Management of Recurrent Retroperitoneal Sarcoma
Abstract
1. Introduction
2. Imaging
3. Chemotherapy
4. Radiation
5. Resection
6. Patient Selection
7. Conclusions
- Recurrence is common after surgery for RPS, and pattern of recurrence (local recurrence vs. distant metastasis) varies by histology.
- Patients with primary and recurrent RPS should be referred for multidisciplinary evaluation at a sarcoma center.
- High-quality, contrast-enhanced CT imaging of the chest, abdomen, and pelvis should be performed when tumor recurrence is first identified.
- MRI may be useful to help delineate pelvic disease or extent of tumor involvement.
- Neoadjuvant therapy may have some limited utility in downsizing large or locally invasive tumors, although data are limited.
- Data on the use of adjuvant therapy and radiation are limited in the setting of recurrent disease.
- Repeat resection is worth considering for technically resectable local and distant recurrence and has an associated survival benefit.
- In general, multifocal recurrence is associated with worse survival and should be reserved for palliation in symptomatic patients.
Author Contributions
Funding
Informed Consent Statement
Conflicts of Interest
References
- Ahlen, J.; Ahuja, N.; Antbacka, R.; Bagaria, S.; Blay, J.Y.; Bonvalot, S.; Callegaro, D.; Canter, R.J.; Cardona, K.; Casali, P.G.; et al. Management of Recurrent Retroperitoneal Sarcoma (RPS) in the Adult: A Consensus Approach from the Trans-Atlantic RPS Working Group. Ann. Surg. Oncol. 2016, 23, 3531–3540. [Google Scholar] [CrossRef]
- Singer, S.; Antonescu, C.R.; Riedel, E.; Brennan, M.F.; Pollock, R.E. Histologic Subtype and Margin of Resection Predict Pattern of Recurrence and Survival for Retroperitoneal Liposarcoma. Ann. Surg. 2003, 238, 358–371. [Google Scholar] [CrossRef]
- Tan, M.C.B.; Brennan, M.F.; Kuk, D.; Agaram, N.P.; Antonescu, C.R.; Qin, L.X.; Moraco, N.; Crago, A.M.; Singer, S. Histology-Based Classification Predicts Pattern of Recurrence and Improves Risk Stratification in Primary Retroperitoneal Sarcoma. Ann. Surg. 2016, 263, 593–600. [Google Scholar] [CrossRef]
- Lehnert, T.; Cardona, S.; Hinz, U.; Willeke, F.; Mechtersheimer, G.; Treiber, M.; Herfarth, C.; Buechler, M.W.; Schwarzbach, M.H.M. Primary and Locally Recurrent Retroperitoneal Soft-Tissue Sarcoma: Local Control and Survival. Eur. J. Surg. Oncol. 2009, 35, 986–993. [Google Scholar] [CrossRef]
- Gronchi, A.; Miceli, R.; Allard, M.A.; Callegaro, D.; le Péchoux, C.; Fiore, M.; Honoré, C.; Sanfilippo, R.; Coppola, S.; Stacchiotti, S.; et al. Personalizing the Approach to Retroperitoneal Soft Tissue Sarcoma: Histology-Specific Patterns of Failure and Postrelapse Outcome after Primary Extended Resection. Ann. Surg. Oncol. 2015, 22, 1447–1454. [Google Scholar] [CrossRef]
- Gronchi, A.; Strauss, D.C.; Miceli, R.; Bonvalot, S.; Swallow, C.J.; Hohenberger, P.; van Coevorden, F.; Rutkowski, P.; Callegaro, D.; Hayes, A.J.; et al. Variability in Patterns of Recurrence after Resection of Primary Retroperitoneal Sarcoma (RPS). A Report on 1007 Patients from the Multi-Institutional Collaborative RPS Working Group. Ann. Surg. 2016, 263, 1002–1009. [Google Scholar] [CrossRef]
- Stojadinovic, A.; Leung, D.H.Y.; Hoos, A.; Jaques, D.P.; Lewis, J.J.; Brennan, M.F. Analysis of the Prognostic Significance of Microscopic Margins in 2,084 Localized Primary Adult Soft Tissue Sarcomas. Ann. Surg. 2002, 235, 424–434. [Google Scholar] [CrossRef] [PubMed]
- Bonvalot, S.; Raut, C.P.; Pollock, R.E.; Rutkowski, P.; Strauss, D.C.; Hayes, A.J.; van Coevorden, F.; Fiore, M.; Stoeckle, E.; Hohenberger, P.; et al. Technical Considerations in Surgery for Retroperitoneal Sarcomas: Position Paper from E-Surge, a Master Class in Sarcoma Surgery, and EORTC-STBSG. Ann. Surg. Oncol. 2012, 19, 2981–2991. [Google Scholar] [CrossRef] [PubMed]
- Villano, A.M.; Zeymo, A.; McDermott, J.; Barrak, D.; Unger, K.R.; Shara, N.M.; Chan, K.S.; Al-Refaie, W.B. Regionalization of Retroperitoneal Sarcoma Surgery to High-Volume Hospitals: Missed Opportunities for Outcome Improvement. J. Oncol. Pr. 2018, 15, e247–e261. [Google Scholar] [CrossRef]
- Gronchi, A.; Miceli, R.; Colombo, C.; Stacchiotti, S.; Collini, P.; Mariani, L.; Sangalli, C.; Radaelli, S.; Sanfilippo, R.; Fiore, M.; et al. Frontline Extended Surgery Is Associated with Improved Survival in Retroperitoneal Low- to Intermediate-Grade Soft Tissue Sarcomas. Ann. Oncol. 2012, 23, 1067–1073. [Google Scholar] [CrossRef]
- Villano, A.M.; Zeymo, A.; Chan, K.S.; Shara, N.; Al-Refaie, W.B. Identifying the Minimum Volume Threshold for Retroperitoneal Soft Tissue Sarcoma Resection: Merging National Data with Consensus Expert Opinion. J. Am. Coll. Surg. 2020, 230, 151–160.e2. [Google Scholar] [CrossRef]
- Keung, E.Z.; Chiang, Y.J.; Cormier, J.N.; Torres, K.E.; Hunt, K.K.; Feig, B.W.; Roland, C.L. Treatment at Low-Volume Hospitals Is Associated with Reduced Short-Term and Long-Term Outcomes for Patients with Retroperitoneal Sarcoma. Cancer 2018, 124, 4495–4503. [Google Scholar] [CrossRef]
- Bonvalot, S.; Rivoire, M.; Castaing, M.; Stoeckle, E.; le Cesne, A.; Blay, J.Y.; Laplanche, A. Primary Retroperitoneal Sarcomas: A Multivariate Analysis of Surgical Factors Associated with Local Control. J. Clin. Oncol. 2009, 27, 31–37. [Google Scholar] [CrossRef] [PubMed]
- Toulmonde, M.; Bonvalot, S.; Méeus, P.; Stoeckle, E.; Riou, O.; Isambert, N.; Bompas, E.; Jafari, M.; Delcambre-Lair, C.; Saada, E.; et al. Retroperitoneal Sarcomas: Patterns of Care at Diagnosis, Prognostic Factors and Focus on Main Histological Subtypes: A Multicenter Analysis of the French Sarcoma Group. Ann. Oncol. 2014, 25, 735–742. [Google Scholar] [CrossRef]
- Tseng, W.W.; Swallow, C.J.; Strauss, D.C.; Bonvalot, S.; Rutkowski, P.; Ford, S.J.; Gonzalez, R.J.; Gladdy, R.A.; Gyorki, D.E.; Fairweather, M.; et al. Management of Locally Recurrent Retroperitoneal Sarcoma in the Adult: An Updated Consensus Approach from the Transatlantic Australasian Retroperitoneal Sarcoma Working Group. Ann. Surg. Oncol. 2022, 29, 7335–7348. [Google Scholar] [CrossRef]
- Raut, C.P.; George, S.; Hornick, J.L.; Butrynski, J.E.; Morgan, J.A.; Ready, J.; Nascimento, A.F.; Fletcher, C.D.; Demetri, G.D.; Baldini, E.H. High Rates of Histopathologic Discordance in Sarcoma with Implications for Clinical Care. J. Clin. Oncol. 2011, 29, 10065. [Google Scholar] [CrossRef]
- Ray-coquard, I.; Montesco, M.C.; Coindre, J.M.; Dei tos, A.P.; Lurkin, A.; Ranchère-vince, D.; Vecchiato, A.; Decouvelaere, A.V.; Mathoulin-pélissier, S.; Albert, S.; et al. Sarcoma: Concordance between Initial Diagnosis and Centralized Expert Review in a Population-Based Study within Three European Regions. Ann. Oncol. 2012, 23, 2442–2449. [Google Scholar] [CrossRef]
- Choi, J.H.; Ro, J.Y. Retroperitoneal Sarcomas: An Update on the Diagnostic Pathology Approach. Diagnostics 2020, 10, 642. [Google Scholar] [CrossRef]
- Matthyssens, L.E.; Creytens, D.; Ceelen, W.P. Retroperitoneal Liposarcoma: Current Insights in Diagnosis and Treatment. Front. Surg. 2015, 2, 4. [Google Scholar] [CrossRef]
- Messiou, C.; Morosi, C. Imaging in Retroperitoneal Soft Tissue Sarcoma. J. Surg. Oncol. 2018, 117, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Subramaniam, S.; Callahan, J.; Bressel, M.; Hofman, M.S.; Mitchell, C.; Hendry, S.; Vissers, F.L.; van der Hiel, B.; Patel, D.; van Houdt, W.J.; et al. The Role of 18F-FDG PET/CT in Retroperitoneal Sarcomas—A Multicenter Retrospective Study. J. Surg. Oncol. 2021, 123, 1081–1087. [Google Scholar] [CrossRef] [PubMed]
- Antman, K.; Crowley, J.; Balcerzak, S.P.; Rivkin, S.E.; Weiss, G.R.; Elias, A.; Natale, R.B.; Cooper, R.M.; Barlogie, B.; Trump, D.L.; et al. An Intergroup Phase III Randomized Study of Doxorubicin and Dacarbazine With or Without Ifosfamide and Mesna in Advanced Soft Tissue and Bone Sarcomas. J. Clin. Oncol. 1993, 11, 1276–1285. [Google Scholar] [CrossRef] [PubMed]
- van der Graaf, W.T.A.; Jones, R.L. Neoadjuvant Chemotherapy in Localised Soft-Tissue Sarcomas: Where Do We Go from Here? Lancet Oncol. 2017, 18, 706–707. [Google Scholar] [CrossRef] [PubMed]
- Reichardt, P.; Tilgner, J.; Hohenberger, P.; D6rken, B. Dose-Intensive Chemotherapy With Ifosfamide, Epirubicin, and Filgrastim for Adult Patients With Metastatic or Locally Advanced Soft Tissue Sarcoma: A Phase II Study. J. Clin. Oncol. 1998, 16, 1438–1443. [Google Scholar] [CrossRef]
- Lorigan, P.; Verweij, J.; Papai, Z.; Rodenhuis, S.; le Cesne, A.; Leahy, M.G.; Radford, J.A.; van Glabbeke, M.M.; Kirkpatrick, A.; Hogendoorn, P.C.W.; et al. Phase III Trial of Two Investigational Schedules of Ifosfamide Compared with Standard-Dose Doxorubicin in Advanced or Metastatic Soft Tissue Sarcoma: A European Organisation for Research and Treatment of Cancer Soft Tissue and Bone Sarcoma Group Study. J. Clin. Oncol. 2007, 25, 3144–3150. [Google Scholar] [CrossRef]
- Gronchi, A.; Ferrari, S.; Quagliuolo, V.; Broto, J.M.; Pousa, A.L.; Grignani, G.; Basso, U.; Blay, J.Y.; Tendero, O.; Beveridge, R.D.; et al. Histotype-Tailored Neoadjuvant Chemotherapy versus Standard Chemotherapy in Patients with High-Risk Soft-Tissue Sarcomas (ISG-STS 1001): An International, Open-Label, Randomised, Controlled, Phase 3, Multicentre Trial. Lancet Oncol. 2017, 18, 812–822. [Google Scholar] [CrossRef]
- Issels, R.D.; Lindner, L.H.; Verweij, J.; Wust, P.; Reichardt, P.; Schem, B.-C.; Rahman, A.-; Daugaard, S.; Salat, C.; Wendtner, C.-M.; et al. Neo-Adjuvant Chemotherapy Alone or with Regional Hyperthermia for Localised High-Risk Soft-Tissue Sarcoma: A Randomised Phase 3 Multicentre Study. Lancet Oncol. 2010, 11, 561–570. [Google Scholar] [CrossRef]
- Woll, P.J.; Reichardt, P.; le Cesne, A.; Bonvalot, S.; Azzarelli, A.; Hoekstra, H.J.; Leahy, M.; van Coevorden, F.; Verweij, J.; Hogendoorn, P.C.W.; et al. Adjuvant Chemotherapy with Doxorubicin, Ifosfamide, and Lenograstim for Resected Soft-Tissue Sarcoma (EORTC 62931): A Multicentre Randomised Controlled Trial. Lancet Oncol. 2012, 13, 1045–1054. [Google Scholar] [CrossRef]
- Pasquali, S.; Pizzamiglio, S.; Touati, N.; Litiere, S.; Marreaud, S.; Kasper, B.; Gelderblom, H.; Stacchiotti, S.; Judson, I.; Dei Tos, A.P.; et al. The Impact of Chemotherapy on Survival of Patients with Extremity and Trunk Wall Soft Tissue Sarcoma: Revisiting the Results of the EORTC-STBSG 62931 Randomised Trial. Eur. J. Cancer 2019, 109, 51–60. [Google Scholar] [CrossRef]
- Bonvalot, S.; Gronchi, A.; le Péchoux, C.; Swallow, C.J.; Strauss, D.; Meeus, P.; van Coevorden, F.; Stoldt, S.; Stoeckle, E.; Rutkowski, P.; et al. Preoperative Radiotherapy plus Surgery versus Surgery Alone for Patients with Primary Retroperitoneal Sarcoma (EORTC-62092: STRASS): A Multicentre, Open-Label, Randomised, Phase 3 Trial. Lancet Oncol. 2020, 21, 1366–1377. [Google Scholar] [CrossRef]
- Sobiborowicz, A.; Spałek, M.J.; Czarnecka, A.M.; Rutkowski, P. Definitive Radiotherapy in the Management of Non-Resectable or Residual Retroperitoneal Sarcomas: Institutional Cohort Analysis and Systematic Review. Cancer Control 2021, 28, 1073274820983028. [Google Scholar] [CrossRef]
- Feng, M.; Murphy, J.; Griffith, K.A.; Baker, L.H.; Sondak, V.K.; Lucas, D.R.; McGinn, C.J.; Ray, M.E. Long-Term Outcomes After Radiotherapy for Retroperitoneal and Deep Truncal Sarcoma. Int. J. Radiat. Oncol. Biol. Phys. 2007, 69, 103–110. [Google Scholar] [CrossRef]
- Yang, B.; Guo, W.H.; Lan, T.; Yuan, F.; Liu, G.J.; Zan, R.Y.; You, X.; Tan, Q.Y.; Liao, Z.Y. CT-Guided 125I Seed Implantation for Inoperable Retroperitoneal Sarcoma: A Technique for Delivery of Local Tumor Brachytherapy. Exp. Med. 2016, 12, 3843–3850. [Google Scholar] [CrossRef] [PubMed]
- Fairweather, M.; Gonzalez, R.J.; Strauss, D.; and Raut, C.P. Current Principles of Surgery for Retroperitoneal Sarcomas. J. Surg. Oncol. 2018, 117, 33–41. [Google Scholar] [CrossRef] [PubMed]
- MacNeill, A.J.; Miceli, R.; Strauss, D.C.; Bonvalot, S.; Hohenberger, P.; van Coevorden, F.; Rutkowski, P.; Callegaro, D.; Hayes, A.J.; Honoré, C.; et al. Post-Relapse Outcomes after Primary Extended Resection of Retroperitoneal Sarcoma: A Report from the Trans-Atlantic RPS Working Group. Cancer 2017, 123, 1971–1978. [Google Scholar] [CrossRef]
- Raut, C.P.; Callegaro, D.; Miceli, R.; Barretta, F.; Rutkowski, P.; Blay, J.Y.; Lahat, G.; Strauss, D.C.; Gonzalez, R.; Ahuja, N.; et al. Predicting Survival in Patients Undergoing Resection for Locally Recurrent Retroperitoneal Sarcoma: A Study and Novel Nomogram from TARPSWG. Clin. Cancer Res. 2019, 25, 2664–2671. [Google Scholar] [CrossRef] [PubMed]
- van Houdt, W.J.; Fiore, M.; Barretta, F.; Rutkowski, P.; Blay, J.Y.; Lahat, G.; Strauss, D.; Gonzalez, R.J.; Ahuja, N.; Grignani, G.; et al. Patterns of Recurrence and Survival Probability after Second Recurrence of Retroperitoneal Sarcoma: A Study from TARPSWG. Cancer 2020, 126, 4917–4925. [Google Scholar] [CrossRef]
- Tropea, S.; Mocellin, S.; Damiani, G.B.; Stramare, R.; Aliberti, C.; del Fiore, P.; Rossi, C.R.; Rastrelli, M. Recurrent Retroperitoneal Sarcomas: Clinical Outcomes of Surgical Treatment and Prognostic Factors. Eur. J. Surg. Oncol. 2021, 47, 1201–1206. [Google Scholar] [CrossRef] [PubMed]
- Yang, J.Y.; Kong, S.H.O.; Ahn, H.S.; Lee, H.J.; Jeong, S.Y.; Ha, J.; Yang, H.K.; Park, K.J.; Lee, K.U.K.; Choe, K.J. Prognostic Factors for Reoperation of Recurrent Retroperitoneal Sarcoma: The Role of Clinicopathological Factors Other than Histologic Grade. J. Surg. Oncol. 2015, 111, 165–172. [Google Scholar] [CrossRef]
- Ikoma, N.; Torres, K.E.; Lin, H.Y.; Ravi, V.; Roland, C.L.; Mann, G.N.; Hunt, K.K.; Cormier, J.N.; Feig, B.W. Recurrence Patterns of Retroperitoneal Leiomyosarcoma and Impact of Salvage Surgery. J. Surg. Oncol. 2017, 116, 313–319. [Google Scholar] [CrossRef]
- Anaya, D.A.; Lahat, G.; Liu, J.; Xing, Y.; Cormier, J.N.; Pisters, P.W.; Lev, D.C.; Pollock, R.E. Multifocality in Retroperitoneal Sarcoma: A Prognostic Factor Critical to Surgical Decision-Making. Ann. Surg. 2009, 249, 137–142. [Google Scholar] [CrossRef] [PubMed]
- Lv, A.; Li, Y.; Li, Z.; Mao, L.; Tian, X.; Hao, C. Treatment Algorithm and Surgical Outcome for Primary and Recurrent Retroperitoneal Sarcomas: A Long-term Single-center Experience of 242 Cases. J. Surg. Oncol. 2022, 126, 1288–1298. [Google Scholar] [CrossRef] [PubMed]
- Park, J.O.; Qin, L.X.; Prete, F.P.; Antonescu, C.; Brennan, M.F.; Singer, S. Predicting Outcome by Growth Rate of Locally Recurrent Retroperitoneal Liposarcoma: The One Centimeter per Month Rule. Ann. Surg. 2009, 250, 977–982. [Google Scholar] [CrossRef] [PubMed]
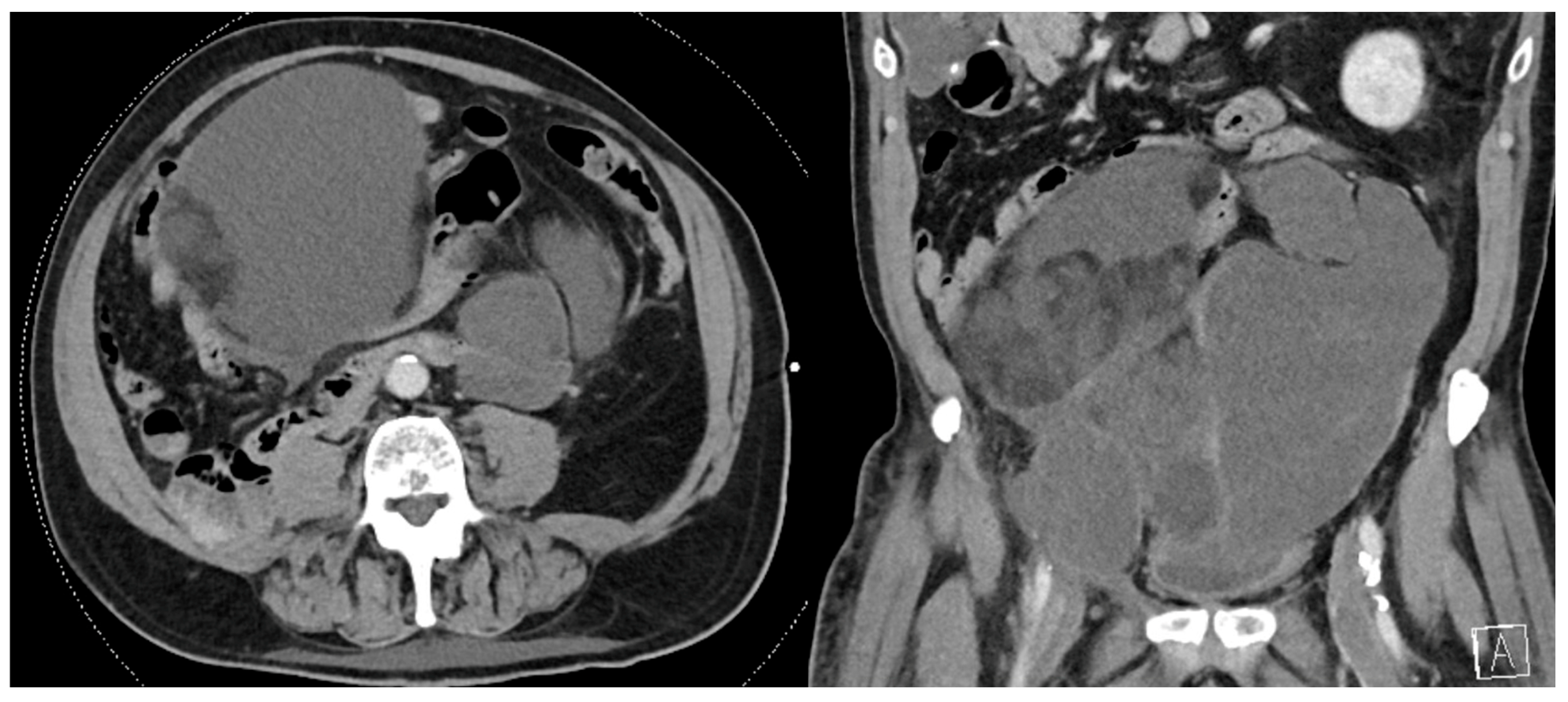
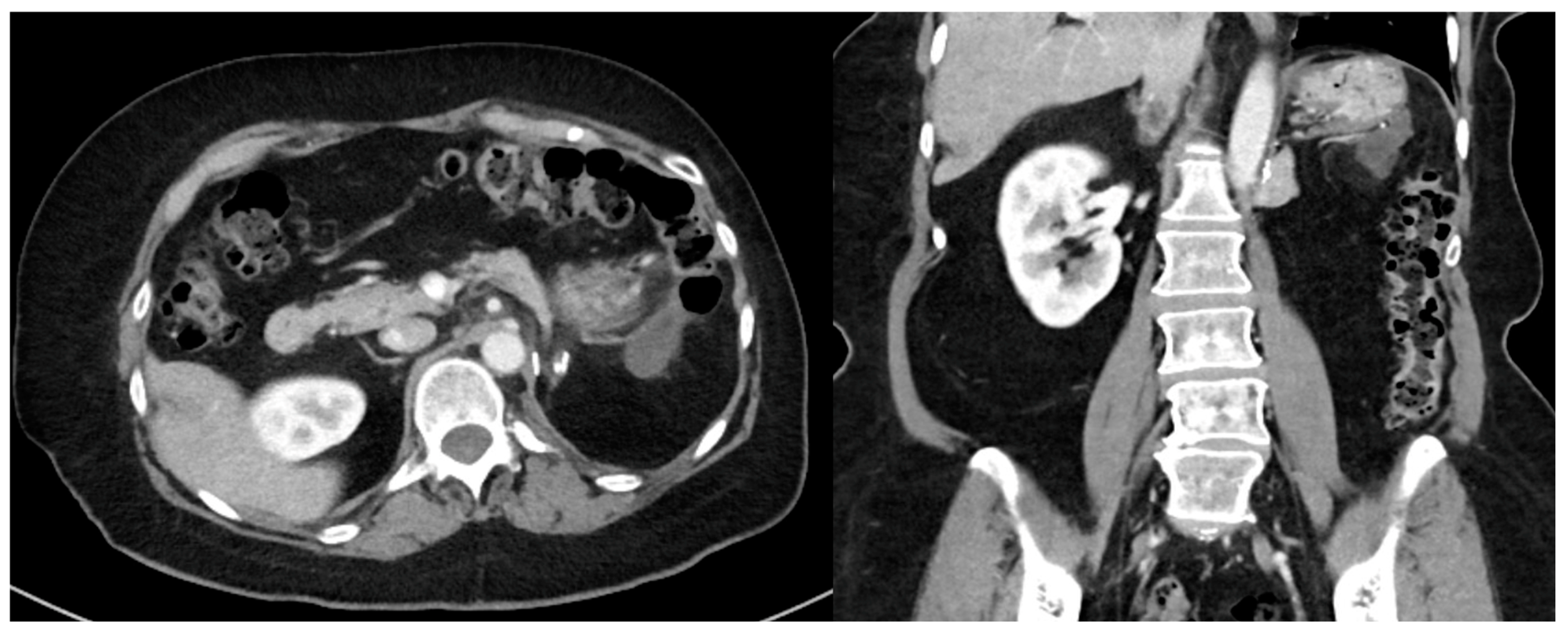
| Incision should maximize exposure and minimize the risk of tumor capsule disruption. |
| A midline laparotomy has the benefit of adequate access to the retroperitoneum, as well as future access in the case of local recurrence. |
| Chevron, Makuuchi, or thoracoabdominal incisions may provide superior exposure for upper quadrant sarcomas. |
| A transverse flank or modified Gibson incision may provide superior exposure of the superior pelvis and iliac vessels, particularly for extraperitoneal pelvic sarcomas. |
| While access to the retroperitoneum may involve mobilization of the colon, a macroscopically complete resection often necessitates en bloc colectomy and resection of any additional involved organs. |
| Preoperative planning and sterile preparation should anticipate the possibility of an end or diverting ostomy. |
| Right-sided tumors may require nephroureterectomy with Kocherization of the duodenum and head of the pancreas and include ipsilateral colectomy, adrenalectomy, and psoas/psoas fascia resection. |
| Left-sided tumors may require nephroureterectomy, as well as distal pancreatectomy and splenectomy and include ipsilateral colectomy, adrenalectomy, and psoas/psoas fascia resection. |
| Tumors arising from the lower 1/3 of the inferior vena cava (IVC) may require a full Cattell-Brasch maneuver for exposure. |
| Tumors arising from the middle 1/3 of the IVC may require hepatic resection of uninvolved tissue for an R0 resection. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jolissaint, J.S.; Raut, C.P.; Fairweather, M. Management of Recurrent Retroperitoneal Sarcoma. Curr. Oncol. 2023, 30, 2761-2769. https://doi.org/10.3390/curroncol30030209
Jolissaint JS, Raut CP, Fairweather M. Management of Recurrent Retroperitoneal Sarcoma. Current Oncology. 2023; 30(3):2761-2769. https://doi.org/10.3390/curroncol30030209
Chicago/Turabian StyleJolissaint, Joshua S., Chandrajit P. Raut, and Mark Fairweather. 2023. "Management of Recurrent Retroperitoneal Sarcoma" Current Oncology 30, no. 3: 2761-2769. https://doi.org/10.3390/curroncol30030209
APA StyleJolissaint, J. S., Raut, C. P., & Fairweather, M. (2023). Management of Recurrent Retroperitoneal Sarcoma. Current Oncology, 30(3), 2761-2769. https://doi.org/10.3390/curroncol30030209





