Iron Status and Gestational Diabetes—A Meta-Analysis
Abstract
1. Introduction
2. Methods
2.1. Study Strategy
2.2. Exposure
2.3. Outcomes
2.4. Inclusion Criteria
2.5. Exclusion Criteria
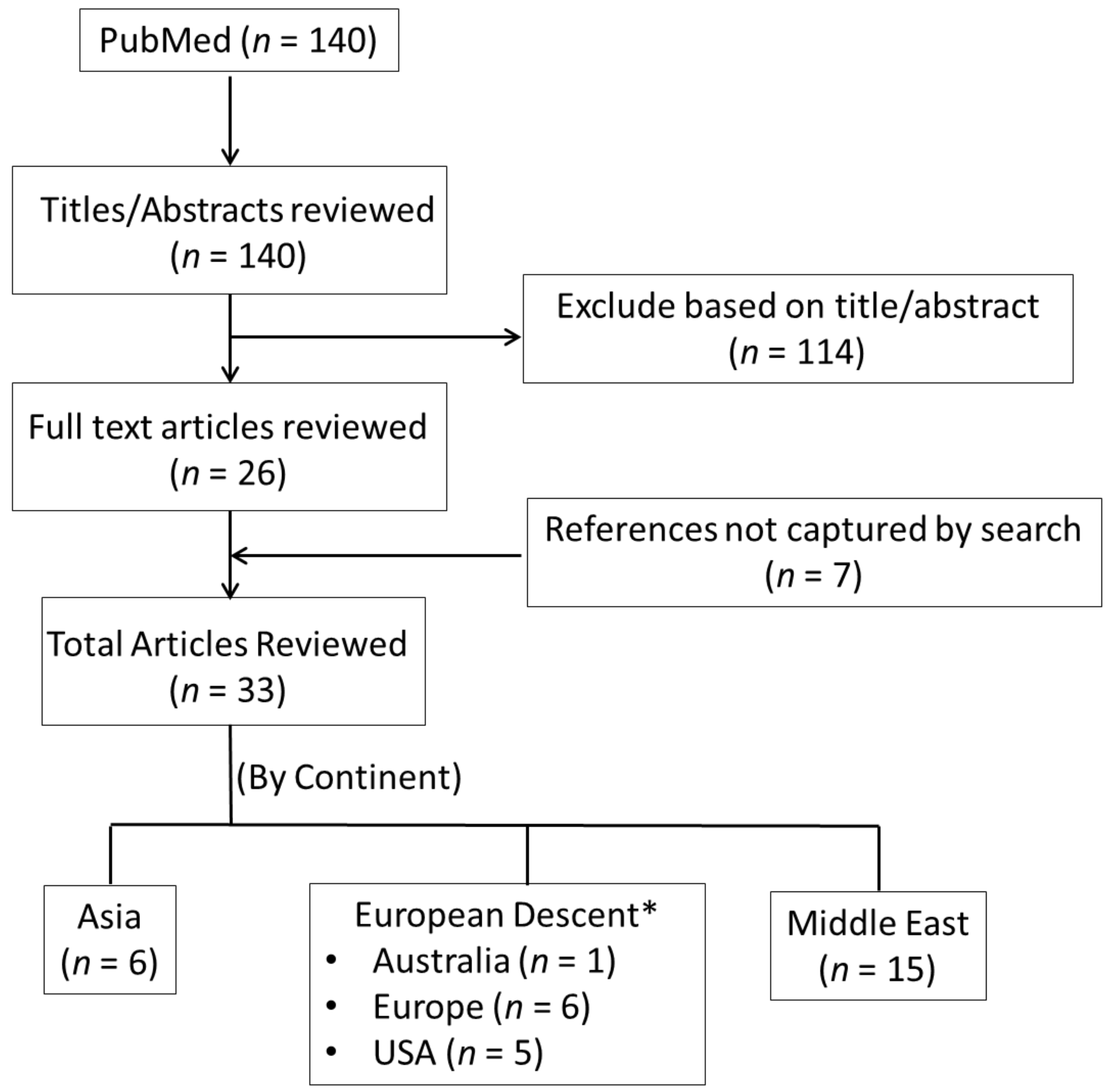
2.6. Study Selection Process
2.7. Risk of Bias and Study Quality Assessment
2.8. Data Extraction
2.9. Data Synthesis and Meta-Analysis
3. Results
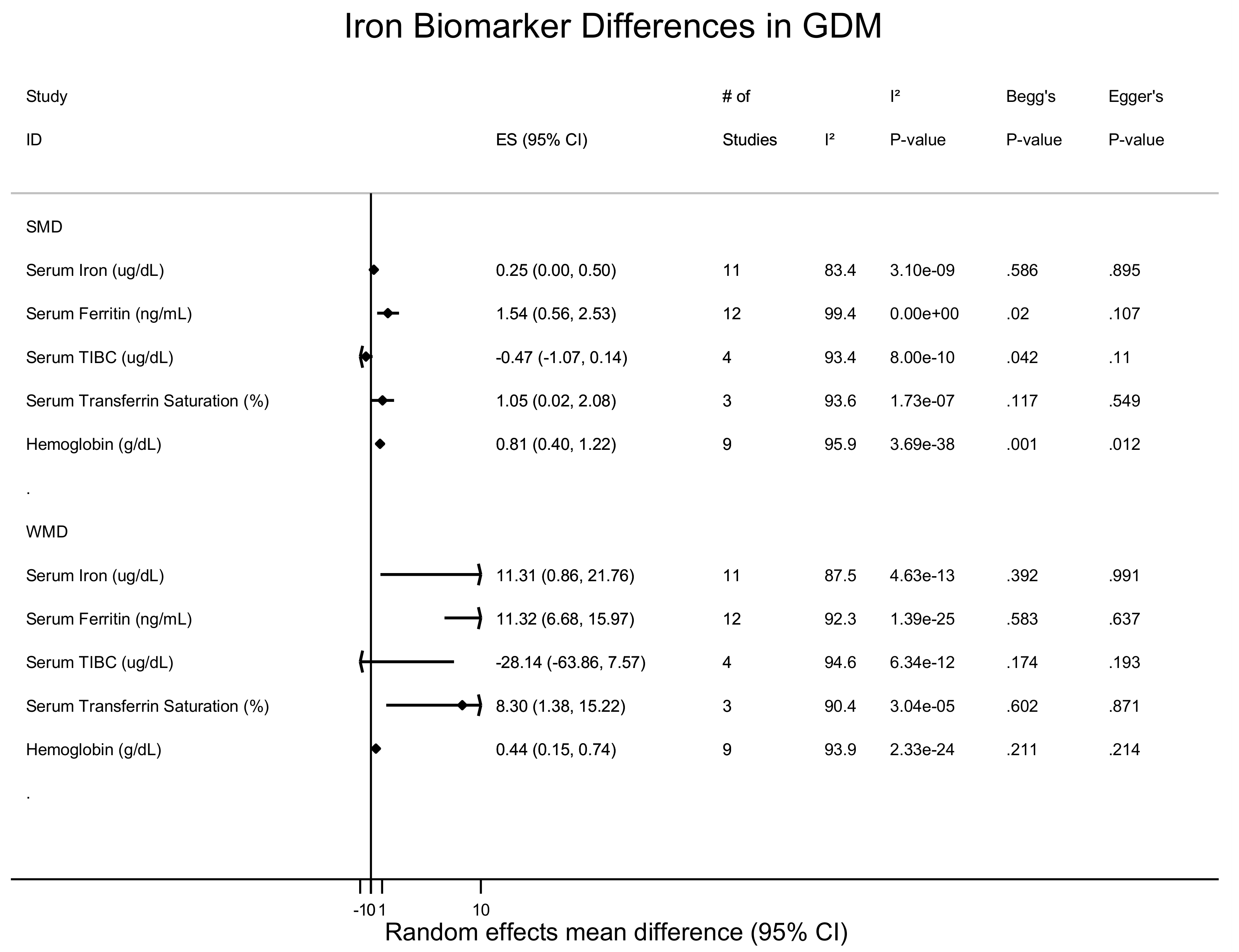
3.1. Serum Iron
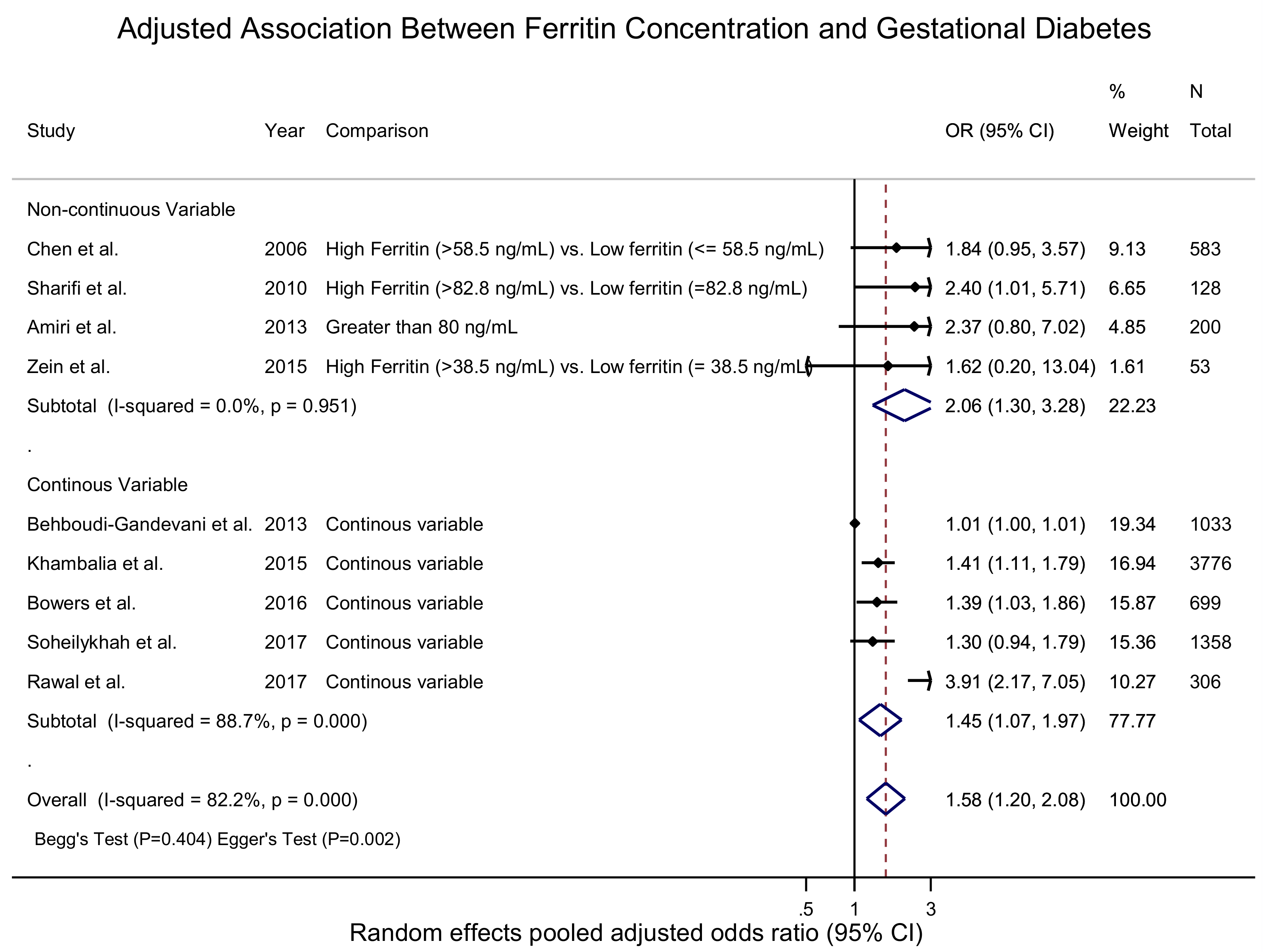
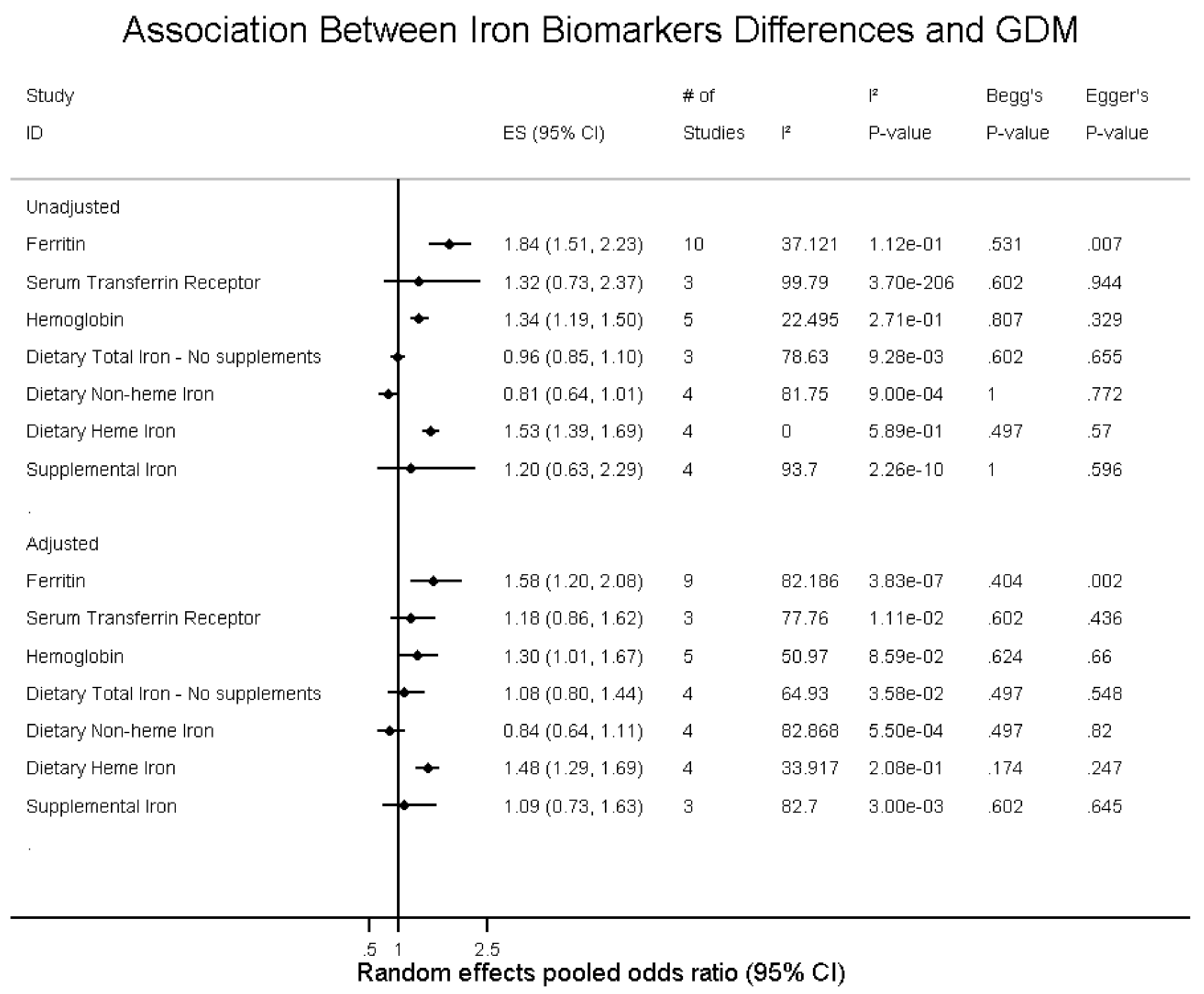
3.2. Serum Ferritin
3.3. Total Iron Binding Capacity
3.4. Transferrin Saturation and Transferrin Receptor
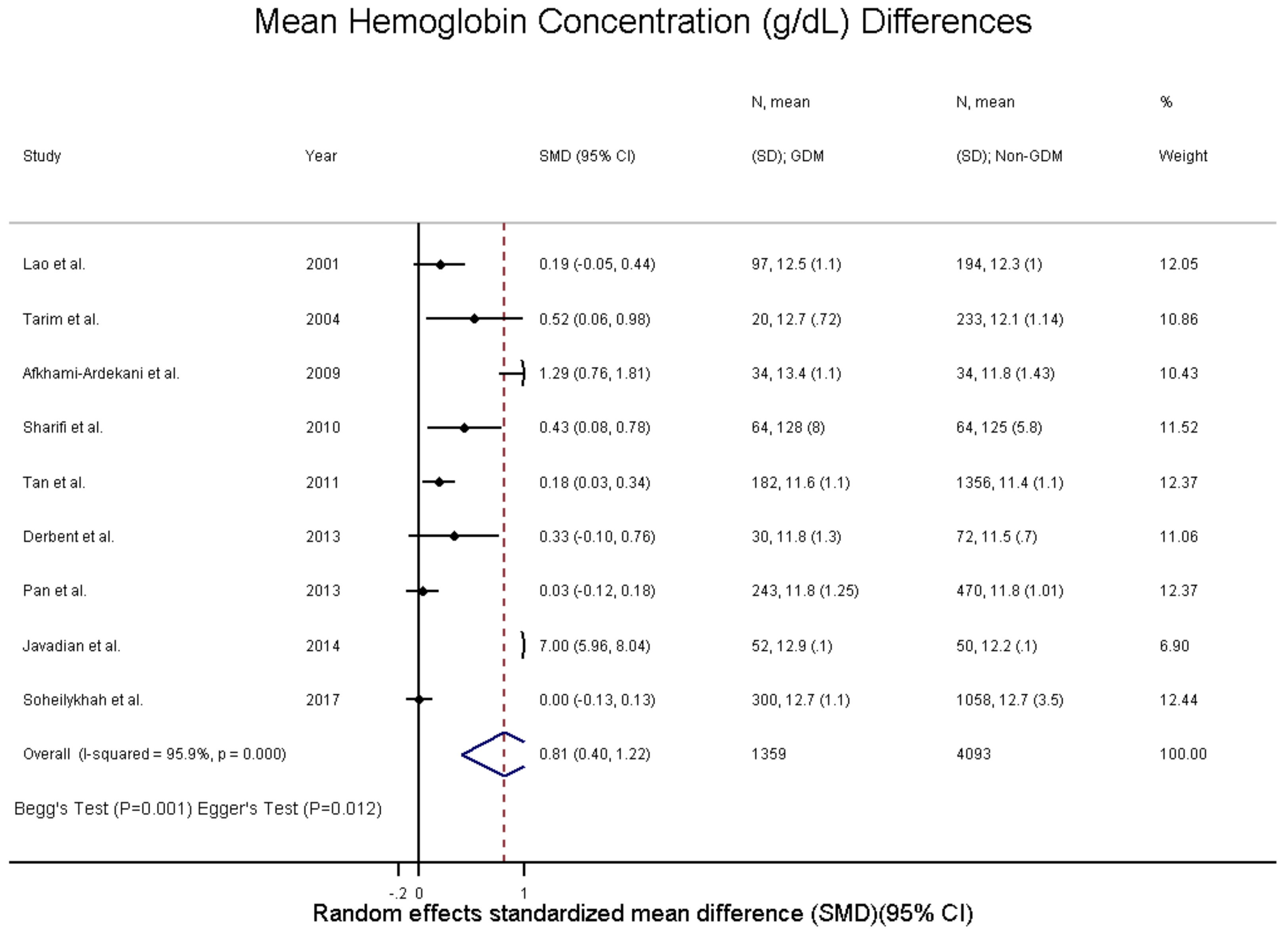
3.5. Hemoglobin
3.6. Dietary Iron Biomarkers
3.7. Heterogeneity and Publication Bias and Sensitivity Analysis
4. Discussion
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Benoist, B.D.; McLean, E.; Egll, I.; Cogswell, M. Worldwide prevalence of anaemia 1993–2005: Who global database on anaemia. In Worldwide Prevalence of Anaemia 1993–2005: WHO Global Database on Anaemia; WHO: Geneva, Switzerland, 2008. [Google Scholar]
- Hansen, J.B.; Moen, I.W.; Mandrup-Poulsen, T. Iron: The hard player in diabetes pathophysiology. Acta Physiol. 2014, 210, 717–732. [Google Scholar] [CrossRef] [PubMed]
- O’Sullivan, J.B.; Mahan, C.M. Criteria for the oral glucose tolerance test in pregnancy. Diabetes 1964, 13, 278. [Google Scholar] [PubMed]
- World Health Organization. Diagnostic Criteria and Classification of Hyperglycaemia First Detected in Pregnancy; WHO: Geneva, Switzerland, 2013. [Google Scholar]
- Chiefari, E.; Arcidiacono, B.; Foti, D.; Brunetti, A. Gestational diabetes mellitus: An updated overview. J. Endocrinol. Investig. 2017, 40, 899–909. [Google Scholar] [CrossRef] [PubMed]
- Setji, T.L.; Brown, A.J.; Feinglos, M.N. Gestational diabetes mellitus. Clin. Diabetes 2005, 23, 17–24. [Google Scholar] [CrossRef]
- Mari-Sanchis, A.; Diaz-Jurado, G.; Basterra-Gortari, F.J.; de la Fuente-Arrillaga, C.; Martinez-Gonzalez, M.A.; Bes-Rastrollo, M. Association between pre-pregnancy consumption of meat, iron intake, and the risk of gestational diabetes: The sun project. Eur. J. Nutr. 2018, 57, 939–949. [Google Scholar] [CrossRef] [PubMed]
- Behboudi-Gandevani, S.; Safary, K.; Moghaddam-Banaem, L.; Lamyian, M.; Goshtasebi, A.; Alian-Moghaddam, N. The relationship between maternal serum iron and zinc levels and their nutritional intakes in early pregnancy with gestational diabetes. Biol. Trace Elem. Res. 2013, 154, 7–13. [Google Scholar] [CrossRef] [PubMed]
- Bowers, K.; Yeung, E.; Williams, M.A.; Qi, L.; Tobias, D.K.; Hu, F.B.; Zhang, C. A prospective study of prepregnancy dietary iron intake and risk for gestational diabetes mellitus. Diabetes Care 2011, 34, 1557–1563. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Scholl, T.O.; Stein, T.P. Association of elevated serum ferritin levels and the risk of gestational diabetes mellitus in pregnant women: The camden study. Diabetes Care 2006, 29, 1077–1082. [Google Scholar] [CrossRef] [PubMed]
- Darling, A.M.; Mitchell, A.A.; Werler, M.M. Preconceptional iron intake and gestational diabetes mellitus. Int. J. Environ. Res. Public Health 2016, 13, 525. [Google Scholar] [CrossRef] [PubMed]
- Helin, A.; Kinnunen, T.I.; Raitanen, J.; Ahonen, S.; Virtanen, S.M.; Luoto, R. Iron intake, haemoglobin and risk of gestational diabetes: A prospective cohort study. BMJ Open 2012, 2, e001730. [Google Scholar] [CrossRef] [PubMed]
- Khambalia, A.Z.; Aimone, A.; Nagubandi, P.; Roberts, C.L.; McElduff, A.; Morris, J.M.; Powell, K.L.; Tasevski, V.; Nassar, N. High maternal iron status, dietary iron intake and iron supplement use in pregnancy and risk of gestational diabetes mellitus: A prospective study and systematic review. Diabet. Med. 2016, 33, 1211–1221. [Google Scholar] [CrossRef] [PubMed]
- Qiu, C.; Zhang, C.; Gelaye, B.; Enquobahrie, D.A.; Frederick, I.O.; Williams, M.A. Gestational diabetes mellitus in relation to maternal dietary heme iron and nonheme iron intake. Diabetes Care 2011, 34, 1564–1569. [Google Scholar] [CrossRef] [PubMed]
- Rawal, S.; Hinkle, S.N.; Bao, W.; Zhu, Y.; Grewal, J.; Albert, P.S.; Weir, N.L.; Tsai, M.Y.; Zhang, C. A longitudinal study of iron status during pregnancy and the risk of gestational diabetes: Findings from a prospective, multiracial cohort. Diabetologia 2017, 60, 249–257. [Google Scholar] [CrossRef] [PubMed]
- Soheilykhah, S.; Mojibian, M.; Jannati Moghadam, M. Serum ferritin concentration in early pregnancy and risk of subsequent development of gestational diabetes: A prospective study. Int. J. Reprod. Biomed. 2017, 15, 155–160. [Google Scholar] [CrossRef]
- Soubasi, V.; Petridou, S.; Sarafidis, K.; Tsantali, C.; Diamanti, E.; Buonocore, G.; Drossou-Agakidou, V. Association of increased maternal ferritin levels with gestational diabetes and intra-uterine growth retardation. Diabetes Metab. 2010, 36, 58–63. [Google Scholar] [CrossRef] [PubMed]
- Tarim, E.; Kilicdag, E.; Bagis, T.; Ergin, T. High maternal hemoglobin and ferritin values as risk factors for gestational diabetes. Int. J. Gynecol. Obstet. 2004, 84, 259–261. [Google Scholar] [CrossRef]
- Chan, K.K.; Chan, B.C.; Lam, K.F.; Tam, S.; Lao, T.T. Iron supplement in pregnancy and development of gestational diabetes—A randomised placebo-controlled trial. BJOG 2009, 116, 789–798. [Google Scholar] [CrossRef] [PubMed]
- Afkhami-Ardekani, M.; Rashidi, M. Iron status in women with and without gestational diabetes mellitus. J. Diabetes Complic. 2009, 23, 194–198. [Google Scholar] [CrossRef] [PubMed]
- Al-Saleh, E.; Nandakumaran, M.; Al-Rashdan, I.; Al-Harmi, J.; Al-Shammari, M. Maternal-foetal status of copper, iron, molybdenum, selenium and zinc in obese gestational diabetic pregnancies. Acta Diabetol. 2007, 44, 106–113. [Google Scholar] [CrossRef] [PubMed]
- Al-Saleh, E.; Nandakumaran, M.; Al-Shammari, M.; Al-Harouny, A. Maternal-fetal status of copper, iron, molybdenum, selenium and zinc in patients with gestational diabetes. J. Matern. Fetal Neonatal Med. 2004, 16, 15–21. [Google Scholar] [CrossRef] [PubMed]
- Amiri, F.N.; Basirat, Z.; Omidvar, S.; Sharbatdaran, M.; Tilaki, K.H.; Pouramir, M. Comparison of the serum iron, ferritin levels and total iron-binding capacity between pregnant women with and without gestational diabetes. J. Nat. Sci. Biol. Med. 2013, 4, 302–305. [Google Scholar] [PubMed]
- Derbent, A.U.; Simavli, S.A.; Kaygusuz, I.; Gumus, I.I.; Yilmaz, S.; Yildirim, M.; Uysal, S. Serum hepcidin is associated with parameters of glucose metabolism in women with gestational diabetes mellitus. J. Matern. Fetal Neonatal Med. 2013, 26, 1112–1115. [Google Scholar] [CrossRef] [PubMed]
- Kaygusuz, I.; Gumus, I.I.; Yilmaz, S.; Simavli, S.; Uysal, S.; Derbent, A.U.; Gozdemir, E.; Kafali, H. Serum levels of visfatin and possible interaction with iron parameters in gestational diabetes mellitus. Gynecol. Obstet. Investig. 2013, 75, 203–209. [Google Scholar] [CrossRef] [PubMed]
- Javadian, P.; Alimohamadi, S.; Gharedaghi, M.H.; Hantoushzadeh, S. Gestational diabetes mellitus and iron supplement; effects on pregnancy outcome. Acta Med. Iran. 2014, 52, 385–389. [Google Scholar] [PubMed]
- Ozyer, S.; Engin-Ustun, Y.; Uzunlar, O.; Katar, C.; Danisman, N. Inflammation and glycemic tolerance status in pregnancy: The role of maternal adiposity. Gynecol. Obstet. Investig. 2014, 78, 53–58. [Google Scholar] [CrossRef] [PubMed]
- Sharifi, F.; Ziaee, A.; Feizi, A.; Mousavinasab, N.; Anjomshoaa, A.; Mokhtari, P. Serum ferritin concentration in gestational diabetes mellitus and risk of subsequent development of early postpartum diabetes mellitus. Diabetes Metab. Syndr. Obes. 2010, 3, 413–419. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Tan, M.; Huang, Z.; Sheng, L.; Ge, Y.; Zhang, H.; Jiang, M.; Zhang, G. Elemental contents in serum of pregnant women with gestational diabetes mellitus. Biol. Trace Elem. Res. 2002, 88, 113–118. [Google Scholar] [CrossRef]
- Akhlaghi, F.; Bagheri, S.M.; Rajabi, O. A comparative study of relationship between micronutrients and gestational diabetes. ISRN Obstet. Gynecol. 2012, 2012, 470419. [Google Scholar] [CrossRef] [PubMed]
- Pan, J.; Zhang, F.; Zhang, L.; Bao, Y.; Tao, M.; Jia, W. Influence of insulin sensitivity and secretion on glycated albumin and hemoglobin a1c in pregnant women with gestational diabetes mellitus. Int. J. Gynaecol. Obstet. 2013, 121, 252–256. [Google Scholar] [CrossRef] [PubMed]
- Lao, T.T.; Chan, L.Y.; Tam, K.F.; Ho, L.F. Maternal hemoglobin and risk of gestational diabetes mellitus in Chinese women. Obstet. Gynecol. 2002, 99, 807–812. [Google Scholar] [PubMed]
- Lao, T.T.; Chan, P.L.; Tam, K.F. Gestational diabetes mellitus in the last trimester—A feature of maternal iron excess? Diabet. Med. 2001, 18, 218–223. [Google Scholar] [CrossRef] [PubMed]
- Bo, S.; Menato, G.; Villois, P.; Gambino, R.; Cassader, M.; Cotrino, I.; Cavallo-Perin, P. Iron supplementation and gestational diabetes in midpregnancy. Am. J. Obstet. Gynecol. 2009, 201, 158.e1–158.e6. [Google Scholar] [CrossRef] [PubMed]
- Palma, S.; Perez-Iglesias, R.; Prieto, D.; Pardo, R.; Llorca, J.; Delgado-Rodriguez, M. Iron but not folic acid supplementation reduces the risk of low birthweight in pregnant women without anaemia: A case-control study. J. Epidemiol. Community Health 2008, 62, 120–124. [Google Scholar] [CrossRef] [PubMed]
- Gungor, E.S.; Danisman, N.; Mollamahmutoglu, L. Maternal serum ferritin and hemoglobin values in patients with gestational diabetes mellitus. Saudi Med. J. 2007, 28, 478–480. [Google Scholar] [PubMed]
- Tan, P.; Chai, J.; Ling, L.; Omar, S. Maternal hemoglobin level and red cell indices as predictors of gestational diabetes in a multi-ethnic Asian population. Clin. Exp. Obstet. Gynecol. 2011, 38, 150–154. [Google Scholar] [PubMed]
- Bowers, K.A.; Olsen, S.F.; Bao, W.; Halldorsson, T.I.; Strom, M.; Zhang, C. Plasma concentrations of ferritin in early pregnancy are associated with risk of gestational diabetes mellitus in women in the Danish national birth cohort. J. Nutr. 2016, 146, 1756–1761. [Google Scholar] [CrossRef] [PubMed]
- Kinnunen, T.I.; Luoto, R.; Helin, A.; Hemminki, E. Supplemental iron intake and the risk of glucose intolerance in pregnancy: Re-analysis of a randomised controlled trial in Finland. Matern. Child Nutr. 2016, 12, 74–84. [Google Scholar] [CrossRef] [PubMed]
- Stang, A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur. J. Epidemiol. 2010, 25, 603–605. [Google Scholar] [CrossRef] [PubMed]
- Fernandez-Cao, J.C.; Aranda, N.; Ribot, B.; Tous, M.; Arija, V. Elevated iron status and risk of gestational diabetes mellitus: A systematic review and meta-analysis. Matern. Child Nutr. 2017, 13. [Google Scholar] [CrossRef] [PubMed]
- Fu, S.; Li, F.; Zhou, J.; Liu, Z. The relationship between body iron status, iron intake and gestational diabetes: A systematic review and meta-analysis. Medicine 2016, 95, e2383. [Google Scholar] [CrossRef] [PubMed]
- Han, S.; Middleton, P.; Shepherd, E.; Van Ryswyk, E.; Crowther, C.A. Different types of dietary advice for women with gestational diabetes mellitus. Cochrane Database Syst. Rev. 2017, 2, CD009275. [Google Scholar] [CrossRef] [PubMed]
- Zhao, L.; Lian, J.; Tian, J.; Shen, Y.; Ping, Z.; Fang, X.; Min, J.; Wang, F. Dietary intake of heme iron and body iron status are associated with the risk of gestational diabetes mellitus: A systematic review and meta-analysis. Asia Pac. J. Clin. Nutr. 2017, 26, 1092–1106. [Google Scholar] [PubMed]
- Zhang, C.; Rawal, S. Dietary iron intake, iron status, and gestational diabetes. Am. J. Clin. Nutr. 2017, 106, 1672S–1680S. [Google Scholar] [CrossRef] [PubMed]
- Ganz, T. Hepcidin and iron regulation, 10 years later. Blood 2011, 117, 4425–4433. [Google Scholar] [CrossRef] [PubMed]
- Nemeth, E.; Rivera, S.; Gabayan, V.; Keller, C.; Taudorf, S.; Pedersen, B.K.; Ganz, T. Il-6 mediates hypoferremia of inflammation by inducing the synthesis of the iron regulatory hormone hepcidin. J. Clin. Investig. 2004, 113, 1271–1276. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Lu, X. Study on correlation between c-reactive protein and gestational diabetes mellitus. J. Nanjing Med. Univ. 2007, 21, 382–385. [Google Scholar] [CrossRef]
- Zein, S.; Rachidi, S.; Awada, S.; Osman, M.; Al-Hajje, A.; Shami, N.; Sharara, I.; Cheikh-Ali, K.; Salameh, P.; Hininger-Favier, I. High iron level in early pregnancy increased glucose intolerance. J. Trace Elem. Med. Biol. 2015, 30, 220–225. [Google Scholar] [CrossRef] [PubMed]
- Khambalia, A.Z.; Collins, C.E.; Roberts, C.L.; Morris, J.M.; Powell, K.L.; Tasevski, V.; Nassar, N. Iron deficiency in early pregnancy using serum ferritin and soluble transferrin receptor concentrations are associated with pregnancy and birth outcomes. Eur. J. Clin. Nutr. 2016, 70, 358–363. [Google Scholar] [CrossRef] [PubMed]
- Jiang, R.; Manson, J.E.; Meigs, J.B.; Ma, J.; Rifai, N.; Hu, F.B. Body iron stores in relation to risk of type 2 diabetes in apparently healthy women. JAMA 2004, 291, 711–717. [Google Scholar] [CrossRef] [PubMed]
- Dongiovanni, P.; Valenti, L.; Ludovica Fracanzani, A.; Gatti, S.; Cairo, G.; Fargion, S. Iron depletion by deferoxamine up-regulates glucose uptake and insulin signaling in hepatoma cells and in rat liver. Am. J. Pathol. 2008, 172, 738–747. [Google Scholar] [CrossRef] [PubMed]
- Bothwell, T.H. Overview and mechanisms of iron regulation. Nutr. Rev. 1995, 53, 237–245. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Storlien, L.H.; Jenkins, A.B.; Tapsell, L.C.; Jin, Y.; Pan, J.F.; Shao, Y.F.; Calvert, G.D.; Moses, R.G.; Shi, H.L.; et al. Dietary variables and glucose tolerance in pregnancy. Diabetes Care 2000, 23, 460–464. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Liu, S.; Solomon, C.G.; Hu, F.B. Dietary fiber intake, dietary glycemic load, and the risk for gestational diabetes mellitus. Diabetes Care 2006, 29, 2223–2230. [Google Scholar] [CrossRef] [PubMed]
- Sivitskaya, L.; Danilenko, N.; Zabarouskaya, Z.; Davydenko, O. Hfe gene mutation associated with the severity of gestational diabetes mellitus in Belarusian women. Age 2013, 28, 5–7. [Google Scholar] [CrossRef]
- Bonfils, L.; Ellervik, C.; Friedrich, N.; Linneberg, A.; Sandholt, C.H.; Jørgensen, M.E.; Jørgensen, T.; Hansen, T.; Pedersen, O.; Allin, K.H. Fasting serum levels of ferritin are associated with impaired pancreatic beta cell function and decreased insulin sensitivity: A population-based study. Diabetologia 2015, 58, 523–533. [Google Scholar] [CrossRef] [PubMed]
- Ellervik, C.; Mandrup-Poulsen, T.; Andersen, H.U.; Tybjærg-Hansen, A.; Frandsen, M.; Birgens, H.; Nordestgaard, B.G. Elevated transferrin saturation and risk of diabetes: Three population-based studies. Diabetes Care 2011, 34, 2256–2258. [Google Scholar] [CrossRef] [PubMed]
- Backe, M.B.; Moen, I.W.; Ellervik, C.; Hansen, J.B.; Mandrup-Poulsen, T. Iron regulation of pancreatic beta-cell functions and oxidative stress. Ann. Rev. Nutr. 2016, 36, 241–273. [Google Scholar] [CrossRef] [PubMed]
- Cejvanovic, V.; Kjær, L.K.; Bergholdt, H.K.M.; Torp-Pedersen, A.; Henriksen, T.; Weimann, A.; Ellervik, C.; Poulsen, H.E. Iron induced rna-oxidation in the general population and in mouse tissue. Free Radic. Biol. Med. 2018, 115, 127–135. [Google Scholar] [CrossRef] [PubMed]
- Leong, W.-I.; Lönnerdal, B. Iron nutrition. In Iron Physiology and Pathophysiology in Humans; Springer: New York, NY, USA, 2012; pp. 81–99. [Google Scholar]

| Author | Year | Country | Design | N Cases | N Total | Ascertainment of GDM | Age a | Dietary Heme Iron | Dietary Non-Heme Iron | Dietary Total Iron | Dietary Supplemental Iron | Serum Iron | Serum Ferritin | Serum Transferrin Receptor | Hemoglobin | CRP | Serum TIBC | Serum Transferrin Saturation | Serum Ferritin Assay |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Marí-Sanchis et al. | 2017 | Spain | Cohort | 172 | 3298 | Self Report | 28.7 | X | X | X | |||||||||
| Behboudi-Gandevani et al. | 2013 | Iran | Cohort | 72 | 1033 | OGTT | 27.6 | X | X | X | X | NR | |||||||
| Bowers et al. | 2011 | US | Cohort | 867 | 13,475 | Self Report | 31.4 | X | X | X | X | ||||||||
| Chen et al. | 2006 | US | Cohort | 45 | 1456 | OGTT | 22.1 | X | X | X | Immunoradiometric | ||||||||
| Darling et al. | 2016 | US | Cohort | 316 | 7229 | Self Report | NR | X | X | ||||||||||
| Helin et al. | 2012 | Finland | Cohort | 72 | 399 | Medical Record/OGTT | 29.3 | X | |||||||||||
| Khambalia et al. | 2015 | Australia | Cohort | 129 | 3776 | Medical Record | NR | X | X | X | ELISA | ||||||||
| Qiu et al. | 2011 | US | Cohort | 158 | 3158 | Medical Record | 32.7 | X | X | ||||||||||
| Rawal et al. | 2017 | US | Case-Control | 107 | 321 | Medical Record | 30.4 | X | X | X | Immunoturbidimetric | ||||||||
| Soheilykhah et al. | 2017 | Iran | Cohort | 300 | 1358 | OGTT | 20.3–31.4 | X | X | X | X | ELISA | |||||||
| Soubasi et al. | 2010 | Greece | Cohort | 6 | 63 | Medical Record | 24–37 | X | ELISA | ||||||||||
| Tarim et al. | 2004 | Turkey | Cohort | 20 | 253 | OGTT | 21.8–32.3 | X | X | NR | |||||||||
| Zein et al. | 2015 | Lebanon | Cohort | 16 | 104 | OGTT | 20–33 | X | X | X | Chemiluminescence | ||||||||
| Chan et al. | 2009 | China | Randomized Control Trial | 116 | 1164 | OGTT | 31.1–31.5 | X | |||||||||||
| Afkhami-Ardekani et al. | 2009 | Iran | Case-Control | 34 | 68 | OGTT | NR | X | X | X | X | X | Immunoradiometric | ||||||
| Al Saleh et al. | 2004 | Kuwait | Case-Control | 15 | 30 | Not Reported | 23.1 | X | |||||||||||
| Al Saleh et al. | 2007 | Kuwait | Case-Control | 10 | 21 | Not Reported | 28.0–33.7 | X | |||||||||||
| Amiri et al. | 2013 | Iran | Case-Control | 100 | 200 | OGTT | 19.6–31.0 | X | X | X | Immunoradiometric | ||||||||
| Derbent et al. | 2013 | Turkey | Case-Control | 30 | 102 | OGTT | 23.9–37 | X | X | X | Electrochemiluminescence | ||||||||
| Gungor et al. | 2007 | Turkey | Case-Control | 56 | 112 | OGTT | 21.1–33.9 | X | MEIA | ||||||||||
| Javadian et al. | 2014 | Iran | Case-Control | 52 | 102 | OGTT | 22.3–37.8 | X | X | Immunoradiometric | |||||||||
| Kaygusuz et al. | 2013 | Turkey | Case-Control | 30 | 58 | OGTT | 28.7–32.8 | X | X | X | |||||||||
| Ozyer et al. | 2014 | Turkey | Case-Control | 35 | 105 | OGTT | 26.8–34.1 | X | |||||||||||
| Sharifi et al. | 2010 | Iran | Case-Control | 64 | 128 | OGTT | 25.1–34.9 | X | X | Immunoradiometric | |||||||||
| Wang et al. | 2002 | China | Cross-sectional | 46 | 136 | OGTT | NR | X | |||||||||||
| Akhlaghi et al. | 2012 | Iran | Case-Control | 30 | 60 | OGTT | 25–30 | X | |||||||||||
| Pan et al. | 2013 | China | Cross-sectional | 243 | 713 | OGTT | 29.5 | X | |||||||||||
| Lao et al. | 2001 | China | Cross-sectional | 97 | 291 | OGTT | 34.9–37.4 | X | X | X | X | MEIA | |||||||
| Lao et al. | 2002 | China | Cross-sectional | 94 | 730 | OGTT | 29.7 | X | |||||||||||
| Tan et al. | 2011 | Malaysia | Cohort | 182 | 1538 | OGTT | 24.6–36.9 | X | |||||||||||
| Bowers et al. | 2016 | Denmark | Case-Control | 350 | 699 | OGTT | 25.7–36.5 | X | X | Immunoturbidimetric | |||||||||
| Bo et al. | 2009 | Italy | Case-Control | 500 | 1000 | OGTT | 28.3–41 | X | |||||||||||
| Palma et al. | 2008 | Spain | Case-Control | 41 | 930 | Medical Record | 20–25 | X |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kataria, Y.; Wu, Y.; Horskjær, P.D.H.; Mandrup-Poulsen, T.; Ellervik, C. Iron Status and Gestational Diabetes—A Meta-Analysis. Nutrients 2018, 10, 621. https://doi.org/10.3390/nu10050621
Kataria Y, Wu Y, Horskjær PDH, Mandrup-Poulsen T, Ellervik C. Iron Status and Gestational Diabetes—A Meta-Analysis. Nutrients. 2018; 10(5):621. https://doi.org/10.3390/nu10050621
Chicago/Turabian StyleKataria, Yachana, Yanxin Wu, Peter De Hemmer Horskjær, Thomas Mandrup-Poulsen, and Christina Ellervik. 2018. "Iron Status and Gestational Diabetes—A Meta-Analysis" Nutrients 10, no. 5: 621. https://doi.org/10.3390/nu10050621
APA StyleKataria, Y., Wu, Y., Horskjær, P. D. H., Mandrup-Poulsen, T., & Ellervik, C. (2018). Iron Status and Gestational Diabetes—A Meta-Analysis. Nutrients, 10(5), 621. https://doi.org/10.3390/nu10050621





