Prospective Validation and Refinement of a Population Pharmacokinetic Model of Fludarabine in Children and Young Adults Undergoing Hematopoietic Cell Transplantation
Abstract
1. Introduction
2. Materials and Methods
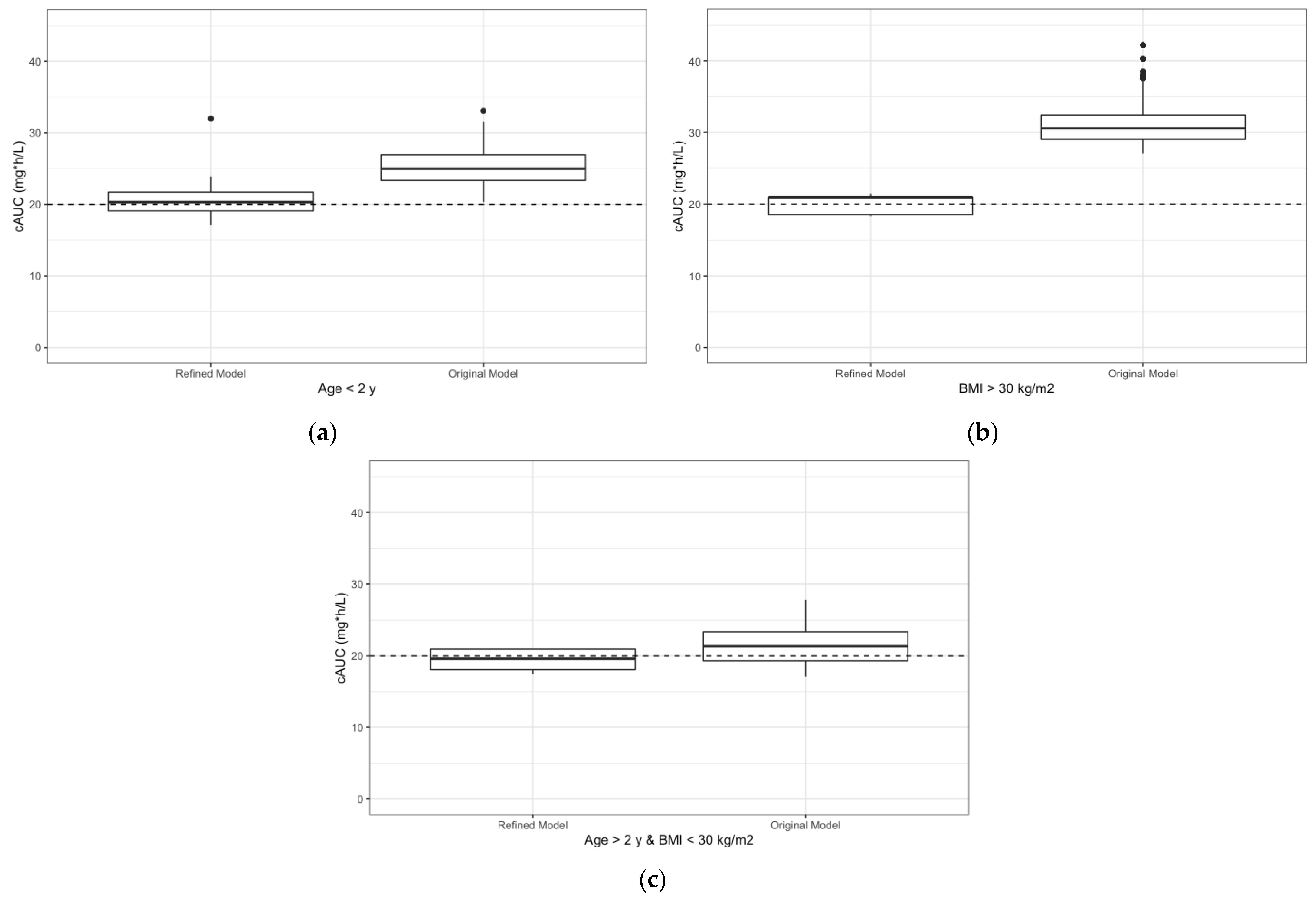
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
References
- Annaloro, C.; Costa, A.; Fracchiolla, N.S.; Mometto, G.; Artuso, S.; Saporiti, G.; Tagliaferri, E.; Grifoni, F.; Onida, F.; Cortelezzi, A. Severe fludarabine neurotoxicity after reduced intensity conditioning regimen to allogeneic hematopoietic stem cell transplantation: A case report. Clin. Case Rep. 2015, 3, 650–655. [Google Scholar] [CrossRef] [PubMed]
- Avramis, V.I.; Wiersma, S.; Krailo, M.D.; Ramilo-Torno, L.V.; Sharpe, A.; Liu-Mares, W.; Kowck, R.; Reaman, G.H.; Sato, J.K. Pharmacokinetic and pharmacodynamic studies of fludarabine and cytosine arabinoside administered as loading boluses followed by continuous infusions after a phase I/II study in pediatric patients with relapsed leukemias. The Children’s Cancer Group. Clin. Cancer Res. 1998, 4, 45–52. [Google Scholar] [PubMed]
- Avramis, V.I.; Champagne, J.; Sato, J.; Krailo, M.; Ettinger, L.J.; Poplack, D.G.; Finkelstein, J.; Reaman, G.; Hammond, G.D.; Holcenberg, J.S. Pharmacology of fludarabine phosphate after a phase I/II trial by a loading bolus and continuous infusion in pediatric patients. Cancer Res. 1990, 50, 7226–7231. [Google Scholar] [PubMed]
- Salinger, D.H.; Blough, D.K.; Vicini, P.; Anasetti, C.; O’Donnell, P.V.; Sandmaier, B.M.; McCune, J.S. A Limited Sampling Schedule to Estimate Individual Pharmacokinetic Parameters of Fludarabine in Hematopoietic Cell Transplant Patients. Clin. Cancer Res. 2009, 15, 5280–5287. [Google Scholar] [CrossRef] [PubMed]
- Long-Boyle, J.R.; Green, K.G.; Brunstein, C.G.; Cao, Q.; Rogosheske, J.; Weisdorf, D.J.; Miller, J.S.; Wagner, J.E.; McGlave, P.B.; Jacobson, P.A. High fludarabine exposure and relationship with treatment-related mortality after nonmyeloablative hematopoietic cell transplantation. Bone Marrow Transplant. 2011, 46, 20–26. [Google Scholar] [CrossRef] [PubMed]
- Bornhäuser, M.; Storer, B.; Slattery, J.T.; Appelbaum, F.R.; Deeg, H.J.; Hansen, J.; Martin, P.J.; McDonald, G.B.; Nichols, W.G.; Radich, J.; et al. Conditioning with fludarabine and targeted busulfan for transplantation of allogeneic hematopoietic stem cells. Blood 2003, 102, 820–826. [Google Scholar] [CrossRef] [PubMed]
- Langenhorst, J.B.; Dorlo, T.P.C.; van Maarseveen, E.M.; Nierkens, S.; Kuball, J.; Boelens, J.J.; van Kesteren, C.; Huitema, A.D.R. Population Pharmacokinetics of Fludarabine in Children and Adults during Conditioning Prior to Allogeneic Hematopoietic Cell Transplantation. Clin. Pharmacokinet. 2019, 58, 627–637. [Google Scholar] [CrossRef] [PubMed]
- Ivaturi, V.; Dvorak, C.C.; Chan, D.; Liu, T.; Cowan, M.J.; Wahlstrom, J.; Stricherz, M.; Jennissen, C.; Orchard, P.J.; Tolar, J.; et al. Pharmacokinetics and Model-Based Dosing to Optimize Fludarabine Therapy in Pediatric Hematopoietic Cell Transplant Recipients. Biol. Blood Marrow Transplant. 2017, 23, 1701–1713. [Google Scholar] [CrossRef] [PubMed]
- Langenhorst, J.B.; Van Kesteren, C.; Van Maarseveen, E.M.; Dorlo, T.P.C.; Nierkens, S.; Lindemans, C.A.; De Witte, M.A.; Van Rhenen, A.; Raijmakers, R.; Bierings, M.; et al. Fludarabine exposure in the conditioning prior to allogeneic hematopoietic cell transplantation predicts outcomes. Blood Adv. 2019, 3, 2179–2187. [Google Scholar] [CrossRef] [PubMed]
- Al-Sallami, H.S.; Goulding, A.; Grant, A.; Taylor, R.; Holford, N.; Duffull, S.B. Prediction of Fat-Free Mass in Children. Clin. Pharmacokinet. 2015, 54, 1169–1178. [Google Scholar] [CrossRef] [PubMed]
- Huang, L.; Lizak, P.; Dvorak, C.C.; Aweeka, F.; Long-Boyle, J. Simultaneous determination of fludarabine and clofarabine in human plasma by LC–MS/MS. J. Chromatogr. B 2014, 960, 194–199. [Google Scholar] [CrossRef] [PubMed]
- Clinical Growth Charts. Available online: https://www.cdc.gov/growthcharts/clinical_charts.htm (accessed on 8 August 2022).
- Kearns, G.L.; Abdel-Rahman, S.M.; Alander, S.W.; Blowey, D.L.; Leeder, J.S.; Kauffman, R.E. Developmental Pharmacology—Drug Disposition, Action, and Therapy in Infants and Children. N. Engl. J. Med. 2003, 349, 1157–1167. [Google Scholar] [CrossRef] [PubMed]
| New Subjects for Model Validation | Combined New and Original Subjects for Model Refinement | ||
|---|---|---|---|
| Characteristic | Value | Characteristic | Value |
| Participants—n | 53 | Participants—n | 186 |
| Dosing Strategy—n (%) | Dosing Strategy—n (%) | ||
| Traditional | 29 (55%) | Traditional | 162 (87%) |
| 40 mg/m2 | 20 | 40 mg/m2 | 75 |
| 12.5–30 mg/m2 | 6 | 12.5–30 mg/m2 | 46 |
| 0.9–1.33 mg/kg | 3 | 0.9–1.33 mg/kg | 41 |
| Model-based dosing | 24 (45%) | Model-based dosing | 24 (13%) |
| Sex—n (%) | Sex—n (%) | ||
| Females | 19 (36%) | Females | 80 (43%) |
| Males | 34 (64%) | Males | 106 (57%) |
| Weight, median (range), kg | 23.6 (7.3–135) | Weight, median (range), kg | 21.6 (3–135) |
| Height, median (range), cm | 121.7 (67–186.1) | Height, median (range), cm | 112.4 (50–186.7) |
| Age, median (range), year | 8.0 (0.4–22)(7 subjects ≤ 2 year) | Age, median (range), year | 6.4 (0.2–22)(55 subjects ≤ 2 year) |
| CrCL, median (range), ml/min/1.73 m2 | 137 (53–337) | CrCL, median (range), mL/min/1.73 m2 | 149 (120–193) |
| Final Model | Bootstrap | |||
|---|---|---|---|---|
| Parameter | Value | RSE * | Value | 95% CI |
| Effect of CrCL f-ara-a CL | 0.00186 | 32.8 | 0.0018 | 0.001–0.004 |
| Vc (L/12 kg of FFM) | 11.5 | 4.9 | 11.4 | 10.22–12.57 |
| Intercompartmental Clearance (L/h/12 kg of FFM) | 1.47 | 9.3 | 1.48 | 1.23–1.79 |
| Vp (L/12 kg of FFM) | 8.48 | 4.6 | 8.53 | 7.75–9.29 |
| Maturation Function Shape | 3.54 | 13.8 | 3.57 | 2.65–4.75 |
| f-ara-a additive residual unexplained variability | 0.36 | 12.6 | 0.36 | 0.27–0.45 |
| Interindividual Variability on CL † | 0.117 | 20.7 | 0.118 | 0.07–0.26 |
| Interindividual Variability on Vc † | 0.303 | 18.1 | 0.314 | 0.21–0.43 |
| Interindividual Variability Correlation CL-Vc | 0.141 | 0.149 | 0.09–0.21 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Brooks, J.T.; Solans, B.P.; Lu, Y.; Kharbanda, S.; Dvorak, C.C.; Lalefar, N.; Long, S.; Gupta, A.O.; Horn, B.; Lamba, J.K.; et al. Prospective Validation and Refinement of a Population Pharmacokinetic Model of Fludarabine in Children and Young Adults Undergoing Hematopoietic Cell Transplantation. Pharmaceutics 2022, 14, 2462. https://doi.org/10.3390/pharmaceutics14112462
Brooks JT, Solans BP, Lu Y, Kharbanda S, Dvorak CC, Lalefar N, Long S, Gupta AO, Horn B, Lamba JK, et al. Prospective Validation and Refinement of a Population Pharmacokinetic Model of Fludarabine in Children and Young Adults Undergoing Hematopoietic Cell Transplantation. Pharmaceutics. 2022; 14(11):2462. https://doi.org/10.3390/pharmaceutics14112462
Chicago/Turabian StyleBrooks, Jordan T., Belen P. Solans, Ying Lu, Sandhya Kharbanda, Christopher C. Dvorak, Nahal Lalefar, Susie Long, Ashish O. Gupta, Biljana Horn, Jatinder K. Lamba, and et al. 2022. "Prospective Validation and Refinement of a Population Pharmacokinetic Model of Fludarabine in Children and Young Adults Undergoing Hematopoietic Cell Transplantation" Pharmaceutics 14, no. 11: 2462. https://doi.org/10.3390/pharmaceutics14112462
APA StyleBrooks, J. T., Solans, B. P., Lu, Y., Kharbanda, S., Dvorak, C. C., Lalefar, N., Long, S., Gupta, A. O., Horn, B., Lamba, J. K., Huang, L., Apsel-Winger, B., Keizer, R. J., Savic, R., & Long-Boyle, J. (2022). Prospective Validation and Refinement of a Population Pharmacokinetic Model of Fludarabine in Children and Young Adults Undergoing Hematopoietic Cell Transplantation. Pharmaceutics, 14(11), 2462. https://doi.org/10.3390/pharmaceutics14112462







