Human Norovirus: Experimental Models of Infection
Abstract
1. Introduction
2. Large Animal Models
2.1. Non-Human Primates (NHPs)
2.2. Gnotobiotic (Gn) Piglets
2.3. Gn Calves
3. Small Animal Models
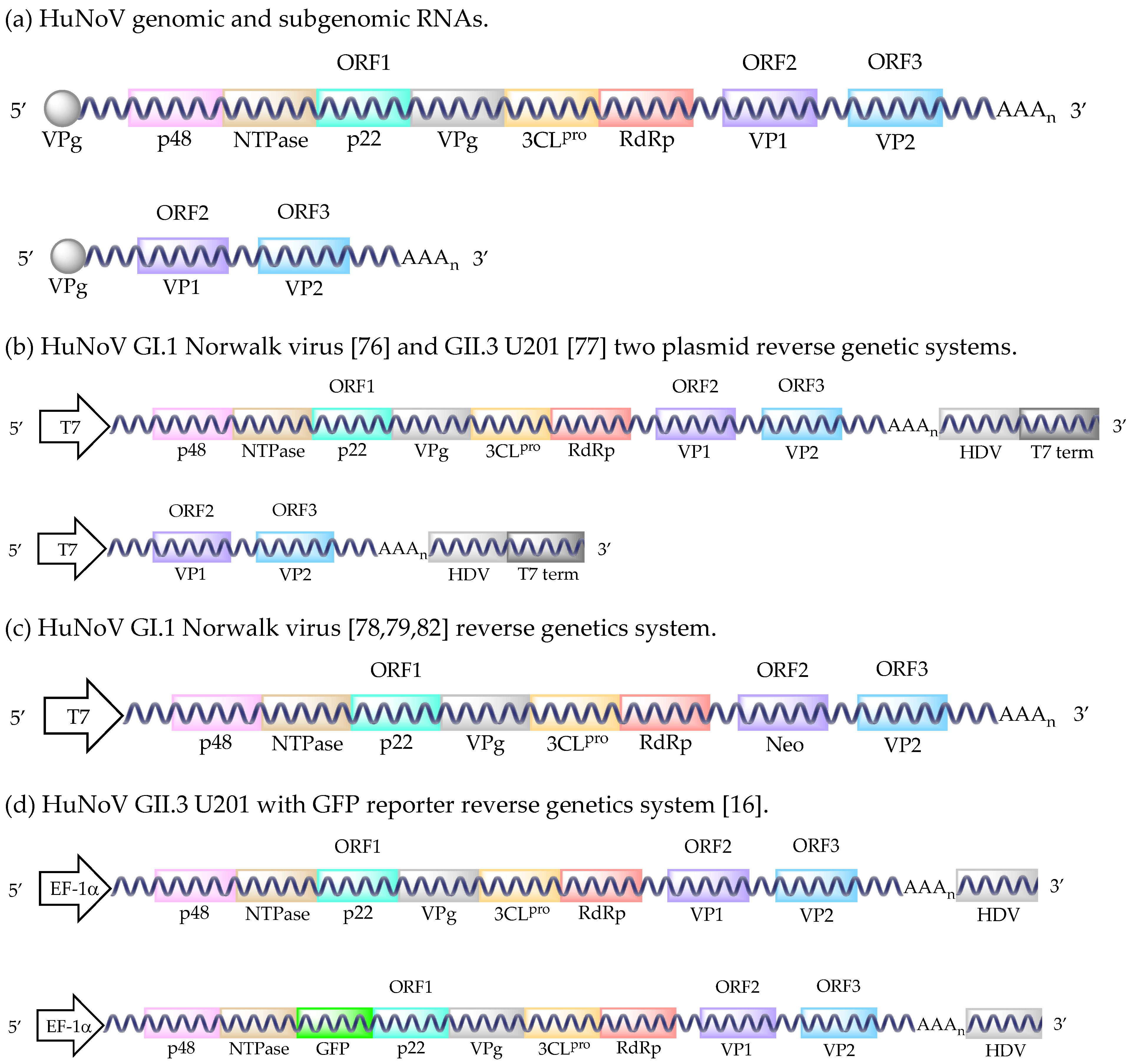
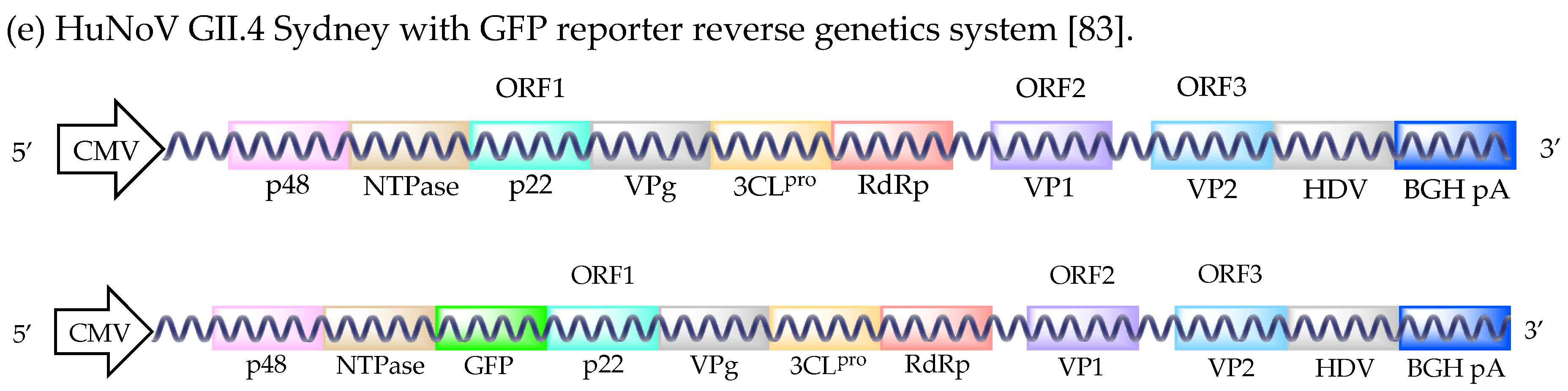
4. Reverse Genetic Systems
5. Conclusions
Author Contributions
Conflicts of Interest
References
- Green, K.Y. Caliciviridae: The Noroviruses, 6th ed.; Wolters Kluwer Health/Lippincott Williams & Wilkins: Philadelphia, PA, USA, 2013; Volume 1, pp. 582–608. [Google Scholar]
- Dolin, R.; Blacklow, N.R.; DuPont, H.; Buscho, R.F.; Wyatt, R.G.; Kasel, J.A.; Hornick, R.; Chanock, R.M. Biological properties of Norwalk agent of acute infectious nonbacterial gastroenteritis. Proc. Soc. Exp. Biol. Med. 1972, 140, 578–583. [Google Scholar] [CrossRef]
- Thorne, L.G.; Goodfellow, I.G. Norovirus gene expression and replication. J. Gen. Virol. 2014, 95, 278–291. [Google Scholar] [CrossRef] [PubMed]
- Lambden, P.R.; Caul, E.O.; Ashley, C.R.; Clarke, I.N. Sequence and genome organization of a human small round-structured (Norwalk-like) virus. Science 1993, 259, 516–519. [Google Scholar] [CrossRef]
- Hardy, M.E. Norovirus protein structure and function. FEMS Microbiol. Lett. 2005, 253, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Jiang, X.; Wang, M.; Graham, D.Y.; Estes, M.K. Expression, self-assembly, and antigenicity of the Norwalk virus capsid protein. J. Virol. 1992, 66, 6527–6532. [Google Scholar] [PubMed]
- Proceedings of the Minutes of the 5th Meeting of the ICTV, Strasbourg, France, 4 August 1981; pp. 1–8.
- Vinje, J. Advances in laboratory methods for detection and typing of norovirus. J. Clin. Microbiol. 2015, 53, 373–381. [Google Scholar] [CrossRef] [PubMed]
- Kroneman, A.; Vega, E.; Vennema, H.; Vinje, J.; White, P.A.; Hansman, G.; Green, K.; Martella, V.; Katayama, K.; Koopmans, M. Proposal for a unified norovirus nomenclature and genotyping. Arch. Virol. 2013, 158, 2059–2068. [Google Scholar] [CrossRef] [PubMed]
- Chhabra, P.; Aswath, K.; Collins, N.; Ahmed, T.; Olortegui, M.P.; Kosek, M.; Cebelinski, E.; Cooper, P.J.; Bucardo, F.; Lopez, M.R.; et al. Near-Complete Genome Sequences of Several New Norovirus Genogroup II Genotypes. Genome Announce. 2018, 6. [Google Scholar] [CrossRef]
- Taube, S.; Wobus, C.E. A novel reverse genetics system for human norovirus. Trends Microbiol. 2014, 22, 604–606. [Google Scholar] [CrossRef]
- Tian, P.; Brandl, M.; Mandrell, R. Porcine gastric mucin binds to recombinant norovirus particles and competitively inhibits their binding to histo-blood group antigens and Caco-2 cells. Lett. Appl. Microbiol. 2005, 41, 315–320. [Google Scholar] [CrossRef]
- Tian, P.; Jiang, X.; Zhong, W.; Jensen, H.M.; Brandl, M.; Bates, A.H.; Engelbrektson, A.L.; Mandrell, R. Binding of recombinant norovirus like particle to histo-blood group antigen on cells in the lumen of pig duodenum. Res. Vet. Sci. 2007, 83, 410–418. [Google Scholar] [CrossRef] [PubMed]
- Tian, P.; Yang, D.; Jiang, X.; Zhong, W.; Cannon, J.L.; Burkhardt, W., 3rd; Woods, J.W.; Hartman, G.; Lindesmith, L.; Baric, R.S.; et al. Specificity and kinetics of norovirus binding to magnetic bead-conjugated histo-blood group antigens. J. Appl. Microbiol. 2010, 109, 1753–1762. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, D.I.; Atmar, R.L.; Lyon, G.M.; Treanor, J.J.; Chen, W.H.; Jiang, X.; Vinje, J.; Gregoricus, N.; Frenck, R.W., Jr.; Moe, C.L.; et al. Norovirus vaccine against experimental human GII.4 virus illness: A challenge study in healthy adults. J. Infect. Dis. 2015, 211, 870–878. [Google Scholar] [CrossRef] [PubMed]
- Katayama, K.; Murakami, K.; Sharp, T.M.; Guix, S.; Oka, T.; Takai-Todaka, R.; Nakanishi, A.; Crawford, S.E.; Atmar, R.L.; Estes, M.K. Plasmid-based human norovirus reverse genetics system produces reporter-tagged progeny virus containing infectious genomic RNA. Proc. Natl. Acad. Sci. USA 2014, 111, E4043–E4052. [Google Scholar] [CrossRef] [PubMed]
- Batz, M.B.; Hoffmann, S.; Morris, J.G., Jr. Ranking the disease burden of 14 pathogens in food sources in the United States using attribution data from outbreak investigations and expert elicitation. J. Food Prot. 2012, 75, 1278–1291. [Google Scholar] [CrossRef] [PubMed]
- Bartsch, S.M.; Lopman, B.A.; Hall, A.J.; Parashar, U.D.; Lee, B.Y. The potential economic value of a human norovirus vaccine for the United States. Vaccine 2012, 30, 7097–7104. [Google Scholar] [CrossRef] [PubMed]
- Scallan, E.; Hoekstra, R.M.; Angulo, F.J.; Tauxe, R.V.; Widdowson, M.A.; Roy, S.L.; Jones, J.L.; Griffin, P.M. Foodborne illness acquired in the United States—Major pathogens. Emerg. Infect. Dis. 2011, 17, 7–15. [Google Scholar] [CrossRef]
- Devasia, T.; Lopman, B.; Leon, J.; Handel, A. Association of host, agent and environment characteristics and the duration of incubation and symptomatic periods of norovirus gastroenteritis. Epidemiol. Infect. 2015, 143, 2308–2314. [Google Scholar] [CrossRef]
- Kaplan, J.E.; Feldman, R.; Campbell, D.S.; Lookabaugh, C.; Gary, G.W. The frequency of a Norwalk-like pattern of illness in outbreaks of acute gastroenteritis. Am. J. Public. Health 1982, 72, 1329–1332. [Google Scholar] [CrossRef]
- Turcios, R.M.; Widdowson, M.A.; Sulka, A.C.; Mead, P.S.; Glass, R.I. Reevaluation of epidemiological criteria for identifying outbreaks of acute gastroenteritis due to norovirus: United States, 1998–2000. Clin. Infect. Dis. 2006, 42, 964–969. [Google Scholar] [CrossRef]
- Atmar, R.L.; Opekun, A.R.; Gilger, M.A.; Estes, M.K.; Crawford, S.E.; Neill, F.H.; Graham, D.Y. Norwalk virus shedding after experimental human infection. Emerg. Infect. Dis. 2008, 14, 1553–1557. [Google Scholar] [CrossRef] [PubMed]
- Atmar, R.L.; Opekun, A.R.; Gilger, M.A.; Estes, M.K.; Crawford, S.E.; Neill, F.H.; Ramani, S.; Hill, H.; Ferreira, J.; Graham, D.Y. Determination of the 50% human infectious dose for Norwalk virus. J. Infect. Dis. 2014, 209, 1016–1022. [Google Scholar] [CrossRef] [PubMed]
- Roth, A.N.; Karst, S.M. Norovirus mechanisms of immune antagonism. Curr. Opin. Virol. 2016, 16, 24–30. [Google Scholar] [CrossRef] [PubMed]
- Gustavsson, L.; Skovbjerg, S.; Lindh, M.; Westin, J.; Andersson, L.M. Low serum levels of CCL5 are associated with longer duration of viral shedding in norovirus infection. J. Clin. Virol. 2015, 69, 133–137. [Google Scholar] [CrossRef] [PubMed]
- Bartsch, S.M.; Lopman, B.A.; Ozawa, S.; Hall, A.J.; Lee, B.Y. Global Economic Burden of Norovirus Gastroenteritis. PLoS ONE 2016, 11, e0151219. [Google Scholar] [CrossRef] [PubMed]
- Ball, J.M.; Hardy, M.E.; Atmar, R.L.; Conner, M.E.; Estes, M.K. Oral immunization with recombinant Norwalk virus-like particles induces a systemic and mucosal immune response in mice. J. Virol. 1998, 72, 1345–1353. [Google Scholar] [PubMed]
- Harrington, P.R.; Lindesmith, L.; Yount, B.; Moe, C.L.; Baric, R.S. Binding of Norwalk virus-like particles to ABH histo-blood group antigens is blocked by antisera from infected human volunteers or experimentally vaccinated mice. J. Virol. 2002, 76, 12335–12343. [Google Scholar] [CrossRef]
- LoBue, A.D.; Lindesmith, L.; Yount, B.; Harrington, P.R.; Thompson, J.M.; Johnston, R.E.; Moe, C.L.; Baric, R.S. Multivalent norovirus vaccines induce strong mucosal and systemic blocking antibodies against multiple strains. Vaccine 2006, 24, 5220–5234. [Google Scholar] [CrossRef]
- Heinimaki, S.; Malm, M.; Vesikari, T.; Blazevic, V. Parenterally Administered Norovirus GII.4 Virus-Like Particle Vaccine Formulated with Aluminum Hydroxide or Monophosphoryl Lipid A Adjuvants Induces Systemic but Not Mucosal Immune Responses in Mice. J. Immunol. Res. 2018, 2018, 3487095. [Google Scholar] [CrossRef]
- Hwang, H.S.; Puth, S.; Tan, W.; Verma, V.; Jeong, K.; Lee, S.E.; Rhee, J.H. More robust gut immune responses induced by combining intranasal and sublingual routes for prime-boost immunization. Hum. Vaccin. Immunother. 2018, 1–9. [Google Scholar] [CrossRef]
- Guerrero, R.A.; Ball, J.M.; Krater, S.S.; Pacheco, S.E.; Clements, J.D.; Estes, M.K. Recombinant Norwalk virus-like particles administered intranasally to mice induce systemic and mucosal (fecal and vaginal) immune responses. J. Virol. 2001, 75, 9713–9722. [Google Scholar] [CrossRef]
- Velasquez, L.S.; Shira, S.; Berta, A.N.; Kilbourne, J.; Medi, B.M.; Tizard, I.; Ni, Y.; Arntzen, C.J.; Herbst-Kralovetz, M.M. Intranasal delivery of Norwalk virus-like particles formulated in an in situ gelling, dry powder vaccine. Vaccine 2011, 29, 5221–5231. [Google Scholar] [CrossRef] [PubMed]
- Springer, M.J.; Ni, Y.; Finger-Baker, I.; Ball, J.P.; Hahn, J.; DiMarco, A.V.; Kobs, D.; Horne, B.; Talton, J.D.; Cobb, R.R. Preclinical dose-ranging studies of a novel dry powder norovirus vaccine formulation. Vaccine 2016, 34, 1452–1458. [Google Scholar] [CrossRef] [PubMed]
- Souza, M.; Costantini, V.; Azevedo, M.S.; Saif, L.J. A human norovirus-like particle vaccine adjuvanted with ISCOM or mLT induces cytokine and antibody responses and protection to the homologous GII.4 human norovirus in a gnotobiotic pig disease model. Vaccine 2007, 25, 8448–8459. [Google Scholar] [CrossRef] [PubMed]
- Han, M.G.; Cheetham, S.; Azevedo, M.; Thomas, C.; Saif, L.J. Immune responses to bovine norovirus-like particles with various adjuvants and analysis of protection in gnotobiotic calves. Vaccine 2006, 24, 317–326. [Google Scholar] [CrossRef] [PubMed]
- Bok, K.; Parra, G.I.; Mitra, T.; Abente, E.; Shaver, C.K.; Boon, D.; Engle, R.; Yu, C.; Kapikian, A.Z.; Sosnovtsev, S.V.; et al. Chimpanzees as an animal model for human norovirus infection and vaccine development. Proc. Natl. Acad. Sci. USA 2011, 108, 325–330. [Google Scholar] [CrossRef] [PubMed]
- Treanor, J.J.; Atmar, R.L.; Frey, S.E.; Gormley, R.; Chen, W.H.; Ferreira, J.; Goodwin, R.; Borkowski, A.; Clemens, R.; Mendelman, P.M. A novel intramuscular bivalent norovirus virus-like particle vaccine candidate—Reactogenicity, safety, and immunogenicity in a phase 1 trial in healthy adults. J. Infect. Dis. 2014, 210, 1763–1771. [Google Scholar] [CrossRef] [PubMed]
- Leroux-Roels, G.; Cramer, J.P.; Mendelman, P.M.; Sherwood, J.; Clemens, R.; Aerssens, A.; De Coster, I.; Borkowski, A.; Baehner, F.; Van Damme, P. Safety and Immunogenicity of Different Formulations of Norovirus Vaccine Candidate in Healthy Adults: A Randomized, Controlled, Double-Blind Clinical Trial. J. Infect. Dis. 2018, 217, 597–607. [Google Scholar] [CrossRef]
- Parra, G.I.; Bok, K.; Taylor, R.; Haynes, J.R.; Sosnovtsev, S.V.; Richardson, C.; Green, K.Y. Immunogenicity and specificity of norovirus Consensus GII.4 virus-like particles in monovalent and bivalent vaccine formulations. Vaccine 2012, 30, 3580–3586. [Google Scholar] [CrossRef]
- Kim, L.; Liebowitz, D.; Lin, K.; Kasparek, K.; Pasetti, M.F.; Garg, S.J.; Gottlieb, K.; Trager, G.; Tucker, S.N. Safety and immunogenicity of an oral tablet norovirus vaccine, a phase I randomized, placebo-controlled trial. JCI Insight 2018, 3. [Google Scholar] [CrossRef]
- Wyatt, R.G.; Greenberg, H.B.; Dalgard, D.W.; Allen, W.P.; Sly, D.L.; Thornhill, T.S.; Chanock, R.M.; Kapikian, A.Z. Experimental infection of chimpanzees with the Norwalk agent of epidemic viral gastroenteritis. J. Med. Virol. 1978, 2, 89–96. [Google Scholar] [CrossRef] [PubMed]
- Taube, S.; Kolawole, A.O.; Hohne, M.; Wilkinson, J.E.; Handley, S.A.; Perry, J.W.; Thackray, L.B.; Akkina, R.; Wobus, C.E. A mouse model for human norovirus. mBio 2013, 4. [Google Scholar] [CrossRef] [PubMed]
- Jones, M.K.; Grau, K.R.; Costantini, V.; Kolawole, A.O.; de Graaf, M.; Freiden, P.; Graves, C.L.; Koopmans, M.; Wallet, S.M.; Tibbetts, S.A.; et al. Human norovirus culture in B cells. Nat. Prot. 2015, 10, 1939–1947. [Google Scholar] [CrossRef] [PubMed]
- Jones, M.K.; Watanabe, M.; Zhu, S.; Graves, C.L.; Keyes, L.R.; Grau, K.R.; Gonzalez-Hernandez, M.B.; Iovine, N.M.; Wobus, C.E.; Vinje, J.; et al. Enteric bacteria promote human and mouse norovirus infection of B cells. Science 2014, 346, 755–759. [Google Scholar] [CrossRef] [PubMed]
- Kolawole, A.O.; Rocha-Pereira, J.; Elftman, M.D.; Neyts, J.; Wobus, C.E. Inhibition of human norovirus by a viral polymerase inhibitor in the B cell culture system and in the mouse model. Antivir. Res. 2016, 132, 46–49. [Google Scholar] [CrossRef] [PubMed]
- Ettayebi, K.; Crawford, S.E.; Murakami, K.; Broughman, J.R.; Karandikar, U.; Tenge, V.R.; Neill, F.H.; Blutt, S.E.; Zeng, X.L.; Qu, L.; et al. Replication of human noroviruses in stem cell-derived human enteroids. Science 2016, 353, 1387–1393. [Google Scholar] [CrossRef] [PubMed]
- Costantini, V.; Morantz, E.K.; Browne, H.; Ettayebi, K.; Zeng, X.L.; Atmar, R.L.; Estes, M.K.; Vinje, J. Human Norovirus Replication in Human Intestinal Enteroids as Model to Evaluate Virus Inactivation. Emerg. Infect. Dis. 2018, 24, 1453–1464. [Google Scholar] [CrossRef] [PubMed]
- Alvarado, G.; Ettayebi, K.; Atmar, R.L.; Bombardi, R.G.; Kose, N.; Estes, M.K.; Crowe, J.E., Jr. Human Monoclonal Antibodies That Neutralize Pandemic GII.4 Noroviruses. Gastroenterology 2018. [Google Scholar] [CrossRef]
- Santiana, M.; Ghosh, S.; Ho, B.A.; Rajasekaran, V.; Du, W.L.; Mutsafi, Y.; De Jesus-Diaz, D.A.; Sosnovtsev, S.V.; Levenson, E.A.; Parra, G.I.; et al. Vesicle-Cloaked Virus Clusters Are Optimal Units for Inter-organismal Viral Transmission. Cell Host Microbe 2018, 24, 208–220.e208. [Google Scholar] [CrossRef]
- WHO. Recommendations for the Evaluation of Animal Cell Cultures as Substrates for the Manufacture of Biological Medicinal Products and for the Characterization of Cells Banks; WHO Press: Geneva, Switzerland, 2013; pp. 79–187. [Google Scholar]
- Subekti, D.S.; Tjaniadi, P.; Lesmana, M.; McArdle, J.; Iskandriati, D.; Budiarsa, I.N.; Walujo, P.; Suparto, I.H.; Winoto, I.; Campbell, J.R.; et al. Experimental infection of Macaca nemestrina with a Toronto Norwalk-like virus of epidemic viral gastroenteritis. J. Med. Virol. 2002, 66, 400–406. [Google Scholar] [CrossRef]
- Rockx, B.H.; Bogers, W.M.; Heeney, J.L.; van Amerongen, G.; Koopmans, M.P. Experimental norovirus infections in non-human primates. J. Med. Virol. 2005, 75, 313–320. [Google Scholar] [CrossRef] [PubMed]
- Cheetham, S.; Souza, M.; Meulia, T.; Grimes, S.; Han, M.G.; Saif, L.J. Pathogenesis of a genogroup II human norovirus in gnotobiotic pigs. J. Virol. 2006, 80, 10372–10381. [Google Scholar] [CrossRef] [PubMed]
- Takanashi, S.; Wang, Q.; Chen, N.; Shen, Q.; Jung, K.; Zhang, Z.; Yokoyama, M.; Lindesmith, L.C.; Baric, R.S.; Saif, L.J. Characterization of emerging GII.g/GII.12 noroviruses from a gastroenteritis outbreak in the United States in 2010. J. Clin. Microbiol. 2011, 49, 3234–3244. [Google Scholar] [CrossRef] [PubMed]
- Bui, T.; Kocher, J.; Li, Y.; Wen, K.; Li, G.; Liu, F.; Yang, X.; LeRoith, T.; Tan, M.; Xia, M.; et al. Median infectious dose of human norovirus GII.4 in gnotobiotic pigs is decreased by simvastatin treatment and increased by age. J. Gen. Virol. 2013, 94, 2005–2016. [Google Scholar] [CrossRef] [PubMed]
- Lei, S.; Ryu, J.; Wen, K.; Twitchell, E.; Bui, T.; Ramesh, A.; Weiss, M.; Li, G.; Samuel, H.; Clark-Deener, S.; et al. Increased and prolonged human norovirus infection in RAG2/IL2RG deficient gnotobiotic pigs with severe combined immunodeficiency. Sci. Rep. 2016, 6, 25222. [Google Scholar] [CrossRef] [PubMed]
- Park, B.J.; Jung, S.T.; Choi, C.S.; Myoung, J.J.; Ahn, H.S.; Han, S.H.; Kim, Y.H.; Go, H.J.; Lee, J.B.; Park, S.Y.; et al. Pathogenesis of human norovirus genogroup II genotype 4 in post-weaning gnotobiotic pigs. J. Microl. Biotechnol. 2018, 28, 2133–2140. [Google Scholar] [CrossRef]
- Kocher, J.; Bui, T.; Giri-Rachman, E.; Wen, K.; Li, G.; Yang, X.; Liu, F.; Tan, M.; Xia, M.; Zhong, W.; et al. Intranasal P particle vaccine provided partial cross-variant protection against human GII.4 norovirus diarrhea in gnotobiotic pigs. J. Virol. 2014, 88, 9728–9743. [Google Scholar] [CrossRef]
- Souza, M.; Cheetham, S.M.; Azevedo, M.S.; Costantini, V.; Saif, L.J. Cytokine and antibody responses in gnotobiotic pigs after infection with human norovirus genogroup II.4 (HS66 strain). J. Virol. 2007, 81, 9183–9192. [Google Scholar] [CrossRef]
- Teunis, P.F.; Moe, C.L.; Liu, P.; Miller, S.E.; Lindesmith, L.; Baric, R.S.; Le Pendu, J.; Calderon, R.L. Norwalk virus: How infectious is it? J. Med. Virol. 2008, 80, 1468–1476. [Google Scholar] [CrossRef]
- Lou, F.; Ye, M.; Ma, Y.; Li, X.; DiCaprio, E.; Chen, H.; Krakowka, S.; Hughes, J.; Kingsley, D.; Li, J. A Gnotobiotic Pig Model for Determining Human Norovirus Inactivation by High-Pressure Processing. Appl. Environ. Microbiol. 2015, 81, 6679–6687. [Google Scholar] [CrossRef]
- Seo, D.J.; Jung, D.; Jung, S.; Ha, S.K.; Ha, S.D.; Choi, I.S.; Myoung, J.; Choi, C. Experimental miniature piglet model for the infection of human norovirus GII. J. Med. Virol. 2017. [Google Scholar] [CrossRef]
- Jung, K.; Wang, Q.; Kim, Y.; Scheuer, K.; Zhang, Z.; Shen, Q.; Chang, K.O.; Saif, L.J. The effects of simvastatin or interferon-alpha on infectivity of human norovirus using a gnotobiotic pig model for the study of antivirals. PLoS ONE 2012, 7, e41619. [Google Scholar] [CrossRef]
- Rondy, M.; Koopmans, M.; Rotsaert, C.; Van Loon, T.; Beljaars, B.; Van Dijk, G.; Siebenga, J.; Svraka, S.; Rossen, J.W.; Teunis, P.; et al. Norovirus disease associated with excess mortality and use of statins: A retrospective cohort study of an outbreak following a pilgrimage to Lourdes. Epidemiol. Infect. 2011, 139, 453–463. [Google Scholar] [CrossRef]
- Lei, S.; Samuel, H.; Twitchell, E.; Bui, T.; Ramesh, A.; Wen, K.; Weiss, M.; Li, G.; Yang, X.; Jiang, X.; et al. Enterobacter cloacae inhibits human norovirus infectivity in gnotobiotic pigs. Sci. Rep. 2016, 6, 25017. [Google Scholar] [CrossRef] [PubMed]
- Pfeiffer, J.K.; Virgin, H.W. Viral immunity. Transkingdom control of viral infection and immunity in the mammalian intestine. Science 2016, 351. [Google Scholar] [CrossRef] [PubMed]
- Erickson, A.K.; Jesudhasan, P.R.; Mayer, M.J.; Narbad, A.; Winter, S.E.; Pfeiffer, J.K. Bacteria Facilitate Enteric Virus Co-infection of Mammalian Cells and Promote Genetic Recombination. Cell Host Microbe 2018, 23, 77–88.e75. [Google Scholar] [CrossRef]
- Almand, E.A.; Moore, M.D.; Outlaw, J.; Jaykus, L.A. Human norovirus binding to select bacteria representative of the human gut microbiota. PLoS ONE 2017, 12, e0173124. [Google Scholar] [CrossRef]
- Tan, M.; Jiang, X. Histo-blood group antigens: A common niche for norovirus and rotavirus. Expert Rev. Mol. Med. 2014, 16, e5. [Google Scholar] [CrossRef]
- Schroten, H.; Hanisch, F.G.; Hansman, G.S. Human Norovirus Interactions with Histo-Blood Group Antigens and Human Milk Oligosaccharides. J. Virol. 2016, 90, 5855–5859. [Google Scholar] [CrossRef]
- Cheetham, S.; Souza, M.; McGregor, R.; Meulia, T.; Wang, Q.; Saif, L.J. Binding patterns of human norovirus-like particles to buccal and intestinal tissues of gnotobiotic pigs in relation to A/H histo-blood group antigen expression. J. Virol. 2007, 81, 3535–3544. [Google Scholar] [CrossRef] [PubMed]
- Souza, M.; Azevedo, M.S.; Jung, K.; Cheetham, S.; Saif, L.J. Pathogenesis and immune responses in gnotobiotic calves after infection with the genogroup II.4-HS66 strain of human norovirus. J. Virol. 2008, 82, 1777–1786. [Google Scholar] [CrossRef] [PubMed]
- Guix, S.; Asanaka, M.; Katayama, K.; Crawford, S.E.; Neill, F.H.; Atmar, R.L.; Estes, M.K. Norwalk virus RNA is infectious in mammalian cells. J. Virol. 2007, 81, 12238–12248. [Google Scholar] [CrossRef] [PubMed]
- Asanaka, M.; Atmar, R.L.; Ruvolo, V.; Crawford, S.E.; Neill, F.H.; Estes, M.K. Replication and packaging of Norwalk virus RNA in cultured mammalian cells. Proc. Natl. Acad. Sci. USA 2005, 102, 10327–10332. [Google Scholar] [CrossRef] [PubMed]
- Katayama, K.; Hansman, G.S.; Oka, T.; Ogawa, S.; Takeda, N. Investigation of norovirus replication in a human cell line. Arch. Virol. 2006, 151, 1291–1308. [Google Scholar] [CrossRef] [PubMed]
- Chang, K.O.; Sosnovtsev, S.V.; Belliot, G.; King, A.D.; Green, K.Y. Stable expression of a Norwalk virus RNA replicon in a human hepatoma cell line. Virology 2006, 353, 463–473. [Google Scholar] [CrossRef] [PubMed]
- Chang, K.O.; George, D.W. Interferons and ribavirin effectively inhibit Norwalk virus replication in replicon-bearing cells. J. Virol. 2007, 81, 12111–12118. [Google Scholar] [CrossRef]
- Rocha-Pereira, J.; Jochmans, D.; Debing, Y.; Verbeken, E.; Nascimento, M.S.; Neyts, J. The viral polymerase inhibitor 2′-C-methylcytidine inhibits Norwalk virus replication and protects against norovirus-induced diarrhea and mortality in a mouse model. J. Virol. 2013, 87, 11798–11805. [Google Scholar] [CrossRef]
- Van Dycke, J.; Arnoldi, F.; Papa, G.; Vandepoele, J.; Burrone, O.R.; Mastrangelo, E.; Tarantino, D.; Heylen, E.; Neyts, J.; Rocha-Pereira, J. A Single Nucleoside Viral Polymerase Inhibitor Against Norovirus, Rotavirus, and Sapovirus-Induced Diarrhea. J. Infect. Dis. 2018, 218, 1753–1758. [Google Scholar] [CrossRef]
- Kitano, M.; Hosmillo, M.; Emmott, E.; Lu, J.; Goodfellow, I. Selection and Characterization of Rupintrivir-Resistant Norwalk Virus Replicon Cells in vitro. Antimicrob. Agents Chemother. 2018. [Google Scholar] [CrossRef]
- Oliveira, L.M.; Blawid, R.; Orilio, A.F.; Andrade, B.Y.G.; Souza, A.C.A.; Nagata, T. Development of an infectious clone and replicon system of norovirus GII.4. J. Virol. Methods 2018, 258, 49–53. [Google Scholar] [CrossRef]
- Meyer, R.C.; Bohl, E.H.; Kohler, E.M. Procurement and Maintenance Of Germ-Free Seine For Microbiological Investigations. Appl. Microbiol. 1964, 12, 295–300. [Google Scholar] [PubMed]
- Yuan, L.; Jobst, P.M.; Weiss, M. Chapter 5—Gnotobiotic Pigs: From Establishing Facility to Modeling Human Infectious Diseases. In Gnotobiotics; Schoeb, T.R., Eaton, K.A., Eds.; Academic Press: Cambridge, MA, USA, 2017; pp. 349–368. [Google Scholar]
- Chaudhry, Y.; Skinner, M.A.; Goodfellow, I.G. Recovery of genetically defined murine norovirus in tissue culture by using a fowlpox virus expressing T7 RNA polymerase. J. Gen. Virol. 2007, 88, 2091–2100. [Google Scholar] [CrossRef] [PubMed]
- Ward, V.K.; McCormick, C.J.; Clarke, I.N.; Salim, O.; Wobus, C.E.; Thackray, L.B.; Virgin, H.W.t.; Lambden, P.R. Recovery of infectious murine norovirus using pol II-driven expression of full-length cDNA. Proc. Natl. Acad. Sci. USA 2007, 104, 11050–11055. [Google Scholar] [CrossRef] [PubMed]
- Yunus, M.A.; Chung, L.M.; Chaudhry, Y.; Bailey, D.; Goodfellow, I. Development of an optimized RNA-based murine norovirus reverse genetics system. J. Virol. Methods 2010, 169, 112–118. [Google Scholar] [CrossRef] [PubMed]
- Orchard, R.C.; Wilen, C.B.; Doench, J.G.; Baldridge, M.T.; McCune, B.T.; Lee, Y.C.; Lee, S.; Pruett-Miller, S.M.; Nelson, C.A.; Fremont, D.H.; et al. Discovery of a proteinaceous cellular receptor for a norovirus. Science 2016, 353, 933–936. [Google Scholar] [CrossRef] [PubMed]
- Haga, K.; Fujimoto, A.; Takai-Todaka, R.; Miki, M.; Doan, Y.H.; Murakami, K.; Yokoyama, M.; Murata, K.; Nakanishi, A.; Katayama, K. Functional receptor molecules CD300lf and CD300ld within the CD300 family enable murine noroviruses to infect cells. Proc. Natl. Acad. Sci. USA 2016, 113, E6248–E6255. [Google Scholar] [CrossRef] [PubMed]
- Thorne, L.; Bailey, D.; Goodfellow, I. High-resolution functional profiling of the norovirus genome. J. Virol. 2012, 86, 11441–11456. [Google Scholar] [CrossRef]
- Thorne, L.; Lu, J.; Chaudhry, Y.; Bailey, D.; Goodfellow, I. Targeting macrophage- and intestinal epithelial cell-specific microRNAs against norovirus restricts replication in vivo. J. Gen. Virol. 2018. [Google Scholar] [CrossRef]
| Model | Ref. | HuNoV Genotype (Strain) | Infect. Route | Fecal Virus Shedding | Shedding Start | Shedding Duration | Diarrhea | Day 1st Detected | Diarrhea Duration | Vomit | AH | HuNoV in Tissue | HuNoV in Serum | Serum Abs | Mucosal Abs |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Chimpanzees | [38] | GI.1 (Norwalk virus) | i.v. | Yes; qRT-PCR | 2, 3, 3, 3, 4, or 5 dpi | 22, 23, 31, 42, 17, or 22 days resp. | No | N/A | N/A | No | No | Yes | NR | IgM and IgG | NR |
| Chimpanzees | [43] | GI.1 (Norwalk virus) passage 0 | oral | Yes; radioimmunoassay | 2, 2.5, or 3 dpi | 2.5, 1.5, or 1 day(s) resp. | No | N/A | N/A | No | NR | NR | NR | IgG | NR |
| Chimpanzees | [43] | GI.1 (Norwalk virus) passage 1 | oral | Yes; radioimmunoassay | 3 or 4 dpi | 3 or 2 days resp. | No | N/A | N/A | No | NR | NR | NR | IgG | NR |
| 1–3 month old pigtail macaques | [53] | GII.3 (Toronto) | oral | Yes; RT-PCR, ELISA, and EM | 1, 2, or 21 dpi | 21, 13, or 1 day(s) resp. | Yes | 2 dpi | 1 or 2 day(s) | No | NR | NR | NR | NR | NR |
| Pigtail macaques (adult) | [53] | GII.3 (Toronto) | oral | Yes; RT-PCR and ELISA | 1 dpi | 21 days | Yes | 3 dpi | 1 day | Yes | NR | NR | NR | IgG | NR |
| Common marmosets | [54] | GI.1 (Norwalk virus) | oral | Yes; RT-PCR | 1 dpi | 3 days | No | N/A | N/A | NR | NR | NR | NR | No | No |
| Cotton-top tamarins | [54] | GI.1 (Norwalk virus) | oral | Yes; RT-PCR | 1 dpi | 4 days | No | N/A | N/A | NR | NR | NR | NR | No | No |
| Cynomolgus macaques | [54] | GI.1 (Norwalk virus) or GII.4 (Grimsby) | oral | No | N/A | N/A | No | N/A | N/A | NR | NR | NR | NR | No | No |
| Rhesus macaques | [54] | GI.1 (Norwalk virus) | oral | Yes; RT-PCR | 1 dpi | 18 days | No | N/A | N/A | NR | NR | NR | NR | IgM and IgG | No |
| 33 day old Gn piglets | [36] | GII.4 (HS66) | oral | Yes; RT-PCR | NR | NR | Yes | DNS | 2 days | NR | NR | NR | NR | No | IgM |
| Gn piglets | [55] | GII.4 (HS66) passage 0 | oral | Yes; RT-PCR | 1 dpi | 3 days | Yes | 2 dpi | 2 days | NR | Yes | Yes | Yes | IgG | NR |
| Gn piglets | [55] | GII.4 (HS66) passage 1 | oral | Yes; RT-PCR | 1 dpi | 2 days | Yes | 2 dpi | 3 days | NR | NR | Yes | No | IgG | NR |
| Gn piglets | [55] | GII.4 (HS66) passage 2 | oral | Yes; RT-PCR | 2 dpi | 2 days | Yes | 2 dpi | 1 day | NR | NR | Yes | No | IgG | NR |
| Gn piglet | [55] | GII.4 (HS66) passage 0 | i.v. | Yes; RT-PCR | DNS | DNS | Yes | DNS | DNS | NR | NR | NR | NR | NR | NR |
| Gn piglet | [55] | GII.4 (HS66) passage 1 | i.v. | No | N/A | N/A | Yes | DNS | DNS | NR | NR | NR | NR | NR | NR |
| 6 day old Gn piglets | [56] | GII.12 (HS206) | oral | Yes; qRT-PCR | 1, 2, 3, or 3 dpi | 3, 3, 8, or 14 days resp. | Yes | 1 dpi | 3 days | NR | NR | NR | NR | NR | NR |
| 4–5 day old Gn piglets | [57] | GII.4 (092895; 2006b variant) | oral | Yes; qRT-PCR | 2 dpi | DNS | Yes | 4 dpi | DNS | NR | Yes | NR | NR | NR | NR |
| 33–34 day old Gn piglets | [57] | GII.4 (092895; 2006b variant) | oral | Yes; qRT-PCR | 3 dpi | DNS | Yes | DNS | DNS | NR | Yes | NR | NR | NR | NR |
| 6–7 day old Gn piglets | [58] | GII.4 (092895; 2006b variant) | oral | Yes; qRT-PCR | 1 dpi | max = 16 days | Yes | DNS | DNS | NR | NR | Yes | Yes | NR | NR |
| 28 day old Gn piglets | [59] | GII.4 (KU131206) | oral | Yes; qRT-PCR | 1 or 2 dpi | 1, 2, or 3 days | Yes | 2 or 3 dpi | 1 or 2 day(s) | NR | Yes | Yes | Yes | NR | NR |
| 32–33 day old Gn piglets | [60] | GII.4 (092895; 2006b variant) | oral | Yes; qRT-PCR | NR | 2 days | Yes | DNS | 2 days | NR | NR | NR | NR | NR | NR |
| 5–7 day old Gn piglets | [61] | GII.4 (HS66) | oral | Yes; RT-PCR and ELISA | NR | 4 days (range = 1–6 days) | Yes | DNS | 4 days (range = 2–6 days) | NR | NR | Yes | Yes | IgM, IgA, and IgG | IgM, IgA, and IgG |
| 2 day old Gn piglets | [63] | GII.4 (765) | oral | Yes; qRT-PCR | 1 or 2 dpi | 6 or 7 days | Yes | DNS | DNS | NR | Yes | Yes | NR | NR | NR |
| 6–7 day old Gn piglets | [65] | GII.4 (HS194) [HuNoV only] | oral | Yes; qRT-PCR | 1 dpi | 11 days | NR | N/A | N/A | NR | NR | NR | NR | NR | NR |
| 6–7 day old Gn piglets | [65] | GII.4 (HS194) [+ IFNα treatment] | oral | Yes; qRT-PCR | 3 dpi | 10 days | NR | N/A | N/A | NR | NR | NR | NR | NR | NR |
| 11 or 13 day old Gn piglets | [65] | GII.4 (HS194) [HuNoV only] | oral | Yes; qRT-PCR | 5 dpi | 9 days | No | N/A | N/A | NR | No | Yes | NR | NR | NR |
| 11 or 13 day old Gn piglets | [65] | GII.4 (HS194) [+ simvastatin treatment] | oral | Yes; qRT-PCR | 2 dpi | 15 days | No | N/A | N/A | NR | No | Yes | NR | NR | NR |
| 6 day old Gn piglets | [67] | GII.4 (092895; 2006b variant) | oral | Yes; qRT-PCR | 2 dpi | 4 days | Yes | 3 dpi | 3 dpi | NR | NR | Yes | Yes | NR | NR |
| RAG2/IL2RG KO Gn piglets | [58] | GII.4 (092895; 2006b variant) | oral | Yes; qRT-PCR | 1 dpi | max = 27 days | Yes | DNS | DNS | NR | NR | Yes | Yes | NR | NR |
| 28 day old miniature piglets | [64] | GII.12/GII.3 (CAU140599) | oral | Yes; qRT-PCR | 1 or 3 dpi (DNS) | 1 day (DNS) | Yes (DNS) | 1, 2, or 3 dpi (DNS) | DNS | NR | No | Yes | Yes | NR | NR |
| 5 day old Gn calves | [74] | GII.4 (HS66) | oral | Yes; qRT-PCR and ELISA | 1 dpi | 3 days (range = 1–6 day(s)) | Yes | 2 dpi | 3 days (range = 2–6 days) | N/A | Yes | Yes | Yes | IgM, IgA, and IgG | IgA and IgG |
| BALB/c mice | [44] | GII mix (GII.4 and GII.6) | oral + i.p. | NR; qRT-PCR | N/A | N/A | NR | N/A | N/A | N/A | No | NR | NR | NR | NR |
| Rag−/−γc−/− BALB/c mice | [44] | GII mix (GII.4 and GII.6) | oral + i.p. | Yes; qRT-PCR | 1 dpi | 2 or 3 days | No | N/A | N/A | N/A | No | Yes | NR | NR | NR |
| Rag−/−γc−/− BALB/c mice | [44] | GI + GII mix (GI.3, GII.4, and GII.6) | oral + i.p. | Yes; qRT-PCR | 1 dpi | 1 day | No | N/A | N/A | N/A | No | Yes | NR | NR | NR |
| Rag−/−γc−/− BALB/c mice | [44] | GII mix (GII.4 and GII.6) | oral | Yes; qRT-PCR | 1 dpi | 1 day | NR | N/A | N/A | N/A | No | No | NR | NR | NR |
| Rag−/−γc−/− BALB/c mice | [44] | GII mix (GII.4 and GII.6) | i.p. | No | N/A | N/A | NR | N/A | N/A | N/A | No | Yes | NR | NR | NR |
| Hum. Rag−/−γc−/− BALB/c mice | [44] | GII mix (GII.4 and GII.6) | oral + i.p. | Yes; qRT-PCR | 1 dpi | 2 days | Yes | 1 dpi | NR | N/A | No | Yes | NR | NR | NR |
| Hum. Rag−/−γc−/− BALB/c mice | [44] | GI + GII mix (GI.3, GII.4, and GII.6) | oral + i.p. | Yes; qRT-PCR | 1 dpi | 1 day | No | N/A | N/A | N/A | No | Yes | NR | NR | NR |
| Rag−/−γc−/− BL/6×BL/10 mice | [44] | GII mix (GII.4 and GII.6) | i.p. | No | N/A | N/A | NR | N/A | N/A | N/A | No | Yes | NR | NR | NR |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Todd, K.V.; Tripp, R.A. Human Norovirus: Experimental Models of Infection. Viruses 2019, 11, 151. https://doi.org/10.3390/v11020151
Todd KV, Tripp RA. Human Norovirus: Experimental Models of Infection. Viruses. 2019; 11(2):151. https://doi.org/10.3390/v11020151
Chicago/Turabian StyleTodd, Kyle V., and Ralph A. Tripp. 2019. "Human Norovirus: Experimental Models of Infection" Viruses 11, no. 2: 151. https://doi.org/10.3390/v11020151
APA StyleTodd, K. V., & Tripp, R. A. (2019). Human Norovirus: Experimental Models of Infection. Viruses, 11(2), 151. https://doi.org/10.3390/v11020151






