M.A.; Rastogi, S.S.; Bajaj, S.; Gaoli, Z.; Shoumin, Z. Current zinc intake and risk of diabetes and coronary artery disease and factors associated with insulin resistance in rural and urban populations of North India. J. Am. Coll. Nutr. 1998, 17, 564–570. [Google Scholar] [CrossRef] [PubMed]
- Caldwell, K.L.; Pirkle, J.L. Laboratory Procedure Manual Serum Multi-Element ICP-DRC-MS. 2014. Available online: https://wwwn.cdc.gov/nchs/data/nhanes/2013-2014/labmethods/CUSEZN_H_met.pdf (accessed on 9 September 2018).
- Carpenter, W.E.; Lam, D.; Toney, G.M.; Weintraub, N.L.; Qin, Z. Zinc, copper, and blood pressure: Human population studies. Med. Sci. Monit. 2013, 19, 1–8. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dziegielewska, S.; Mackowiak, K.; Wysocka, E.; Torlinski, L. Serum copper and zinc status in elderly people with arterial hypertension. Now. Lek. 2013, 82, 9–18. [Google Scholar]
- Berridge, M.J. Regulation of ion channels by inositol trisphosphate and diacylglycerol. J. Exp. Biol. 1986, 124, 323–335. [Google Scholar] [PubMed]
- Henrotte, J.G.; Santarromana, M.; Franck, G.; Guicheney, P.; Boulu, R.; Bourdon, R. High cardiac zinc levels in spontaneously hypertensive rats. J. Hypertens. 1992, 10, 553–559. [Google Scholar] [CrossRef] [PubMed]
- Goodman, L.S.; Hardman, J.G.; Limbird, L.E.; Gilman, A.G. The Pharmacological Basis of Therapeutics; Goodman, L.S., Ed.; Goodman Gilman’s: New York, NY, USA, 2001; ISBN 0071354697. [Google Scholar]
- Suliburska, J.; Bogdanski, P.; Jakubowski, H. The influence of selected antihypertensive drugs on zinc, copper, and iron status in spontaneously hypertensive rats. Eur. J. Pharmacol. 2014, 738, 326–331. [Google Scholar] [CrossRef] [PubMed]
- Swislocki, A.L.M.; Kinney Lapier, T.L.; Khuu, D.T.; Fann, K.Y.; Tait, M.; Rodnick, K.J. Metabolic, hemodynamic, and cardiac effects of captopril in young, spontaneously hypertensive rats. Am. J. Hypertens. 1999, 12, 581–589. [Google Scholar] [CrossRef] [Green Version]
- Kataoka, C.; Egashira, K.; Ishibashi, M.; Inoue, S.; Ni, W.; Hiasa, K.; Kitamoto, S.; Usui, M.; Takeshita, A. Novel anti-inflammatory actions of amlodipine in a rat model of arteriosclerosis induced by long-term inhibition of nitric oxide synthesis. AJP Hear. Circ. Physiol. 2004, 286, 768H–774. [Google Scholar] [CrossRef] [PubMed]
- Suliburska, J.; Krejpcio, Z.; Staniek, H.; Król, E.; Bogdanski, P.; Kupsz, J.; Hertig, I. The Effects of Antihypertensive Drugs on Chromium Status, Glucose Metabolism, and Antioxidant and Inflammatory Indices in Spontaneously Hypertensive Rats. Biol. Trace Elem. Res. 2014, 157, 60–66. [Google Scholar] [CrossRef] [PubMed]
- Costa, R.M.; Filgueira, F.P.; Tostes, R.C.; Carvalho, M.H.C.; Akamine, E.H.; Lobato, N.S. H2O2 generated from mitochondrial electron transport chain in thoracic perivascular adipose tissue is crucial for modulation of vascular smooth muscle contraction. Vascul. Pharmacol. 2016, 84, 28–37. [Google Scholar] [CrossRef] [PubMed]
- Behringer, E.J.; Segal, S.S. Impact of Aging on Calcium Signaling and Membrane Potential in Endothelium of Resistance Arteries: A Role for Mitochondria. J. Gerontol. A Biol. Sci. Med. Sci. 2017, 72, 1627–1637. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Iturbe, B.; Sepassi, L.; Quiroz, Y.; Ni, Z.; Vaziri, N.D. Association of mitochondrial SOD deficiency with salt-sensitive hypertension and accelerated renal senescence. J. Appl. Physiol. 2007, 102, 255–260. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Siasos, G.; Tsigkou, V.; Kosmopoulos, M.; Theodosiadis, D.; Simantiris, S.; Tagkou, N.M.; Tsimpiktsioglou, A.; Stampouloglou, P.K.; Oikonomou, E.; Mourouzis, K.; et al. Mitochondria and cardiovascular diseases—from pathophysiology to treatment. Ann. Transl. Med. 2018, 6, 256. [Google Scholar] [CrossRef] [PubMed]
- Touyz, R.M. Reactive Oxygen Species, Vascular Oxidative Stress, and Redox Signaling in Hypertension: What Is the Clinical Significance? Hypertension 2004, 44, 248–252. [Google Scholar] [CrossRef] [PubMed]
- Cogliati, S.; Frezza, C.; Soriano, M.E.; Varanita, T.; Quintana-Cabrera, R.; Corrado, M.; Cipolat, S.; Costa, V.; Casarin, A.; Gomes, L.C.; et al. Mitochondrial Cristae Shape Determines Respiratory Chain Supercomplexes Assembly and Respiratory Efficiency. Cell 2013, 155, 160–171. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gongora, M.C.; Qin, Z.; Laude, K.; Kim, H.W.; McCann, L.; Folz, J.R.; Dikalov, S.; Fukai, T.; Harrison, D.G. Role of extracellular superoxide dismutase in hypertension. Hypertension 2006, 48, 473–481. [Google Scholar] [CrossRef] [PubMed]
- Ozumi, K.; Sudhahar, V.; Kim, H.W.; Chen, G.F.; Kohno, T.; Finney, L.; Vogt, S.; McKinney, R.D.; Ushio-Fukai, M.; Fukai, T. Role of copper transport protein antioxidant 1 in angiotensin ii-induced hypertension: A key regulator of extracellular superoxide dismutase. Hypertension 2012, 60, 476–486. [Google Scholar] [CrossRef] [PubMed]
- Vaziri, N.D. Protective effect of Nrf2 and catalase in maternal diabetes-induced perinatal hypertension and kidney disease. Diabetes 2012, 61, 2400–2402. [Google Scholar] [CrossRef] [PubMed]
- Shi, Y.; Lo, C.-S.; Chenier, I.; Maachi, H.; Filep, J.G.; Ingelfinger, J.R.; Zhang, S.-L.; Chan, J.S.D. Overexpression of catalase prevents hypertension and tubulointerstitial fibrosis and normalization of renal angiotensin-converting enzyme-2 expression in Akita mice. AJP Ren. Physiol. 2013, 304, F1335–F1346. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Sirivarasai, J.; Kaojarern, S.; Chanprasertyothin, S.; Panpunuan, P.; Petchpoung, K.; Tatsaneeyapant, A.; Yoovathaworn, K.; Sura, T.; Kaojarern, S.; Sritara, P. Environmental lead exposure, catalase gene, and markers of antioxidant and oxidative stress relation to hypertension: An analysis based on the EGAT study. Biomed. Res. Int. 2015, 2015, 856319. [Google Scholar] [CrossRef] [PubMed]
- Sundaram, A.; Siew Keah, L.; Sirajudeen, K.N.S.; Singh, H.J. Upregulation of catalase and downregulation of glutathione peroxidase activity in the kidney precede the development of hypertension in pre-hypertensive SHR. Hypertens. Res. 2013, 36, 213–218. [Google Scholar] [CrossRef] [PubMed]
- Dessy, C.; Feron, O. Pathophysiological roles of nitric oxide: In the heart and the coronary vasculature. Curr. Med. Chem. Anti-Inflamm. Anti-Allergy Agents 2004, 3, 207–216. [Google Scholar] [CrossRef]
- Pinheiro, L.C.; Tanus-Santos, J.E.; Castro, M.M. The potential of stimulating nitric oxide formation in the treatment of hypertension. Expert Opin. Ther. Targets 2017, 21, 543–556. [Google Scholar] [CrossRef] [PubMed]
| Parameter | Mean ± SD |
|---|---|
| N | 98 |
| Gender (F/M) | 61/37 |
| Age (year) | 53.6 ± 13.7 |
| BMI (kg/m2) | 33.3 ± 8.7 |
| WHR | 0.9 ± 0.1 |
| Monotherapy | n |
| Diuretic: | 36 |
| Indapamide | 29 |
| Torasemide | 5 |
| Spironolactone | 2 |
| Calcium antagonist | 18 |
| Amlodipine | 13 |
| Nitrendipine | 5 |
| β-blocker | 18 |
| Bisoprolol | 7 |
| Metoprolol | 7 |
| Nebivolol | 4 |
| Angiotensin-converting enzyme inhibitor | 14 |
| Perindopril | 9 |
| Captopril | 3 |
| Ramipril | 2 |
| Angiotensin II receptor antagonist | 12 |
| Losartan | 8 |
| Valsartan | 2 |
| Telmisartan | 2 |
| Parameter | Diuretics | Ca-Antagonists | β-Blockers | ACE-I | ARB | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| I Stage | II Stage | (Δ) | I Stage | II Stage | (Δ) | I Stage | II Stage | (Δ) | I Stage | II Stage | (Δ) | I Stage | II Stage | (Δ) | |
| SBP (mmHg) | 158.5 ± 16.1 | 136.7 ± 23.2 * | −0.14 | 161.9 ± 17.4 | 139.0 ± 13.3 * | −0.14 | 160.4 ± 17.9 | 141.6 ± 11.2 * | −0.12 | 162.1 ± 17.9 | 145.3 ± 13.8 * | −0.10 | 168.2 ± 21.1 | 146.2 ± 10.0 * | −0.13 |
| DBP (mmHg) | 91.3 ± 7.8 | 81.6 ± 9.2 * | −0.11 | 92.7 ± 8.5 | 86.4 ± 13.0 * | −0.07 | 90.1 ± 7.0 | 82.0 ± 5.5 * | −0.09 | 91.5 ± 8.1 | 80.6 ± 8.4 * | −0.12 | 95.4 ± 11.2 | 82.4 ± 10.8 * | −0.14 |
| TCH (mmol/L) | 5.9 ± 1.5 | 5.6 ± 1.1 | −0.05 | 5.1 ± 0.9 | 4.9 ± 1.3 | −0.04 | 4.8 ± 0.8 | 4.6 ± 1.0 | −0.04 | 5.4 ± 0.8 | 4.9 ± 0.8 | −0.09 | 5.7 ± 0.8 | 5.0 ± 1.2 | −0.12 |
| LDL (mmol/L) | 3.2 ± 0.9 | 3.4 ± 1.1 | 0.06 | 2.8 ± 0.7 | 2.7 ± 1.0 | −0.04 | 2.7 ± 0.6 | 2.7 ± 0.8 | 0.00 | 3.1 ± 0.6 | 2.9 ± 0.6 | −0.06 | 3.5 ± 0.8 | 2.7 ± 1.0 | −0.23 |
| HDL (mmol/L) | 1.5 ± 0.3 | 1.4 ± 0.3 | −0.07 | 1.4 ± 0.3 | 1.6 ± 0.6 | 0.14 | 1.3 ± 0.3 | 1.2 ± 0.3 | −0.08 | 1.3 ± 0.3 | 1.2 ± 0.4 | −0.08 | 1.5 ± 0.3 | 1.5 ± 0.3 | 0.00 |
| TG (mmol/L) | 1.9 ± 0.9 | 1.9 ± 0.9 | 0.00 | 1.9 ± 0.7 | 2.2 ± 0.3 | 0.16 | 1.8 ± 0.6 | 1.6 ± 0.6 | −0.11 | 2.5 ± 1.0 | 1.9 ± 0.6 * | −0.24 | 2.0 ± 0.6 | 1.5 ± 0.7 | −0.25 |
| Glu (mmol/L) | 5.4 ± 1.0 | 5.6 ± 1.1 | 0.04 | 5.3 ± 0.4 | 5.4 ± 0.8 | 0.02 | 5.8 ± 2.0 | 5.4 ± 1.2 | −0.07 | 5.6 ± 0.4 | 5.2 ± 0.3 | −0.07 | 5.7 ± 0.9 | 5.9 ± 1.4 | 0.04 |
| Alb (g/L) | 42.6 ± 4.1 | 42.5 ± 4.5 | 0.00 | 42.3 ± 4.1 | 44.1 ± 6.1 | 0.04 | 41.9 ± 5.3 | 41.3 ± 5.7 | −0.01 | 43.6 ± 3.3 | 43.4 ± 3.7 | 0.00 | 41.7 ± 4.8 | 42.3 ± 5.6 | 0.01 |
| CRP (mg/L) | 5.5 ± 2.4 | 5.0 ± 2.3 | −0.09 | 4.5 ± 1.6 | 4.1 ± 2.3 | −0.09 | 4.5 ± 2.7 | 4.8 ± 3.1 | 0.07 | 4.8 ± 2.0 | 4.5 ± 2.1 | −0.06 | 5.1 ± 1.8 | 4.9 ± 2.1 | −0.04 |
| TNF-α (pg/mL) | 4.4 ± 0.8 | 4.3 ± 0.8 | −0.02 | 4.9 ± 0.9 | 3.8 ± 0.7 * | −0.22 | 4.6 ± 0.7 | 4.4 ± 0.8 | −0.04 | 4.3 ± 0.8 | 4.4 ± 0.9 | 0.02 | 4.2 ± 0.8 | 3.9 ± 0.7 | −0.07 |
| Ferr (µg/L) | 122.1 ± 102.1 | 127.2 ± 105.2 | 0.04 | 191.6 ± 120.6 | 139.9 ± 95.5 | −0.27 | 115.1 ± 55.7 | 133.1 ± 117.8 | 0.16 | 128.4 ± 102.3 | 115.4 ± 94.1 | −0.10 | 115.1 ± 105.2 | 186.8 ± 118.9 | 0.62 |
| Cer (g/L) | 0.4 ± 0.1 | 0.4 ± 0.2 | 0.00 | 0.4 ± 0.2 | 0.5 ± 0.3 | 0.25 | 0.4 ± 0.2 | 0.5 ± 0.3 | 0.25 | 0.4 ± 0.2 | 0.3 ± 0.1 | −0.25 | 0.3 ± 0.05 | 0.3 ± 0.1 | 0.00 |
| TIBC (µmol/L) | 62.9 ± 11.5 | 58.7 ± 13.7 | −0.07 | 53.3 ± 5.6 | 54.3 ± 5.5 | 0.02 | 66.2 ± 2.7 | 57.9 ± 11.4 | −0.13 | 63.3 ± 12.1 | 53.4 ± 16.2 | −0.16 | 65.4 ± 9.9 | 54.9 ± 8.4 | −0.16 |
| NO (µmol/L) | 10.9 ± 3.4 | 14.9 ± 3.2 * | 0.37 | 11.1 ± 2.0 | 13.7 ± 0.9 | 0.23 | 10.1 ± 2.4 | 14.2 ± 3.6 * | 0.41 | 11.3 ± 1.0 | 16.0 ± 2.5 * | 0.42 | 10.1 ± 1.9 | 16.5 ± 1.8 * | 0.63 |
| CA (U/mL) | 4.4 ± 0.4 | 4.3 ± 0.5 | −0.02 | 4.4 ± 0.5 | 4.5 ± 0.4 | 0.02 | 4.6 ± 0.2 | 4.5 ± 0.2 | −0.02 | 4.5 ± 0.2 | 4.5 ± 0.2 | 0.00 | 4.8 ± 0.3 | 4.3 ± 0.5 | −0.10 |
| CAT (U/gHg) | 76.3 ± 10.1 | 60.2 ± 4.9 * | −0.21 | 76.9 ± 8.1 | 63.6 ± 5.3* | −0.17 | 75.7 ± 11.0 | 64.1 ± 4.1 * | −0.15 | 75.5 ± 3.5 | 61.9 ± 5.1 * | −0.18 | 70.9 ± 9.3 | 64.3 ± 5.8 | −0.09 |
| SOD (U/gHg) | 2301.9 ± 157.1 | 1908.6 ± 61.0 * | −0.17 | 2334.1 ± 159.1 | 1864.9 ± 54.2 * | −0.20 | 2279.6 ± 236.6 | 1699.9 ± 337.3 * | −0.25 | 2231.5 ± 250.3 | 1692.4 ± 342.5 * | −0.24 | 2170.1 ± 230.0 | 1865.1 ± 65.4 * | −0.14 |
| WBC (103/µL) | 7.4 ± 2.2 | 7.2 ± 2.1 | −0.03 | 6.8 ± 1.5 | 7.5 ± 1.7 * | 0.10 | 7.4 ± 2.0 | 7.4 ± 3.3 | 0.00 | 8.6 ± 2.3 | 8.2 ± 2.4 | −0.05 | 6.5 ± 1.1 | 8.2 ± 2.6 | 0.26 |
| RBC (106/µL) | 4.7 ± 0.3 | 4.7 ± 0.4 | 0.00 | 4.6 ± 0.4 | 4.6 ± 0.4 | 0.00 | 4.8 ± 0.3 | 4.7 ± 0.3 | −0.02 | 4.9 ± 0.3 | 4.8 ± 0.3 | −0.02 | 4.8 ± 0.4 | 4.7 ± 0.3 | −0.02 |
| Hgb (g/dL) | 9.0 ± 1.6 | 8.5 ± 0.5 | −0.06 | 8.6 ± 0.7 | 8.2 ± 0.7 | −0.05 | 9.4 ± 2.0 | 9.2 ± 1.9 | −0.02 | 9.1 ± 1.5 | 8.6 ± 0.7 | −0.05 | 9.3 ± 2.1 | 8.8 ± 0.6 | −0.05 |
| HCT (%) | 41.4 ± 3.1 | 41.5 ± 2.7 | 0.00 | 40.2 ± 3.1 | 40.6 ± 3.4 | 0.01 | 43.0 ± 2.0 | 41.1 ± 2.8 | −0.04 | 42.0 ± 2.9 | 42.5 ± 2.6 | 0.01 | 40.5 ± 4.4 | 41.6 ± 2.0 | 0.03 |
| Parameter | Diuretics | Ca-Antagonists | Β-blockers | ACE-I | ARB | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| I Stage | II Stage | (Δ) | I Stage | II Stage | (Δ) | I Stage | II Stage | (Δ) | I Stage | II Stage | (Δ) | I Stage | II Stage | (Δ) | |
| Serum (µmol/L) | |||||||||||||||
| Fe | 16.5 ± 7.0 | 17.7 ± 6.2 | 0.07 | 19.2 ± 6.8 | 18.8 ± 8.3 | −0.02 | 16.5 ± 6.1 | 16.7 ± 6.6 | 0.01 | 18.0 ± 8.1 | 17.9 ± 7.4 | −0.01 | 17.9 ± 5.0 | 18.5 ± 5.6 | 0.03 |
| Zn | 10.1 ± 1.5 | 9.1 ± 1.2 * | −0.10 | 9.8 ± 1.8 | 9.5 ± 1.5 | −0.03 | 9.9 ± 1.7 | 9.8 ± 1.5 | −0.01 | 10.2 ± 1.8 | 9.4 ± 1.5 * | −0.08 | 11.2 ± 1.8 | 9.9 ± 1.5 | −0.12 |
| Cu | 15.3 ± 2.0 | 15.5 ± 2.1 | 0.01 | 16.4 ± 3.1 | 16.3 ± 2.1 | −0.01 | 15.7 ± 3.0 | 15.2 ± 2.9 | −0.03 | 15.3 ± 2.1 | 17.2 ± 2.3 | 0.12 | 14.7 ± 1.6 | 15.0 ± 1.4 | 0.02 |
| Erythrocytes (µmol/g Hgb) | |||||||||||||||
| Fe | 48.9 ± 8.1 | 49.9 ± 8.7 | 0.02 | 51.2 ± 7.4 | 53.4 ± 8.3 | 0.04 | 48.8 ± 7.3 | 53.2 ± 9.5 | 0.09 | 49.8 ± 9.8 | 53.6 ± 12.0 | 0.08 | 49.6 ± 9.4 | 53.6 ± 11.2 | 0.08 |
| Zn | 0.5 ± 0.1 | 0.4 ± 0.1 * | −0.20 | 0.5 ± 0.1 | 0.4 ± 0.1 * | −0.20 | 0.5 ± 0.1 | 0.5 ± 0.1 | 0.00 | 0.4 ± 0.1 | 0.4 ± 0.1 | 0.00 | 0.4 ± 0.1 | 0.4 ± 0.1 | 0.00 |
| Cu | 44.0 ± 10.2 | 46.1 ± 10.6 | 0.05 | 40.3 ± 10.4 | 44.5 ± 11.0 | 0.10 | 41.6 ± 10.6 | 42.7 ± 9.7 | 0.03 | 41.9 ± 10.9 | 43.0 ± 10.2 | 0.03 | 44.6 ± 10.5 | 43.2 ± 9.6 | −0.03 |
| Urine (µmol/24 h) | |||||||||||||||
| Fe | 2.1 ± 1.2 | 2.3 ± 1.2 | 0.10 | 2.2 ± 0.9 | 2.1 ± 0.7 | −0.05 | 2.2 ± 0.8 | 3.1 ± 1.9 | 0.41 | 1.2 ± 0.2 | 1.6 ± 0.4 | 0.33 | 2.2 ± 0.9 | 2.0 ± 0.9 | −0.09 |
| Zn | 4.8 ± 2.0 | 7.2 ± 1.8 * | 0.50 | 6.0 ± 2.0 | 7.3 ± 2.1 | 0.22 | 5.2 ± 1.4 | 5.5 ± 1.2 | 0.06 | 5.6 ± 1.9 | 5.7 ± 2.0 | 0.02 | 6.4 ± 2.6 | 6.1 ± 1.9 | −0.05 |
| Cu | 0.7 ± 0.2 | 0.8 ± 0.2 | 0.14 | 0.8 ± 0.2 | 0.8 ± 0.2 | 0.00 | 0.7 ± 0.3 | 0.8 ± 0.3 | 0.14 | 0.8 ± 0.4 | 0.6 ± 0.1 | −0.25 | 1.0 ± 0.3 | 1.1 ± 0.3 | 0.10 |
| Hair (µg/g) | |||||||||||||||
| Fe | 16.0 ± 4.1 | 17.5 ± 4.0 | 0.09 | 14.4 ± 1.8 | 13.5 ± 1.7 | −0.06 | 13.9 ± 4.3 | 14.3 ± 4.9 | 0.03 | 17.6 ± 3.2 | 16.2 ± 3.3 | −0.08 | 9.8 ± 5.6 | 8.9 ± 5.4 | −0.09 |
| Zn | 134.9 ± 25.9 | 131.9 ± 24.8 | −0.02 | 123.2 ± 19.9 | 119.2 ± 19.1 | −0.03 | 135.1 ± 21.1 | 128.2 ± 20.1 | −0.05 | 109.8 ± 30.2 | 104.2 ± 28.9 | −0.05 | 122.2 ± 20.0 | 117.1 ± 19.3 | −0.04 |
| Cu | 14.9 ± 6.2 | 15.6 ± 6.4 | 0.05 | 14.3 ± 5.0 | 13.0 ± 4.1 | −0.09 | 20.1 ± 12.1 | 21.6 ± 13.1 | 0.07 | 15.7 ± 9.6 | 16.6 ± 10.5 | 0.06 | 20.7 ± 5.5 | 21.5 ± 6.1 | 0.04 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Suliburska, J.; Skrypnik, K.; Szulińska, M.; Kupsz, J.; Markuszewski, L.; Bogdański, P. Diuretics, Ca-Antagonists, and Angiotensin-Converting Enzyme Inhibitors Affect Zinc Status in Hypertensive Patients on Monotherapy: A Randomized Trial. Nutrients 2018, 10, 1284. https://doi.org/10.3390/nu10091284
Suliburska J, Skrypnik K, Szulińska M, Kupsz J, Markuszewski L, Bogdański P. Diuretics, Ca-Antagonists, and Angiotensin-Converting Enzyme Inhibitors Affect Zinc Status in Hypertensive Patients on Monotherapy: A Randomized Trial. Nutrients. 2018; 10(9):1284. https://doi.org/10.3390/nu10091284
Chicago/Turabian StyleSuliburska, Joanna, Katarzyna Skrypnik, Monika Szulińska, Justyna Kupsz, Leszek Markuszewski, and Paweł Bogdański. 2018. "Diuretics, Ca-Antagonists, and Angiotensin-Converting Enzyme Inhibitors Affect Zinc Status in Hypertensive Patients on Monotherapy: A Randomized Trial" Nutrients 10, no. 9: 1284. https://doi.org/10.3390/nu10091284
APA StyleSuliburska, J., Skrypnik, K., Szulińska, M., Kupsz, J., Markuszewski, L., & Bogdański, P. (2018). Diuretics, Ca-Antagonists, and Angiotensin-Converting Enzyme Inhibitors Affect Zinc Status in Hypertensive Patients on Monotherapy: A Randomized Trial. Nutrients, 10(9), 1284. https://doi.org/10.3390/nu10091284








