Exploring the Reservoir Hosts of Tick-Borne Encephalitis Virus
Abstract
1. Introduction
2. Tick-Borne Encephalitis: Etiological Agent and Clinical Manifestation
3. TBEV Transmission Cycle: The Tick Vector
4. TBEV Transmission Cycle: The Mammalian Reservoir Hosts
5. TBEV Prevalence in Wild Small Vertebrate Hosts
6. Distribution
7. Situation of other Tick-Borne Flaviviruses
8. Discussion
Author Contributions
Funding
Conflicts of Interest
References
- Weaver, S.C.; Reisen, W.K. Present and future arboviral threats. Antivir. Res. 2010, 85, 328–345. [Google Scholar] [CrossRef] [PubMed]
- Gubler, D.J. Human arbovirus infections worldwide. Ann. N. Y. Acad. Sci. 2001, 951, 13–24. [Google Scholar] [CrossRef] [PubMed]
- Pfeffer, M.; Dobler, G. Emergence of zoonotic arboviruses by animal trade and migration. Parasites Vectors 2010, 3, 35. [Google Scholar] [CrossRef] [PubMed]
- Haydon, D.T.; Cleaveland, S.; Taylor, L.H.; Laurenson, M.K. Identifying reservoirs of infection: A conceptual and practical challenge. Emerg. Infect. Dis. 2002, 8, 1468–1473. [Google Scholar] [CrossRef] [PubMed]
- Süss, J. Tick-borne encephalitis in Europe and beyond—The epidemiological situation as of 2007. Euro Surveill. 2008, 13, 717–727. [Google Scholar]
- Füzik, T.; Formanová, P.; Růžek, D.; Yoshii, K.; Niedrig, M.; Plevka, P. Structure of tick-borne encephalitis virus and its neutralization by a monoclonal antibody. Nat. Commun. 2018, 9, 436. [Google Scholar] [CrossRef] [PubMed]
- Ecker, M.; Allison, S.L.; Meixner, T.; Heinz, F.X. Sequence analysis and genetic classification of tick-borne encephalitis viruses from Europe and Asia. J. Gen. Virol. 1999, 80, 179–185. [Google Scholar] [CrossRef] [PubMed]
- Kovalev, S.Y.; Mukhacheva, T.A. Reconsidering the classification of tick-borne encephalitis virus within the Siberian subtype gives new insights into its evolutionary history. Infect. Genet. Evol. 2017, 55, 159–165. [Google Scholar] [CrossRef]
- Dai, X.; Shang, G.; Lu, S.; Yang, J.; Xu, J. A new subtype of eastern tick-borne encephalitis virus discovered in Qinghai-Tibet Plateau, China. Emerg. Microbes Infect. 2018, 7, 1–9. [Google Scholar] [CrossRef]
- Korenberg, E.I. Natural focality of infections: Current problems and prospects of research. Biol. Bull. 2010, 37, 665–676. [Google Scholar] [CrossRef]
- Calisher, C.H.; Karabatsos, N.; Dalrymple, J.M.; Shope, R.E.; Porterfield, J.S.; Westaway, E.G.; Brandt, W.E. Antigenic relationships between flaviviruses as determined by cross-neutralization tests with polyclonal antisera. J. Gen. Virol. 1989, 70, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Taba, P.; Schmutzhard, E.; Forsberg, P.; Lutsar, I.; Ljøstad, U.; Mygland, A.; Levchenko, I.; Strle, F.; Steiner, I. EAN consensus review on prevention, diagnosis and management of tick-borne encephalitis. Eur. J. Neurol. 2017, 24, 1214–1227. [Google Scholar] [CrossRef] [PubMed]
- Hansson, E.K.; Rosdahl, A.; Insulander, M.; Vene, S.; Lindquist, L.; Gredmark-Russ, S.; Askling, H.H. Tick-borne encephalitis (TBE) vaccine failures: A ten-year retrospective study supporting the rationale for adding an extra priming dose in individuals from the age of 50 years. Clin. Infect. Dis. 2019. [Google Scholar] [CrossRef] [PubMed]
- Yoshii, K.; Song, J.Y.; Park, S.B.; Yang, J.; Schmitt, H.J. Tick-borne encephalitis in Japan, Republic of Korea and China. Emerg. Microbes Infect. 2017, 6, 1–10. [Google Scholar] [CrossRef]
- Lu, Z.; Bröker, M.; Liang, G. Tick-borne encephalitis in mainland China. Vector-Borne Zoonotic Dis. 2008, 8, 713–720. [Google Scholar] [CrossRef] [PubMed]
- Pfeffer, M.; Dobler, G. Tick-borne encephalitis virus in dogs—Is this an issue? Parasites Vectors 2011, 4, 59. [Google Scholar] [CrossRef] [PubMed]
- Klaus, C.; Hörügel, U.; Hoffmann, B.; Beer, M. Tick-borne encephalitis virus (TBEV) infection in horses: Clinical and laboratory findings and epidemiological investigations. Vet. Microbiol. 2013, 163, 368–372. [Google Scholar] [CrossRef] [PubMed]
- Süss, J.; Dobler, G.; Zöller, G.; Essbauer, S.; Pfeffer, M.; Klaus, C.; Liebler-Tenorio, E.M.; Gelpi, E.; Stark, B.; Hotzel, H. Genetic characterisation of a tick-borne encephalitis virus isolated from the brain of a naturally exposed monkey (Macaca sylvanus). Int. J. Med. Microbiol. 2008, 298, 295–300. [Google Scholar] [CrossRef]
- Böhm, B.; Schade, B.; Bauer, B.; Hoffmann, B.; Hoffmann, D.; Ziegler, U.; Beer, M.; Klaus, C.; Weissenböck, H.; Böttcher, J. Tick-borne encephalitis in a naturally infected sheep. BMC Vet. Res. 2017, 13, 267. [Google Scholar] [CrossRef] [PubMed]
- Zindel, W.; Wyler, R. Tick-borne encephalitis in a goat in lower Prätigau. Schweiz. Arch. Tierheilkd. 1983, 125, 383–386. [Google Scholar]
- Bagó, Z.; Bauder, B.; Kolodziejek, J.; Nowotny, N.; Weissenböck, H. Tickborne encephalitis in a mouflon (Ovis ammon musimon). Vet. Rec. 2002, 150, 218–220. [Google Scholar] [CrossRef] [PubMed]
- Balling, A.; Plessow, U.; Beer, M.; Pfeffer, M. Prevalence of antibodies against tick-borne encephalitis virus in wild game from Saxony, Germany. Ticks Tick-Borne Dis. 2014, 5, 805–809. [Google Scholar] [CrossRef] [PubMed]
- Leutloff, R.; Nübling, M.; Neumann-Haefelin, D.; Rieger, M.A. Cows as indicators for TBE endemic regions: Suitability of testing for antibodies in serum and milk. Int. J. Med. Microbiol. 2006, 296, 87–88. [Google Scholar]
- Hoogstraal, H. Ticks in relation to human diseases caused by viruses. Annu. Rev. Entomol. 1966, 11, 261–308. [Google Scholar] [CrossRef] [PubMed]
- Rubel, F.; Brugger, K.; Walter, M.; Vogelgesang, J.R.; Didyk, Y.M.; Fu, S.; Kahl, O. Geographical distribution, climate adaptation and vector competence of the Eurasian hard tick Haemaphysalis concinna. Ticks Tick-Borne Dis. 2018. [Google Scholar] [CrossRef] [PubMed]
- Hayasaka, D.; Ivanov, L.; Leonova, G.; Goto, A.; Yoshii, K.; Mizutani, T.; Kariwa, H.; Takashima, I. Distribution and characterization of tick-borne encephalitis viruses from Siberia and far-eastern Asia. J. Gen. Virol. 2001, 82, 1319–1328. [Google Scholar] [CrossRef]
- Süss, J. Epidemiology and ecology of TBE relevant to the production of effective vaccines. Vaccine 2003, 21, S19–S35. [Google Scholar] [CrossRef]
- Chitimia-Dobler, L.; Mackenstedt, U.; Kahl, O.; Petney, T.N. Transmission and natural cycles of TBE virus. The TBE Book 2019, 2, 62–86. [Google Scholar]
- Belova, O.A.; Litov, A.G.; Kholodilov, I.S.; Kozlovskaya, L.I.; Bell-Sakyi, L.; Romanova, L.I.; Karganova, G.G. Properties of the tick-borne encephalitis virus population during persistent infection of ixodid ticks and tick cell lines. Ticks Tick-Borne Dis. 2017, 8, 895–906. [Google Scholar] [CrossRef]
- Mierzejewska, E.J.; Pawelczyk, A.; Radkowski, M.; Welc-Faleciak, R.; Bajer, A. Pathogens vectored by the tick, Dermacentor reticulatus, in endemic regions and zones of expansion in Poland. Parasites Vectors 2015, 8, 490. [Google Scholar] [CrossRef]
- Mehlhorn, H.; Mehlhorn, T.; Muller, M.; Vogt, M.; Rissland, J. Tick survey for prevalent pathogens in peri-urban recreation sites in Saarland and Rhineland-Palatinate (Germany). Parasitol. Res. 2016, 115, 1167–1172. [Google Scholar] [CrossRef] [PubMed]
- Földvári, G.; Široký, P.; Szekeres, S.; Majoros, G.; Sprong, H. Dermacentor reticulatus: A vector on the rise. Parasites Vectors 2016, 9, 314. [Google Scholar] [CrossRef] [PubMed]
- Biernat, B.; Karbowiak, G.; Werszko, J.; Stanczak, J. Prevalence of tick-borne encephalitis virus (TBEV) RNA in Dermacentor reticulatus ticks from natural and urban environment, Poland. Exp. Appl. Acarol. 2014, 64, 543–551. [Google Scholar] [CrossRef] [PubMed]
- Korenberg, E.; Kovalevskii, Y.V. A Model for Relationships among the Tick-Borne Encephalitis Virus, Its Main Vectors, and Hosts. Zool Zhurnal 1994, 10, 65–92. [Google Scholar] [CrossRef]
- Karbowiak, G.; Biernat, B. The role of particular tick developmental stages in the circulation of tick-borne pathogens affecting humans in Central Europe. 2. Tick-borne encephalitis virus. Ann. Parasitol. 2016, 62, 3–9. [Google Scholar] [CrossRef] [PubMed]
- Danielová, V.; Holubová, J.; Pejčoch, M.; Daniel, M. Potential significance of transovarial transmission in the circulation of tick-borne encephalitis virus. Folia Parasitol. 2002, 49, 323–325. [Google Scholar] [CrossRef] [PubMed]
- Slovák, M.; Kazimírová, M.; Siebenstichová, M.; Ustaníková, K.; Klempa, B.; Gritsun, T.; Gould, E.A.; Nuttall, P.A. Survival dynamics of tick-borne encephalitis virus in Ixodes ricinus ticks. Ticks Tick-Borne Dis. 2014, 5, 962–969. [Google Scholar] [CrossRef] [PubMed]
- Labuda, M.; Nuttall, P.A. Tick-borne viruses. Parasitology 2005, 129, 221–245. [Google Scholar] [CrossRef]
- Burtis, J.C.; Fahey, T.J.; Yavitt, J.B. Survival and energy use of Ixodes scapularis nymphs throughout their overwintering period. Parasitology 2019, 146, 781–790. [Google Scholar] [CrossRef]
- Belova, O.A.; Burenkova, L.A.; Karganova, G.G. Different tick-borne encephalitis virus (TBEV) prevalences in unfed versus partially engorged ixodid ticks—Evidence of virus replication and changes in tick behavior. Ticks Tick-Borne Dis. 2012, 3, 240–246. [Google Scholar] [CrossRef]
- Labuda, M.; Kozuch, O.; Zuffová, E.; Elecková, E.; Hails, R.S.; Nuttall, P.A. Tick-borne encephalitis virus transmission between ticks cofeeding on specific immune natural rodent hosts. Virology 1997, 235, 138–143. [Google Scholar] [CrossRef] [PubMed]
- Randolph, S.E. Transmission of tick-borne pathogens between co-feeding ticks: Milan Labuda’s enduring paradigm. Ticks Tick-Borne Dis. 2011, 2, 179–182. [Google Scholar] [CrossRef] [PubMed]
- Labuda, M.; Randolph, S.E. Survival strategy of tick-borne encephalitis virus: Cellular basis and environmental determinants. Zentralblatt Bakteriol. 1999, 289, 513–524. [Google Scholar] [CrossRef]
- Havlíková, S.; Ličková, M.; Klempa, B. Non-viraemic transmission of tick-borne viruses. Acta Virol. 2013, 57, 123–129. [Google Scholar] [CrossRef]
- Foppa, I.M. The basic reproductive number of tick-borne encephalitis virus. An empirical approach. J. Math. Biol. 2005, 51, 616–628. [Google Scholar] [CrossRef]
- Bogovic, P.; Strle, F. Tick-borne encephalitis: A review of epidemiology, clinical characteristics, and management. World J. Clin. Cases 2015, 3, 430–441. [Google Scholar] [CrossRef]
- Brockmann, S.O.; Oehme, R.; Buckenmaier, T.; Beer, M.; Jeffery-Smith, A.; Spannenkrebs, M.; Haag-Milz, S.; Wagner-Wiening, C.; Schlegel, C.; Fritz, J.; et al. A cluster of two human cases of tick-borne encephalitis (TBE) transmitted by unpasteurised goat milk and cheese in Germany, May 2016. Euro Surveill. 2018, 23. [Google Scholar] [CrossRef]
- Saksida, A.; Duh, D.; Lotrič-Furlan, S.; Strle, F.; Petrovec, M.; Avšič-Županc, T. The importance of tick-borne encephalitis virus RNA detection for early differential diagnosis of tick-borne encephalitis. J. Clin. Virol. 2005, 33, 331–335. [Google Scholar] [CrossRef]
- Dobler, G. Zoonotic tick-borne flaviviruses. Vet. Microbiol. 2010, 140, 221–228. [Google Scholar] [CrossRef]
- Černý, V. The role of mammals in natural foci of tick-borne encephalitis in Central Europe. Folia Parasitol. 1975, 22, 271–273. [Google Scholar]
- Klaus, C.; Gethmann, J.; Hoffmann, B.; Ziegler, U.; Heller, M.; Beer, M. Tick infestation in birds and prevalence of pathogens in ticks collected from different places in Germany. Parasitol. Res. 2016, 115, 2729–2740. [Google Scholar] [CrossRef] [PubMed]
- Hofmeester, T.R.; Sprong, H.; Jansen, P.A.; Prins, H.H.T.; van Wieren, S.E. Deer presence rather than abundance determines the population density of the sheep tick, Ixodes ricinus, in Dutch forests. Parasites Vectors 2017, 10, 433. [Google Scholar] [CrossRef] [PubMed]
- Jaenson, T.G.T.; Petersson, E.H.; Jaenson, D.G.E.; Kindberg, J.; Pettersson, J.H.; Hjertqvist, M.; Medlock, J.M.; Bengtsson, H. The importance of wildlife in the ecology and epidemiology of the TBE virus in Sweden: Incidence of human TBE correlates with abundance of deer and hares. Parasites Vectors 2018, 11, 477. [Google Scholar] [CrossRef] [PubMed]
- Hubálek, Z.; Rudolf, I. Tick-borne viruses in Europe. Parasitol. Res. 2012, 111, 9–36. [Google Scholar] [CrossRef] [PubMed]
- Richardson, J.H.; Shore, R.F.; Treweek, J.R.; Larkin, S.B.C. Are major roads a barrier to small mammals? J. Zool. 1997, 243, 840–846. [Google Scholar] [CrossRef]
- Hasle, G. Transport of ixodid ticks and tick-borne pathogens by migratory birds. Front. Cell. Infect. Microbiol. 2013, 3, 48. [Google Scholar] [CrossRef]
- Waldenström, J.; Lundkvist, Å.; Falk, K.I.; Garpmo, U.; Bergström, S.; Lindegren, G.; Sjöstedt, A.; Mejlon, H.; Fransson, T.; Haemig, P.D. Migrating birds and tickborne encephalitis virus. Emerg. Infect. Dis. 2007, 13, 1215–1218. [Google Scholar] [CrossRef]
- Spielman, A.; Pollack, R.J.; Kiszewski, A.E.; Telford, S.R., III. Issues in Public Health Entomology. Vector Borne Zoonotic Dis. 2001, 1, 3–19. [Google Scholar] [CrossRef]
- Ernek, E.; Kožuch, O.; Lichard, M.; Nosek, J.; Albrecht, P. Experimental infection of Clethrionomys glareolus and Apodemus flavicollis with tick-borne encephalitis virus. Acta Virol. 1963, 7, 434–436. [Google Scholar]
- Gliwicz, J.; Taylor, J.R.E. Comparing life histories of shrews and rodents. Acta Theriol. 2002, 47, 185–208. [Google Scholar] [CrossRef]
- Cull, B.; Vaux, A.G.C.; Ottowell, L.J.; Gillingham, E.L.; Medlock, J.M. Tick infestation of small mammals in an English woodland. J. Vector Ecol. 2017, 42, 74–83. [Google Scholar] [CrossRef] [PubMed]
- Labuda, M.; Nuttall, P.A.; Kožuch, O.; Elečková, E.; Williams, T.; Žuffová, E.; Sabó, A. Non-viraemic transmission of tick-borne encephalitis virus: A mechanism for arbovirus survival in nature. Experientia 1993, 49, 802–805. [Google Scholar] [CrossRef] [PubMed]
- Kožuch, O.; Grešíková, M.; Nosek, J.; Lichard, M.; Sekeyová, M. The role of small rodents and hedgehogs in a natural focus of tick-borne encephalitis. Bull. World Health Organ. 1967, 36, 61–66. [Google Scholar] [PubMed]
- Schönbächler, K.; Hatt, J.; Silaghi, C.; Merz, N.; Fraefel, C.; Bachofen, C. Confirmation of tick-borne encephalitis virus in an European hedgehog (Erinaceus europaeus). Schweiz. Arch. Tierheilkd. 2019, 161, 23–31. [Google Scholar] [CrossRef] [PubMed]
- Bakhvalova, V.N.; Potapova, O.F.; Panov, V.V.; Morozova, O.V. Vertical transmission of tick-borne encephalitis virus between generations of adapted reservoir small rodents. Virus Res. 2009, 140, 172–178. [Google Scholar] [CrossRef] [PubMed]
- Tonteri, E.; Kipar, A.; Voutilainen, L.; Vene, S.; Vaheri, A.; Vapalahti, O.; Lundkvist, A. The three subtypes of tick-borne encephalitis virus induce encephalitis in a natural host, the bank vole (Myodes glareolus). PLoS ONE 2013, 8, e81214. [Google Scholar] [CrossRef] [PubMed]
- Heigl, Z.; Zeipel, G.V. Experimental infection with tick-borne encephalitis virus in Clethrionomys glareolus, Apodemus flavicollis, Apodemus sylvaticus and Mus musculus. Acta Pathol. Microbiol. Scand. 1966, 66, 489–509. [Google Scholar] [CrossRef] [PubMed]
- Kopecký, J.; Tomková, E.; Vlček, M. Immune response of the long-tailed field mouse (Apodemus sylvaticus) to tick-borne encephalitis virus infection. Folia Parasitol. 1991, 38, 275–282. [Google Scholar] [PubMed]
- Achazi, K.; Růžek, D.; Donoso-Mantke, O.; Schlegel, M.; Ali, H.; Wenk, M.; Schmidt-Chanasit, J.; Ohlmeyer, L.; Rühe, F.; Vor, T.; et al. Rodents as sentinels for the prevalence of tick-borne encephalitis virus. Vector Borne Zoonotic Dis. 2011, 11, 641–647. [Google Scholar] [CrossRef] [PubMed]
- Burri, C.; Korva, M.; Bastic, V.; Knap, N.; Avšič-Županc, T.; Gern, L. Serological Evidence of tick-borne encephalitis virus infection in rodents captured at four sites in Switzerland. J. Med. Entomol. 2012, 49, 436–439. [Google Scholar] [CrossRef] [PubMed]
- Knap, N.; Korva, M.; Dolinšek, V.; Sekirnik, M.; Trilar, T.; Avšič-Županc, T. Patterns of tick-borne encephalitis virus infection in rodents in Slovenia. Vector Borne Zoonotic Dis. 2012, 12, 236–242. [Google Scholar] [CrossRef] [PubMed]
- Weidmann, M.; Schmidt, P.; Hufert, F.T.; Krivanec, K.; Meyer, H. Tick-borne encephalitis virus in Clethrionomys glareolus in the Czech Republic. Vector Borne Zoonotic Dis. 2006, 6, 379–381. [Google Scholar] [CrossRef] [PubMed]
- Zeman, P.; Januška, J. Epizootiologic background of dissimilar distribution of human cases of Lyme borreliosis and tick-borne encephalitis in a joint endemic area. Comp. Immunol. Microbiol. Infect. Dis. 1999, 22, 247–260. [Google Scholar] [CrossRef]
- Pintér, R.; Madai, M.; Horváth, G.; Németh, V.; Oldal, M.; Kemenesi, G.; Dallos, B.; Bányai, K.; Jakab, F. Molecular detection and phylogenetic analysis of tick-borne encephalitis virus in rodents captured in the transdanubian region of Hungary. Vector Borne Zoonotic Dis. 2014, 14, 621–624. [Google Scholar] [CrossRef] [PubMed]
- Zöldi, V.; Papp, T.; Reiczigel, J.; Egyed, L. Bank voles show high seropositivity rates in a natural TBEV focus in Hungary. Infect. Dis. 2015, 47, 178–181. [Google Scholar] [CrossRef] [PubMed]
- Kožuch, O.; Labuda, M.; Lysý, J.; Weismann, P.; Krippel, E. Longitudinal study of natural foci of Central European encephalitis virus in West Slovakia. Acta Virol. 1990, 34, 537–544. [Google Scholar]
- Kocianová, E.; Kožuch, O.; Bakoss, P.; Řeháček, J.; Kováčová, E. The prevalence of small terrestrial mammals infected with tick-borne encephalitis virus and leptospirae in the foothills of the southern Bavarian forest, Germany. Appl. Parasitol. 1993, 34, 283–290. [Google Scholar]
- Tonteri, E.; Jääskeläinen, A.E.; Tikkakoski, T.; Voutilainen, L.; Niemimaa, J.; Henttonen, H.; Vaheri, A.; Vapalahti, O. Tick-borne encephalitis virus in wild rodents in winter, Finland, 2008–2009. Emerg. Infect. Dis. 2011, 17, 72–75. [Google Scholar] [CrossRef]
- Bakhvalova, V.N.; Chicherina, G.S.; Potapova, O.F.; Panov, V.V.; Glupov, V.V.; Potapov, M.A.; Seligman, S.J.; Morozova, O.V. Tick-borne encephalitis virus diversity in Ixodid ticks and small mammals in south-western Siberia, Russia. Vector Borne Zoonotic Dis. 2016, 16, 541–549. [Google Scholar] [CrossRef]
- Bakhvalova, V.N.; Dobrotvorsky, A.K.; Panov, V.V.; Matveeva, V.A.; Tkachev, S.E.; Morozova, O.V. Natural tick-borne encephalitis virus infection among wild small mammals in the southeastern part of western Siberia, Russia. Vector Borne Zoonotic Dis. 2006, 6, 32–41. [Google Scholar] [CrossRef]
- Takeda, T.; Ito, T.; Osada, M.; Takahashi, K.; Takashima, I. Isolation of tick-borne encephalitis virus from wild rodents and a seroepizootiologic survey in Hokkaido, Japan. Am. J. Trop. Med. Hyg. 1999, 60, 287–291. [Google Scholar] [CrossRef] [PubMed]
- Yoshii, K.; Mottate, K.; Omori-Urabe, Y.; Chiba, Y.; Seto, T.; Sanada, T.; Maeda, J.; Obara, M.; Ando, S.; Ito, N.; et al. Epizootiological Study of Tick-Borne Encephalitis Virus Infection in Japan. J. Vet. Med. Sci. 2011, 73, 409–412. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.Y.; Yun, S.M.; Han, M.G.; Lee, I.Y.; Lee, N.Y.; Jeong, Y.E.; Lee, B.C.; Ju, Y.R. Isolation of tick-borne encephalitis viruses from wild rodents, South Korea. Vector Borne Zoonotic Dis. 2008, 8, 7–13. [Google Scholar] [CrossRef] [PubMed]
- Demina, T.V.; Tkachev, S.E.; Kozlova, I.V.; Doroshchenko, E.K.; Lisak, O.V.; Suntsova, O.V.; Verkhozina, M.M.; Dzhioev, Y.P.; Paramonov, A.I.; Tikunov, A.Y. Comparative analysis of complete genome sequences of European subtype tick-borne encephalitis virus strains isolated from Ixodes persulcatus ticks, long-tailed ground squirrel (Spermophilus undulatus), and human blood in the Asian part of Russia. Ticks Tick-Borne Dis. 2017, 8, 547–553. [Google Scholar] [CrossRef] [PubMed]
- Kovalev, S.Y.; Chernykh, D.N.; Kokorev, V.S.; Snitkovskaya, T.E.; Romanenko, V.V. Origin and distribution of tick-borne encephalitis virus strains of the Siberian subtype in the Middle Urals, the north-west of Russia and the Baltic countries. J. Gen. Virol. 2009, 90, 2884–2892. [Google Scholar] [CrossRef] [PubMed]
- Jääskeläinen, A.E.; Sironen, T.; Murueva, G.B.; Subbotina, N.; Alekseev, A.N.; Castrén, J.; Alitalo, I.; Vaheri, A.; Vapalahti, O. Tick-borne encephalitis virus in ticks in Finland, Russian Karelia and Buryatia. J. Gen. Virol. 2010, 91, 2706–2712. [Google Scholar] [CrossRef] [PubMed]
- Jääskeläinen, A.E.; Tonteri, E.; Sironen, T.; Pakarinen, L.; Vaheri, A.; Vapalahti, O. European subtype tick-borne encephalitis virus in Ixodes persulcatus ticks. Emerg. Infect. Dis. 2011, 17, 323–325. [Google Scholar] [CrossRef] [PubMed]
- Kovalev, S.Y.; Mukhacheva, T.A. Tick-borne encephalitis virus subtypes emerged through rapid vector switches rather than gradual evolution. Ecol. Evol. 2014, 4, 4307–4316. [Google Scholar] [CrossRef] [PubMed]
- Michaux, J.R.; Libois, R.; Filippucci, M.G. So close and so different: Comparative phylogeography of two small mammal species, the Yellow-necked fieldmouse (Apodemus flavicollis) and the Woodmouse (Apodemus sylvaticus) in the Western Palearctic region. Heredity 2005, 94, 52–63. [Google Scholar] [CrossRef] [PubMed]
- Tschirren, B.; Andersson, M.; Scherman, K.; Westerdahl, H.; Råberg, L. Contrasting patterns of diversity and population differentiation at the innate immunity gene toll-like receptor 2 (TLR2) in two sympatric rodent species. Evolution 2012, 66, 720–731. [Google Scholar] [CrossRef]
- Cowled, C.; Wang, L.F. Animal genomics in natural reservoirs of infectious diseases. Rev. Sci. Tech. 2016, 35, 159–174. [Google Scholar] [CrossRef] [PubMed]
- Dubois, A.; Castel, G.; Murri, S.; Pulido, C.; Pons, J.B.; Benoit, L.; Loiseau, A.; Lakhdar, L.; Galan, M.; Charbonnel, N.; et al. Experimental infections of wild bank voles (Myodes glareolus) from nephropathia epidemica endemic and non-endemic regions revealed slight differences in Puumala virological course and immunological responses. Virus Res. 2017, 235, 67–72. [Google Scholar] [CrossRef] [PubMed]
- Wójcik, J.M.; Kawałko, A.; Marková, S.; Searle, J.B.; Kotlík, P. Phylogeographic signatures of northward post-glacial colonization from high-latitude refugia: A case study of bank voles using museum specimens. J. Zool. 2010, 281, 249–262. [Google Scholar] [CrossRef]
- Donoso Mantke, O.; Escadafal, C.; Niedrig, M.; Pfeffer, M. Tick-borne encephalitis in Europe, 2007 to 2009. Euro Surveill. 2011, 16. [Google Scholar] [CrossRef] [PubMed]
- Chrdle, A.; Chmelík, V.; Růžek, D. Tick-borne encephalitis: What travelers should know when visiting an endemic country. Hum. Vaccines Immunother. 2016, 12, 2694–2699. [Google Scholar] [CrossRef] [PubMed]
- Süss, J.; Klaus, C.; Gerstengarbe, F.W.; Werner, P.C. What makes ticks tick? Climate change, ticks, and tick-borne diseases. J. Travel Med. 2008, 15, 39–45. [Google Scholar] [CrossRef] [PubMed]
- Donoso-Mantke, O.; Karan, L.S.; Ruzek, D. Tick-borne encephalitis virus: A general overview. In Flavivirus Encephalitis, 1st ed.; Ruzek, D., Ed.; InTech: Rijeka, Croatia, 2011; Volume 1, pp. 133–156. [Google Scholar]
- Aspöck, H. The synecological system of arboviruses and its possible modification by man. Zentralblatt Bakteriol. Orig. 1970, 213, 434–454. [Google Scholar]
- Jaenson, T.G.; Hjertqvist, M.; Bergström, T.; Lundkvist, Å. Why is tick-borne encephalitis increasing? A review of the key factors causing the increasing incidence of human TBE in Sweden. Parasites Vectors 2012, 5, 184. [Google Scholar] [CrossRef]
- Randolph, S.E.; Asokliene, L.; Avsic-Zupanc, T.; Bormane, A.; Burri, C.; Gern, L.; Golovljova, I.; Hubalek, Z.; Knap, N.; Kondrusik, M.; et al. Variable spikes in tick-borne encephalitis incidence in 2006 independent of variable tick abundance but related to weather. Parasites Vectors 2008, 1, 44. [Google Scholar] [CrossRef]
- Daniel, M.; Danielová, V.; Fialová, A.; Malý, M.; Kříž, B.; Nuttall, P.A. Increased relative risk of tick-borne encephalitis in warmer weather. Front. Cell. Infect. Microbiol. 2018, 8, 90. [Google Scholar] [CrossRef]
- Randolph, S.E.; Green, R.M.; Peacey, M.F.; Rogers, D.J. Seasonal synchrony: The key to tick-borne encephalitis foci identified by satellite data. Parasitology 2000, 121, 15–23. [Google Scholar] [CrossRef] [PubMed]
- Lindquist, L.; Vapalahti, O. Tick-borne encephalitis. Lancet 2008, 371, 1861–1871. [Google Scholar] [CrossRef]
- Zeman, P. Objective assessment of risk maps of tick-borne encephalitis and Lyme borreliosis based on spatial patterns of located cases. Int. J. Epidemiol. 1997, 26, 1121–1129. [Google Scholar] [CrossRef] [PubMed]
- Korenberg, E.I.; Kovalevskii, Y.V. Main features of tick-borne encephalitis eco-epidemiology in Russia. Zentralblatt Bakteriol. 1999, 289, 525–539. [Google Scholar] [CrossRef]
- Dobler, G.; Hufert, F.T.; Pfeffer, M.; Essbauer, S. Tick-borne encephalitis: From microfocus to human disease. In Progress in Parasitology, 1st ed.; Mehlhorn, H., Ed.; Springer: Berlin/Heidelberg, Germany, 2011; Volume 2, pp. 323–331. [Google Scholar]
- Klaus, C.; Hoffmann, B.; Hering, U.; Mielke, B.; Sachse, K.; Beer, M.; Süss, J. Tick-borne encephalitis (TBE) virus prevalence and virus genome characterization in field-collected ticks (Ixodes ricinus) from risk, non-risk and former risk areas of TBE, and in ticks removed from humans in Germany. Clin. Microbiol. Infect. 2010, 16, 238–244. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Corrin, T.; Greig, J.; Harding, S.; Young, I.; Mascarenhas, M.; Waddell, L.A. Powassan virus, a scoping review of the global evidence. Zoonoses Public Health 2018. [Google Scholar] [CrossRef] [PubMed]
- Fatmi, S.S.; Zehra, R.; Carpenter, D.O. Powassan virus—A new reemerging tick-borne disease. Front. Public Health 2017, 5, 342. [Google Scholar] [CrossRef]
- Deardorff, E.R.; Nofchissey, R.A.; Cook, J.A.; Hope, A.G.; Tsvetkova, A.; Talbot, S.L.; Ebel, G.D. Powassan virus in mammals, Alaska and New Mexico, USA, and Russia, 2004–2007. Emerg. Infect. Dis. 2013, 19, 2012–2016. [Google Scholar] [CrossRef]
- Dupuis, A.P., 2nd; Peters, R.J.; Prusinski, M.A.; Falco, R.C.; Ostfeld, R.S.; Kramer, L.D. Isolation of deer tick virus (Powassan virus, lineage II) from Ixodes scapularis and detection of antibody in vertebrate hosts sampled in the Hudson Valley, New York State. Parasites Vectors 2013, 6, 185. [Google Scholar] [CrossRef]
- Zanotto, P.M.; Gao, G.F.; Gritsun, T.; Marin, M.S.; Jiang, W.R.; Venugopal, K.; Reid, H.W.; Gould, E.A. An arbovirus cline across the northern hemisphere. Virology 1995, 210, 152–159. [Google Scholar] [CrossRef]
- Gilbert, L.; Jones, L.D.; Hudson, P.J.; Gould, E.A.; Reid, H.W. Role of small mammals in the persistence of louping-ill virus: Field survey and tick co-feeding studies. Med. Vet. Entomol. 2000, 14, 277–282. [Google Scholar] [CrossRef]
- Gilbert, L. Louping ill virus in the UK: A review of the hosts, transmission and ecological consequences of control. Exp. Appl. Acarol. 2016, 68, 363–374. [Google Scholar] [CrossRef] [PubMed]
- Korenberg, E. Small mammals and problem of natural focality of tick-borne encephalitis. Zool. Zhurnal 1979, 58, 542–552. [Google Scholar]
- Radda, A.; Hofmann, H.; Pretzmann, G. Threshold of viraemia in Apodemus flavicollis for infection of Ixodes ricinus with tick-borne encephalitis virus. Acta Virol. 1969, 13, 74–77. [Google Scholar] [PubMed]
- Nuttall, P.; Labuda, M. Saliva-assisted transmission of tick-borne pathogens. In Ticks: Biology, Disease and Control, 1st ed.; Bowman, A., Nuttall, P., Eds.; Cambridge University Press: New York, NY, USA, 2008; Volume 1, pp. 205–253. [Google Scholar]
- Voutilainen, L.; Sironen, T.; Tonteri, E.; Tuiskunen Bäck, A.; Razzauti, M.; Karlsson, M.; Wahlström, M.; Niemimaa, J.; Henttonen, H.; Lundkvist, Å. Life-long shedding of puumala hantavirus in wild bank voles (Myodes glareolus). J. Gen. Virol. 2015, 96, 1238–1247. [Google Scholar] [CrossRef] [PubMed]
- Kožuch, O.; Nosek, J.; Ernek, E.; Lichard, M.; Albrecht, P. Persistence of tick-borne encephalitis virus in hibernating hedgehogs and dormice. Acta Virol. 1963, 7, 430–433. [Google Scholar] [PubMed]
 ), but can be found in a variety of animals (
), but can be found in a variety of animals ( ). Additionally, humans can become infected by consuming unpasteurized dairy products originating from viremic animals (6). Infected birds are suspected to be a vector for virus passage to new endemic foci, although a spatial restriction seems likely (5). TBEV is distributed within the tick population mainly through trans-stadial (1) transmission, and occasionally through trans-ovarial (2) transmission. For successful virus circulation, the virus needs to be spread within the tick population. This is achieved through naïve ticks consuming their blood meal on viremic host animals, as well as through co-feeding (4).
). Additionally, humans can become infected by consuming unpasteurized dairy products originating from viremic animals (6). Infected birds are suspected to be a vector for virus passage to new endemic foci, although a spatial restriction seems likely (5). TBEV is distributed within the tick population mainly through trans-stadial (1) transmission, and occasionally through trans-ovarial (2) transmission. For successful virus circulation, the virus needs to be spread within the tick population. This is achieved through naïve ticks consuming their blood meal on viremic host animals, as well as through co-feeding (4).
 ), but can be found in a variety of animals (
), but can be found in a variety of animals ( ). Additionally, humans can become infected by consuming unpasteurized dairy products originating from viremic animals (6). Infected birds are suspected to be a vector for virus passage to new endemic foci, although a spatial restriction seems likely (5). TBEV is distributed within the tick population mainly through trans-stadial (1) transmission, and occasionally through trans-ovarial (2) transmission. For successful virus circulation, the virus needs to be spread within the tick population. This is achieved through naïve ticks consuming their blood meal on viremic host animals, as well as through co-feeding (4).
). Additionally, humans can become infected by consuming unpasteurized dairy products originating from viremic animals (6). Infected birds are suspected to be a vector for virus passage to new endemic foci, although a spatial restriction seems likely (5). TBEV is distributed within the tick population mainly through trans-stadial (1) transmission, and occasionally through trans-ovarial (2) transmission. For successful virus circulation, the virus needs to be spread within the tick population. This is achieved through naïve ticks consuming their blood meal on viremic host animals, as well as through co-feeding (4).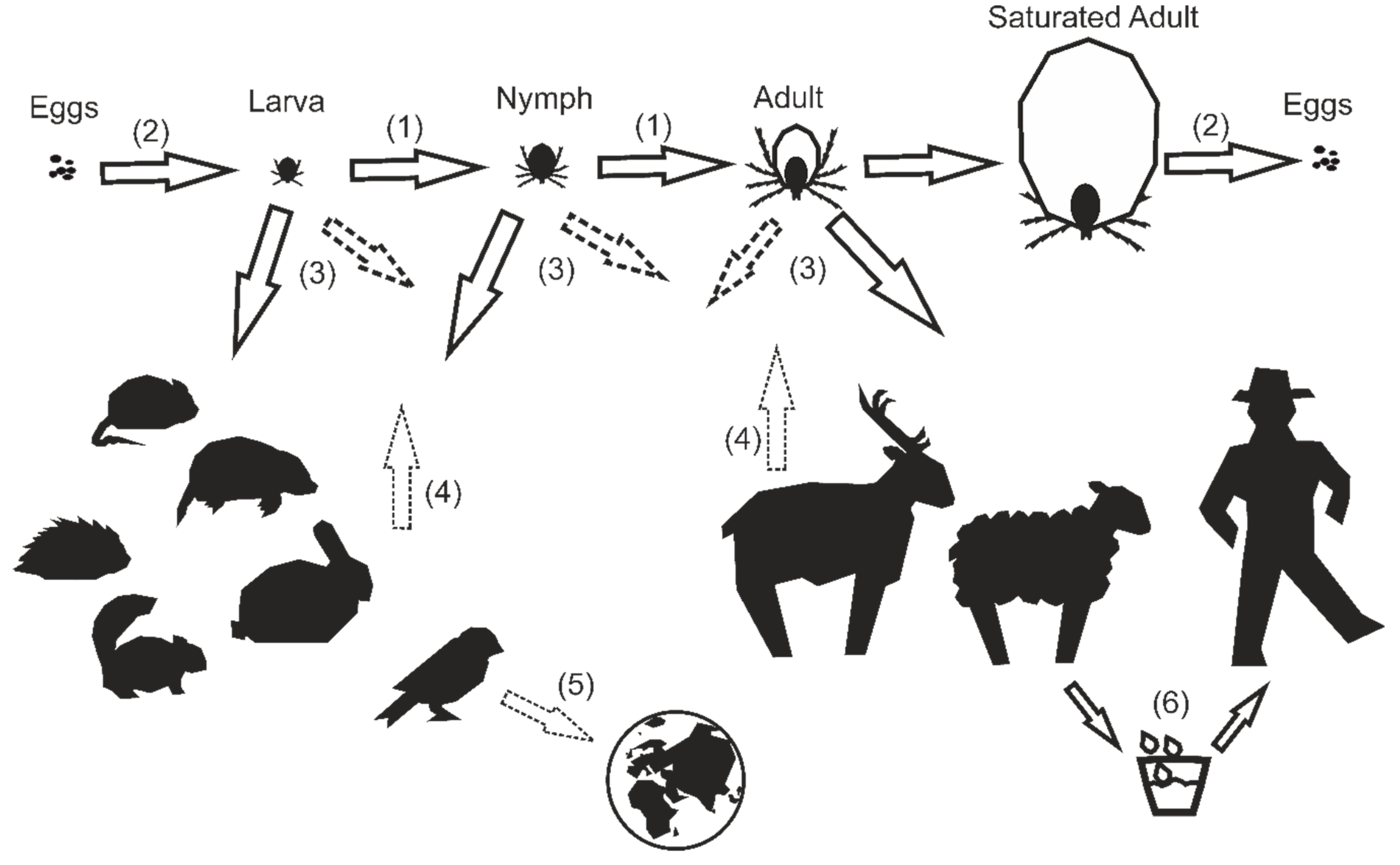
 ) to the animal host (1), leading to viremia (2). Naïve ticks acquire TBEV by consuming the blood of a viremic host (3). As soon as viremia comes to an end, this route of transmission is blocked by circulating antibodies (
) to the animal host (1), leading to viremia (2). Naïve ticks acquire TBEV by consuming the blood of a viremic host (3). As soon as viremia comes to an end, this route of transmission is blocked by circulating antibodies ( ) (4). Co-feeding enables ticks to pass TBEV among themselves without the need for a viremic host. When naïve ticks feed in close proximity with an infected tick, the animal host acts as a transmission bridge (5). This can take place even when the host has antibodies against TBEV (6).
) (4). Co-feeding enables ticks to pass TBEV among themselves without the need for a viremic host. When naïve ticks feed in close proximity with an infected tick, the animal host acts as a transmission bridge (5). This can take place even when the host has antibodies against TBEV (6).
 ) to the animal host (1), leading to viremia (2). Naïve ticks acquire TBEV by consuming the blood of a viremic host (3). As soon as viremia comes to an end, this route of transmission is blocked by circulating antibodies (
) to the animal host (1), leading to viremia (2). Naïve ticks acquire TBEV by consuming the blood of a viremic host (3). As soon as viremia comes to an end, this route of transmission is blocked by circulating antibodies (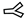 ) (4). Co-feeding enables ticks to pass TBEV among themselves without the need for a viremic host. When naïve ticks feed in close proximity with an infected tick, the animal host acts as a transmission bridge (5). This can take place even when the host has antibodies against TBEV (6).
) (4). Co-feeding enables ticks to pass TBEV among themselves without the need for a viremic host. When naïve ticks feed in close proximity with an infected tick, the animal host acts as a transmission bridge (5). This can take place even when the host has antibodies against TBEV (6).
| Genus | Apodemus | Myodes | Microtus | Sorex | Sicista | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Species | A. flavicollis | A. sylvaticus | A. agrarius | My. glareolus | M. arvalis | M. agrestis | M. subterraneus | M. oeconomus | S. araneus | S. sp. | ||||
| pos./total | pos./total | pos./total | pos./total | pos./total | pos./total | pos./total | pos./total | pos./total | pos./total | |||||
| Country | Publication | |||||||||||||
| CZE | [73] | 2/144 | 0/17 | 2/92 | 0/8 | 0/3 | ||||||||
| [72] | 0/77 | 0/34 | 1/41 | 0/2 | 0/1 | 0/1 | ||||||||
| SVN | [71] | 33/820 | 7/66 | 4/160 | 39/272 | |||||||||
| SVK | [63] | 18/290 | 2/14 | 2/12 | ||||||||||
| [76] | 130/717 | 36/408 | 233/1538 | 14/161 | 0/2 | 4/29 | ||||||||
| HUN | [74] | 4/100 | 0/11 | 4/55 | 6/150 | 3/48 | 0/2 | 0/31 | 0/8 | |||||
| [75] | 12/327 | 8/174 | 8/39 | 0/1 | ||||||||||
| DEU | [69] | 10/123 | 2/7 | 3/24 | 21/163 | 2/21 | 7/101 | |||||||
| [77] | 14/103 | 1/19 | 14/91 | 1/2 | ||||||||||
| CHE | [70] | 1/77 | 3/104 | 8/152 | ||||||||||
| FIN | [78] | 12/80 | 17/95 | 0/23 | ||||||||||
| Species | A. agrarius | My. rutilus | My. rufocans | S. araneus | Si. betulina | |||||||||
| pos./total | pos./total | pos./total | pos./total | pos./total | ||||||||||
| Country | ||||||||||||||
| KOR | [83] | 5/24 | ||||||||||||
| RUS | [79] 1 | 12/34 (16/34) | 25/32 (37/45) | 18/39 | 22/30 | 14/18 | ||||||||
| pos.% | pos.% | pos.% | ||||||||||||
| RUS | [80] | 43.3 ± 9 | 80.0 ± 9.2 | 69.2 ± 12.8 | ||||||||||
| 40.6 ± 8.7 | 61.9 ± 10.8 | 83.3 ± 6.8 | ||||||||||||
| Species | A. speciosus | A. aregenteus | My. smithii | My. rufocans | M. montebelli | M. minutus | S. unguiculatus | S. sp. | ||||||
| pos./total. | pos./total. | pos./total. | pos./total. | pos./total. | pos./total. | pos./total. | pos./total. | |||||||
| Country | ||||||||||||||
| JPN | [81] | 4/24 | 1/37 | 14/95 | 0/6 | 0/2 | ||||||||
| [82] | 2/455 | 0/36 | 0/24 | 0/47 | 0/1 | 0/5 | ||||||||
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Michelitsch, A.; Wernike, K.; Klaus, C.; Dobler, G.; Beer, M. Exploring the Reservoir Hosts of Tick-Borne Encephalitis Virus. Viruses 2019, 11, 669. https://doi.org/10.3390/v11070669
Michelitsch A, Wernike K, Klaus C, Dobler G, Beer M. Exploring the Reservoir Hosts of Tick-Borne Encephalitis Virus. Viruses. 2019; 11(7):669. https://doi.org/10.3390/v11070669
Chicago/Turabian StyleMichelitsch, Anna, Kerstin Wernike, Christine Klaus, Gerhard Dobler, and Martin Beer. 2019. "Exploring the Reservoir Hosts of Tick-Borne Encephalitis Virus" Viruses 11, no. 7: 669. https://doi.org/10.3390/v11070669
APA StyleMichelitsch, A., Wernike, K., Klaus, C., Dobler, G., & Beer, M. (2019). Exploring the Reservoir Hosts of Tick-Borne Encephalitis Virus. Viruses, 11(7), 669. https://doi.org/10.3390/v11070669





