On Your Own: Older Adults’ Food Choice and Dietary Habits
Abstract
:1. Introduction
2. Materials and Methods
2.1. Recruitment and Participants
2.2. Focus-Group Interviews
2.3. Data Analysis
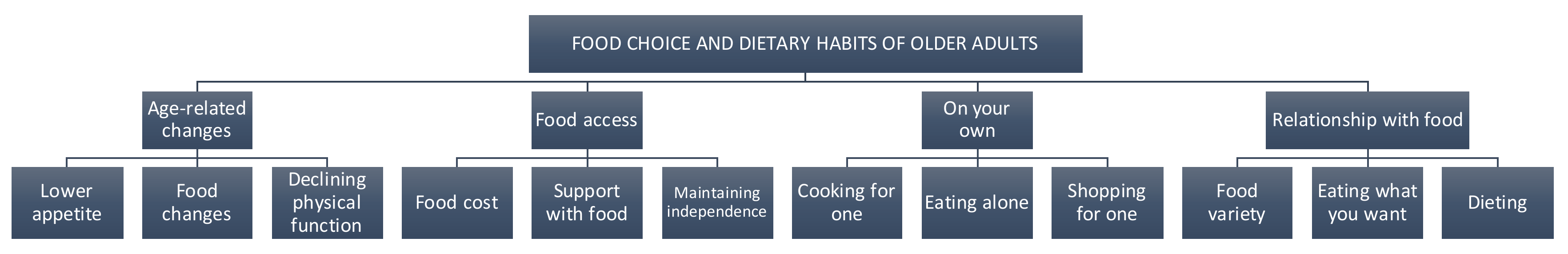
3. Results
3.1. Age-Related Changes
3.1.1. Lower Appetite
… I eat smaller meals, because I can’t eat … at one-time big plate like this [gestures piled-up plate]: lovely! But now it’s, you know, I just can’t face it anymore. (P24)I went for my dinner to my daughter’s on Sunday and I said, “Don’t pile my plate up because I won’t be able to eat it!” (P19)Yeah, you eat less. It’s like filling a car—you don’t put petrol [in] if you aren’t going anywhere. (P12)P8: So here [lunch club at community centre] we always say, “Smaller pile on my plate please” … but they don’t, and then we just leave it, but we don’t want to leave it.P7: It’s wasting, which is going against the grain for us; our age, we don’t waste nothing […] waste not, want not.P8: No matter what we say, they don’t change it [portion size].P7: It out faces you …
We went to Bridlington on Friday, and we went into this pub for our dinner, and it were a child’s dinner. And it was really ample enough for an adult, and it were only 3 pounds something, and it were a child’s one. And all four of us had one and it were lovely. (P23)
3.1.2. Food Changes
When I was younger and [with] a family I probably ate more meat, but as I’ve got older I eat more fish and probably lighter meals, rather than heavy meals. (P27)Your taste buds change. Some food don’t taste the same as it used to. I think that’s why I dose it with salt. (P4)P7: I could do without meat.P9: I could do without meat too.P7: I like fish, but meat: I’m not bothered about … I think [it’s a recent change] … and I don’t know why … it’s probably the chewing! I don’t know.
3.1.3. Declining Physical Function
I do have a lot of pain and I’d be sat there sometimes and be like, “I can’t be bothered, getting up and cooking a dinner now!” and I’d have a sandwich or something. (P8)I always used to sort of do wedding cakes and anniversary cakes, but as I’ve got older my hands won’t let me do that … So, I’ve lost interest in doing a lot of baking. I can’t do what I want to do, so I’ve just not bothered. I get so frustrated otherwise. (P24)I used to bake a lot, you know, apples pies, custard tarts and everything, and it all got eaten—but I don’t now for myself. I go to Morrisons (supermarket retailer) and look on the naughty counter … I think it’s [baking] too much hassle because I’ve moved into a flat and I’ve got an oven-cooker, whereas in my house my cooker was there [standing height], but now it’s down there [near the floor] … and it’s a problem getting the stuff out, sat down getting it out. (P7)
3.2. Food Access
3.2.1. Food Cost
I always used to go for a brand name, a particular one, but I keep trying now the cheaper one [supermarket’s own brand]. (P16)Well when I go into town I eat at McDonald’s or I go to the pound bakery and buy stuff there, because it’s so expensive to go and eat in a café now. Years ago when I was working I’d go to a café and eat, but not now. (P10)Well I go to Aldi and I usually try to go early in the morning because of the reduced stuff. You can get meat 30% off or 50% off … if you are lucky you find. (P12)I usually go to Tesco or Aldi; I prefer Tesco—it’s the first place I go. I have my list and my wheelie trolley. When I go to Tesco, the first place I go is the reduced counter. Have a look there, and if there’s anything worth buying I’ll plan my meals around that. And I go to Fultons (value food store) as well because they do some good bargains in there. (P10)
3.2.2. Support with Food
I used to go [food shopping] with a friend that I had, and she drove a car and I don’t. We used to go somewhere out for the day and then go to the supermarket. But unfortunately, she died recently. So, my son started getting it [food shopping] for me. (P8)I shop once a week at Morrisons on the Access Bus (door-to-door bus service). It picks us up and drops us off. We have an hour shopping … and I do my weekly shop there. (P7)
The beauty of going to a carvery when you’re on your own is that you have a choice of a roast joint, and I think everyone would possibly agree with me on this one: we buy chops, or mince, or we buy pieces of steak because you can’t buy a joint for one …. because if you buy a small joint and roast it, it ends up looking like an Oxo cube—it shrinks. If you go to a carvery you’ve got the benefit of this lovely roast which is what we did years ago as a family. (P17)
3.2.3. Maintaining Independence
You don’t want someone arranging your life for you. You want to decide for yourself. (P1)It’s about maintaining your independence. (P4)
3.3. On Your Own
3.3.1. Cooking for One
Unfortunately, I woke up one morning a widow so I thought I might as well use the microwave. I just couldn’t be bothered. (P30)When you’re on your own you just can’t be bothered, you know. (P28)P19: I do think you neglect yourself when you’re on your own. Definitely, yeah.P18: Because you know you’ve got to make it if someone’s there, don’t you.I think I could just about still make a roast dinner if I had the need to, but I haven’t done it for years because you don’t cook like that when you’re on your own. (P17)P27: It’s motivation I think really: “Owh, I’m on my own—it don’t matter.”P28: You get like that …P27: But I think sort of spending a bit of time cooking … it can be lonely, you see, when people live on their own.P28: Yes it can.P27: Especially at meal times you know.
3.3.2. Eating Alone
We go out on a Wednesday, bowling or something like that, then we usually enjoy a meal. You go through it [the food] but you don’t realise the time’s gone, whereas you sit on your own [pretends to stare into the distance] … (P20)
If I’ve done myself what I call a ‘proper big dinner’, I’ll cook it and put it on my plate and look at it and think, “I don’t really want that now”. (P24)
P20: … I have my grandkids round at the weekend and that’s much better because I can sit with them. And I’ve cooked them a meal and probably on a Sunday or something we’ve had a big roast dinner […] You enjoy it because someone else is there, but sat on your own sometimes it’s …P24: It [food] looks a bit overpowering sometimes, don’t it?P14: My wife used to do it [cooking]. I can cook but I just can’t be bothered. When you do it for yourself, by the time you’ve done it you don’t feel like eating it … well, I don’t.P16: That’s true actually.P17: You don’t enjoy it the same when you’re sitting and eating on your own because there is no one to say sort of, “That was nice” or “I’ll do the dishes”. It’s the other bits that go with it isn’t it, the social part of it.
P20: … although he [husband] was very awkward with his food there was still somebody there. We didn’t always have the same meals but you’ve got somebody there. Somebody else in the room with you, and you were eating.P21: Yeah, it makes a difference […] You’ve sort of lost the incentive.P20: I sometimes think when you’re on your own and you sit down the moment’s gone.P21: Mind you that’s the same … when they were sat in the chair and you were maybe sat reading or knitting but they were there in the chair … and it’s that sort of feeling.P20: Yeah that’s it … and even if there was no sort of communication there was somebody there.P21: And [now] you end up talking to yourself.P20: There was still somebody there, but now you’re sat there.P21: It’s amazing what difference it makes i’nt it?
3.3.3. Shopping for One
Sometimes when you’ve cooked for family throughout your life and then all of a sudden you’re on your own, you’re sat on your own, you’ve got to sort of think, “I’m just doing it for me”. I found that hard, to stop shopping for a family when there were only me. (P26)I find when you buy packs of vegetables from Morrisons there’s too much in them. I love spring cabbage and I haven’t bought any for ages because there’s a load of it. (P7)P16: There’s not much in supermarkets for one.P14: A lot of things are in packs.P17: You can buy an orange, apple, grapefruit and snap a banana off—but the rest of it’s in packs.P15: Even parsnips, things like that; you don’t want a pack of 6 or 7 parsnips. I just want one.I like small portions because if I get a big bag of potatoes they end up sprouting. (P1)We’ve found Morrisons is a little bit expensive. “Buy 2 for 1”; we don’t want two. There are a lot of things like that in Morrisons. (P12)
That’s the biggest problem when you’re on your own—boredom. It’s no good sat there watching the television all the time. Watching the television all day, I call it a ‘no day’. You’re just sat there watching the telly like a zombie. (P12)Well I go [food shopping] every day. Mostly it’s something to do, you know. I know it’s a bit sad. (P14)I try and go shopping every day, basically because it gets me out of the house. (P10)
3.4. Relationship with Food
3.4.1. Food Variety
I like interesting meals and I like varied meals. I don’t like the same thing over and over again. (P21)I tried scallops the other day. They’re quite nice aren’t they! I wouldn’t cook it though—I went to someone’s Christmas party. (P1)
P18: You could get a tin out and make a sandwich, but now I look and I think, “I don’t want that” […] I think it’s because you’re bored, I don’t really know.P19: I think it’s boredom … because you, I don’t know, you just seem to eat the same sort of food day in day out, sort of thing.I like interesting food. I like interesting meals and I like varied meals. I don’t like the same thing over and over again. I’d eat it, don’t get me wrong, I’d eat it, but I would wish for a change. (P21)
3.4.2. Eating What You Want
I’ve got a very sweet tooth, I’ve not got a savoury tooth. Well I eat things I shouldn’t eat really; but if I want it I have it. (P4)… I used to look at calories, once upon a time, but not now. Not watching my figure now! (P1)I think you come to a stage you think, “Right that’s it, enjoy yourself!” … But as I say: in moderation. I like most things, especially if they’re cooked for me. I’d eat anything … I eat more or less anything. (P14)… They all say: a little bit of what you fancy does you good. (P16)
3.4.3. Dieting
I think once you get to 60 you find it really hard to get your weight off, don’t you? (P18)I’ll go as far as saying, I found it much, much easier to stop smoking than diet. And I just said, “Right that’s it; I’m having no more!” and no more did I have. Now I couldn’t do that with a diet! (P19)I put weight on very quickly, I always have done—so I now make a conscious effort. I’ve yo-yoed, my weight all my life. But I think I’m realising now you can still eat and eat well without the rubbishy food. But I still have it, everything in moderation. A little bit of what you fancy does you good. So I try to keep it that way. (P15)
I did it [went on a diet and lost weight] when they told me I needed a new hip, didn’t I. I did it then. They didn’t do my hips, so that disheartened me. So now I think I will do it because I’m due back to see them in December. (P18)
4. Discussion
Implications for Policy and Practice
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Office for National Statistics. Population Estimates for UK, England and Wales, Scotland and Northern Ireland: Mid 2015; Office for National Statistics: Newport, UK, 2016. [Google Scholar]
- United Nations. World Population Ageing 2015 (ST/ESA/SER.A/390); United Nations: New York, NY, USA, 2015. [Google Scholar]
- Age UK. Briefing: Health and Care of Older People in England 2017; Age UK: London, UK, 2017. [Google Scholar]
- Mak, T.N.; Caldeira, S. The Role of Nutrition in Active and Healthy Ageing; Publications Office of the European Union: Luxembourg, 2014. [Google Scholar]
- Ahmed, T.; Haboubi, N. Assessment and management of nutrition in older people and its importance to health. Clin. Interv. Aging 2010, 5, 207–216. [Google Scholar] [PubMed]
- Illario, M.; Vollenbroek-Hutten, M.M.R.; Molloy, D.W.; Menditto, E.; Iaccarino, G.; Eklund, P. Active and Healthy Ageing and Independent Living 2016. J. Aging Res. 2016, 2016, 8062079. [Google Scholar] [CrossRef] [PubMed]
- Host, A.; McMahon, A.-T.; Walton, K.; Charlton, K. Factors Influencing Food Choice for Independently Living Older People—A Systematic Literature Review. J. Nutr. Gerontol. Geriatr. 2016, 35, 67–94. [Google Scholar] [CrossRef] [PubMed]
- Pilgrim, A.L.; Robinson, S.M.; Sayer, A.A.; Roberts, H.C. An overview of appetite decline in older people. Nurs. Older People 2015, 27, 29–35. [Google Scholar] [CrossRef] [PubMed]
- Nieuwenhuizen, W.F.; Weenen, H.; Rigby, P.; Hetherington, M.M. Older adults and patients in need of nutritional support: Review of current treatment options and factors influencing nutritional intake. Clin. Nutr. 2010, 29, 160–169. [Google Scholar] [CrossRef] [PubMed]
- Di Francesco, V.; Fantin, F.; Residori, L.; Bissoli, L.; Micciolo, R.; Zivelonghi, A.; Zoico, E.; Omizzolo, F.; Bosello, O.; Zamboni, M. Effect of age on the dynamics of acylated ghrelin in fasting conditions and in response to a meal. J. Am. Geriatr. Soc. 2008, 56, 1369–1370. [Google Scholar] [CrossRef] [PubMed]
- De Boer, A.; Ter Horst, G.J.; Lorist, M.M. Physiological and psychosocial age-related changes associated with reduced food intake in older persons. Ageing Res. Rev. 2013, 12, 316–328. [Google Scholar] [CrossRef] [PubMed]
- Wysokiński, A.; Sobów, T.; Kłoszewska, I.; Kostka, T. Mechanisms of the anorexia of aging—A review. Age (Dordr.) 2015, 37, 9821. [Google Scholar] [CrossRef] [PubMed]
- Doty, R.L. Influence of age and age-related diseases on olfactory function. Ann. N. Y. Acad. Sci. 1989, 561, 76–86. [Google Scholar] [CrossRef] [PubMed]
- Schiffman, S.S. Taste and smell losses in normal aging and disease. JAMA 1997, 278, 1357–1362. [Google Scholar] [CrossRef] [PubMed]
- Toussaint, N.; de Roon, M.; van Campen, J.P.C.M.; Kremer, S.; Boesveldt, S. Loss of Olfactory Function and Nutritional Status in Vital Older Adults and Geriatric Patients. Chem. Senses 2015, 40, 197–203. [Google Scholar] [CrossRef] [PubMed]
- Gopinath, B.; Russell, J.; Sue, C.M.; Flood, V.M.; Burlutsky, G.; Mitchell, P. Olfactory impairment in older adults is associated with poorer diet quality over 5 years. Eur. J. Nutr. 2016, 55, 1081–1087. [Google Scholar] [CrossRef] [PubMed]
- Forde, C.G.; Delahunty, C.M. Examination of chemical irritation and textural influence on food preferences in two age cohorts using complex food systems. Food Qual. Prefer. 2002, 13, 571–581. [Google Scholar] [CrossRef]
- Pelchat, M.L.; Schaefer, S. Dietary monotony and food cravings in young and elderly adults. Physiol. Behav. 2000, 68, 353–359. [Google Scholar] [CrossRef]
- Kremer, S.; Bult, J.H.F.; Mojet, J.; Kroeze, J.H.A. Food Perception with Age and Its Relationship to Pleasantness. Chem. Senses 2007, 32, 591–602. [Google Scholar] [CrossRef] [PubMed]
- Hildebrandt, G.H.; Dominguez, B.L.; Schork, M.A.; Loesche, W.J. Functional units, chewing, swallowing, and food avoidance among the elderly. J. Prosthet. Dent. 1997, 77, 588–595. [Google Scholar] [CrossRef]
- Smith, M.B.; Parnell, W. Teeth for life? Aspects of oral health status influencing the nutrition of older adults. Nutr. Diet. 2008, 65, 211–215. [Google Scholar]
- Shatenstein, B. Impact of health conditions on food intakes among older adults. J. Nutr. Elder. 2008, 27, 333–361. [Google Scholar] [CrossRef] [PubMed]
- Age UK. Later Life in the United Kingdom; Age UK: London, UK, 2017. [Google Scholar]
- Hickson, M. Malnutrition and ageing. Postgrad. Med. J. 2006, 82, 2–8. [Google Scholar] [CrossRef] [PubMed]
- Harrop, A.; Jopling, K. One Voice. Shaping Our Ageing Society; Age UK: London, UK, 2009. [Google Scholar]
- Host, A.; McMahon, A.-T.; Walton, K.; Charlton, K. “While we can, we will”: Exploring food choice and dietary behaviour amongst independent older Australians. Nutr. Diet. 2016, 73, 463–473. [Google Scholar] [CrossRef]
- Wham, C.A.; Bowden, J.A. Eating for health: Perspectives of older men who live alone. Nutr. Diet. 2011, 68, 221–226. [Google Scholar] [CrossRef]
- Kamphuis, C.B.; de Bekker-Grob, E.W.; van Lenthe, F.J. Factors affecting food choices of older adults from high and low socioeconomic groups: A discrete choice experiment. Am. J. Clin. Nutr. 2015, 101, 768–774. [Google Scholar] [CrossRef] [PubMed]
- Sinclair, A.; Ryan, B.; Hill, D. Sight Loss in Older People: The Essential Guide for General Practice; RNIB: London, UK, 2014. [Google Scholar]
- Rosenbloom, C.A.; Whittington, F.J. The effects of bereavement on eating behaviors and nutrient intakes in elderly widowed persons. J. Gerontol. 1993, 48, S223–S229. [Google Scholar] [CrossRef] [PubMed]
- Johnson, C.S. Nutritional considerations for bereavement and coping with grief. J. Nutr. Health Aging 2002, 6, 171–176. [Google Scholar] [PubMed]
- Office for National Statistics. Families and Households; Office for National Statistics: Newport, UK, 2017. [Google Scholar]
- Atkins, J.L.; Ramsay, S.E.; Whincup, P.H.; Morris, R.W.; Lennon, L.T.; Wannamethee, S.G. Diet quality in older age: The influence of childhood and adult socio-economic circumstances. Br. J. Nutr. 2015, 113, 1441–1452. [Google Scholar] [CrossRef] [PubMed]
- Beatty, T.K.M.; Blow, L.; Crossley, T.F. Is there a “heat-or-eat” trade-off in the UK? J. R. Stat. Soc. Ser. A Stat. Soc. 2014, 177, 281–294. [Google Scholar] [CrossRef]
- Public Health Institue. Conducting Aging Well Focus Groups Aging Well in Communities: A Toolkit for Planning, Engagement & Action; Public Health Institute: Sacramento, CA, USA, 2010. [Google Scholar]
- Draper, A.; Swift, J.A. Qualitative research in nutrition and dietetics: Data collection issues. J. Hum. Nutr. Diet. 2011, 24, 3–12. [Google Scholar] [CrossRef] [PubMed]
- Guest, G.; Bunce, A.; Johnson, L. How Many Interviews Are Enough? Field Methods 2006, 18, 59–82. [Google Scholar] [CrossRef]
- Oliver, D.G.; Serovich, J.M.; Mason, T.L. Constraints and Opportunities with Interview Transcription: Towards Reflection in Qualitative Research. Soc. Forces 2005, 84, 1273–1289. [Google Scholar] [CrossRef] [PubMed]
- Fade, S.A.; Swift, J.A. Qualitative research in nutrition and dietetics: Data analysis issues. J. Hum. Nutr. Diet. 2011, 24, 106–114. [Google Scholar] [CrossRef] [PubMed]
- Thomas, D.R. A General Inductive Approach for Analyzing Qualitative Evaluation Data. Am. J. Eval. 2006, 27, 237–246. [Google Scholar] [CrossRef]
- Bloom, I.; Lawrence, W.; Barker, M.; Baird, J.; Dennison, E.; Sayer, A.A.; Cooper, C.; Robinson, S. What influences diet quality in older people? A qualitative study among community-dwelling older adults from the Hertfordshire Cohort Study, UK. Public Health Nutr. 2017, 20, 2685–2693. [Google Scholar] [PubMed]
- Hughes, G.; Bennett, K.M.; Hetherington, M.M. Old and alone: Barriers to healthy eating in older men living on their own. Appetite 2004, 43, 269–276. [Google Scholar] [CrossRef]
- Sidenvall, B.; Nydahl, M.; Fjellström, C. The Meal as a Gift—The Meaning of Cooking Among Retired Women. J. Appl. Gerontol. 2000, 19, 405–423. [Google Scholar] [CrossRef]
- Wham, C.; McLean, C.; Teh, R.; Moyes, S.; Peri, K.; Kerse, N. The bright trial: What are the factors associated with nutrition risk? J. Nutr. Health Aging 2014, 18, 692–697. [Google Scholar] [CrossRef] [PubMed]
- Locher, J.L.; Ritchie, C.S.; Roth, D.L.; Baker, P.S.; Bodner, E.V.; Allman, R.M. Social isolation, support, and capital and nutritional risk in an older sample: Ethnic and gender differences. Soc. Sci. Med. 2005, 60, 747–761. [Google Scholar] [CrossRef] [PubMed]
- Vesnaver, E.; Keller, H.H.; Sutherland, O.; Maitland, S.B.; Locher, J.L. Alone at the Table: Food Behavior and the Loss of Commensality in Widowhood. J. Gerontol. Ser. B Psychol. Sci. Soc. Sci. 2016, 71, 1059–1069. [Google Scholar] [CrossRef] [PubMed]
- Ferry, M.; Sidobre, B.; Lambertin, A.; Barberger-Gateau, P. The SOLINUT study: Analysis of the interaction between nutrition and loneliness in persons aged over 70 years. J. Nutr. Health Aging 2005, 9, 261–268. [Google Scholar] [PubMed]
- Wylie, C. A20. Health and social factors affecting the food choices and nutritional intake of elderly people with restricted mobility. J. Hum. Nutr. Diet. 2000, 13, 363–371. [Google Scholar]
- Liu, L.; Gou, Z.; Zuo, J. Social support mediates loneliness and depression in elderly people. J. Health Psychol. 2016, 21, 750–758. [Google Scholar] [CrossRef] [PubMed]
- Cabrera, M.A.S.; Mesas, A.E.; Garcia, A.R.L.; de Andrade, S.M. Malnutrition and Depression among Community-dwelling Elderly People. J. Am. Med. Dir. Assoc. 2007, 8, 582–584. [Google Scholar] [CrossRef] [PubMed]
- Holmes, B.A.; Roberts, C.L. Diet quality and the influence of social and physical factors on food consumption and nutrient intake in materially deprived older people. Eur. J. Clin. Nutr. 2011, 65, 538–545. [Google Scholar] [CrossRef] [PubMed]
- Delaney, M.; McCarthy, M. Food Choice and Health across the Life Course: A Qualitative Study Examining Food Choice in Older Irish Adults. J. Food Prod. Mark. 2011, 17, 114–140. [Google Scholar] [CrossRef]
- Locher, J.L.; Ritchie, C.S.; Roth, D.L.; Sen, B.; Vickers, K.S.; Vailas, L.I. Food choice among homebound older adults: motivations and perceived barriers. J. Nutr. Health Aging 2009, 13, 659–664. [Google Scholar] [CrossRef] [PubMed]
- Lane, K.; Poland, F.; Fleming, S.; Lambert, N.; Macdonald, H.; Potter, J.; Raats, M.; Skidmore, P.; Vince, C.; Wellings, A.; et al. Older women’s reduced contact with food in the Changes Around Food Experience (CAFE) study: Choices, adaptations and dynamism. Ageing Soc. 2014, 34, 645–669. [Google Scholar] [CrossRef]
- Devine, C.M. A life course perspective: understanding food choices in time, social location, and history. J. Nutr. Educ. Behav. 2005, 37, 121–128. [Google Scholar] [CrossRef]
- Malnutrition Task Force. State of the Nation Older People and Malnutrition in the UK Today; Malnutrition Task Force: London, UK, 2017. [Google Scholar]
- Stratton, R.J.; Elia, M. Deprivation linked to malnutrition risk and mortality in hospital. Br. J. Nutr. 2006, 96, 870–876. [Google Scholar] [CrossRef] [PubMed]
- Blane, D.; Abraham, L.; Gunnell, D.; Maynard, M.; Ness, A. Background influences on dietary choice in early old age. J. R. Soc. Promot. Health 2003, 123, 204–209. [Google Scholar] [CrossRef] [PubMed]
- Vesnaver, E.; Keller, H.H.; Sutherland, O.; Maitland, S.B.; Locher, J.L. Food behavior change in late-life widowhood: A two-stage process. Appetite 2015, 95, 399–407. [Google Scholar] [CrossRef] [PubMed]
- Age UK. Evidence Review: Loneliness in Later Life; Age UK: London, UK, 2014. [Google Scholar]
- Bloom, I.; Edwards, M.; Jameson, K.A.; Syddall, H.E.; Dennison, E.; Gale, C.R.; Baird, J.; Cooper, C.; Aihie Sayer, A.; Robinson, S. Influences on diet quality in older age: The importance of social factors. Age Ageing 2017, 46, 277–283. [Google Scholar] [CrossRef] [PubMed]
- Stokes-Lampard, H. RCGP Conference 2017 Speech. Available online: https://www.gponline.com/read-professor-helen-stokes-lampards-rcgp-conference-2017-speech-full/article/1447175 (accessed on 23 January 2018).
- Jo Cox Commission on Loneliness. Combatting Loneliness One Conversation at A Time. Available online: https://www.jocoxloneliness.org/pdf/a_call_to_action.pdf (accessed on 23 January 2018).
| Characteristic | N |
|---|---|
| Gender | |
| Male | 5 |
| Female | 25 |
| Age (years) | |
| 60–65 | 1 |
| 66–70 | 7 |
| 71–75 | 4 |
| 76–80 | 10 |
| 81–85 | 6 |
| 86–90 | 2 |
| Ethnic origin | |
| White British | 29 |
| White Irish | 1 |
| Employment status | |
| Retired | 28 |
| Unemployed | 2 |
| Relationship status | |
| Married | 3 |
| Divorced | 5 |
| Separated | 1 |
| Single | 3 |
| Widowed | 17 |
| In a relationship but not cohabiting | 1 |
| IMD decile * | |
| 1 | 15 |
| 2 | 4 |
| 3 | 3 |
| 5 | 2 |
| 6 | 3 |
| 7 | 1 |
| Number of people in household including self | |
| 1 Adult | 26 |
| 2 Adults | 2 |
| 3 Adults | 2 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Whitelock, E.; Ensaff, H. On Your Own: Older Adults’ Food Choice and Dietary Habits. Nutrients 2018, 10, 413. https://doi.org/10.3390/nu10040413
Whitelock E, Ensaff H. On Your Own: Older Adults’ Food Choice and Dietary Habits. Nutrients. 2018; 10(4):413. https://doi.org/10.3390/nu10040413
Chicago/Turabian StyleWhitelock, Emily, and Hannah Ensaff. 2018. "On Your Own: Older Adults’ Food Choice and Dietary Habits" Nutrients 10, no. 4: 413. https://doi.org/10.3390/nu10040413
APA StyleWhitelock, E., & Ensaff, H. (2018). On Your Own: Older Adults’ Food Choice and Dietary Habits. Nutrients, 10(4), 413. https://doi.org/10.3390/nu10040413




