Research on Mixed and Classification Simulation Models of Medical Waste—A Case Study in Beijing, China
Abstract
1. Introduction
2. Literature Review
3. Case Study
3.1. Background
3.2. Problems
- (1)
- Lack of strict classification of medical waste: Medical waste is not classified strictly according to different categories of waste during the recycling process, with recyclable waste often being mixed with other medical wastes.
- (2)
- Low recycling rate: In addition to direct recoverable medical wastes, such as metal, glass, and plastic, most of the recyclable wastes are disposed of as nonrecyclable wastes without careful classification.
- (3)
- Lack of strict supervision of medical waste classification data: Most business processes rely on manual work, lack effective supervision methods, and suffer from poor communication, meaning the disposal process of medical waste is opaque.
- (4)
- Insufficient awareness of environmental safety: Some small and medium-sized hospitals, health clinics, and other medical institutions collect, store, incinerate, and send medical waste to landfill as ordinary waste due to the high cost of medical waste treatment. Healthcare staff and cleaners are often injured by needles, blades, and other sharp tools. Cross-infection with various pathogens increases the risk of disease transmission and environmental pollution.
3.3. Data
4. Design of Recycling Business Model
4.1. The Classification of Medical Waste
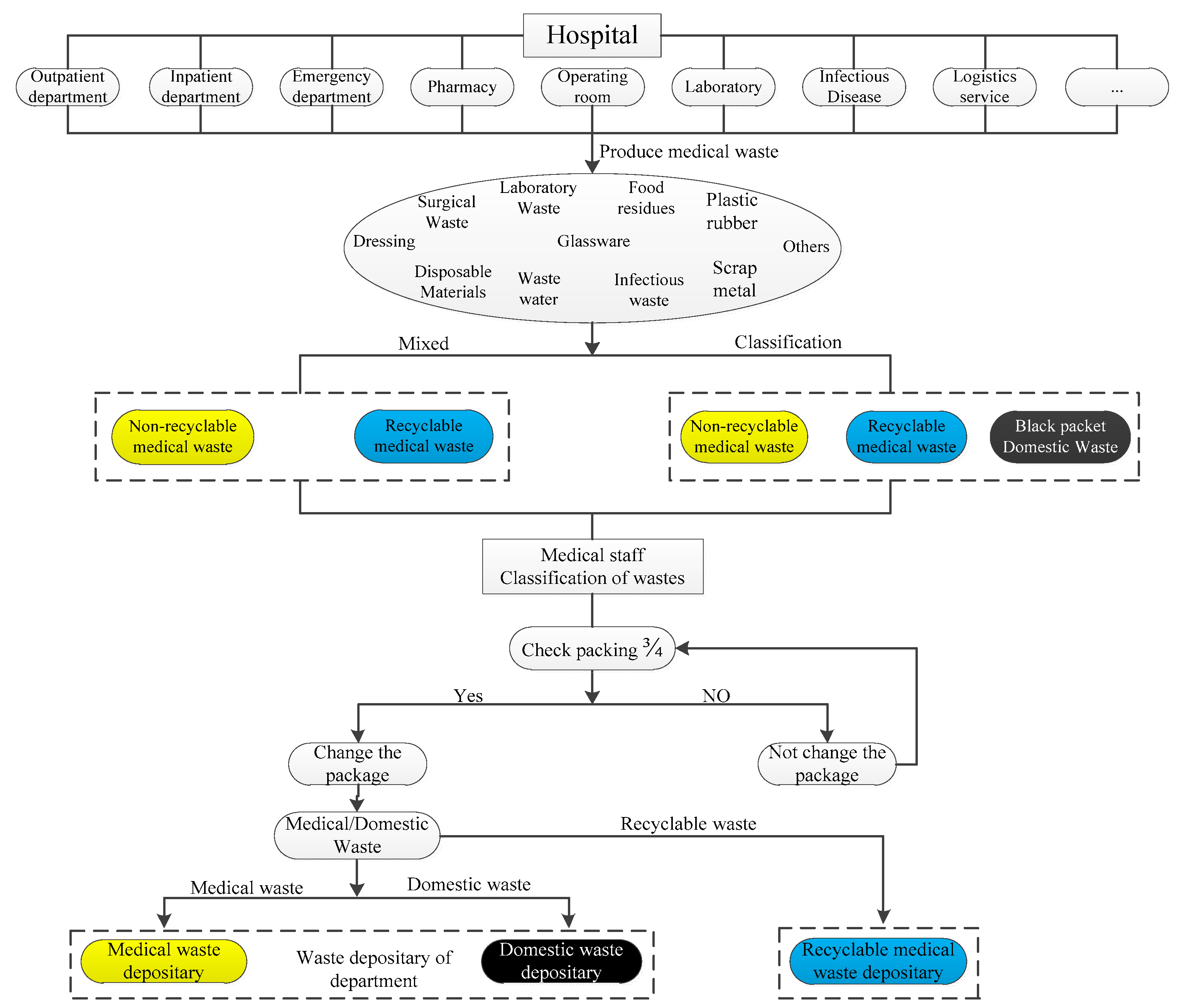
4.2. Medical Waste Recycling Business Model
- (1)
- Waste generation: Medical waste is generated in related activities such as medical care and preventive health care in various departments of the hospital. Medical waste includes waste water, surgical waste, laboratory waste, disposable consumables, dressings, food waste, infectious waste, glass, plastic, metal, and other wastes.
- (2)
- Waste classification: Medical waste has strict classification criteria. It can be classified as nonrecyclable medical waste, recyclable medical waste, and domestic waste according to the classification criteria of resource availability, and the yellow, blue, and black garbage bags are used for packaging them, respectively. Nonrecoverable medical waste is classified into infectious, pathological, injured, drug-induced, and chemical waste.In reality, some small and medium-sized hospitals and health clinics do not strictly carry out the classification standards for medical waste. Except for recyclable medical waste such as metals, plastics, paper, and glass, most of them are mixed together as nonrecyclable medical waste for disposal.
- (3)
- Temporary storage: Garbage bags for medical waste storage are generally made of polyethylene (PE), and the color is yellow. Medical waste is stored in the packaging bag and uniformly placed in the turnover box (bucket) in order to facilitate storage and transportation [32]. The turnover box (bucket) is generally made of high-density polyethylene (HDPE) [32], and the color is yellow. The medical waste marks should be printed.
5. Simulation Experiment
5.1. Basic Requirements for the Experiment
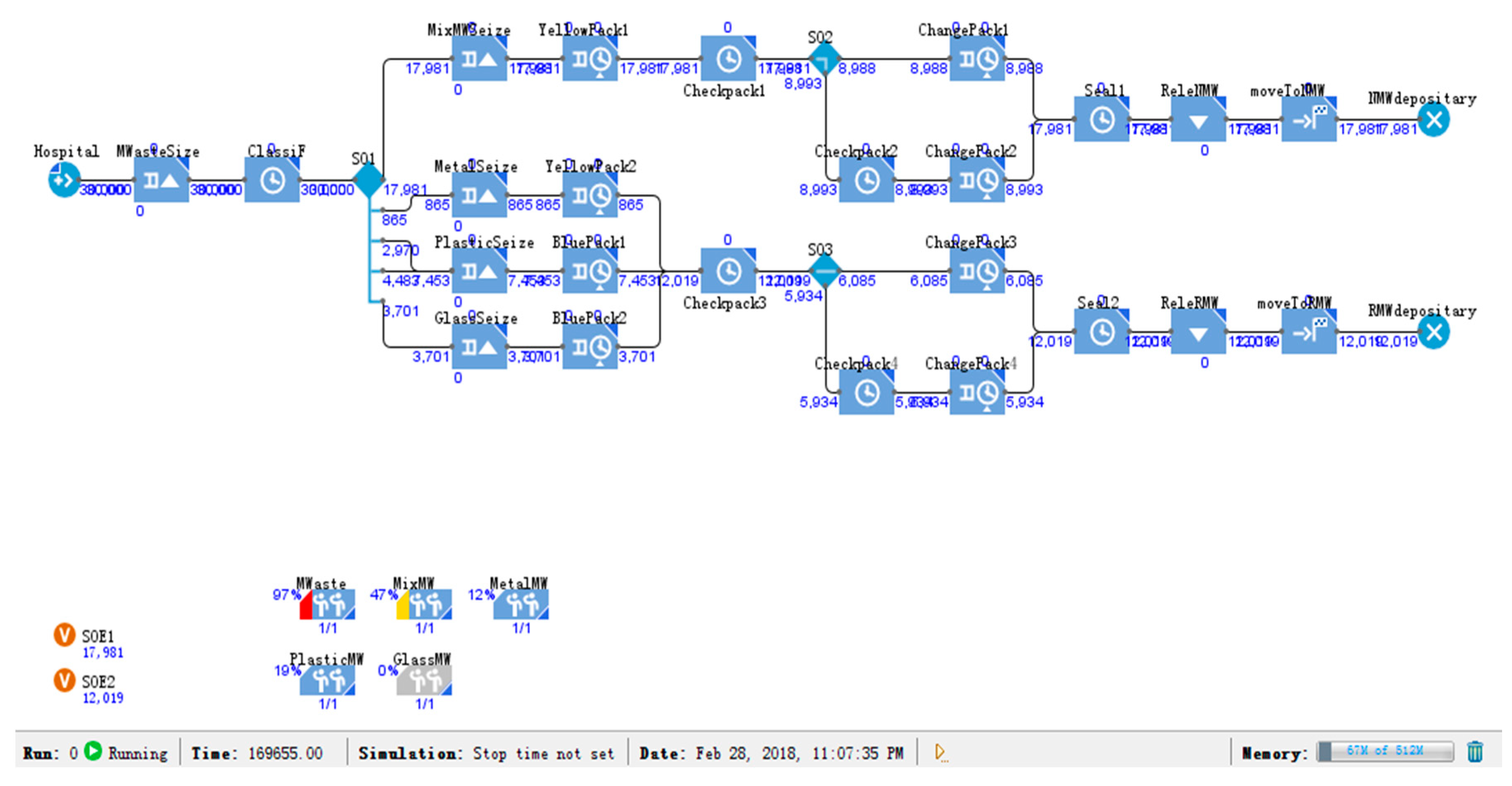
5.2. Medical Waste: Mixed Simulation Model
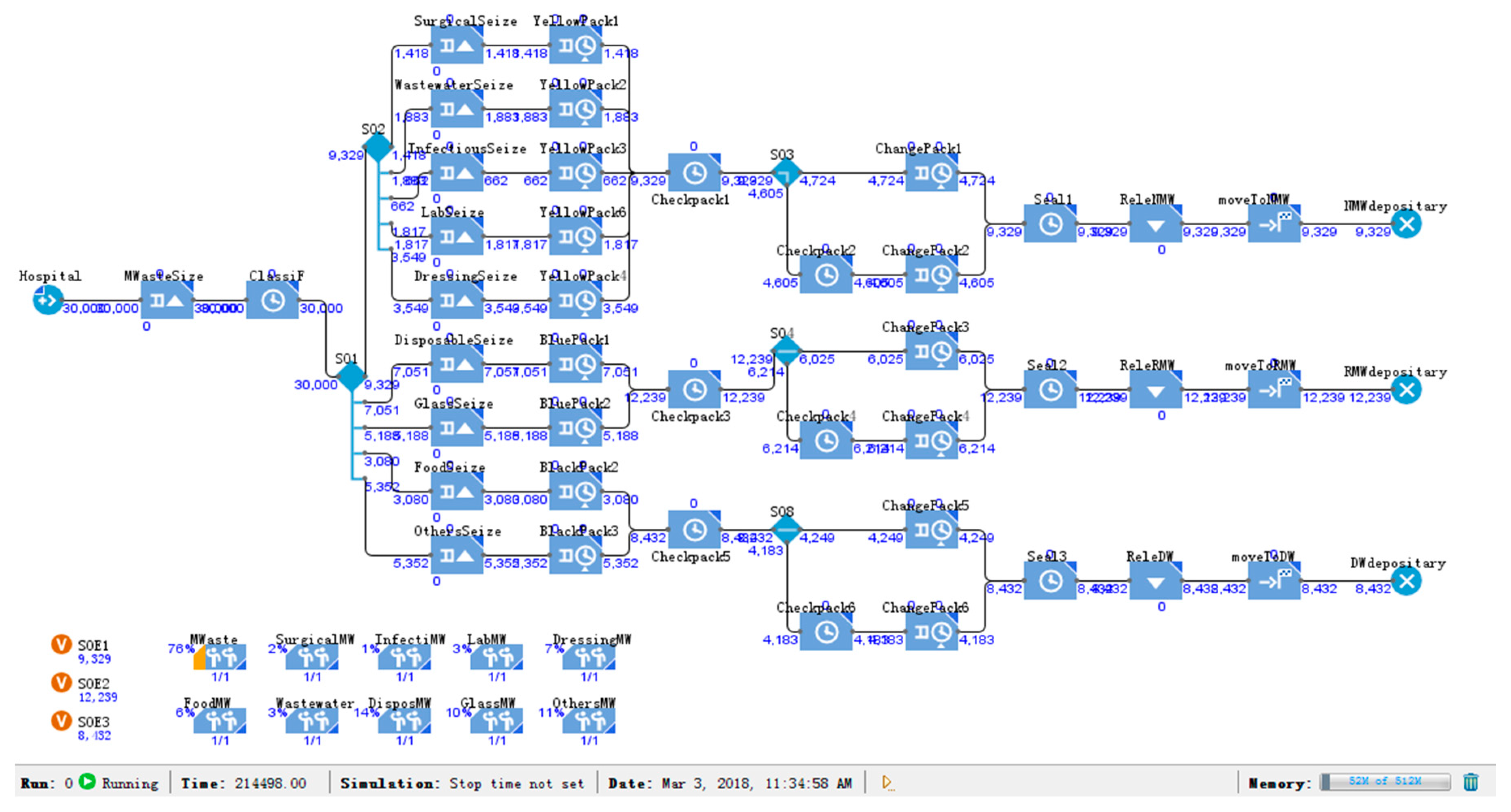
5.3. Medical Waste: Classification Simulation Model 1
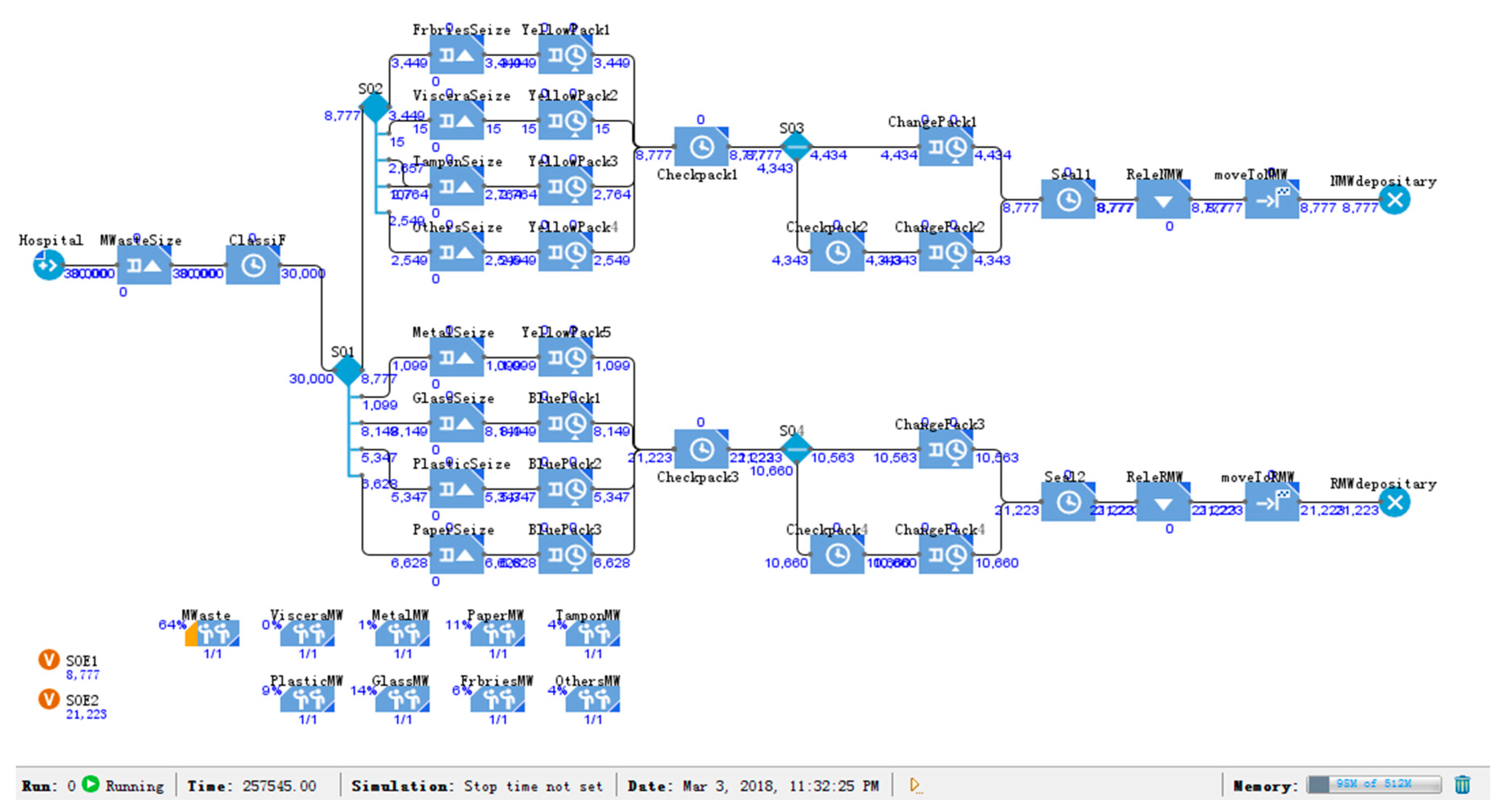
5.4. Medical Waste: Classification Simulation Model 2
6. Results
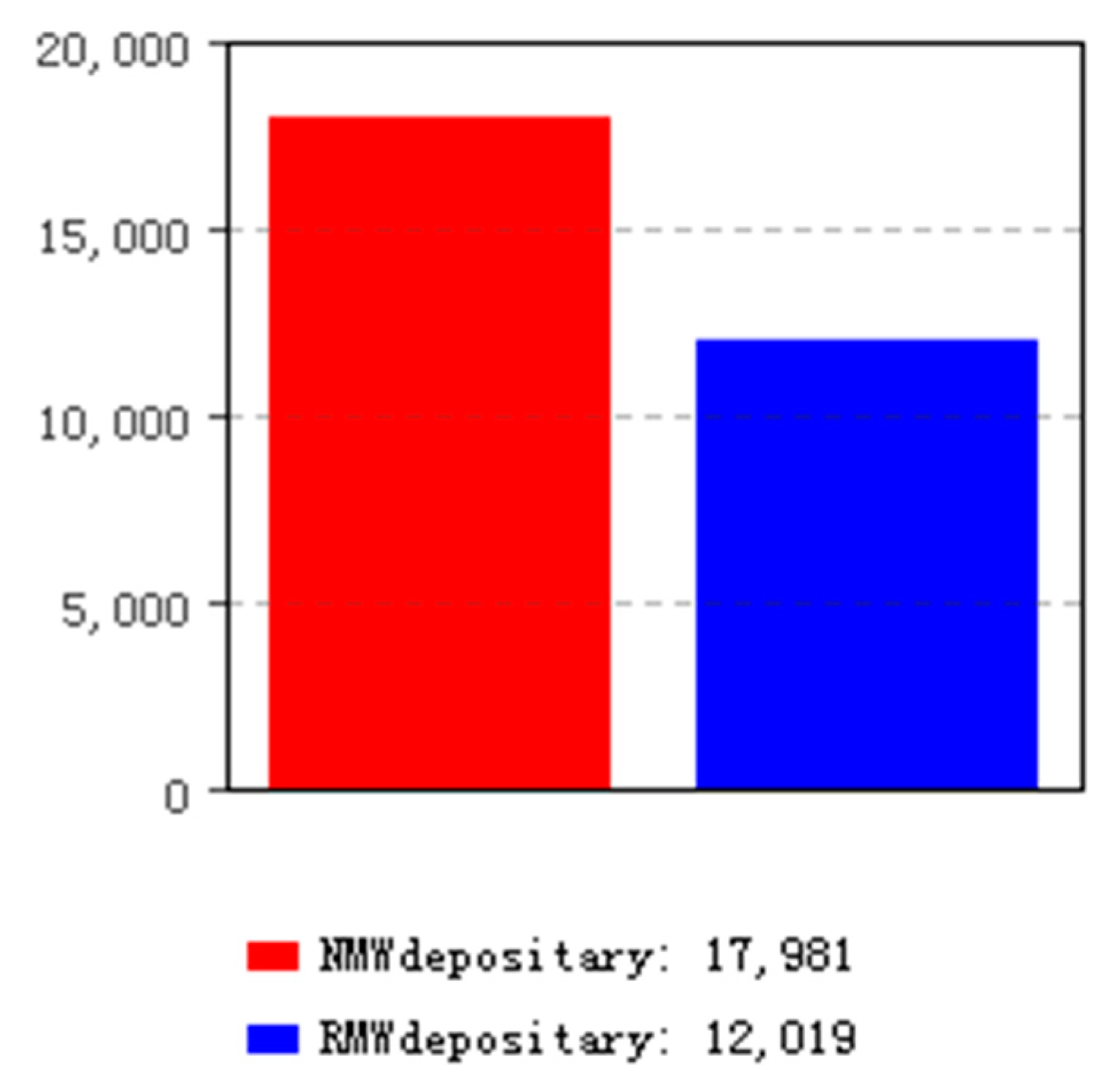
6.1. Simulation Results of the Mixed Model
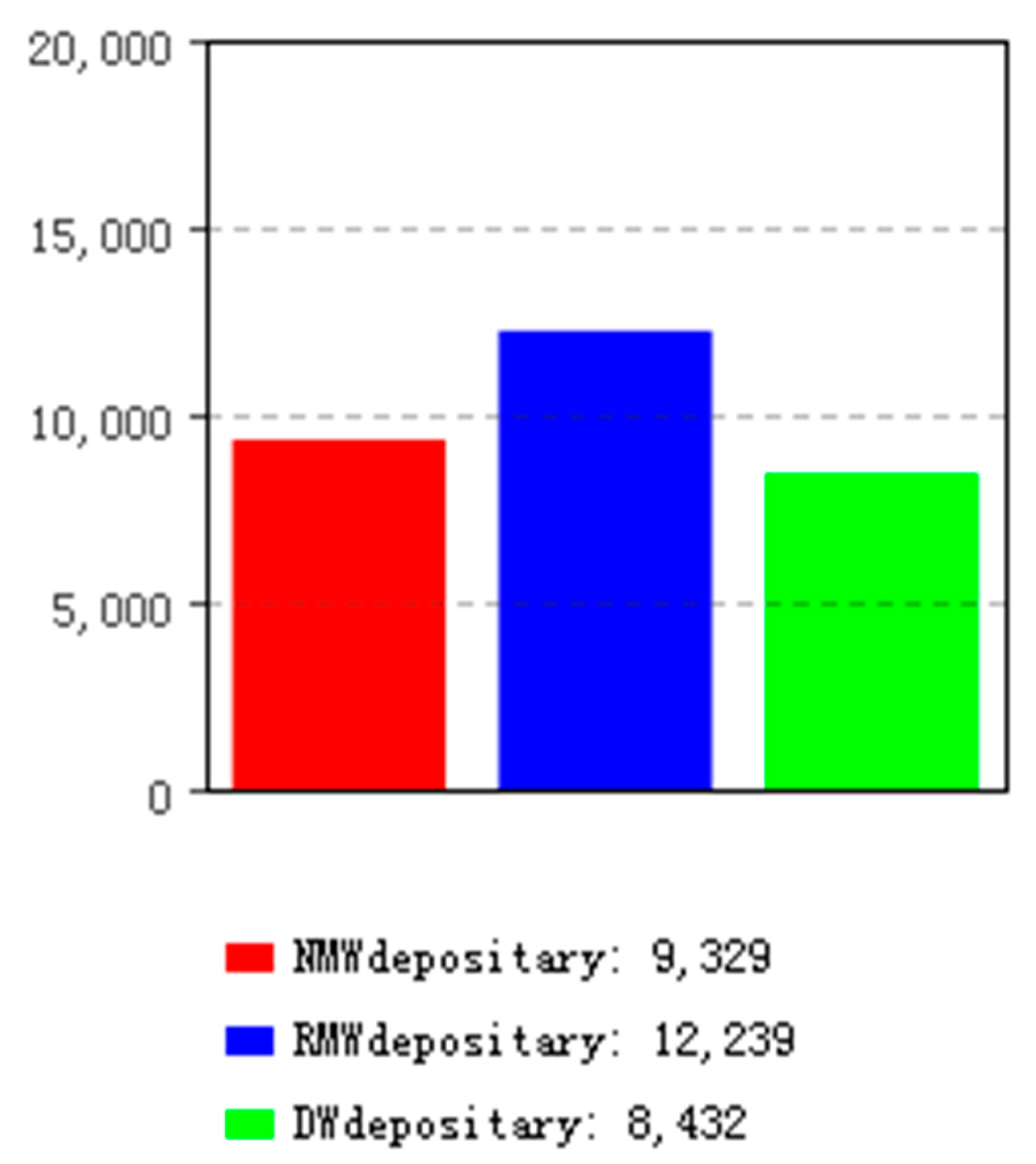
6.2. Simulation Results of Classification Model 1
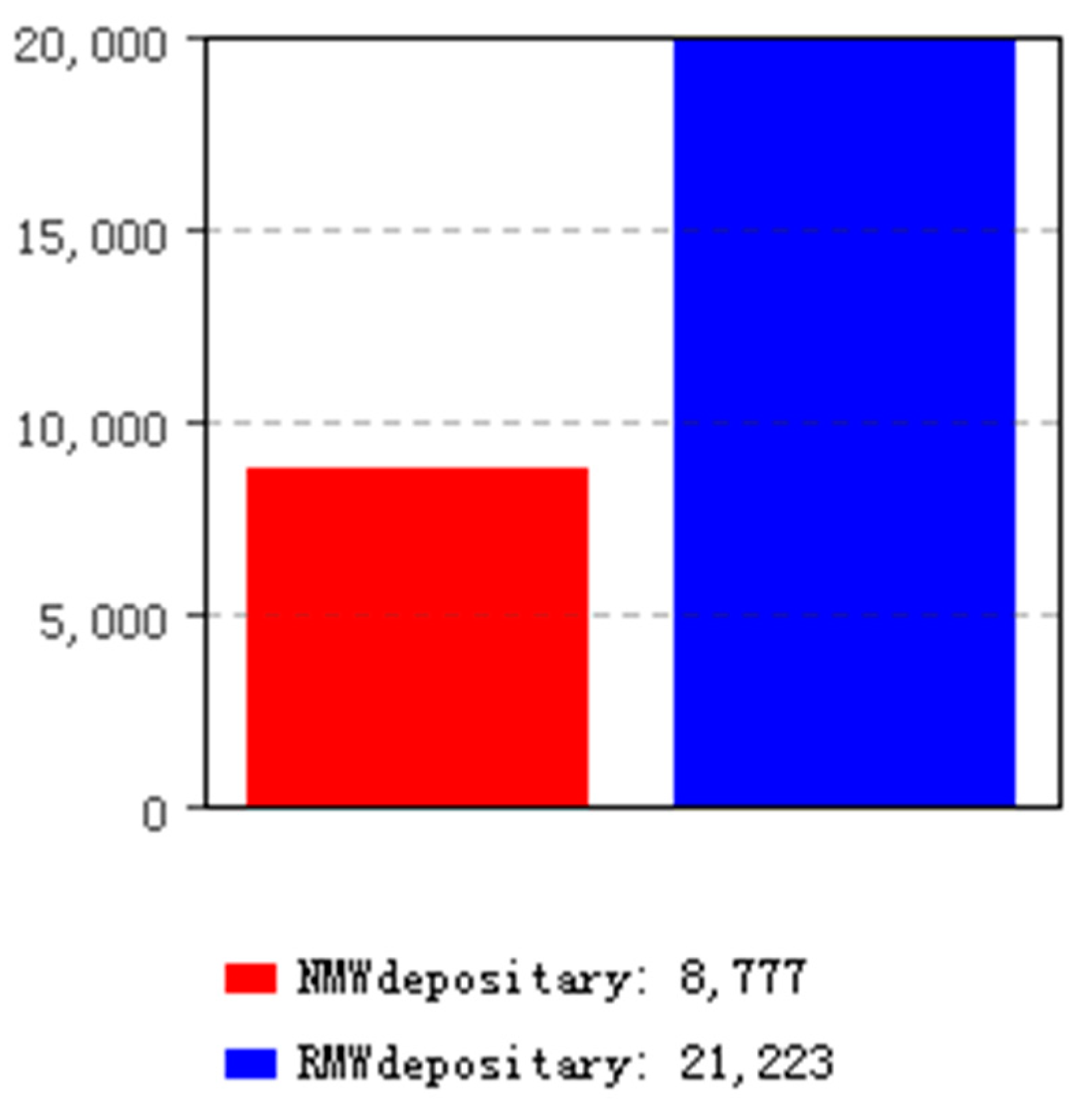
6.3. Simulation Results of Classification Model 2
7. Discussion
7.1. Output/Generation Rate
7.2. Disposal Cost
7.3. Recycling Revenue
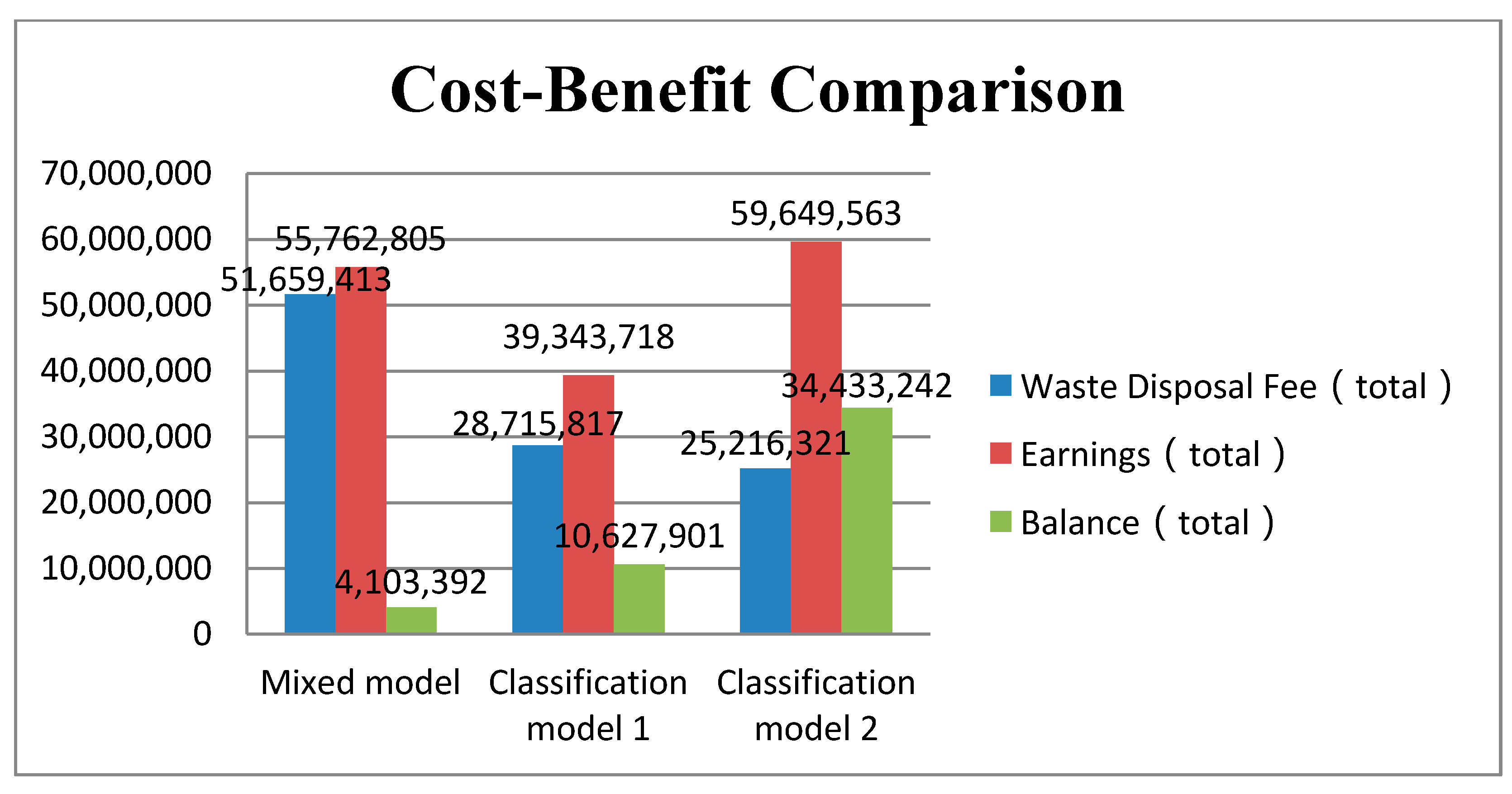
7.4. Cost–Benefit Comparison Analysis
8. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Decree of the State Council of the People’s Republic of China No. 380. Medical Waste Management Regulations. 2003. Available online: http://www.nhfpc.gov.cn/mohzcfgs/pfg/200804/18302.shtml (accessed on 16 April 2018).
- National Health and Family Planning Commission of the People’s Republic of China. Catalogue of Classified Medical Waste. 2013. Available online: http://www.moh.gov.cn/zwgkzt/mdml/201306/65605243db4e4635a9a4f819d8e6de5f.shtml (accessed on 16 April 2018).
- World Health Organization (WHO). Health-Care Waste. Fact Sheet. 2018. Available online: http://www.who.int/mediacentre/factsheets/fs253/en/ (accessed on 15 April 2018).
- Mathur, P.; Patan, S.; Shobhawat, S.A. Need of biomedical waste management system in hospitals—An emerging issue—A review. Curr. World Environ. 2012, 7, 117–124. [Google Scholar] [CrossRef]
- Liu, H.; Yao, Z.; Zhang, Q. A temporary storage systematic model for medical waste based on RFID technology. Fresenius Environ. Bull. 2018, 27, 6152–6161. [Google Scholar]
- Zhang, H.J.; Zhang, Y.H.; Wang, Y.; Yang, Y.H.; Zhang, J.; Wang, Y.L.; Wang, J.L. Investigation of medical waste management in Gansu Province, China. Waste Manag. Res. 2013, 31, 655–659. [Google Scholar] [CrossRef] [PubMed]
- Gai, R.Y.; Xu, L.Z.; Li, H.J.; Zhou, C.C.; He, J.J.; Yoshihisa, S.; Tang, W.; Chushi, K. Investigation of health care waste management in Binzhou District, China. Waste Manag. 2010, 30, 246–250. [Google Scholar] [CrossRef]
- Zhang, Y.; Xiao, G.; Wang, G.X.; Zhou, T.; Jiang, D.W. Medical waste management in China: A case study of Nanjing. Waste Manag. 2009, 29, 1376–1382. [Google Scholar] [CrossRef]
- Jang, Y.C.; Lee, C.; Yoon, O.S.; Kim, H. Medical waste management in Korea. J. Environ. Manag. 2006, 80, 107–115. [Google Scholar] [CrossRef] [PubMed]
- Windfeld, E.S.; Brooks, M.S.L. Medical waste management—A review. J. Environ. Manag. 2015, 163, 98–108. [Google Scholar] [CrossRef] [PubMed]
- Askarian, M.; Heidarpoor, P.; Assadian, O. A total quality management approach to healthcare waste management in Namazi Hospital, Iran. Waste Manag. 2010, 30, 2321–2326. [Google Scholar] [CrossRef] [PubMed]
- Kei Robert, M.; Njagi Ananias, N. Management of Health-Care Waste: A Case Study of Two National Teaching and Referral Hospitals in Kenya. JETEAS 2013, 4, 588–593. [Google Scholar]
- Hossain, M.S.; Santhanam, A.; Norulaini, N.N.; Omar, A.K.M. Clinical solid waste management practices and its impact on human health and environment—A review. Waste Manag. 2011, 31, 754–766. [Google Scholar] [CrossRef] [PubMed]
- El-Salam, M.M.A. Hospital waste management in El-Beheira Governorate, Egypt. J. Environ. Manag. 2010, 91, 618–629. [Google Scholar] [CrossRef] [PubMed]
- Mohamed, L.F.; Ebrahim, S.A.; Al-Thukair, A.A. Hazardous healthcare waste management in the Kingdom of Bahrain. Waste Manag. 2009, 29, 2404–2409. [Google Scholar] [CrossRef] [PubMed]
- Moreira, A.M.M.; Günther, W.M.R. Assessment of medical waste management at a primary health-care center in São Paulo, Brazil. Waste Manag. 2013, 33, 162–167. [Google Scholar] [CrossRef] [PubMed]
- Janagi, R.; Shah, J.; Maheshwari, D. Scenario of Management of Medical Waste in US and UK: A Review. JGTPS 2015, 6, 2328–2339. [Google Scholar]
- Minoglou, M.; Komilis, D. Describing health care waste generation rates using regression modeling and principal component analysis. Waste Manag. 2018, 78, 811–818. [Google Scholar] [CrossRef]
- Korkut, E.N. Estimations and analysis of medical waste amounts in the city of Istanbul and proposing a new approach for the estimation of future medical waste amounts. Waste Manag. 2018, 81, 168–176. [Google Scholar] [CrossRef]
- Xin, Y.T. Comparison of hospital medical waste generation rate based on diagnosis-related groups. J. Clean. Prod. 2015, 100, 202–207. [Google Scholar] [CrossRef]
- Graikos, A.; Voudrias, E.; Papazachariou, A.; Iosifidis, N.; Kalpakidou, M. Composition and production rate of medical waste from a small producer in Greece. Waste Manag. 2010, 30, 1683–1689. [Google Scholar] [CrossRef] [PubMed]
- Sharma, S.K.; Gupta, S. Healthcare waste management scenario: A case of Himachal Pradesh (India). CEGH 2017, 5, 169–172. [Google Scholar] [CrossRef]
- Kalogiannidou, K.; Nikolakopoulou, E.; Komilis, D. Generation and composition of waste from medical histopathology laboratories. Waste Manag. 2018, 79, 435–442. [Google Scholar] [CrossRef] [PubMed]
- Rabeie, O.L.; Miranzadeh, M.B.; Fallah, S.H.; Dehqan, S.; Moulana, Z.; Amouei, A.; Mohammadi, A.A.; Asgharnia, H.A.; Babaie, M. Determination of hospital waste composition and management in Amol city, Iran. Health Scope 2012, 1, 127–131. [Google Scholar] [CrossRef]
- Caniato, M.; Tudor, T.L.; Vaccari, M. Assessment of health-care waste management in a humanitarian crisis: A case study of the Gaza Strip. Waste Manag. 2016, 58, 386–396. [Google Scholar] [CrossRef] [PubMed]
- Komilis, D.; Makroleivaditis, N.; Nikolakopoulou, E. Generation and composition of medical wastes from private medical microbiology laboratories. Waste Manag. 2017, 61, 539–546. [Google Scholar] [CrossRef] [PubMed]
- Al-Khatib, I.A. Medical waste management practices in a Palestinian District hospitals, Palestine. In Proceedings of the International Conference on Agriculture, Environment and Biological Sciences (ICFAE’14), Antalya, Turkey, 4–5 June 2014; pp. 34–36. [Google Scholar]
- Birpınar, M.E.; Bilgili, M.S.; Erdoğan, T. Medical waste management in Turkey: A case study of Istanbul. Waste Manag. 2009, 29, 445–448. [Google Scholar] [CrossRef] [PubMed]
- Mbarki, A.; Kabbachi, B.; Ezaidi, A.; Benssaou, M. Medical waste management: A case Study of the Souss-Massa-Drâa Region, Morocco. J. Environ. Prot. 2013, 4, 914–919. [Google Scholar] [CrossRef]
- Ministry of Environmental Protection of the People’s Republic of China. Annual Report on Environmental Prevention and Control of Solid Waste Pollution in Large and Medium-Sized Cities in China in 2016. 2016. Available online: http://www.mee.gov.cn/gkml/sthjbgw/qt/201611/t20161122_368001.htm (accessed on 10 November 2017).
- Beijing Municipal Commission of Health and Family Planning. Beijing Municipal Health and Family Planning Development Statistical Bulletin in 2015. 2016. Available online: http://www.phic.org.cn/tonjixinxi/weishengtongjigongbao/201603/t20160325_134342.htm (accessed on 11 November 2017).
- The Environmental Protection Administration of the People’s Republic of China. Regulations on Special Packing, Vessel Standard and Warning Sign for Medical Waste. UNCED NO:188. 2003. Available online: http://www.zhb.gov.cn/gkml/zj/wj/200910/t20091022_172239.htm (accessed on 5 May 2018).
- He, Z.G.; Li, Q.; Fang, J. The solutions and recommendations for logistics problems in the collection of medical waste in China. Procedia Environ. Sci. 2016, 31, 447–456. [Google Scholar] [CrossRef]
- Ananth, A.P.; Prashanthini, V.; Visvanathan, C. Healthcare waste management in Asia. Waste Manag. 2010, 30, 154–161. [Google Scholar] [CrossRef] [PubMed]
- Geng, Y.; Ren, W.X.; Xue, B.; Fujita, T.; Xi, F.M.; Liu, Y.; Wang, M.L. Regional medical waste management in China: A case study of Shenyang. J. Mater. Cycles Waste Manag. 2013, 15, 310–320. [Google Scholar] [CrossRef]
- Chen, Y. Studies on Optimized Medical Waste Disposal Technology and Management Model for China. Ph.D. Thesis, Institute of Applied Ecology, Chinese Academy of Sciences, Shenyang, China, 2009; p. 25. (In Chinese). [Google Scholar]
- Charges Standard for Disposal of Medical Waste, Pricing Documents of the Beijing Municipal Commission of Development and Reform. Beijing Price (Charge). No. 303. 2003. Available online: http://www.bjpc.gov.cn/cxfw/jgsfcx/ylfwjg/201208/t9779282.htm (accessed on 12 June 2018).
- Price Adjustment Formula of Beijing’s GaoAnTun Medical Waste Disposal Plant, Beijing Municipal Commission of Development and Reform. No. 771. 2011. Available online: http://www.bjpc.gov.cn/cxfw/jgsfcx/ylfwjg/201208/t9779282.htm (accessed on 12 June 2018).
- Disposal Cost of Medical Waste at Beijing GaoAnTun Medical Waste Disposal Plant, Beijing Municipal Commission of Development and Reform. No. 2137. 2014. Available online: http://www.bjpc.gov.cn/cxfw/jgsfcx/ylfwjg/201208/t9779282.htm (accessed on 12 June 2018).
- Charges Standard for Sanitation, Pricing Documents of the Beijing Municipal Commission of Development and Reform. Beijing Municipal Commission of Development and Reform. No. 2662. 2013. Available online: http://www.bjpc.gov.cn/cxfw/jgsfcx/jzjg/201208/t9779300.htm (accessed on 12 June 2018).
- China Renewable Resources Price Index. Available online: http://www.crrainfo.org/ (accessed on 15 June 2018).
| Waste Category | Characteristics | Name and Composition of Waste |
|---|---|---|
| Infectious | Medical waste that easily causes infectious diseases. | It includes objects contaminated by patients’ blood, body fluids, and excretions; discarded medical specimens; disposable hygiene products; etc. |
| Pathological | Human tissues and animal carcasses generated during diagnosis. | It includes human tissues, organs, animals in medical experiments, the pathological section, etc. |
| Injured | Sharp medical waste that can easily stab or cut the body. | Needles, blades, glass tubes, slides, ampoules, etc. |
| Drug-induced | Medicines that are outdated, obsolete, spoiled, or contaminated. | Drugs, vaccines, etc. that are discarded or metamorphic. |
| Chemical | Chemical wastes that have toxic, corrosive, flammable, explosive, and other properties. | Chemical reagents, discarded contrast agents, chemical disinfectants, etc. |
| Recyclable | Waste that is not seriously polluted and can be recycled. | Infusion bottles, paper packaging, needles, scalpels, and other plastic, metal, paper, and glass. |
| Domestic | Uncontaminated ordinary rubbish produced by medical staff and patients. | Food waste, common household goods, etc. |
| Medical Waste Model | Recyclable Medical Waste (Tons/%) | Nonrecyclable Medical Waste (Tons/%) | Domestic Waste (Tons/%) |
|---|---|---|---|
| Mixed model | 12,019/40.06% | 17,981/59.94% | 0 |
| Classification model 1 | 12,239/40.8% | 9329/31.1% | 8432/28.1% |
| Classification model 2 | 21,223/70.74% | 8777/29.25% | 0 |
| Medical Waste Model | Nonrecyclable Medical Waste (CNY) | Domestic Waste (CNY) | Waste Disposal Fee (Total) (CNY) |
|---|---|---|---|
| Mixed model | 51,659,413 | 0 | 51,659,413 |
| Classification model 1 | 26,802,217 | 1,913,600 | 28,715,817 |
| Classification model 2 | 25,216,321 | 0 | 25,216,321 |
| Medical Waste Model | Glasses (Tons) | Paper (Tons) | Plastics (Tons) | Metals (Tons) | Disposable Materials (Tons) |
|---|---|---|---|---|---|
| Mixed model | 3701 | 0 | 7453 | 865 | 0 |
| Classification model 1 | 5188 | 0 | 0 | 0 | 7051 |
| Classification model 2 | 8149 | 6628 | 5347 | 1099 | 0 |
| Medical Waste Model | Glasses (CNY) | Paper (CNY) | Plastics (CNY) | Metals (CNY) | Earnings (Total) (CNY) |
|---|---|---|---|---|---|
| Mixed model | 1,665,450 | 0 | 52,171,000 | 1,926,355 | 55,762,805 |
| Classification model 1 | 2,334,600 | 5,311,980 | 30,597,000 | 1,100,138 | 39,343,718 |
| Classification model 2 | 3,667,050 | 16,106,040 | 37,429,000 | 2,447,473 | 59,649,563 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, H.; Yao, Z. Research on Mixed and Classification Simulation Models of Medical Waste—A Case Study in Beijing, China. Sustainability 2018, 10, 4226. https://doi.org/10.3390/su10114226
Liu H, Yao Z. Research on Mixed and Classification Simulation Models of Medical Waste—A Case Study in Beijing, China. Sustainability. 2018; 10(11):4226. https://doi.org/10.3390/su10114226
Chicago/Turabian StyleLiu, Hao, and Zhong Yao. 2018. "Research on Mixed and Classification Simulation Models of Medical Waste—A Case Study in Beijing, China" Sustainability 10, no. 11: 4226. https://doi.org/10.3390/su10114226
APA StyleLiu, H., & Yao, Z. (2018). Research on Mixed and Classification Simulation Models of Medical Waste—A Case Study in Beijing, China. Sustainability, 10(11), 4226. https://doi.org/10.3390/su10114226





