Immunohistochemistry for Prostate Biopsy—Impact on Histological Prostate Cancer Diagnoses and Clinical Decision Making
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population
2.2. IHC Stains
2.3. Changes in Biopsy Results and Changes in Clinical Decision Making
2.4. Statistical Analysis
3. Results
3.1. Descriptive Baseline Characteristics: IHC vs. No IHC
3.2. IHC in Patients with and without Prostate Cancer Detection
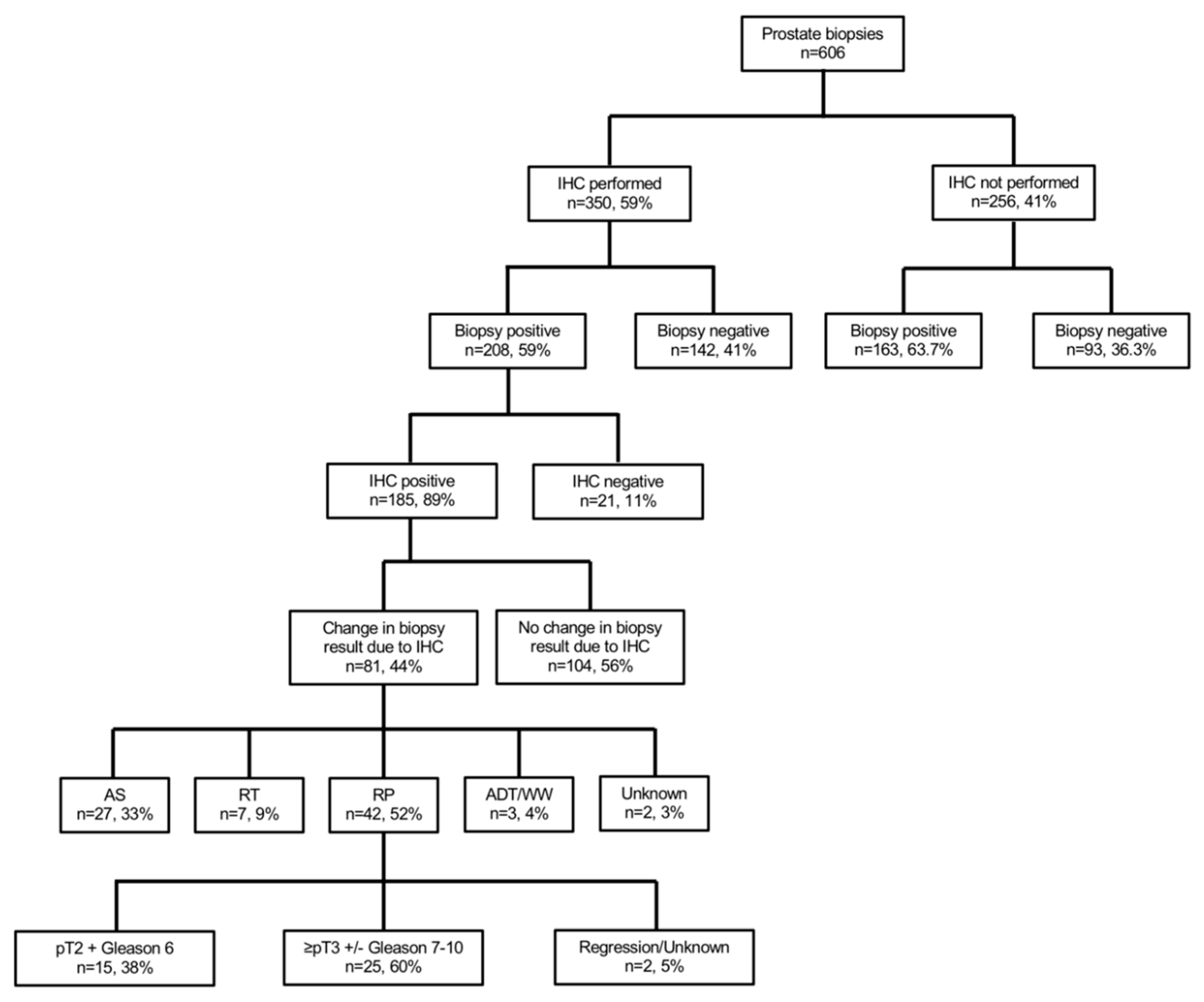
3.3. Changes in Prostate Biopsy Results due to IHC Stains
3.4. Treatments of Patients with Changes in Prostate Biopsy due to Positive IHC
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Ferlay, J.; Colombet, M.; Soerjomataram, I.; Dyba, T.; Randi, G.; Bettio, M.; Gavin, A.; Visser, O.; Bray, F. Cancer incidence and mortality patterns in Europe: Estimates for 40 countries and 25 major cancers in 2018. Eur. J. Cancer Oxf. Engl. 1990 2018, 103, 356–387. [Google Scholar] [CrossRef]
- Mottet, N.; van den Bergh, R.C.; Briers, E.; Van den Broeck, T.; Cumberbatch, M.G.; De Santis, M.; Fanti, S.; Fossati, N.; Gandaglia, G.; Gillessen, S.; et al. EAU–EANM–ESTRO–ESUR–SIOG. Guidelines on Prostate Cancer. Eur. Urol. 2020, 79, 263–282. [Google Scholar]
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics, 2019. CA Cancer J. Clin. 2019, 69, 7–34. [Google Scholar] [CrossRef]
- Mohler, J.L.; Antonarakis, E.S.; Armstrong, A.J.; D’Amico, A.V.; Davis, B.J.; Dorff, T.; Eastham, J.A.; Enke, C.A.; Farrington, T.A.; Higano, C.S.; et al. Prostate cancer, version 1.2020, NCCN clinical practice guidelines in oncology. J. Natl. Compr. Cancer Netw. 2020, 17, 479–505. [Google Scholar] [CrossRef]
- Cher, M.L.; Dhir, A.; Auffenberg, G.B.; Linsell, S.; Gao, Y.; Rosenberg, B.; Jafri, S.M.; Klotz, L.; Miller, D.C.; Ghani, K.R.; et al. Appropriateness Criteria for Active Surveillance of Prostate Cancer. J. Urol. 2017, 197, 67–74. [Google Scholar] [CrossRef]
- Delahunt, B.; Hammond, E.; Egevad, L.; Samaratunga, H.; Srigley, J.R.; Humphrey, P.A.; Rubin, M.; Epstein, J.I.; Lin, D.W.; Gore, J.L.; et al. Active surveillance for prostate cancer: The role of the pathologist. Pathology 2015, 47, 1–3. [Google Scholar] [CrossRef]
- Vellekoop, A.; Loeb, S.; Folkvaljon, Y.; Stattin, P. Population based study of predictors of adverse pathology among candidates for active surveillance with Gleason 6 prostate cancer. J. Urol. 2014, 191, 350–357. [Google Scholar] [CrossRef]
- Boccon-Gibod, L.M.; Dumonceau, O.; Toublanc, M.; Ravery, V.; Boccon-Gibod, L.A. Micro-focal prostate cancer: A comparison of biopsy and radical prostatectomy specimen features. Eur. Urol. 2005, 48, 895–899. [Google Scholar] [CrossRef]
- Stolzenbach, L.F.; Rosiello, G.; Pecoraro, A.; Palumbo, C.; Luzzago, S.; Deuker, M.; Tian, Z.; Knipper, A.-S.; Pompe, R.; Zorn, K.C.; et al. Prostate Cancer Grade and Stage Misclassification in Active Surveillance Candidates: Black Versus White Patients. J. Natl. Compr. Cancer Netw. 2020, 18, 1492–1499. [Google Scholar] [CrossRef]
- Leyh-Bannurah, S.-R.; Abou-Haidar, H.; Dell’Oglio, P.; Schiffmann, J.; Tian, Z.; Heinzer, H.; Huland, H.; Graefen, M.; Budäus, L.; Karakiewicz, P.I. Primary Gleason pattern upgrading in contemporary patients with D’Amico low-risk prostate cancer: Implications for future biomarkers and imaging modalities. BJU Int. 2017, 119, 692–699. [Google Scholar] [CrossRef]
- Capitanio, U.; Karakiewicz, P.I.; Valiquette, L.; Perrotte, P.; Jeldres, C.; Briganti, A.; Gallina, A.; Suardi, N.; Cestari, A.; Guazzoni, G.F.; et al. Biopsy core number represents one of foremost predictors of clinically significant gleason sum upgrading in patients with low-risk prostate cancer. Urology 2009, 73, 1087–1091. [Google Scholar] [CrossRef]
- Chun, F.K.-H.; Briganti, A.; Shariat, S.F.; Graefen, M.; Montorsi, F.; Erbersdobler, A.; Steuber, T.; Salonia, A.; Currlin, E.; Scattoni, V.; et al. Significant upgrading affects a third of men diagnosed with prostate cancer: Predictive nomogram and internal validation. BJU Int. 2006, 98, 329–334. [Google Scholar] [CrossRef]
- Chun, F.K.-H.; Steuber, T.; Erbersdobler, A.; Currlin, E.; Walz, J.; Schlomm, T.; Haese, A.; Heinzer, H.; McCormack, M.; Huland, H.; et al. Development and internal validation of a nomogram predicting the probability of prostate cancer Gleason sum upgrading between biopsy and radical prostatectomy pathology. Eur. Urol. 2006, 49, 820–826. [Google Scholar] [CrossRef] [PubMed]
- Epstein, J.I.; Egevad, L.; Humphrey, P.A.; Montironi, R. Members of the ISUP Immunohistochemistry in Diagnostic Urologic Pathology Group. Best practices recommendations in the application of immunohistochemistry in the prostate: Report from the International Society of Urologic Pathology consensus conference. Am. J. Surg. Pathol. 2014, 38, e6–e19. [Google Scholar] [CrossRef]
- Current prostate biopsy interpretation: Criteria for cancer, atypical small acinar proliferation, high-grade prostatic intraepithelial neoplasia, and use of immunostains. Arch. Pathol. Lab. Med. 2006, 130, 835–843. [CrossRef]
- Carneiro, A.; Barbosa, Á.R.G.; Takemura, L.S.; Kayano, P.P.; Moran, N.K.S.; Chen, C.K.; Wroclawski, M.L.; Lemos, G.C.; Da Cunha, I.W.; Obara, M.T.; et al. The Role of Immunohistochemical Analysis as a Tool for the Diagnosis, Prognostic Evaluation and Treatment of Prostate Cancer: A Systematic Review of the Literature. Front. Oncol. 2018, 8, 377. [Google Scholar] [CrossRef]
- Magi-Galluzzi, C. Prostate cancer: Diagnostic criteria and role of immunohistochemistry. Mod. Pathol. 2018, 31, S12–S21. [Google Scholar] [CrossRef]
- Bokhorst, L.P.; Roobol, M.J.; Bangma, C.H.; van Leenders, G.J. Effect of pathologic revision and Ki67 and ERG immunohistochemistry on predicting radical prostatectomy outcome in men initially on active surveillance. Prostate 2017, 77, 1137–1143. [Google Scholar] [CrossRef]
- Wenzel, M.; Welte, M.N.; Theissen, L.H.; Wittler, C.; Hoeh, B.; Humke, C.; Preisser, F.; Würnschimmel, C.; Tilki, D.; Graefen, M.; et al. Comparison of Complication Rates with Antibiotic Prophylaxis with Cefpodoxime Versus Fluoroquinolones After Transrectal Prostate Biopsy. Eur. Urol. Focus 2020. [Google Scholar] [CrossRef]
- Preisser, F.; Theissen, L.; Wenzel, M.; Humke, C.; Bodelle, B.; Köllermann, J.; Kluth, L.; Banek, S.; Becker, A.; Roos, F.; et al. Performance of Combined Magnetic Resonance Imaging/Ultrasound Fusion-guided and Systematic Biopsy of the Prostate in Biopsy-naïve Patients and Patients with Prior Biopsies. Eur. Urol. Focus 2021, 7, 39–46. [Google Scholar] [CrossRef]
- Matoso, A.; Epstein, J.I. Defining clinically significant prostate cancer on the basis of pathological findings. Histopathology 2019, 74, 135–145. [Google Scholar] [CrossRef]
- Porcaro, A.B.; Inverardi, D.; Corsi, P.; Sebben, M.; Cacciamani, G.; Tafuri, A.; Processali, T.; Pirozzi, M.; Mattevi, D.; De Marchi, D.; et al. Prostate-specific antigen levels and proportion of biopsy positive cores are independent predictors of upgrading patterns in low-risk prostate cancer. Minerva Urol. Nefrol. 2020, 72, 66–71. [Google Scholar] [CrossRef]
- PPreston, M.A.; Gerke, T.; Carlsson, S.V.; Signorello, L.; Sjoberg, D.D.; Markt, S.; Kibel, A.S.; Trinh, Q.-D.; Steinwandel, M.; Blot, W.; et al. Baseline Prostate-specific Antigen Level in Midlife and Aggressive Prostate Cancer in Black Men. Eur. Urol. 2019, 75, 399–407. [Google Scholar] [CrossRef]
- Molinié, V.; Fromont, G.; Sibony, M.; Vieillefond, A.; Vassiliu, V.; Cochand-Priollet, B.; Hervé, J.M.; Lebret, T.; Baglin, A.C.; Molini, V.; et al. Diagnostic utility of a p63/alpha-methyl-CoA-racemase (p504s) cocktail in atypical foci in the prostate. Mod. Pathol. 2004, 17, 1180–1190. [Google Scholar] [CrossRef]
- Rathod, S.G.; Jaiswal, D.G.; Bindu, R.S. Diagnostic utility of triple antibody (AMACR, HMWCK and P63) stain in prostate neoplasm. J. Fam. Med. Prim. Care 2019, 8, 2651–2655. [Google Scholar] [CrossRef]
- Kristiansen, G. Markers of clinical utility in the differential diagnosis and prognosis of prostate cancer. Mod. Pathol. 2018, 31, S143–S155. [Google Scholar] [CrossRef]
- Ericson, K.J.; Wenger, H.C.; Rosen, A.M.; Kiriluk, K.J.; Gerber, G.S.; Paner, G.P.; Eggener, S.E. Prostate cancer detection following diagnosis of atypical small acinar proliferation. Can. J. Urol. 2017, 24, 8714–8720. [Google Scholar]
- Schoenfield, L.; Jones, J.S.; Zippe, C.D.; Reuther, A.M.; Klein, E.; Zhou, M.; Magi-Galluzzi, C. The incidence of high-grade prostatic intraepithelial neoplasia and atypical glands suspicious for carcinoma on first-time saturation needle biopsy, and the subsequent risk of cancer. BJU Int. 2007, 99, 770–774. [Google Scholar] [CrossRef]
- van der Poel, H.G.; Bergh, R.C.V.D.; Briers, E.; Cornford, P.; Govorov, A.; Henry, A.M.; Lam, T.B.; Mason, M.D.; Rouvière, O.; De Santis, M.; et al. Focal Therapy in Primary Localised Prostate Cancer: The European Association of Urology Position in 2018. Eur Urol. 2018, 74, 84–91. [Google Scholar] [CrossRef]
- Ahdoot, M.; Lebastchi, A.H.; Turkbey, B.; Wood, B.; Pinto, P.A. Contemporary treatments in prostate cancer focal therapy. Curr. Opin. Oncol. 2019, 31, 200–206. [Google Scholar] [CrossRef]
- Wenzel, M.; Borgmann, H.; Von Hardenberg, J.; Cash, H.; Welte, M.N.; Bründl, J.; Hoffmann, M.A.; Höfner, T.; Borkowetz, A. Acceptance, Indications And Chances Of Focal Therapy In Localized Prostate Cancer: A Real-World Perspective Of Urologists In Germany. J. Endourol. 2020, 35. [Google Scholar] [CrossRef]
- Watson, K.; Wang, C.; Yilmaz, A.; Bismar, T.A.; Trpkov, K. Use of immunohistochemistry in routine workup of prostate needle biopsies: A tertiary academic institution experience. Arch. Pathol. Lab. Med. 2013, 137, 541–545. [Google Scholar] [CrossRef]
| Variable | - | No IHC N = 256 (41.3%) | IHC N = 350 (58.7%) | p Value |
|---|---|---|---|---|
| Age | Median (IQR) | 67 (61–72) | 66 (60–72) | 0.6 |
| Prostate volume | Median (IQR) | 48 (35–70) | 50 (38–70) | 0.4 |
| PSA | Median (IQR) | 8.1 (5.3–15.8) | 7.3 (5.2–11.9) | 0.08 |
| PSA ≥ 4 ng/mL | Yes | 222 (86.7) | 293 (83.7) | 0.4 |
| No | 34 (13.3) | 57 (16.3) | ||
| Cores per biopsy | Median (IQR) | 13 (12–14) | 13 (12–14) | 0.06 |
| Positive cores per biopsy | Median (IQR) | 3 (0–7) | 1 (0–5) | <0.01 |
| Percentage of positive cores | Median (IQR) | 50 (30–80) | 40 (20–60) | <0.01 |
| Highest tumor infiltration per core | Median (IQR) | 60 (15–90) | 30 (1–60) | <0.01 |
| DRE | Non-suspicious | 109 (42.6) | 179 (51.1) | <0.01 |
| Suspicious | 102 (39.8) | 86 (24.6) | ||
| cT stage | cT1 | 109 (42.6) | 177 (50.6) | <0.01 |
| cT2 | 86 (33.6) | 74 (21.1) | ||
| cT3–4 | 16 (6.2) | 12 (3.4) | ||
| Previous biopsies | Biopsy naive | 200 (78.1) | 258 (73.7) | 0.3 |
| Repeat biopsy | 56 (21.9) | 90 (25.7) | ||
| Fusion biopsy | Yes | 131 (51.2) | 211 (60.3) | 0.03 |
| No | 125 (48.8) | 138 (39.4) | ||
| MRI lesion | PIRADS 1–2 | 2 (0.8) | 3 (0.9) | 0.03 |
| PIRADS 3 | 23 (9.0) | 55 (15.7) | ||
| PIRADS 4 | 59 (23.0) | 101 (28.9) | ||
| PIRADS 5 | 44 (17.2) | 48 (13.7) | ||
| Unknown /no MRI | 128 (50.0) | 143 (40.9) | ||
| Biopsy positive? | No | 93 (36.3) | 142 (40.6) | 0.3 |
| Yes | 163 (63.7) | 208 (59.4) | ||
| IHC | Negative/Unclear | - | 165 (47.1) | - |
| Positive | - | 185 (52.9) | ||
| Change of biopsy result after positive IHC | No | - | 104 (56.2) | - |
| Yes | - | 81 (43.8) | ||
| Gleason Score at biopsy | 6 | 8 (3.1) | 62 (17.8) | <0.01 |
| 7 | 80 (31.0) | 80 (22.9) | ||
| 8–10 | 73 (28.3) | 59 (16.9) | ||
| No PCa | 93 (36.3) | 142 (40.6) | ||
| Unknown GS | 4 (1.6) | 6 (1.7) |
| Variable | - | Changes in Biopsy Results due to Positive IHC N = 81 (43.8%) | No Changes in Biopsy Results due to Positive IHC N = 104 (56.2%) | p Value |
|---|---|---|---|---|
| Age | Median (IQR) | 67 (61–72) | 68 (64–74) | 0.18 |
| Prostate volume | Median (IQR) | 54 (38–74) | 45 (35–55) | 0.051 |
| PSA | Median (IQR) | 7.1 (5.1–10.0) | 9.8 (6.8–19.9) | <0.01 |
| Cores per biopsy | Median (IQR) | 13 (12–14) | 13 (12–14) | 0.3 |
| Positive cores per biopsy | Median (IQR) | 2 (1–4) | 6 (4–8) | <0.01 |
| Percentage of positive cores | Median (IQR) | 20 (10–30) | 50 (30–70) | <0.01 |
| Highest tumor infiltration per core | Median (IQR) | 20 (5–50) | 60 (40–80) | <0.01 |
| IHC slides per biopsy | Median (IQR) | 4 (2–8) | 4 (2–6) | 0.06 |
| DRE | non-suspicous | 59 (72.8) | 44 (42.3) | <0.01 |
| suspicous | 22 (27.2) | 54 (51.9) | ||
| cT stage | cT1 | 58 (71.6) | 44 (42.3) | <0.01 |
| cT2 | 21 (25.9) | 46 (44.2) | ||
| cT3–4 | 1 (1.2) | 8 (7.7) | ||
| Previous biopsies | Biopsy naive | 55 (67.9) | 87 (83.7) | 0.01 |
| Repeat biopsy | 26 (32.1) | 16 (15.4) | ||
| Fusion biopsy | No | 53 (65.4) | 58 (55.8) | 0.2 |
| Yes | 28 (34.6) | 46 (44.2) | ||
| Gleason Score at biopsy | 6 | 50 (61.7) | 9 (8.7) | <0.01 |
| 7 | 20 (24.7) | 50 (48.1) | ||
| ≥8–10 | 8 (9.9) | 43 (41.3) | ||
| Unknown GS | 3 (3.7) | 2 (1.9) |
| Variable | - | Changes in Biopsy Results due to Positive IHC N = 81 |
|---|---|---|
| Changes in biopsy results due to positive IHC | ASAP to PCa Gleason 6 | 43 (53.0) |
| ASAP to PCa Gleason 7 | 10 (12.3) | |
| ASAP to PCa Gleason 8–10 | 2 (2.5) | |
| Unilateral PCa to bilateral PCa Gleason 6 | 10 (12.3) | |
| Unilateral PCa to bilateral PCa Gleason 7 | 11 (13.6) | |
| Unilateral PCa to bilateral PCa Gleason 8–10 | 4 (4.9) | |
| Unilateral PCa to bilateral PCa Gleason unknown | 1 (1.2) | |
| Changes in biopsy results due to positive IHC | ASAP to PCa | 55 (67.9) |
| Unilateral PCa to bilateral PCa | 26 (32.1) | |
| Therapy after biopsy changes due to positive IHC | RP | 42 (51.9) |
| RT | 7 (8.6) | |
| AS | 27 (33.3) | |
| ADT/WW | 3 (3.7) | |
| Unknown | 2 (2.5) | |
| Pathology at RP in patients with changed biopsy results due to positive IHC | pT2 + Gleason 6 | 15 (35.7) |
| pT3 and/or Gleason 7–10 | 25 (59.5) | |
| Regression/unknown | 2 (4.8) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mandel, P.; Wenzel, M.; Hoeh, B.; Welte, M.N.; Preisser, F.; Inam, T.; Wittler, C.; Humke, C.; Köllermann, J.; Wild, P.; et al. Immunohistochemistry for Prostate Biopsy—Impact on Histological Prostate Cancer Diagnoses and Clinical Decision Making. Curr. Oncol. 2021, 28, 2123-2133. https://doi.org/10.3390/curroncol28030197
Mandel P, Wenzel M, Hoeh B, Welte MN, Preisser F, Inam T, Wittler C, Humke C, Köllermann J, Wild P, et al. Immunohistochemistry for Prostate Biopsy—Impact on Histological Prostate Cancer Diagnoses and Clinical Decision Making. Current Oncology. 2021; 28(3):2123-2133. https://doi.org/10.3390/curroncol28030197
Chicago/Turabian StyleMandel, Philipp, Mike Wenzel, Benedikt Hoeh, Maria N. Welte, Felix Preisser, Tahir Inam, Clarissa Wittler, Clara Humke, Jens Köllermann, Peter Wild, and et al. 2021. "Immunohistochemistry for Prostate Biopsy—Impact on Histological Prostate Cancer Diagnoses and Clinical Decision Making" Current Oncology 28, no. 3: 2123-2133. https://doi.org/10.3390/curroncol28030197
APA StyleMandel, P., Wenzel, M., Hoeh, B., Welte, M. N., Preisser, F., Inam, T., Wittler, C., Humke, C., Köllermann, J., Wild, P., Würnschimmel, C., Tilki, D., Graefen, M., Kluth, L. A., Karakiewicz, P. I., Chun, F. K.-H., & Becker, A. (2021). Immunohistochemistry for Prostate Biopsy—Impact on Histological Prostate Cancer Diagnoses and Clinical Decision Making. Current Oncology, 28(3), 2123-2133. https://doi.org/10.3390/curroncol28030197





