Modulating Inflammation-Mediated Diseases via Natural Phenolic Compounds Loaded in Nanocarrier Systems
Abstract
1. Introduction
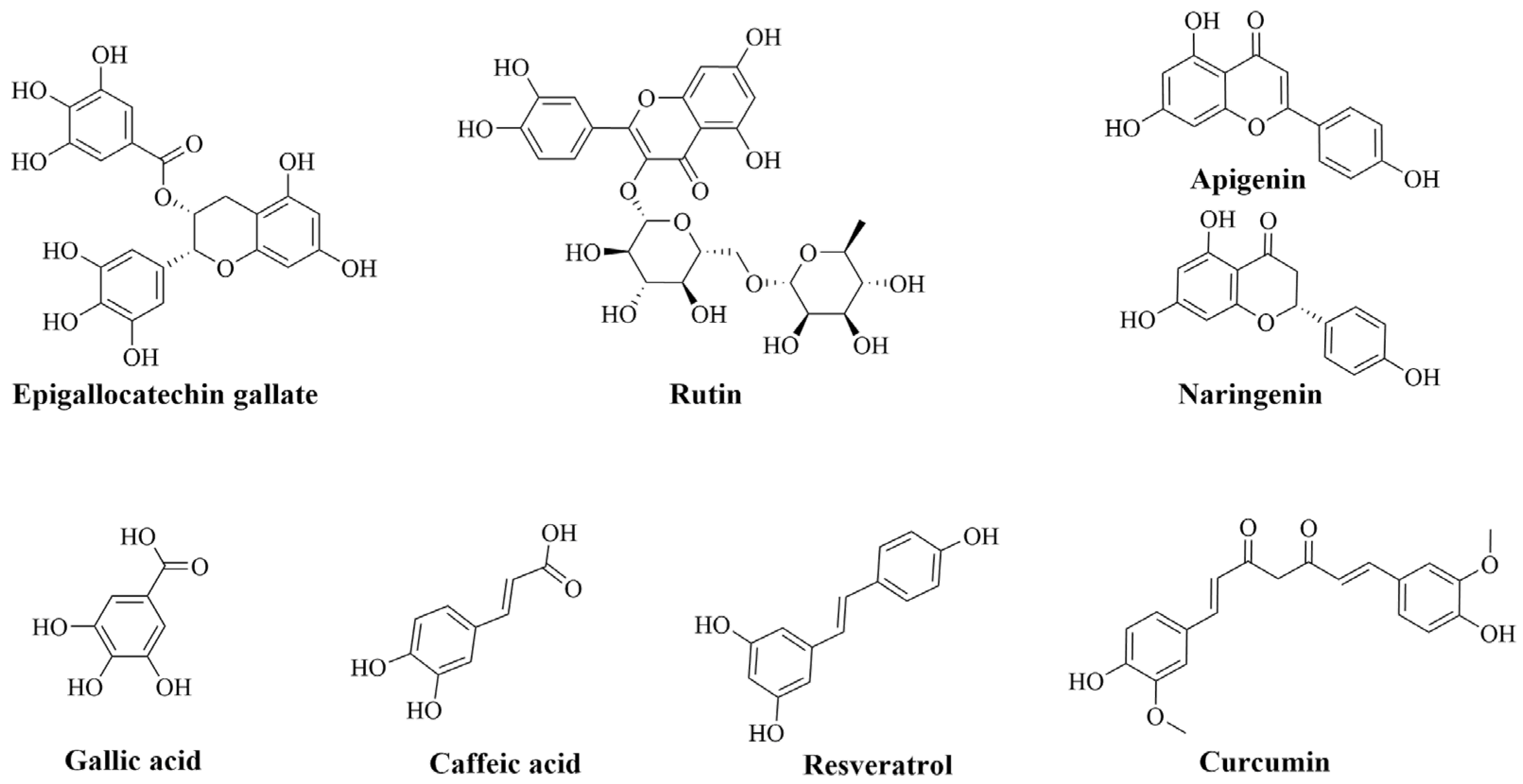
2. Natural Phenolic Compounds in Inflammatory Mitigation and Their Challenges
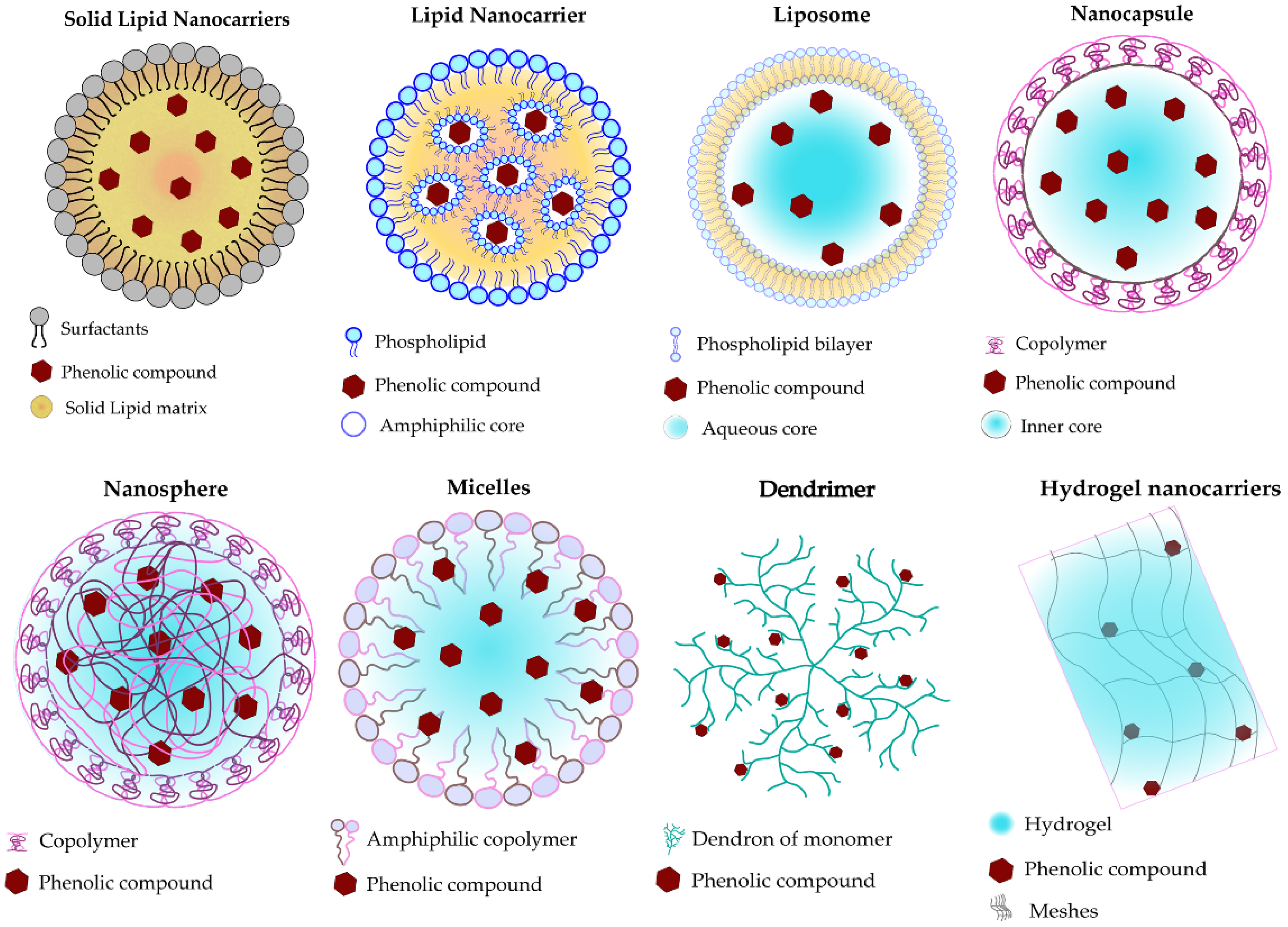
3. Nanocarriers Systems Used for Loading Phenolic Compounds
3.1. Organic Nanocarriers
3.2. Inorganic Nanocarriers
4. Designed Polyphenolic-Loaded Nanocarriers for Inflammation-Mediated Diseases
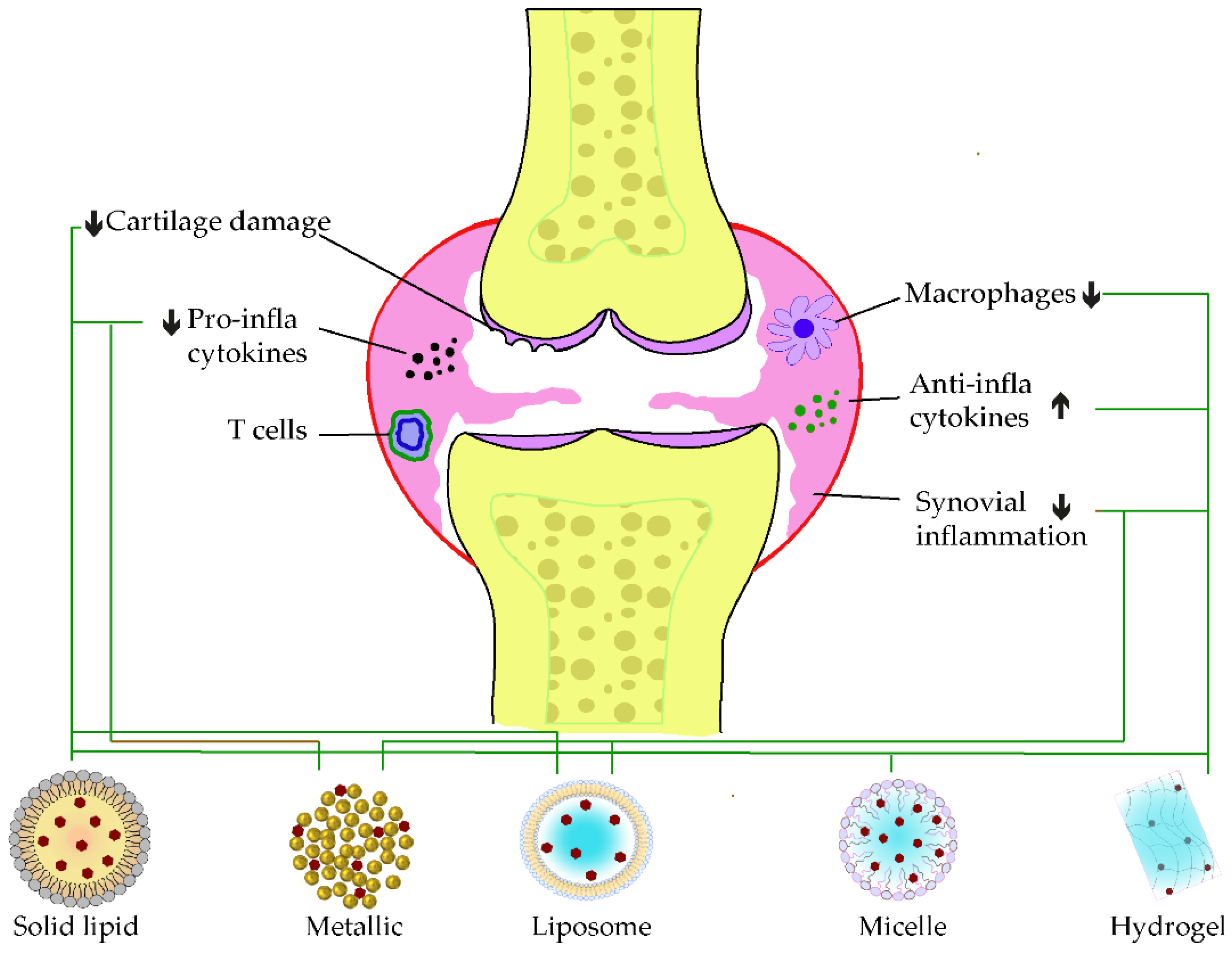
4.1. Polyphenolic Nano Delivery for Rheumatoid Arthritis
4.2. Polyphenolic Nano Delivery for Neurodegenerative Disease
4.3. Polyphenolic Nano Delivery for Skin Inflammation and Wound
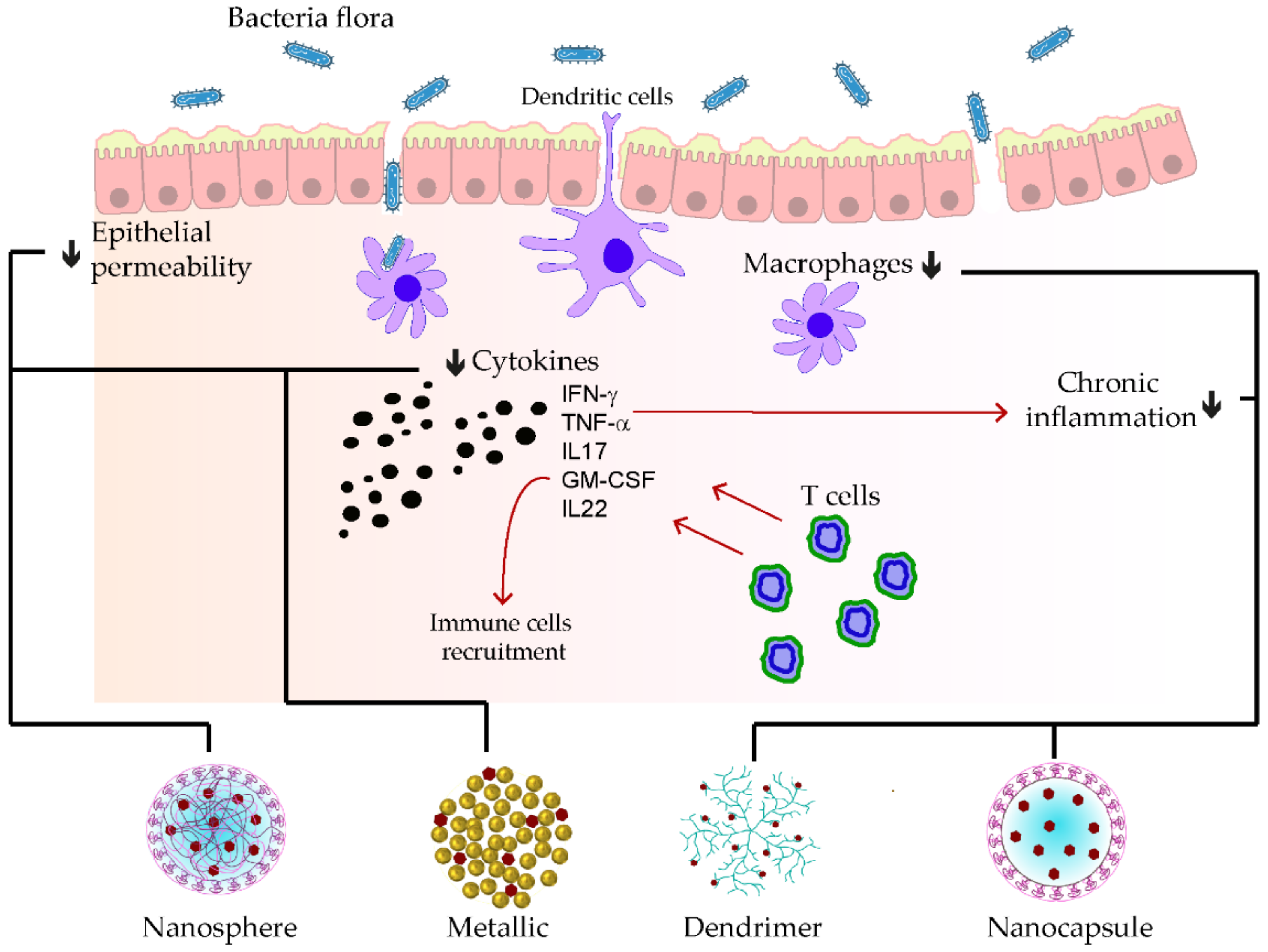
4.4. Polyphenolic Nano Delivery in Inflammatory Bowel Disease
4.5. Polyphenolic Nano Delivery for Metabolic Disorder
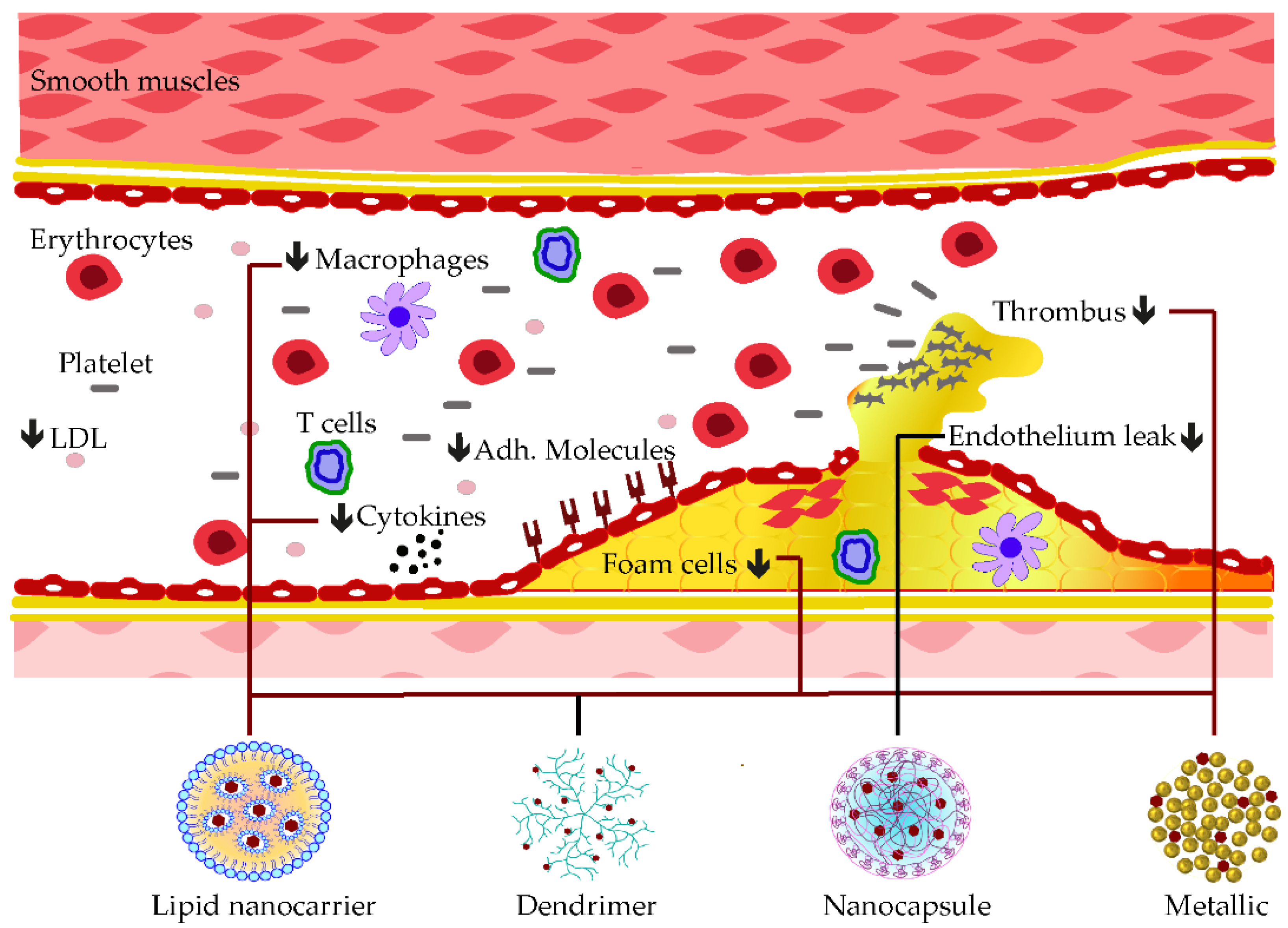
4.6. Polyphenolic Nano Delivery for Cardiovascular Disease
5. Conclusions and Future Perspectives
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- He, Y.; Yue, Y.; Zheng, X.; Zhang, K.; Chen, S.; Du, Z. Curcumin, Inflammation, and Chronic Diseases: How Are They Linked? Molecules 2015, 20, 9183–9213. [Google Scholar] [CrossRef]
- Placha, D.; Jampilek, J. Chronic Inflammatory Diseases, Anti-Inflammatory Agents and Their Delivery Nanosystems. Pharmaceutics 2021, 13, 64. [Google Scholar] [CrossRef]
- Jogpal, V.; Sanduja, M.; Dutt, R.; Garg, V.; Tinku. Advancement of Nanomedicines in Chronic Inflammatory Disorders. Inflammopharmacology 2022, 30, 355–368. [Google Scholar] [CrossRef]
- Cronkite, D.A.; Strutt, T.M. The Regulation of Inflammation by Innate and Adaptive Lymphocytes. J. Immunol. Res. 2018, 2018, e1467538. [Google Scholar] [CrossRef]
- Conte, R.; Marturano, V.; Peluso, G.; Calarco, A.; Cerruti, P. Recent Advances in Nanoparticle-Mediated Delivery of Anti-Inflammatory Phytocompounds. Int. J. Mol. Sci. 2017, 18, 709. [Google Scholar] [CrossRef]
- Tang, D.-W.; Yu, S.-H.; Ho, Y.-C.; Huang, B.-Q.; Tsai, G.-J.; Hsieh, H.-Y.; Sung, H.-W.; Mi, F.-L. Characterization of Tea Catechins-Loaded Nanoparticles Prepared from Chitosan and an Edible Polypeptide. Food Hydrocoll. 2013, 30, 33–41. [Google Scholar] [CrossRef]
- Garavand, F.; Jalai-Jivan, M.; Assadpour, E.; Jafari, S.M. Encapsulation of Phenolic Compounds within Nano/Microemulsion Systems: A Review. Food Chem. 2021, 364, 130376. [Google Scholar] [CrossRef]
- Patra, J.K.; Das, G.; Fraceto, L.F.; Campos, E.V.R.; Rodriguez-Torres, M.D.P.; Acosta-Torres, L.S.; Diaz-Torres, L.A.; Grillo, R.; Swamy, M.K.; Sharma, S.; et al. Nano Based Drug Delivery Systems: Recent Developments and Future Prospects. J. Nanobiotechnology 2018, 16, 71. [Google Scholar] [CrossRef]
- Rashmi, H.B.; Negi, P.S. Phenolic Acids from Vegetables: A Review on Processing Stability and Health Benefits. Food Res. Int. 2020, 136, 109298. [Google Scholar] [CrossRef]
- Albuquerque, B.R.; Heleno, S.A.; Oliveira, M.B.P.P.; Barros, L.; Ferreira, I.C.F.R. Phenolic Compounds: Current Industrial Applications, Limitations and Future Challenges. Food Funct. 2021, 12, 14–29. [Google Scholar] [CrossRef]
- Tao, H.; Li, L.; He, Y.; Zhang, X.; Zhao, Y.; Wang, Q.; Hong, G. Flavonoids in Vegetables: Improvement of Dietary Flavonoids by Metabolic Engineering to Promote Health. Crit. Rev. Food Sci. Nutr. 2022, 11, 1–15. [Google Scholar] [CrossRef]
- Călinoiu, L.F.; Vodnar, D.C. Whole Grains and Phenolic Acids: A Review on Bioactivity, Functionality, Health Benefits and Bioavailability. Nutrients 2018, 10, 1615. [Google Scholar] [CrossRef]
- Fechtner, S.; Singh, A.; Chourasia, M.; Ahmed, S. Molecular Insights into the Differences in Anti-Inflammatory Activities of Green Tea Catechins on IL-1β Signaling in Rheumatoid Arthritis Synovial Fibroblasts. Toxicol. Appl. Pharmacol. 2017, 329, 112–120. [Google Scholar] [CrossRef]
- Miao, Z.; Zhao, Y.; Chen, M.; He, C. Using Flavonoids as a Therapeutic Intervention against Rheumatoid Arthritis: The Known and Unknown. Pharm. Res. Mod. Chin. Med. 2022, 3, 100014. [Google Scholar] [CrossRef]
- Lin, Y.; Luo, T.; Weng, A.; Huang, X.; Yao, Y.; Fu, Z.; Li, Y.; Liu, A.; Li, X.; Chen, D.; et al. Gallic Acid Alleviates Gouty Arthritis by Inhibiting NLRP3 Inflammasome Activation and Pyroptosis Through Enhancing Nrf2 Signaling. Front. Immunol. 2020, 11, 580593. [Google Scholar] [CrossRef]
- Ide, K.; Matsuoka, N.; Yamada, H.; Furushima, D.; Kawakami, K. Effects of Tea Catechins on Alzheimer’s Disease: Recent Updates and Perspectives. Molecules 2018, 23, 2357. [Google Scholar] [CrossRef]
- Devi, S.; Kumar, V.; Singh, S.K.; Dubey, A.K.; Kim, J.-J. Flavonoids: Potential Candidates for the Treatment of Neurodegenerative Disorders. Biomedicines 2021, 9, 99. [Google Scholar] [CrossRef]
- Caruso, G.; Godos, J.; Privitera, A.; Lanza, G.; Castellano, S.; Chillemi, A.; Bruni, O.; Ferri, R.; Caraci, F.; Grosso, G. Phenolic Acids and Prevention of Cognitive Decline: Polyphenols with a Neuroprotective Role in Cognitive Disorders and Alzheimer’s Disease. Nutrients 2022, 14, 819. [Google Scholar] [CrossRef]
- Fan, F.-Y.; Sang, L.-X.; Jiang, M. Catechins and Their Therapeutic Benefits to Inflammatory Bowel Disease. Molecules 2017, 22, 484. [Google Scholar] [CrossRef]
- Hoensch, H.P.; Weigmann, B. Regulation of the Intestinal Immune System by Flavonoids and Its Utility in Chronic Inflammatory Bowel Disease. World J. Gastroenterol. 2018, 24, 877–881. [Google Scholar] [CrossRef]
- Ginwala, R.; Bhavsar, R.; Chigbu, D.G.I.; Jain, P.; Khan, Z.K. Potential Role of Flavonoids in Treating Chronic Inflammatory Diseases with a Special Focus on the Anti-Inflammatory Activity of Apigenin. Antioxidants 2019, 8, 35. [Google Scholar] [CrossRef]
- Dinda, B.; Dinda, M.; Roy, A.; Dinda, S. Dietary Plant Flavonoids in Prevention of Obesity and Diabetes. Adv. Protein Chem. Struct. Biol. 2020, 120, 159–235. [Google Scholar] [CrossRef]
- Vinayagam, R.; Jayachandran, M.; Xu, B. Antidiabetic Effects of Simple Phenolic Acids: A Comprehensive Review. Phyto. Res. 2016, 30, 184–199. [Google Scholar] [CrossRef]
- Pourhabibi-Zarandi, F.; Shojaei-Zarghani, S.; Rafraf, M. Curcumin and Rheumatoid Arthritis: A Systematic Review of Literature. Int. J. Clin. Pract. 2021, 75, e14280. [Google Scholar] [CrossRef]
- Karimi, A.; Azar, P.S.; Kadkhodayi, M.; Tandorost, A.; Vajdi, M.; Shoorei, H.; Farhangi, M.A. A Comprehensive Insight into Effects of Resveratrol on Molecular Mechanism in Rheumatoid Arthritis: A Literature Systematic Review. Int. J. Rheum. Dis. 2022, 25, 827–843. [Google Scholar] [CrossRef]
- Eghbaliferiz, S.; Farhadi, F.; Barreto, G.E.; Majeed, M.; Sahebkar, A. Effects of Curcumin on Neurological Diseases: Focus on Astrocytes. Pharmacol. Rep. 2020, 72, 769–782. [Google Scholar] [CrossRef]
- Huang, J.; Huang, N.; Xu, S.; Luo, Y.; Li, Y.; Jin, H.; Yu, C.; Shi, J.; Jin, F. Signaling Mechanisms Underlying Inhibition of Neuroinflammation by Resveratrol in Neurodegenerative Diseases. J. Nutr. Biochem. 2021, 88, 108552. [Google Scholar] [CrossRef]
- Fallahi, F.; Borran, S.; Ashrafizadeh, M.; Zarrabi, A.; Pourhanifeh, M.H.; Khaksary Mahabady, M.; Sahebkar, A.; Mirzaei, H. Curcumin and Inflammatory Bowel Diseases: From in Vitro Studies to Clinical Trials. Mol. Immunol. 2021, 130, 20–30. [Google Scholar] [CrossRef]
- Karthikeyan, A.; Young, K.N.; Moniruzzaman, M.; Beyene, A.M.; Do, K.; Kalaiselvi, S.; Min, T. Curcumin and Its Modified Formulations on Inflammatory Bowel Disease (IBD): The Story So Far and Future Outlook. Pharmaceutics 2021, 13, 484. [Google Scholar] [CrossRef]
- Nunes, S.; Danesi, F.; Del Rio, D.; Silva, P. Resveratrol and Inflammatory Bowel Disease: The Evidence so Far. Nutr. Res. Rev. 2018, 31, 85–97. [Google Scholar] [CrossRef]
- Gowd, V.; Kanika; Jori, C.; Chaudhary, A.A.; Rudayni, H.A.; Rashid, S.; Khan, R. Resveratrol and Resveratrol Nano-Delivery Systems in the Treatment of Inflammatory Bowel Disease. J. Nutr. Biochem. 2022, 109, 109101. [Google Scholar] [CrossRef]
- Meng, X.; Zhou, J.; Zhao, C.-N.; Gan, R.-Y.; Li, H.-B. Health Benefits and Molecular Mechanisms of Resveratrol: A Narrative Review. Foods 2020, 9, 340. [Google Scholar] [CrossRef]
- Thakur, L.; Ghodasra, U.; Patel, N.; Dabhi, M. Novel Approaches for Stability Improvement in Natural Medicines. Phcog. Rev. 2011, 5, 48. [Google Scholar] [CrossRef]
- Krupkova, O.; Ferguson, S.J.; Wuertz-Kozak, K. Stability of (−)-Epigallocatechin Gallate and Its Activity in Liquid Formulations and Delivery Systems. J. Nutr. Biochem. 2016, 37, 1–12. [Google Scholar] [CrossRef]
- Kyriakoudi, A.; Spanidi, E.; Mourtzinos, I.; Gardikis, K. Innovative Delivery Systems Loaded with Plant Bioactive Ingredients: Formulation Approaches and Applications. Plants 2021, 10, 1238. [Google Scholar] [CrossRef]
- Fendler, J.H.; Romero, A. Liposomes as Drug Carriers. Life Sci. 1977, 20, 1109–1120. [Google Scholar] [CrossRef]
- Couvreur, P.; Vauthier, C. Polyalkylcyanoacrylate Nanoparticles as Drug Carrier: Present State and Perspectives. J. Control. Release 1991, 17, 187–198. [Google Scholar] [CrossRef]
- Harrington, K.J.; Lewanski, C.; Northcote, A.D.; Whittaker, J.; Peters, A.M.; Vile, R.G.; Stewart, J.S.W. Phase II Study of Pegylated Liposomal Doxorubicin (Caelyx™) as Induction Chemotherapy for Patients with Squamous Cell Cancer of the Head and Neck. Eur. J. Cancer 2001, 37, 2015–2022. [Google Scholar] [CrossRef]
- Mehnert, W.; Mäder, K. Solid Lipid Nanoparticles: Production, Characterization and Applications. Adv. Drug Deliv. Rev. 2001, 47, 165–196. [Google Scholar] [CrossRef]
- Sarfraz, M.; Qamar, S.; Rehman, M.U.; Tahir, M.A.; Ijaz, M.; Ahsan, A.; Asim, M.H.; Nazir, I. Nano-Formulation Based Intravesical Drug Delivery Systems: An Overview of Versatile Approaches to Improve Urinary Bladder Diseases. Pharmaceutics 2022, 14, 1909. [Google Scholar] [CrossRef]
- Vanti, G. Recent Strategies in Nanodelivery Systems for Natural Products: A Review. Environ. Chem. Lett. 2021, 19, 4311–4326. [Google Scholar] [CrossRef]
- Ajeeshkumar, K.K.; Aneesh, P.A.; Raju, N.; Suseela, M.; Ravishankar, C.N.; Benjakul, S. Advancements in Liposome Technology: Preparation Techniques and Applications in Food, Functional Foods, and Bioactive Delivery: A Review. Compr. Rev. Food Sci. Food Saf. 2021, 20, 1280–1306. [Google Scholar] [CrossRef]
- Filipczak, N.; Pan, J.; Yalamarty, S.S.K.; Torchilin, V.P. Recent Advancements in Liposome Technology. Adv. Drug Deliv. Rev. 2020, 156, 4–22. [Google Scholar] [CrossRef]
- Figueroa-Robles, A.; Antunes-Ricardo, M.; Guajardo-Flores, D. Encapsulation of Phenolic Compounds with Liposomal Improvement in the Cosmetic Industry. Int. J. Pharm. 2021, 593, 120125. [Google Scholar] [CrossRef]
- Nishimoto-Sauceda, D.; Romero-Robles, L.E.; Antunes-Ricardo, M. Biopolymer Nanoparticles: A Strategy to Enhance Stability, Bioavailability, and Biological Effects of Phenolic Compounds as Functional Ingredients. J. Sci. Food Agric. 2022, 102, 41–52. [Google Scholar] [CrossRef]
- Faridi Esfanjani, A.; Jafari, S.M. Biopolymer Nano-Particles and Natural Nano-Carriers for Nano-Encapsulation of Phenolic Compounds. Colloids Surf. B Biointerfaces. 2016, 146, 532–543. [Google Scholar] [CrossRef]
- Kedar, U.; Phutane, P.; Shidhaye, S.; Kadam, V. Advances in Polymeric Micelles for Drug Delivery and Tumor Targeting. Nanomedicine. 2010, 6, 714–729. [Google Scholar] [CrossRef]
- Chai, Q.; Jiao, Y.; Yu, X. Hydrogels for Biomedical Applications: Their Characteristics and the Mechanisms behind Them. Gels 2017, 3, 6. [Google Scholar] [CrossRef]
- Wang, Y.; Zhao, Q.; Han, N.; Bai, L.; Li, J.; Liu, J.; Che, E.; Hu, L.; Zhang, Q.; Jiang, T.; et al. Mesoporous Silica Nanoparticles in Drug Delivery and Biomedical Applications. Nanomedicine 2015, 11, 313–327. [Google Scholar] [CrossRef]
- Li, Y.; Li, N.; Pan, W.; Yu, Z.; Yang, L.; Tang, B. Hollow Mesoporous Silica Nanoparticles with Tunable Structures for Controlled Drug Delivery. ACS Appl. Mater. Interfaces 2017, 9, 2123–2129. [Google Scholar] [CrossRef]
- Liu, S.; Chen, X.; Ai, W.; Wei, C. A New Method to Prepare Mesoporous Silica from Coal Gasification Fine Slag and Its Application in Methylene Blue Adsorption. J. Clean. Prod. 2019, 212, 1062–1071. [Google Scholar] [CrossRef]
- Chandrakala, V.; Aruna, V.; Angajala, G. Review on Metal Nanoparticles as Nanocarriers: Current Challenges and Perspectives in Drug Delivery Systems. Emergent. Mater. 2022, 5, 1593–1615. [Google Scholar] [CrossRef]
- Soliman, M.G.; Pelaz, B.; Parak, W.J.; del Pino, P. Phase Transfer and Polymer Coating Methods toward Improving the Stability of Metallic Nanoparticles for Biological Applications. Chem. Mater. 2015, 27, 990–997. [Google Scholar] [CrossRef]
- Jurašin, D.D.; Ćurlin, M.; Capjak, I.; Crnković, T.; Lovrić, M.; Babič, M.; Horák, D.; Vinković Vrček, I.; Gajović, S. Surface Coating Affects Behavior of Metallic Nanoparticles in a Biological Environment. Beilstein J. Nanotechnol. 2016, 7, 246–262. [Google Scholar] [CrossRef]
- Desai, N.; Momin, M.; Khan, T.; Gharat, S.; Ningthoujam, R.S.; Omri, A. Metallic Nanoparticles as Drug Delivery System for the Treatment of Cancer. Expert Opin. Drug Deliv. 2021, 18, 1261–1290. [Google Scholar] [CrossRef]
- Nicolas, J.; Mura, S.; Brambilla, D.; Mackiewicz, N.; Couvreur, P. Design, Functionalization Strategies and Biomedical Applications of Targeted Biodegradable/Biocompatible Polymer-Based Nanocarriers for Drug Delivery. Chem. Soc. Rev. 2013, 42, 1147–1235. [Google Scholar] [CrossRef]
- Li, Y.; Champion, J.A. Self-Assembling Nanocarriers from Engineered Proteins: Design, Functionalization, and Application for Drug Delivery. Adv. Drug Deliv. Rev. 2022, 189, 114462. [Google Scholar] [CrossRef]
- Jiang, Q.; Wang, X.; Huang, E.; Wang, Q.; Wen, C.; Yang, G.; Lu, L.; Cui, D. Inflammasome and Its Therapeutic Targeting in Rheumatoid Arthritis. Front. Immunol. 2022, 12, 816839. [Google Scholar] [CrossRef]
- Kennedy, A.; Fearon, U.; Veale, D.J.; Godson, C. Macrophages in Synovial Inflammation. Front. Immunol. 2011, 2, 52. [Google Scholar] [CrossRef]
- Macfarlane, E.; Seibel, M.J.; Zhou, H. Arthritis and the Role of Endogenous Glucocorticoids. Bone Res. 2020, 8, 33. [Google Scholar] [CrossRef]
- Zheng, Y.; Xiao, L.; Yu, C.; Jin, P.; Qin, D.; Xu, Y.; Yin, J.; Liu, Z.; Du, Q. Enhanced Antiarthritic Efficacy by Nanoparticles of (−)-Epigallocatechin Gallate–Glucosamine–Casein. J. Agric. Food Chem. 2019, 67, 6476–6486. [Google Scholar] [CrossRef]
- Vyawahare, A.; Prakash, R.; Jori, C.; Ali, A.; Raza, S.; Khan, R. Caffeic Acid Modified Nanomicelles Inhibit Articular Cartilage Deterioration and Reduce Disease Severity in Experimental Inflammatory Arthritis. ACS Nano 2022, 16, 18579–18591. [Google Scholar] [CrossRef]
- Munir, A.; Muhammad, F.; Zaheer, Y.; Ali, A.; Iqbal, M.; Rehman, M.; Munir, M.U.; Akhtar, B.; Webster, T.J.; Sharif, A.; et al. Synthesis of Naringenin Loaded Lipid Based Nanocarriers and Their In-Vivo Therapeutic Potential in a Rheumatoid Arthritis Model. J. Drug Deliv. Sci. Technol. 2021, 66, 102854. [Google Scholar] [CrossRef]
- Mohanty, S.; Sahoo, A.K.; Konkimalla, V.B.; Pal, A.; Si, S.C. Naringin in Combination with Isothiocyanates as Liposomal Formulations Potentiates the Anti-Inflammatory Activity in Different Acute and Chronic Animal Models of Rheumatoid Arthritis. ACS Omega 2020, 5, 28319–28332. [Google Scholar] [CrossRef]
- Mohanty, S.; Konkimalla, V.B.; Pal, A.; Sharma, T.; Si, S.C. Naringin as Sustained Delivery Nanoparticles Ameliorates the Anti-Inflammatory Activity in a Freund’s Complete Adjuvant-Induced Arthritis Model. ACS Omega 2021, 6, 28630–28641. [Google Scholar] [CrossRef]
- Zhang, G.; Sun, G.; Guan, H.; Li, M.; Liu, Y.; Tian, B.; He, Z.; Fu, Q. Naringenin Nanocrystals for Improving Anti-Rheumatoid Arthritis Activity. Asian J. Pharm. Sci. 2021, 16, 816–825. [Google Scholar] [CrossRef]
- Chen, X.; Zhu, X.; Ma, L.; Lin, A.; Gong, Y.; Yuan, G.; Liu, J. A Core–Shell Structure QRu-PLGA-RES-DS NP Nanocomposite with Photothermal Response-Induced M2 Macrophage Polarization for Rheumatoid Arthritis Therapy. Nanoscale 2019, 11, 18209–18223. [Google Scholar] [CrossRef]
- Kamel, R.; Abbas, H.; Shaffie, N.M. Development and Evaluation of PLA-Coated Co-Micellar Nanosystem of Resveratrol for the Intra-Articular Treatment of Arthritis. Int. J. Pharm. 2019, 569, 118560. [Google Scholar] [CrossRef]
- Poonia, N.; Lather, V.; Kaur, B.; Kirthanashri, S.V.; Pandita, D. Optimization and Development of Methotrexate- and Resveratrol-Loaded Nanoemulsion Formulation Using Box–Behnken Design for Rheumatoid Arthritis. Assay Drug Dev. Technol. 2020, 18, 356–368. [Google Scholar] [CrossRef]
- Cui, N.; Xu, Z.; Zhao, X.; Yuan, M.; Pan, L.; Lu, T.; Du, A.; Qin, L. In Vivo Effect of Resveratrol-Cellulose Aerogel Drug Delivery System to Relieve Inflammation on Sports Osteoarthritis. Gels 2022, 8, 544. [Google Scholar] [CrossRef]
- Arora, R.; Kuhad, A.; Kaur, I.P.; Chopra, K. Curcumin Loaded Solid Lipid Nanoparticles Ameliorate Adjuvant-Induced Arthritis in Rats. Eur. J. Pain 2015, 19, 940–952. [Google Scholar] [CrossRef]
- Coradini, K.; Friedrich, R.B.; Fonseca, F.N.; Vencato, M.S.; Andrade, D.F.; Oliveira, C.M.; Battistel, A.P.; Guterres, S.S.; da Rocha, M.I.U.M.; Pohlmann, A.R.; et al. A Novel Approach to Arthritis Treatment Based on Resveratrol and Curcumin Co-Encapsulated in Lipid-Core Nanocapsules: In Vivo Studies. Eur. J. Pharm. Sci. 2015, 78, 163–170. [Google Scholar] [CrossRef]
- Yan, F.; Li, H.; Zhong, Z.; Zhou, M.; Lin, Y.; Tang, C.; Li, C. Co-Delivery of Prednisolone and Curcumin in Human Serum Albumin Nanoparticles for Effective Treatment of Rheumatoid Arthritis. Int. J. Nanomed. 2019, 14, 9113–9125. [Google Scholar] [CrossRef]
- Naz, Z.; Ahmad, F.J. Curcumin-Loaded Colloidal Carrier System: Formulation Optimization, Mechanistic Insight, Ex Vivo and in Vivo Evaluation. Int. J. Nanomed. 2015, 10, 4293–4307. [Google Scholar] [CrossRef]
- Dewangan, A.K.; Perumal, Y.; Pavurala, N.; Chopra, K.; Mazumder, S. Preparation, Characterization and Anti-Inflammatory Effects of Curcumin Loaded Carboxymethyl Cellulose Acetate Butyrate Nanoparticles on Adjuvant Induced Arthritis in Rats. J. Drug Deliv. Sci. Tech. 2017, 41, 269–279. [Google Scholar] [CrossRef]
- Fan, Z.; Li, J.; Liu, J.; Jiao, H.; Liu, B. Anti-Inflammation and Joint Lubrication Dual Effects of a Novel Hyaluronic Acid/Curcumin Nanomicelle Improve the Efficacy of Rheumatoid Arthritis Therapy. ACS Appl. Mater. Interfaces 2018, 10, 23595–23604. [Google Scholar] [CrossRef]
- Kang, C.; Jung, E.; Hyeon, H.; Seon, S.; Lee, D. Acid-Activatable Polymeric Curcumin Nanoparticles as Therapeutic Agents for Osteoarthritis. Nanomedicine 2020, 23, 102104. [Google Scholar] [CrossRef]
- Chamani, S.; Bianconi, V.; Tasbandi, A.; Pirro, M.; Barreto, G.E.; Jamialahmadi, T.; Sahebkar, A. Resolution of Inflammation in Neurodegenerative Diseases: The Role of Resolvins. Mediat. Inflamm. 2020, 2020, e3267172. [Google Scholar] [CrossRef]
- Wang, R.-X.; Zhou, M.; Ma, H.-L.; Qiao, Y.-B.; Li, Q.-S. The Role of Chronic Inflammation in Various Diseases and Anti-Inflammatory Therapies Containing Natural Products. Chem. Med. Chem. 2021, 16, 1576–1592. [Google Scholar] [CrossRef]
- Forloni, G.; La Vitola, P.; Cerovic, M.; Balducci, C. Inflammation and Parkinson’s Disease Pathogenesis: Mechanisms and Therapeutic Insight. Prog. Mol. Biol. Transl. Sci. 2021, 177, 175–202. [Google Scholar] [CrossRef]
- Singh, N.A.; Bhardwaj, V.; Ravi, C.; Ramesh, N.; Mandal, A.K.A.; Khan, Z.A. EGCG Nanoparticles Attenuate Aluminum Chloride Induced Neurobehavioral Deficits, Beta Amyloid and Tau Pathology in a Rat Model of Alzheimer’s Disease. Front. Aging Neurosci. 2018, 10, 244. [Google Scholar] [CrossRef]
- Cano, A.; Ettcheto, M.; Chang, J.-H.; Barroso, E.; Espina, M.; Kühne, B.A.; Barenys, M.; Auladell, C.; Folch, J.; Souto, E.B.; et al. Dual-Drug Loaded Nanoparticles of Epigallocatechin-3-Gallate (EGCG)/Ascorbic Acid Enhance Therapeutic Efficacy of EGCG in a APPswe/PS1dE9 Alzheimer’s Disease Mice Model. J. Control. Release 2019, 301, 62–75. [Google Scholar] [CrossRef]
- Lv, L.; Yang, F.; Li, H.; Yuan, J. Brain-Targeted Co-Delivery of β-Amyloid Converting Enzyme 1 ShRNA and Epigallocatechin-3-Gallate by Multifunctional Nanocarriers for Alzheimer’s Disease Treatment. IUBMB Life 2020, 72, 1819–1829. [Google Scholar] [CrossRef]
- Li, Y.; Chen, Z.; Lu, Z.; Yang, Q.; Liu, L.; Jiang, Z.; Zhang, L.; Zhang, X.; Qing, H. “Cell-Addictive” Dual-Target Traceable Nanodrug for Parkinson’s Disease Treatment via Flotillins Pathway. Theranostics 2018, 8, 5469–5481. [Google Scholar] [CrossRef]
- Zhang, J.; Zhou, X.; Yu, Q.; Yang, L.; Sun, D.; Zhou, Y.; Liu, J. Epigallocatechin-3-Gallate (EGCG)-Stabilized Selenium Nanoparticles Coated with Tet-1 Peptide To Reduce Amyloid-β Aggregation and Cytotoxicity. ACS Appl. Mater. Interfaces 2014, 6, 8475–8487. [Google Scholar] [CrossRef]
- Wang, Y.; Luo, W.; Lin, F.; Liu, W.; Gu, R. Epigallocatechin-3-Gallate Selenium Nanoparticles for Neuroprotection by Scavenging Reactive Oxygen Species and Reducing Inflammation. Front. Bioeng. Biotechnol. 2022, 10, 989602. [Google Scholar] [CrossRef]
- Pandian, S.R.K.; Pavadai, P.; Vellaisamy, S.; Ravishankar, V.; Palanisamy, P.; Sundar, L.M.; Chandramohan, V.; Sankaranarayanan, M.; Panneerselvam, T.; Kunjiappan, S. Formulation and Evaluation of Rutin-Loaded Solid Lipid Nanoparticles for the Treatment of Brain Tumor. Naunyn Schmiedebergs Arch. Pharmacol. 2021, 394, 735–749. [Google Scholar] [CrossRef]
- Ahmad, H.; Arya, A.; Agrawal, S.; Mall, P.; Samuel, S.S.; Sharma, K.; Singh, P.K.; Singh, S.K.; Valicherla, G.R.; Mitra, K.; et al. Rutin Phospholipid Complexes Confer Neuro-Protection in Ischemic-Stroke Rats. RSC Adv. 2016, 6, 96445–96454. [Google Scholar] [CrossRef]
- Hu, B.; Dai, F.; Fan, Z.; Ma, G.; Tang, Q.; Zhang, X. Nanotheranostics: Congo Red/Rutin-MNPs with Enhanced Magnetic Resonance Imaging and H2O2-Responsive Therapy of Alzheimer’s Disease in APPswe/PS1dE9 Transgenic Mice. Adv. Mat. 2015, 27, 5499–5505. [Google Scholar] [CrossRef]
- Rahman, M.; Kumar, V. Apigenin Loaded Phospholipid Based Nanoemulsion in Therapeutics of Parkinson’s Disease via Attenuation of Oxidative Stress and Upregulation of Dopamine. J. Neur. Sci. 2019, 405, 247. [Google Scholar] [CrossRef]
- Md, S.; Gan, S.Y.; Haw, Y.H.; Ho, C.L.; Wong, S.; Choudhury, H. In Vitro Neuroprotective Effects of Naringenin Nanoemulsion against β-Amyloid Toxicity through the Regulation of Amyloidogenesis and Tau Phosphorylation. Int. J. Biol. Macromol. 2018, 118, 1211–1219. [Google Scholar] [CrossRef]
- Gaba, B.; Khan, T.; Haider, M.F.; Alam, T.; Baboota, S.; Parvez, S.; Ali, J. Vitamin E Loaded Naringenin Nanoemulsion via Intranasal Delivery for the Management of Oxidative Stress in a 6-OHDA Parkinson’s Disease Model. Biomed. Res. Int. 2019, 2019, e2382563. [Google Scholar] [CrossRef]
- Ahmad, A.; Fauzia, E.; Kumar, M.; Mishra, R.K.; Kumar, A.; Khan, M.A.; Raza, S.S.; Khan, R. Gelatin-Coated Polycaprolactone Nanoparticle-Mediated Naringenin Delivery Rescue Human Mesenchymal Stem Cells from Oxygen Glucose Deprivation-Induced Inflammatory Stress. ACS Biomater. Sci. Eng. 2019, 5, 683–695. [Google Scholar] [CrossRef]
- Zhao, Y.; Li, D.; Zhu, Z.; Sun, Y. Improved Neuroprotective Effects of Gallic Acid-Loaded Chitosan Nanoparticles Against Ischemic Stroke. Rejuv. Res. 2020, 23, 284–292. [Google Scholar] [CrossRef]
- Frozza, R.L.; Bernardi, A.; Hoppe, J.B.; Meneghetti, A.B.; Battastini, A.M.O.; Pohlmann, A.R.; Guterres, S.S.; Salbego, C. Lipid-Core Nanocapsules Improve the Effects of Resveratrol Against Aβ-Induced Neuroinflammation. J. Biomed. Nanotech. 2013, 9, 2086–2104. [Google Scholar] [CrossRef]
- Frozza, R.L.; Bernardi, A.; Hoppe, J.B.; Meneghetti, A.B.; Matté, A.; Battastini, A.M.O.; Pohlmann, A.R.; Guterres, S.S.; Salbego, C. Neuroprotective Effects of Resveratrol Against Aβ Administration in Rats Are Improved by Lipid-Core Nanocapsules. Mol. Neurobiol. 2013, 47, 1066–1080. [Google Scholar] [CrossRef]
- Da Rocha Lindner, G.; Bonfanti Santos, D.; Colle, D.; Gasnhar Moreira, E.L.; Daniel Prediger, R.; Farina, M.; Khalil, N.M.; Mara Mainardes, R. Improved Neuroprotective Effects of Resveratrol-Loaded Polysorbate 80-Coated Poly(Lactide) Nanoparticles in MPTP-Induced Parkinsonism. Nanomedicine 2015, 10, 1127–1138. [Google Scholar] [CrossRef]
- Loureiro, J.A.; Andrade, S.; Duarte, A.; Neves, A.R.; Queiroz, J.F.; Nunes, C.; Sevin, E.; Fenart, L.; Gosselet, F.; Coelho, M.A.N.; et al. Resveratrol and Grape Extract-Loaded Solid Lipid Nanoparticles for the Treatment of Alzheimer’s Disease. Molecules 2017, 22, 277. [Google Scholar] [CrossRef]
- Li, C.; Wang, N.; Zheng, G.; Yang, L. Oral Administration of Resveratrol-Selenium-Peptide Nanocomposites Alleviates Alzheimer’s Disease-like Pathogenesis by Inhibiting Aβ Aggregation and Regulating Gut Microbiota. ACS Appl. Mater. Interfaces 2021, 13, 46406–46420. [Google Scholar] [CrossRef]
- Abozaid, O.A.R.; Sallam, M.W.; El-Sonbaty, S.; Aziza, S.; Emad, B.; Ahmed, E.S.A. Resveratrol-Selenium Nanoparticles Alleviate Neuroinflammation and Neurotoxicity in a Rat Model of Alzheimer’s Disease by Regulating Sirt1/MiRNA-134/GSK3β Expression. Biol. Trace Elem. Res. 2022, 200, 5104–5114. [Google Scholar] [CrossRef]
- Mourtas, S.; Lazar, A.N.; Markoutsa, E.; Duyckaerts, C.; Antimisiaris, S.G. Multifunctional Nanoliposomes with Curcumin–Lipid Derivative and Brain Targeting Functionality with Potential Applications for Alzheimer Disease. Eur. J. Med. Chem. 2014, 80, 175–183. [Google Scholar] [CrossRef]
- Barbara, R.; Belletti, D.; Pederzoli, F.; Masoni, M.; Keller, J.; Ballestrazzi, A.; Vandelli, M.A.; Tosi, G.; Grabrucker, A.M. Novel Curcumin Loaded Nanoparticles Engineered for Blood-Brain Barrier Crossing and Able to Disrupt Abeta Aggregates. Int. J. Pharm. 2017, 526, 413–424. [Google Scholar] [CrossRef]
- Huang, N.; Lu, S.; Liu, X.-G.; Zhu, J.; Wang, Y.-J.; Liu, R.-T. PLGA Nanoparticles Modified with a BBB-Penetrating Peptide Co-Delivering Aβ; Generation Inhibitor and Curcumin Attenuate Memory Deficits and Neuropathology in Alzheimer’s Disease Mice. Oncotarget 2017, 8, 81001–81013. [Google Scholar] [CrossRef]
- Yang, R.; Zheng, Y.; Wang, Q.; Zhao, L. Curcumin-Loaded Chitosan–Bovine Serum Albumin Nanoparticles Potentially Enhanced Aβ 42 Phagocytosis and Modulated Macrophage Polarization in Alzheimer’s Disease. Nanoscale Res. Lett. 2018, 13, 330. [Google Scholar] [CrossRef]
- Maiti, P.; Paladugu, L.; Dunbar, G.L. Solid Lipid Curcumin Particles Provide Greater Anti-Amyloid, Anti-Inflammatory and Neuroprotective Effects than Curcumin in the 5xFAD Mouse Model of Alzheimer’s Disease. BMC Neurosci. 2018, 19, 7. [Google Scholar] [CrossRef]
- Huo, X.; Zhang, Y.; Jin, X.; Li, Y.; Zhang, L. A Novel Synthesis of Selenium Nanoparticles Encapsulated PLGA Nanospheres with Curcumin Molecules for the Inhibition of Amyloid β Aggregation in Alzheimer’s Disease. J Photochem. Photobiol. B 2019, 190, 98–102. [Google Scholar] [CrossRef]
- Kundu, P.; Das, M.; Tripathy, K.; Sahoo, S.K. Delivery of Dual Drug Loaded Lipid Based Nanoparticles across the Blood–Brain Barrier Impart Enhanced Neuroprotection in a Rotenone Induced Mouse Model of Parkinson’s Disease. ACS Chem. Neurosci. 2016, 7, 1658–1670. [Google Scholar] [CrossRef]
- Saalbach, A.; Kunz, M. Impact of Chronic Inflammation in Psoriasis on Bone Metabolism. Front. Immunol. 2022, 13, 925503. [Google Scholar] [CrossRef]
- Tashiro, T.; Sawada, Y. Psoriasis and Systemic Inflammatory Disorders. Int. J. Mol. Sci. 2022, 23, 4457. [Google Scholar] [CrossRef]
- Yang, S.-C.; Alalaiwe, A.; Lin, Z.-C.; Lin, Y.-C.; Aljuffali, I.A.; Fang, J.-Y. Anti-Inflammatory MicroRNAs for Treating Inflammatory Skin Diseases. Biomolecules 2022, 12, 1072. [Google Scholar] [CrossRef]
- Abdel-Mottaleb, M.M.; Try, C.; Pellequer, Y.; Lamprecht, A. Nanomedicine Strategies for Targeting Skin Inflammation. Nanomedicine 2014, 9, 1727–1743. [Google Scholar] [CrossRef]
- Yang, G.; Seok, J.K.; Kang, H.C.; Cho, Y.-Y.; Lee, H.S.; Lee, J.Y. Skin Barrier Abnormalities and Immune Dysfunction in Atopic Dermatitis. Int. J. Mol. Sci. 2020, 21, 2867. [Google Scholar] [CrossRef]
- Chamcheu, J.C.; Siddiqui, I.A.; Adhami, V.M.; Esnault, S.; Bharali, D.J.; Babatunde, A.S.; Adame, S.; Massey, R.J.; Wood, G.S.; Longley, B.J.; et al. Chitosan-Based Nanoformulated (−)-Epigallocatechin-3-Gallate (EGCG) Modulates Human Keratinocyte-Induced Responses and Alleviates Imiquimod-Induced Murine Psoriasiform Dermatitis. Int. J Nanomed. 2018, 13, 4189–4206. [Google Scholar] [CrossRef]
- Han, M.; Wang, X.; Wang, J.; Lang, D.; Xia, X.; Jia, Y.; Chen, Y. Ameliorative Effects of Epigallocatechin-3-Gallate Nanoparticles on 2,4-Dinitrochlorobenzene Induced Atopic Dermatitis: A Potential Mechanism of Inflammation-Related Necroptosis. Front. Nutr. 2022, 9, 953646. [Google Scholar] [CrossRef]
- Sun, M.; Xie, Q.; Cai, X.; Liu, Z.; Wang, Y.; Dong, X.; Xu, Y. Preparation and Characterization of Epigallocatechin Gallate, Ascorbic Acid, Gelatin, Chitosan Nanoparticles and Their Beneficial Effect on Wound Healing of Diabetic Mice. Int. J. Biol. Macromol. 2020, 148, 777–784. [Google Scholar] [CrossRef]
- Kar, A.K.; Singh, A.; Dhiman, N.; Purohit, M.P.; Jagdale, P.; Kamthan, M.; Singh, D.; Kumar, M.; Ghosh, D.; Patnaik, S. Polymer-Assisted In Situ Synthesis of Silver Nanoparticles with Epigallocatechin Gallate (EGCG) Impregnated Wound Patch Potentiate Controlled Inflammatory Responses for Brisk Wound Healing. Int. J. Nanomed. 2019, 14, 9837–9854. [Google Scholar] [CrossRef]
- Li, J.; Ni, W.; Aisha, M.; Zhang, J.; Sun, M. A Rutin Nanocrystal Gel as an Effective Dermal Delivery System for Enhanced Anti-Photoaging Application. Drug. Dev. Ind. Pharm. 2021, 47, 429–439. [Google Scholar] [CrossRef]
- Cristiano, M.C.; Barone, A.; Mancuso, A.; Torella, D.; Paolino, D. Rutin-Loaded Nanovesicles for Improved Stability and Enhanced Topical Efficacy of Natural Compound. J. Funct. Biomater. 2021, 12, 74. [Google Scholar] [CrossRef]
- Shen, L.-N.; Zhang, Y.-T.; Wang, Q.; Xu, L.; Feng, N.-P. Enhanced in Vitro and in Vivo Skin Deposition of Apigenin Delivered Using Ethosomes. Int. J. Pharm. 2014, 460, 280–288. [Google Scholar] [CrossRef]
- Pleguezuelos-Villa, M.; Mir-Palomo, S.; Díez-Sales, O.; Buso, M.A.O.V.; Sauri, A.R.; Nácher, A. A Novel Ultradeformable Liposomes of Naringin for Anti-Inflammatory Therapy. Colloids Surf. B Biointerfaces 2018, 162, 265–270. [Google Scholar] [CrossRef]
- Akrawi, S.H.; Gorain, B.; Nair, A.B.; Choudhury, H.; Pandey, M.; Shah, J.N.; Venugopala, K.N. Development and Optimization of Naringenin-Loaded Chitosan-Coated Nanoemulsion for Topical Therapy in Wound Healing. Pharmaceutics 2020, 12, 893. [Google Scholar] [CrossRef]
- Caddeo, C.; Manca, M.L.; Matos, M.; Gutierrez, G.; Díez-Sales, O.; Peris, J.E.; Usach, I.; Fernàndez-Busquets, X.; Fadda, A.M.; Manconi, M. Functional Response of Novel Bioprotective Poloxamer-Structured Vesicles on Inflamed Skin. Nanomedicine 2017, 13, 1127–1136. [Google Scholar] [CrossRef]
- Shandil, A.; Yadav, M.; Sharma, N.; Nagpal, K.; Jindal, D.K.; Deep, A.; Kumar, S. Targeting Keratinocyte Hyperproliferation, Inflammation, Oxidative Species and Microbial Infection by Biological Macromolecule-Based Chitosan Nanoparticle-Mediated Gallic Acid–Rutin Combination for the Treatment of Psoriasis. Polym. Bull. 2020, 77, 4713–4738. [Google Scholar] [CrossRef]
- Thi, P.L.; Lee, Y.; Tran, D.L.; Thi, T.T.H.; Kang, J.I.; Park, K.M.; Park, K.D. In Situ Forming and Reactive Oxygen Species-Scavenging Gelatin Hydrogels for Enhancing Wound Healing Efficacy. Acta Biomater. 2020, 103, 142–152. [Google Scholar] [CrossRef]
- Wang, X.-C.; Huang, H.-B.; Gong, W.; He, W.-Y.; Li, X.; Xu, Y.; Gong, X.-J.; Hu, J.-N. Resveratrol Triggered the Quick Self-Assembly of Gallic Acid into Therapeutic Hydrogels for Healing of Bacterially Infected Wounds. Biomacromolecules 2022, 23, 1680–1692. [Google Scholar] [CrossRef]
- Oh, G.-W.; Ko, S.-C.; Je, J.-Y.; Kim, Y.-M.; Oh, J.; Jung, W.-K. Fabrication, Characterization and Determination of Biological Activities of Poly(ε-Caprolactone)/Chitosan-Caffeic Acid Composite Fibrous Mat for Wound Dressing Application. Int. J. Biol. Macromol. 2016, 93, 1549–1558. [Google Scholar] [CrossRef]
- Kaya, S.; Yilmaz, D.E.; Akmayan, I.; Egri, O.; Arasoglu, T.; Derman, S. Caffeic Acid Phenethyl Ester Loaded Electrospun Nanofibers for Wound Dressing Application. J. Pharm. Sci. 2022, 111, 734–742. [Google Scholar] [CrossRef]
- Caddeo, C.; Nacher, A.; Vassallo, A.; Armentano, M.F.; Pons, R.; Fernàndez-Busquets, X.; Carbone, C.; Valenti, D.; Fadda, A.M.; Manconi, M. Effect of Quercetin and Resveratrol Co-Incorporated in Liposomes against Inflammatory/Oxidative Response Associated with Skin Cancer. Int. J. Pharm. 2016, 513, 153–163. [Google Scholar] [CrossRef]
- Caldas, A.R.; Catita, J.; Machado, R.; Ribeiro, A.; Cerqueira, F.; Horta, B.; Medeiros, R.; Lúcio, M.; Lopes, C.M. Omega-3- and Resveratrol-Loaded Lipid Nanosystems for Potential Use as Topical Formulations in Autoimmune, Inflammatory, and Cancerous Skin Diseases. Pharmaceutics 2021, 13, 1202. [Google Scholar] [CrossRef]
- Zhao, C.-C.; Zhu, L.; Wu, Z.; Yang, R.; Xu, N.; Liang, L. Resveratrol-Loaded Peptide-Hydrogels Inhibit Scar Formation in Wound Healing through Suppressing Inflammation. Regen. Biomater. 2020, 7, 99–107. [Google Scholar] [CrossRef]
- Li, X.; Chen, S.; Zhang, B.; Li, M.; Diao, K.; Zhang, Z.; Li, J.; Xu, Y.; Wang, X.; Chen, H. In Situ Injectable Nano-Composite Hydrogel Composed of Curcumin, N,O-Carboxymethyl Chitosan and Oxidized Alginate for Wound Healing Application. Int. J. Pharm. 2012, 437, 110–119. [Google Scholar] [CrossRef]
- Gong, C.; Wu, Q.; Wang, Y.; Zhang, D.; Luo, F.; Zhao, X.; Wei, Y.; Qian, Z. A Biodegradable Hydrogel System Containing Curcumin Encapsulated in Micelles for Cutaneous Wound Healing. Biomaterials 2013, 34, 6377–6387. [Google Scholar] [CrossRef]
- Alibolandi, M.; Mohammadi, M.; Taghdisi, S.M.; Abnous, K.; Ramezani, M. Synthesis and Preparation of Biodegradable Hybrid Dextran Hydrogel Incorporated with Biodegradable Curcumin Nanomicelles for Full Thickness Wound Healing. Int. J. Pharm. 2017, 532, 466–477. [Google Scholar] [CrossRef]
- Sun, L.; Liu, Z.; Wang, L.; Cun, D.; Tong, H.H.Y.; Yan, R.; Chen, X.; Wang, R.; Zheng, Y. Enhanced Topical Penetration, System Exposure and Anti-Psoriasis Activity of Two Particle-Sized, Curcumin-Loaded PLGA Nanoparticles in Hydrogel. J. Control. Release 2017, 254, 44–54. [Google Scholar] [CrossRef]
- Dai, X.; Liu, J.; Zheng, H.; Wichmann, J.; Hopfner, U.; Sudhop, S.; Prein, C.; Shen, Y.; Machens, H.-G.; Schilling, A.F. Nano-Formulated Curcumin Accelerates Acute Wound Healing through Dkk-1-Mediated Fibroblast Mobilization and MCP-1-Mediated Anti-Inflammation. NPG Asia Mater. 2017, 9, e368. [Google Scholar] [CrossRef]
- Bajpai, S.K.; Ahuja, S.; Chand, N.; Bajpai, M. Nano Cellulose Dispersed Chitosan Film with Ag NPs/Curcumin: An in Vivo Study on Albino Rats for Wound Dressing. Int. J. Biol. Macromol. 2017, 104, 1012–1019. [Google Scholar] [CrossRef]
- Lee, H.-J.; Jeong, M.; Na, Y.-G.; Kim, S.-J.; Lee, H.-K.; Cho, C.-W. An EGF- and Curcumin-Co-Encapsulated Nanostructured Lipid Carrier Accelerates Chronic-Wound Healing in Diabetic Rats. Molecules 2020, 25, 4610. [Google Scholar] [CrossRef]
- Mirzahosseinipour, M.; Khorsandi, K.; Hosseinzadeh, R.; Ghazaeian, M.; Shahidi, F.K. Antimicrobial Photodynamic and Wound Healing Activity of Curcumin Encapsulated in Silica Nanoparticles. Photodiagnosis Photodyn. Ther. 2020, 29, 101639. [Google Scholar] [CrossRef]
- Graham, D.B.; Xavier, R.J. Pathway Paradigms Revealed from the Genetics of Inflammatory Bowel Disease. Nature 2020, 578, 527–539. [Google Scholar] [CrossRef]
- Papoutsopoulou, S.; Burkitt, M.D.; Bergey, F.; England, H.; Hough, R.; Schmidt, L.; Spiller, D.G.; White, M.H.R.; Paszek, P.; Jackson, D.A.; et al. Macrophage-Specific NF-ΚB Activation Dynamics Can Segregate Inflammatory Bowel Disease Patients. Front. Immunol. 2019, 10, 2168. [Google Scholar] [CrossRef]
- Haep, L.; Britzen-Laurent, N.; Weber, T.G.; Naschberger, E.; Schaefer, A.; Kremmer, E.; Foersch, S.; Vieth, M.; Scheuer, W.; Wirtz, S.; et al. Interferon Gamma Counteracts the Angiogenic Switch and Induces Vascular Permeability in Dextran Sulfate Sodium Colitis in Mice. Inflamm. Bowel. Dis. 2015, 21, 2360–2371. [Google Scholar] [CrossRef]
- Jovani, M.; Fiorino, G.; Danese, S. Anti-IL-13 in Inflammatory Bowel Disease: From the Bench to the Bedside. Curr. Drug. Targets 2013, 14, 1444–1452. [Google Scholar] [CrossRef]
- Shen, W.; Wang, Q.; Shen, Y.; Gao, X.; Li, L.; Yan, Y.; Wang, H.; Cheng, Y. Green Tea Catechin Dramatically Promotes RNAi Mediated by Low-Molecular-Weight Polymers. ACS Cent. Sci. 2018, 4, 1326–1333. [Google Scholar] [CrossRef]
- Gou, S.; Chen, Q.; Liu, Y.; Zeng, L.; Song, H.; Xu, Z.; Kang, Y.; Li, C.; Xiao, B. Green Fabrication of Ovalbumin Nanoparticles as Natural Polyphenol Carriers for Ulcerative Colitis Therapy. ACS Sustain. Chem. Eng. 2018, 6, 12658–12667. [Google Scholar] [CrossRef]
- Guo, Z.; Bai, G.; Zhan, X.; Zhuo, K.; Wang, J.; Wang, Y. Supramolecular Vector/Drug Coassemblies of Polyglycerol Dendrons and Rutin Enhance the PH Response. Langmuir 2022, 38, 3392–3402. [Google Scholar] [CrossRef]
- Lv, F.; Zhang, Y.; Peng, Q.; Zhao, X.; Hu, D.; Wen, J.; Liu, K.; Li, R.; Wang, K.; Sun, J. Apigenin-Mn(II) Loaded Hyaluronic Acid Nanoparticles for Ulcerative Colitis Therapy in Mice. Front. Chem. 2022, 10, 969962. [Google Scholar] [CrossRef]
- Priyadarshi, K.; Shirsath, K.; Waghela, N.B.; Sharma, A.; Kumar, A.; Pathak, C. Surface Modified PAMAM Dendrimers with Gallic Acid Inhibit, Cell Proliferation, Cell Migration and Inflammatory Response to Augment Apoptotic Cell Death in Human Colon Carcinoma Cells. J. Biomol. Struct. Dyn. 2021, 39, 6853–6869. [Google Scholar] [CrossRef]
- Wang, J.; Tao, Z.; Tian, T.; Qiu, J.; Qian, H.; Zha, Z.; Miao, Z.; Ma, Y.; Wang, H. Polyoxometalate Nanoclusters: A Potential Preventative and Therapeutic Drug for Inflammatory Bowel Disease. Chem. Eng. J. 2021, 416, 129137. [Google Scholar] [CrossRef]
- Tambuwala, M.M.; Khan, M.N.; Thompson, P.; McCarron, P.A. Albumin Nano-Encapsulation of Caffeic Acid Phenethyl Ester and Piceatannol Potentiated Its Ability to Modulate HIF and NF-KB Pathways and Improves Therapeutic Outcome in Experimental Colitis. Drug Deliv. Transl. Res. 2019, 9, 14–24. [Google Scholar] [CrossRef]
- Pujara, N.; Wong, K.Y.; Qu, Z.; Wang, R.; Moniruzzaman, M.; Rewatkar, P.; Kumeria, T.; Ross, B.P.; McGuckin, M.; Popat, A. Oral Delivery of β-Lactoglobulin-Nanosphere-Encapsulated Resveratrol Alleviates Inflammation in Winnie Mice with Spontaneous Ulcerative Colitis. Mol. Pharm. 2021, 18, 627–640. [Google Scholar] [CrossRef]
- Siu, F.Y.; Ye, S.; Lin, H.; Li, S. Galactosylated PLGA Nanoparticles for the Oral Delivery of Resveratrol: Enhanced Bioavailability and in Vitro Anti-Inflammatory Activity. Int. J. Nanomed. 2018, 13, 4133–4144. [Google Scholar] [CrossRef] [PubMed]
- Rachmawati, H.; Pradana, A.T.; Safitri, D.; Adnyana, I.K. Multiple Functions of D-α-Tocopherol Polyethylene Glycol 1000 Succinate (TPGS) as Curcumin Nanoparticle Stabilizer: In Vivo Kinetic Profile and Anti-Ulcerative Colitis Analysis in Animal Model. Pharmaceutics 2017, 9, 24. [Google Scholar] [CrossRef]
- Oshi, M.A.; Lee, J.; Naeem, M.; Hasan, N.; Kim, J.; Kim, H.J.; Lee, E.H.; Jung, Y.; Yoo, J.-W. Curcumin Nanocrystal/PH-Responsive Polyelectrolyte Multilayer Core–Shell Nanoparticles for Inflammation-Targeted Alleviation of Ulcerative Colitis. Biomacromolecules 2020, 21, 3571–3581. [Google Scholar] [CrossRef] [PubMed]
- Kelly, T.; Yang, W.; Chen, C.-S.; Reynolds, K.; He, J. Global Burden of Obesity in 2005 and Projections to 2030. Int. J. Obes. 2008, 32, 1431–1437. [Google Scholar] [CrossRef]
- Tsalamandris, S.; Antonopoulos, A.S.; Oikonomou, E.; Papamikroulis, G.-A.; Vogiatzi, G.; Papaioannou, S.; Deftereos, S.; Tousoulis, D. The Role of Inflammation in Diabetes: Current Concepts and Future Perspectives. Eur. Cardiol. 2019, 14, 50–59. [Google Scholar] [CrossRef]
- Feuerer, M.; Shen, Y.; Littman, D.R.; Benoist, C.; Mathis, D. How Punctual Ablation of Regulatory T Cells Unleashes an Autoimmune Lesion within the Pancreatic Islets. Immunity 2009, 31, 654–664. [Google Scholar] [CrossRef]
- Laveti, D.; Kumar, M.; Hemalatha, R.; Sistla, R.; Naidu, V.G.M.; Talla, V.; Verma, V.; Kaur, N.; Nagpal, R. Anti-Inflammatory Treatments for Chronic Diseases: A Review. Inflamm. Allergy Drug Targets. 2013, 12, 349–361. [Google Scholar] [CrossRef]
- Divella, R.; Gadaleta Caldarola, G.; Mazzocca, A. Chronic Inflammation in Obesity and Cancer Cachexia. J. Clin. Med. 2022, 11, 2191. [Google Scholar] [CrossRef]
- Shoelson, S.E.; Herrero, L.; Naaz, A. Obesity, Inflammation, and Insulin Resistance. Gastroenterology 2007, 132, 2169–2180. [Google Scholar] [CrossRef]
- Zagury, Y.; Chen, S.; Edelman, R.; Karnieli, E.; Livney, Y.D. β-Lactoglobulin Delivery System for Enhancing EGCG Biological Efficacy in HFD Obesity Mice Model. J. Funct. Foods 2019, 59, 362–370. [Google Scholar] [CrossRef]
- Zhang, X.-Z.; Guan, J.; Cai, S.-L.; Du, Q.; Guo, M.-L. Polymeric In Situ Hydrogel Implant of Epigallocatechin Gallate (EGCG) for Prolonged and Improved Antihyperlipidemic and Anti-Obesity Activity: Preparation and Characterization. J. Biomater. Tissue Eng. 2015, 5, 813–817. [Google Scholar] [CrossRef]
- Bhattacherjee, A.; Chakraborti, A.S. Argpyrimidine-Tagged Rutin-Encapsulated Biocompatible (Ethylene Glycol Dimers) Nanoparticles: Application for Targeted Drug Delivery in Experimental Diabetes (Part 2). Int. J. Pharm. 2017, 528, 8–17. [Google Scholar] [CrossRef]
- Amjadi, S.; Shahnaz, F.; Shokouhi, B.; Azarmi, Y.; Siahi-Shadbad, M.; Ghanbarzadeh, S.; Kouhsoltani, M.; Ebrahimi, A.; Hamishehkar, H. Nanophytosomes for Enhancement of Rutin Efficacy in Oral Administration for Diabetes Treatment in Streptozotocin-Induced Diabetic Rats. Int. J. Pharm. 2021, 610, 121208. [Google Scholar] [CrossRef]
- Zaghloul, R.A.; Abdelghany, A.M.; Samra, Y.A. Rutin and Selenium Nanoparticles Protected against STZ-Induced Diabetic Nephropathy in Rats through Downregulating Jak-2/Stat3 Pathway and Upregulating Nrf-2/HO-1 Pathway. Eur. J. Pharmacol. 2022, 933, 175289. [Google Scholar] [CrossRef]
- Feng, W.; Guo, H.; Xue, T.; Wang, X.; Tang, C.; Ying, B.; Gong, H.; Cui, G. Anti-Inflammation and Anti-Fibrosis with PEGylated, Apigenin Loaded PLGA Nanoparticles in Chronic Pancreatitis Disease. RSC Adv. 2015, 5, 83628–83635. [Google Scholar] [CrossRef]
- Maity, S.; Chakraborti, A.S. Formulation, Physico-Chemical Characterization and Antidiabetic Potential of Naringenin-Loaded Poly D, L Lactide-Co-Glycolide (N-PLGA) Nanoparticles. Eur. Polymer. J. 2020, 134, 109818. [Google Scholar] [CrossRef]
- Chen, C.; Jie, X.; Ou, Y.; Cao, Y.; Xu, L.; Wang, Y.; Qi, R. Nanoliposome Improves Inhibitory Effects of Naringenin on Nonalcoholic Fatty Liver Disease in Mice. Nanomedicine 2017, 12, 1791–1800. [Google Scholar] [CrossRef]
- Zhang, Y.; Zhang, L.; Ban, Q.; Li, J.; Li, C.-H.; Guan, Y.-Q. Preparation and Characterization of Hydroxyapatite Nanoparticles Carrying Insulin and Gallic Acid for Insulin Oral Delivery. Nanomedicine 2018, 14, 353–364. [Google Scholar] [CrossRef]
- Hou, Y.; Huang, H.; Gong, W.; Wang, R.; He, W.; Wang, X.; Hu, J. Co-Assembling of Natural Drug-Food Homologous Molecule into Composite Hydrogel for Accelerating Diabetic Wound Healing. Biomat. Adv. 2022, 140, 213034. [Google Scholar] [CrossRef]
- Shahin, N.N.; Shamma, R.N.; Ahmed, I.S. A Nano-Liposomal Formulation of Caffeic Acid Phenethyl Ester Modulates Nrf2 and NF-Κβ Signaling and Alleviates Experimentally Induced Acute Pancreatitis in a Rat Model. Antioxidants 2022, 11, 1536. [Google Scholar] [CrossRef]
- Mangrulkar, S.; Shah, P.; Navnage, S.; Mazumdar, P.; Chaple, D. Phytophospholipid Complex of Caffeic Acid: Development, In Vitro Characterization, and In Vivo Investigation of Antihyperlipidemic and Hepatoprotective Action in Rats. AAPS Pharm. Sci. Tech. 2021, 22, 28. [Google Scholar] [CrossRef] [PubMed]
- Wan, S.; Zhang, L.; Quan, Y.; Wei, K. Resveratrol-Loaded PLGA Nanoparticles: Enhanced Stability, Solubility and Bioactivity of Resveratrol for Non-Alcoholic Fatty Liver Disease Therapy. R. Soc. Open Sci. 2018, 5, 181457. [Google Scholar] [CrossRef]
- Wang, Z.; Yan, Y.; Wang, Y.; Tong, F. The Interaction between CSE/H2S and the INOS/NO-Mediated Resveratrol/Poly(Ethylene Glycol)-Poly(Phenylalanine) Complex Alleviates Intestinal Ischemia/Reperfusion Injuries in Diabetic Rats. Biomed. Pharmacother. 2019, 112, 108736. [Google Scholar] [CrossRef]
- Mohseni, R.; ArabSadeghabadi, Z.; Ziamajidi, N.; Abbasalipourkabir, R.; RezaeiFarimani, A. Oral Administration of Resveratrol-Loaded Solid Lipid Nanoparticle Improves Insulin Resistance Through Targeting Expression of SNARE Proteins in Adipose and Muscle Tissue in Rats with Type 2 Diabetes. Nanoscale Res. Lett. 2019, 14, 227. [Google Scholar] [CrossRef] [PubMed]
- Dong, Y.; Wan, G.; Yan, P.; Qian, C.; Li, F.; Peng, G. Fabrication of Resveratrol Coated Gold Nanoparticles and Investigation of Their Effect on Diabetic Retinopathy in Streptozotocin Induced Diabetic Rats. J. Photochem. Photobiol. B 2019, 195, 51–57. [Google Scholar] [CrossRef]
- Zu, Y.; Zhao, L.; Hao, L.; Mechref, Y.; Zabet-Moghaddam, M.; Keyel, P.A.; Abbasi, M.; Wu, D.; Dawson, J.A.; Zhang, R.; et al. Browning White Adipose Tissue Using Adipose Stromal Cell-Targeted Resveratrol-Loaded Nanoparticles for Combating Obesity. J. Control. Release 2021, 333, 339–351. [Google Scholar] [CrossRef]
- Devadasu, V.R.; Wadsworth, R.M.; Kumar, M.N.V.R. Protective Effects of Nanoparticulate Coenzyme Q10 and Curcumin on Inflammatory Markers and Lipid Metabolism in Streptozotocin-Induced Diabetic Rats: A Possible Remedy to Diabetic Complications. Drug Deliv. Transl. Res. 2011, 1, 448–455. [Google Scholar] [CrossRef]
- El-Naggar, M.E.; Al-Joufi, F.; Anwar, M.; Attia, M.F.; El-Bana, M.A. Curcumin-Loaded PLA-PEG Copolymer Nanoparticles for Treatment of Liver Inflammation in Streptozotocin-Induced Diabetic Rats. Colloids Surf. B Biointerfaces 2019, 177, 389–398. [Google Scholar] [CrossRef]
- Bateni, Z.; Rahimi, H.R.; Hedayati, M.; Afsharian, S.; Goudarzi, R.; Sohrab, G. The Effects of Nano-Curcumin Supplementation on Glycemic Control, Blood Pressure, Lipid Profile, and Insulin Resistance in Patients with the Metabolic Syndrome: A Randomized, Double-Blind Clinical Trial. Phytother. Res. 2021, 35, 3945–3953. [Google Scholar] [CrossRef]
- Yücel, Ç.; Karatoprak, G.Ş.; Aktaş, Y. Nanoliposomal Resveratrol as a Novel Approach to Treatment of Diabetes Mellitus. J. Nanosci. Nanotechnol. 2018, 18, 3856–3864. [Google Scholar] [CrossRef]
- Frąk, W.; Wojtasińska, A.; Lisińska, W.; Młynarska, E.; Franczyk, B.; Rysz, J. Pathophysiology of Cardiovascular Diseases: New Insights into Molecular Mechanisms of Atherosclerosis, Arterial Hypertension, and Coronary Artery Disease. Biomedicines 2022, 10, 1938. [Google Scholar] [CrossRef] [PubMed]
- Kotlyarov, S.; Kotlyarova, A. Molecular Pharmacology of Inflammation Resolution in Atherosclerosis. Int. J. Mol. Sci. 2022, 23, 4808. [Google Scholar] [CrossRef]
- Mirhafez, S.R.; Mohebati, M.; Feiz Disfani, M.; Saberi Karimian, M.; Ebrahimi, M.; Avan, A.; Eslami, S.; Pasdar, A.; Rooki, H.; Esmaeili, H.; et al. An Imbalance in Serum Concentrations of Inflammatory and Anti-Inflammatory Cytokines in Hypertension. J. Am. Soc. Hypertens. 2014, 8, 614–623. [Google Scholar] [CrossRef] [PubMed]
- Hong, Z.; Xu, Y.; Yin, J.-F.; Jin, J.; Jiang, Y.; Du, Q. Improving the Effectiveness of (−)-Epigallocatechin Gallate (EGCG) against Rabbit Atherosclerosis by EGCG-Loaded Nanoparticles Prepared from Chitosan and Polyaspartic Acid. J. Agric. Food Chem. 2014, 62, 12603–12609. [Google Scholar] [CrossRef]
- Zhang, J.; Nie, S.; Zu, Y.; Abbasi, M.; Cao, J.; Li, C.; Wu, D.; Labib, S.; Brackee, G.; Shen, C.-L.; et al. Anti-Atherogenic Effects of CD36-Targeted Epigallocatechin Gallate-Loaded Nanoparticles. J. Control. Release 2019, 303, 263–273. [Google Scholar] [CrossRef]
- Zhang, J.; Nie, S.; Wang, S. Nanoencapsulation Enhances Epigallocatechin-3-Gallate Stability and Its Antiatherogenic Bioactivities in Macrophages. J. Agric. Food Chem. 2013, 61, 9200–9209. [Google Scholar] [CrossRef]
- Wu, H.; Su, M.; Jin, H.; Li, X.; Wang, P.; Chen, J.; Chen, J. Rutin-Loaded Silver Nanoparticles With Antithrombotic Function. Front. Bioeng. Biotechnol. 2020, 8, 598977. [Google Scholar] [CrossRef]
- Chen, D.; Liu, Y.; Liu, P.; Zhou, Y.; Jiang, L.; Yuan, C.; Huang, M. Orally Delivered Rutin in Lipid-Based Nano-Formulation Exerts Strong Antithrombotic Effects by Protein Disulfide Isomerase Inhibition. Drug Deliv. 2022, 29, 1824–1835. [Google Scholar] [CrossRef]
- Guo, M.; He, Z.; Jin, Z.; Huang, L.; Yuan, J.; Qin, S.; Wang, X.; Cao, L.; Song, X. Oral Nanoparticles Containing Naringenin Suppress Atherosclerotic Progression by Targeting Delivery to Plaque Macrophages. Nano Res. 2023, 16, 925–937. [Google Scholar] [CrossRef]
- He, Y.; Wang, J.; Yan, W.; Huang, N. Gallic Acid and Gallic Acid-Loaded Coating Involved in Selective Regulation of Platelet, Endothelial and Smooth Muscle Cell Fate. RSC Adv. 2014, 4, 212–221. [Google Scholar] [CrossRef]
- Alfei, S.; Grazia Signorello, M.; Schito, A.; Catena, S.; Turrini, F. Reshaped as Polyester-Based Nanoparticles, Gallic Acid Inhibits Platelet Aggregation, Reactive Oxygen Species Production and Multi-Resistant Gram-Positive Bacteria with an Efficiency Never Obtained. Nanoscale Adv. 2019, 1, 4148–4157. [Google Scholar] [CrossRef]
- Zhou, H.; Shan, Y.; Tong, F.; Zhang, Y.; Tang, J.; Shen, R.; Chen, D. Resveratrol Nanoparticle Complex: Potential Therapeutic Applications in Myocardial Ischemia Reperfusion Injury. J. Biomed. Nanotechnol. 2020, 16, 382–389. [Google Scholar] [CrossRef]
- Sun, L.; Hu, Y.; Mishra, A.; Sreeharsha, N.; Moktan, J.B.; Kumar, P.; Wang, L. Protective Role of Poly(Lactic-co-glycolic) Acid Nanoparticle Loaded with Resveratrol against Isoproterenol-induced Myocardial Infarction. BioFactors 2020, 46, 421–431. [Google Scholar] [CrossRef]
- Yadav, Y.C.; Pattnaik, S.; Swain, K. Curcumin Loaded Mesoporous Silica Nanoparticles: Assessment of Bioavailability and Cardioprotective Effect. Drug Dev. Ind. Pharm. 2019, 45, 1889–1895. [Google Scholar] [CrossRef]
- Li, X.; Xiao, H.; Lin, C.; Sun, W.; Wu, T.; Wang, J.; Chen, B.; Chen, X.; Cheng, D. Synergistic Effects of Liposomes Encapsulating Atorvastatin Calcium and Curcumin and Targeting Dysfunctional Endothelial Cells in Reducing Atherosclerosis. Int. J. Nanomed. 2019, 14, 649–665. [Google Scholar] [CrossRef]

| Phenolic Compounds | Type of Nanocarriers (Size) | Targets | Mechanism of Action | Ref. |
|---|---|---|---|---|
| EGCG | Hybrid nanocarriers: EGCG@Se-Tet-1 coated | PC12 and NIH/3T3 cells | Disrupts Aβ aggregation and mitigates Aβ fibrillation. Protects PC12 cells from damages | [85] |
| EGCG | Polymeric nanocarriers: PEGylated PLGA (124 nm) | Alzeimer mice model (APP/PS1 mice) | Improves EGCG stability and efficacy by reducing neuroinflammation, Aβ plaque/peptide burden, and enhancing synaptogenesis | [82] |
| EGCG | Polymeric nanocarriers: PLA-PEG-PVA-EGCG (317 nm) | AlCl3-induced neurobehavioral deficit model | Attenuates neurobehavioral impairments, reduces the generation of Aβ plaque, neurofibrillary tangles, level of Aβ1–42, and Ache activity | [81] |
| EGCG | Micelle nanocarriers: PEG-PLGA-shRNA-RVG29 (152 nm) | BACE1, APP/PS1 mice | Reduces Aβ and BACE1 protein expression and enhances synaptogenesis, memory, and learning processes | [83] |
| EGCG | Selenium nanocarrier: Selenium (91 nm) | LPS-induced PC12 cells and SCI rats | Reduces the levels of inflammatory cytokines, improves locomotor capacity, and diminishes injury region | [86] |
| EGCG | Micelle nanocarriers –Hybrid (B6ME-NPs with SPIONS) | SH-SY5Y neuroblastoma cells | Improves the delivery to PD lesions and inhibits α-syn aggregation | [84] |
| Rutin | Phospholipid nanocarrier: RU-RPLC (<100 nm) | MCAO induced rats | Reduces toxicity and infiltrates well in BBB | [88] |
| Rutin | Metallic nanoparticle: Iron oxide-congo red-MNPS (oleic acid coated) | Aβ-induced SH-SY5Y cells | Inhibits Aβ-induced cytotoxicity and reduces the production of NO and ROS | [89] |
| Rutin | Solid lipid nanocarrier 100 nm | Rattus norvegicus rats | Infiltrates well in BBB | [87] |
| Apigenin | Lipid nanocarrier | Haloperidol-induced Parkinson’s model | Upregulates dopamine level | [90] |
| Naringenin | Nanoemulsion: Capryol 90-tween 20 (113 nm) | Aβ- induced SH-SY5Y cells | Decreases Aβ levels, APP, BACE, and tau expressions | [91] |
| Naringenin | Nanoemulsion: Capryol 90-tween 80-Vit E (38 nm) | 6-OHDA-induced Parkinson’s disease in rats | Reverses PD symptoms in rats | [92] |
| Naringenin | Polymeric nanocarrier: PCL-gelatin-coated (192 nm) | OGD-induced mesenchymal stem cells | Reduces the levels of proinflammatory cytokines and biomarkers | [93] |
| Gallic acid | Lipid nanocarrier: GA-NPs | MCAO rats | Presents neuroprotection | [94] |
| Resveratrol | Lipid nanocarrier: RSV LNC (242 nm) | Aβ1–42-induced rats | Rescues deleterious effect of Aβ1–42 | [96] |
| Resveratrol | Lipid core nanocapsule: RSV-LNC (242 nm) | Hypocamplal culture | Modulates neuroinflammation | [95] |
| Resveratrol | Polymeric nanocarrier: PLA-PS80 | MPTP-induced C57BL/6 mice | Presents neuroprotection | [97] |
| Resveratrol | Solid lipid nanocarrier: RSV-SLN-OX26 (254 nm) | Endothelial human brain | Enhances Aβ-aggregation clearance, and blockades Aβ fibrillation | [98] |
| Resveratrol | Res-selenium-peptide: TGN-Res@SeNPs | AlCl3-AD model mice | Decreases Aβ aggregation in the hippocampus, and downregulates neuroinflammation | [99] |
| Resveratrol | RSV-Se nanoparticles (RSV-SeNPs) | AlCl3-AD rat model | Attenuates the mitochondrial dysfunction, downregulates inflammatory pathways: STAT3, GSK-3B, and triggers PI3K | [100] |
| Curcumin | Polymeric nanocarrier: PLGA-CU-g7 (204 nm) | Hippocampal cell cultures | Reduces the aggregation of Aβ | [102] |
| Curcumin | Solid lipid nanocarrier: SLNP-CU (Ni) | 5XFAD mice | Improves neuroprotection and reduces astrocytic and microglia immune responses in AD-mice | [105] |
| Curcumin | Polymeric nanocarrier PLGA-NPs-CRT (128 nm) | (APP/PS1dE9) AD mouse model | Diminishes Aβ burden, astrogliosis, microgliosis, and memory impairment | [103] |
| Curcumin | Polymeric Se-NP-PLGA (160 nm) | (5XFAD) model | Diminishes Aβ burden and reduces memory impairment | [106] |
| Curcumin | Nanoliposomes Lip-PEG-CU-mAb (153 nm) | AD brain patients | Interrupts Aβ1–42 aggregations | [101] |
| Curcumin | Polymeric nanocarrier: Chit-BSA (143 nm) | hCMEC/D3 BBB cell model | Reduces NF-kB signaling and improves Aβ42 uptakes | [104] |
| Curcumin | Lipid nanocarrier: Cur-Pip-GMO-based NPs (93 nm) | Rat cell line, a cellular model of PD, | Inhibits α-syn aggregation and stimulates autophagy | [107] |
| Phenolic Compounds | Type of Nanocarriers (Size) | Targets | Mechanism of Action | Ref. |
|---|---|---|---|---|
| EGCG | Polymeric nanocarrier: PEG-PLGA (176 nm) | DNCB-induced dermatitis model | Reduces ear and skin thickness, mitigates the inflammatory cytokines releases (TNF-α, IFN-γ, IL-4, IL-6, and IL-17A), blockades necroptosis (RIP1, RIP3, and MLKL expressions), and regulates MAPK pathways (p-p38, ERK1, and ERK2) | [114] |
| EGCG | Polymeric nanocarrier: CHI-EGCG-NPs (211 nm) | Cultured keratinocytes and IMQ-induced model | Reduces inflammatory responses and modulates psoriasis-related inflammatory cytokines | [113] |
| EGCG | Hydrogel nanocarrier: HG-Ag-EGCG (217 nm) | Subcutaneous wound in Wistar rats | Accelerates wound properties (modulates growth factors and cytokines) | [116] |
| EGCG | Polymeric nanocarrier: EGCG-Vit C-Gelatin, chitosan (200 nm) | Wound on STZ-induced diabetic mice | Promotes wound healing by raising collagen accumulation, promoting angiogenesis, and reducing inflammatory cell infiltrations | [115] |
| Rutin | Hydrogel nanocarrier: NC-RU-gel (447 nm) | UV-induced BALB/c mice | Increases the skin permeability of rutin | [117] |
| Rutin | Ethosomal nanocarrier: ETOH-PL90G-H2O (112 nm) | Keratinocyte cells (NCTC2544) and volunteer patients | Improves anti-inflammatory effect | [118] |
| Apigenin | Ethosomal nanocarrier (36 nm) | UV-induced skin inflammation | Reduces COX-2 levels | [119] |
| Naringenin | Liposome: NAR-Polysorbate 80-Lipoid® (100 nm) | 3T3 fibroblasts and TPA-induced mice | Reduces skin inflammation | [120] |
| Naringenin | Liposome: chitosan-coated naringenin nanoemulsion (105 nm) | Abrasion wound in rat model | Controls the delivery and ameliorates the wounds construction and skin regeneration | [121] |
| Gallic acid | Polymeric nanocarrier: Tween 80-chitosan (330 nm) | HaCaT cell line | Reduces keratinocyte proliferation and exerts protein protection in vitro. | [123] |
| Gallic acid | Hydrogel nanocarrier | Total skin defect model | Enhance wound healing by reducing the expression of IL-6, IL-1β, and TNF-α | [125] |
| Gallic acid | Hydrogel nanocarrier: GH/GGA | Skin wounded mice | Speeds up the wound healing by scavenging the ROS and promoting tissue regeneration | [124] |
| Gallic acid | Polymeric nanocarrier: liposome, glycosome GA polyxomer (70 nm) | TPA induced mice | Improves the skin target delivery and blockades leukocytes infiltration | [122] |
| Caffeic acid | Nanofiber nanocarrier: PLGA | In vitro scratch assay | Presents better wound healing properties on human fibroblast | [127] |
| Caffeic acid | Nanofiber nanocarrier: Chitosan-PCL/CCA | NHDF-neo cell line | Improves cell attachment | [126] |
| Resveratrol | Lipid nanocarrier: Oleic acid-S75 (79 nm) | TPA induced mice | Neutralizes the inflammatory response | [128] |
| Resveratrol | Lipid nanocarrier: DSPC/DOPE/ω3 (156 nm) | RAW 264.7 cell line | Inhibits COX and NO productions | [129] |
| Resveratrol | Peptide-hydrogel nanocarrier: Fmoc-FFGGRGD | Rat skin damage model | Inhibits macrophage production of pro-inflammatory cytokines | [130] |
| Curcumin | Hydrogel nanocarriers: PLGA NPS in hydrogel (150 nm) | IMQ-induced-C57/BL6 mice | Improves anti-psoriasis activity | [134] |
| Curcumin | Gelatin nanofiber mats | Rat wounded model | Improves the wounds by increasing fibroblast proliferation and migration, inhibiting macrophages, and reducing pro-inflammatory cytokines | [135] |
| Curcumin | Nanocrystal coated nanocarrier: Ch/CNC (Ag NPx/Cury) | Injured rat model | Accelerates wound closure and repairs tissues | [136] |
| Curcumin | Silica nanocarrier: CU-Si-Nps (36 nm) | HDF fibroblast cell | Enhances fibroblast migrations | [138] |
| Curcumin | Nanostructured lipid carrier: EGF–Cur-NLC (331 nm) | Punched wound on the skin | Accelerates wound closure | [137] |
| Curcumin | Hydrogel nanocarrier: PEG-PLA in dextran hydrogel (65 nm) | BALB/c mice | Accelerates angiogenesis, fibroblast accumulation, and wound healing | [133] |
| Curcumin | Hydrogel nanocarrier: MPEG-PCL in CCS-OA hydrogel (nano: 40 nm) | Injured tissue | Improves re-epithelialization of the injury | [131] |
| Curcumin | Hydrogel nanocarrier: PEG-PCL-PEG in hydrogel (micelle: 26 nm) | Wound model | Enhances cutaneous repair, and increases collagen content and wound maturity | [132] |
| Phenolic Compounds | Type of Nanocarriers (Size) | Targets | Mechanism of Action | Ref. |
|---|---|---|---|---|
| EGCG | Polymeric nanocarrier: EGCG-PLGA-in hydrogel (112 nm) | SC model | Increases delivery and reduces cholesterol, LDL-cholesterol while increasing HDL | [161] |
| EGCG | Hybrid nanocarrier HG-AG-EGCG | HFD-induced T2DM C57BL/6 | Improves wound healing in diabetes by suppressing related inflammation | [116] |
| EGCG | Protein nanocarrier: EGCG-β-Lg (22 nm) | HFD obese mice | Lowers triglycerides amount in the model and improved glycemic homeostasis, as well as insulin sensitivity | [160] |
| Rutin | Lipid nanocarrier: Lecithin nanophytosome: (72 nm) | STZ-induced diabetic rats | Mitigates hyperglycemia and hyperlipidemia, reduces the induced damage of the kidney, liver, and pancreas in rats | [163] |
| Rutin | Polymeric nanocarrier: ARG-EG-RU (68 nm) | STZ-induced diabetic rats | Reduces glucose, GHb, and lipid levels, while increasing insulin amount | [162] |
| Rutin | Selenium nanocarrier: RU+Se-NPs | Sprague-Dawley rats | Upregulates SIRT-1, Nrf-2, and HO-1 and downregulates JAK-2/STAT3 pathways, as well as inflammatory markers | [164] |
| Apigenin | Polymeric nanocarrier: PEGlated-PLGA (160 nm) | Cholecystokinin- induced C57/BL6 mice | Inhibits PSC growth, promotes PSC apoptosis, reduce the expression of PSC-related inflammation | [165] |
| Naringenin | Lipid nanocarrier: NRG-Nano (98 nm) | Methionine choline-induced mice | Improved absorption and showed protection in fatty liver | [167] |
| Naringenin | Polymeric nanocarrier: N-PLGA (129 nm) | STZ-induced diabetic rat | Ameliorates diabetogenic (increases insulin level, and improves dyslipidemia) | [166] |
| Gallic acid | Hydrogel nanocarrier: GA-KGM | STZ-induced diabetic rats | Reduces the expression of IL-1β, TNF-α, and COX-2 | [169] |
| Gallic acid | Polymeric nanocarrier: HAP-PEG-GA-INS (396 nm) | STZ-induced T1D rats | Reduces blood glucose level in diabetic rats due to a higher delivery of insulin | [168] |
| Caffeic acid | Lipid nanocarrier: CAPE-loaded-NL (309 nm) | L-ornithine induced rat | Modulated Nrf2 and NF-kB signaling | [170] |
| Caffeic acid | Lipid nanocarrier: CA–PC (168 nm) | HFD-induced hyperlipidemic model | Maintain hepatocyte structure which promotes lipid absorption | [171] |
| Resveratrol | Lipid nanocarrier: RSV-LPs (215 nm) | Glucose/STZ-induced β- TC cell | Reduces glucose and increased insulin level | [180] |
| Resveratrol | Metallic nanocarrier: RES-Au-NPs (20 nm) | STZ- induced diabetic rats | Overcomes blood-retinal barrier, reduces VEGF-1, TNF-α, MCP-1, ICAM-1, IL-6, and blockades of ERK1/2 signaling pathway | [175] |
| Resveratrol | Polymeric nanocarrier: RES/PEG-PPhe | Intestine of STZ-induced diabetic rats | Reduces glucose level and increases insulin level while alleviating intestine injury | [173] |
| Resveratrol | Solid lipid nanocarrier: SLN-RES (248 nm) | STZ-induced rats | Displays hypoglycemic activity, reduces Snap 23, Stx4 and Vamp2 in insulin resistance | [174] |
| Resveratrol | Polymeric nanocarrier: RSV-PLGA-NPs (176 nm) | OA-induced HepG2 | Promotes lipolysis and mitigates hepatocellular proliferation | [172] |
| Resveratrol | Hybrid nanocarrier: L-Rnano (90 nm) | HFD-C57BL/6 J mice | Decreases fat mass and inflammation while improving glucose homeostasis | [176] |
| Curcumin | Polymeric nanocarrier: CU-PLA-PEG (117 nm) | STZ-induced rat | Reduces NF-κB activation, COX-2, TGF-β, and PPARγ expressions | [178] |
| Curcumin | Polymeric nanocarrier: CoQ10-PLGA (115 nm) | STZ-induced rat | Reduces CRP, IL-6, TNF-α, triglyceride, and total cholesterol levels in plasma. | [177] |
| Curcumin | Micelle nanocarrier: C3-CU-GRAS (12 nm) | MetS patients for 12 weeks | Reduces the level of triglyceride and HOMA-b index | [179] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Rakotondrabe, T.F.; Fan, M.-X.; Muema, F.W.; Guo, M.-Q. Modulating Inflammation-Mediated Diseases via Natural Phenolic Compounds Loaded in Nanocarrier Systems. Pharmaceutics 2023, 15, 699. https://doi.org/10.3390/pharmaceutics15020699
Rakotondrabe TF, Fan M-X, Muema FW, Guo M-Q. Modulating Inflammation-Mediated Diseases via Natural Phenolic Compounds Loaded in Nanocarrier Systems. Pharmaceutics. 2023; 15(2):699. https://doi.org/10.3390/pharmaceutics15020699
Chicago/Turabian StyleRakotondrabe, Tojofaniry Fabien, Min-Xia Fan, Felix Wambua Muema, and Ming-Quan Guo. 2023. "Modulating Inflammation-Mediated Diseases via Natural Phenolic Compounds Loaded in Nanocarrier Systems" Pharmaceutics 15, no. 2: 699. https://doi.org/10.3390/pharmaceutics15020699
APA StyleRakotondrabe, T. F., Fan, M.-X., Muema, F. W., & Guo, M.-Q. (2023). Modulating Inflammation-Mediated Diseases via Natural Phenolic Compounds Loaded in Nanocarrier Systems. Pharmaceutics, 15(2), 699. https://doi.org/10.3390/pharmaceutics15020699








