Chemistry of Therapeutic Oligonucleotides That Drives Interactions with Biomolecules
Abstract
1. Introduction
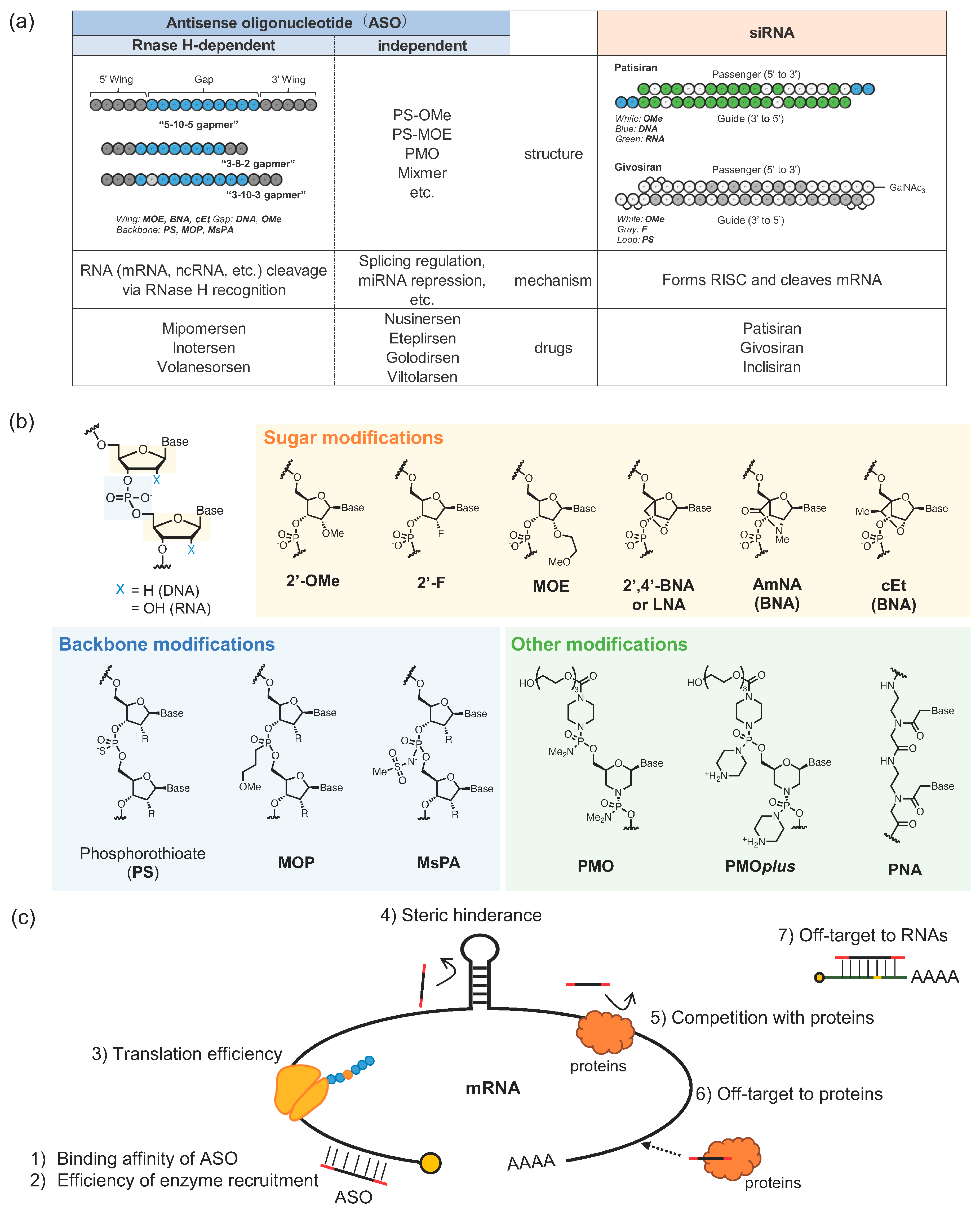
2. In-Plasma Dynamics of Oligonucleotide Drugs with Chemical Modifications
2.1. Oligonucleotide Therapeutics with Phosphorothioate Modification
2.2. Oligonucleotide Therapeutics with Phosphate Backbone Comprising Unnatural Modifications Other Than Phosphorothioate Modification
2.2.1. Phosphorodiamidate Morpholino Oligomer (PMO)
2.2.2. Peptide Nucleic Acids (PNAs)
3. Cellular Uptake of Oligonucleotides
3.1. Molecular Mechanisms of Cellular Intake
3.2. Delivery of Nucleic Acid via Specific Molecular Interactions
3.2.1. Asialoglycoprotein Receptor (ASGPR)
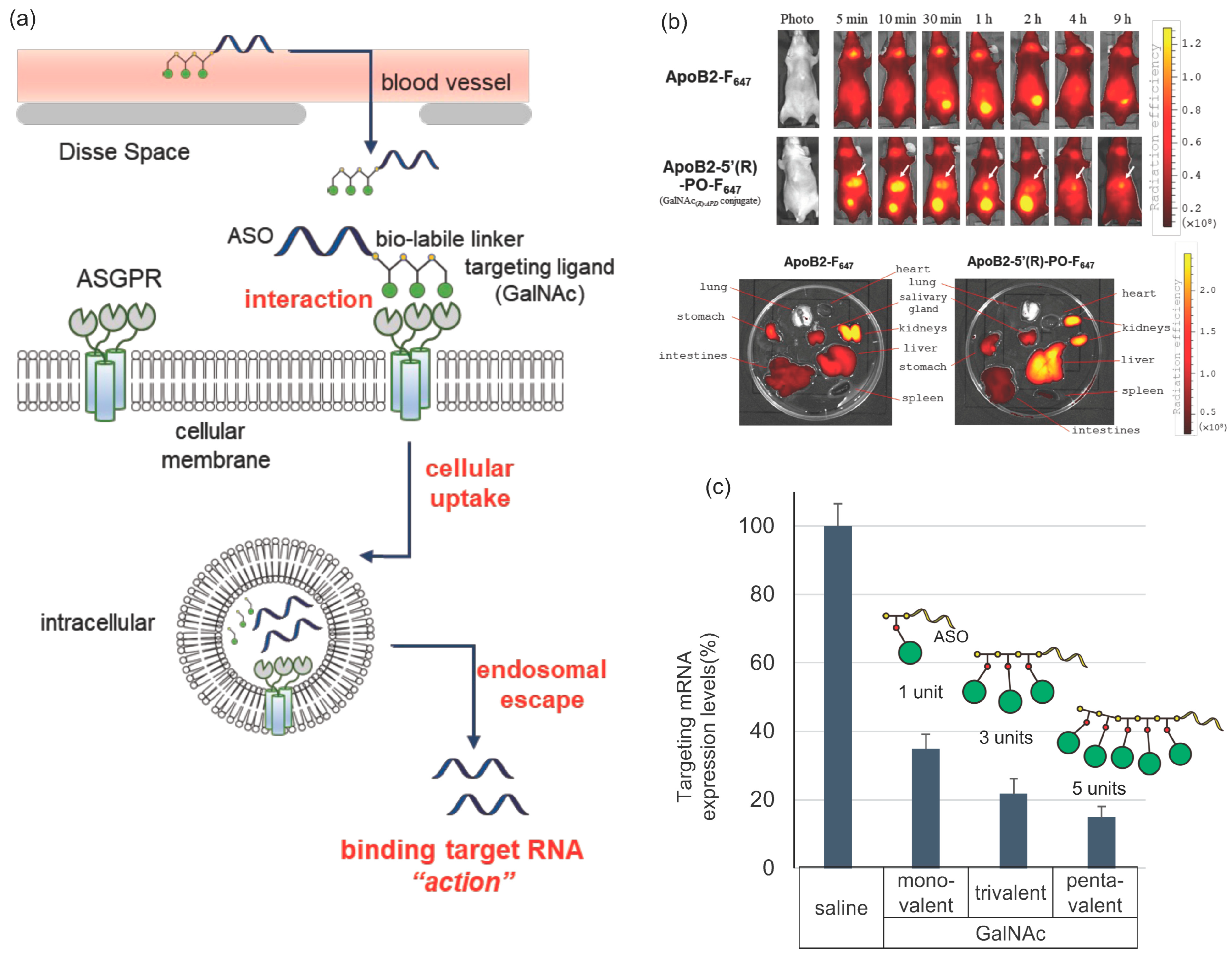
3.2.2. Glucagon-Like Peptide-1 Receptor (GLP1R)
3.2.3. Glucose Transporter (GLUT1)
3.2.4. Specific Delivery Using Different Kinds of Cell Surface Receptors
4. Intracellular Kinetics of Nucleic Acid Drugs and Their Regulation
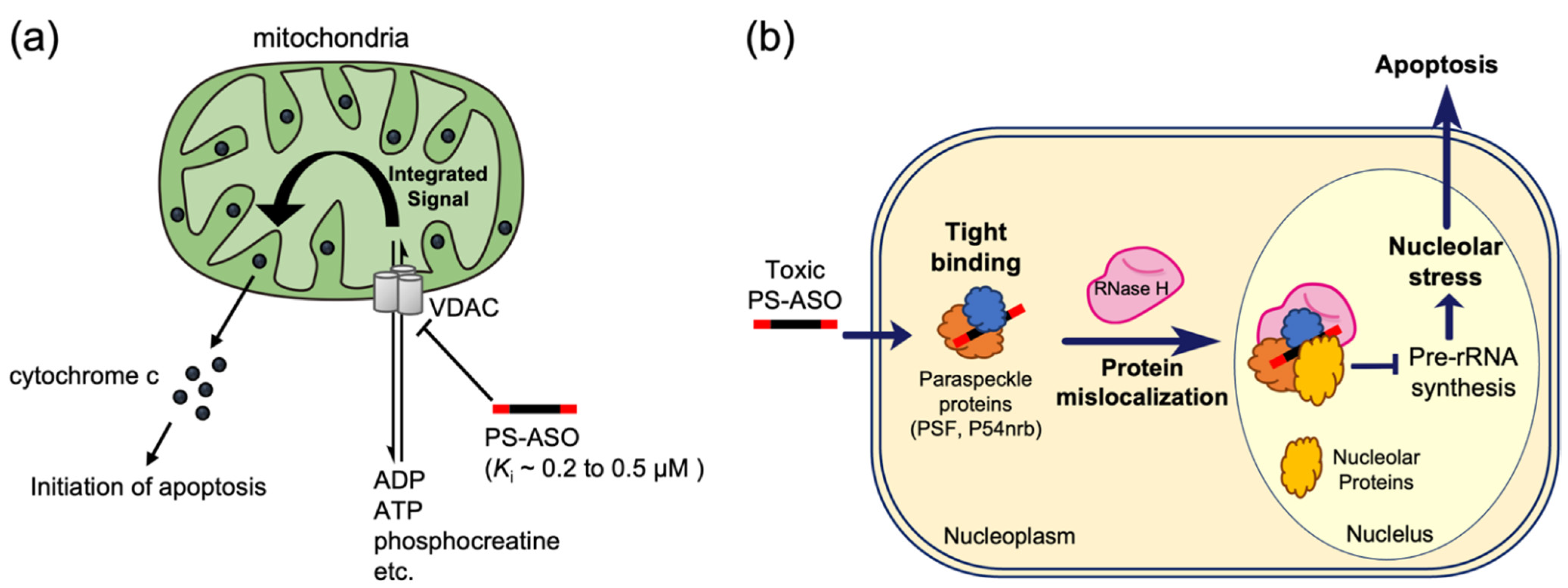
4.1. Interactions between Nucleic Acids and Organelles
4.2. Interactions with Proteins
4.3. Interactions with Intracellular Nucleic Acids
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Eaton, B.E.; Gold, L.; Zichi, D.A. Let’s Get Specific: The Relationship between Specificity and Affinity. Chem. Biol. 1995, 2, 633–638. [Google Scholar] [CrossRef] [PubMed]
- Liang, X.H.; Nichols, J.G.; de Hoyos, C.L.; Crooke, S.T. Some ASOs That Bind in the Coding Region of MRNAs and Induce RNase H1 Cleavage Can Cause Increases in the Pre-MRNAs That May Blunt Total Activity. Nucleic Acids Res. 2020, 48, 9840–9858. [Google Scholar] [CrossRef] [PubMed]
- Dieckmann, A.; Hagedorn, P.H.; Burki, Y.; Brügmann, C.; Berrera, M.; Ebeling, M.; Singer, T.; Schuler, F. A Sensitive In Vitro Approach to Assess the Hybridization-Dependent Toxic Potential of High Affinity Gapmer Oligonucleotides. Mol. Ther. Nucleic Acids 2018, 10, 45–54. [Google Scholar] [CrossRef]
- Reyderman, L.; Stavchansky, S. Pharmacokinetics and Biodistribution of a Nucleotide-Based Thrombin Inhibitor in Rats. Pharm. Res. 1998, 15, 904–910. [Google Scholar] [CrossRef] [PubMed]
- Gaus, H.J.; Gupta, R.; Chappell, A.E.; Østergaard, M.E.; Swayze, E.E.; Seth, P.P. Characterization of the Interactions of Chemically-Modified Therapeutic Nucleic Acids with Plasma Proteins Using a Fluorescence Polarization Assay. Nucleic Acids Res. 2019, 47, 1110–1122. [Google Scholar] [CrossRef] [PubMed]
- Crooke, S.T.; Seth, P.P.; Vickers, T.A.; Liang, X.H. The Interaction of Phosphorothioate-Containing RNA Targeted Drugs with Proteins Is a Critical Determinant of the Therapeutic Effects of These Agents. J. Am. Chem. Soc. 2020, 142, 14754–14771. [Google Scholar] [CrossRef]
- Yacyshyn, B.R.; Beth Bowen-Yacyshyn, M.; Jewell, L.; Tami, J.A.; Frank Bennett, C.; Kisner, D.L.; Shanahan, W.R. A Placebo-Controlled Trial of ICAM-1 Antisense Oligonucleotide in the Treatment of Crohn’s Disease. Gastroenterology 1998, 114, 1133–1142. [Google Scholar] [CrossRef]
- Scott Henrya, A.P.; Bolte, H.; Auletta, C. Evaluation of the Toxicity of ISIS 2302, a Phosphorothioate Oligonucleotide, in a Four-Week Study in Cynomolgus Monkeys. Toxicology 1997, 120, 145–155. [Google Scholar] [CrossRef]
- Sheehan, J.P.; Lan, H.-C. Phosphorothioate Oligonucleotides Inhibit the Intrinsic Tenase Complex A NTISENSE THERAPY Targets Specific MRNA Sequences. Blood 1998, 92, 1617–1625. [Google Scholar] [CrossRef]
- Geary, R.S.; Baker, B.F.; Crooke, S.T. Clinical and Preclinical Pharmacokinetics and Pharmacodynamics of Mipomersen (Kynamro®): A Second-Generation Antisense Oligonucleotide Inhibitor of Apolipoprotein B. Clin. Pharmacokinet. 2015, 54, 133–146. [Google Scholar] [CrossRef]
- Bosgra, S.; Sipkens, J.; de Kimpe, S.; den Besten, C.; Datson, N.; van Deutekom, J. The Pharmacokinetics of 2′-O-Methyl Phosphorothioate Antisense Oligonucleotides: Experiences from Developing Exon Skipping Therapies for Duchenne Muscular Dystrophy. Nucleic Acid Ther. 2019, 29, 305–322. [Google Scholar] [CrossRef] [PubMed]
- Yu, R.Z.; Wang, Y.; Norris, D.A.; Kim, T.-W.; Narayanan, P.; Geary, R.S.; Monia, B.P.; Henry, S.P. Immunogenicity Assessment of Inotersen, a 2′-O-(2-Methoxyethyl) Antisense Oligonucleotide in Animals and Humans: Effect on Pharmacokinetics, Pharmacodynamics, and Safety. Nucleic Acid Ther. 2020, 30, 265–275. [Google Scholar] [CrossRef] [PubMed]
- Oka, N.; Yamamoto, M.; Sato, T.; Wada, T. Solid-Phase Synthesis of Stereoregular Oligodeoxyribonucleoside Phosphorothioates Using Bicyclic Oxazaphospholidine Derivatives as Monomer Units. J. Am. Chem. Soc. 2008, 130, 16031–16037. [Google Scholar] [CrossRef] [PubMed]
- Knouse, K.W.; de Gruyter, J.N.; Schmidt, M.A.; Zheng, B.; Vantourout, J.C.; Kingston, C.; Mercer, S.E.; Mcdonald, I.M.; Olson, R.E.; Zhu, Y.; et al. Unlocking P(V): Reagents for Chiral Phosphorothioate Synthesis. Science (1979) 2018, 361, 1234–1238. [Google Scholar] [CrossRef]
- Iwamoto, N.; Butler, D.C.D.; Svrzikapa, N.; Mohapatra, S.; Zlatev, I.; Sah, D.W.Y.; Meena; Standley, S.M.; Lu, G.; Apponi, L.H.; et al. Control of Phosphorothioate Stereochemistry Substantially Increases the Efficacy of Antisense Oligonucleotides. Nat. Biotechnol. 2017, 35, 845–851. [Google Scholar] [CrossRef]
- Østergaard, M.E.; de Hoyos, C.L.; Wan, W.B.; Shen, W.; Low, A.; Berdeja, A.; Vasquez, G.; Murray, S.; Migawa, M.T.; Liang, X.H.; et al. Understanding the Effect of Controlling Phosphorothioate Chirality in the DNA Gap on the Potency and Safety of Gapmer Antisense Oligonucleotides. Nucleic Acids Res. 2020, 48, 1691–1700. [Google Scholar] [CrossRef]
- Liu, Y.; Dodart, J.C.; Tran, H.; Berkovitch, S.; Braun, M.; Byrne, M.; Durbin, A.F.; Hu, X.S.; Iwamoto, N.; Jang, H.G.; et al. Variant-Selective Stereopure Oligonucleotides Protect against Pathologies Associated with C9orf72-Repeat Expansion in Preclinical Models. Nat. Commun. 2021, 12, 1–15. [Google Scholar] [CrossRef]
- Moulton, J. Guide for Morpholino Users: Toward Therapeutics. J. Drug Discov. Dev. Deliv. 2016, 3, 1023. [Google Scholar]
- Amantana, A.; Moulton, H.M.; Cate, M.L.; Reddy, M.T.; Whitehead, T.; Hassinger, J.N.; Youngblood, D.S.; Iversen, P.L. Pharmacokinetics, Biodistribution, Stability and Toxicity of a Cell-Penetrating Peptide—Morpholino Oligomer Conjugate. Bioconjug. Chem. 2007, 18, 1325–1331. [Google Scholar] [CrossRef]
- Frank, D.E.; Schnell, F.J.; Akana, C.; El-Husayni, S.H.; Desjardins, C.A.; Morgan, J.; Charleston, J.S.; Sardone, V.; Domingos, J.; Dickson, G.; et al. Increased Dystrophin Production with Golodirsen in Patients with Duchenne Muscular Dystrophy. Neurology 2020, 94, e2270–e2282. [Google Scholar] [CrossRef]
- Cirak, S.; Arechavala-Gomeza, V.; Guglieri, M.; Feng, L.; Torelli, S.; Anthony, K.; Abbs, S.; Garralda, M.E.; Bourke, J.; Wells, D.J.; et al. Exon Skipping and Dystrophin Restoration in Patients with Duchenne Muscular Dystrophy after Systemic Phosphorodiamidate Morpholino Oligomer Treatment: An Open-Label, Phase 2, Dose-Escalation Study. Lancet 2011, 378, 595–605. [Google Scholar] [CrossRef]
- Shadid, M.; Badawi, M.; Abulrob, A. Antisense Oligonucleotides: Absorption, Distribution, Metabolism, and Excretion. Expert Opin. Drug Metab. Toxicol. 2021, 17, 1281–1292. [Google Scholar] [CrossRef]
- Heald, A.E.; Iversen, P.L.; Saoud, J.B.; Sazani, P.; Charleston, J.S.; Axtelle, T.; Wong, M.; Smith, W.B.; Vutikullird, A.; Kaye, E. Safety and Pharmacokinetic Profiles of Phosphorodiamidate Morpholino Oligomers with Activity against Ebola Virus and Marburg Virus: Results of Two Single-Ascending-Dose Studies. Antimicrob Agents Chemother. 2014, 58, 6639–6647. [Google Scholar] [CrossRef]
- Tsoumpra, M.K.; Fukumoto, S.; Matsumoto, T.; Takeda, S.; Wood, M.J.A.; Aoki, Y. Peptide-Conjugate Antisense Based Splice-Correction for Duchenne Muscular Dystrophy and Other Neuromuscular Diseases. EBioMedicine 2019, 45, 630–645. [Google Scholar] [CrossRef]
- Moulton, H.M.; Moulton, J.D. Morpholinos and Their Peptide Conjugates: Therapeutic Promise and Challenge for Duchenne Muscular Dystrophy. Biochim Biophys. Acta Biomembr. 2010, 1798, 2296–2303. [Google Scholar] [CrossRef]
- Nielsen, P.E.; Egholm, M.; Berg, R.H.; Buchardt, O. Sequence-Selective Recognition of DNA by Strand Displacement with a Thymine-Substituted Polyamide. Science 1991, 254, 1497–1500. [Google Scholar] [CrossRef]
- Hyrup, B.; Nielsen, P.E. Peptide Nucleic Acids (PNA): Synthesis, Properties and Potential Applications. Bioorg. Med. Chem. 1996, 4, 5–23. [Google Scholar] [CrossRef]
- Egholm, M.; Buchardt, O.; Christensen, L.; Behrens, C.; Freier, S.M.; Driver, D.A.; Berg, R.H.; Kim, S.K.; Norden, B.; Nielsen, P.E. PNA Hybridizes to Complementary Oligonucleotides Obeying the Watson-Crick Hydrogen-Bonding Rules. Nature 1993, 365, 566–568. [Google Scholar] [CrossRef]
- McMahon, B.M.; Mays, D.; Lipsky, J.; Stewart, J.A.; Fauq, A.; Richelson, E. Pharmacokinetics and Tissue Distribution of a Peptide Nucleic Acid after Intravenous Administration. Antisense Nucleic Acid Drug Dev. 2002, 12, 65–70. [Google Scholar] [CrossRef]
- Juliano, R.L. The Delivery of Therapeutic Oligonucleotides. Nucleic Acids Res. 2016, 44, 6518–6548. [Google Scholar] [CrossRef]
- Crooke, S.T.; Wang, S.; Vickers, T.A.; Shen, W.; Liang, X.-H. Cellular Uptake and Trafficking of Antisense Oligonucleotides. Nat. Biotechnol. 2017, 35, 230–237. [Google Scholar] [CrossRef]
- Wang, S.; Sun, H.; Tanowitz, M.; Liang, X.H.; Crooke, S.T. Annexin A2 Facilitates Endocytic Trafficking of Antisense Oligonucleotides. Nucleic Acids Res. 2016, 44, 7314–7330. [Google Scholar] [CrossRef]
- Linnane, E.; Davey, P.; Zhang, P.; Puri, S.; Edbrooke, M.; Chiarparin, E.; Revenko, A.S.; Robert Macleod, A.; Norman, J.C.; Ross, S.J. Differential Uptake, Kinetics and Mechanisms of Intracellular Trafficking of next-Generation Antisense Oligonucleotides across Human Cancer Cell Lines. Nucleic Acids Res. 2019, 47, 4375–4392. [Google Scholar] [CrossRef]
- Wang, S.; Sun, H.; Tanowitz, M.; Liang, X.H.; Crooke, S.T. Intra-Endosomal Trafficking Mediated by Lysobisphosphatidic Acid Contributes to Intracellular Release of Phosphorothioate-Modified Antisense Oligonucleotides. Nucleic Acids Res. 2017, 45, 5309–5322. [Google Scholar] [CrossRef]
- Crooke, S.T.; Liang, X.H.; Baker, B.F.; Crooke, R.M. Antisense Technology: A Review. J. Biol. Chem. 2021, 296, 100416. [Google Scholar] [CrossRef]
- Geary, R.S.; Norris, D.; Yu, R.; Bennett, C.F. Pharmacokinetics, Biodistribution and Cell Uptake of Antisense Oligonucleotides. Adv. Drug Deliv. Rev. 2015, 87, 46–51. [Google Scholar] [CrossRef]
- Oyama, S.; Yamamoto, T.; Yamayoshi, A. Recent Advances in the Delivery Carriers and Chemical Conjugation Strategies for Nucleic Acid Drugs. Cancers 2021, 13, 3881. [Google Scholar] [CrossRef]
- Spiess, M.; Lodish, H.F. Sequence of a Second Human Asialoglycoprotein Receptor: Conservation of Two Receptor Genes during Evolution. Proc. Natl. Acad. Sci. USA 1985, 82, 6465–6469. [Google Scholar] [CrossRef]
- Mamidyala, S.K.; Dutta, S.; Chrunyk, B.A.; Préville, C.; Wang, H.; Withka, J.M.; McColl, A.; Subashi, T.A.; Hawrylik, S.J.; Griffor, M.C.; et al. Glycomimetic Ligands for the Human Asialoglycoprotein Receptor. J. Am. Chem. Soc. 2012, 134, 1978–1981. [Google Scholar] [CrossRef]
- Schmidt, K.; Prakash, T.P.; Donner, A.J.; Kinberger, G.A.; Gaus, H.J.; Low, A.; Østergaard, M.E.; Bell, M.; Swayze, E.E.; Seth, P.P. Characterizing the Effect of GalNAc and Phosphorothioate Backbone on Binding of Antisense Oligonucleotides to the Asialoglycoprotein Receptor. Nucleic Acids Res. 2017, 45, 2294–2306. [Google Scholar] [CrossRef]
- Hangeland, J.J.; Flesher, J.E.; Deamond, S.F.; Lee, Y.C.; Ts’O, P.O.; Frost, J.J. Tissue Distribution and Metabolism of the [32P]-Labeled Oligodeoxynucleoside Methylphosphonate-Neoglycopeptide Conjugate, [YEE(Ah-GalNAc)3]-SMCC-AET-PUmpT7, in the Mouse. Antisense Nucleic Acid Drug Dev. 1997, 7, 141–149. [Google Scholar] [CrossRef] [PubMed]
- Prakash, T.P.; Graham, M.J.; Yu, J.; Carty, R.; Low, A.; Chappell, A.; Schmidt, K.; Zhao, C.; Aghajan, M.; Murray, H.F.; et al. Targeted Delivery of Antisense Oligonucleotides to Hepatocytes Using Triantennary N-Acetyl Galactosamine Improves Potency 10-Fold in Mice. Nucleic Acids Res. 2014, 42, 8796–8807. [Google Scholar] [CrossRef] [PubMed]
- Nair, J.K.; Willoughby, J.L.S.; Chan, A.; Charisse, K.; Alam, M.R.; Wang, Q.; Hoekstra, M.; Kandasamy, P.; Kel’in, A.V.; Milstein, S.; et al. Multivalent N-Acetylgalactosamine-Conjugated SiRNA Localizes in Hepatocytes and Elicits Robust RNAi-Mediated Gene Silencing. J. Am. Chem. Soc. 2014, 136, 16958–16961. [Google Scholar] [CrossRef]
- Khorev, O.; Stokmaier, D.; Schwardt, O.; Cutting, B.; Ernst, B. Trivalent, Gal/GalNAc-Containing Ligands Designed for the Asialoglycoprotein Receptor. Bioorg. Med. Chem. 2008, 16, 5216–5231. [Google Scholar] [CrossRef] [PubMed]
- Yamamoto, T.; Sawamura, M.; Wada, F.; Harada-Shiba, M.; Obika, S. Serial Incorporation of a Monovalent GalNAc Phosphoramidite Unit into Hepatocyte-Targeting Antisense Oligonucleotides. Bioorg. Med. Chem. 2016, 24, 26–32. [Google Scholar] [CrossRef]
- Terada, C.; Wada, F.; Uchida, M.; Yasutomi, Y.; Oh, K.; Kawamoto, S.; Kayaba, Y.; Yamayoshi, A.; Harada-Shiba, M.; Obika, S.; et al. Programmed Instability of Ligand Conjugation Manifold for Efficient Hepatocyte Delivery of Therapeutic Oligonucleotides. Nucleic Acid Ther. 2021, 31, 404–416. [Google Scholar] [CrossRef]
- Wada, F.; Yamamoto, T.; Kobayashi, T.; Tachibana, K.; Ito, K.R.; Hamasaki, M.; Kayaba, Y.; Terada, C.; Yamayoshi, A.; Obika, S.; et al. Drug Discovery and Development Scheme for Liver-Targeting Bridged Nucleic Acid Antisense Oligonucleotides. Mol. Ther. Nucleic Acids 2021, 26, 957–969. [Google Scholar] [CrossRef]
- Ämmälä, C.; Drury, W.J.; Knerr, L.; Ahlstedt, I.; Stillemark-Billton, P.; Wennberg-Huldt, C.; Andersson, E.M.; Valeur, E.; Jansson-Löfmark, R.; Janzén, D.; et al. Targeted Delivery of Antisense Oligonucleotides to Pancreatic β-Cells. Sci. Adv. 2018, 4, eaat3386. [Google Scholar] [CrossRef]
- Knerr, L.; Prakash, T.P.; Lee, R.; Drury, W.J.; Nikan, M.; Fu, W.; Pirie, E.; de Maria, L.; Valeur, E.; Hayen, A.; et al. Glucagon like Peptide 1 Receptor Agonists for Targeted Delivery of Antisense Oligonucleotides to Pancreatic Beta Cell. J. Am. Chem. Soc. 2021, 143, 3416–3429. [Google Scholar] [CrossRef]
- Min, H.S.; Kim, H.J.; Naito, M.; Ogura, S.; Toh, K.; Hayashi, K.; Kim, B.S.; Fukushima, S.; Anraku, Y.; Miyata, K.; et al. Systemic Brain Delivery of Antisense Oligonucleotides across the Blood–Brain Barrier with a Glucose-Coated Polymeric Nanocarrier. Angew. Chem. Int. Ed. 2020, 59, 8173–8180. [Google Scholar] [CrossRef]
- Yamayoshi, A.; Oyama, S.; Kishimoto, Y.; Konishi, R.; Yamamoto, T.; Kobori, A.; Harada, H.; Ashihara, E.; Sugiyama, H.; Murakami, A. Development of Antibody–Oligonucleotide Complexes for Targeting Exosomal Microrna. Pharmaceutics 2020, 12, 545. [Google Scholar] [CrossRef] [PubMed]
- Buntz, A.; Killian, T.; Schmid, D.; Seul, H.; Brinkmann, U.; Ravn, J.; Lindholm, M.; Knoetgen, H.; Haucke, V.; Mundigl, O. Quantitative Fluorescence Imaging Determines the Absolute Number of Locked Nucleic Acid Oligonucleotides Needed for Suppression of Target Gene Expression. Nucleic Acids Res. 2019, 47, 953–969. [Google Scholar] [CrossRef] [PubMed]
- Tan, W.; Loke, Y.H.; Stein, C.A.; Miller, P.; Colombini, M. Phosphorothioate Oligonucleotides Block the VDAC Channel. Biophys. J. 2007, 93, 1184–1191. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Tan, W.; Lai, J.C.; Miller, P.; Stein, C.A.; Colombini, M. Phosphorothioate Oligonucleotides Reduce Mitochondrial Outer Membrane Permeability to ADP. Am. J. Physiol. Cell Physiol. 2007, 292, C1388–C1397. [Google Scholar] [CrossRef][Green Version]
- Shen, W.; de Hoyos, C.L.; Migawa, M.T.; Vickers, T.A.; Sun, H.; Low, A.; Bell, T.A.; Rahdar, M.; Mukhopadhyay, S.; Hart, C.E.; et al. Chemical Modification of PS-ASO Therapeutics Reduces Cellular Protein-Binding and Improves the Therapeutic Index. Nat. Biotechnol. 2019, 37, 640–650. [Google Scholar] [CrossRef]
- Vickers, T.A.; Rahdar, M.; Prakash, T.P.; Crooke, S.T. Kinetic and Subcellular Analysis of PS-ASO/Protein Interactions with P54nrb and RNase H1. Nucleic Acids Res. 2019, 47, 10865–10880. [Google Scholar] [CrossRef]
- Liang, X.H.; Sun, H.; Shen, W.; Crooke, S.T. Identification and Characterization of Intracellular Proteins That Bind Oligonucleotides with Phosphorothioate Linkages. Nucleic Acids Res. 2015, 43, 2927–2945. [Google Scholar] [CrossRef]
- Liang, X.H.; Shen, W.; Sun, H.; Kinberger, G.A.; Prakash, T.P.; Nichols, J.G.; Crooke, S.T. Hsp90 Protein Interacts with Phosphorothioate Oligonucleotides Containing Hydrophobic 2′-Modifications and Enhances Antisense Activity. Nucleic Acids Res. 2016, 44, 3892–3907. [Google Scholar] [CrossRef]
- Vickers, T.A.; Crooke, S.T. Development of a Quantitative BRET Affinity Assay for Nucleic Acid-Protein Interactions. PLoS ONE 2016, 11, e0161930. [Google Scholar] [CrossRef]
- Zhang, L.; Bernardo, K.D.; Vickers, T.A.; Tian, J.; Liang, X.H.; Crooke, S.T. NAT10 and DDX21 Proteins Interact with RNase H1 and Affect the Performance of Phosphorothioate Oligonucleotides. Nucleic Acid Ther. 2022, 32, 280–299. [Google Scholar] [CrossRef]
- Wan, W.B.; Seth, P.P. The Medicinal Chemistry of Therapeutic Oligonucleotides. J. Med. Chem. 2016, 59, 9645–9667. [Google Scholar] [CrossRef] [PubMed]
- Hagedorn, P.H.; Pontoppidan, M.; Bisgaard, T.S.; Berrera, M.; Dieckmann, A.; Ebeling, M.; Møller, M.R.; Hudlebusch, H.; Jensen, M.L.; Hansen, H.F.; et al. Identifying and Avoiding Off-Target Effects of RNase H-Dependent Antisense Oligonucleotides in Mice. Nucleic Acids Res. 2018, 46, 5366–5380. [Google Scholar] [CrossRef] [PubMed]
- Kasuya, T.; Hori, S.I.; Watanabe, A.; Nakajima, M.; Gahara, Y.; Rokushima, M.; Yanagimoto, T.; Kugimiya, A. Ribonuclease H1-Dependent Hepatotoxicity Caused by Locked Nucleic Acid-Modified Gapmer Antisense Oligonucleotides. Sci. Rep. 2016, 6, 30377. [Google Scholar] [CrossRef] [PubMed]
- Kamola, P.J.; Maratou, K.; Wilson, P.A.; Rush, K.; Mullaney, T.; McKevitt, T.; Evans, P.; Ridings, J.; Chowdhury, P.; Roulois, A.; et al. Strategies for In Vivo Screening and Mitigation of Hepatotoxicity Associated with Antisense Drugs. Mol. Ther. Nucleic Acids 2017, 8, 383–394. [Google Scholar] [CrossRef]
| Plasma Protein | Kd (10−6 M) (FP Assay) | MW (kDa) | Plasma Concentration (10−6 M) |
|---|---|---|---|
| Albumin | 12.7 | 69 | 600 |
| Immunogloblin gamma-1 heavy chain (IgG) | 1.6 | 150 | 75 |
| Apolipoprotein A-I (ApoA-I) | 5.3 | 30 | 40 |
| Apolipoprotein A-II (ApoA-II) | >500 | 11 | 24 |
| Complement Factor C3 | 0.5 | 187 | 20 |
| Transferrin | 7 | 77 | 12 |
| Alpha-1-Antitrypsin | >100 | 46 | 11 |
| Haptoglobin | 54.7 | 45 | 11 |
| Hemopexin | 13.9 | 52 | 9.9 |
| Fibrinogen | 0.87 | 24 | 9 |
| Alpha-2-macroglobulin (A2M) | 0.05 | 163 | 6 |
| Transthyretin (TTR) | 132 | 16 | 6 |
| Antithrombin III (ATIII) | 8.7 | 52 | 3.5 |
| Alpha-1-antichymotrypsin (ACT) | 21.3 | 47 | 3.3 |
| Beta-2-Glycoprotein | 57.1 | 38 | 2.7 |
| Ceruloplasmin | 22.6 | 122 | 2 |
| Alpha-1-Acid Glycoprotein | >500 | 23 | 1.7 |
| Complement Component C1q | 3.4 | 26 | 1.6 |
| Complement Factor C4 | 0.43 | 192 | 1.4 |
| Histidine–rich glycoprotein | 0.009 | 59 | 1.3 |
| Plasminogen | 2.1 | 90 | 1.2 |
| Fibronectin (FN) | 0.54 | 272 | 0.9 |
| Apolipoprotein B-100 (Apo B-100) | >10 | 515 | 0.7 |
| Factor H | 0.5 | 139 | 0.6 |
| Apolipoprotein E (Apo-E) | 0.027 | 36 | 0.5 |
| Factor V | 0.032 | 251 | 0.02 |
| Intracellular protein | Kd (10−6 M) (BRET assay) | MW (kDa) | |
| cEt | MOE | ||
| Leucine-rich PPR motif-containing protein, mitochondrial (LRPPRC) | 0.16 | 0.77 | 41 |
| RNA-binding protein FUS (FUS) | 0.6 | 1.8 | 52 |
| Proprotein convertase subtilisin/kexin type 4 (PC4) | 1.1 | 6.1 | 14 |
| 60S ribosomal protein L5 (RPL5) | 1.3 | 3.7 | 20 |
| Nucleolin (NCL [RBD 1-4]) | 1.7 | 0.009 | 39 |
| Splicing factor, proline- and glutamine-rich (SFPQ) | 2.7 | 3.7 | 76 |
| X-ray repair cross-complementing protein 6 (Ku70) | 4 | 15 | 69 |
| Ribonulease H1 (RNase H1) | 5 | 2 | 32 |
| Lupus La protein (La) | 5 | 9.3 | 46 |
| Non-POU domain-containing octamer-binding protein (NonO protein, P54nrb) | 9.3 | 82.9 | 54 |
| 60S ribosomal protein L11 (RPL11) | 17.4 | 15.7 | 34 |
| Heat shock protein 90 (HSP90 [mid]) | 43 | 167 | 47 |
| Staufen | 100 | - | 55 |
| T-complex protein 1 subunit beta (TCP1-B) | 113 | 398 | 57 |
| Actin, cytoplasmic 1 (ACTB) | 295 | 252 | 42 |
| Nuclear matrix protein 1 (NMP1) | >1000 | >1000 | 28 |
| Annexin A2 (ANXA2) | >1000 | >1000 | 38 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Terada, C.; Kawamoto, S.; Yamayoshi, A.; Yamamoto, T. Chemistry of Therapeutic Oligonucleotides That Drives Interactions with Biomolecules. Pharmaceutics 2022, 14, 2647. https://doi.org/10.3390/pharmaceutics14122647
Terada C, Kawamoto S, Yamayoshi A, Yamamoto T. Chemistry of Therapeutic Oligonucleotides That Drives Interactions with Biomolecules. Pharmaceutics. 2022; 14(12):2647. https://doi.org/10.3390/pharmaceutics14122647
Chicago/Turabian StyleTerada, Chisato, Seiya Kawamoto, Asako Yamayoshi, and Tsuyoshi Yamamoto. 2022. "Chemistry of Therapeutic Oligonucleotides That Drives Interactions with Biomolecules" Pharmaceutics 14, no. 12: 2647. https://doi.org/10.3390/pharmaceutics14122647
APA StyleTerada, C., Kawamoto, S., Yamayoshi, A., & Yamamoto, T. (2022). Chemistry of Therapeutic Oligonucleotides That Drives Interactions with Biomolecules. Pharmaceutics, 14(12), 2647. https://doi.org/10.3390/pharmaceutics14122647







