Application of Machine Learning in Predicting Perioperative Outcomes in Patients with Cancer: A Narrative Review for Clinicians
Abstract
1. Introduction
2. Methods
Search Strategy and Source Selection
3. Understanding the Data
4. ML Application in the Perioperative Continuum
4.1. Understanding Machine Learning
4.2. Supervised Machine Learning
4.3. Forms of Supervised Machine Learning
5. Classification Models: Logistic Regression, Classification (Decision) Tree
6. Confusion Matrix
Classification (Decision) Trees
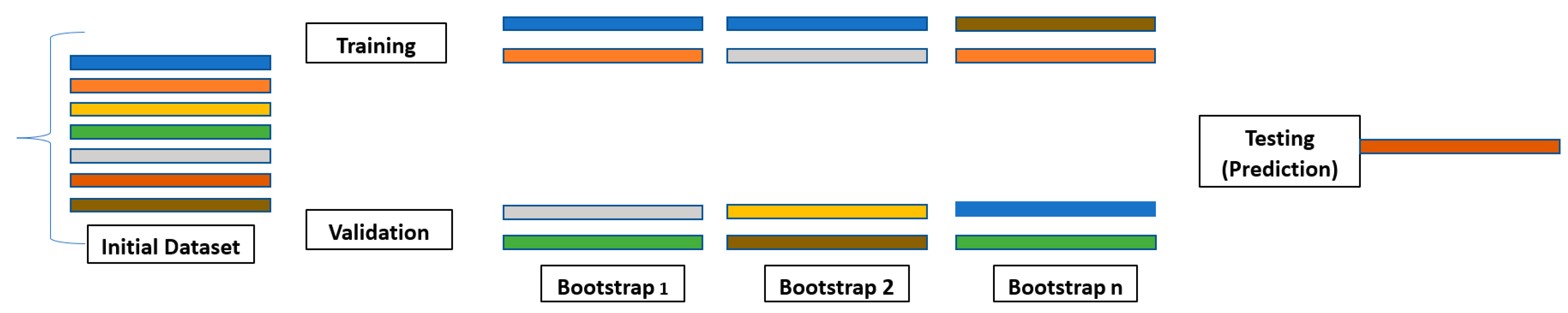
7. Bootstrapping in Machine Learning [16,18]
7.1. Ensemble Techniques: Bagging, Random Forest, and Boosting
7.2. Supervised Learning Limitations
8. Neural Networks
9. Discussion
9.1. Application to the Perioperative Setting (Key Finding)
9.2. Limitations
9.3. Future Research
10. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ozaydin, B.; Berner, E.; Cimono, J. Appropriate use of machine learning in healthcare. Intell. Based Med. 2021, 5, 100041. [Google Scholar] [CrossRef]
- Bellini, V.; Valente, M.; Bertorelli, G.; Pifferi, B.; Craca, M.; Mordonini, M.; Lombardo, G.; Bottani, E.; Del Rio, P.; Bignami, E. Machine learning in perioperative medicine: A systematic review. J. Anesth. Analg. Crit. Care 2022, 2, 2. [Google Scholar] [CrossRef] [PubMed]
- Chelazzi, C.; Villa, G.; Manno, A.; Ranfagni, V.; Gemmi, E.; Romagnoli, S. The new SUMPOT to predict postoperative complications using an artificial neural network. Sci. Rep. 2021, 11, 22692. [Google Scholar] [CrossRef]
- Morris, M.X.; Rajesh, A.; Asaad, M.; Hassan, A.; Saadoun, R.; Butler, C.E. Deep learning applications in surgery: Current uses and future directions. Am. Surg. 2023, 89, 36–42. [Google Scholar] [CrossRef] [PubMed]
- James, G.; Witten, D.; Hastie, T.; Tibshirani, R.; Taylor, J. An Introduction to Statistical Learning with Applications in Python, 1st ed.; Springer International Publishing: Cham, Switzerland, 2023. [Google Scholar] [CrossRef]
- Minsky, M.; Papert, S. Perceptrons: An Introduction to Computational Geometry; MIT Press: Cambridge, MA, USA, 1969. [Google Scholar]
- Rosenblatt, Frank. Final Summary Report on Contract Nonr 401-40 Cognitive Systems Research Program. Cornell University. 1971. Available online: https://web.archive.org/web/20231109035045/https://apps.dtic.mil/sti/pdfs/AD0720416.pdf (accessed on 17 February 2024).
- Rothman, D. Artificial Intelligence by Example: Acquire Advanced AI, Machine Learning, and Deep Learning Design Skills, 2nd ed.; Packt Publishing: Birmingham, UK, 2020; pp. 1–119. [Google Scholar]
- Capre Capretti, G.; Bonifacio, C.; De Palma, C.; Nebbia, M.; Giannitto, C.; Cancian, P.; Laino, M.E.; Balzarini, L.; Papanikolaou, N.; Savevski, V.; et al. A machine learning risk model based on preoperative computed tomography scan to predict postoperative outcomes after pancreatoduodenectomy. Updates Surg. 2022, 74, 235–243. [Google Scholar] [CrossRef]
- Fernandes, M.P.B.; Armengol de la Hoz, M.; Rangasamy, V.; Subramaniam, B. Machine learning models with preoperative risk factors and intraoperative hypotension parameters predict mortality after cardiac surgery. J. Cardiothorac. Vasc. Anesth. 2021, 35, 857–865. [Google Scholar] [CrossRef] [PubMed]
- Zhang, H.; Wang, A.Y.; Wu, S.; Ngo, J.; Feng, Y.; He, X.; Zhang, Y.; Wu, X.; Hong, D. Artificial intelligence for the prediction of acute kidney injury during the perioperative period: Systematic review and meta-analysis of diagnostic test accuracy. BMC Nephrol. 2022, 23, 405. [Google Scholar] [CrossRef] [PubMed]
- Stiglic, G.; Kocbek, P.; Fijacko, N.; Zitnik, M.; Verbert, K.; Cilar, L. Interpretability of machine learning-based prediction models in healthcare. Wiley Interdiscip. Rev. Data Min. Knowl. Discov. 2020, 10, 1–13. [Google Scholar] [CrossRef]
- Bishara, A.; Wong, A.; Wang, L.; Chopra, M.; Fan, W.; Lin, A.; Fong, N.; Palacharla, A.; Spinner, J.; Armstrong, R.; et al. Opal: An implementation science tool for machine learning clinical decision support in anesthesia. J. Clin. Monit. Comput. 2022, 36, 1367–1377. [Google Scholar] [CrossRef]
- Javaid, M.; Haleem, A.; Pratap Singh, R.; Suman, R.; Rab, S. Significance of machine learning in healthcare: Features, pillars and applications. Int. J. Intell. Netw. 2022, 3, 58–73. [Google Scholar] [CrossRef]
- Bhardwaj, A. Promise and provisos of artificial intelligence and machine learning in healthcare. J. Health Leadersh. 2022, 14, 113–118. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Zhang, H.; Fan, Y.; Ying, P.; Li, J.; Xie, C.; Zhao, T. Propofol anesthesia depth monitoring based on self-attention and residual structure convolutional neural network. Comput. Math. Methods Med. 2022, 2022, 8501948. [Google Scholar] [CrossRef] [PubMed]
- Bishara, A.; Chiu, C.; Whitlock, E.L.; Douglas, V.C.; Lee, S.; Butte, A.J.; Leung, J.M.; Donovan, A.L. Postoperative delirium prediction using machine learning models and preoperative electronic health record data. BMC Anesth. 2022, 22, 8. [Google Scholar] [CrossRef] [PubMed]
- Kitcharanant, N.; Chotiyarnwong, P.; Tanphiriyakun, T.; Vanitcharoenkul, E.; Mahaisavariya, C.; Boonyaprapa, W.; Unnanuntana, A. Development and internal validation of a machine-learning-developed model for predicting 1-year mortality after fragility hip fracture. BMC Geriatr. 2022, 22, 451. [Google Scholar] [CrossRef] [PubMed]
- Feng, C.H.; Disis, M.L.; Cheng, C.; Zhang, L. Multimetric feature selection for analyzing multicategory outcomes of colorectal cancer: Random forest and multinomial logistic regression models. Lab. Investig. 2022, 102, 236–244. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Déniz, E.; Calderin-Ojeda, E.; Gomez, H. Asymmetric versus symmetric binary regression: A new proposal with applications. Symmetry 2022, 14, 733. [Google Scholar] [CrossRef]
- Fergus, P.; Chalmers, C. Applied Deep Learning: Tools, Techniques, and Implementation; Springer: Cham, Switzerland, 2022; pp. 1–170. [Google Scholar]
- Koprinska, I.; Kamp, M.; Appice, A.; Loglisci, C.; Antonie, L.; Zimmermann, A.; Guidotti, R.; Özgöbek, Ö.; Ribeiro, R.P.; Gavaldà, R. Interpretable Machine Learning—A Brief History, State-of-the-Art and Challenges. In ECML PKDD 2020 Workshops; Springer International Publishing AG: Cham, Switzerland, 2021; Volume 1323, pp. 417–431. [Google Scholar] [CrossRef]
- El Khouli, R.H.; Macura, K.J.; Barker, P.B.; Habba, M.R.; Jacobs, M.A.; Bluemke, D.A. Relationship of temporal resolution to diagnostic performance for dynamic contrast enhanced MRI of the breast. J. Magn. Reson. Imaging 2009, 30, 999–1004. [Google Scholar] [CrossRef] [PubMed]
- Hanczar, B.; Hua, J.; Sima, C.; Weinstein, J.; Bittner, M.; Dougherty, E.R. Small-sample precision of ROC-related estimates. Bioinformatics 2010, 26, 822–830. [Google Scholar] [CrossRef] [PubMed]
- Jena, O.P.; Bhushan, B.; Rakesh, N.; Astya, P.N.; Farhaoui, Y. Machine Learning and Deep Learning in Efficacy Improvement of Healthcare Systems; CRC Press: Boca Raton, FL, USA, 2022; pp. 1–372. [Google Scholar]
- Yun, K.; Oh, J.; Hong, T.H.; Kim, E.Y. Prediction of mortality in surgical intensive care unit patients using machine learning algorithms. Front. Med. 2021, 8, 621861. [Google Scholar] [CrossRef]
- Muslim, M.A.; Herowati, A.J.; Sugiharti, E.; Prasetiyo, B. Application of the pessimistic pruning to increase the accuracy of C4.5 algorithm in diagnosing chronic kidney disease. J. Phys. Conf. Ser. 2018, 983, 12062. [Google Scholar] [CrossRef]
- Bloch, D.A.; Olshen, R.A.; Walker, M.G. Risk Estimation for Classification Trees. J. Comput. Graph. Stat. 2002, 11, 263–288. [Google Scholar] [CrossRef]
- Kleiner, A.; Talwalkar, A.; Sarkar, P.; Jordan, M.I. A scalable bootstrap for massive data. J. R. Stat. Soc. Ser. B Stat. Methodol. 2014, 76, 795–816. [Google Scholar] [CrossRef]
- Kang, H.; Lee, B.; Jo, J.H.; Lee, H.S.; Park, J.Y.; Bang, S.; Park, S.W.; Song, S.Y.; Park, J.; Shim, H.; et al. Machine-learning model for the prediction of hypoxaemia during endoscopic retrograde cholangiopancreatography under monitored anaesthesia care. Yonsei Med. J. 2023, 64, 25–34. [Google Scholar] [CrossRef] [PubMed]
- Gabriel, R.A.; Harjai, B.; Prasad, R.S.; Simpson, S.; Chu, I.; Fisch, K.M.; Said, E.T. Machine learning approach to predicting persistent opioid use following lower extremity joint arthroplasty. Reg. Anesth. Pain Med. 2022, 47, 313–319. [Google Scholar] [CrossRef]
- Gabriel, R.A.; Harjai, B.; Simpson, S.; Goldhaber, N.; Curran, B.P.; Waterman, R.S. Machine learning-based models predicting outpatient surgery end time and recovery room discharge at an ambulatory surgery center. Anesth. Analg. 2022, 135, 159–169. [Google Scholar] [CrossRef]
- Yang, S.; Li, H.; Lin, Z.; Song, Y.; Lin, C.; Zhou, T. Quantitative analysis of anesthesia recovery time by machine learning prediction models. Mathematics 2022, 10, 2772. [Google Scholar] [CrossRef]
- Trindade, P.H.E.; Mello, J.F.S.R.D.; Silva, N.E.O.F.; Luna, S.P.L. Improving ovine behavioral pain diagnosis by implementing statistical weightings based on logistic regression and random forest algorithms. Animal 2022, 12, 940. [Google Scholar] [CrossRef]
- Shim, J.-G.; Ryu, K.-H.; Cho, E.-A.; Ahn, J.H.; Cha, Y.B.; Lim, G.; Lee, S.H. Machine learning for prediction of postoperative nausea and vomiting in patients with intravenous patient-controlled analgesia. PLoS ONE 2022, 17, e0277957. [Google Scholar] [CrossRef] [PubMed]
- Miyaguchi, N.; Takeuchi, K.; Kashima, H.; Morita, M.; Morimatsu, H. Predicting anesthetic infusion events using machine learning. Sci. Rep. 2021, 11, 23648. [Google Scholar] [CrossRef]
- Kim, J.H.; Kim, H.; Jang, J.S.; Hwang, S.M.; Lim, S.Y.; Lee, J.J.; Kwon, Y.S. Development and validation of a difficult laryngoscopy prediction model using machine learning of neck circumference and thyromental height. BMC Anesth. 2021, 21, 125. [Google Scholar] [CrossRef]
- Ward, A.; Jani, T.; De Souza, E.; Scheinker, D.; Bambos, N.; Anderson, T.A. Prediction of prolonged opioid use after surgery in adolescents: Insights from machine learning. Anesth. Analg. 2021, 133, 304–313. [Google Scholar] [CrossRef]
- Song, Y.; Yang, X.; Luo, Y.; Ouyang, C.; Yu, Y.; Ma, Y.; Li, H.; Lou, J.; Liu, Y.; Chen, Y.; et al. Comparison of logistic regression and machine learning methods for predicting postoperative delirium in elderly patients: A retrospective study. CNS Neurosci. Ther. 2023, 29, 158–167. [Google Scholar] [CrossRef]
- Famularo, S.; Milana, F.; Cimino, M.; Franchi, E.; Giuffrida, M.; Costa, G.; Procopio, F.; Donadon, M.; Torzilli, G. Upfront surgery versus neoadjuvant perioperative chemotherapy for resectable colorectal liver metastases: A machine-learning decision tree to identify the best potential candidates under a parenchyma-sparing policy. Cancers 2023, 15, 613. [Google Scholar] [CrossRef]
- Schmidt, D.; English, G.; Gent, T.C.; Yanik, M.F.; von der Behrens, W. Machine learning reveals interhemispheric somatosensory coherence as indicator of anesthetic depth. Front. Neuroinform. 2022, 16, 971231. [Google Scholar] [CrossRef] [PubMed]
- Pai, K.-C.; Su, S.-A.; Chan, M.-C.; Wu, C.-L.; Chao, W.-C. Explainable machine learning approach to predict extubation in critically ill ventilated patients: A retrospective study in central Taiwan. BMC Anesth. 2022, 22, 351. [Google Scholar] [CrossRef]
- Jung, J.W.; Hwang, S.; Ko, S.; Jo, C.; Park, H.Y.; Han, H.-S.; Lee, M.C.; Park, J.E.; Ro, D.H. A machine-learning model to predict postoperative delirium following knee arthroplasty using electronic health records. BMC Psychiatry 2022, 22, 436. [Google Scholar] [CrossRef] [PubMed]
- Yoshimura, M.; Shiramoto, H.; Koga, M.; Morimoto, Y. Preoperative echocardiography predictive analytics for postinduction hypotension prediction. PLoS ONE 2022, 17, e0278140. [Google Scholar] [CrossRef] [PubMed]
- Zhou, C.-M.; Wang, Y.; Xue, Q.; Yang, J.-J.; Zhu, Y. Predicting difficult airway intubation in thyroid surgery using multiple machine learning and deep learning algorithms. Front. Public Health 2022, 10, 937471. [Google Scholar] [CrossRef]
- Lu, Y.; Chen, Q.; Zhang, H.; Huang, M.; Yao, Y.; Ming, Y.; Yan, M.; Yu, Y.; Yu, L. Machine learning models of postoperative atrial fibrillation prediction after cardiac surgery. J. Cardiothorac. Vasc. Anesth. 2022, 37, 360–366. [Google Scholar] [CrossRef]
- Zhang, Y.; Li, L.; Li, Y.; Zeng, Z. Machine learning model-based risk prediction of severe complications after off-pump coronary artery bypass grafting. Adv. Clin. Exp. Med. 2023, 32, 185–194. [Google Scholar] [CrossRef]
- Ezuma, C.O.; Lu, Y.; Pareek, A.; Wilbur, R.; Krych, A.J.; Forsythe, B.; Camp, C.L. A machine learning algorithm outperforms traditional multiple regression to predict risk of unplanned overnight stay following outpatient medial patellofemoral ligament reconstruction. Arthrosc. Sports Med. Rehab. 2022, 4, e1103–e1110. [Google Scholar] [CrossRef]
- Fransén, J.; Lundin, J.; Fredén, F.; Huss, F. A proof-of-concept study on mortality prediction with machine learning algorithms using burn intensive care data. Scars Burn. Health 2022, 8, 20595131211066585. [Google Scholar] [CrossRef] [PubMed]
- Yan, X.; Goldsmith, J.; Mohan, S.; Turnbull, Z.A.; Freundlich, R.E.; Billings th Kiran, R.P.; Li, G.; Kim, M. Impact of intraoperative data on risk prediction for mortality after intra-abdominal surgery. Anesth. Analg. 2022, 134, 102–113. [Google Scholar] [CrossRef] [PubMed]
- Palla, K.; Hyland, S.L.; Posner, K.; Ghosh, P.; Nair, B.; Bristow, M.; Paleva, Y.; Williams, B.; Fong, C.; Van Cleve, W.; et al. Intraoperative prediction of postanaesthesia care unit hypotension. Br. J. Anaesth. 2022, 128, 623–635. [Google Scholar] [CrossRef]
- Cao, Y.; Naslund, I.; Naslund, E.; Ottosson, J.; Montgomery, S.; Stenberg, E. Using a convolutional neural network to predict remission of diabetes after gastric bypass surgery: Machine learning study from the scandinavian obesity surgery register. JMIR Med. Inf. 2021, 9, e25612. [Google Scholar] [CrossRef] [PubMed]
- Jean, W.-H.; Sutikno, P.; Fan, S.-Z.; Abbod, M.F.; Shieh, J.-S. Comparison of deep learning algorithms in predicting expert assessments of pain scores during surgical operations using analgesia nociception index. Sensors 2022, 22, 5496. [Google Scholar] [CrossRef]
- Chen, P.-F.; Chen, L.; Lin, Y.-K.; Li, G.-H.; Lai, F.; Lu, C.-W.; Yang, C.-Y.; Chen, K.-C.; Lin, T.-Y. Predicting postoperative mortality with deep neural networks and natural language processing: Model development and validation. JMIR Med. Inf. 2022, 10, e38241. [Google Scholar] [CrossRef] [PubMed]
- Jiao, Y.; Xue, B.; Lu, C.; Avidan, M.S.; Kannampallil, T. Continuous real-time prediction of surgical case duration using a modular artificial neural network. Br. J. Anaesth. 2022, 128, 829–837. [Google Scholar] [CrossRef]
- Maciąg, T.T.; van Amsterdam, K.; Ballast, A.; Cnossen, F.; Struys, M.M. Machine learning in anesthesiology: Detecting adverse events in clinical practice. Health Inform. J. 2022, 28, 146045822211128. [Google Scholar] [CrossRef]
- Peng, X.; Zhu, T.; Chen, G.; Wang, Y.; Hao, X. A multicenter prospective study on postoperative pulmonary complications prediction in geriatric patients with deep neural network model. Front. Surg. 2022, 9, 976536. [Google Scholar] [CrossRef]
- Ishii, E.; Nawa, N.; Hashimoto, S.; Shigemitsu, H.; Fujiwara, T. Development, validation, and feature extraction of a deep learning model predicting in-hospital mortality using Japan’s largest national ICU database: A validation framework for transparent clinical artificial intelligence (cAI) development. Anaesth. Crit. Care Pain Med. 2023, 42, 101167. [Google Scholar] [CrossRef] [PubMed]
- Kowadlo, G.; Mittelberg, Y.; Ghomlaghi, M.; Stiglitz, D.K.; Kishore, K.; Guha, R.; Nazareth, J.; Weinberg, L. Development and Validation of ‘Patient Optimizer’ (POP) Algorithms for Predicting Surgical Risk with Machine Learning. BMC Med. Inform. Decis. Mak. 2024, 24, 70. [Google Scholar] [CrossRef] [PubMed]
- Ashraf Ganjouei, A.; Romero-Hernandez, F.; Wang, J.J.; Casey, M.; Frye, W.; Hoffman, D.; Hirose, K.; Nakakura, E.; Corvera, C.; Maker, A.V.; et al. A Machine Learning Approach to Predict Postoperative Pancreatic Fistula After Pancreaticoduodenectomy Using Only Preoperatively Known Data. Ann. Surg. Oncol. 2023, 30, 7738–7747. [Google Scholar] [CrossRef] [PubMed]
- Syed Musthafa, A.; Sankar, K.; Benil, T.; Rao, Y.N. A Hybrid Machine Learning Technique for Early Prediction of Lung Nodules from Medical Images Using a Learning-based Neural Network Classifier. Concurr. Comput. 2023, 35, e7488. [Google Scholar] [CrossRef]
- Nwaiwu, C.A.; Rivera Perla, K.M.; Abel, L.B.; Sears, I.J.; Barton, A.T.; Peterson, R.C.; Liu, Y.Z.; Khatri, I.S.; Sarkar, I.N.; Shah, N. Predicting Colonic Neoplasia Surgical Complications: A Machine Learning Approach. Dis. Colon Rectum 2024, 67, 700–713. [Google Scholar] [CrossRef] [PubMed]
- Szrama, J.; Gradys, A.; Bartkowiak, T.; Woźniak, A.; Nowak, Z.; Zwoliński, K.; Lohani, A.; Jawień, N.; Smuszkiewicz, P.; Kusza, K. The Incidence of Perioperative Hypotension in Patients Undergoing Major Abdominal Surgery with the Use of Arterial Waveform Analysis and the Hypotension Prediction Index Hemodynamic Monitoring-A Retrospective Analysis. J. Pers. Med. 2024, 14, 174. [Google Scholar] [CrossRef]
- Xu, Y.; Ju, L.; Tong, J.; Zhou, C.-M.; Yang, J.-J. Machine Learning Algorithms for Predicting the Recurrence of Stage IV Colorectal Cancer After Tumor Resection. Sci. Rep. 2020, 10, 2519. [Google Scholar] [CrossRef] [PubMed]
- Jeon, Y.; Kim, Y.-J.; Jeon, J.; Nam, K.-H.; Hwang, T.-S.; Kim, K.-G.; Baek, J.-H. Machine Learning Based Prediction of Recurrence after Curative Resection for Rectal Cancer. PLoS ONE 2023, 18, e0290141. [Google Scholar] [CrossRef] [PubMed]
- Merath, K.; Hyer, J.M.; Mehta, R.; Farooq, A.; Bagante, F.; Sahara, K.; Tsilimigras, D.I.; Beal, E.; Paredes, A.Z.; Wu, L.; et al. Use of Machine Learning for Prediction of Patient Risk of Postoperative Complications After Liver, Pancreatic, and Colorectal Surgery. J. Gastrointest. Surg. 2020, 24, 1843–1851. [Google Scholar] [CrossRef]
- Jo, Y.-Y.; Han, J.; Park, H.W.; Jung, H.; Lee, J.D.; Jung, J.; Cha, H.S.; Sohn, D.K.; Hwangbo, Y. Prediction of Prolonged Length of Hospital Stay After Cancer Surgery Using Machine Learning on Electronic Health Records: Retrospective Cross-Sectional Study. JMIR Med. Inform. 2021, 9, e23147. [Google Scholar] [CrossRef]
- Howell, T.C.; Lumpkin, S.; Chaumont, N. Predicting Colorectal Surgery Readmission Risk: A Surgery-Specific Predictive Model. IISE Trans. Healthc. Syst. Eng. 2023, 13, 175–181. [Google Scholar] [CrossRef] [PubMed]
- Mao, W.-B.; Lyu, J.-Y.; Vaishnani, D.K.; Lyu, Y.-M.; Gong, W.; Xue, X.-L.; Shentu, Y.-P.; Ma, J. Application of artificial neural networks in detection and diagnosis of gastrointestinal and liver tumors. World J. Clin. Cases 2020, 8, 3971–3977. [Google Scholar] [CrossRef] [PubMed]
- Mikhael, P.G.; Wohlwend, J.; Yala, A.; Karstens, L.; Xiang, J.; Takigami, A.K.; Bourgouin, P.P.; Chan, P.; Mrah, S.; Amayri, W.; et al. Sybil: A validated deep learning model to predict future lung cancer risk from a single low-dose chest computed tomography. J. Clin. Oncol. 2023, 41, 2191–2200. [Google Scholar] [CrossRef] [PubMed]
- Altini, N.; Marvulli, T.M.; Zito, F.A.; Caputo, M.; Tommasi, S.; Azzariti, A.; Brunetti, A.; Prencipe, B.; Mattioli, E.; De Summa, S.; et al. The role of unpaired image-to-image translation for stain color normalization in colorectal cancer histology classification. Comput. Methods Programs Biomed. 2023, 234, 107511. [Google Scholar] [CrossRef]
- Schamberg, G.; Badgeley, M.; Meschede-Krasa, B.; Kwon, O.; Brown, E.N. Continuous action deep reinforcement learning for propofol dosing during general anesthesia. Artif. Intell. Med. 2022, 123, 102227. [Google Scholar] [CrossRef]

| ML Subdomain | Definition |
|---|---|
| Supervised learning (SL) | SL involves learning to predict future events by utilizing past events to perform dataset analysis (training) through inferred functions to make predictions (testing) regarding outcomes. The outcome (target) variable is known for predictions. ML algorithms enable error prediction and self-correction. Types of SL include (i) classification and (ii) regression [8]. Examples include training prediction models for risk indices and clinical research. |
| Unsupervised learning (UL) | UL learning involves algorithms that analyze and cluster unlabeled data according to hidden patterns or data groupings. Types of UL include (i) clustering, (ii) association rules, and (iii) dimensionality reduction [5]. Examples: medical imaging in pathology and radiology and clinical decision support. |
| Semi-supervised learning (SSL) | SSL learning combines supervised and unsupervised learning by utilizing a small sampling of labeled data plus a large amount of unlabeled data. Examples: speech recognition and text identification in the electronic health record [5]. |
| Reinforced learning (RL) | RL learning operates through sequential decision-making (trial and error) to maximize total reward through random trialing. Example: bioprosthetic devices [5]. |
| Performance Measure | Performance Measure Calculation |
|---|---|
| Accuracy | = TP + TN/(TP TN + FP + FN) = 1 − (error rate) |
| Precision | = TP/TP + FP |
| Recall (Sensitivity) | = TP/TP + FN (True Positive Rate) |
| F1 Score | = (2 × Precision × Recall)/(Precision + Recall) |
| Specificity (True Negative Rate) | = TN/TN + FP |
| Classification Error Rate | = Type I Error + Type 2 Error |
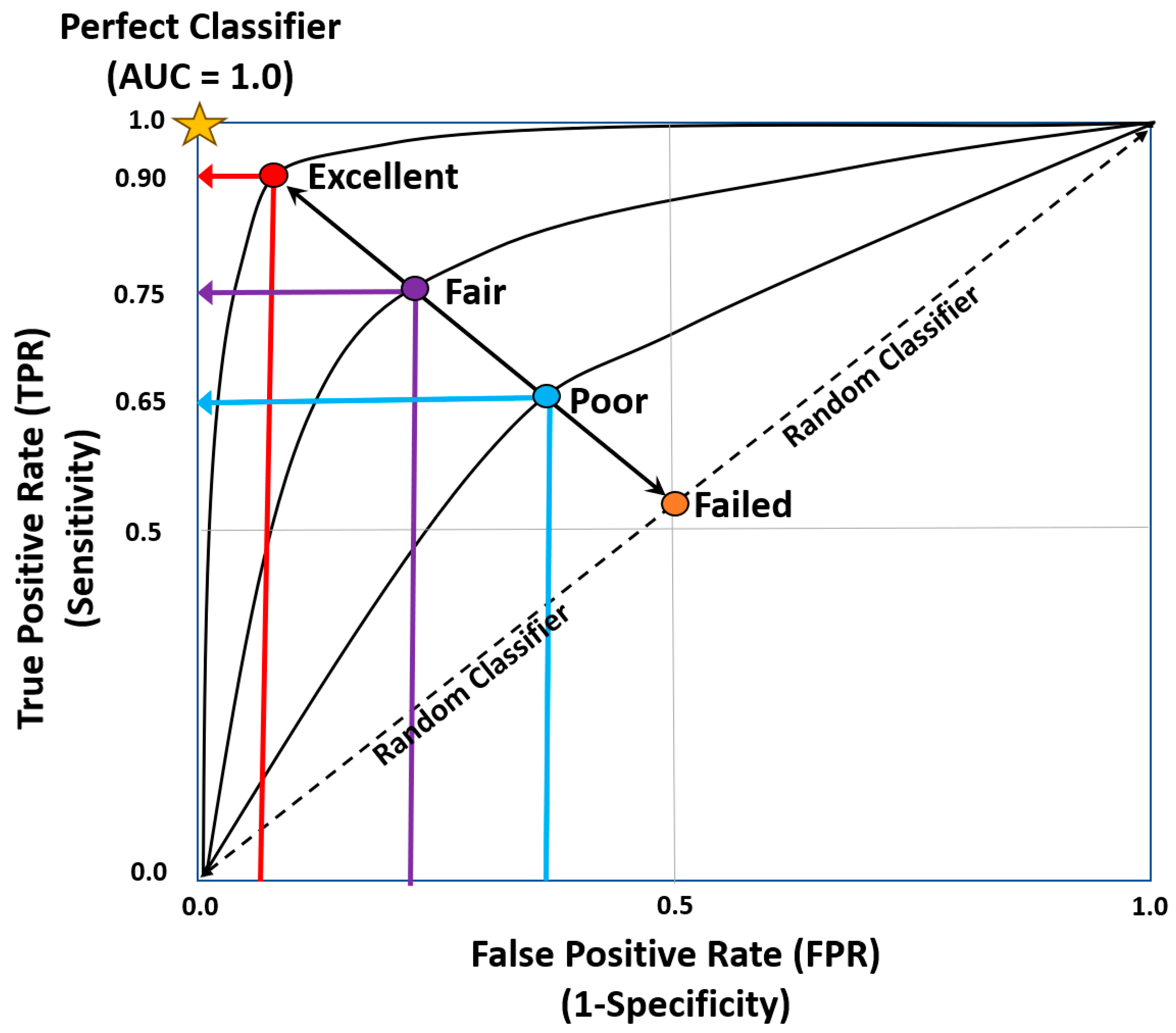
| ≤0.5 | Failed |
|---|---|
| 0.5 to 0.7 | Poor |
| 0.7 to 0.8 | Fair |
| 0.8 to 0.9 | Good |
| 0.9 to 1.0 | Excellent |
| Non-Parametric Nature | Applicable to a Wide Range of Data Types without Requiring Specific Assumptions about Their Distribution. |
|---|---|
| Flexibility | Can be used to estimate various statistics and assess their variability. |
| Computational Efficiency | Relatively fast to implement, especially when compared to other resampling techniques. |
| Program | Country | Website Link | Additional Resources |
|---|---|---|---|
| Surveillance, Epidemiology, and End Results (SEER) Program | United States | SEER Program: https://seer.cancer.gov/, accessed on 10 May 2024 | Explore the following resources to potentially find relevant data science trajectory resources: American Association for Cancer Research (AACR) Careers (https://www.aacr.org/, accessed on 10 May 2024) and National Cancer Institute (NCI) Career Development (https://www.cancer.gov/grants-training/training, accessed on 10 May 2024) |
| National Cancer Database (NCDB) | United States | NCDB: https://www.facs.org/quality-programs/cancer/ncdb, accessed on 10 May 2024 | Same as above |
| Stanford Cancer Institute Research Database (SCIRDB) | United States | SCIRDB: https://med.stanford.edu/ric/data-coordination/scirdb.html, accessed on 10 May 2024 | Same as above |
| Cancer Data Registry of Idaho (CDRI) | United States | CDRI: https://www.idcancer.org/, accessed on 10 May 2024 | Same as above |
| National Cancer Institute of Canada (NCIC) | Canada | NCIC: https://www.cancer.ca/, accessed on 10 May 2024 | Explore the Canadian Cancer Research Society (CCRS) Training and Education: https://www.reproductivefreedomca.org/, accessed on 10 May 2024 |
| Cancer Research UK (CRUK) | United Kingdom | CRUK: https://www.cancerresearchuk.org/, accessed on 10 May 2024 | Explore CRUK’s Career Development programs: https://www.cancerresearchuk.org/about-us/careers, accessed on 10 May 2024 |
| Danish Cancer Registry (DCR) | Denmark | DCR: https://ncrr.au.dk/danish-registers/the-danish-cancer-register, accessed on 10 May 2024 | Consider searching for resources offered by universities in Denmark with data science programs |
| Netherlands Cancer Registry (NCR) | Netherlands | NCR: https://www.iknl.nl/, accessed on 10 May 2024 | Explore the Netherlands Organization for Scientific Research’s (NWO) career development opportunities: https://www.nwo.nl/, accessed on 10 May 2024 |
| Cancer Registry of Norway (CRN) | Norway | CRN: https://www.kreftregisteret.no/, accessed on 10 May 2024 | Investigate resources at the University of Oslo or other Norwegian universities with data science programs |
| Australian Cancer Database (ACD) | Australia | ACD: https://www.aihw.gov.au/about-our-data/our-data-collections/australian-cancer-database, accessed on 10 May 2024 | Explore resources provided by the Australian Institute of Health and Welfare (AIHW): https://www.aihw.gov.au/reports/workforce/health-workforce, accessed on 10 May 2024 |
| Japan Cancer Surveillance Research Group (JCSRG) | Japan | JCSRG: https://www.ncc.go.jp/en/cis/divisions/stat/index.html, accessed on 10 May 2024 | Consider searching for data science programs at Japanese universities and research institutions |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Brydges, G.; Uppal, A.; Gottumukkala, V. Application of Machine Learning in Predicting Perioperative Outcomes in Patients with Cancer: A Narrative Review for Clinicians. Curr. Oncol. 2024, 31, 2727-2747. https://doi.org/10.3390/curroncol31050207
Brydges G, Uppal A, Gottumukkala V. Application of Machine Learning in Predicting Perioperative Outcomes in Patients with Cancer: A Narrative Review for Clinicians. Current Oncology. 2024; 31(5):2727-2747. https://doi.org/10.3390/curroncol31050207
Chicago/Turabian StyleBrydges, Garry, Abhineet Uppal, and Vijaya Gottumukkala. 2024. "Application of Machine Learning in Predicting Perioperative Outcomes in Patients with Cancer: A Narrative Review for Clinicians" Current Oncology 31, no. 5: 2727-2747. https://doi.org/10.3390/curroncol31050207
APA StyleBrydges, G., Uppal, A., & Gottumukkala, V. (2024). Application of Machine Learning in Predicting Perioperative Outcomes in Patients with Cancer: A Narrative Review for Clinicians. Current Oncology, 31(5), 2727-2747. https://doi.org/10.3390/curroncol31050207