The Mediating Role of Overweight and Obesity in the Prospective Association between Overall Dietary Quality and Healthy Aging
Abstract
1. Introduction
2. Materials and Methods
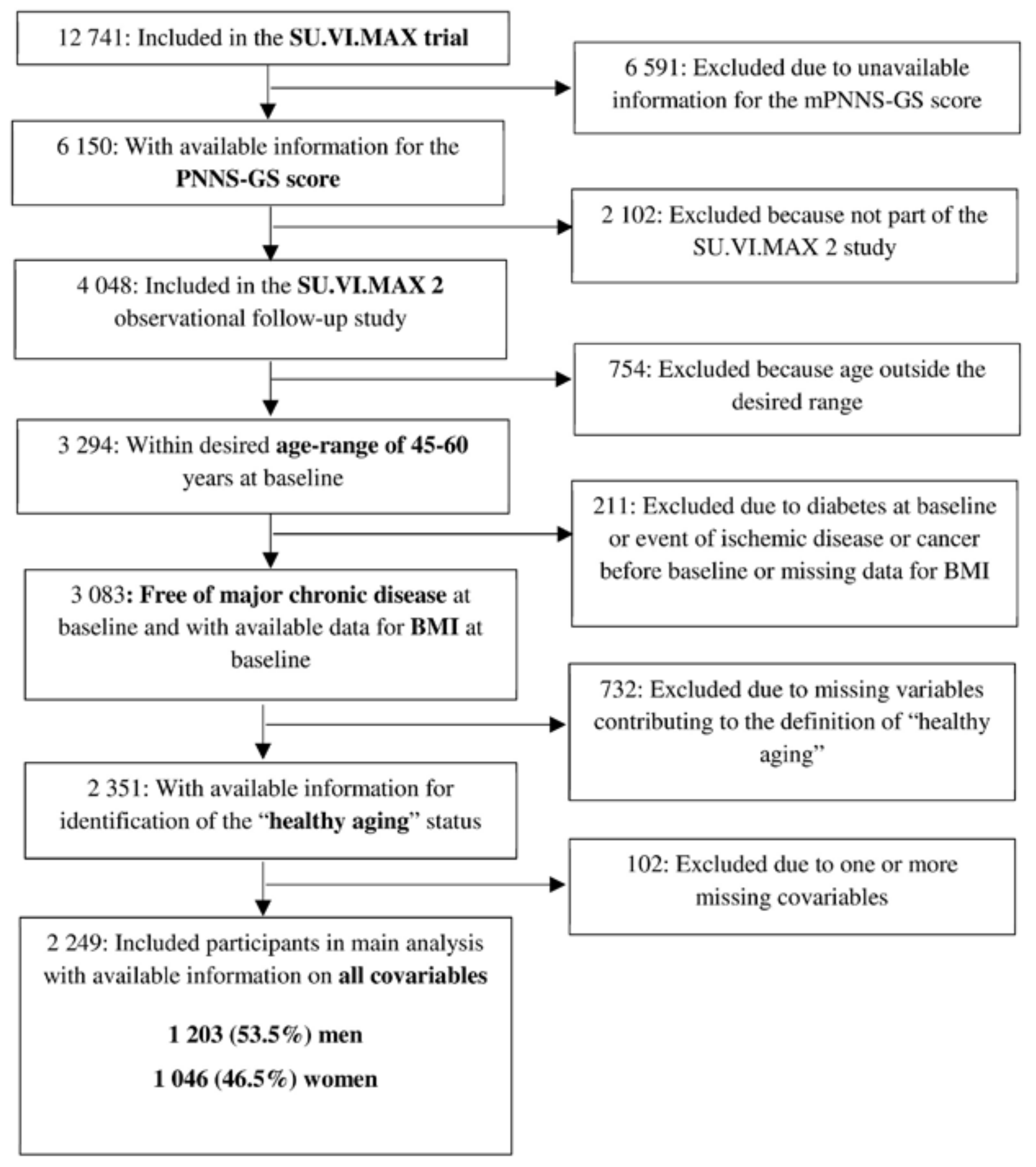
2.1. Study Population
2.2. Data Collection
2.2.1. Timeline of Data Collection
2.2.2. Healthy Aging (HA) Status (2007–2009)
2.2.3. Baseline Dietary Data (1994–1996)
2.2.4. Anthropometric Data (1995–1996)
2.2.5. Baseline Covariates (1994–1996)
2.3. Statistical Analysis
2.3.1. Descriptive Statistics and Results on the Simple Association between Dietary Quality and HA
2.3.2. Main Analysis: Mediating Role of BMI Status in the Association between Diet Quality and HA
3. Results
3.1. Descriptive Statistics
3.2. Relationship between Dietary Quality and Overall Healthy Aging (HA)
3.3. The Mediating Role of Body Mass Index (BMI) Status
4. Discussion
Acknowledgments
Author Contributions
Conflicts of Interest
References
- United Nations, Department of Economic and Social Affairs, Population Division. World Population Ageing; United Nations: New York, NY, USA, 2009. [Google Scholar]
- Heller, T.; Fisher, D.; Marks, B.; Hsieh, K. Interventions to promote health: Crossing networks of intellectual and developmental disabilities and aging. Disabil. Health J. 2014, 7, S24–S32. [Google Scholar] [CrossRef] [PubMed]
- Martinson, M.; Berridge, C. Successful aging and its discontents: A Systematic Review of the Social Gerontology Literature. Gerontologist 2015, 55, 58–69. [Google Scholar] [CrossRef] [PubMed]
- Rowe, J.W.; Kahn, R.L. Successful aging. Gerontologist 1997, 37, 433–440. [Google Scholar] [CrossRef] [PubMed]
- Rowe, J.W.; Kahn, R.L. Successful Aging 2.0: Conceptual Expansions for the 21st Century. J. Gerontol. B Psychol. Sci. Soc. Sci. 2015, 70, 593–596. [Google Scholar] [CrossRef] [PubMed]
- Franzon, K.; Zethelius, B.; Cederholm, T.; Kilander, L. Modifiable midlife risk factors, independent aging, and survival in older men: Report on long-term follow-up of the Uppsala Longitudinal Study of Adult Men cohort. J. Am. Geriatr. Soc. 2015, 63, 877–885. [Google Scholar] [CrossRef] [PubMed]
- Reed, D.M.; Foley, D.J.; White, L.R.; Heimovitz, H.; Burchfiel, C.M.; Masaki, K. Predictors of health aging in men with high life expectancies. Am. J. Public Health 1998, 88, 1463–1468. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Willcox, B.J.; He, Q.; Chen, R.; Yano, K.; Masaki, K.H.; Grove, J.S.; Donlon, T.A.; Willcox, D.C.; Curb, J.D. Midlife risk factors and healthy survival in men. JAMA 2006, 296, 2343–2350. [Google Scholar] [CrossRef] [PubMed]
- Singh-Manoux, A.; Czernichow, S.; Elbaz, A.; Dugravot, A.; Sabia, S.; Hagger-Johnson, G.; Kaffashian, S.; Zins, M.; Brunner, E.J.; Nabi, H.; et al. Obesity phenotpes in midlife and cognition in early old age: The Whitehall II cohort study. Neurology 2012, 79, 755–762. [Google Scholar] [CrossRef] [PubMed]
- Daskalopoulou, C.; Stubbs, B.; Kralj, C.; Koukounari, A.; Prince, M.; Prina, A.M. Physical activity and healthy ageing: A systematic review and meta-analysis of longitudinal cohort studies. Ageing Res. Rev. 2017, 38, 6–17. [Google Scholar] [CrossRef] [PubMed]
- Sabia, S.; Singh-Manoux, A.; Hagger-Johnson, G.; Cambois, E.; Brunner, E.J.; Kivimaki, M. Influence of individual and combined healthy behaviours on successful aging. Can. Med. Assoc. J. 2012, 184, 1985–1992. [Google Scholar] [CrossRef] [PubMed]
- Cohen, G.; Gerber, Y. Air pollution and successful aging: Recent evidence and new perspectives. Curr. Environ. Health Rep. 2017, 4, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Kiefte-de Jong, J.C.; Mathers, J.C.; Franco, O.H. Nutrition and healthy ageing: The key ingredients. Proc. Nutr. Soc. 2014, 73, 249–259. [Google Scholar] [CrossRef] [PubMed]
- Akbaraly, T.; Sabia, S.; Hagger-Johnson, G.; Tabak, A.G.; Shipley, M.J.; Jokela, M.; Brunner, E.J.; Hamer, M.; Batty, G.D.; Singh-Manoux, A.; et al. Does overall diet in midlife predict future aging phenotypes? A cohort study. Am. J. Med. 2013, 126, 411–419. [Google Scholar] [CrossRef] [PubMed]
- Assmann, K.E.; Andreeva, V.A.; Camilleri, G.M.; Verger, E.O.; Jeandel, C.; Hercberg, S.; Galan, P.; Kesse-Guyot, E. Dietary scores at midlife and healthy ageing in a French prospective cohort. Br. J. Nutr. 2016, 116, 666–676. [Google Scholar] [CrossRef] [PubMed]
- Assmann, K.E.; Lassale, C.; Andreeva, V.A.; Jeandel, C.; Hercberg, S.; Galan, P.; Kesse-Guyot, E. A healthy dietary pattern at midlife, combined with a regulated energy intake, is related to increased odds for healthy aging. J. Nutr. 2015, 145, 2139–2145. [Google Scholar] [CrossRef] [PubMed]
- Gopinath, B.; Russell, J.; Kifley, A.; Flood, V.M.; Mitchell, P. Adherence to dietary guidelines and successful aging over 10 years. J. Gerontol. A Biol. Sci. Med. Sci. 2016, 71, 349–355. [Google Scholar] [CrossRef] [PubMed]
- Hodge, A.M.; O’Dea, K.; English, D.R.; Giles, G.G.; Flicker, L. Dietary patterns as predictors of successful ageing. J. Nutr. Health Aging 2014, 18, 221–227. [Google Scholar] [CrossRef] [PubMed]
- Samieri, C.; Sun, Q.; Townsend, M.K.; Chiuve, S.E.; Okereke, O.I.; Willett, W.C.; Stampfer, M.; Grodstein, F. The association between dietary patterns at midlife and health in aging: An observational study. Ann. Intern. Med. 2013, 159, 584–591. [Google Scholar] [CrossRef] [PubMed]
- Assmann, K.E.; Adjibade, M.; Andreeva, V.A.; Hercberg, S.; Galan, P.; Kesse-Guyot, E. Association between adherence to the mediterranean diet at midlife and healthy aging in a cohort of french adults. J. Gerontol. A Biol. Sci. Med. Sci. 2018, 73, 347–354. [Google Scholar] [CrossRef] [PubMed]
- Bell, C.L.; Chen, R.; Masaki, K.; Yee, P.; He, Q.; Grove, J.; Donlon, T.; Curb, J.D.; Willcox, D.C.; Poon, L.W.; et al. Late-life factors associated with healthy aging in older men. J. Am. Geriatr. Soc. 2014, 62, 880–888. [Google Scholar] [CrossRef] [PubMed]
- Singh-Manoux, A.; Sabia, S.; Bouillon, K.; Brunner, E.J.; Grodstein, F.; Elbaz, A.; Kivimaki, M. Association of body mass index and waist circumference with successful aging. Obes. Silver Spring 2014, 22, 1172–1178. [Google Scholar] [CrossRef] [PubMed]
- Tyrovolas, S.; Haro, J.-M.; Mariolis, A.; Piscopo, S.; Valacchi, G.; Bountziouka, V.; Anastasiou, F.; Zeimbekis, A.; Tyrovola, D.; Foscolou, A.; et al. Skeletal muscle mass and body fat in relation to successful ageing of older adults: The multi-national MEDIS study. Arch. Gerontol. Geriatr. 2016, 66, 95–101. [Google Scholar] [CrossRef] [PubMed]
- Yates, L.B.; Djoussé, L.; Kurth, T.; Buring, J.E.; Gaziano, J.M. Exceptional longevity in men: Modifiable factors associated with survival and function to age 90 years. Arch. Intern. Med. 2008, 168, 284–290. [Google Scholar] [CrossRef] [PubMed]
- Frasca, D.; Blomberg, B.B.; Paganelli, R. Aging, obesity, and inflammatory age-related diseases. Front. Immunol. 2017, 8. [Google Scholar] [CrossRef] [PubMed]
- Kohlgruber, A.; Lynch, L. Adipose tissue inflammation in the pathogenesis of type 2 diabetes. Curr. Diabetes Rep. 2015, 15, 92. [Google Scholar] [CrossRef] [PubMed]
- Berg, A.H.; Scherer, P.E. Adipose tissue, inflammation, and cardiovascular disease. Circ. Res. 2005, 96, 939–949. [Google Scholar] [CrossRef] [PubMed]
- Shelton, R.C.; Miller, A.H. Inflammation in depression: Is adiposity a cause? Dialogues Clin. Neurosci. 2011, 13, 41–53. [Google Scholar] [PubMed]
- Nguyen, J.C.D.; Killcross, A.S.; Jenkins, T.A. Obesity and cognitive decline: Role of inflammation and vascular changes. Front. Neurosci. 2014, 8. [Google Scholar] [CrossRef] [PubMed]
- Dye, L.; Boyle, N.B.; Champ, C.; Lawton, C. The relationship between obesity and cognitive health and decline. Proc. Nutr. Soc. 2017, 76, 443–454. [Google Scholar] [CrossRef] [PubMed]
- Ruhunuhewa, I.; Adjibade, M.; Andreeva, V.A.; Galan, P.; Hercberg, S.; Assmann, K.E.; Kesse-Guyot, E. Prospective association between body mass index at midlife and healthy aging among French adults. Obes. Silver Spring 2017, 25, 1254–1262. [Google Scholar] [CrossRef] [PubMed]
- Hruby, A.; Manson, J.E.; Qi, L.; Malik, V.S.; Rimm, E.B.; Sun, Q.; Willett, W.C.; Hu, F.B. Determinants and consequences of obesity. Am. J. Public Health. 2016, 106, 1656–1662. [Google Scholar] [CrossRef] [PubMed]
- Hill, J.O.; Wyatt, H.R.; Peters, J.C. Energy Balance and Obesity. Circulation 2012, 126, 126–132. [Google Scholar] [CrossRef] [PubMed]
- Millen, B.E.; Abrams, S.; Adams-Campbell, L.; Anderson, C.A.; Brenna, J.T.; Campbell, W.W.; Clinton, S.; Hu, F.; Nelson, M.; Neuhouser, M.L.; et al. The 2015 dietary guidelines advisory committee scientific report: development and major conclusions. Adv. Nutr. 2016, 7, 438–444. [Google Scholar] [CrossRef] [PubMed]
- Schisterman, E.F.; Cole, S.R.; Platt, R.W. Overadjustment bias and unnecessary adjustment in epidemiologic studies. Epidemiol. Camb. MA 2009, 20, 488–495. [Google Scholar] [CrossRef] [PubMed]
- Hercberg, S.; Galan, P.; Preziosi, P.; Bertrais, S.; Mennen, L.; Malvy, D.; Roussel, A.-M.; Favier, A.; Briançon, S. The SU.VI.MAX Study: A randomized, placebo-controlled trial of the health effects of antioxidant vitamins and minerals. Arch. Intern. Med. 2004, 164, 2335–2342. [Google Scholar] [CrossRef] [PubMed]
- Assmann, K.E.; Andreeva, V.A.; Jeandel, C.; Hercberg, S.; Galan, P.; Kesse-Guyot, E. Healthy aging 5 years after a period of daily supplementation with antioxidant nutrients: A post hoc analysis of the french randomized trial SU.VI.MAX. Am. J. Epidemiol. 2015, 182, 694–704. [Google Scholar] [CrossRef] [PubMed]
- Guralnik, J.M.; Simonsick, E.M.; Ferrucci, L.; Glynn, R.J.; Berkman, L.F.; Blazer, D.G.; Scherr, P.A.; Wallace, R.B. A short physical performance battery assessing lower extremity function: Association with self-reported disability and prediction of mortality and nursing home admission. J. Gerontol. 1994, 49, M85–M94. [Google Scholar] [CrossRef] [PubMed]
- Folstein, M.F.; Robins, L.N.; Helzer, J.E. The Mini-Mental State Examination. Arch. Gen. Psychiatrys 1983, 40, 812. [Google Scholar] [CrossRef]
- Adam, S.; Van der Linden, M.; Ivanoiu, A.; Juillerat, A.-C.; Bechet, S.; Salmon, E. Optimization of encoding specificity for the diagnosis of early AD: The RI-48 task. J. Clin. Exp. Neuropsychol. 2007, 29, 477–487. [Google Scholar] [CrossRef] [PubMed]
- Swanson, J. The Delis-Kaplan Executive Function System A Review. Can. J. Sch. Psychol. 2005, 20, 117–128. [Google Scholar] [CrossRef]
- Homack, S.; Lee, D.; Riccio, C.A. Test review: Delis-Kaplan executive function system. J. Clin. Exp. Neuropsychol. 2005, 27, 599–609. [Google Scholar] [CrossRef] [PubMed]
- Graf, C. Hartford Institute for Geriatric Nursing. The Lawton instrumental activities of daily living (IADL) scale. Medsurg. Nurs. Off. J. Acad. Med. Surg. Nurs. 2008, 17, 343–344. [Google Scholar]
- Morin, A.J.S.; Moullec, G.; Maïano, C.; Layet, L.; Just, J.-L.; Ninot, G. Psychometric properties of the center for epidemiologic studies depression scale (CES-D) in French clinical and nonclinical adults. Rev. Epidemiol. Sante Publique 2011, 59, 327–340. [Google Scholar] [CrossRef] [PubMed]
- Leplège, A.; Ecosse, E.; Verdier, A.; Perneger, T.V. The French SF-36 Health Survey: Translation, cultural adaptation and preliminary psychometric evaluation. J. Clin. Epidemiol. 1998, 51, 1013–1023. [Google Scholar] [CrossRef]
- Moullec, N.L.; Deheeger, M.; Preziosi, P.; Monteiro, P.; Valeix, P.; Rolland-Cachera, M.F.; Courcy, G.P.D.; Christides, J.P.; Cherouvrier, F.; Galan, P.; et al. Validation du manuel-photos utilisé pour l’enquête alimentaire de l’étude SU.VI.MAX. Cah. Nutr. Diététique 1996, 31, 158–164. [Google Scholar]
- Kesse-Guyot, E.; Touvier, M.; Henegar, A.; Czernichow, S.; Galan, P.; Hercberg, S.; Castetbon, K. Higher adherence to French dietary guidelines and chronic diseases in the prospective SU.VI.MAX cohort. Eur. J. Clin. Nutr. 2011, 65, 887–894. [Google Scholar] [CrossRef] [PubMed]
- Lasfargues, G.; Vol, S.; Le Clésiau, H.; Bedouet, M.; Hagel, L.; Constans, T.; Tichet, J. Validity of a short self-administered dietary questionnaire compared with a dietetic interview. Presse Med. Paris Fr. 1990, 19, 953–957. [Google Scholar]
- Estaquio, C.; Kesse-Guyot, E.; Deschamps, V.; Bertrais, S.; Dauchet, L.; Galan, P.; Hercberg, S.; Castetbon, K. Adherence to the French programme national nutrition santé guideline score is associated with better nutrient intake and nutritional status. J. Am. Diet. Assoc. 2009, 109, 1031–1041. [Google Scholar] [CrossRef] [PubMed]
- Zou, G. A modified poisson regression approach to prospective studies with binary data. Am. J. Epidemiol. 2004, 159, 702–706. [Google Scholar] [CrossRef] [PubMed]
- Lange, T.; Vansteelandt, S.; Bekaert, M. A Simple unified approach for estimating natural direct and indirect effects. Am. J. Epidemiol. 2012, 176, 190–195. [Google Scholar] [CrossRef] [PubMed]
- Aron-Wisnewsky, J.; Clément, K. The gut microbiome, diet, and links to cardiometabolic and chronic disorders. Nat. Rev. Nephrol. 2016, 12, 169–181. [Google Scholar] [CrossRef] [PubMed]
- Szarc vel Szic, K.; Declerck, K.; Vidaković, M.; Vanden Berghe, W. From inflammaging to healthy aging by dietary lifestyle choices: Is epigenetics the key to personalized nutrition? Clin. Epigenetics 2015, 7, 33. [Google Scholar] [CrossRef] [PubMed]
- Fardet, A.; Boirie, Y. Associations between diet-related diseases and impaired physiological mechanisms: A holistic approach based on meta-analyses to identifys targets for preventive nutrition. Nutr. Rev. 2013, 71, 643–656. [Google Scholar] [CrossRef] [PubMed]
- Franceschi, C.; Campisi, J. Chronic inflammation (inflammaging) and its potential contribution to age-associated diseases. J. Gerontol. A Biol. Sci. Med. Sci. 2014, 69 (Suppl. S1), S4–S9. [Google Scholar] [CrossRef] [PubMed]
- Harman, D. Free radical theory of aging. Mutat. Res. 1992, 275, 257–266. [Google Scholar] [CrossRef]
- Ritchie, S.A.; Connell, J.M.C. The link between abdominal obesity, metabolic syndrome and cardiovascular disease. Nutr. Metab. Cardiovasc. Dis. 2007, 17, 319–326. [Google Scholar] [CrossRef] [PubMed]
- Cancello, R.; Tordjman, J.; Poitou, C.; Guilhem, G.; Bouillot, J.L.; Hugol, D.; Coussieu, C.; BaSDevant, A.; Bar Hen, A.; Bedossa, P.; et al. Increased infiltration of macrophages in omental adipose tissue is associated with marked hepatic lesions in morbid human obesity. Diabetes 2006, 55, 1554–1561. [Google Scholar] [CrossRef] [PubMed]
- Shivappa, N.; Steck, S.E.; Hurley, T.G.; Hussey, J.R.; Hébert, J.R. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014, 17, 1689–1696. [Google Scholar] [CrossRef] [PubMed]
- Barbaresko, J.; Koch, M.; Schulze, M.B.; Nöthlings, U. Dietary pattern analysis and biomarkers of low-grade inflammation: A systematic literature review. Nutr. Rev. 2013, 71, 511–527. [Google Scholar] [CrossRef] [PubMed]
| Dimension 1 | Definition |
|---|---|
| Good physical functioning (yes/no) | Short Physical Performance Battery (SPPB) score ≥11/12 The SPPB includes 3 tests (administered by trained physicians): Repeated chair stands, balance testing, gait speed testing [38]. Higher scores on the SPPB indicate better performance. |
| Good cognitive functioning (yes/no) | Mini Mental State Examination (MMSE) score ≥27/30 and rappel indicé—48 items (RI-48) score ≥19/48 and Delis-Kaplan Trail-making test (DK-TMT) scaled score ≥5.5 The MMSE [39] tests global cognitive functioning, the RI-48 tests verbal episodic memory [40], and the DK-TMT tests mental flexibility [41,42]. Higher scores on each test indicate better performances. All three tests were administered by trained neuropsychologists or geriatric physicians. |
| No limitations in IADL (yes/no) | <1 limitation on the Lawton Scale of Instrumental Activites of Daily Living (IADL) The Lawton IADL scale [43] is a self-administered questionnaire (including, amongst others, questions on the ability to travel, go shopping, and do housekeeping). Having more limitations on the scale indicates lower independence in daily life. |
| No depressive symptoms (yes/no) | Center for Epidemiological Studies Depression Scale (CES-D) score <16/60 The CES-D [44] is a self-administered questionnaire developed for the evaluation of depressive symptoms in the general population, within epidemiological studies. Higher scores indicate more depressive symptoms. |
| No health-related limitations in social life (yes/no) | No/only slight and only infrequent (perceived) interference of health problems with social life Data were collected via the Medical Outcome Study Short Form-36 (SF-36) questionnaire [45], a very widely used, self-administered questionnaire designed to measure vitality, physical functioning, bodily pain, general health perceptions, physical role functioning, emotional role functioning, social role functioning, and mental health |
| Good overall self-perceived health (yes/no) | To meet this criterion, participants had to declare that their health was generally “good” to “excellent” Participants’ responses were collected via the SF-36 questionnaire [45]. |
| No function-limiting pain (yes/no) | To meet this criterion, participants had to report having experienced no more than “mild” physical pain during the previous month or that such pain had only limited or no impact on their daily activities Participants’ responses were collected via the SF-36 questionnaire [45]. |
| No incident major chronic disease (yes/no) | No incident cancer, cardiovascular disease, or diabetes during follow-up Events of cancer and of cardiovascular disease were recorded during follow-up and validated by an independent external committee of medical doctors. Cancer was defined as cancer of any kind, except for basal cell carcinoma. Cardiovascular disease was defined as codes I20–I25, I63, I65, I66, I70, I71, and I74 from the 10th International World Health Organization Classification of Diseases). Incident diabetes was defined as having a fasting blood glucose value ≥ 1.26 g/L, anti-diabetic medication use, or self-reported diabetes at the end of follow-up. |
| Overall healthy aging | Participants meeting all of the above criteria were considered to be aging healthily, while participants for which at least one criterion was = “no” were not considered to be aging healthily → Thus, a binary indicator of overall healthy aging was obtained (yes/no). |
| Healthy Aging Status | |||
|---|---|---|---|
| Sample Characteristics a | Number | Yes | P-Value b |
| Number (%) | 1368 (60.8) | 881 (39.2) | |
| Age, y, mean (SD) | 52.3 (4.6) | 51.3 (4.3) | <0.0001 |
| Gender (male), % | 51.3 | 56.9 | 0.01 |
| Region of residence, % | 0.19 | ||
| Larger Paris-region (“Ile de France“) | 22.2 | 20.8 | |
| North-east and north-west of France | 15.8 | 13.1 | |
| West, mid-west, and “Rhone Alpes”- regions | 45.3 | 48.6 | |
| South-west and Mediterranean regions | 16.7 | 17.6 | |
| Educational level, % | <0.0001 | ||
| Primary education only | 23.6 | 16.6 | |
| Secondary education | 40.4 | 38.5 | |
| University level | 36.0 | 44.9 | |
| Occupational status, % | <0.0001 | ||
| Homemaker | 8.0 | 6.2 | |
| Manual worker | 6.8 | 4.1 | |
| Office employee | 57.2 | 52.0 | |
| Intellectual profession c | 28.0 | 37.7 | |
| Smoking status, % | 0.10 | ||
| Non-smoker | 50.1 | 51.8 | |
| Former smoker | 38.4 | 39.5 | |
| Current smoker | 11.5 | 8.7 | |
| Family situation | 0.01 | ||
| Living alone | 14.2 | 10.7 | |
| Married/cohabiting | 85.8 | 89.3 | |
| Physical activity level, % | <0.0001 | ||
| Irregular or none | 25.9 | 18.5 | |
| <1 h/day | 30.0 | 29.8 | |
| ≥1 h/day | 44.1 | 51.7 | |
| Antioxidant supplementation (yes), % | 51.5 | 54.7 | 0.14 |
| Alcohol consumption, g/day, mean (SD) | 16.8 (17.4) | 17.0 (17.2) | 0.40 |
| Number of 24h records, mean (SD) | 10.1 (3.2) | 10.4 (2.9) | 0.04 |
| PNNS-GS (points), mean (SD) | 7.7 (1.9) | 8.0 (1.9) | 0.001 |
| Body mass index (kg/m2), mean (SD) | 24.5 (3.5) | 24.0 (2.9) | 0.01 |
| Body mass index status, % | 0.0002 | ||
| BMI < 25 kg/m2 | 61.5 | 66.3 | |
| BMI ≥ 25 and <30 kg/m2 | 31.1 | 30.3 | |
| BMI ≥ 30 kg/m2 | 7.4 | 3.4 | |
| Total energy intake (kcal/d), mean (SD) | 2194.5 (629.0) | 2221.7 (595.7) | 0.22 |
| Protein (% energy/d), mean (SD) | 16.7 (2.6) | 16.5 (2.5) | 0.09 |
| CarbohyDrates (% energy/d), mean (SD) | 39.6 (6.7) | 39.9 (6.3) | 0.55 |
| Total fat (% energy/d), mean (SD) | 37.6 (5.1) | 37.6 (4.7) | 0.88 |
| SFA (% energy/d), mean (SD) | 15.4 (2.7) | 15.5 (2.5) | 0.71 |
| MUFA (% energy/d), mean (SD) | 14.2 (2.2) | 14.2 (2.1) | 0.85 |
| PUFA (% energy/d), mean (SD) | 5.7 (1.5) | 5.7 (1.4) | 0.93 |
| Fiber intake (g/d), mean (SD) | 20.1 (7.3) | 20.6 (7.1) | 0.04 |
| Sodium intake (mg/d), mean (SD) | 3613.6 (1231.7) | 3623.2 (1188.1) | 0.72 |
| Nutritional Score | RR (95% CI) | p-Value |
|---|---|---|
| PNNS-GS | 1.06 (1.03, 1.09) | 0.0001 |
| PNNS-GS without Physical activity component | 1.04 (1.01, 1.08) | 0.0109 |
| PNNS-GS without Seafood component | 1.06 (1.02, 1.09) | 0.0009 |
| PNNS-GS without Fruits and vegetables component | 1.06 (1.03, 1.10) | 0.0006 |
| PNNS-GS without Whole grain food component | 1.06 (1.03, 1.10) | 0.0001 |
| PNNS-GS without Total added fats component | 1.06 (1.03, 1.09) | 0.0002 |
| PNNS-GS without Salt component | 1.06 (1.03, 1.09) | 0.0002 |
| PNNS-GS without Vegetable added fats component | 1.07 (1.04, 1.10) | <0001 |
| PNNS-GS without Alcohol component | 1.06 (1.03, 1.09) | 0.0002 |
| PNNS-GS without Meat and poultry, seafood and eggs component | 1.06 (1.03, 1.09) | 0.0002 |
| PNNS-GS without Milk and dairy products component | 1.06 (1.03, 1.09) | 0.0001 |
| PNNS-GS without Sweetened foods component c | 1.06 (1.03, 1.09) | 0.0002 |
| PNNS-GS without Bread, cereals, potatoes and legumes | 1.06 (1.03, 1.09) | 0.0001 |
| PNNS-GS without Beverages component d | 1.06 (1.03, 1.09) | 0.0002 |
| PNNS-GS Quartiles RR (95% CI) b | |||||
|---|---|---|---|---|---|
| Q1 <6.55 | Q2 (6.55–7.80) | Q3 (7.80–9.05) | Q4 >9.05 | Ptrend | |
| Direct effect a | 1.00 (ref) | 1.08 (0.92, 1.26) | 1.20 (1.03, 1.40) | 1.31 (1.13, 1.53) | 0.0002 |
| Indirect effect c | 1.00 (ref) | 1.01 (1.00, 1.01) | 1.01 (1.00, 1.01) | 1.01 (1.01, 1.02) | 0.0003 |
| Total effect d | 1.00 (ref) | 1.09 (0.92, 1.26) | 1.21 (1.03, 1.41) | 1.33 (1.13, 1.55) | |
| Mediation (%) e | 7% | 5% | 5% | ||
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Assmann, K.E.; Ruhunuhewa, I.; Adjibade, M.; Li, Z.; Varraso, R.; Hercberg, S.; Galan, P.; Kesse-Guyot, E. The Mediating Role of Overweight and Obesity in the Prospective Association between Overall Dietary Quality and Healthy Aging. Nutrients 2018, 10, 515. https://doi.org/10.3390/nu10040515
Assmann KE, Ruhunuhewa I, Adjibade M, Li Z, Varraso R, Hercberg S, Galan P, Kesse-Guyot E. The Mediating Role of Overweight and Obesity in the Prospective Association between Overall Dietary Quality and Healthy Aging. Nutrients. 2018; 10(4):515. https://doi.org/10.3390/nu10040515
Chicago/Turabian StyleAssmann, Karen E., Indunil Ruhunuhewa, Moufidath Adjibade, Zhen Li, Raphaëlle Varraso, Serge Hercberg, Pilar Galan, and Emmanuelle Kesse-Guyot. 2018. "The Mediating Role of Overweight and Obesity in the Prospective Association between Overall Dietary Quality and Healthy Aging" Nutrients 10, no. 4: 515. https://doi.org/10.3390/nu10040515
APA StyleAssmann, K. E., Ruhunuhewa, I., Adjibade, M., Li, Z., Varraso, R., Hercberg, S., Galan, P., & Kesse-Guyot, E. (2018). The Mediating Role of Overweight and Obesity in the Prospective Association between Overall Dietary Quality and Healthy Aging. Nutrients, 10(4), 515. https://doi.org/10.3390/nu10040515





