The Relationship between Vegetable Intake and Weight Outcomes: A Systematic Review of Cohort Studies
Abstract
1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Eligibility Criteria
2.3. Study Selection
2.4. Data Extraction
2.5. Quality and Risk of Bias Assessment for Individual Studies
2.6. GRADE Assessment for Quality of Overall Body of Evidence
3. Results
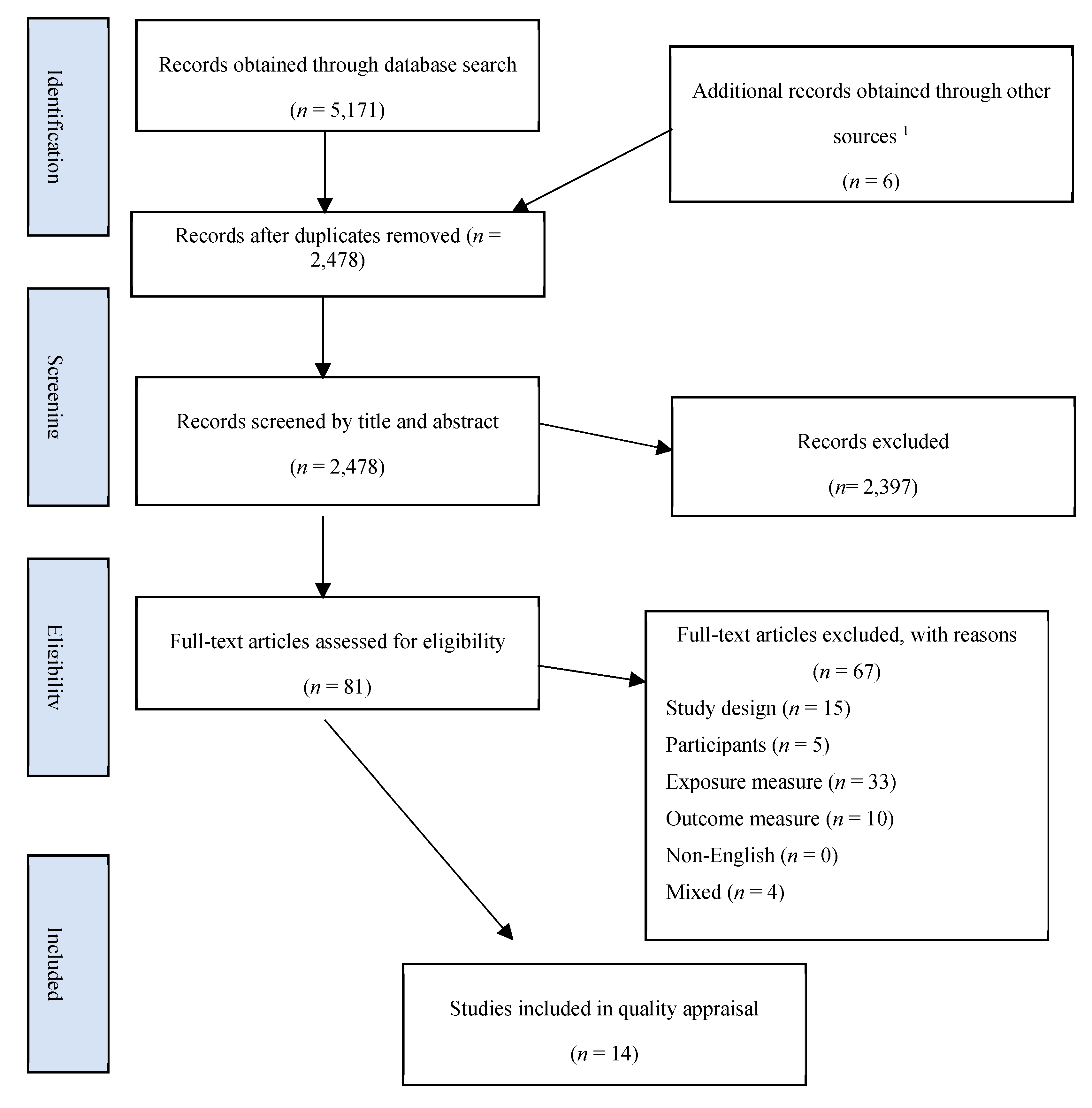
3.1. Study Selection
3.2. Quality and Risk of Bias Assessment Using the Joanna Briggs Institute (JBI) Critical Appraisal Checklist for Cohort Studies
3.3. Summary of Included Studies
3.4. Measurement of Exposure
3.5. Measurement of Outcome
3.6. Association between Vegetable Intake and Anthropometric Outcomes
3.7. Associations from Studies with Change in Vegetable Intake over Time
3.8. Associations from Studies with Baseline Vegetable Intake
3.9. Association from Excluded Studies
3.10. Grading of Recommendations Assessment, Development and Evaluation (GRADE) Assessment for Quality of Overall Body of Evidence
3.10.1. Study Limitations
3.10.2. Inconsistencies
3.10.3. Directness
3.10.4. Precision
3.10.5. Publication Bias
4. Discussion
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Ng, M.; Fleming, T.; Robinson, M.; Thomson, B.; Graetz, N.; Margono, C.; Mullany, E.C.; Biryukov, S.; Abbafati, C.; Abera, S.F. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2014, 384, 766–781. [Google Scholar] [CrossRef]
- Obesity and Overweight Fact Sheet, World Health Organization Media Centre. Available online: http://www.who.int/mediacentre/factsheets/fs311/en/ (accessed on 11 December 2017).
- Global Strategy on Diet, Physical Activity and Health, Promoting Fruit and Vegetable Consumption Around the World: Information Sheet. Available online: http://www.who.int/dietphysicalactivity/fruit/en/index2.html (accessed on 12 December 2017).
- Boeing, H.; Bechthold, A.; Bub, A.; Ellinger, S.; Haller, D.; Kroke, A.; Leschik-Bonnet, E.; Müller, M.J.; Oberritter, H.; Schulze, M. Critical review: Vegetables and fruit in the prevention of chronic diseases. Eur. J. Nut. 2012, 51, 637–663. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Ouyang, Y.; Liu, J.; Zhu, M.; Zhao, G.; Bao, W.; Hu, F.B. Fruit and vegetable consumption and mortality from all causes, cardiovascular disease, and cancer: Systematic review and dose-response meta-analysis of prospective cohort studies. BMJ 2014, 349, g4490. [Google Scholar] [CrossRef] [PubMed]
- NHS Choices Rough Guide: Fruit and Vegetable Portion Sizes. Available online: http://www.nhs.uk/livewell/5aday/documents/downloads/5aday_portion_guide.pdf (accessed on 25 September 2015).
- Office of Disease Prevention and Health Promotion. 2015–2020 Dietary Guidelines for Americans. Available online: https://health.gov/dietaryguidelines/2015/ (accessed on 11 December 2017).
- Australian Government: Department of Health. Australian Dietary Guidelines: National Health and Medical Research Council; NHMRC: Canberra, Australia, 2013. Available online: https://www.eatforhealth.gov.au/guidelines (accessed on 11 December 2017).
- Ruel, G.; Shi, Z.; Zhen, S.; Zuo, H.; Kröger, E.; Sirois, C.; Lévesque, J.-F.; Taylor, A.W. Association between nutrition and the evolution of multimorbidity: The importance of fruits and vegetables and whole grain products. Clin. Nutr. 2014, 33, 513–520. [Google Scholar] [CrossRef] [PubMed]
- Vos, T.; Barber, R.M.; Bell, B.; Bertozzi-Villa, A.; Biryukov, S.; Bolliger, I.; Charlson, F.; Davis, A.; Degenhardt, L.; Dicker, D. Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990–2013: A systematic analysis for the Global Burden of Disease Study 2013. Lancet 2015, 386, 743–800. [Google Scholar] [CrossRef]
- World Health Organization. Diet, Nutrition and the Prevention of Chronic Diseases: Report of a Joint WHO/FAO Expert Consultation; World Health Organization: Geneva, Switzerland, 2003. [Google Scholar]
- Recommendations and Public Health and Policy Implications 2018: World Cancer Research Fund and American Institute for Cancer Research. Continuous Update Project: Analysing Research on Cancer Prevention and Survival. Available online: https://www.wcrf.org/sites/default/files/Cancer-Prevention-Recommendations-2018.pdf (accessed on 19 October 2018).
- Lock, K.; Pomerleau, J.; Causer, L.; Altmann, D.R.; McKee, M. The global burden of disease attributable to low consumption of fruit and vegetables: Implications for the global strategy on diet. Bull. World Health Organ. 2005, 83, 100. [Google Scholar] [PubMed]
- Howarth, N.C.; Saltzman, E.; Roberts, S.B. Dietary fiber and weight regulation. Nutr. Rev. 2001, 59, 129–139. [Google Scholar] [CrossRef] [PubMed]
- Rolls, B.J. The relationship between dietary energy density and energy intake. Physiology & Behavior 2009, 97, 609–615. [Google Scholar] [CrossRef]
- Pomerleau, J.; Lock, K.; Knai, C.; McKee, M. Effectiveness of Interventions and Programmes Promoting Fruit and Vegetable Intake; WHO: Geneva, Switzerland, 2005. [Google Scholar]
- Rolls, B.J.; Ello-Martin, J.A.; Tohill, B.C. What can intervention studies tell us about the relationship between fruit and vegetable consumption and weight management? Nutr. Rev. 2004, 62, 1–17. [Google Scholar] [CrossRef] [PubMed]
- Mytton, O.T.; Nnoaham, K.; Eyles, H.; Scarborough, P.; Ni Mhurchu, C. Systematic review and meta-analysis of the effect of increased vegetable and fruit consumption on body weight and energy intake. BMC Public Health 2014, 14, 886. [Google Scholar] [CrossRef] [PubMed]
- Kaiser, K.A.; Brown, A.W.; Brown, M.M.B.; Shikany, J.M.; Mattes, R.D.; Allison, D.B. Increased fruit and vegetable intake has no discernible effect on weight loss: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2014, 100, 567–576. [Google Scholar] [CrossRef] [PubMed]
- Tapsell, L.C.; Dunning, A.; Warensjo, E.; Lyons-Wall, P.; Dehlsen, K. Effects of vegetable consumption on weight loss: A review of the evidence with implications for design of randomized controlled trials. Crit. Rev. Food Sci. Nutr. 2014, 54, 1529–1538. [Google Scholar] [CrossRef] [PubMed]
- Esposito, K.; Kastorini, C.-M.; Panagiotakos, D.B.; Giugliano, D. Mediterranean diet and weight loss: Meta-analysis of randomized controlled trials. Metab. Syndr. Relat. Disord. 2011, 9, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Buckland, G.; Bach, A.; Serra-Majem, L. Obesity and the Mediterranean diet: A systematic review of observational and intervention studies. Obes. Rev. 2008, 9, 582–593. [Google Scholar] [CrossRef] [PubMed]
- Soltani, S.; Shirani, F.; Chitsazi, M.J.; Salehi-Abargouei, A. The effect of dietary approaches to stop hypertension (DASH) diet on weight and body composition in adults: A systematic review and meta-analysis of randomized controlled clinical trials: Effect of DASH diet on weight and body composition. Obes. Rev. 2016, 17, 442–454. [Google Scholar] [CrossRef] [PubMed]
- Ledoux, T.A.; Hingle, M.D.; Baranowski, T. Relationship of fruit and vegetable intake with adiposity: A systematic review. Obes. Rev. 2011, 12, e143–e150. [Google Scholar] [CrossRef] [PubMed]
- Tohill, B.C.; Seymour, J.; Serdula, M.; Kettel-Khan, L.; Rolls, B.J. What Epidemiologic Studies Tell Us about the Relationship between Fruit and Vegetable Consumption and Body Weight. Nutr. Rev. 2004, 62, 365–374. [Google Scholar] [CrossRef] [PubMed]
- Moore, L.V.; Hamner, H.C.; Kim, S.A.; Dalenius, K. Common ways Americans are incorporating fruits and vegetables into their diet: Intake patterns by meal, source and form, National Health and Nutrition Examination Survey 2007–2010. Public Health Nutr. 2016, 19, 2535–2539. [Google Scholar] [CrossRef] [PubMed]
- Hebden, L.; O’Leary, F.; Rangan, A.; Singgih Lie, E.; Hirani, V.; Allman-Farinelli, M. Fruit consumption and adiposity status in adults: A systematic review of current evidence. Crit. Rev. Food Sci. Nutr. 2017, 57, 2526–2540. [Google Scholar] [CrossRef] [PubMed]
- Alinia, S.; Hels, O.; Tetens, I. The potential association between fruit intake and body weight—A review. Obes. Rev. 2009, 10, 639–647. [Google Scholar] [CrossRef] [PubMed]
- Schwingshackl, L.; Hoffmann, G.; Kalle-Uhlmann, T.; Arregui, M.; Buijsse, B.; Boeing, H. Fruit and vegetable consumption and changes in anthropometric variables in adult populations: A systematic review and meta-analysis of prospective cohort studies. PLoS ONE 2015, 10. [Google Scholar] [CrossRef] [PubMed]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. BMJ 2009, 339, 332–336. [Google Scholar] [CrossRef] [PubMed]
- Moola, S.; Munn, Z.; Sears, K.; Sfetcu, R.; Currie, M.; Lisy, K.; Tufanaru, C.; Qureshi, R.; Mattis, P.; Mu, P. Conducting systematic reviews of association (etiology): The Joanna Briggs Institute’s approach. Int. J. Evid. Based Healthc. 2015, 13, 163. [Google Scholar] [CrossRef] [PubMed]
- Atkins, D.; Best, D.; Briss, P.A.; Eccles, M.; Falck-Ytter, Y.; Flottorp, S.; Guyatt, G.H.; Harbour, R.T.; Haugh, M.C.; Henry, D. Grading quality of evidence and strength of recommendations. BMJ 2004, 328, 1490. [Google Scholar] [PubMed]
- Bertoia, M.L.; Mukamal, K.J.; Cahill, L.E.; Hou, T.; Ludwig, D.S.; Mozaffarian, D.; Willett, W.C.; Hu, F.B.; Rimm, E.B. Changes in Intake of Fruits and Vegetables and Weight Change in United States Men and Women Followed for Up to 24 Years: Analysis from Three Prospective Cohort Studies. PLoS Med. 2015, 12, e1001878. [Google Scholar] [CrossRef] [PubMed]
- Butler, S.M.; Black, D.R.; Blue, C.L.; Gretebeck, R.J. Change in diet, physical activity, and body weight in female college freshman. Am. J. Health Behav. 2004, 28, 24–32. [Google Scholar] [CrossRef] [PubMed]
- Esfahani, F.H.; Ejtahed, H.S.; Mirmiran, P.; Delshad, H.; Azizi, F. Alterations in food group intakes and subsequent weight changes in adults: Tehran lipid and glucose study. Int. J. Endocrinol. Metab. 2014, 12. [Google Scholar] [CrossRef]
- Halkjaer, J.; Tjonneland, A.; Overvad, K.; Sorensen, T.I.A. Dietary Predictors of 5-Year Changes in Waist Circumference. J. Am. Diet. Assoc. 2009, 109, 1356–1366. [Google Scholar] [CrossRef] [PubMed]
- He, K.; Hu, F.B.; Colditz, G.A.; Manson, J.E.; Willett, W.C.; Liu, S. Changes in intake of fruits and vegetables in relation to risk of obesity and weight gain among middle-aged women. Int. J. Obes. 2004, 28, 1569–1574. [Google Scholar] [CrossRef] [PubMed]
- Kahn, H.S.; Tatham, L.M.; Rodriguez, C.; Calle, E.E.; Thun, M.J.; Heath Jr, C.W. Stable behaviors associated with adults’ 10-year change in body mass index and likelihood of gain at the waist. Am. J. Public Health 1997, 87, 747–754. [Google Scholar] [CrossRef] [PubMed]
- Koenders, P.G.; Van Strien, T. Emotional eating, rather than lifestyle behavior, drives weight gain in a prospective study in 1562 employees. J. Occup. Environ. Med. 2011, 53, 1287–1293. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D.; Hao, T.; Rimm, E.B.; Willett, W.C.; Hu, F.B. Changes in Diet and Lifestyle and Long-Term Weight Gain in Women and Men. N. Engl. J. Med. 2011, 364, 2392–2404. [Google Scholar] [CrossRef] [PubMed]
- Quick, V.; Wall, M.; Larson, N.; Haines, J.; Neumark-Sztainer, D. Personal, behavioral and socio-environmental predictors of overweight incidence in young adults: 10-yr longitudinal findings. Int. J. Behav. Nutr. Phys. Act. 2013, 10. [Google Scholar] [CrossRef] [PubMed]
- Rautiainen, S.; Wang, L.; Lee, I.M.; Manson, J.E.; Buring, J.E.; Sesso, H.D. Higher intake of fruit, but not vegetables or fiber, at baseline is associated with lower risk of becoming overweight or obese inmiddle-aged and older women of normal BMI at baseline. J. Nutr. 2015, 145, 960–968. [Google Scholar] [CrossRef] [PubMed]
- Sawada, K.; Murayama, N.; Takemi, Y.; Ishida, H. Cohort study examining the association between vegetable consumption and weight gain in a single year among Japanese employees at a manufacturing company. Asia Pac. J. Clin. Nutr. 2015, 24, 633–638. [Google Scholar] [CrossRef] [PubMed]
- Vergnaud, A.C.; Norat, T.; Romaguera, D.; Mouw, T.; May, A.M.; Romieu, I.; Freisling, H.; Slimani, N.; Boutron-Ruault, M.C.; Clavel-Chapelon, F.; et al. Fruit and vegetable consumption and prospective weight change in participants of the European prospective investigation into cancer and nutrition-physical activity, nutrition, alcohol, cessation of smoking, eating out of home, and obesity study. Am. J. Clin. Nutr. 2012, 95, 184–193. [Google Scholar] [CrossRef] [PubMed]
- Vioque, J.; Weinbrenner, T.; Castelló, A.; Asensio, L.; de la Hera, M.G. Intake of Fruits and Vegetables in Relation to 10-year Weight Gain Among Spanish Adults. Obesity 2008, 16, 664–670. [Google Scholar] [CrossRef] [PubMed]
- Souza, L.G.; Jardim, T.V.; Rezende, A.C.; Sousa, A.L.L.; Moreira, H.G.; Perillo, N.B.; de Souza, S.G.; de Souza, W.K.S.B.; Araújo, Y.C.L.; Peixoto, M.d.R.G. Predictors of overweight/obesity in a Brazilian cohort after 13 years of follow-up. Nutr. J. 2018, 17, 10. [Google Scholar] [CrossRef] [PubMed]
- Rimm, E.B.; Giovannucci, E.L.; Stampfer, M.J.; Colditz, G.A.; Litin, L.B.; Willett, W.C. Reproducibility and validity of an expanded self-administered semiquantitative food frequency questionnaire among male health professionals. Am. J. Epidemiol. 1992, 135, 1114–1126. [Google Scholar] [CrossRef] [PubMed]
- Rimm, E.B.; Stampfer, M.J.; Colditz, G.A.; Chute, C.G.; Litin, L.B.; Willett, W.C. Validity of Self-Reported Waist and Hip Circumferences in Men and Women. Epidemiology 1990, 1, 466–473. [Google Scholar] [CrossRef] [PubMed]
- Block, G.; Hartman, A.M.; Dresser, C.M.; Carroll, M.D.; Gannon, J.; Gardner, L. A data-based approach to diet questionnaire design and testing. Am. J. Epidemiol. 1986, 124, 453–469. [Google Scholar] [CrossRef] [PubMed]
- Esfahani, F.H.; Asghari, G.; Mirmiran, P.; Azizi, F. Reproducibility and relative validity of food group intake in a food frequency questionnaire developed for the Tehran Lipid and Glucose Study. J. Epidemiol. 2010, 20, 150–158. [Google Scholar] [CrossRef] [PubMed]
- Tjønneland, A.O.K.; Haraldsdottir, J.; Bang, S.; Ewertz, M.; Jensen, O.M. Validation of a semiquantitative food frequency questionnaire developed in Denmark. Int. J. Epidemiol. 1991, 20, 906–912. [Google Scholar]
- Bigaard, J.; Spanggaard, I.; Thomsen, B.L.; Overvad, K.; Tjonneland, A. Self-reported and technician-measured waist circumferences differ in middle-aged men and women. J. Nutr. 2005, 135, 2263–2270. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.C.; Sampson, L.; Stampfer, M.J.; Rosner, B.; Bain, C.; Witschi, J.; Hennekens, C.H.; Speizer, F.E. Reproducibility and validity of a semiquantitative food frequency questionnaire. Am. J. Epidemiol. 1985, 122, 51–65. [Google Scholar] [CrossRef] [PubMed]
- Willett, W.; Stampfer, M.J.; Bain, C.; Lipnick, R.; Speizer, F.E.; Rosner, B.; Cramer, D.; Hennekens, C.H. Cigarette smoking, relative weight, and menopause. Am. J. Epidemiol. 1983, 117, 651–658. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B.; Satija, A.; Rimm, E.B.; Spiegelman, D.; Sampson, L.; Rosner, B.; Camargo, J.C.A.; Stampfer, M.; Willett, W.C. Diet Assessment Methods in the Nurses’ Health Studies and Contribution to Evidence-Based Nutritional Policies and Guidelines. Am J. Public Health 2016, 106, 1567–1572. [Google Scholar] [CrossRef] [PubMed]
- Hu, F.B.; Rimm, E.; Smith-Warner, S.A.; Feskanich, D.; Stampfer, M.J.; Ascherio, A.; Sampson, L.; Willett, W.C. Reproducibility and validity of dietary patterns assessed with a food-frequency questionnaire. Am. J. Clin. Nutr. 1999, 69, 243. [Google Scholar] [CrossRef] [PubMed]
- Coakley, E.H.; Rimm, E.B.; Colditz, G.; Kawachi, I.; Willett, W. Predictors of weight change in men: Results from The Health Professionals Follow-Up Study. Int. J. Obes. 1998, 22, 89–96. [Google Scholar] [CrossRef]
- Feskanich, D.; Rimm, E.B.; Giovannucci, E.L.; Colditz, G.A.; Stampfer, M.J.; Litin, L.B.; Willett, W.C. Reproducibility and validity of food intake measurements from a semiquantitative food frequency questionnaire. J. Am. Diet. Assoc. 1993, 93, 790–796. [Google Scholar] [CrossRef]
- Rockett, H.R.; Wolf, A.M.; Colditz, G.A. Development and reproducibility of a food frequency questionnaire to assess diets of older children and adolescents. J. Am. Diet. Assoc. 1995, 95, 336–340. [Google Scholar] [CrossRef]
- Himes, J.H.; Hannan, P.; Wall, M.; Neumark-Sztainer, D. Factors associated with errors in self-reports of stature, weight, and body mass index in Minnesota adolescents. Ann. Epidemiol. 2005, 15, 272–278. [Google Scholar] [CrossRef] [PubMed]
- Kobayashi, S.; Murakami, K.; Sasaki, S.; Okubo, H.; Hirota, N.; Notsu, A.; Fukui, M.; Date, C. Comparison of relative validity of food group intakes estimated by comprehensive and brief-type self-administered diet history questionnaires against 16 d dietary records in Japanese adults. Public Health Nutr. 2011, 14, 1200–1211. [Google Scholar] [CrossRef] [PubMed]
- Al-Delaimy, W.; Slimani, N.; Ferrari, P.; Key, T.; Spencer, E.; Johansson, I.; Johansson, G.; Mattisson, I.; Wirfalt, E.; Sieri, S. Plasma carotenoids as biomarkers of intake of fruits and vegetables: Ecological-level correlations in the European Prospective Investigation into Cancer and Nutrition (EPIC). Eur. J. Clin. Nutr. 2005, 59, 1397–1408. [Google Scholar] [CrossRef] [PubMed]
- Vioque, J.; Gonzalez, L. Validity of a food frequency questionnaire (preliminary results). Eur. J. Cancer Prev. 1991, 1, 19. [Google Scholar] [CrossRef]
- Tjonneland, A.; Olsen, A.; Boll, K.; Stripp, C.; Christensen, J.; Engholm, G.; Overvad, K. Study design, exposure variables, and socioeconomic determinants of participation in Diet, Cancer and Health: A population-based prospective cohort study of 57,053 men and women in Denmark. Scand. J. Public Health 2007, 35, 432–441. [Google Scholar] [CrossRef] [PubMed]
- Livingstone, M.B.E.; Robson, P.J.; Wallace, J.M.W. Issues in dietary intake assessment of children and adolescents. Br. J. Nutr. 2004, 92, S213–S222. [Google Scholar] [CrossRef]
- Ludwig, D.S. The glycemic index: Physiological mechanisms relating to obesity, diabetes, and cardiovascular disease. JAMA 2002, 287, 2414–2423. [Google Scholar] [CrossRef] [PubMed]
- Partridge, S.R.; McGeechan, K.; Bauman, A.; Phongsavan, P.; Allman-Farinelli, M. Improved eating behaviours mediate weight gain prevention of young adults: Moderation and mediation results of a randomised controlled trial of TXT2BFiT, mHealth program. Int. J. Behav. Nutr. Phys. Act. 2016, 13, 44. [Google Scholar] [CrossRef] [PubMed]
- Sartorelli, D.S.; Franco, L.J.; Cardoso, M.A. High intake of fruits and vegetables predicts weight loss in Brazilian overweight adults. Nutr. Res. 2008, 28, 233–238. [Google Scholar] [CrossRef] [PubMed]
- Arabshahi, S.; van der Pols, J.C.; Williams, G.M.; Marks, G.C.; Lahmann, P.H. Diet quality and change in anthropometric measures: 15-year longitudinal study in Australian adults. Br. J. Nutr. 2012, 107, 1376–1385. [Google Scholar] [CrossRef] [PubMed]
- Thiele, S.; Mensink, G.B.; Beitz, R. Determinants of diet quality. Public Health Nutr. 2004, 7, 29–37. [Google Scholar] [CrossRef] [PubMed]
- Hall, J.N.; Moore, S.; Harper, S.B.; Lynch, J.W. Global variability in fruit and vegetable consumption. Am. J. Prev. Med. 2009, 36, 402–409. [Google Scholar] [CrossRef] [PubMed]
| Search No. | Search Statement | No. of Citations Retrieved |
|---|---|---|
| 1 | ((((MESH MAJOR TOPIC: exp: (((((body weight) OR Body Weight Maintenance) OR Body Weight) OR Body Weight Changes) OR Weight Gain) OR Weight Loss) OR MESH MAJOR TOPIC: exp: (Obesity)) OR MESH MAJOR TOPIC: exp: (overweight)) OR TOPIC: (increase NEAR/2 weight)) OR TOPIC: (change NEAR/2 weight)) OR ((TOPIC: (maintenance NEAR/2 weight AND LANGUAGE: (English)) AND SPECIES: (Humans)) | 438,097 |
| 2 | (MESH MAJOR TOPIC: (vegetable *) AND LANGUAGE: (English)) AND SPECIES: (Humans)) | 3566 |
| 3 | (MESH MAJOR TOPIC: exp: (Cohort Studies OR Longitudinal Studies) AND LANGUAGE: (English)) AND SPECIES: (Humans)) | 1,428,860 |
| 4 | #3 AND #2 AND #1 | 39 |
| JBI Checklist no. Study | Joanna Briggs Institute Critical Appraisal Checklist for Cohort Studies | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Two Groups Similar and Recruited from the Same Population? | 2. Were the Exposures Measured Similarly to Assign People to Both Exposed and Unexposed Groups? | 3. Was the Exposure Measured in a Valid and Reliable Way? | 4. Were Confounding Factors Identified? | 5. Were Strategies to Deal with Confounding Factors Stated? | 6. Were the Groups/Participants Free of the Outcome at the Start of the Study (or at the Moment of Exposure)? | 7. Were the Outcomes Measured in a Valid and Reliable Way? | 8. Was the Follow-Up Time Reported and Sufficient to Be Long Enough for Outcomes to Occur? | 9. Was Follow-Up Complete, and If Not, Were the Reasons to Loss of Follow-Up Described and Explored? | 10. Were Strategies to Address Incomplete Follow-Up Utilized? | 11. Was Appropriate Statistical Analysis Used? | Overall * | |
| Bertoia et al., (2015) [33] | Y | Y | Y | Y | Y | N/A | Y | Y | Y | Y | Y | Include |
| Butler et al., (2004) [34] | U | Y | Y | N | N | N/A | Y | Y | N | Y | N | Exclude |
| Esfahani et al., (2014) [35] | Y | Y | Y | N!! | Y | N/A | Y | Y | Y | N | Y | Include |
| Halkjaer et al., (2009) [36] | Y | Y | N # | Y | Y | N/A | Y | Y | Y | N | Y | Include |
| He et al., (2004) [37] | Y | Y | Y | Y | Y | N/A | Y | Y | Y | N | Y | Include |
| Kahn et al., (1997) [38] | Y | Y | N | Y | Y | N/A | N | Y | Y | U | Y | Exclude |
| Koenders et al., (2011) [39] | Y | Y | N | N | N | N/A | N | Y | U | N | Y | Exclude |
| Mozaffarian et al., (2011) [40] | Y | Y | Y | Y | Y | N/A | Y | Y | Y | Y | Y | Include |
| Quick et al., (2013) [41] | Y | Y | Y | Y | Y | N/A | Y | Y | N | U | Y | Include |
| Rautiainen et al., (2015) [42] | Y | Y | N # | Y | Y | N/A | Y | Y | Y | U | Y | Include |
| Sawada et al., (2015) [43] | Y | Y | N # | Y | Y | N/A | Y | Y | Y | N | Y | Include |
| Souza et al., (2018) [46] | Y | Y | U # | N♦ | N♦ | N/A | Y | Y | Y | N | Y | Exclude |
| Vergnaud et al., (2012) [44] | Y | Y | N # | Y | Y | N/A | Y | Y | Y | N | Y | Include |
| Vioque et al., (2008) [45] | Y | Y | N ^ | Y | Y | N/A | Y | Y | N | U | Y | Include |
| Author | Dietary Assessment Method for Vegetables and Unit of Measure | Method for Assessing Anthropometric Variables |
|---|---|---|
| Bertoia M et al., 2015 [33] | Validated FFQ [47] servings/day | Self-reported weight (lb) and height, validated in a subsample of cohort (r = 0.97) [48] |
| Butler et al., (2004) [34] | Validated Block FFQ [49], servings/day | Measured by trained technicians using Detecto balance beam scales |
| Esfahani et al., 2014 [35] | Validated semi-quantitative FFQ [50], servings/day | Measured by trained technicians using digital scales |
| Halkjaer, et al., 2009 [36] | Validated FFQ [51] potatoes separated from vegetables, only assessed at baseline, food groups converted to kilocalories/day | Baseline waist circumference and weight measured by trained technicians. Follow-up was self-measured validated in a subsample of the cohort with some degree of over/underestimation found [52]. |
| He, et al., 2004 [37] | Validated FFQ [53], servings/day | Self-reported weight and height validated in subsample of cohort, (r = 0.96) [54] |
| Kahn et al., 1997 [38] | Self-report questionnaire 28 food items (6 vegetables) (non-validated), quintiles of intake | Self-reported weight and height (non-validated) |
| Koenders et al., (2011) [39] | Short question with three items (non-validated), g per day | Self-reported weight and height (non-validated) |
| Mozaffarian, D et al., 2011 [40] | Validated FFQs [55,56], vegetables and potatoes are separated, servings/day | Self-reported weight and height validated in subsample of cohort (r = 0.96) [48,57] |
| Quick, et al., 2013 [41] | Validated FFQ [58,59], servings/day | Self-reported height and weight, (male r = 0.88; female r = 0.85) [60]. |
| Rautiainen, S et al., 2015 [42] | Validated FFQ [53], only assessed at baseline, servings/day | Self-reported weight and height, validated in a subsample of the cohort (r = 0.95 males; r = 0.98 females) [48] |
| Sawada, et al., 2015 [43] | Validated BDHQ (brief-type self-administered diet history questionnaire) at baseline only [61], g/1000 kcal/day | Weight and height measured by trained technicians |
| Souza et al., (2018) [46] | Frequency of food intake questionnaire (non-validated), daily frequency of intake of vegetables | Weight and height were measured using standardized scales and stadiometer |
| Vergnaud, et al., 2012 [44] | Validated dietary questionnaire [62] with country-specific adaptations, only assessed at baseline, g/day | Weight and height were measured at the centres using standardized procedures # |
| Vioque, et al., 2008 [45] | Validated FFQ [63], g/day | Weight and height measured by trained technicians |
| Author, Year, Country, Cohort | Follow-up Period (in Years), Retention % | Size of Sample, Median/Mean Age at Baseline (in Years), Gender | Eligibility Criteria of Population Included in Results |
|---|---|---|---|
| Bertoia M et al., 2015 [33] USA Nurses’ Health Study (NHS), Health Professionals Follow-Up Study (HPFS), Nurses’ Health Study II (NHS II) | Results reported per 4 year interval with a total of 6 4-year time intervals in the NHS and HPFS (1986–2010, 24 years) & four 4-year time intervals in the NHS II (1991–2007, 16 years). NHS: >90% retention, NHS II: >90% retention, HPFS: 96% retention | NHS: 35,408 women (~48.7 years) HPFS: 17,996 men (~47 years) NHS II: 64,514 women (~36.4 years) | Exclusions: history of chronic disease at baseline, gastric bypass surgery, pregnancy (one 4-year interval only), aged over 65 years old, missing data, implausible energy intake. Censored individuals who developed these conditions during follow-up: at time of diagnosis for CVD and 6 years prior for all other diseases. |
| Butler et al., (2004) [34] USA Female College Freshman | 20 weeks Retention: 66% | N = 54, all women Mean age 17.79 years | Exclusions: None specified |
| Esfahani et al., 2014 [35] Iran Tehran Lipid and Glucose Study (TLGS) | Study used data from those measured after a 3 year time interval with baseline data collected between 2005–2008 and follow up between 2008–2011, 83% retention before exclusions | 851 adults Men: 378 (mean age 40.2 years) Women: 473 (mean age 38.6 years) | Exclusions: Those who were pregnant, had cancer, stroke, or consumed drugs affecting body weight. Those with no follow-up data, under- or over reporters and those with extreme changes in weight (> 5 kg/years). |
| Halkjaer et al., 2009 [36] Denmark Danish Diet, Cancer, and Health Study | 5.3 years (median) Retention: 83% [64] | 44,897 adults Women: 22,570 (median age 56 years) Men: 20,126 (median age 55 years) | Exclusions: those registered in the Danish Cancer Registry with a previous cancer diagnosis, those who were not aged 50–64 years, were not born in Denmark or living in the greater Copenhagen or Aarhus areas |
| He, K et al., 2004 [37] USA, NHS | 12 years >90% retention | 74063 females Mean age 50.7 years (38–63 years) | Exclusions: women with history of cardiovascular disease, cancer or diabetes; or who provided incomplete or implausible information. |
| Kahn et al., 1997 [38] USA Cancer Prevention Study II | 10 years Retention: N/A (baseline sample size not reported so retention could not be calculated) | 79,236 Women: 44,080 Men: 35,156 Mean age not reported | Exclusions: those more than 54 years old at baseline, very overweight (BMI ≥ 32 kg/m2) or very underweight (BMI < 18 kg/m2) or if they reported an extreme 10-year change in BMI (increase or decrease of greater than 8 kg/m2. Those reporting regular use of diuretics, have a cancer history other than nonmelanoma skin cancer, diabetes, or race/ethnicity other than White non-Hispanic |
| Koenders et al., (2011) [39] Netherlands Workers within large banking corporation | 2 years Retention: 52% | 1562 Women:599 Men:963 Mean age: 44.10 years | Exclusions: None reported. |
| Mozaffarian et al., 2011 [40] USA NHS, NHS II, HPFS | Data based on 20 years follow-up (1986–2006) in NHS, 12 years follow-up (1991–2003) in NHS II, and 20 years follow-up (1986–2006) in HPFS. NHS: >90% retention, NHS II: >90% retention, HPFS: 96% retention | NHS: 50,422 (all women) mean age 52.2 years NHS II: 47,898 (all women) mean age 37.5 years HPFS: 22,557 (all men) mean age 50.8 years | Exclusions: participants with obesity, diabetes, cancer, or cardiovascular, pulmonary, renal or liver disease at baseline; those with missing data; those with an implausible energy intake; those who were newly pregnant during follow-up; those over 65 years |
| Quick et al., 2013 [41] USA, Project EAT (eating and activity in teens and young adults) | 10 years 66.4% response rate | 2134 participants (1133 female, 1001 male) mean age 15 years at baseline, 25.4 years at follow-up | Exclusions: those with missing data, or pregnant at follow-up. |
| Rautiainen et al., 2015 [42] USA, Women’s Health Study (WHS) | Mean follow-up of 15.9 years Annual questionnaires, Retention: 85% | 18,146 women aged 45 or over mean age ~53.8 years | Exclusions: If diagnosed with CVD or cancer with an initial BMI less than 18.5 or greater than 25 kg/m2 |
| Sawada et al., 2015 [43] Japan, Food manufacturing employees | 1 year Retention N/A | 478 (mean age 36.9) Aged 19–60 years | Exclusions: participants who had not received an annual health check-up or who had complete data. |
| Souza et al., (2018) [46] Brazil Local residents from Firminópolis town in Brzail | 13.2 years Retention: 69% | 1167 individuals (430 men and 737 women) | Exclusions: At follow-up were if respondent moved to another city, not found at their homes, those refusing to participate, those with physical or mental incapacity or 10 incomplete data on weight and height. |
| Vergnaud et al., 2012 [44] Participants from 10 European countries European Prospective Investigation into Cancer and Nutrition study (EPIC) | 2–11 years Retention: 81% | 373,803 (103,455 men and 270,348 women) mean age 52.7 years | Exclusions: participants with chronic disease at baseline, who were pregnant, had missing information, or those in the lowest and highest 1% of the ratio of reported total energy intake: energy requirement |
| Vioque et al., 2008 [45] Spain | 10 years 51% response rate | 206 (89 men and 117 women) Mean age 41.52 years (15–80 years) | Exclusions: those with incomplete/missing data |
| Study Author, Year | Anthropometric Measure | Units of Vegetable Intake | Results | Summary of Direction of Change |
| Bertoia et al., ^ (2015) [33] | Weight loss (kg) | Per ↑ 1 vegetable serving/day | −0.1 kg per daily serving; 95% confidence intervals (CI) −0.35 to −0.14 Potatoes α +0.3 kg per daily serving; 95% CI 0.19 to 1.30 1 | Non-starchy veg = ↓ weight Potatoes = ↑ weight |
| Butler et al., (2004) [34] | Body weight (kg), BMI, Body Composition (% fat), Fat mass, Fat-free mass | Per ↓ 0.34 vegetable serving/day | per 0.34 ↓ in daily vegetable servings: Weight +0.72 kg (SD 0.14) BMI +0.27 kg/m2 (SD 0.02) % Fat +1.79 (0.24) Fat mass: +2.89 (0.38) Fat-free mass: −1.35 (0.53) p < 0.01 for all of above 2 | Decreased veg intake = ↑ in weight, Body Mass Index (BMI), % fat and fat mass |
| Esfahani et al., (2014) [35] | Odds ratio (OR) for weight loss (kg) | Per mean ↑ of 0.2 servings/day in men and 0.3 servings/day in women | Decreased vegetable intake compared to no change, reduced the likelihood of weight loss in women by 56% (OR: 0.44, 95% CI: 0.21−0.91). MEN: no significant associations. 3 | WOMEN: Decreased veg intake = ↓ likelihood of weight loss MEN: NS |
| He et al., (2004) [37] Women only | OR for risk of Obesity | Per ↑ by 1.2 vegetable servings/day | Q4 (1.2 servings) vs. Q1 (−1.72 servings) OR = 0.85; 95% CI 0.76 to 0.94(p trend 0.0002) 4 | ↓ risk obesity |
| OR for major weight gain (>25 kg) | Per ↑2.8 vegetable servings/day | Q5 (2.8 servings) vs. Q1 (−1.72 servings) OR = 0.76; 95% CI 0.59 to 0.99 (p trend 0.05) 4 | ↓ risk major weight gain >25 kg | |
| Kahn et al., 1997 [38] | Change in BMI | Lowest quintile intake compared to highest quintile | Men: −0.12 kg/m2 SE 0.05 (p = 0.012) Women: −0.12 kg/m2 SE 0.05 (p = 0.009) 5 | ↓ BMI by 0.12 kg/m2 |
| OR for weight gain at the waist | Men: OR: 0.81 95% CI 0.71, 0.93 Women: OR: 0.71 95% CI 0.59, 0.86 5 | ↓ risk weight gain at the waist | ||
| Koenders et al., (2011) [39] | Change in BMI | Unclear | −0.045 standard error (SE): 0.055 (p = 0.416) 6 | NS |
| Mozaffarian et al., ^ (2011) [40] | Weight loss (kg) | Per ↑ 1 vegetable serving/day | −0.09 kg per daily serving; 95% CI −0.34 to −0.11 Potatoes α +0.6 kg; 95% CI 0.87 to 1.70 (p < 0.001) 7 | Non-starchy veg = ↓ weight Potatoes = ↑ weight |
| Souza et al., (2018) [46] | Risk of new-onset overweight/obesity | Quartiles of mean daily frequency of intake | RESULTS NOT REPORTED, only p value (p = 0.850) 8 | NS |
| Quick et al., (2013) [41] | OR for risk of becoming overweight | Per ↑ 1 vegetable serving/day | MEN: OR = 0.88, 95% CI = 0.78 to 0.99 9 | MEN: ↓ risk overweight |
| WOMEN: no significant associations 9. | WOMEN: NS | |||
| Vioque et al., (2008) [45] | OR for weight gain (>3.4 kg) | Q4 (>333 g/day) vs. Q1 (<166 g/day) adjusted baseline intakes * | Q4 vs. Q1: OR: 0.18; 95% CI 0.05 to 0.66 (p trend 0.032) 10 | ↓ risk weight gain >3.4 kg |
| Measured Vegetable Intake at BASELINE ONLY | ||||
| Study Author, Year | Anthropometric Measure | Units of Vegetable Intake | Results | Summary of Direction of Change |
| Halkjaer et al., (2009) [36] | Waist circumference (WC) (cm) | Per 1 vegetable serving ** | WOMEN: −0.36 cm per veg serving/day (excluding potatoes) 95% CI −0.52 to −0.21, Potatoes 0.10 cm WC per serving potato/day # 95% CI: 0.006 to 0.19 11 | WOMEN: ↓ WC POTATOES: ↑ WC |
| MEN: no significant associations with WC 11 | MEN: NS | |||
| Rautiainen et al., (2015) [42] Women only | OR for overweight or obesity | Intake Quintile 1 (<2 servings/day) vs. Quintile 5(>5.4 servings per day) | No significant associations between vegetable intake and risk of becoming overweight or obese 12. | NS |
| Sawada et al., (2015) [43] | OR gaining >3 kg in 1 year | Intake Quartile 1(<57.2 g/1000 kcal) vs. Quartile 4 (>143.7 g/1000 kcal) | Q4 vs. Q1: OR = 0.27; 95% CI 0.08 to 0.99 (p trend 0.028) 13 | ↓ risk weight gain >3 kg in 1 year |
| Vergnaud et al., (2012) [44] | Weight loss (g) | Per ↑ vegetables by 100 g per day | MEN: −10 g; 95% CI −17 to −3; p = 0.007) (association disappeared with calibrated♦ data) 14 | MEN: NS when use calibrated data |
| WOMEN: No significant observations were made 14 | WOMEN: NS | |||
| Category | Rating with Reasoning |
|---|---|
| Limitations | −1 quality levels due to limitations related to measurement of exposure |
| Inconsistency | No subtraction of levels, as inconsistency does not affect confidence in results |
| Directness of evidence | −1 level due to indirect measure of exposure over time |
| Precision | No subtraction of levels as the total sample size of included studies was large |
| Publication bias | No subtraction of levels, as studies with both significant and insignificant outcomes included and grey literature adequately searched |
| Upgrading factors: Dose response | +1 as 3 studies clearly indicated a dose response whereby higher vegetable intakes were associated with the lowest risks of weight gain |
| Overall quality | Moderate: our confidence in the overall evidence is moderate, as the true effect is likely to be close to the estimate of the effect but there is possibility that it is different |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Nour, M.; Lutze, S.A.; Grech, A.; Allman-Farinelli, M. The Relationship between Vegetable Intake and Weight Outcomes: A Systematic Review of Cohort Studies. Nutrients 2018, 10, 1626. https://doi.org/10.3390/nu10111626
Nour M, Lutze SA, Grech A, Allman-Farinelli M. The Relationship between Vegetable Intake and Weight Outcomes: A Systematic Review of Cohort Studies. Nutrients. 2018; 10(11):1626. https://doi.org/10.3390/nu10111626
Chicago/Turabian StyleNour, Monica, Sarah Alice Lutze, Amanda Grech, and Margaret Allman-Farinelli. 2018. "The Relationship between Vegetable Intake and Weight Outcomes: A Systematic Review of Cohort Studies" Nutrients 10, no. 11: 1626. https://doi.org/10.3390/nu10111626
APA StyleNour, M., Lutze, S. A., Grech, A., & Allman-Farinelli, M. (2018). The Relationship between Vegetable Intake and Weight Outcomes: A Systematic Review of Cohort Studies. Nutrients, 10(11), 1626. https://doi.org/10.3390/nu10111626






