Multiple HPV Infections and Viral Load Association in Persistent Cervical Lesions in Mexican Women
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. Sample Collection and DNA Extraction
2.3. HPV Genotyping and Viral Load
2.4. Follow-Up Samples
2.5. Statistical Analysis
3. Results
3.1. Sample Collection
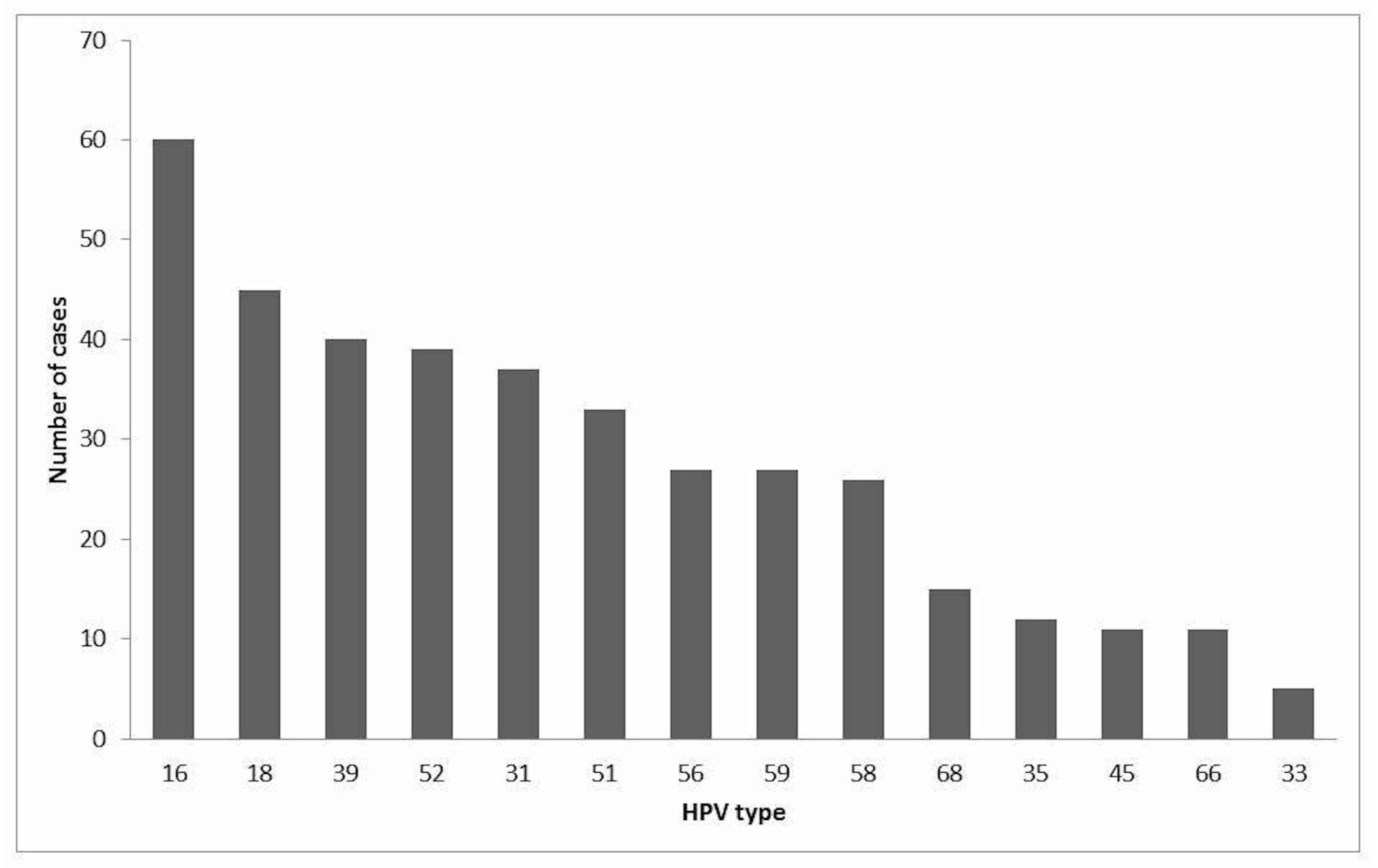
3.2. Pap Smears and HPV Genotyping at the First Consultation
3.3. Multiple HPV Infections at the First Consultation
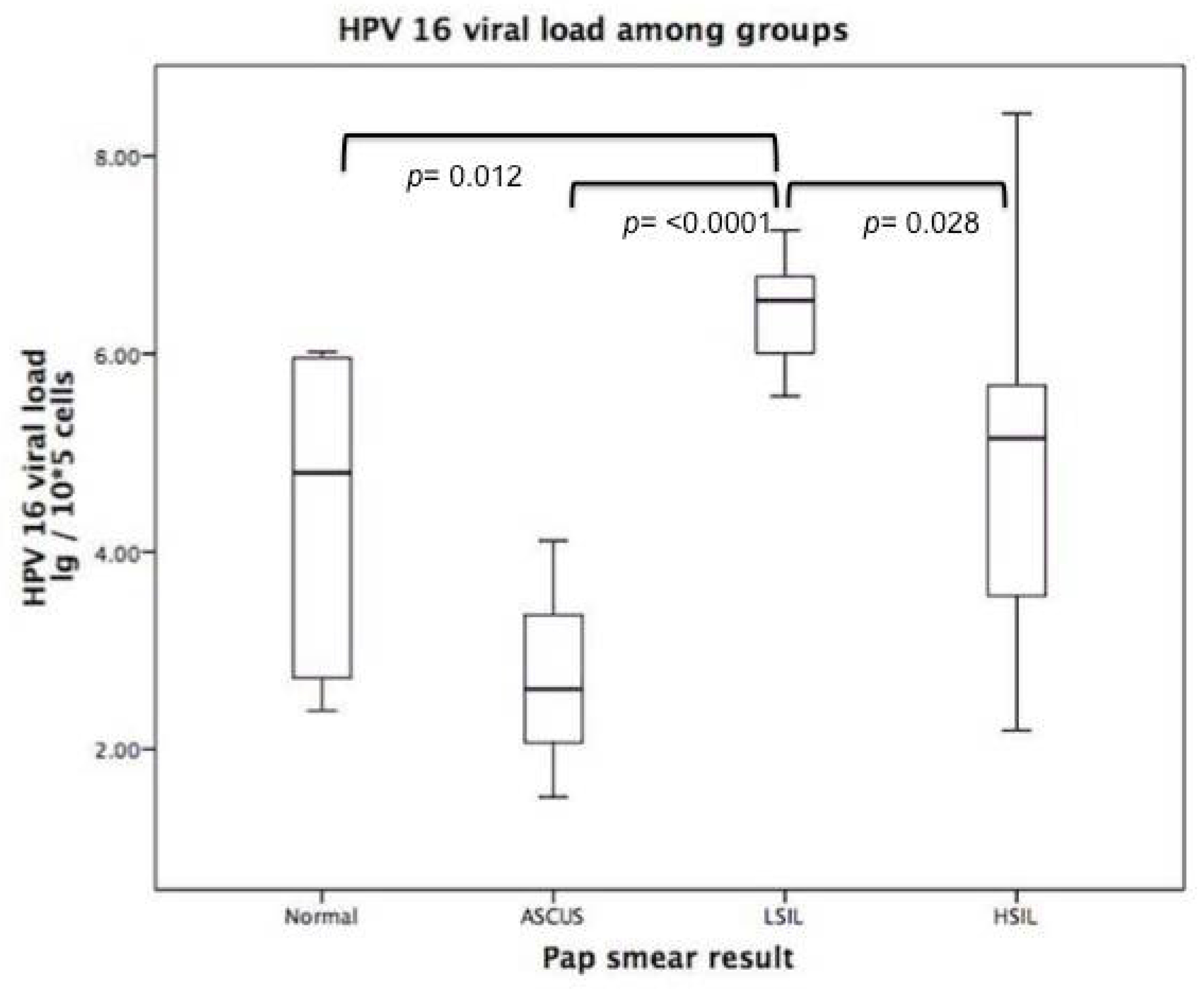
3.4. HPV Viral Load
3.5. HPV-Positive Patients Follow-Up
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Burger, E.A.; Smith, M.A.; Killen, J.; Sy, S.; Simms, K.T.; Canfell, K.; Kim, J.J. Projected time to elimination of cervical cancer in the USA: A comparative modelling study. Lancet Public Health 2020. [Google Scholar] [CrossRef]
- Baezconde-Garbanati, L.; Agurto, I.; Gravitt, P.E.; Luciani, S.; Murphy, S.; Ochoa, C.; Gallegos, K.; Barahona, R.; Rodriguez, Y. Barriers and innovative interventions for early detection of cervical cancer. Salud Publica México 2019, 61, 456–460. [Google Scholar] [CrossRef] [PubMed]
- Hurtado-Salgado, E.; Ortiz-Panozo, E.; Salmeron, J.; Saavedra-Lara, N.; Kuri-Morales, P.; Pesqueira-Villegas, E.; Luna-Gordillo, R.; Franco, E.L.; Lazcano-Ponce, E. Use of HPV testing in cervical cancer screening services in Mexico, 2008–2018: A nationwide database study. Salud Publica México 2018, 60, 722–733. [Google Scholar] [CrossRef] [PubMed]
- Lazcano-Ponce, E.; Palacio-Mejia, L.S.; Allen-Leigh, B.; Yunes-Diaz, E.; Alonso, P.; Schiavon, R.; Hernandez-Avila, M. Decreasing cervical cancer mortality in Mexico: Effect of Papanicolaou coverage, birthrate, and the importance of diagnostic validity of cytology. Cancer Epidemiol Biomark. Prev. 2008, 17, 2808–2817. [Google Scholar] [CrossRef] [PubMed]
- Bruni, L.; Albero, G.; Serrano, B.; Mena, M.; Gómez, D.; Muñoz, J.; Bosch, F.X.; de Sanjosé, S.; ICO/IARC Information Centre on HPV and Cancer (HPV Information Centre). Human Papillomavirus and Related Diseases in the World. Summ. Rep. 2019. [Google Scholar]
- Bodily, J.; Laimins, L.A. Persistence of human papillomavirus infection: Keys to malignant progression. Trends Microbiol. 2011, 19, 33–39. [Google Scholar] [CrossRef] [PubMed]
- Human Papillomavirus and Related Diseases in Mexico. Summary Report—IARC Information Centre on HPV and Cancer (HPV Information Centre). Available online: http://www.hpvcentre.net/statistics/reports/MEX.pdf (accessed on 24 November 2019).
- Makuza, J.D.; Nsanzimana, S.; Muhimpundu, M.A.; Pace, L.E.; Ntaganira, J.; Riedel, D.J. Prevalence and risk factors for cervical cancer and pre-cancerous lesions in Rwanda. Pan Afr. Med. J. 2015, 22, 26. [Google Scholar] [CrossRef]
- Sasagawa, T.; Takagi, H.; Makinoda, S. Immune responses against human papillomavirus (HPV) infection and evasion of host defense in cervical cancer. J. Infect. Chemother. 2012, 18, 807–815. [Google Scholar] [CrossRef]
- Arbyn, M.; Tommasino, M.; Depuydt, C.; Dillner, J. Are 20 human papillomavirus types causing cervical cancer? J. Pathol. 2014, 234, 431–435. [Google Scholar] [CrossRef]
- OMS. Available online: http://www.who.int/immunization/diseases/hpv/en/ (accessed on 13 September 2017).
- Smith Jennifer, S.; Lindsay, L.; Hoots, B.; Keys, J.; Franceschi, S.; Winer, R.; Clifford Gary, M. Human papillomavirus type distribution in invasive cervical cancer and high-grade cervical lesions: A meta-analysis update. Int. J. Cancer 2007, 121, 621–632. [Google Scholar] [CrossRef]
- Ciapponi, A.; Bardach, A.; Glujovsky, D.; Gibbons, L.; Picconi, M.A. Type-Specific HPV Prevalence in Cervical Cancer and High-Grade Lesions in Latin America and the Caribbean: Systematic Review and Meta-Analysis. PLoS ONE 2011, 6, e25493. [Google Scholar] [CrossRef]
- Fajardo-Ramírez Oscar, R.; Barboza-Cerda María, C.; Ortiz-López, R.; Rojas-Martínez, A.; Garza-Rodríguez María, L.; Sepúlveda-Flores, A.; González-Guerrero Juan, F.; Bernal-Silva, S.; Cerda-Flores Ricardo, M.; Calleja-Macías Itzel, E.; et al. Prevalence and 3-year persistence of human papillomavirus serotypes in asymptomatic patients in Northern Mexico. Int. J. Gynecol. Obstet. 2016, 136, 40–46. [Google Scholar] [CrossRef] [PubMed]
- Illades-Aguiar, B.; Alarcon-Romero Ldel, C.; Antonio-Vejar, V.; Zamudio-Lopez, N.; Sales-Linares, N.; Flores-Alfaro, E.; Fernandez-Tilapa, G.; Vences-Velazquez, A.; Munoz-Valle, J.F.; Leyva-Vazquez, M.A. Prevalence and distribution of human papillomavirus types in cervical cancer, squamous intraepithelial lesions, and with no intraepithelial lesions in women from Southern Mexico. Gynecol. Oncol. 2010, 117, 291–296. [Google Scholar] [CrossRef]
- Peralta-Rodriguez, R.; Romero-Morelos, P.; Villegas-Ruiz, V.; Mendoza-Rodriguez, M.; Taniguchi-Ponciano, K.; Gonzalez-Yebra, B.; Marrero-Rodriguez, D.; Salcedo, M. Prevalence of human papillomavirus in the cervical epithelium of Mexican women: Meta-analysis. Infect. Agents Cancer 2012, 7, 34. [Google Scholar] [CrossRef] [PubMed]
- Giuliano, A.R.; Papenfuss, M.; Abrahamsen, M.; Denman, C.; de Zapien, J.G.; Henze, J.L.N.; Ortega, L.; de Galaz, E.M.B.; Stephan, J.; Feng, J.; et al. Human Papillomavirus Infection at the United States-Mexico Border. Cancer Epidemiol. Biomark. Prev. 2001, 10, 1129. [Google Scholar]
- PAHO. Centro Nacional de Equidad de Género y Salud Reproductiva Secretaría de Salud México. Experiencia de México Introducción de vacuna preventiva y prueba de detección del Virus del Papiloma Humano (VPH) Programa de Cáncer Cérvico Uterino; Pan American Health Organization: Ciudad de México, México, 2010. [Google Scholar]
- Cuzick, J.; Wheeler, C. Need for expanded HPV genotyping for cervical screening. Papillomavirus Res. 2016, 2, 112–115. [Google Scholar] [CrossRef] [PubMed]
- Secretaría de Salud. Available online: https://www.gob.mx/salud/acciones-y-programas/cancer-de-cuello-uterino-prevencion-y-deteccion-oportuna (accessed on 5 March 2020).
- Depuydt, C.E.; Jonckheere, J.; Berth, M.; Salembier, G.M.; Vereecken, A.J.; Bogers, J.J. Serial type-specific human papillomavirus (HPV) load measurement allows differentiation between regressing cervical lesions and serial virion productive transient infections. Cancer Med. 2015, 4, 1294–1302. [Google Scholar] [CrossRef]
- Chang, M.S.; Oh, S.; Jung, E.J.; Park, J.H.; Jeon, H.W.; Lee, T.S.; Kim, J.H.; Choi, E.; Byeon, S.J.; Park, I.A. High-risk human papillomavirus load and biomarkers in cervical intraepithelial neoplasia and cancer. Acta Pathol. Microbiol. Immunol. Scand. 2014, 122, 427–436. [Google Scholar] [CrossRef]
- Sun, C.-A.; Lai, H.-C.; Chang, C.-C.; Neih, S.; Yu, C.-P.; Chu, T.-Y. The Significance of Human Papillomavirus Viral Load in Prediction of Histologic Severity and Size of Squamous Intraepithelial Lesions of Uterine Cervix. Gynecol. Oncol. 2001, 83, 95–99. [Google Scholar] [CrossRef]
- Sun, Z.; Zhang, R.; Liu, Z.; Liu, C.; Li, X.; Zhou, W.; Yang, L.; Ruan, Q.; Zhang, X. Development of a fluorescence–based multiplex genotyping method for simultaneous determination of human papillomavirus infections and viral loads. BMC Cancer 2015, 15, 860. [Google Scholar] [CrossRef] [PubMed]
- Castle, P.E.; Schiffman, M.; Gravitt, P.E.; Kendall, H.; Fishman, S.; Dong, H.; Hildesheim, A.; Herrero, R.; Bratti, M.C.; Sherman, M.E.; et al. Comparisons of HPV DNA detection by MY09/11 PCR methods. J. Med Virol. 2002, 68, 417–423. [Google Scholar] [CrossRef]
- Peyton, C.L.; Gravitt, P.E.; Hunt, W.C.; Hundley, R.S.; Zhao, M.; Apple, R.J.; Wheeler, C.M. Determinants of genital human papillomavirus detection in a US population. J. Infect. Dis. 2001, 183, 1554–1564. [Google Scholar] [CrossRef] [PubMed]
- Kuevda, D.A.; Shipulina, O.Y.; Minkina, G.N.; Piksasova, O.; Dvoryaninova, O.Y.; NEG, B.V.A.; Litvyakov, N.V. Genetic aspects of determining papillomavirus infection in tumor and adjacent tissue of patients with squamous cell carcinoma of the larynx // (Voprosy virusologii). Virolo. issues 2016, 61. [Google Scholar]
- Lu, S.; Cong, X.; Li, M.; Chang, F.; Ma, L.; Cao Yong, T. Distribution of high-risk human papillomavirus genotypes in HPV-infected women in Beijing, China. J. Med. Virol. 2015, 87, 504–507. [Google Scholar] [CrossRef] [PubMed]
- Flores-Miramontes, M.G.; Torres-Reyes, L.A.; Aguilar-Lemarroy, A.; Vallejo-Ruiz, V.; Pina-Sanchez, P.; Cortes-Gutierrez, E.; Reyes-Leyva, J.; Jave-Suarez, L.F. HPV genotypes prevalence in Mexico and worldwide detected by Linear Array. Revista Médica del Instituto Mexicano del Seguro Social 2015, 53 (Suppl. 2), S122–S130. [Google Scholar] [PubMed]
- Campos, R.G.; Malacara Rosas, A.; Gutierrez Santillan, E.; Delgado Gutierrez, M.; Torres Orozco, R.E.; Garcia Martinez, E.D.; Torres Bernal, L.F.; Rosas Cabral, A. Unusual prevalence of high-risk genotypes of human papillomavirus in a group of women with neoplastic lesions and cervical cancer from Central Mexico. PLoS ONE 2019, 14, e0215222. [Google Scholar] [CrossRef] [PubMed]
- Rudolph, S.E.; Lorincz, A.; Wheeler, C.M.; Gravitt, P.; Lazcano-Ponce, E.; Torres-Ibarra, L.; Leon-Maldonado, L.; Ramirez, P.; Rivera, B.; Hernandez, R.; et al. Population-based prevalence of cervical infection with human papillomavirus genotypes 16 and 18 and other high risk types in Tlaxcala, Mexico. BMC Infect. Dis. 2016, 16, 461. [Google Scholar] [CrossRef]
- Mittal, S.; Basu, P.; Muwonge, R.; Banerjee, D.; Ghosh, I.; Sengupta Mitali, M.; Das, P.; Dey, P.; Mandal, R.; Panda, C.; et al. Risk of high-grade precancerous lesions and invasive cancers in high-risk HPV-positive women with normal cervix or CIN 1 at baseline—A population-based cohort study. Int. J. Cancer 2017, 140, 1850–1859. [Google Scholar] [CrossRef]
- Oh, H.Y.; Seo, S.-S.; Kim, M.K.; Lee, D.O.; Chung, Y.K.; Lim, M.C.; Kim, J.-Y.; Lee, C.W.; Park, S.-Y. Synergistic Effect of Viral Load and Alcohol Consumption on the Risk of Persistent High-Risk Human Papillomavirus Infection. PLoS ONE 2014, 9, e104374. [Google Scholar] [CrossRef]
- Hirth, J.; McGrath, C.J.; Kuo, Y.F.; Rupp, R.E.; Starkey, J.M.; Berenson, A.B. Impact of human papillomavirus vaccination on racial/ethnic disparities in vaccine-type human papillomavirus prevalence among 14–26year old females in the U.S. Vaccine 2018, 36, 7682–7688. [Google Scholar] [CrossRef]
- Pirtea, L.; Grigoraş, D.; Matusz, P.; Pirtea, M.; Moleriu, L.; Tudor, A.; Ilina, R.; Secoşan, C.; Horhat, F.; Mazilu, O. Age and HPV type as risk factors for HPV persistence after loop excision in patients with high grade cervical lesions: An observational study. BMC Surg. 2016, 16, 70. [Google Scholar] [CrossRef]
- Mastutik, G.; Alia, R.; Rahniayu, A.; Rahaju, A.S.; Kurniasari, N.; Putra, S.T. Genotyping of Human Pappilomavirus in Cervical Precancerous Lesion and Squamous Cell Carcinoma at Dr. Soetomo Hospital, Surabaya, Indonesia. Afr. J. Infect. Dis. 2018, 12 (Suppl. 1), 7–12. [Google Scholar] [CrossRef] [PubMed]
- Salazar, K.L.; Zhou, H.S.; Xu, J.; Peterson, L.E.; Schwartz, M.R.; Mody, D.R.; Ge, Y. Multiple Human Papilloma Virus Infections and Their Impact on the Development of High-Risk Cervical Lesions. Acta Cytol. 2015, 59, 391–398. [Google Scholar] [CrossRef] [PubMed]
- Lorincz, A.T.; Castle, P.E.; Sherman, M.E.; Scott, D.R.; Glass, A.G.; Wacholder, S.; Rush, B.B.; Gravitt, P.E.; Schussler, J.E.; Schiffman, M. Viral load of human papillomavirus and risk of CIN3 or cervical cancer. Lancet 2002, 360, 228–229. [Google Scholar] [CrossRef]
- De Brot, L.; Pellegrini, B.; Moretti, S.T.; Carraro, D.M.; Soares, F.A.; Rocha, R.M.; Baiocchi, G.; da Cunha, I.W.; de Andrade, V.P. Infections with multiple high-risk HPV types are associated with high-grade and persistent low-grade intraepithelial lesions of the cervix. Cancer Cytopathol. 2017, 125, 138–143. [Google Scholar] [CrossRef]
- Manawapat-Klopfer, A.; Wang, L.; Haedicke-Jarboui, J.; Stubenrauch, F.; Munk, C.; Thomsen, L.T.; Martus, P.; Kjaer, S.K.; Iftner, T. HPV16 viral load and physical state measurement as a potential immediate triage strategy for HR-HPV-infected women: A study in 644 women with single HPV16 infections. Am. J. Cancer Res. 2018, 8, 715–722. [Google Scholar] [PubMed]
- Carcopino, X.; Henry, M.; Mancini, J.; Giusiano, S.; Boubli, L.; Olive, D.; Tamalet, C. Significance of HPV 16 and 18 viral load quantitation in women referred for colposcopy. J. Med Virol. 2011, 84, 306–313. [Google Scholar] [CrossRef]
- Long, W.; Yang, Z.; Li, X.; Chen, M.; Liu, J.; Zhang, Y.; Sun, X. HPV-16, HPV-58, and HPV-33 are the most carcinogenic HPV genotypes in Southwestern China and their viral loads are associated with severity of premalignant lesions in the cervix. Virol. J. 2018, 15, 94. [Google Scholar] [CrossRef]
- Huang, C.-G.; Lee, L.-A.; Tsao, K.-C.; Liao, C.-T.; Yang, L.-Y.; Kang, C.-J.; Chang, K.-P.; Huang, S.-F.; Chen, I.H.; Yang, S.-L.; et al. Human papillomavirus 16/18 E7 viral loads predict distant metastasis in oral cavity squamous cell carcinoma. J. Clin. Virol. 2014, 61, 230–236. [Google Scholar] [CrossRef]
- Chang, L.; He, X.; Yu, G.; Wu, Y. Effectiveness of HPV 16 viral load and the E2/E6 ratio for the prediction of cervical cancer risk among Chinese women. J. Med. Virol. 2013, 85, 646–654. [Google Scholar] [CrossRef]
- Sundström, K.; Ploner, A.; Dahlström, L.A.; Palmgren, J.; Dillner, J.; Adami, H.-O.; Ylitalo, N.; Sparén, P. Prospective Study of HPV16 Viral Load and Risk of In Situ and Invasive Squamous Cervical Cancer. Cancer Epidemiol. Biomark. Prev. 2013, 22, 150–158. [Google Scholar] [CrossRef]
- Fu Xi, L.; Schiffman, M.; Ke, Y.; Hughes, J.P.; Galloway, D.A.; He, Z.; Hulbert, A.; Winer, R.L.; Koutsky, L.A.; Kiviat, N.B. Type-dependent association between risk of cervical intraepithelial neoplasia and viral load of oncogenic human papillomavirus types other than types 16 and 18. Int. J. Cancer 2017, 140, 1747–1756. [Google Scholar] [CrossRef] [PubMed]
- Kulmala, S.M.; Syrjanen, S.M.; Gyllensten, U.B.; Shabalova, I.P.; Petrovichev, N.; Tosi, P.; Syrjanen, K.J.; Johansson, B.C. Early integration of high copy HPV16 detectable in women with normal and low grade cervical cytology and histology. J. Clin. Pathol. 2006, 59, 513–517. [Google Scholar] [CrossRef] [PubMed]
- Bennett, R.; Cerigo, H.; Coutlée, F.; Roger, M.; Franco, E.L.; Brassard, P. Incidence, Persistence, and Determinants of Human Papillomavirus Infection in a Population of Inuit Women in Northern Quebec. Sex. Transm. Dis. 2015, 42, 272–278. [Google Scholar] [CrossRef] [PubMed]
- Stensen, S.; Kjaer Susanne, K.; Jensen Signe, M.; Frederiksen, K.; Junge, J.; Iftner, T.; Munk, C. Factors associated with type-specific persistence of high-risk human papillomavirus infection: A population-based study. Int. J. Cancer 2015, 138, 361–368. [Google Scholar] [CrossRef] [PubMed]
- Rositch, A.F.; Koshiol, J.; Hudgens, M.G.; Razzaghi, H.; Backes, D.M.; Pimenta, J.M.; Franco, E.L.; Poole, C.; Smith, J.S. Patterns of persistent genital human papillomavirus infection among women worldwide: A literature review and meta-analysis. Int. J. Cancer 2013, 133, 1271–1285. [Google Scholar] [CrossRef] [PubMed]
- Bouvard, V.; Baan, R.; Straif, K.; Grosse, Y.; Secretan, B.; Ghissassi, F.E.; Benbrahim-Tallaa, L.; Guha, N.; Freeman, C.; Galichet, L.; et al. A review of human carcinogens—Part B: Biological agents. Lancet Oncol. 2009, 10, 321–322. [Google Scholar] [CrossRef]
- Muñoz, N.; Hernandez-Suarez, G.; Méndez, F.; Molano, M.; Posso, H.; Moreno, V.; Murillo, R.; Ronderos, M.; Meijer, C.; Muñoz, A.; et al. Persistence of HPV infection and risk of high-grade cervical intraepithelial neoplasia in a cohort of Colombian women. Br. J. Cancer 2009, 100, 1184–1190. [Google Scholar] [CrossRef]
- Koshiol, J.; Lindsay, L.; Pimenta, J.M.; Poole, C.; Jenkins, D.; Smith, J.S. Persistent human papillomavirus infection and cervical neoplasia: A systematic review and meta-analysis. Am. J. Epidemiol. 2008, 168, 123–137. [Google Scholar] [CrossRef]
- Trottier, H.; Ferreira, S.; Thomann, P.; Costa, M.C.; Sobrinho, J.S.; Prado, J.C.; Rohan, T.E.; Villa, L.L.; Franco, E.L. Human papillomavirus infection and reinfection in adult women: The role of sexual activity and natural immunity. Cancer Res. 2010, 70, 8569–8577. [Google Scholar] [CrossRef]
- Cullen, M.; Boland, J.F.; Schiffman, M.; Zhang, X.; Wentzensen, N.; Yang, Q.; Chen, Z.; Yu, K.; Mitchell, J.; Roberson, D.; et al. Deep sequencing of HPV16 genomes: A new high-throughput tool for exploring the carcinogenicity and natural history of HPV16 infection. Papillomavirus Res. 2015, 1, 3–11. [Google Scholar] [CrossRef]
- Gaffikin, L.; Lauterbach, M.; Blumenthal, P.D. Performance of visual inspection with acetic acid for cervical cancer screening: A qualitative summary of evidence to date. Obstet. Gynecol. Surv. 2003, 58, 543–550. [Google Scholar] [CrossRef] [PubMed]
- Robles, C.; Hernandez, M.L.; Almonte, M. Alternative HPV vaccination schedules in Latin America. Salud Publica México 2018, 60, 693–702. [Google Scholar] [CrossRef] [PubMed]
- Torres-Poveda, K.J.; Cuadra-Hernández, S.M.; Castro-Romero, J.I.; Madrid-Marina, V. La política focalizada en el programa de vacunación contra el Vi- rus del Papiloma Humano en México: Aspectos éticos. Acta Bioethica 2011, 17, 85–94. [Google Scholar] [CrossRef]
- Flores, Y.N.; Salmeron, J.; Glenn, B.A.; Lang, C.M.; Chang, L.C.; Bastani, R. Clinician offering is a key factor associated with HPV vaccine uptake among Mexican mothers in the USA and Mexico: A cross-sectional study. Int. J. Public Health 2019, 64, 323–332. [Google Scholar] [CrossRef]
- de Ruiz, P.A.; Lazcano Ponce, E.C.; Duarte Torres, R.; Ruiz Juarez, I.; Martinez Cortez, I. Diagnostic reproducibility of Pap testing in two regions of Mexico: The need for quality control mechanisms. Bull. Pan Am. Health Organ. 1996, 30, 330–338. [Google Scholar]
| Clinical Variable | Median | p-Value |
|---|---|---|
| Age | ||
| HPV positive | 34.90 | 0.169 |
| HPV negative | 37.05 | |
| Number of sexual contacts | ||
| HPV positive | 2.95 | 0.586 |
| HPV negative | 2.90 | |
| Age of first sexual contact | ||
| HPV positive | 17.88 | 0.032 |
| HPV negative | 18.66 | |
| Treatment received* | cases | % |
| Cervical conization surgery | 31 | 17.4 |
| LEEP | 17 | 9.6 |
| Hysterectomy | 20 | 11.2 |
| Cryotherapy | 11 | 6.2 |
| Pap Smear Result | Total Cases per Group | Total Cases of Multiple HPV Infections | p-Value | |
|---|---|---|---|---|
| Number of Cases | % of Cases | |||
| Normal | 48 | 36 | 75.0 | 0.2431 |
| ASCUS | 10 | 0 | 0.0 | 0.0147 |
| LSIL | 57 | 31 | 54.3 | 0.7598 |
| HSIL | 47 | 30 | 63.8 | 0.7968 |
| CC | 3 | 1 | 33.3 | 1.0000 |
| Not available | 13 | - | - | |
| Overall | 178 | 105 | 59.0 | |
| Patients Groups HPV Type | # cases | Multiple Infection # Cases | % | p-Value Chi |
|---|---|---|---|---|
| Overall HPV types (top) | ||||
| 16 | 60 | 47 | 78.3 | 0.0001 |
| 18 | 45 | 38 | 84.4 | 0.0001 |
| 39 | 40 | 34 | 85.0 | 0.0001 |
| 52 | 39 | 32 | 82.1 | 0.001 |
| 51 | 33 | 26 | 78.8 | 0.011 |
| Normal | ||||
| 52 | 18 | 16 | 88.9 | 0.009 |
| 18 | 17 | 16 | 94.1 | 0.002 |
| 16 | 16 | 15 | 93.8 | 0.005 |
| 39 | 14 | 12 | 85.7 | 0.062 |
| 51 | 13 | 10 | 76.9 | 0.338 |
| LSIL | ||||
| 18 | 15 | 12 | 80.0 | 0.034 |
| 52 | 13 | 9 | 69.2 | 0.345 |
| 16 | 12 | 11 | 91.7 | 0.007 |
| 51 | 12 | 9 | 75.0 | 0.191 |
| 39 | 11 | 9 | 81.8 | 0.880 |
| 58 | 11 | 8 | 72.7 | 0.312 |
| HSIL | ||||
| 16 | 23 | 17 | 73.9 | 0.145 |
| 39 | 12 | 10 | 83.3 | 0.167 |
| 18 | 11 | 9 | 81.8 | 0.171 |
| 31 | 11 | 9 | 81.8 | 0.171 |
| 56 | 9 | 9 | 100.0 | 0.018 |
| Most Frequent HR-HPV Multiple Infections | |
|---|---|
| HPV types | Cases |
| 16, 18 | 15 |
| 18, 51 | 13 |
| 18, 52 | 12 |
| 39, 51 | 12 |
| 39, 52 | 12 |
| Others | 41 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Oyervides-Muñoz, M.A.; Pérez-Maya, A.A.; Sánchez-Domínguez, C.N.; Berlanga-Garza, A.; Antonio-Macedo, M.; Valdéz-Chapa, L.D.; Cerda-Flores, R.M.; Trevino, V.; Barrera-Saldaña, H.A.; Garza-Rodríguez, M.L. Multiple HPV Infections and Viral Load Association in Persistent Cervical Lesions in Mexican Women. Viruses 2020, 12, 380. https://doi.org/10.3390/v12040380
Oyervides-Muñoz MA, Pérez-Maya AA, Sánchez-Domínguez CN, Berlanga-Garza A, Antonio-Macedo M, Valdéz-Chapa LD, Cerda-Flores RM, Trevino V, Barrera-Saldaña HA, Garza-Rodríguez ML. Multiple HPV Infections and Viral Load Association in Persistent Cervical Lesions in Mexican Women. Viruses. 2020; 12(4):380. https://doi.org/10.3390/v12040380
Chicago/Turabian StyleOyervides-Muñoz, Mariel A., Antonio A. Pérez-Maya, Celia N. Sánchez-Domínguez, Anais Berlanga-Garza, Mauro Antonio-Macedo, Lezmes D. Valdéz-Chapa, Ricardo M. Cerda-Flores, Victor Trevino, Hugo A. Barrera-Saldaña, and María L. Garza-Rodríguez. 2020. "Multiple HPV Infections and Viral Load Association in Persistent Cervical Lesions in Mexican Women" Viruses 12, no. 4: 380. https://doi.org/10.3390/v12040380
APA StyleOyervides-Muñoz, M. A., Pérez-Maya, A. A., Sánchez-Domínguez, C. N., Berlanga-Garza, A., Antonio-Macedo, M., Valdéz-Chapa, L. D., Cerda-Flores, R. M., Trevino, V., Barrera-Saldaña, H. A., & Garza-Rodríguez, M. L. (2020). Multiple HPV Infections and Viral Load Association in Persistent Cervical Lesions in Mexican Women. Viruses, 12(4), 380. https://doi.org/10.3390/v12040380








