In Vitro Generation of Novel Functionalized Biomaterials for Use in Oral and Dental Regenerative Medicine Applications
Abstract
1. Introduction
2. Materials and Methods
2.1. Generation of Acellular Fibrin–Agarose Scaffolds (AFAS)
2.2. Generation of Non-Functionalized Fibrin–Agarose Oral Mucosa Stroma Substitutes (n-FAOM)
2.3. Generation of Functionalized Fibrin–Agarose Oral Mucosa Stroma Substitutes (F-FAOM)
2.4. Histological Analyses
2.5. Analysis of ECM Components by Histochemistry
2.6. Immunohistochemical Analysis
2.7. Statistical Analyses
3. Results
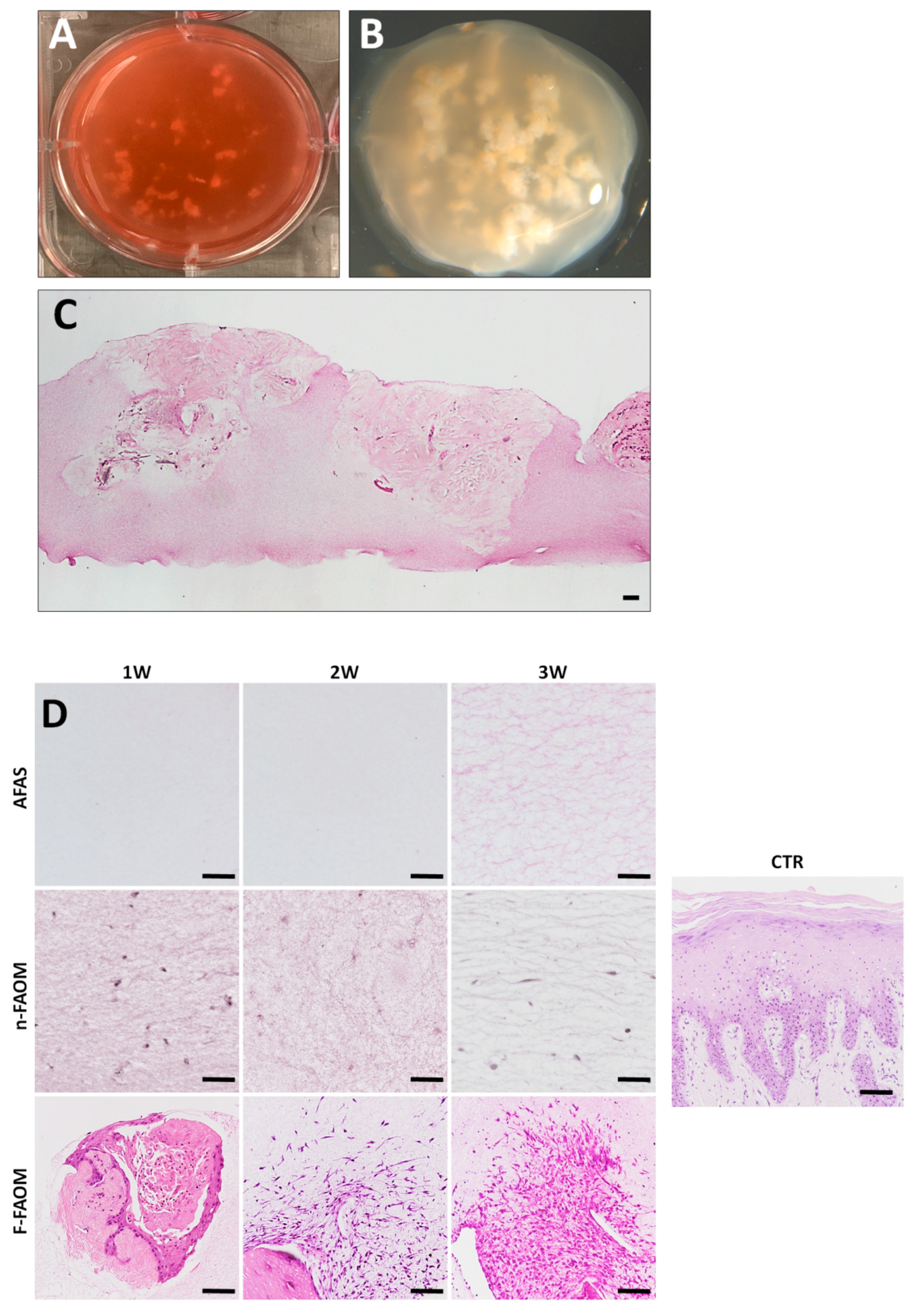
3.1. Histological Analysis of Functionalized and Non-Functionalized Fibrin–Agarose Oral Mucosa Stroma Substitutes
3.2. Cell Proliferation in the Fibrin–Agarose Biomaterial
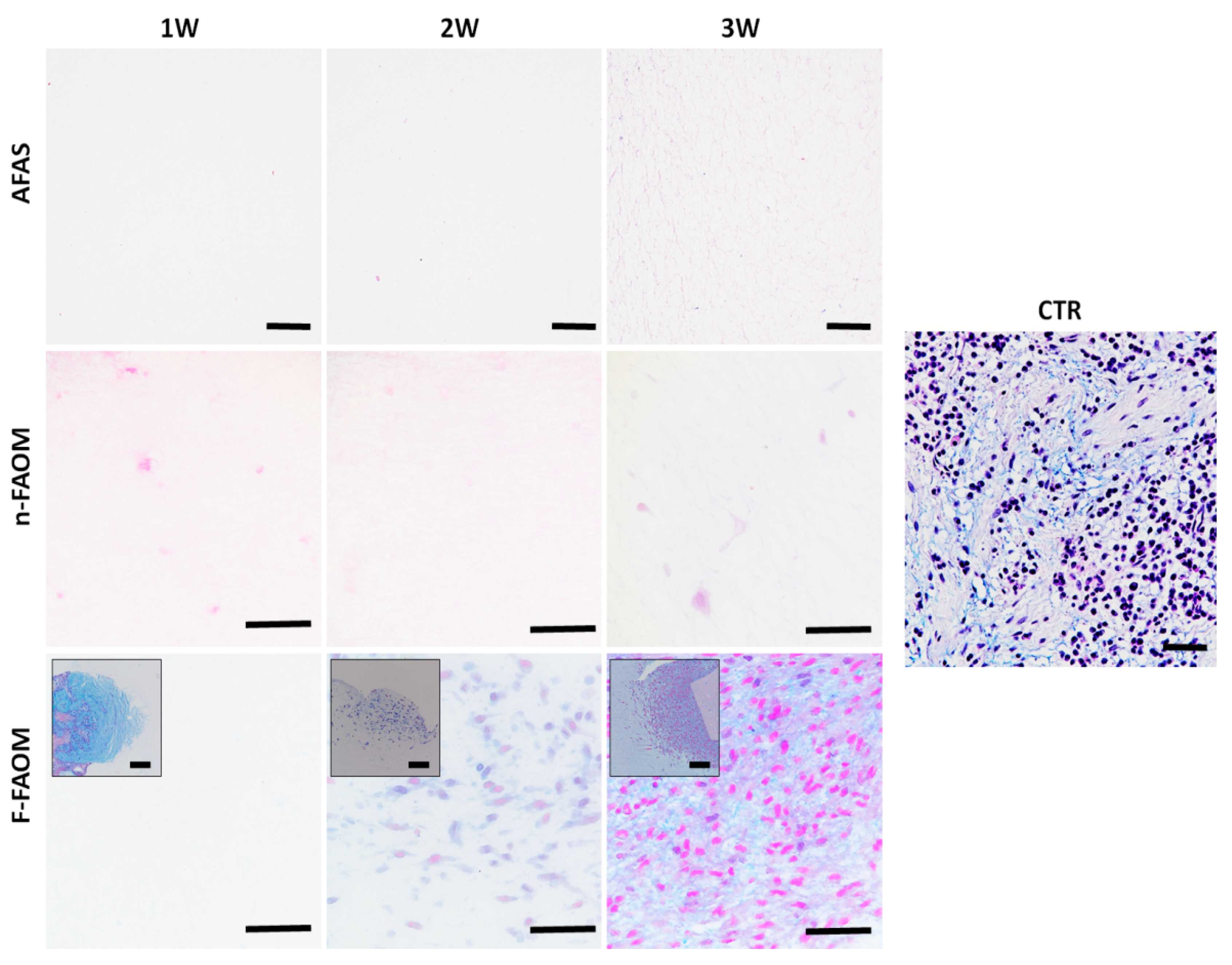
3.3. Development of Non-Fibrillar ECM Components in the Fibrin–Agarose Biomaterial
3.4. Development of Fibrillar ECM Components in the Fibrin–Agarose Biomaterial
4. Discussion
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Witten, C.M.; McFarland, R.D.; Simek, S.L. Concise Review: The US Food and Drug Administration and Regenerative Medicine. Stem Cells Transl. Med. 2015, 4, 1495–1499. [Google Scholar] [CrossRef] [PubMed]
- Fagogeni, I.; Metlerska, J.; Lipski, M.; Falgowski, T.; Maciej, G.; Nowicka, A. Materials used in regenerative endodontic procedures and their impact on tooth discoloration. J. Oral Sci. 2019, 61, 379–385. [Google Scholar] [CrossRef] [PubMed]
- Larsson, L.; Decker, A.M.; Nibali, L.; Pilipchuk, S.P.; Berglundh, T.; Giannobile, W.V. Regenerative Medicine for Periodontal and Peri-implant Diseases. J. Dent. Res. 2016, 95, 255–266. [Google Scholar] [CrossRef] [PubMed]
- Langer, R.; Vacanti, J.P. Tissue engineering. Science 1993, 260, 920–926. [Google Scholar] [CrossRef] [PubMed]
- Garzon, I.; Sanchez-Quevedo, M.C.; Moreu, G.; Gonzalez-Jaranay, M.; Gonzalez-Andrades, M.; Montalvo, A.; Campos, A.; Alaminos, M. In vitro and in vivo cytokeratin patterns of expression in bioengineered human periodontal mucosa. J. Periodontal Res. 2009, 44, 588–597. [Google Scholar] [CrossRef]
- Rana, D.; Ramasamy, K.; Leena, M.; Pasricha, R.; Manivasagam, G.; Ramalingam, M. Surface functionalization of biomaterials. In Biology and Engineering of Stem Cell Niches; Vishwakarma, A., Karp, J.M., Eds.; Academic Press: Boston, MA, USA, 2017; pp. 331–343. [Google Scholar]
- Taraballi, F.; Zanini, S.; Lupo, C.; Panseri, S.; Cunha, C.; Riccardi, C.; Marcacci, M.; Campione, M.; Cipolla, L. Amino and carboxyl plasma functionalization of collagen films for tissue engineering applications. J. Colloid Interface Sci. 2013, 394, 590–597. [Google Scholar] [CrossRef]
- Stadlinger, B.; Hintze, V.; Bierbaum, S.; Moller, S.; Schulz, M.C.; Mai, R.; Kuhlisch, E.; Heinemann, S.; Scharnweber, D.; Schnabelrauch, M.; et al. Biological functionalization of dental implants with collagen and glycosaminoglycans-A comparative study. J. Biomed. Mater. Res. B Appl. Biomater. 2012, 100, 331–341. [Google Scholar] [CrossRef]
- Sapudom, J.; Rubner, S.; Martin, S.; Thoenes, S.; Anderegg, U.; Pompe, T. The interplay of fibronectin functionalization and TGF-beta1 presence on fibroblast proliferation, differentiation and migration in 3D matrices. Biomater. Sci. 2015, 3, 1291–1301. [Google Scholar] [CrossRef]
- Koh, H.S.; Yong, T.; Chan, C.K.; Ramakrishna, S. Enhancement of neurite outgrowth using nano-structured scaffolds coupled with laminin. Biomaterials 2008, 29, 3574–3582. [Google Scholar] [CrossRef]
- Rosellini, E.; Cristallini, C.; Guerra, G.D.; Barbani, N. Surface chemical immobilization of bioactive peptides on synthetic polymers for cardiac tissue engineering. J. Biomater. Sci. Polym. Ed. 2015, 26, 515–533. [Google Scholar] [CrossRef]
- Rana, D.; Ramasamy, K.; Leena, M.; Jimenez, C.; Campos, J.; Ibarra, P.; Haidar, Z.S.; Ramalingam, M. Surface functionalization of nanobiomaterials for application in stem cell culture, tissue engineering, and regenerative medicine. Biotechnol Prog 2016, 32, 554–567. [Google Scholar] [CrossRef] [PubMed]
- Martin-Piedra, M.A.; Alaminos, M.; Fernandez-Valades-Gamez, R.; Espana-Lopez, A.; Liceras-Liceras, E.; Sanchez-Montesinos, I.; Martinez-Plaza, A.; Sanchez-Quevedo, M.C.; Fernandez-Valades, R.; Garzon, I. Development of a multilayered palate substitute in rabbits: A histochemical ex vivo and in vivo analysis. Histochem. Cell Biol. 2017, 147, 377–388. [Google Scholar] [CrossRef]
- Garzon, I.; Miyake, J.; Gonzalez-Andrades, M.; Carmona, R.; Carda, C.; Sanchez-Quevedo Mdel, C.; Campos, A.; Alaminos, M. Wharton’s jelly stem cells: A novel cell source for oral mucosa and skin epithelia regeneration. Stem Cells Transl Med 2013, 2, 625–632. [Google Scholar] [CrossRef] [PubMed]
- Garzon, I.; Martin-Piedra, M.A.; Alfonso-Rodriguez, C.; Gonzalez-Andrades, M.; Carriel, V.; Martinez-Gomez, C.; Campos, A.; Alaminos, M. Generation of a biomimetic human artificial cornea model using Wharton’s jelly mesenchymal stem cells. Investig. Ophthalmol. Vis. Sci. 2014, 55, 4073–4083. [Google Scholar] [CrossRef] [PubMed]
- Scionti, G.; Moral, M.; Toledano, M.; Osorio, R.; Duran, J.D.; Alaminos, M.; Campos, A.; Lopez-Lopez, M.T. Effect of the hydration on the biomechanical properties in a fibrin-agarose tissue-like model. J. Biomed. Mater. Res. A 2014, 102, 2573–2582. [Google Scholar] [CrossRef] [PubMed]
- Alfonso-Rodriguez, C.A.; Gonzalez-Andrades, E.; Jaimes-Parra, B.D.; Fernandez-Valades, R.; Campos, A.; Sanchez-Quevedo, M.C.; Alaminos, M.; Garzon, I. Ex vivo and in vivo modulatory effects of umbilical cord Wharton’s jelly stem cells on human oral mucosa stroma substitutes. Histol. Histopathol. 2015, 30, 1321–1332. [Google Scholar] [PubMed]
- Vinuela-Prieto, J.M.; Sanchez-Quevedo, M.C.; Alfonso-Rodriguez, C.A.; Oliveira, A.C.; Scionti, G.; Martin-Piedra, M.A.; Moreu, G.; Campos, A.; Alaminos, M.; Garzon, I. Sequential keratinocytic differentiation and maturation in a three-dimensional model of human artificial oral mucosa. J. Periodontal Res. 2015, 50, 658–665. [Google Scholar] [CrossRef]
- Oliveira, A.C.; Garzon, I.; Ionescu, A.M.; Carriel, V.; Cardona Jde, L.; Gonzalez-Andrades, M.; Perez Mdel, M.; Alaminos, M.; Campos, A. Evaluation of small intestine grafts decellularization methods for corneal tissue engineering. PLoS ONE 2013, 8, e66538. [Google Scholar] [CrossRef]
- Fernandez-Valades-Gamez, R.; Garzon, I.; Liceras-Liceras, E.; Espana-Lopez, A.; Carriel, V.; Martin-Piedra, M.A.; Munoz-Miguelsanz, M.A.; Sanchez-Quevedo, M.C.; Alaminos, M.; Fernandez-Valades, R. Usefulness of a bioengineered oral mucosa model for preventing palate bone alterations in rabbits with a mucoperiostial defect. Biomed. Mater. 2016, 11, 015015. [Google Scholar] [CrossRef]
- Martin-Piedra, M.A.; Garzon, I.; Gomez-Sotelo, A.; Garcia-Abril, E.; Jaimes-Parra, B.D.; Lopez-Cantarero, M.; Alaminos, M.; Campos, A. Generation and Evaluation of Novel Stromal Cell-Containing Tissue Engineered Artificial Stromas for the Surgical Repair of Abdominal Defects. Biotechnol. J. 2017, 12, 1700078. [Google Scholar] [CrossRef]
- Egea-Guerrero, J.J.; Carmona, G.; Correa, E.; Mata, R.; Arias-Santiago, S.; Alaminos, M.; Gacto, P.; Cuende, N. Transplant of Tissue-Engineered Artificial Autologous Human Skin in Andalusia: An Example of Coordination and Institutional Collaboration. Transpl. Proc. 2019, 51, 3047–3050. [Google Scholar] [CrossRef] [PubMed]
- Gonzalez-Andrades, M.; Mata, R.; Gonzalez-Gallardo, M.D.C.; Medialdea, S.; Arias-Santiago, S.; Martinez-Atienza, J.; Ruiz-Garcia, A.; Perez-Fajardo, L.; Lizana-Moreno, A.; Garzon, I.; et al. A study protocol for a multicentre randomised clinical trial evaluating the safety and feasibility of a bioengineered human allogeneic nanostructured anterior cornea in patients with advanced corneal trophic ulcers refractory to conventional treatment. BMJ Open 2017, 7, e016487. [Google Scholar] [CrossRef] [PubMed]
- Moussa, D.G.; Aparicio, C. Present and future of tissue engineering scaffolds for dentin-pulp complex regeneration. J. Tissue Eng. Regen. Med. 2019, 13, 58–75. [Google Scholar] [CrossRef] [PubMed]
- Kasai, Y.; Takagi, R.; Kobayashi, S.; Owaki, T.; Yamaguchi, N.; Fukuda, H.; Sakai, Y.; Sumita, Y.; Kanai, N.; Isomoto, H.; et al. A stable protocol for the fabrication of transplantable human oral mucosal epithelial cell sheets for clinical application. Regen. Ther. 2020, 14, 87–94. [Google Scholar] [CrossRef]
- Heathman, T.R.; Glyn, V.A.; Picken, A.; Rafiq, Q.A.; Coopman, K.; Nienow, A.W.; Kara, B.; Hewitt, C.J. Expansion, harvest and cryopreservation of human mesenchymal stem cells in a serum-free microcarrier process. Biotechnol. Bioeng. 2015, 112, 1696–1707. [Google Scholar] [CrossRef]
- Costa, A.; Naranjo, J.D.; Londono, R.; Badylak, S.F. Biologic Scaffolds. Cold Spring Harb. Perspect. Med. 2017, 7, a025676. [Google Scholar] [CrossRef]
- Halper, J.; Kjaer, M. Basic components of connective tissues and extracellular matrix: Elastin, fibrillin, fibulins, fibrinogen, fibronectin, laminin, tenascins and thrombospondins. Adv. Exp. Med. Biol. 2014, 802, 31–47. [Google Scholar]
- Aviezer, D.; Levy, E.; Safran, M.; Svahn, C.; Buddecke, E.; Schmidt, A.; David, G.; Vlodavsky, I.; Yayon, A. Differential structural requirements of heparin and heparan sulfate proteoglycans that promote binding of basic fibroblast growth factor to its receptor. J. Biol. Chem. 1994, 269, 114–121. [Google Scholar]
- Browning, K.N. Extracellular matrix proteins in the gastrointestinal tract: More than a supporting role. J. Physiol. 2018, 596, 3831–3832. [Google Scholar] [CrossRef]
- Gandolfi, M.G.; Gardin, C.; Zamparini, F.; Ferroni, L.; Esposti, M.D.; Parchi, G.; Ercan, B.; Manzoli, L.; Fava, F.; Fabbri, P.; et al. Mineral-Doped Poly(L-lactide) Acid Scaffolds Enriched with Exosomes Improve Osteogenic Commitment of Human Adipose-Derived Mesenchymal Stem Cells. Nanomaterials 2020, 10, 432. [Google Scholar] [CrossRef]
- Kubo, K. Effects of static stretching on mechanical properties and collagen fiber orientation of the Achilles tendon in vivo. Clin. Biomech. 2018, 60, 115–120. [Google Scholar] [CrossRef] [PubMed]
- Osorio, R.; Alfonso-Rodriguez, C.A.; Osorio, E.; Medina-Castillo, A.L.; Alaminos, M.; Toledano-Osorio, M.; Toledano, M. Novel potential scaffold for periodontal tissue engineering. Clin. Oral Investig. 2017, 21, 2695–2707. [Google Scholar] [CrossRef] [PubMed]




| Sample | Alcian Blue | PAS | Picrosirius Red | Type-I Collagen | |
|---|---|---|---|---|---|
| Control oral mucosa | CTR | 100 ± 26.01 | 100 ± 27.38 | 100 ± 42.28 | 100 ± 39.4 |
| Global groups | AFAS | 23 ± 1.35 | 16.34 ± 1.94 | 12.11 ± 6.04 | 22.05 ± 1.45 |
| n-FAOM | 21.22 ± 2.72 | 19.84 ± 10.42 | 19.66 ± 11.06 | 30.93 ± 5.85 | |
| F-FAOM | 41.79 ± 13.44 | 54.51 ± 23.97 | 55.79 ± 31.03 | 36.16 ± 17.33 | |
| Specific samples | AFAS-1W | 22.87 ± 1.1 | 15.61 ± 0.79 | 6.04 ± 0.71 | 22.03 ± 0.48 |
| AFAS-2W | 22.7 ± 1.14 | 16.71 ± 2 | 14.83 ± 2.76 | 22.11 ± 1.71 | |
| AFAS-3W | 23.4 ± 1.81 | 16.71 ± 2.63 | 15.47 ± 3.82 | 22.03 ± 1.89 | |
| n-FAOM-1W | 17.91 ± 1.2 | 21.1 ± 10.71 | 11.68 ± 8.1 | 28.64 ± 4.18 | |
| n-FAOM-2W | 18.97 ± 1.7 | 22.32 ± 5.21 | 20.95 ± 10.48 | 30.99 ± 4.19 | |
| n-FAOM-3W | 26.77 ± 1.73 | 16.1 ± 13.85 | 26.35 ± 5.54 | 33.17 ± 7.69 | |
| F-FAOM-1W | 17.55 ± 0.74 | 21.1 ± 10.04 | 29.81 ± 6.41 | 21.86 ± 4.23 | |
| F-FAOM-2W | 39.72 ± 4.4 | 55.61 ± 10.63 | 51.57 ± 9.26 | 34.17 ± 12.36 | |
| F-FAOM-3W | 68.09 ± 10.42 | 86.83 ± 4.64 | 85.98 ± 15.2 | 52.43 ± 6.9 | |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Blanco-Elices, C.; España-Guerrero, E.; Mateu-Sanz, M.; Sánchez-Porras, D.; García-García, Ó.D.; Sánchez-Quevedo, M.d.C.; Fernández-Valadés, R.; Alaminos, M.; Martín-Piedra, M.Á.; Garzón, I. In Vitro Generation of Novel Functionalized Biomaterials for Use in Oral and Dental Regenerative Medicine Applications. Materials 2020, 13, 1692. https://doi.org/10.3390/ma13071692
Blanco-Elices C, España-Guerrero E, Mateu-Sanz M, Sánchez-Porras D, García-García ÓD, Sánchez-Quevedo MdC, Fernández-Valadés R, Alaminos M, Martín-Piedra MÁ, Garzón I. In Vitro Generation of Novel Functionalized Biomaterials for Use in Oral and Dental Regenerative Medicine Applications. Materials. 2020; 13(7):1692. https://doi.org/10.3390/ma13071692
Chicago/Turabian StyleBlanco-Elices, Cristina, Enrique España-Guerrero, Miguel Mateu-Sanz, David Sánchez-Porras, Óscar Darío García-García, María del Carmen Sánchez-Quevedo, Ricardo Fernández-Valadés, Miguel Alaminos, Miguel Ángel Martín-Piedra, and Ingrid Garzón. 2020. "In Vitro Generation of Novel Functionalized Biomaterials for Use in Oral and Dental Regenerative Medicine Applications" Materials 13, no. 7: 1692. https://doi.org/10.3390/ma13071692
APA StyleBlanco-Elices, C., España-Guerrero, E., Mateu-Sanz, M., Sánchez-Porras, D., García-García, Ó. D., Sánchez-Quevedo, M. d. C., Fernández-Valadés, R., Alaminos, M., Martín-Piedra, M. Á., & Garzón, I. (2020). In Vitro Generation of Novel Functionalized Biomaterials for Use in Oral and Dental Regenerative Medicine Applications. Materials, 13(7), 1692. https://doi.org/10.3390/ma13071692





