Dietary Carotenoids Intake and the Risk of Gastric Cancer: A Case—Control Study in Korea
Abstract
1. Introduction
2. Materials and Methods
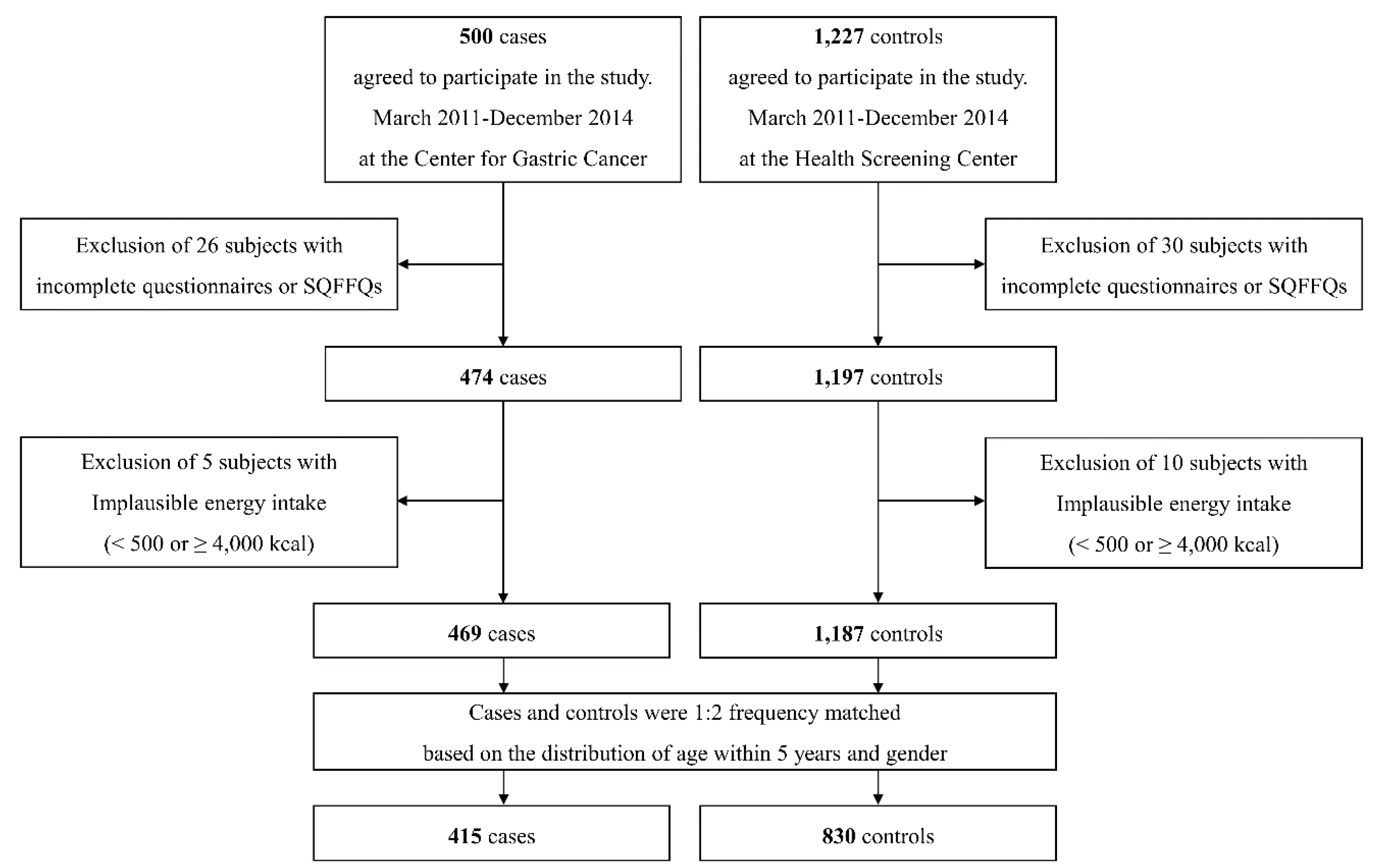
2.1. Study Population
2.2. Data Collection and Management
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Ferlay, J.; Soerjomataram, I.; Dikshit, R.; Eser, S.; Mathers, C.; Rebelo, M.; Parkin, D.M.; Forman, D.; Bray, F. Cancer incidence and mortality worldwide: Sources, methods and major patterns in GLOBOCAN 2012. Int. J. Cancer 2015, 136, E359–E386. [Google Scholar] [CrossRef] [PubMed]
- Jung, K.W.; Won, Y.J.; Kong, H.J.; Lee, E.S.; Kim, C.H.; Yoo, C.I.; Park, J.H.; Nam, H.S.; Huh, J.S.; Youm, J.H.; et al. Cancer statistics in Korea: Incidence, mortality, survival, and prevalence in 2015. Cancer Res. Treat. 2018, 50, 303–316. [Google Scholar] [CrossRef] [PubMed]
- International Agency for Research on Cancer, Schistosomes, Liver Flukes and Helicobacter pylori: IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. Volume 61. Available online: https://monographs.iarc.fr/ENG/Monographs/vol61/mono61.pdf (accessed on 31 March 2018).
- International Agency for Research on Cancer, Tobacco Smoke and Involuntary Smoking: IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. Volume 83. Available online: https://monographs.iarc.fr/ENG/Monographs/vol83/mono83.pdf (accessed on 31 March 2018).
- Doll, R.; Peto, R. The causes of cancer: Quantitative estimates of avoidable risks of cancer in the United States today. J. Natl. Cancer Inst. 1981, 66, 1192–1308. [Google Scholar] [CrossRef]
- Willett, W.C. Diet, nutrition, and avoidable cancer. Environ. Health Perspect. 1995, 103, 165–170. [Google Scholar] [CrossRef] [PubMed]
- Colquhoun, A.; Arnold, M.; Ferlay, J.; Goodman, K.; Forman, D.; Soerjomataram, I. Global patterns of cardia and non-cardia gastric cancer incidence in 2012. Gut 2015, 64, 1881–1888. [Google Scholar] [CrossRef] [PubMed]
- De Martel, C.; Parsonnet, J. Helicobacter pylori infection and gender: A meta-analysis of population-based prevalence surveys. Dig. Dis. Sci. 2006, 51, 2292–2301. [Google Scholar] [CrossRef] [PubMed]
- Freedman, N.; Derakhshan, M.; Abnet, C.; Schatzkin, A.; Hollenbeck, A.; McColl, K. Male predominance of upper gastrointestinal adenocarcinoma cannot be explained by differences in tobacco smoking in men versus women. Eur. J. Cancer 2010, 46, 2473–2478. [Google Scholar] [CrossRef] [PubMed]
- World Cancer Research Fund International. Diet, Nutrition, Physical Activity and Stomach Cancer; World Cancer Research Fund International: London, UK, 2018. [Google Scholar]
- Stange, C. Carotenoids in Nature: Biosynthesis, Regulation and Function; Springer Nature: Basel, Switzerland, 2016. [Google Scholar]
- Tanumihardjo, S.A. Carotenoids and Human Health; Humana Press: New York, NY, USA, 2013. [Google Scholar]
- Wardlaw, G.M.; Smith, A.M.; Lindeman, A.K. Contemporary Nutrition: A Functional Approach; McGraw-Hill: New York, NY, USA, 2010; Volume 2. [Google Scholar]
- Tanaka, T.; Shnimizu, M.; Moriwaki, H. Cancer chemoprevention by carotenoids. Molecules 2012, 17, 3202–3242. [Google Scholar] [CrossRef] [PubMed]
- Lissowska, J.; Gail, M.H.; Pee, D.; Groves, F.D.; Sobin, L.H.; Nasierowska Guttmejer, A.; Sygnowska, E.; Zatonski, W.; Blot, W.J.; Chow, W.H. Diet and stomach cancer risk in Warsaw, Poland. Nutr. Cancer 2004, 48, 149–159. [Google Scholar] [CrossRef] [PubMed]
- Pelucchi, C.; Tramacere, I.; Bertuccio, P.; Tavani, A.; Negri, E.; La Vecchia, C. Dietary intake of selected micronutrients and gastric cancer risk: An Italian case-control study. Ann. Oncol. 2008, 20, 160–165. [Google Scholar] [CrossRef] [PubMed]
- De S., E.; Boffetta, P.; Brennan, P.; Deneo Pellegrini, H.; Carzoglio, J.; Ronco, A.; Mendilaharsu, M. Dietary carotenoids and risk of gastric cancer: A case-control study in Uruguay. Eur. J. Cancer Prev. 2000, 9, 329–334. [Google Scholar]
- Larsson, S.C.; Bergkvist, L.; Näslund, I.; Rutegård, J.; Wolk, A. Vitamin A, retinol, and carotenoids and the risk of gastric cancer: A prospective cohort study. Am. J. Clin. Nutr. 2007, 85, 497–503. [Google Scholar] [CrossRef] [PubMed]
- Garcia Closas, R.; Gonzalez, C.A.; Agudo, A.; Riboli, E. Intake of specific carotenoids and flavonoids and the risk of gastric cancer in Spain. Cancer Cause Control 1999, 10, 71–75. [Google Scholar] [CrossRef]
- Harrison, L.E.; Zhang, Z.F.; Karpeh, M.S.; Sun, M.; Kurtz, R.C. The role of dietary factors in the intestinal and diffuse histologic subtypes of gastric adenocarcinoma: A case-control study in the US. Cancer 1997, 80, 1021–1028. [Google Scholar] [CrossRef]
- Botterweck, A.A.; Van den Brandt, P.A.; Goldbohm, R.A. Vitamins, carotenoids, dietary fiber, and the risk of gastric carcinoma: Results from a prospective study after 6.3 years of follow-up. Cancer 2000, 88, 737–748. [Google Scholar] [CrossRef]
- Ekström, A.M.; Serafini, M.; Nyrén, O.; Hansson, L.E.; Ye, W.; Wolk, A. Dietary antioxidant intake and the risk of cardia cancer and noncardia cancer of the intestinal and diffuse types: A population-based case-control study in Sweden. Int. J. Cancer 2000, 87, 133–140. [Google Scholar] [CrossRef]
- Mayne, S.T.; Risch, H.A.; Dubrow, R.; Chow, W.H.; Gammon, M.D.; Vaughan, T.L.; Farrow, D.C.; Schoenberg, J.B.; Stanford, J.L.; Ahsan, H. Nutrient intake and risk of subtypes of esophageal and gastric cancer. Cancer Epidemiol. Biomark. 2001, 10, 1055–1062. [Google Scholar]
- Nomura, A.M.; Hankin, J.H.; Kolonel, L.N.; Wilkens, L.R.; Goodman, M.T.; Stemmermann, G.N. Case-control study of diet and other risk factors for gastric cancer in Hawaii (United States). Cancer Cause Control 2003, 14, 547–558. [Google Scholar] [CrossRef]
- Terry, P.; Lagergren, J.; Ye, W.; Nyrén, O.; Wolk, A. Antioxidants and cancers of the esophagus and gastric cardia. Int. J. Cancer 2000, 87, 750–754. [Google Scholar] [CrossRef]
- Nouraie, M.; Pietinen, P.; Kamangar, F.; Dawsey, S.M.; Abnet, C.C.; Albanes, D.; Virtamo, J.; Taylor, P.R. Fruits, vegetables, and antioxidants and risk of gastric cancer among male smokers. Cancer Epidemiol. Biomark. 2005, 14, 2087–2092. [Google Scholar] [CrossRef] [PubMed]
- Hamilton, S.R.; Aaltonen, L.A. World Health Organization Classification of Tumors: Pathology and Genetics of Tumours of the Digestive System; IARC Press: Lyon, France, 2000. [Google Scholar]
- Ahn, Y.; Kwon, E.; Shim, J.; Park, M.; Joo, Y.; Kim, K.; Park, C.; Kim, D. Validation and reproducibility of food frequency questionnaire for Korean genome epidemiologic study. Eur. J. Clin. Nutr. 2007, 61, 1435–1441. [Google Scholar] [CrossRef] [PubMed]
- United States Department of Agriculture, USDA Food Composition Databases. Available online: https://ndb.nal.usda.gov/ndb/nutrients/index (accessed on 31 March 2018).
- Tables of Food Functional Composition, 1st ed.; Korea National Academy of Agricultural Science: Suwon, Korea, 2009.
- Willett, W.C. Nutritional Epidemiology; Oxford University Press: New York, NY, USA, 2013; Volume 3. [Google Scholar]
- Yang, T.; Yang, X.; Wang, X.; Wang, Y.; Song, Z. The role of tomato products and lycopene in the prevention of gastric cancer: A meta-analysis of epidemiologic studies. Med. Hypotheses 2013, 80, 383–388. [Google Scholar] [CrossRef] [PubMed]
- Zhou, Y.; Wang, T.; Meng, Q.; Zhai, S. Association of carotenoids with risk of gastric cancer: A meta-analysis. Clin. Nutr. 2016, 35, 109–116. [Google Scholar] [CrossRef] [PubMed]
- Murphy, M.M.; Barraj, L.M.; Herman, D.; Bi, X.; Cheatham, R.; Randolph, R.K. Phytonutrient intake by adults in the United States in relation to fruit and vegetable consumption. J. Am. Diet Assoc. 2012, 112, 222–229. [Google Scholar] [CrossRef]
- O’neill, M.; Carroll, Y.; Corridan, B.; Olmedilla, B.; Granado, F.; Blanco, I.; Van den Berg, H.; Hininger, I.; Rousell, A.; Chopra, M. A European carotenoid database to assess carotenoid intakes and its use in a five-country comparative study. Br. J. Nutr. 2001, 85, 499–507. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.S.; Cho, Y.H.; Park, J.; Shin, H.R.; Sung, M.K. Dietary intake of phytonutrients in relation to fruit and vegetable consumption in Korea. J. Acad. Nutr. Diet 2013, 113, 1194–1199. [Google Scholar] [CrossRef] [PubMed]
- Alda, L.M.; Gogoasa, I.; Bordean, D.M.; Gergen, I.; Alda, S.; Moldovan, C.; Nita, L. Lycopene content of tomatoes and tomato products. J. Agroaliment. Process. Technol. 2009, 15, 540–542. [Google Scholar]
- Tonucci, L.H.; Holden, J.M.; Beecher, G.R.; Khachik, F.; Davis, C.S.; Mulokozi, G. Carotenoid content of thermally processed tomato-based food products. J. Agric. Food Chem. 1995, 43, 579–586. [Google Scholar] [CrossRef]
- Story, E.N.; Kopec, R.E.; Schwartz, S.J.; Harris, G.K. An update on the health effects of tomato lycopene. Annu. Rev. Food Sci. Technol. 2010, 1, 189–210. [Google Scholar] [CrossRef] [PubMed]
- Rao, A.; Waseem, Z.; Agarwal, S. Lycopene content of tomatoes and tomato products and their contribution to dietary lycopene. Food Res. Int. 1998, 31, 737–741. [Google Scholar] [CrossRef]
- Correa, P.; Fontham, E.; Pickle, L.W.; Chen, V.; Lin, Y.; Haenszel, W. Dietary determinants of gastric cancer in south Louisiana inhabitants. J. Natl. Cancer Inst. 1985, 75, 645–654. [Google Scholar] [PubMed]
- Hansson, L.E.; Nyrén, O.; Bergström, R.; Wolk, A.; Lindgren, A.; Baron, J.; Adami, H.O. Diet and risk of gastric cancer. A population-based case-control study in Sweden. Int. J. Cancer 1993, 55, 181–189. [Google Scholar] [CrossRef] [PubMed]
- González, C.A.; Sanz, J.M.; Marcos, G.; Pita, S.; Brullet, E.; Saigi, E.; Badia, A.; Riboli, E. Dietary factors and stomach cancer in Spain: A multi-centre case-control study. Int. J. Cancer 1991, 49, 513–519. [Google Scholar] [CrossRef] [PubMed]
- Takezaki, T.; Gao, C.M.; Wu, J.Z.; Ding, J.H.; Liu, Y.T.; Zhang, Y.; Li, S.P.; Su, P.; Liu, T.K.; Tajima, K. Dietary protective and risk factors for esophageal and stomach cancers in a low-epidemic area for stomach cancer in Jiangsu Province, China: Comparison with those in a high-epidemic area. Jpn. J. Cancer Res. 2001, 92, 1157–1165. [Google Scholar] [CrossRef] [PubMed]
- Navarro Silvera, S.A.; Mayne, S.T.; Risch, H.; Gammon, M.D.; Vaughan, T.L.; Chow, W.H.; Dubrow, R.; Schoenberg, J.B.; Stanford, J.L.; West, A.B. Food group intake and risk of subtypes of esophageal and gastric cancer. Int. J. Cancer 2008, 123, 852–860. [Google Scholar] [CrossRef] [PubMed]
- Steevens, J.; Schouten, L.J.; Goldbohm, R.A.; Van den Brandt, P.A. Vegetables and fruits consumption and risk of esophageal and gastric cancer subtypes in the Netherlands cohort study. Int. J. Cancer 2011, 129, 2681–2693. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.J.; Kim, H. Anticancer effect of lycopene in gastric carcinogenesis. J. Cancer Prev. 2015, 20, 92–96. [Google Scholar] [CrossRef] [PubMed]
- Rao, A.V.; Rao, L.G. Carotenoids and human health. Pharmacol. Res. 2007, 55, 207–216. [Google Scholar] [CrossRef] [PubMed]
- Martí, R.; Roselló, S.; Cebolla Cornejo, J. Tomato as a source of carotenoids and polyphenols targeted to cancer prevention. Cancers 2016, 8, 58. [Google Scholar] [CrossRef] [PubMed]
| Total (n = 1245) | Men (n = 810) | Women (n = 435) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Controls (n = 830) | Cases (n = 415) | pb | Controls (n = 540) | Cases (n = 270) | pb | Controls (n = 290) | Cases (n = 145) | pb | |
| Age (years) | 53.7 ± 9.0 | 53.8 ± 9.3 | 0.892 | 54.8 ± 8.4 | 54.9 ± 8.7 | 0.905 | 51.6 ± 9.8 | 51.7 ± 10.0 | 0.942 |
| <50 | 285 (34.3) | 139 (33.5) | 0.816 | 153 (28.3) | 77 (28.5) | >0.999 | 132 (45.5) | 62 (42.8) | 0.658 |
| ≥50 | 545 (65.7) | 276 (66.5) | 387 (71.7) | 193 (71.5) | 158 (54.5) | 83 (57.2) | |||
| Male, n (%) | 540 (65.1) | 270 (65.1) | >0.999 | ||||||
| BMI (kg/m2) | 23.9 ± 2.9 | 23.9 ±3.0 | 0.627 | 24.4 ± 2.7 | 24.2 ± 3.0 | 0.390 | 23.1 ± 3.1 | 23.2 ± 3.0 | 0.533 |
| <23 | 314 (37.8) | 159 (38.3) | 0.975 | 161 (29.8) | 91 (33.7) | 0.509 | 153 (52.8) | 68 (46.9) | |
| 23–25 | 249 (30.0) | 122 (29.4) | 170 (31.5) | 78 (28.9) | 79 (27.2) | 44 (30.3) | |||
| ≥25 | 266 (32.1) | 133 (32.1) | 209 (38.7) | 101 (37.4) | 57 (19.7) | 32 (22.1) | |||
| H. pylori infection | |||||||||
| Positive | 486 (58.6) | 382 (92.1) | <0.001 | 333 (61.7) | 252 (93.3) | <0.001 | 153 (52.8) | 130 (89.7) | <0.001 |
| Negative | 320 (38.6) | 33 (8.0) | 187 (34.6) | 18 (6.7) | 133 (45.9) | 15 (10.3) | |||
| First-degree family history of GC | |||||||||
| Yes | 103 (12.4) | 82 (19.8) | 0.001 | 74 (13.7) | 60 (22.2) | 0.003 | 29 (10.0) | 22 (15.2) | 0.155 |
| No | 725 (87.4) | 332 (80.0) | 464 (85.9) | 209 (77.4) | 261 (90.0) | 123 (84.8) | |||
| Smoking status, n (%) | |||||||||
| Current-smoker | 162 (19.5) | 128 (30.8) | <0.001 | 157 (29.1) | 121 (44.8) | <0.001 | 5 (1.7) | 7 (4.8) | 0.021 |
| Ex-smoker | 284 (34.2) | 119 (28.7) | 277 (51.3) | 110 (40.7) | 7 (2.4) | 9 (6.2) | |||
| Non-smoker | 384 (46.3) | 167 (40.2) | 106 (19.6) | 39 (14.4) | 278 (95.9) | 128 (88.3) | |||
| Alcohol intake | |||||||||
| Current-drinker | 534 (64.3) | 254 (61.2) | 0.243 | 404 (74.8) | 193 (71.5) | 0.282 | 130 (44.8) | 61 (42.1) | 0.819 |
| Ex-drinker | 60 (7.2) | 41 (9.9) | 47 (8.7) | 33 (12.2) | 13 (4.5) | 8 (5.5) | |||
| Non-drinker | 236 (28.4) | 119 (28.7) | 89 (16.5) | 44 (16.3) | 147 (50.7) | 75 (51.7) | |||
| Regular exercise | |||||||||
| Yes | 466 (56.1) | 147 (35.4) | <0.001 | 303 (56.1) | 109 (40.4) | <0.001 | 163 (56.2) | 38 (26.2) | <0.001 |
| No | 361 (43.5) | 268 (64.6) | 234 (43.3) | 161 (59.6) | 127 (43.8) | 107 (73.8) | |||
| Education, n (%) | |||||||||
| Middle school or less | 119 (14.3) | 142 (34.2) | <0.001 | 71 (13.2) | 91 (33.7) | <0.001 | 48 (16.6) | 51 (35.2) | <0.001 |
| High school | 253 (30.5) | 174 (41.9) | 140 (25.9) | 112 (41.5) | 113 (39.0) | 62 (42.8) | |||
| College or more | 426 (51.3) | 97 (23.4) | 301 (55.7) | 66 (24.4) | 125 (43.1) | 31 (21.4) | |||
| Marital status, n (%) | |||||||||
| Married | 716 (86.3) | 361 (87.0) | 0.674 | 478 (88.5) | 243 (90.0) | 0.553 | 238 (82.1) | 118 (81.4) | >0.999 |
| Others | 113 (13.6) | 52 (12.5) | 61 (11.3) | 26 (9.6) | 52 (17.9) | 26 (17.9) | |||
| Occupation, n (%) | |||||||||
| Professional, administrative | 156 (18.8) | 70 (16.9) | 0.001 | 117 (21.7) | 59 (21.9) | 0.010 | 39 (13.5) | 11 (7.6) | 0.002 |
| Office, sales and service | 266 (32.1) | 122 (29.4) | 203 (37.6) | 81 (30.0) | 63 (21.7) | 41 (28.3) | |||
| Laborer, agricultural | 128 (15.4) | 104 (25.1) | 111 (20.6) | 83 (30.7) | 17 (5.9) | 21 (14.5) | |||
| Others, unemployed | 277 (33.4) | 117 (28.2) | 106 (19.6) | 46 (17.0) | 171 (59.0) | 71 (49.0) | |||
| Monthly household income, 10,000 won/month, n (%) | |||||||||
| <200 | 149 (18.0) | 133 (32.1) | <0.001 | 85 (15.7) | 85 (31.5) | <0.001 | 64 (22.1) | 48 (33.1) | 0.016 |
| 200–400 | 341 (41.1) | 148 (35.7) | 232 (43.0) | 106 (39.3) | 109 (37.6) | 42 (29.0) | |||
| >400 | 273 (32.9) | 96 (23.1) | 168 (31.1) | 55 (20.4) | 105 (36.2) | 41 (28.3) | |||
| Histological subtype of GC (Lauren’s classification) | |||||||||
| Intestinal | - | 158 (38.1) | - | - | 132 (48.9) | - | - | 26 (17.9) | - |
| Diffuse | - | 164 (39.5) | - | 77 (28.5) | - | 87 (60.0) | |||
| Mixed | - | 59 (14.2) | - | 40 (14.8) | - | 19 (13.1) | |||
| Indeterminate | - | 4 (1.0) | - | 3 (1.1) | - | 1 (0.7) | |||
| Total (n = 1245) | Men (n = 810) | Women (n = 435) | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Controls (n = 830) | Cases (n = 415) | pb | Controls (n = 540) | Cases (n = 270) | pb | Controls (n = 290) | Cases (n = 145) | pb | |
| Total energy intake (kcal) | 1713.6 ± 545.5 | 1924.1 ± 612.9 | <0.001 | 1760.6 ± 541.5 | 2038.5 ± 634.8 | <0.001 | 1626.0 ± 543.1 | 1711.1 ± 507.0 | 0.116 |
| Total carotenoid intake (μg/day) | |||||||||
| Total carotenoids | 12,121.5 ± 7762.4 | 10,799.2 ± 6987.1 | 0.003 | 10,785.7 ± 6632.5 | 9990.7 ± 6294.5 | 0.102 | 14,608.7 ± 9014.1 | 12,304.7 ± 7927.0 | 0.009 |
| α-Carotene | 947.5 ± 913.8 | 925.3 ± 966.0 | 0.692 | 839.8 ± 805.4 | 833.1 ± 861.7 | 0.913 | 1148.0 ± 1059.9 | 1096.9 ± 1118.1 | 0.642 |
| β-Carotene | 5075.9 ± 3276.2 | 4632.6 ± 3009.4 | 0.018 | 4529.7 ± 2682.8 | 4226.4 ± 2568.0 | 0.124 | 6093.1 ± 3971.2 | 5388.9 ± 3582.4 | 0.073 |
| β-Cryptoxanthin | 393.7 ± 438.8 | 330.5 ± 364.6 | 0.007 | 310.0 ± 269.7 | 314.3 ± 390.1 | 0.872 | 549.6 ± 615.7 | 360.6 ± 310.5 | <0.001 |
| Lutein/Zeaxanthin | 3531.7 ± 2584.6 | 3455.2 ± 2764.4 | 0.631 | 3256.6 ± 2200.2 | 3268.1 ± 2726.8 | 0.952 | 4044.0 ± 3119.2 | 3803.7 ± 2809.2 | 0.435 |
| Lycopene | 2218.0 ± 3847.2 | 1439.0 ± 2135.7 | <0.001 | 1869.8 ± 3433.0 | 1312.1 ± 2110.4 | 0.005 | 2866.4 ± 4452.9 | 1675.3 ± 2169.5 | <0.001 |
| Median Intake (μg/day) | No. of Controls/Cases | Model 1 | Model 2 | Model 3 | ||||
|---|---|---|---|---|---|---|---|---|
| OR | (95% CI) | OR | (95% CI) | OR | (95% CI) | |||
| Total Carotenoids | ||||||||
| Total (n = 1245) | ||||||||
| T1 | 6064.75 | 276/162 | 1.00 | 1.00 | 1.00 | |||
| T2 | 10,171.44 | 277/146 | 0.88 | (0.67–1.17) | 0.98 | (0.71–1.34) | 1.01 | (0.72–1.42) |
| T3 | 17,946.94 | 277/107 | 0.64 | (0.47–0.86) | 0.75 | (0.53–1.06) | 0.79 | (0.55–1.15) |
| p for trend b | 0.003 | 0.082 | 0.185 | |||||
| Men (n = 810) | ||||||||
| T1 | 5603.87 | 180/106 | 1.00 | 1.00 | 1.00 | |||
| T2 | 8921.20 | 180/88 | 0.83 | (0.58–1.17) | 0.95 | (0.63–1.43) | 1.09 | (0.70–1.68) |
| T3 | 15,850.62 | 180/76 | 0.71 | (0.49–1.02) | 0.78 | (0.51–1.20) | 0.84 | (0.54–1.33) |
| p for trend b | 0.073 | 0.236 | 0.386 | |||||
| Women (n = 435) | ||||||||
| T1 | 7151.14 | 96/74 | 1.00 | 1.00 | 1.00 | |||
| T2 | 12,377.35 | 97/38 | 0.50 | (0.31–0.81) | 0.51 | (0.30–0.88) | 0.51 | (0.29–0.91) |
| T3 | 21,678.14 | 97/33 | 0.43 | (0.26–0.71) | 0.56 | (0.32–0.99) | 0.65 | (0.35–1.18) |
| p for trend b | 0.001 | 0.051 | 0.169 | |||||
| α-Carotene | ||||||||
| Total (n = 1245) | ||||||||
| T1 | 321.92 | 276/151 | 1.00 | 1.00 | 1.00 | |||
| T2 | 665.17 | 277/136 | 0.90 | (0.67–1.19) | 0.99 | (0.71–1.36) | 0.94 | (0.67–1.33) |
| T3 | 1527.25 | 277/128 | 0.84 | (0.62–1.12) | 0.99 | (0.71–1.38) | 1.00 | (0.70–1.41) |
| p for trend b | 0.269 | 0.969 | 0.957 | |||||
| Men (n = 810) | ||||||||
| T1 | 291.35 | 180/100 | 1.00 | 1.00 | 1.00 | |||
| T2 | 587.52 | 180/78 | 0.78 | (0.54–1.12) | 0.95 | (0.63–1.44) | 0.95 | (0.61–1.48) |
| T3 | 1404.67 | 180/92 | 0.92 | (0.65–1.31) | 0.98 | (0.65–1.48) | 0.95 | (0.61–1.47) |
| p for trend b | 0.879 | 0.972 | 0.839 | |||||
| Women (n = 435) | ||||||||
| T1 | 427.91 | 96/52 | 1.00 | 1.00 | 1.00 | |||
| T2 | 853.57 | 97/42 | 0.80 | (0.49–1.31) | 0.84 | (0.48–1.48) | 0.83 | (0.46–1.50) |
| T3 | 1704.44 | 97/51 | 0.97 | (0.60–1.57) | 1.48 | (0.85–2.58) | 1.49 | (0.83–2.70) |
| p for trend b | 0.961 | 0.113 | 0.125 | |||||
| β-Carotene | ||||||||
| Total (n = 1245) | ||||||||
| T1 | 2574.39 | 276/162 | 1.00 | 1.00 | 1.00 | |||
| T2 | 4339.20 | 277/134 | 0.82 | (0.61–1.08) | 0.81 | (0.58–1.11) | 0.84 | (0.60–1.18) |
| T3 | 7353.32 | 277/119 | 0.71 | (0.53–0.96) | 0.77 | (0.55–1.08) | 0.85 | (0.59–1.22) |
| p for trend b | 0.030 | 0.158 | 0.426 | |||||
| Men (n = 810) | ||||||||
| T1 | 2447.55 | 180/100 | 1.00 | 1.00 | 1.00 | |||
| T2 | 3791.98 | 180/93 | 0.93 | (0.65–1.32) | 1.00 | (0.67–1.50) | 1.10 | (0.72–1.70) |
| T3 | 6504.49 | 180/77 | 0.76 | (0.53–1.10) | 0.76 | (0.49–1.17) | 0.89 | (0.56–1.41) |
| p for trend b | 0.136 | 0.179 | 0.535 | |||||
| Women (n = 435) | ||||||||
| T1 | 3178.03 | 96/68 | 1.00 | 1.00 | 1.00 | |||
| T2 | 5104.57 | 97/35 | 0.50 | (0.31–0.83) | 0.52 | (0.30–0.92) | 0.53 | (0.29–0.97) |
| T3 | 8683.53 | 97/42 | 0.60 | (0.37–0.97) | 0.73 | (0.42–1.25) | 0.79 | (0.44–1.41) |
| p for trend b | 0.062 | 0.351 | 0.551 | |||||
| β-Cryptoxanthin | ||||||||
| Total (n = 1245) | ||||||||
| T1 | 128.90 | 276/170 | 1.00 | 1.00 | 1.00 | |||
| T2 | 270.81 | 277/136 | 0.79 | (0.60–1.05) | 0.90 | (0.66–1.24) | 0.94 | (0.67–1.32) |
| T3 | 594.01 | 277/109 | 0.62 | (0.46–0.84) | 0.79 | (0.56–1.10) | 0.77 | (0.54–1.10) |
| p for trend b | 0.003 | 0.172 | 0.142 | |||||
| Men (n = 810) | ||||||||
| T1 | 116.88 | 180/104 | 1.00 | 1.00 | 1.00 | |||
| T2 | 229.41 | 180/86 | 0.83 | (0.58–1.18) | 0.86 | (0.57–1.30) | 0.96 | (0.62–1.49) |
| T3 | 483.12 | 180/80 | 0.77 | (0.54–1.10) | 0.85 | (0.56–1.29) | 0.92 | (0.59–1.43) |
| p for trend b | 0.180 | 0.502 | 0.717 | |||||
| Women (n = 435) | ||||||||
| T1 | 180.27 | 96/68 | 1.00 | 1.00 | 1.00 | |||
| T2 | 369.16 | 97/46 | 0.67 | (0.42–1.07) | 0.92 | (0.54–1.57) | 0.84 | (0.47–1.48) |
| T3 | 851.83 | 97/31 | 0.45 | (0.27–0.75) | 0.60 | (0.34–1.07) | 0.55 | (0.30–1.02) |
| p for trend b | 0.003 | 0.076 | 0.054 | |||||
| Lutein/Zeaxanthin | ||||||||
| Total (n = 1245) | ||||||||
| T1 | 1716.04 | 276/152 | 1.00 | 1.00 | 1.00 | |||
| T2 | 2832.71 | 277/135 | 0.88 | (0.66–1.17) | 0.93 | (0.67–1.28) | 1.00 | (0.71–1.41) |
| T3 | 5188.69 | 277/128 | 0.83 | (0.62–1.12) | 0.87 | (0.63–1.22) | 0.91 | (0.64–1.30) |
| p for trend b | 0.245 | 0.440 | 0.575 | |||||
| Men (n = 810) | ||||||||
| T1 | 1676.82 | 180/91 | 1.00 | 1.00 | 1.00 | |||
| T2 | 2691.75 | 180/89 | 0.98 | (0.68–1.40) | 1.18 | (0.78–1.79) | 1.41 | (0.91–2.20) |
| T3 | 4679.81 | 180/90 | 0.99 | (0.69–1.41) | 1.03 | (0.68–1.58) | 1.13 | (0.72–1.76) |
| p for trend b | 0.954 | 0.996 | 0.788 | |||||
| Women (n = 435) | ||||||||
| T1 | 1894.17 | 96/61 | 1.00 | 1.00 | 1.00 | |||
| T2 | 3268.31 | 97/39 | 0.63 | (0.38–1.03) | 0.60 | (0.35–1.05) | 0.64 | (0.36–1.15) |
| T3 | 5678.59 | 97/45 | 0.71 | (0.44–1.17) | 0.83 | (0.48–1.45) | 0.82 | (0.45–1.47) |
| p for trend b | 0.240 | 0.636 | 0.602 | |||||
| Lycopene | ||||||||
| Total (n = 1245) | ||||||||
| T1 | 327.68 | 276/209 | 1.00 | 1.00 | 1.00 | |||
| T2 | 1105.49 | 277/112 | 0.53 | (0.40–0.70) | 0.67 | (0.49–0.92) | 0.67 | (0.48–0.94) |
| T3 | 3666.52 | 277/94 | 0.44 | (0.33–0.59) | 0.57 | (0.41–0.80) | 0.60 | (0.42–0.85) |
| p for trend b | <0.001 | 0.003 | 0.012 | |||||
| Men (n = 810) | ||||||||
| T1 | 268.48 | 180/138 | 1.00 | 1.00 | 1.00 | |||
| T2 | 934.05 | 180/65 | 0.47 | (0.33–0.68) | 0.51 | (0.34–0.78) | 0.55 | (0.35–0.86) |
| T3 | 2963.59 | 180/67 | 0.49 | (0.34–0.69) | 0.60 | (0.40–0.91) | 0.60 | (0.39–0.93) |
| p for trend b | 0.001 | 0.056 | 0.062 | |||||
| Women (n = 435) | ||||||||
| T1 | 442.87 | 96/69 | 1.00 | 1.00 | 1.00 | |||
| T2 | 1528.34 | 97/46 | 0.66 | (0.41–1.05) | 0.77 | (0.45–1.31) | 0.81 | (0.46–1.42) |
| T3 | 4843.59 | 97/30 | 0.43 | (0.26–0.72) | 0.54 | (0.30–0.96) | 0.60 | (0.32–1.11) |
| p for trend b | 0.002 | 0.039 | 0.113 | |||||
| Median Intake (μg/day) | H. pylori-Positive (n = 868) | H. pylori-Negative (n = 353) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| No. of Controls/Cases | Model 1 | Model 2 | No. of Controls/Cases | Model 1 | Model 2 | ||||||
| OR | (95% CI) | OR | (95% CI) | OR | (95% CI) | OR | (95% CI) | ||||
| Lycopene | |||||||||||
| Total (n = 1221) | |||||||||||
| T1 | 327.68 | 169/194 | 1.00 | 1.00 | 100/15 | 1.00 | 1.00 | ||||
| T2 | 1105.49 | 166/100 | 0.52 | (0.37–0.72) | 0.60 | (0.42–0.86) | 102/12 | 0.75 | (0.33–1.69) | 1.23 | (0.48–3.18) |
| T3 | 3666.52 | 151/88 | 0.49 | (0.35–0.69) | 0.61 | (0.42–0.90) | 118/6 | 0.30 | (0.11–0.81) | 0.50 | (0.16–1.54) |
| p for trend b | <0.001 | 0.037 | 0.017 | 0.168 | |||||||
| Median Intake (μg/day) | Ever-Smoker (n = 693) b | Non-Smoker (n = 551) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| No. of Controls/Cases | Model 1 | Model 2 | No. of Controls/Cases | Model 1 | Model 2 | ||||||
| OR | (95% CI) | OR | (95% CI) | OR | (95% CI) | OR | (95% CI) | ||||
| Lycopene | |||||||||||
| Total (n = 1244) | |||||||||||
| T1 | 327.68 | 166/138 | 1.00 | 1.00 | 110/70 | 1.00 | 1.00 | ||||
| T2 | 1105.49 | 152/63 | 0.49 | (0.34–0.71) | 0.49 | (0.31–0.77) | 125/49 | 0.61 | (0.39–0.96) | 0.88 | (0.52–1.48) |
| T3 | 3666.52 | 128/46 | 0.40 | (0.26–0.60) | 0.39 | (0.23–0.65) | 149/48 | 0.49 | (0.32–0.77) | 0.75 | (0.45–1.27) |
| p for trend c | <0.001 | 0.001 | 0.006 | 0.307 | |||||||
| Food Consumption (g/day) | Total (n = 1245) | Men (n = 810) | Women (n = 435) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Cumulative (%) b | Controls (n = 830) | Cases (n = 415) | pc | Controls (n = 540) | Cases (n = 270) | pc | Controls (n = 290) | Cases (n = 145) | pc | |
| Watermelon | 34.56 | 21.02 ± 69.39 | 13.45 ± 21.73 | 0.004 | 15.25 ± 36.47 | 11.27 ± 21.19 | 0.050 | 31.75 ± 105.62 | 17.50 ± 22.22 | 0.028 |
| Tomato | 66.68 | 32.61 ± 90.50 | 14.71 ± 31.94 | <0.001 | 27.01 ± 91.31 | 12.68 ± 32.60 | 0.001 | 43.05 ± 88.19 | 18.50 ± 30.43 | <0.001 |
| Tomato ketchup | 90.26 | 5.64 ± 15.31 | 2.62 ± 5.67 | <0.001 | 4.71 ± 15.51 | 2.28 ± 5.79 | 0.001 | 7.38 ± 14.81 | 3.25 ± 5.40 | <0.001 |
| Range (g/day) | Median Intake (g/day) | No. of Controls/Cases | Model 1 | Model 2 | Model 3 | ||||
|---|---|---|---|---|---|---|---|---|---|
| OR | (95% CI) | OR | (95% CI) | OR | (95% CI) | ||||
| Watermelon | |||||||||
| Total (n = 1245) | |||||||||
| T1 | <3.91 | 1.47 | 276/188 | 1.00 | 1.00 | 1.00 | |||
| T2 | 3.91–13.59 | 7.23 | 277/116 | 0.61 | (0.46–0.81) | 0.75 | (0.54–1.04) | 0.73 | (0.52–1.03) |
| T3 | ≥13.59 | 29.32 | 277/111 | 0.58 | (0.43–0.77) | 0.77 | (0.55–1.07) | 0.71 | (0.50–1.02) |
| p for trend a | 0.002 | 0.233 | 0.130 | ||||||
| Men (n = 810) | |||||||||
| T1 | <3.16 | 1.30 | 180/121 | 1.00 | 1.00 | 1.00 | |||
| T2 | 3.16–10.63 | 5.34 | 180/75 | 0.62 | (0.44–0.88) | 0.75 | (0.50–1.13) | 0.78 | (0.51–1.20) |
| T3 | ≥10.63 | 24.63 | 180/74 | 0.61 | (0.43–0.87) | 0.84 | (0.56–1.27) | 0.78 | (0.50–1.21) |
| p for trend a | 0.034 | 0.657 | 0.391 | ||||||
| Women (n = 435) | |||||||||
| T1 | <6.14 | 2.50 | 96/63 | 1.00 | 1.00 | 1.00 | |||
| T2 | 6.14–22.08 | 11.35 | 97/42 | 0.66 | (0.41–1.07) | 0.80 | (0.46–1.40) | 0.83 | (0.46–1.51) |
| T3 | ≥22.08 | 43.54 | 97/40 | 0.63 | (0.39–1.02) | 0.76 | (0.44–1.34) | 0.77 | (0.42–1.39) |
| p for trend a | 0.117 | 0.421 | 0.440 | ||||||
| Tomato | |||||||||
| Total (n = 1245) | |||||||||
| T1 | <4.70 | 1.70 | 276/217 | 1.00 | 1.00 | 1.00 | |||
| T2 | 4.70–20.12 | 10.15 | 277/120 | 0.55 | (0.41–0.72) | 0.66 | (0.48–0.90) | 0.66 | (0.47–0.91) |
| T3 | ≥20.12 | 47.87 | 277/78 | 0.34 | (0.25–0.47) | 0.54 | (0.38–0.77) | 0.59 | (0.41–0.85) |
| p for trend a | <0.001 | 0.002 | 0.016 | ||||||
| Men (n = 810) | |||||||||
| T1 | <4.03 | 1.33 | 180/144 | 1.00 | 1.00 | 1.00 | |||
| T2 | 4.03–16.68 | 8.75 | 180/72 | 0.50 | (0.35–0.71) | 0.67 | (0.45–1.00) | 0.64 | (0.42–0.99) |
| T3 | ≥16.68 | 35.92 | 180/54 | 0.37 | (0.26–0.54) | 0.57 | (0.37–0.88) | 0.58 | (0.37–0.92) |
| p for trend a | <0.001 | 0.022 | 0.043 | ||||||
| Women (n = 435) | |||||||||
| T1 | <6.13 | 2.74 | 96/67 | 1.00 | 1.00 | 1.00 | |||
| T2 | 6.13–30.90 | 14.03 | 97/54 | 0.79 | (0.50–1.25) | 0.98 | (0.58–1.65) | 0.97 | (0.56–1.68) |
| T3 | ≥30.90 | 63.63 | 97/24 | 0.34 | (0.20–0.60) | 0.47 | (0.25–0.87) | 0.57 | (0.30–1.12) |
| p for trend a | <0.001 | 0.010 | 0.084 | ||||||
| Tomato ketchup | |||||||||
| Total (n = 1245) | |||||||||
| T1 | <0.84 | 0.30 | 276/217 | 1.00 | 1.00 | 1.00 | |||
| T2 | 0.84–3.58 | 1.81 | 277/123 | 0.56 | (0.42–0.74) | 0.66 | (0.49–0.90) | 0.66 | (0.48–0.92) |
| T3 | ≥3.58 | 8.34 | 277/75 | 0.33 | (0.24–0.45) | 0.51 | (0.36–0.72) | 0.55 | (0.38–0.80) |
| p for trend a | <0.001 | 0.001 | 0.005 | ||||||
| Men (n = 810) | |||||||||
| T1 | <0.71 | 0.24 | 180/140 | 1.00 | 1.00 | 1.00 | |||
| T2 | 0.71–2.98 | 1.52 | 180/75 | 0.54 | (0.38–0.76) | 0.72 | (0.49–1.08) | 0.69 | (0.45–1.06) |
| T3 | ≥2.98 | 6.45 | 180/55 | 0.39 | (0.27–0.57) | 0.61 | (0.40–0.94) | 0.62 | (0.39–0.97) |
| p for trend a | <0.001 | 0.039 | 0.067 | ||||||
| Women (n = 435) | |||||||||
| T1 | <1.08 | 0.50 | 96/67 | 1.00 | 1.00 | 1.00 | |||
| T2 | 1.08–5.19 | 2.43 | 97/54 | 0.79 | (0.50–1.25) | 0.97 | (0.58–1.64) | 0.96 | (0.56–1.67) |
| T3 | ≥5.19 | 10.94 | 97/24 | 0.34 | (0.20–0.60) | 0.47 | (0.25–0.88) | 0.58 | (0.30–1.12) |
| p for trend a | <0.001 | 0.011 | 0.089 | ||||||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kim, J.H.; Lee, J.; Choi, I.J.; Kim, Y.-I.; Kwon, O.; Kim, H.; Kim, J. Dietary Carotenoids Intake and the Risk of Gastric Cancer: A Case—Control Study in Korea. Nutrients 2018, 10, 1031. https://doi.org/10.3390/nu10081031
Kim JH, Lee J, Choi IJ, Kim Y-I, Kwon O, Kim H, Kim J. Dietary Carotenoids Intake and the Risk of Gastric Cancer: A Case—Control Study in Korea. Nutrients. 2018; 10(8):1031. https://doi.org/10.3390/nu10081031
Chicago/Turabian StyleKim, Ji Hyun, Jeonghee Lee, Il Ju Choi, Young-Il Kim, Oran Kwon, Hyesook Kim, and Jeongseon Kim. 2018. "Dietary Carotenoids Intake and the Risk of Gastric Cancer: A Case—Control Study in Korea" Nutrients 10, no. 8: 1031. https://doi.org/10.3390/nu10081031
APA StyleKim, J. H., Lee, J., Choi, I. J., Kim, Y.-I., Kwon, O., Kim, H., & Kim, J. (2018). Dietary Carotenoids Intake and the Risk of Gastric Cancer: A Case—Control Study in Korea. Nutrients, 10(8), 1031. https://doi.org/10.3390/nu10081031






