Assessment of Mycotoxin Exposure in Breastfeeding Mothers with Celiac Disease
Abstract
:1. Introduction
2. Materials and Methods
2.1. Exclusion Criteria
- (A)
- Lactation in the first two weeks after delivery for the following reasons: to avoid the generation of anxiety in breastfeeding women at-risk for stress-induced hypogalactia in the early weeks of lactation; and to consider only mature milk rather than colostrum in the analysis.
- (B)
- Lactation for more than four months, as we attempted to estimate exposure to mycotoxins in breastfed babies rather than in children on complementary feeding during weaning.
- (C)
- Diagnosis of diabetes mellitus (both type-1 and type-2), since it might have slightly changed food choices.
- (D)
- Feeding disorders or food allergy, since it might have slightly changed food choices.
- (E)
- Being on a restricted diet for medical/ethical/religious reasons (including non-celiac gluten sensitivity among controls), since it might have slightly changed food choices.
- (F)
- Family history of CD (control group only). This exclusion criterion was set to minimize possible switch to gluten-free foods by chance (e.g., shared meals in family) during the study period.
2.2. Human Milk Analysis
2.3. Dietary Survey
2.4. Statistics
3. Results
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Wu, F.; Groopman, J.D.; Pestka, J.J. Public health impacts of foodborne mycotoxins. Annu. Rev. Food Sci. Technol. 2014, 5, 351–372. [Google Scholar] [CrossRef] [PubMed]
- Some Naturally Occurring Substances: Food Items and Constituents, Heterocyclic Aromatic Amines and Mycotoxins. IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. 1996, Volume 56. Available online: https://monographs.iarc.fr/ENG/Monographs/vol56/mono56.pdf (accessed on 12 December 2017).
- Wild, C.P.; Gong, Y.Y. Mycotoxins and human disease: A largely ignored global health issue. Carcinogenesis 2010, 31, 71–82. [Google Scholar] [CrossRef] [PubMed]
- Marroquín-Cardona, A.G.; Johnson, N.M.; Phillips, T.D.; Hayes, A.W. Mycotoxins in a changing global environment—A review. Food Chem. Toxicol. 2014, 69, 220–230. [Google Scholar] [CrossRef] [PubMed]
- Warth, B.; Braun, D.; Ezekiel, C.N.; Turner, P.C.; Degen, G.H.; Marko, D. Biomonitoring of Mycotoxins in Human Breast Milk: Current State and Future Perspectives. Chem. Res. Toxicol. 2016, 29, 1087–1097. [Google Scholar] [CrossRef] [PubMed]
- Zhou, M.; Yang, L.; Shao, M.; Wang, Y.; Yang, W.; Huang, L.; Zhou, X.; Jiang, S.; Yang, Z. Effects of Zearalenone Exposure on the TGF-β1/Smad3 Signaling Pathway and the Expression of Proliferation or Apoptosis Related Genes of Post-Weaning Gilts. Toxins 2018, 10, E49. [Google Scholar] [CrossRef] [PubMed]
- Massart, F.; Micillo, F.; Rivezzi, G.; Perrone, L.; Baggiani, A.; Miccoli, M.; Meucci, V. Zearalenone screening of human breast milk from the Naples area. Toxicol. Environ. Chem. 2016, 98, 128–136. [Google Scholar] [CrossRef]
- Assessment of Dietary Intake of Ochratoxin A by the Population of EU Member States. Reports on Tasks for Scientific Cooperation. EU Directorate General Health and Consumer Protection. SCOOP Task 3.2.7. 2002. Available online: https://ec.europa.eu/food/sites/food/files/safety/docs/cs_contaminants_catalogue_patulin_3.2.8_en.pdf (accessed on 17 December 2017).
- Ariño, A.; Herrera, M.; Juan, T.; Estopañan, G.; Carramiñana, J.J.; Rota, C.; Herrera, A. Influence of agricultural practices on the contamination of maize by fumonisin mycotoxins. J. Food Prot. 2009, 72, 898–902. [Google Scholar] [CrossRef] [PubMed]
- Fasano, A.; Catassi, C. Clinical practice. Celiac disease. NEJM 2012, 367, 2419–2426. [Google Scholar] [CrossRef] [PubMed]
- Plugis, N.M.; Khosla, C. Therapeutic approaches for celiac disease. Best Pract. Res. Clin. Gastroenterol. 2015, 29, 503–521. [Google Scholar] [CrossRef] [PubMed]
- Caldas, E.D.; Silva, A.C.S. Mycotoxins in corn-based food products consumed in Brazil: An exposure assessment for fumonisins. J. Agric. Food Chem. 2007, 55, 7974–7980. [Google Scholar] [CrossRef] [PubMed]
- Silva, L.J.G.; Lino, C.M.; Pena, A.; Moltó, J.C. Occurrence of fumonisins B1 and B2 in Portuguese maize and maize-based foods intended for human consumption. Food Addit. Contam. 2007, 24, 381–390. [Google Scholar] [CrossRef] [PubMed]
- Dall’Asta, C.; Galaverna, G.; Mangia, M.; Sforza, S.; Dossena, A.; Marchelli, R. Free and bound fumonisins in gluten-free food products. Mol. Nutr. Food Res. 2009, 53, 492–499. [Google Scholar] [CrossRef] [PubMed]
- Dall’Asta, C.; Scarlato, A.P.; Galaverna, G.; Brighenti, F.; Pellegrini, N. Dietary exposure to fumonisins and evaluation of nutrient intake in a group of adult celiac patients on a gluten-free diet. Mol. Nutr. Food Res. 2012, 56, 632–640. [Google Scholar] [CrossRef] [PubMed]
- Cano-Sancho, G.; Sanchis, V.; Marín, S.; Ramos, A.J. Occurrence and exposure assessment of aflatoxins in Catalonia (Spain). Food Chem. Toxicol. 2013, 51, 188–193. [Google Scholar] [CrossRef] [PubMed]
- Brera, C.; Debegnach, F.; De Santis, B.; Di Ianni, S.; Gregori, E.; Neuhold, S.; Valitutti, F. Exposure assessment to mycotoxins in gluten-free diet for celiac patients. Food Chem. Toxicol. 2014, 69, 13–17. [Google Scholar] [CrossRef] [PubMed]
- Rubert, J.; León, N.; Sáez, C.; Martins, C.P.B.; Godul, M.; Yusà, V.; Manes, J.; Soriano, J.M.; Soler, C. Evaluation of mycotoxins and their metabolites in human breast milk using liquid chromatography coupled to high resolution mass spectrometry. Anal. Chim. Acta 2014, 820, 439–469. [Google Scholar] [CrossRef] [PubMed]
- Joint FAO/WHO Expert Committee on Food Additives (JECFA). Safety evaluation of certain mycotoxins in food. WHO Food Addit. Ser. 2001, 47, 103–279. [Google Scholar]
- Sanchis, V.; Balcells, X.; Torres, M.; Sala, N.; Vinas, I.; Canela, R. A survey of aflatoxins and aflatoxigenic Aspergillus flavus in corn-based products from the Spanish market. Microbiol. Res. 1995, 150, 437–440. [Google Scholar] [CrossRef]
- Hussein, H.S.; Brasel, J.M. Toxicity, metabolism, and impact of mycotoxins on humans and animals. Toxicology 2001, 167, 101–134. [Google Scholar] [CrossRef]
- Van De Kamer, J.H.; Weijers, H.A.; Dicke, W.K. Coeliac disease. An investigation into the injurious constituents of wheat in connection with their action on patients with coeliac disease. Acta Paediatr. 1953, 42, 223–231. [Google Scholar] [CrossRef] [PubMed]
- Singh, J.; Whelan, K. Limited availability and higher cost of gluten-free foods. J. Hum. Nutr. Diet. 2011, 24, 479–486. [Google Scholar] [CrossRef] [PubMed]
- Ishikawa, A.T.; Takabayashi-Yamashita, C.R.; Ono, E.Y.S.; Bagatin, A.K.; Rigobello, F.F.; Kawamura, O.; Hirooka, E.Y.; Itano, E.N. Exposure assessment of infants to aflatoxin M1 through consumption of breast milk and infant powdered milk in Brazil. Toxins 2016, 8, 246. [Google Scholar] [CrossRef] [PubMed]
- Tchana, A.N.; Moundipa, P.F.; Tchouanguep, F.M. Aflatoxin contamination in food and body fluids in relation to malnutrition and cancer status in Cameroon. Int. J. Environ. Res. Public Health 2010, 7, 178–188. [Google Scholar] [CrossRef] [PubMed]
- Polychronaki, N.; West, R.M.; Turner, P.C.; Amra, H.; Abdel-Wahhab, M.; Mykkänen, H.; El-Nezami, H. A longitudinal assessment of aflatoxin M1 excretion in breast milk of selected Egyptian mothers. Food Chem. Toxicol. 2007, 45, 1210–1215. [Google Scholar] [CrossRef] [PubMed]
- Sadeghia, N.; Oveisia, M.R.; Jannatb, B.; Hajimahmoodia, M.; Bonyania, H.; Jannatc, F. Incidence of aflatoxin M1 in human breast milk in Tehran, Iran. Food Control 2009, 20, 75–78. [Google Scholar] [CrossRef]
- Adejumo, O.; Atanda, O.; Raiola, A.; Somorin, Y.; Bandyopadhyay, R.; Ritieni, A. Correlation between aflatoxin M1 content of breast milk, dietary exposure to aflatoxin B1 and socioeconomic status of lactating mothers in Ogun State, Nigeria. Food Chem. Toxicol. 2013, 56, 171–177. [Google Scholar] [CrossRef] [PubMed]
- Atasever, M.; Yildirim, Y.; Atasever, M.; Tastekin, A. Assessment of aflatoxin M1 in maternal breast milk in Eastern Turkey. Food Chem. Toxicol. 2014, 66, 147–149. [Google Scholar] [CrossRef] [PubMed]
- El-Tras, W.F.; El-Kady, N.N.; Tayel, A.A. Infants exposure to aflatoxin M1 as a novel foodborne zoonosis. Food Chem. Toxicol. 2011, 49, 2816–2819. [Google Scholar] [CrossRef] [PubMed]
- Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein, and Amino Acids (Macronutrients); The National Academies Press: Washington, DC, USA, 2005. [Google Scholar]
- WHO Child Growth Standards. Available online: http://www.who.int/childgrowth/en (accessed on 21 December 2017).
- Oppe, T.E. Present Day Practice in Infant Feeding: Third Report of a Working Party of the Panel on Child Nutrition, Committee on Medical Aspects of Food Policy. In Report on Health and Social Subjects; Her Majesty’s Stationery Office: London, UK, 1988; Volume 32. [Google Scholar]
- Setting Maximum Levels for Certain Contaminants in Foodstuffs. Off. J. Eur. Union 2006, 364–365. Available online: https://www.fsai.ie/uploadedFiles/Consol_Reg1881_2006.pdf (accessed on 21 December 2017).
- Sahindokuyucu Kocasari, F. Occurrence of aflatoxin M1 in UHT milk and infant formula samples consumed in Burdur, Turkey. Environ. Monit. Assess. 2014, 186, 6363–6368. [Google Scholar] [CrossRef] [PubMed]
- Er, B.; Demirhan, B.; Yentür, G. Short communication: Investigation of aflatoxin M1 levels in infant follow-on milks and infant formulas sold in the markets of Ankara, Turkey. J. Dairy Sci. 2014, 97, 3328–3331. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Arranz, E.; Navarro-Blasco, I. Aflatoxin M1 in Spanish infant formulae: Occurrence and dietary intake regarding type, protein-base and physical state. Food Addit. Contam. Part B Surveill. 2010, 3, 193–199. [Google Scholar] [CrossRef] [PubMed]
- Galvano, F.; Galofaro, V.; Ritieni, A.; Bognanno, M.; De Angelis, A.; Galvano, G. Survey of the occurrence of aflatoxin M1 in dairy products marketed in Italy: Second year of observation. Food Addit. Contam. 2001, 18, 644–646. [Google Scholar] [CrossRef] [PubMed]
- Meucci, V.; Razzuoli, E.; Soldani, G.; Massart, F. Mycotoxin detection in infant formula milks in Italy. Food Addit. Contam. Part A 2010, 27, 64–71. [Google Scholar] [CrossRef] [PubMed]
- Galvano, F.; Pietri, A.; Bertuzzi, T.; Gagliardi, L.; Ciotti, S.; Luisi, S.; Bognanno, M.; La Fauci, L.; Iacopino, A.M.; Nigro, F.; et al. Maternal dietary habits and mycotoxin occurrence in human mature milk. Mol. Nutr. Food Res. 2008, 52, 496–501. [Google Scholar] [CrossRef] [PubMed]
| Celiac Disease (CD) Mothers | Control Mothers | |
|---|---|---|
| Maternal age | 31.6 years (±6.4 years) | 33.1 years (±8.5 years) |
| Maternal weight | 66.1 kg (±11.4 kg) | 61.7 kg (±16.5 kg) |
| Children age | 1.5 months (±0.8 months) | 1.9 months (±1.0 months) |
| Children weight | 4.8 kg (±1.3 kg) | 5.3 kg (±0.7 kg) |
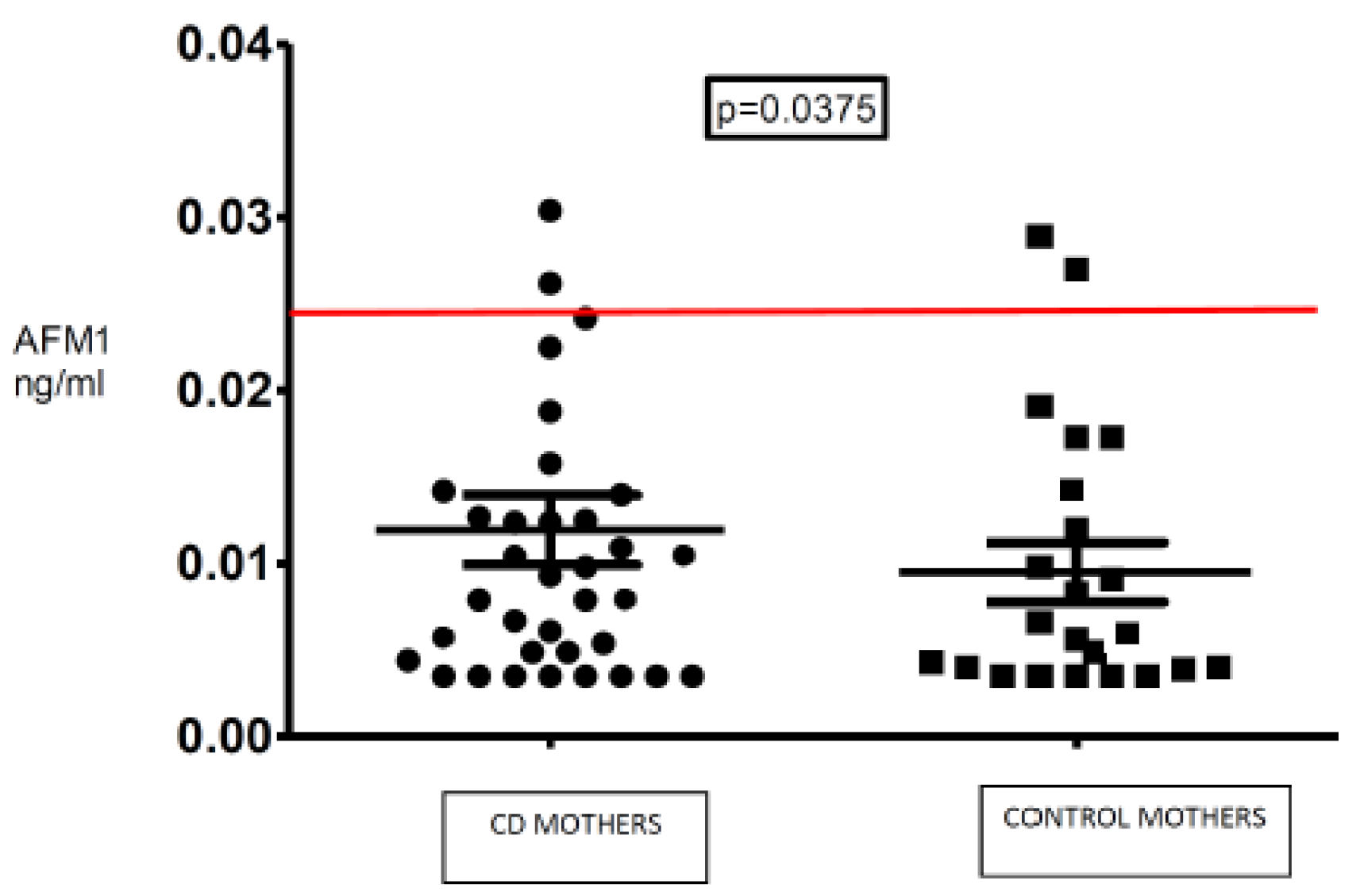
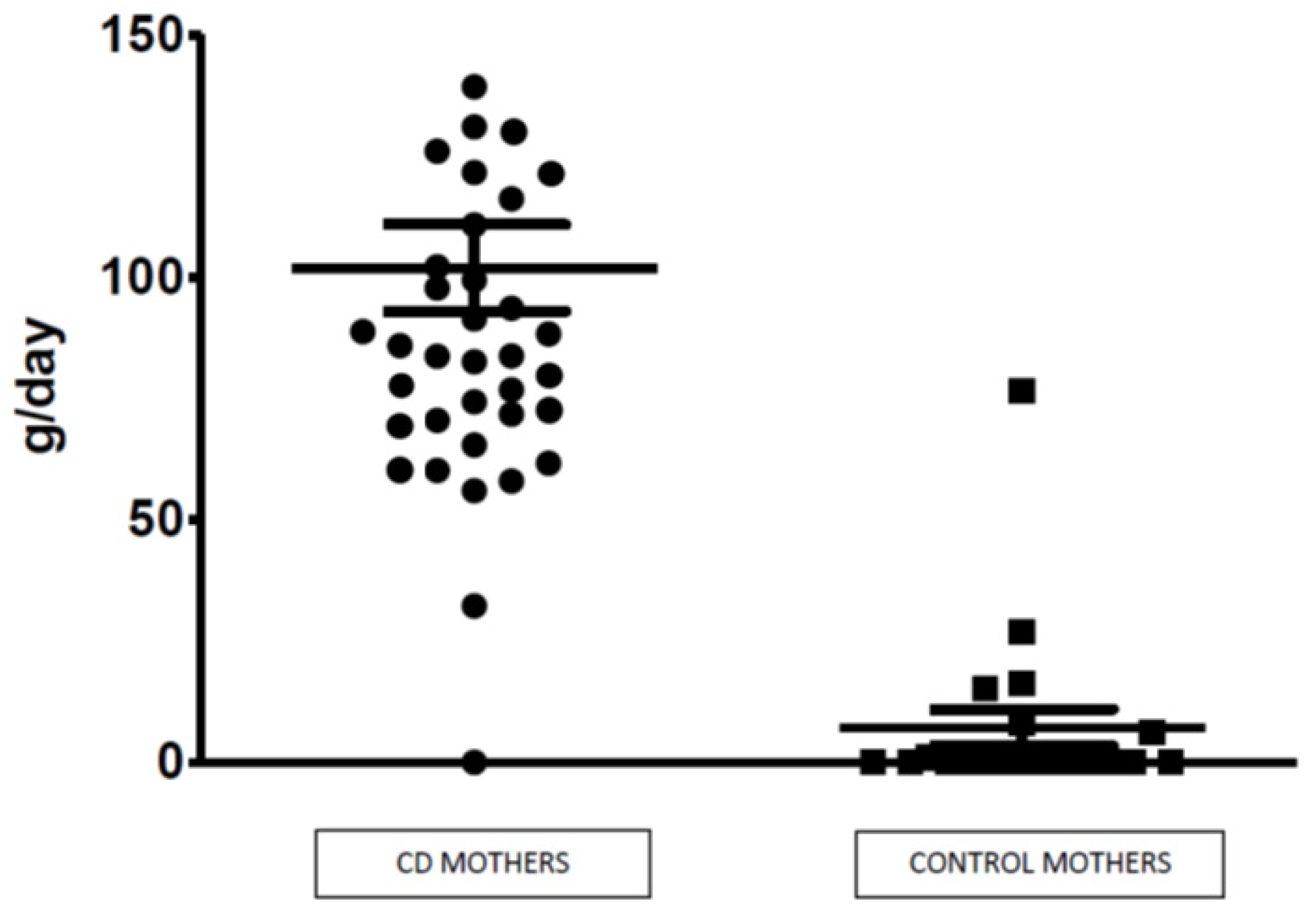
| AFM1 | ZEA | OTA | |
|---|---|---|---|
| CD mothers—n of sample positives (%) | 104 (37%) | 12 (4%) | 6 (2%) |
| Mean (ng/mL) | 0.012 | 2.1 | NA |
| Median (ng/mL) | 0.010 | 2.9 | NA |
| Range (ng/mL) | 0.003–0.340 | 2.0–17 | 0.017–0.123 |
| Controls—n of sample positives (%) | 43 (24%) | 15 (8%) | 1 (0.5%) |
| Mean (ng/mL) | 0.009 | 2.7 | NA |
| Median (ng/mL) | 0.005 | 2.2 | NA |
| Range (ng/mL) | 0.003–0.067 | 2.0–22 | 0.017–0.056 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Valitutti, F.; De Santis, B.; Trovato, C.M.; Montuori, M.; Gatti, S.; Oliva, S.; Brera, C.; Catassi, C. Assessment of Mycotoxin Exposure in Breastfeeding Mothers with Celiac Disease. Nutrients 2018, 10, 336. https://doi.org/10.3390/nu10030336
Valitutti F, De Santis B, Trovato CM, Montuori M, Gatti S, Oliva S, Brera C, Catassi C. Assessment of Mycotoxin Exposure in Breastfeeding Mothers with Celiac Disease. Nutrients. 2018; 10(3):336. https://doi.org/10.3390/nu10030336
Chicago/Turabian StyleValitutti, Francesco, Barbara De Santis, Chiara Maria Trovato, Monica Montuori, Simona Gatti, Salvatore Oliva, Carlo Brera, and Carlo Catassi. 2018. "Assessment of Mycotoxin Exposure in Breastfeeding Mothers with Celiac Disease" Nutrients 10, no. 3: 336. https://doi.org/10.3390/nu10030336
APA StyleValitutti, F., De Santis, B., Trovato, C. M., Montuori, M., Gatti, S., Oliva, S., Brera, C., & Catassi, C. (2018). Assessment of Mycotoxin Exposure in Breastfeeding Mothers with Celiac Disease. Nutrients, 10(3), 336. https://doi.org/10.3390/nu10030336








