Compliance with Dietary Guidelines Varies by Weight Status: A Cross-Sectional Study of Australian Adults
Abstract
:1. Introduction
2. Materials and Methods
2.1. CSIRO Healthy Diet Score Survey
2.2. Data Collection and Preparation
2.3. Statistical Analysis
3. Results
3.1. Variation in Diet Score by Weight Status
3.2. Likelihood of Overweight and Obesity by Diet Score Quintile
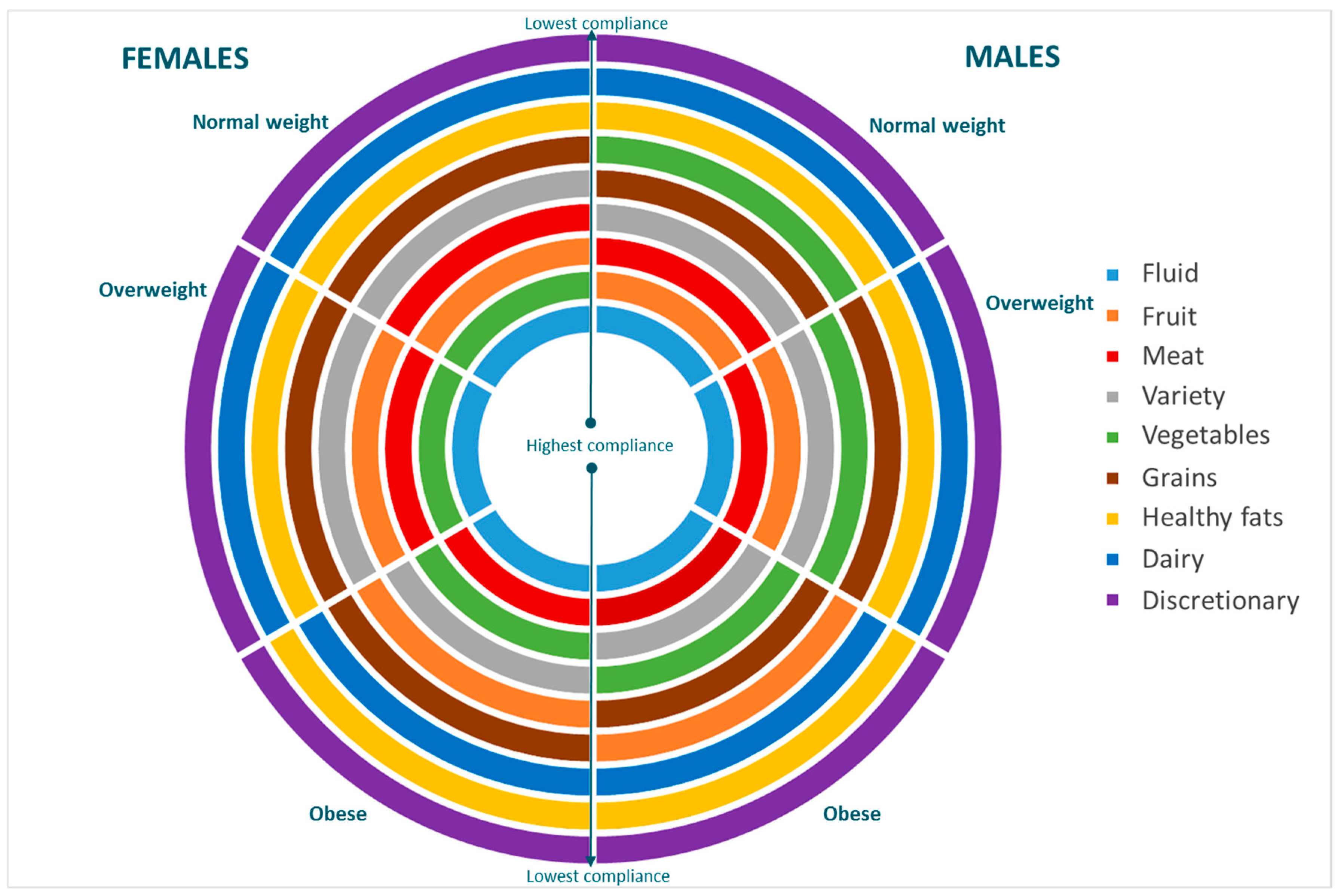
3.3. Rank Order of Components of Diet Quality
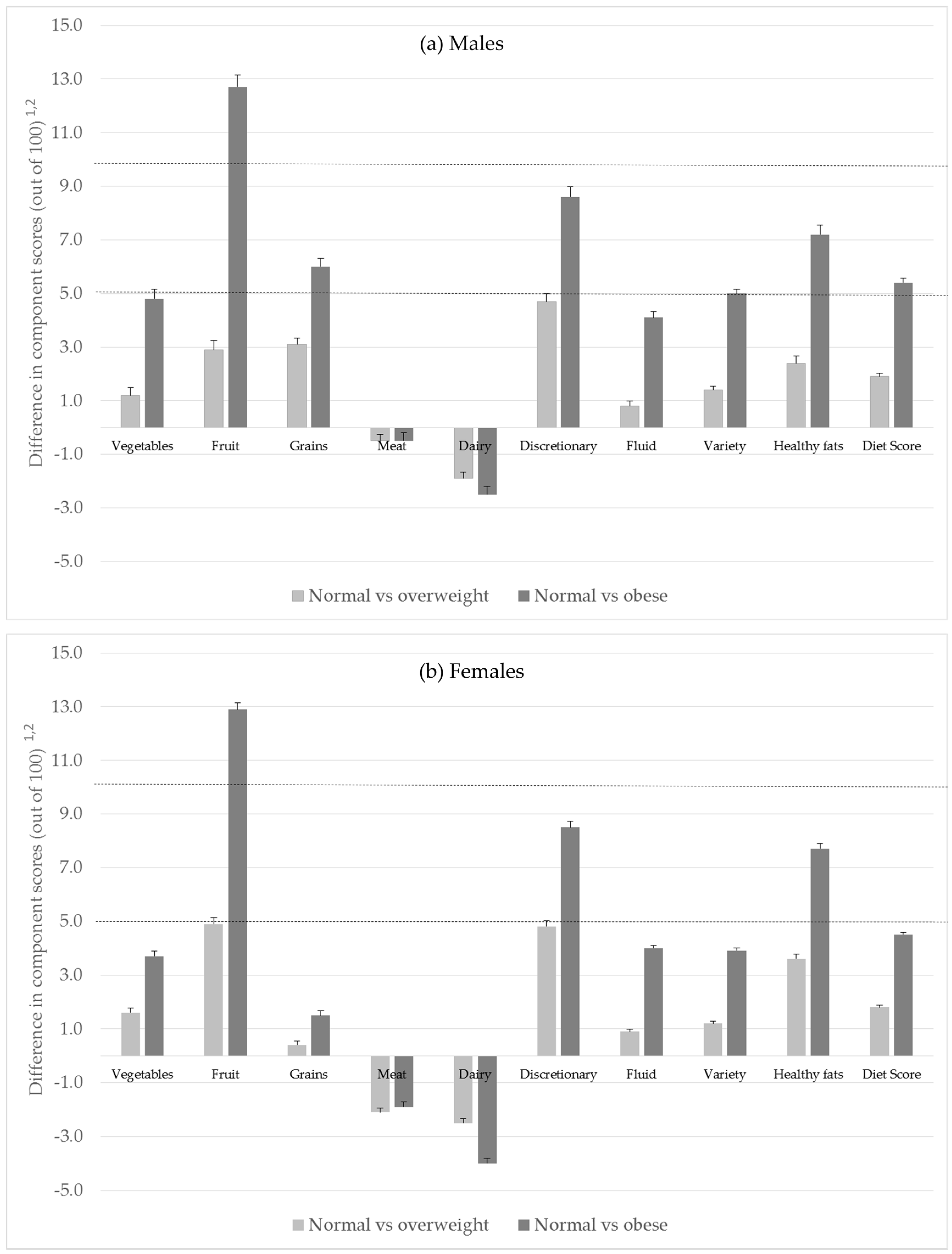
3.4. Differences in Diet Quality Compliance Scores by Weight Status and Gender
4. Discussion
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- World Health Organization (WHO). Diet, Nutrition and the Prevention of Chronic Diseases. Report of a Joint Food and Agriculture Organization/Who Expert Consultation; Who Technical Report Series 916; World Health Organization (WHO): Geneva, Switzerland, 2003. [Google Scholar]
- NCD Risk Factor Collaboration (NCD-RisC). Trends in adult body-mass index in 200 countries from 1975 to 2014: A pooled analysis of 1698 population-based measurement studies with 19.2 million participants. Lancet 2016, 387, 1377–1396. [Google Scholar]
- Ogden, C.L.; Carroll, M.D.; Fryar, C.D.; Flegal, K.M. Prevalence of Obesity among Adults and Youth: United States, 2011–2014; U.S. Department of Health and Human Services: Washington, DC, USA, 2015.
- Australian Bureau of Statistics. Australian Health Survey: Nutrition First Results—Foods and Nutrients, 2011–-12; 4364.0.55.007; Australian Bureau of Statistics: Canberra, Australia, 2013.
- World Health Organization. Global Action Plan for the Prevention and Control of Noncommunicable Disease 2013–2020; World Health Organization: Geneva, Switzerland, 2013. [Google Scholar]
- Togo, P.; Osler, M.; Sorense, T.I.A.; Heitmann, B.L. Food intake patterns and body mass index in observational studies. Int. J. Obes. 2001, 25, 1741–1751. [Google Scholar] [CrossRef] [PubMed]
- Moeller, S.M.; Reedy, J.; Millen, A.E.; Dixon, L.B.; Newby, P.K.; Tucker, K.L. Dietary patterns: Challenges and opportunitites in dietary patterns research an experimental biology workshop. J. Am. Diet. Assoc. 2006, 107, 1233–1239. [Google Scholar] [CrossRef] [PubMed]
- Newby, P.K. Examining energy density: Comments on diet quality, dietary advice, and the cost of healthful eating. J. Am. Diet. Assoc. 2006, 106, 1166–1169. [Google Scholar] [CrossRef] [PubMed]
- Asghari, G.; Mirmiran, P.; Yuzbashian, E.; Azizi, F. A systematic review of diet quality indices in relation to obesity. Br. J. Nutr. 2017, 117, 1055–1065. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.; Haines, P.S.; Seiga-Riz, A.M.; Popkin, B.M. The diet quality index-international (DQI-I) provides an effective tool for cross-national comparison of diet quality as illustrated by China and the United States. J. Nutr. 2003, 133, 3476–3484. [Google Scholar] [CrossRef] [PubMed]
- Kennedy, E.T.; Ohls, J.; Carlson, S.; Fleming, K. The Healthy Eating Index: Design and applications. J. Am. Diet. Assoc. 1995, 95, 1103–1108. [Google Scholar] [CrossRef]
- Kant, A.K. Indexes of overall diet quality: A review. J. Am. Diet. Assoc. 1996, 96, 785–791. [Google Scholar] [CrossRef]
- McNaughton, S.A.; Ball, K.; Crawford, D.; Mishra, G.D. An index of diet and eating patterns is a valid measure of diet quality in an australian population. J. Nutr. 2008, 138, 86–93. [Google Scholar] [CrossRef] [PubMed]
- Arabshahi, S.; Lahmann, P.H.; Williams, G.M.; Marks, G.C.; van der Pols, J.C. Longitudinal change in diet quality in australian adults varies by demographic, socio-economic, and lifestyle characteristics. J. Nutr. 2011, 141, 1871–1879. [Google Scholar] [CrossRef] [PubMed]
- Livingstone, K.M.; McNaughton, S.A. Diet quality is associated with obesity and hypertension in Australian adults: A cross sectional study. BMC Public Health 2016, 16, 1037. [Google Scholar] [CrossRef] [PubMed]
- Thorpe, M.G.; Milte, C.M.; Crawford, D.; McNaughton, S.A. A revised australian dietary guideline index and its association with key sociodemographic factors, health behaviors and body mass index in peri-retirement aged adults. Nutrients 2016, 8, 160. [Google Scholar] [CrossRef] [PubMed]
- Hendrie, G.A.; Baird, D.; Golley, R.K.; Noakes, M. The csiro healthy diet score: An online survey to estimate compliance with the australian dietary guidelines. Nutrients 2017, 9, 47. [Google Scholar] [CrossRef] [PubMed]
- Hendrie, G.A.; Rebuli, M.; Golley, R.K. Reliability and relative validity of a diet index score for adults derived from a self-reported short food survey. Nutr. Diet. 2017, 74, 291–297. [Google Scholar] [CrossRef] [PubMed]
- National Health & Medical Research Council; Department of Health and Ageing. Eat for Health. Australian Dietary Guidelines: Summary; Commonwealth of Australia: Canberra, Australia, 2013.
- Golley, R.K.; Hendrie, G.A.; McNaughton, S.A. Scores on the dietary guideline index for children and adolescents are associated with nutrient intake and socio-economic position but not adiposity. J. Nutr. 2011, 141, 1340–1347. [Google Scholar] [CrossRef] [PubMed]
- Hendrie, G.A.; Viner-Smith, B.; Golley, R.K. The reliability and relative validity of a diet index score for 4-11 year old children derived from a parent reported short food survey. Public Health Nutr. 2013, 17, 1486–1497. [Google Scholar] [CrossRef] [PubMed]
- Australian Bureau of Statistics. 2016 Census; Australian Bureau of Statistics: Canberra, Australia, 2016.
- Tapsell, L.C.; Neale, E.P.; Satija, A.; Hu, F.B. Foods, nutrients, and dietary patterns: Interconnections and implications for dietary guidelines. Adv. Nutr. 2016, 7, 445–454. [Google Scholar] [CrossRef] [PubMed]
- World Cancer Research Fund International. Cancer Prevention & Survival. Summary of Golbal Evidence on Diet, Weight, Physical Activity & What Increases or Decreases Your Risk of Cancer; World Cancer Research Fund International: London, UK, 2016. [Google Scholar]
- Salehi-Abargouei, A.; Akbari, F.; Bellissimo, N.; Azadbakht, L. Dietary diversity score and obesity: A systematic review and meta-analysis of observational studies. Eur. J. Clin. Nutr. 2016, 70, 1–9. [Google Scholar] [CrossRef] [PubMed]
- He, F.J.; Nowson, C.A.; Lucas, M.; MacGregor, G.A. Increased consumption of fruit and vegetables is related to a reduced risk of coronary heart disease: Meta-analysis of cohort studies. J. Hum. Hypertens. 2007, 21, 717–728. [Google Scholar] [CrossRef] [PubMed]
- Liu, S.; Manson, J.E.; Lee, I.-M.; Cole, S.R.; Hennekens, C.H.; Willet, W.C.; Buring, J.E. Fruit and vegetable intake and risk of cardiovascular disease: The women’s health study. Am. J. Clin. Nutr. 2000, 72, 922–928. [Google Scholar] [PubMed]
- Boeing, H.; Bechthold, A.; Bub, A.; Ellinger, S.; Haller, D.; Kroke, A.; Leschik-Bonnet, E.; Müller, M.J.; Oberritter, H.; Schulze, M.; et al. Critical review: Vegetables and fruit in the prevention of chronic diseases. Eur. J. Nutr. 2012, 51, 637–663. [Google Scholar] [CrossRef] [PubMed]
- Seidell, J.C. Dietary fat and obesity: An epidemiologic perspective. Am. J. Clin. Nutr. 1998, 67, 546S–550S. [Google Scholar] [CrossRef] [PubMed]
- Barrett, M.A.; Humblet, O.; Hiatt, R.A.; Adler, N.E. Big data and disease prevention: From quantified self to quantified communities. Big Data 2013, 1, 168–175. [Google Scholar] [CrossRef] [PubMed]
- Stommel, M.; Schoenborn, C.A. Accuracy and usefulness of bmi measures based on self-reported weight and height: Findings from the NHANES & NHIS 2001–2006. BMC Public Health 2009, 9, 421. [Google Scholar]
- Johansson, G.; Wikman, A.; Ahren, A.M.; Hallmans, G.; Johansson, I. Underreporting of energy intake in repeated 24-hour recalls related to gender, age, weight status, day of interview, educational level, reported food intake, smoking habits and area of living. Public Health Nutr. 2001, 4, 919–927. [Google Scholar] [CrossRef] [PubMed]
- Macdiarmid, J.; Blundell, J. Assessing dietary intake: Who, what and why of under-reporting. Nutr. Res. Rev. 1998, 11, 231–253. [Google Scholar] [CrossRef] [PubMed]
- Briefel, R.R.; Sempos, C.T.; McDowell, M.A.; Chien, S.; Alaimo, K. Dietary methods research in the third national health and nutrition examination survey: Underreporting of energy intake. Am. J. Clin. Nutr. 1997, 65, 1203S–1209S. [Google Scholar] [CrossRef] [PubMed]
| Compliance Score out of 100 (Mean (Standard Deviation)) | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Male (n = 52,400) | Female (n = 133,551) | Total (n = 185,951) | |||||||
| Food Group | Normal (n = 22,101) | Overweight (n = 20,761) | Obese (n = 9538) | Normal (n = 70,410) | Overweight (n = 36,073) | Obese (n = 27,068) | Normal (n = 92,511) | Overweight (n = 56,834) | Obese (n = 36,606) |
| Vegetables | 64.4 (29.1) | 63.2 (29.4) | 59.8 (30.7) | 76.2 (26.7) | 75 (27.5) | 72.9 (28.5) | 71.2 (28.4) | 68.4 (29.2) | 67.2 (30.2) |
| Fruit | 70.7 (35.3) | 67.7 (36.2) | 58.2 (38.8) | 74.3 (33) | 70.5 (34.8) | 62.8 (37.3) | 72.8 (34) | 69 (35.6) | 60.8 (38) |
| Grains | 65.1 (24.7) | 62.3 (24.2) | 59.2 (25.2) | 63.3 (24.5) | 63.5 (25.1) | 62.6 (25.9) | 64.1 (24.6) | 62.9 (24.6) | 61.1 (25.6) |
| Meat | 68.7 (26.1) | 69.0 (25.8) | 69.3 (26.1) | 72.3 (25.2) | 74.4 (24.4) | 74.2 (24.4) | 70.8 (25.7) | 71.4 (25.3) | 72 (25.3) |
| Dairy | 46.5 (24.8) | 48.3 (25.5) | 48.7 (26) | 46.7 (26) | 49.1 (26.2) | 50.5 (26.6) | 46.7 (25.5) | 48.7 (25.8) | 49.7 (26.3) |
| Discretionary | 29.5 (32.1) | 24.7 (30.6) | 20.9 (29.4) | 35.1 (32.7) | 30.6 (32) | 26.8 (31.6) | 32.7 (32.5) | 27.3 (31.3) | 24.2 (30.8) |
| Fluid | 90.1 (16.6) | 89.1 (18) | 86.1 (21.5) | 94.9 (11.7) | 94.2 (13.1) | 91.3 (17.2) | 92.8 (14.2) | 91.4 (16.2) | 89.1 (19.4) |
| Variety | 66.3 (13) | 64.9 (12.9) | 61.4 (14) | 67.1 (12.3) | 66.1 (12.7) | 63.4 (13.6) | 66.7 (12.6) | 65.5 (12.8) | 62.5 (13.8) |
| Healthy fats | 53.1 (29.1) | 50.7 (28) | 46 (27.8) | 56 (26.8) | 52.6 (25.6) | 48.7 (25.2) | 54.7 (27.8) | 51.5 (27) | 47.5 (26.4) |
| Diet Score | 58.4 (13.1) | 56.5 (12.6) | 53.1 (13.2) | 62.1 (12.2) | 60.7 (12.3) | 58 (13) | 60.5 (12.8) | 58.3 (12.7) | 55.8 (13.3) |
| Diet Score | |||||
|---|---|---|---|---|---|
| Variable | Q1 (Lowest) | Q2 | Q3 | Q4 | Q5 (Highest) |
| Cases | (n = 36,525) | (n = 37,134) | (n = 37,437) | (n = 37,494) | (n = 37,068) |
| Diet score (out of 100) | |||||
| Mean | 40.3 | 52.1 | 59.1 | 66.0 | 76.7 |
| Range | 3.7–47.8 | 47.9–55.7 | 55.8–62.3 | 62.4–69.9 | 70.0–99.0 |
| Obese | |||||
| Crude odds ratio | 2.19 (2.11, 2.27) | 1.60 (1.54, 1.66) | 1.30 (1.25, 1.35) | 1.16 (1.12, 1.21) | 1.0 |
| Adjusted model1 | 2.99 (2.88, 3.11) | 1.91 (1.84, 1.99) | 1.45 (1.39, 1.50) | 1.22 (1.17, 1.27) | 1.0 |
| Overweight or obese | |||||
| Crude odds ratio | 2.01 (1.95, 2.07) | 1.58 (1.54, 1.63) | 1.38 (1.34, 1.42) | 1.23 (1.19, 1.26) | 1.0 |
| Adjusted model1 | 2.64 (2.56,2.73) | 1.85 (1.80, 1.91) | 1.52 (1.47, 1.56) | 1.28 (1.24, 1.32) | 1.0 |
| Compliance Score Out of 100 (Mean (Standard Deviation)) | ||||||
|---|---|---|---|---|---|---|
| Male (n = 52,400) | Female (n = 133,551) | Total (n = 185,951) | ||||
| Food Group | Normal vs. Overweight | Normal vs. Obese | Normal vs. Overweight | Normal vs. Obese | Normal vs. Overweight | Normal vs. Obese |
| Vegetables | 1.2 * (0.5:2.0) | 4.8 * (3.8:5.8) | 1.6 * (1.1:2.0) | 3.7 (3.1:4.2) | 2.9 * (2.5:3.3) | 4.2 * (3.7:4.7) |
| Fruit | 2.9 * (2.0:3.9) | 12.7 * (11.5:13.9) | 4.9 * (4.3:5.5) | 12.9 (12.2:13.5) | 4.6 * (4.1:5.1) | 12.9 * (12.3:13.5) |
| Grains | 3.1 * (2.5:3.7) | 6.0 * (5.2:6.8) | 0.4 (0.0:0.8) | 1.5 * (1.0:2.0) | 1.0 * (0.6:1.3) | 2.6 * (2.2:3.0) |
| Meat | −0.5 (−1.2:0.1) | −0.5 (−1.3:0.3) | −2.1 * (−2.5:−1.7) | −1.9 * (−2.3:−1.4) | −1.2 * (−1.6:−0.9) | −1.5 * (−1.9:−1.0) |
| Dairy | −1.9 * (−2.5:−1.2) | −2.5 * (−3.4:−1.7) | −2.5 * (−3.0:−2.1) | −4.0 * (−4.5:−3.5) | −2.3 * (−2.7:−2.0) | −3.6 * (−4.0:−3.2) |
| Discretionary | 4.7 * (3.9:5.5) | 8.6 * (7.6:9.6) | 4.8 * (4.3:5.4) | 8.5 * (7.9:9.1) | 5.5 * (5.0:5.9) | 8.7 * (8.1:9.2) |
| Fluid | 0.8 * (0.4:1.3) | 4.1 * (3.5:4.7) | 0.9 * (0.6:1.1) | 4.0 * (3.7:4.2) | 1.4 * (1.2:1.7) | 4.1 * (3.8:4.3) |
| Variety | 1.4 * (1.0:1.7) | 5.0 * (4.5:5.4) | 1.2 * (1.0:1.4) | 3.9 * (3.7:4.2) | 1.3 * (1.1:1.5) | 4.2 * (4.0:4.4) |
| Healthy fats | 2.4 * (1.7:3.2) | 7.2 * (6.3:8.2) | 3.6 * (3.1:4.1) | 7.7 * (7.2:8.3) | 3.6 * (3.2:4) | 7.7 * (7.2:8.1) |
| Healthy Diet Score | 1.9 * (1.6:2.2) | 5.4 * (4.9:5.8) | 1.8 * (1.5:2.0) | 4.5 * (4.3:4.7) | 2.2 * (2:2.4) | 4.8 * (4.6:5.0) |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hendrie, G.A.; Golley, R.K.; Noakes, M. Compliance with Dietary Guidelines Varies by Weight Status: A Cross-Sectional Study of Australian Adults. Nutrients 2018, 10, 197. https://doi.org/10.3390/nu10020197
Hendrie GA, Golley RK, Noakes M. Compliance with Dietary Guidelines Varies by Weight Status: A Cross-Sectional Study of Australian Adults. Nutrients. 2018; 10(2):197. https://doi.org/10.3390/nu10020197
Chicago/Turabian StyleHendrie, Gilly A., Rebecca K. Golley, and Manny Noakes. 2018. "Compliance with Dietary Guidelines Varies by Weight Status: A Cross-Sectional Study of Australian Adults" Nutrients 10, no. 2: 197. https://doi.org/10.3390/nu10020197
APA StyleHendrie, G. A., Golley, R. K., & Noakes, M. (2018). Compliance with Dietary Guidelines Varies by Weight Status: A Cross-Sectional Study of Australian Adults. Nutrients, 10(2), 197. https://doi.org/10.3390/nu10020197






