Effects of Fluoride on Two Chemical Models of Enamel Demineralization
Abstract
1. Introduction
2. Results
3. Discussion
4. Materials and Methods
4.1. Preparation of Enamel Blocks
4.2. Assessment of Enamel Demineralization
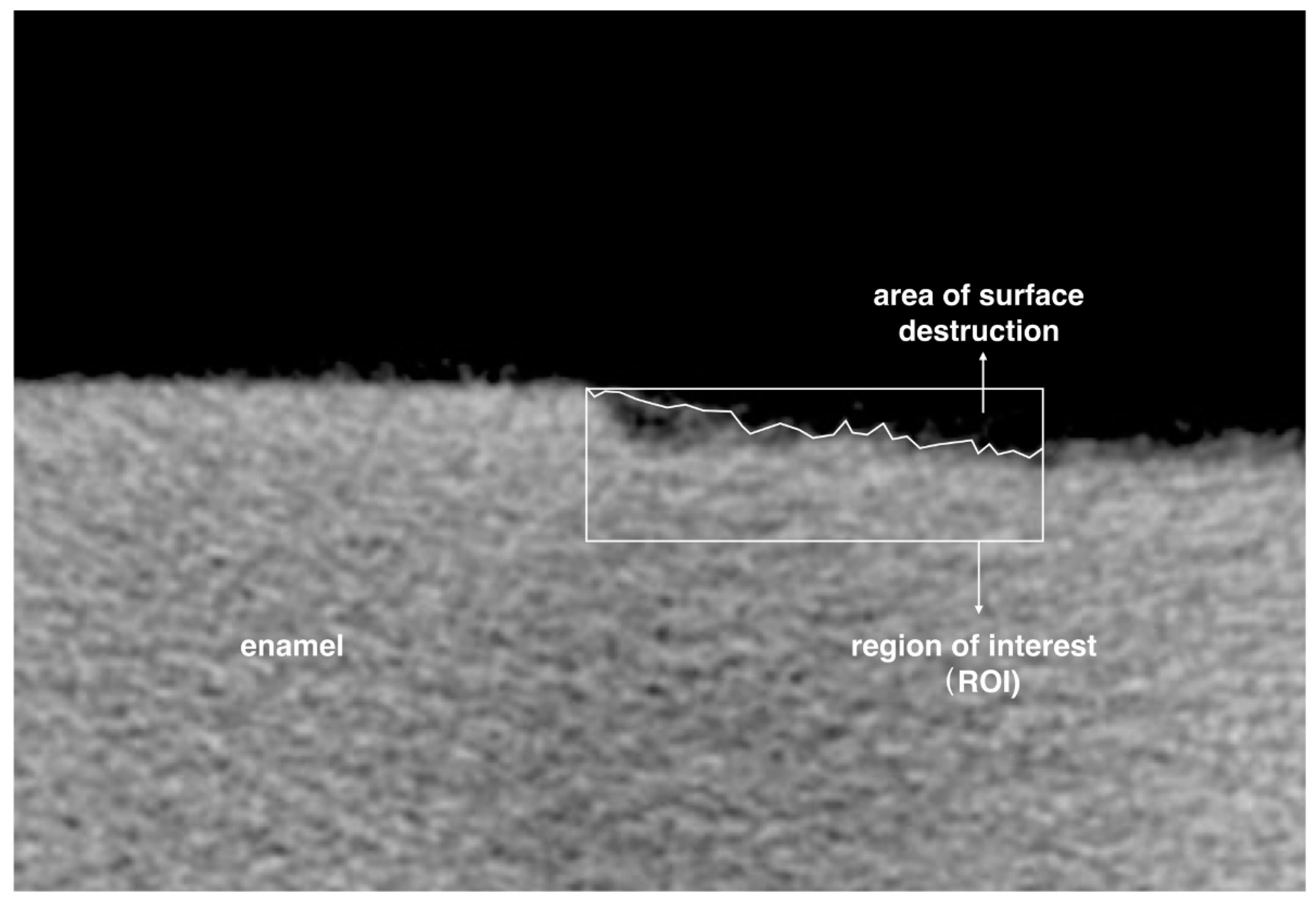
4.2.1. Lesion Depth, Mineral Loss and Surface Destruction
4.2.2. Elemental Analysis
4.2.3. Surface Micro-Hardness
4.2.4. Statistical Analysis
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| SDP | surface destruction percentage |
| CaCl2 | calcium chloride |
| KH2PO4 | potassium dihydrogen phosphate |
| NaN3 | sodium azide |
| TEMDP | tetraethyl methyl diphosphonate |
| NaF | sodium fluoride |
| F | fluoride |
| Micro-CT | micro-computed tomography |
| MDV | mineral density value |
| ROI | region of interest |
| SEM | scanning electron microscopy |
| EDS | energy-dispersive X-ray spectroscopy |
| KHN | Knoop hardness number |
References
- West, N.X.; Joiner, A. Enamel mineral loss. J. Dent. 2014, 42, S2–S11. [Google Scholar] [CrossRef]
- Buzalaf, M.A.; Pessan, J.P.; Honorio, H.M.; ten Cate, J.M. Mechanisms of action of fluoride for caries control. Monogr. Oral Sci. 2011, 22, 97–114. [Google Scholar] [PubMed]
- Yu, O.Y.; Zhao, I.S.; Mei, M.L.; Lo, E.C.-M.; Chu, C.-H. A review of the common models used in mechanistic studies on demineralization-remineralization for cariology research. Dent. J. 2017, 5, 20. [Google Scholar] [CrossRef]
- Xuelian, H.; Qiang, G.; Biao, R.; Yuqing, L.; Xuedong, Z. Models in caries research. In Dental Caries; Springer: Berlin, Germany, 2016; pp. 157–173. [Google Scholar]
- Marquezan, M.; Correa, F.N.P.; Sanabe, M.E.; Rodrigues, L.E.; Hebling, J.; Guedes-Pinto, A.C.; Mendes, F.M. Artificial methods of dentine caries induction: A hardness and morphological comparative study. Arch. Oral Biol. 2009, 54, 1111–1117. [Google Scholar] [CrossRef] [PubMed]
- Schwendicke, F.; Eggers, K.; Meyer-Lueckel, H.; Dorfer, C.; Kovalev, A.; Gorb, S.; Paris, S. In vitro induction of residual caries lesions in dentin: Comparative mineral loss and nano-hardness analysis. Caries Res. 2015, 49, 259–265. [Google Scholar] [CrossRef] [PubMed]
- Ten Cate, J.; Larsen, M.J.; Pearce, E.; Fejerskov, O. Chemical interactions between the tooth and oral fluids. In Dental Caries. The Disease and Its Clinical Management; Blackwell Publishing Ltd.: Oxford, UK, 2008; pp. 209–231. [Google Scholar]
- Cury, J.; Tenuta, L. How to maintain a cariostatic fluoride concentration in the oral environment. Adv. Dent. Res. 2008, 20, 13–16. [Google Scholar] [CrossRef] [PubMed]
- Hicks, M.J.; Flaitz, C.M. Enamel caries formation and lesion progression with a fluoride dentifrice and a calcium-phosphate containing fluoride dentifrice: A polarized light microscopic study. ASDC J. Dent. Child. 2000, 67, 21–28. [Google Scholar] [PubMed]
- Queiroz, C.S.; Hara, A.T.; Paes Leme, A.F.; Cury, J.A. Ph-cycling models to evaluate the effect of low fluoride dentifrice on enamel de- and remineralization. Braz. Dent. J. 2008, 19, 21–27. [Google Scholar] [CrossRef] [PubMed]
- Lippert, F.; Juthani, K. Fluoride dose-response of human and bovine enamel artificial caries lesions under ph-cycling conditions. Clin. Oral Investig. 2015, 19, 1947–1954. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Lv, X.P.; Shi, W.; Li, J.Y.; Li, D.X.; Zhou, X.D.; Zhang, L.L. 8DSS-promoted remineralization of initial enamel caries in vitro. J. Dent. Res. 2014, 93, 520–524. [Google Scholar] [CrossRef] [PubMed]
- Kiranmayi, M.; Nirmala, S.; Nuvvula, S. Appraisal of the remineralizing potential of child formula dentifrices on primary teeth: An in vitro ph cycling model. Contemp. Clin. Dent. 2015, 6, S81. [Google Scholar] [PubMed]
- Chien, Y.C.; Burwell, A.K.; Saeki, K.; Fernandez-Martinez, A.; Pugach, M.K.; Nonomura, G.; Habelitz, S.; Ho, S.P.; Rapozo-Hilo, M.; Featherstone, J.D.; et al. Distinct decalcification process of dentin by different cariogenic organic acids: Kinetics, ultrastructure and mechanical properties. Arch. Oral Biol. 2016, 63, 93–105. [Google Scholar] [CrossRef] [PubMed]
- Buskes, J.A.K.M.; Christoffersen, J.; Arends, J. Lesion formation and lesion remineralization in enamel under constant composition conditions—A new technique with applications. Caries Res. 1985, 19, 490–496. [Google Scholar] [CrossRef] [PubMed]
- Moron, B.M.; Comar, L.P.; Wiegand, A.; Buchalla, W.; Yu, H.; Buzalaf, M.A.R.; Magalhaes, A.C. Different protocols to produce artificial dentine carious lesions in vitro and in situ: Hardness and mineral content correlation. Caries Res. 2013, 47, 162–170. [Google Scholar] [CrossRef] [PubMed]
- Buchalla, W. Histological and clinical appearance of caries. In Caries Management—Science and Clinical Practice, 1st ed.; Hendrik, M.-L.P., Sebastian, P., Susanne, E., Ekstrand, K.R., Eds.; Thieme: New York, NY, USA, 2013; pp. 39–63. [Google Scholar]
- Skucha-Nowak, M.; Gibas, M.; Tanasiewicz, M.; Twardawa, H.; Szklarski, T. Natural and controlled demineralization for study purposes in minimally invasive dentistry. Adv. Clin. Exp. Med. 2015, 24, 891–898. [Google Scholar] [CrossRef] [PubMed]
- Ten Cate, J.M. Contemporary perspective on the use of fluoride products in caries prevention. Br. Dent. J. 2013, 214, 161–167. [Google Scholar] [CrossRef] [PubMed]
- Arends, J.; Christoffersen, J. The nature of early caries lesions in enamel. J. Dent. Res. 1986, 65, 2–11. [Google Scholar] [CrossRef] [PubMed]
- Banerjee, A. Minimal intervention dentistry: Part 7. Minimally invasive operative caries management: Rationale and techniques. Br. Dent. J. 2013, 214, 107–111. [Google Scholar] [CrossRef] [PubMed]
- Magalhaes, A.C.; Moron, B.M.; Comar, L.P.; Wiegand, A.; Buchalla, W.; Buzalaf, M.A.R. Comparison of cross-sectional hardness and transverse microradiography of artificial carious enamel lesions induced by different demineralising solutions and gels. Caries Res. 2009, 43, 474–483. [Google Scholar] [CrossRef] [PubMed]
- Noronha Mdos, S.; Romao, D.A.; Cury, J.A.; Tabchoury, C.P. Effect of fluoride concentration on reduction of enamel demineralization according to the cariogenic challenge. Braz. Dent. J. 2016, 27, 393–398. [Google Scholar] [CrossRef] [PubMed]
- Haghgou, H.R.; Haghgoo, R.; Asdollah, F.M. Comparison of the microhardness of primary and permanent teeth after immersion in two types of carbonated beverages. J. Int. Soc. Prev. Community Dent. 2016, 6, 344–348. [Google Scholar] [CrossRef] [PubMed]
- Sfondrini, M.F.; Scribante, A.; Cacciafesta, V.; Gandini, P. Shear bond strength of deciduous and permanent bovine enamel. J. Adhes. Dent. 2011, 13, 227–230. [Google Scholar] [PubMed]
- Scribante, A.; Contreras-Bulnes, R.; Montasser, M.A.; Vallittu, P.K. Orthodontics: Bracket materials, adhesives systems, and their bond strength. BioMed Res. Int. 2016, 2016, 1329814. [Google Scholar] [CrossRef] [PubMed]
- Correr, G.M.; Alonso, R.C.; Consani, S.; Puppin-Rontani, R.M.; Ferracane, J.L. In vitro wear of primary and permanent enamel. Simultaneous erosion and abrasion. Am. J. Dent. 2007, 20, 394–399. [Google Scholar] [PubMed]
- Borges, A.F.S.; Puppin-Rontani, R.M.; Bittar, R.A.; Kantowitz, K.R.; Pascon, F.M.; Martin, A.A. Effects of acidic primer/adhesives on primary and permanent dentin. Am. J. Dent. 2009, 22, 30–36. [Google Scholar] [PubMed]
- ten Cate, J.M.; Duijsters, P.P. Alternating demineralization and remineralization of artificial enamel lesions. Caries Res. 1982, 16, 201–210. [Google Scholar] [CrossRef] [PubMed]
- Liu, B.Y.; Lo, E.C.M.; Li, C.M.T. Effect of silver and fluoride ions on enamel demineralization: A quantitative study using micro-computed tomography. Aust. Dent. J. 2012, 57, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Hamba, H.; Nikaido, T.; Sadr, A.; Nakashima, S.; Tagami, J. Enamel lesion parameter correlations between polychromatic micro-ct and tmr. J. Dent. Res. 2012, 91, 586–591. [Google Scholar] [CrossRef] [PubMed]
- Chu, C.H.; Lo, E.C.M. Microhardness of dentine in primary teeth after topical fluoride applications. J. Dent. 2008, 36, 387–391. [Google Scholar] [CrossRef] [PubMed]


| Enamel Demineralization | Acetate Buffer | Lactate Buffer | Acetate Buffer with Fluoride | Lactate Buffer with Fluoride | p-Value Bonferroni Test |
|---|---|---|---|---|---|
| Lesion depth (μm) | 134.1 ± 27.2 a | 96.1 ± 16.5 b | 97.5 ± 22.4 b | 91.1 ± 16.2 c | <0.001 a > b > c |
| Mineral loss (g·cm−3) | 1.18 ± 0.21 a | 1.13 ± 0.27 a | 0.87 ± 0.29 b | 1.06 ± 0.22 a | <0.001 a > b |
| Surface destruction (%) | 7.8 ± 8.93 a | 0.71 ± 1.6 b | 0.36 ± 1.70 b | 1.36 ± 2.94 b | <0.001 a > b |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yu, O.Y.; Mei, M.L.; Zhao, I.S.; Lo, E.C.-M.; Chu, C.-H. Effects of Fluoride on Two Chemical Models of Enamel Demineralization. Materials 2017, 10, 1245. https://doi.org/10.3390/ma10111245
Yu OY, Mei ML, Zhao IS, Lo EC-M, Chu C-H. Effects of Fluoride on Two Chemical Models of Enamel Demineralization. Materials. 2017; 10(11):1245. https://doi.org/10.3390/ma10111245
Chicago/Turabian StyleYu, Ollie Yiru, May Lei Mei, Irene Shuping Zhao, Edward Chin-Man Lo, and Chun-Hung Chu. 2017. "Effects of Fluoride on Two Chemical Models of Enamel Demineralization" Materials 10, no. 11: 1245. https://doi.org/10.3390/ma10111245
APA StyleYu, O. Y., Mei, M. L., Zhao, I. S., Lo, E. C.-M., & Chu, C.-H. (2017). Effects of Fluoride on Two Chemical Models of Enamel Demineralization. Materials, 10(11), 1245. https://doi.org/10.3390/ma10111245






