Validation of the Upper Limb Functional Index on Breast Cancer Survivor
Abstract
1. Introduction
2. Materials and Methods
2.1. Design
2.2. Participants, Setting, and Procedure
2.3. Statistics
2.3.1. Structural Validity
2.3.2. Reliability: Internal Consistency
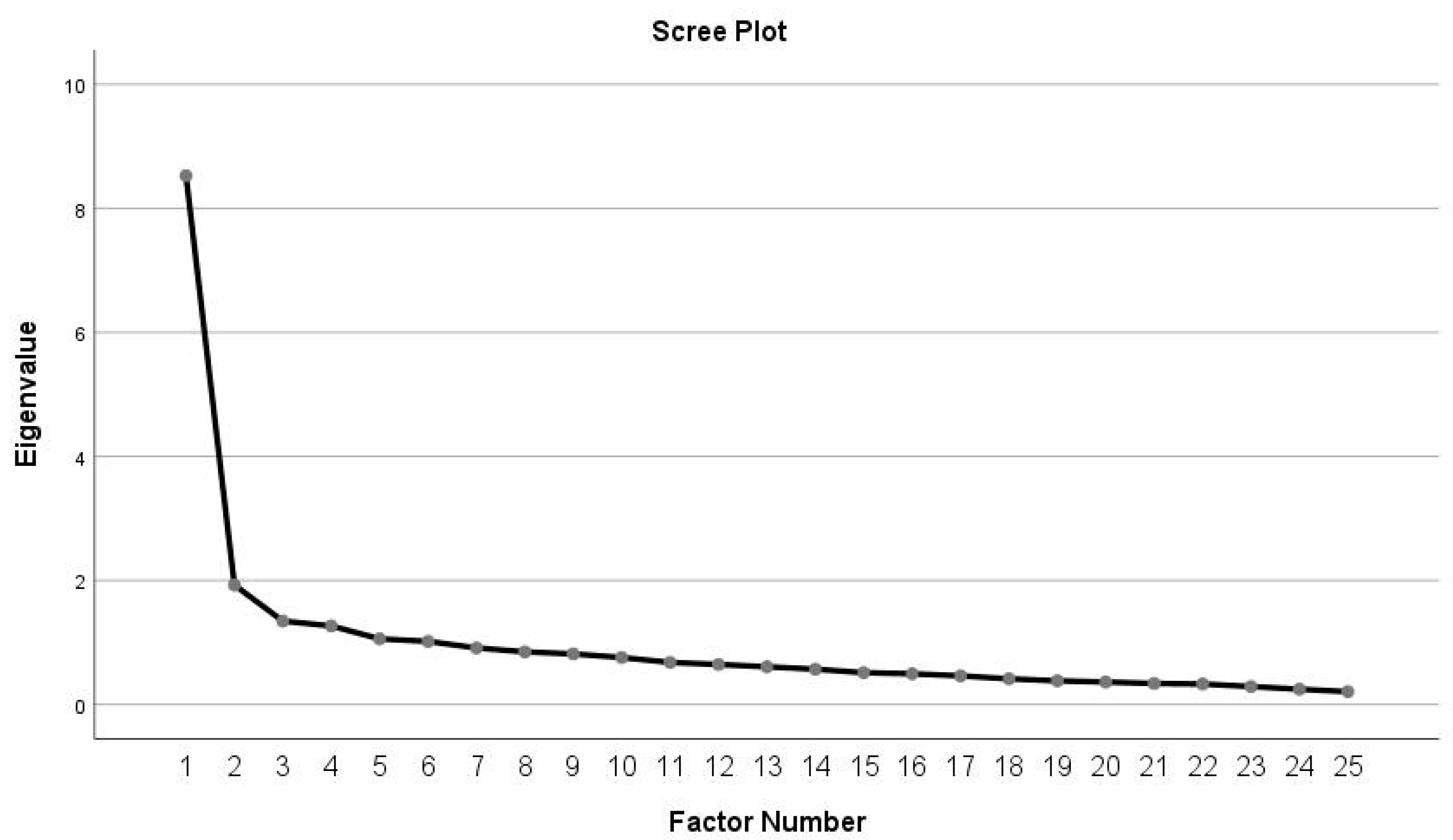
2.3.3. Factor Analysis
3. Results
3.1. Sample Description
3.2. Structural Validity
3.3. New 14-Item Model
4. Discussion
4.1. Structural Validity
4.2. Reliability: Internal Consistency
4.3. Factor Analysis
4.4. Short Version
4.5. Clinical Implications
4.6. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- WHO | Breast Cancer: Prevention and Control. Available online: http://www.who.int/cancer/detection/breastcancer/en/ (accessed on 13 May 2019).
- Sagen, A.; Kaaresen, R.; Sandvik, L.; Thune, I.; Risberg, M.A. Upper Limb Physical Function and Adverse Effects after Breast Cancer Surgery: A Prospective 2.5-Year Follow-up Study and Preoperative Measures. Arch. Phys. Med. Rehabil 2014, 95, 875–881. [Google Scholar] [CrossRef]
- Schmitz, K.H.; Speck, R.M.; Rye, S.A.; DiSipio, T.; Hayes, S.C. Prevalence of Breast Cancer Treatment Sequelae over 6 Years of Follow-up: The Pulling Through Study. Cancer 2012, 118, 2217–2225. [Google Scholar] [CrossRef]
- Yang, E.J.; Park, W.-B.; Seo, K.S.; Kim, S.-W.; Heo, C.-Y.; Lim, J.-Y. Longitudinal Change of Treatment-Related Upper Limb Dysfunction and Its Impact on Late Dysfunction in Breast Cancer Survivors: A Prospective Cohort Study. J. Surg. Oncol. 2010, 101, 84–91. [Google Scholar] [CrossRef]
- Harris, S.R. Axillary Web Syndrome in Breast Cancer: A Prevalent But Under-Recognized Postoperative Complication. Breast Care 2018, 13, 132–135. [Google Scholar] [CrossRef] [PubMed]
- Hagstrom, A.D.; Shorter, K.A.; Marshall, P.W.M. Changes in Unilateral Upper Limb Muscular Strength and Electromyographic Activity After a 16-Week Strength Training Intervention in Survivors of Breast Cancer. J. Strength Cond. Res. 2019, 33, 225–233. [Google Scholar] [CrossRef]
- Garratt, A. Patient Reported Outcome Measures in Trials. BMJ 2009, 338, a2597. [Google Scholar] [CrossRef] [PubMed]
- Cella, D.; Yount, S.; Rothrock, N.; Gershon, R.; Cook, K.; Reeve, B.; Ader, D.; Fries, J.F.; Bruce, B.; Rose, M.; et al. The Patient-Reported Outcomes Measurement Information System (PROMIS): Progress of an NIH Roadmap Cooperative Group during Its First Two Years. Med Care 2007, 45, S3–S11. [Google Scholar] [CrossRef]
- Fayers, P.M.; Machin, D. Quality of Life: The Assessment, Analysis and Interpretation of Patient-Reported Outcomes; John Wiley & Sons: Hoboken, NJ, USA, 2013; ISBN 1-118-69945-9. [Google Scholar]
- Angst, F.; Schwyzer, H.-K.; Aeschlimann, A.; Simmen, B.R.; Goldhahn, J. Measures of Adult Shoulder Function: Disabilities of the Arm, Shoulder, and Hand Questionnaire (DASH) and Its Short Version (QuickDASH), Shoulder Pain and Disability Index (SPADI), American Shoulder and Elbow Surgeons (ASES) Society Standardized Shoulder Assessment Form, Constant (Murley) Score (CS), Simple Shoulder Test (SST), Oxford Shoulder Score (OSS), Shoulder Disability Questionnaire (SDQ), and Western Ontario Shoulder Instability Index (WOSI). Arthritis Care Res. 2011, 63 (Suppl. 11), S174–S188. [Google Scholar] [CrossRef]
- Williams, A.E.; Rapport, F.; Russell, I.T.; Hutchings, H.A. Psychometric Development of the Upper Limb Lymphedema Quality of Life Questionnaire Demonstrated the Patient-Reported Outcome Measure to Be a Robust Measure for Breast Cancer-Related Lymphedema. J. Clin. Epidemiol. 2018, 100, 61–70. [Google Scholar] [CrossRef]
- Dawson, J.; Rogers, K.; Fitzpatrick, R.; Carr, A. The Oxford Shoulder Score Revisited. Arch. Orthop. Trauma Surg. 2009, 129, 119–123. [Google Scholar] [CrossRef]
- Hudak, P.L.; Amadio, P.C.; Bombardier, C. Development of an Upper Extremity Outcome Measure: The DASH (Disabilities of the Arm, Shoulder and Hand) [Corrected]. The Upper Extremity Collaborative Group (UECG). Am. J. Ind. Med. 1996, 29, 602–608. [Google Scholar] [CrossRef]
- Gabel, C.P.; Michener, L.A.; Burkett, B.; Neller, A. The Upper Limb Functional Index: Development and Determination of Reliability, Validity, and Responsiveness. J. Hand Ther. 2006, 19, 328–348, quiz 349. [Google Scholar] [CrossRef] [PubMed]
- Gabel, C.P.; Michener, L.A.; Melloh, M.; Burkett, B. Modification of the Upper Limb Functional Index to a Three-Point Response Improves Clinimetric Properties. J. Hand Ther. 2010, 23, 41–52. [Google Scholar] [CrossRef]
- Harrington, S.; Michener, L.A.; Kendig, T.; Miale, S.; George, S.Z. Patient-Reported Upper Extremity Outcome Measures Used in Breast Cancer Survivors: A Systematic Review. Arch. Phys. Med. Rehabil. 2014, 95, 153–162. [Google Scholar] [CrossRef] [PubMed]
- Jay, M.; Creelman, B.; Baliski, C. Patient Reported Outcomes Associated with Surgical Intervention for Breast Cancer. Am. J. Surg. 2019, 219, 816–822. [Google Scholar] [CrossRef]
- Coster, S.; Poole, K.; Fallowfield, L.J. The Validation of a Quality of Life Scale to Assess the Impact of Arm Morbidity in Breast Cancer Patients Post-Operatively. Breast Cancer Res. Treat. 2001, 68, 273–282. [Google Scholar] [CrossRef]
- Nesvold, I.-L.; Fosså, S.D.; Naume, B.; Dahl, A.A. Kwan’s Arm Problem Scale: Psychometric Examination in a Sample of Stage II Breast Cancer Survivors. Breast Cancer Res. Treat. 2009, 117, 281–288. [Google Scholar] [CrossRef]
- Wingate, L. Efficacy of Physical Therapy for Patients Who Have Undergone Mastectomies. A Prospective Study. Phys. Ther. 1985, 65, 896–900. [Google Scholar] [CrossRef]
- Gabel, C.P. Development and Initial Validation of a New Regional Outcome Measure: The Upper Limb Disability Questionnaire (ULDQ), 2003. Available online: https://researchers.cdu.edu.au/en/studentTheses/development-and-initial-validation-of-a-new-regional-outcome-meas (accessed on 12 December 2022).
- LeBlanc, M.; Stineman, M.; DeMichele, A.; Stricker, C.; Mao, J.J. Validation of QuickDASH Outcome Measure in Breast Cancer Survivors for Upper Extremity Disability. Arch. Phys. Med. Rehabil. 2014, 95, 493–498. [Google Scholar] [CrossRef]
- Binkley, J.M.; Stratford, P.; Kirkpatrick, S.; Farley, C.R.; Okoli, J.; Gabram, S. Estimating the Reliability and Validity of the Upper Extremity Functional Index in Women After Breast Cancer Surgery. Clin. Breast Cancer 2018, 18, e1261–e1267. [Google Scholar] [CrossRef]
- Torres-Lacomba, M.; Sánchez-Sánchez, B.; Prieto-Gómez, V.; Pacheco-da-Costa, S.; Yuste-Sánchez, M.J.; Navarro-Brazález, B.; Gutiérrez-Ortega, C. Spanish Cultural Adaptation and Validation of the Shoulder Pain and Disability Index, and the Oxford Shoulder Score after Breast Cancer Surgery. Health Qual. Life Outcomes 2015, 13, 63. [Google Scholar] [CrossRef] [PubMed]
- Roldán-Jiménez, C.; Martín-Martín, J.; Pajares, B.; Ribelles, N.; Alba, E.; Cuesta-Vargas, A.I. Factors Associated with Upper Limb Function in Breast Cancer Survivors. PM R 2021, 15, 151–156. [Google Scholar] [CrossRef] [PubMed]
- Roldán-Jiménez, C.; Pajares, B.; Ruiz-Medina, S.; Trinidad-Fernández, M.; González-Sánchez, M.; Ribelles, N.; García-Almeida, J.M.; Ríos-López, M.J.; Alba, E.; Cuesta-Vargas, A.I. Design and Implementation of a Standard Care Programme of Therapeutic Exercise and Education for Breast Cancer Survivors. Support. Care Cancer 2021, 30, 1243–1251. [Google Scholar] [CrossRef] [PubMed]
- Cuesta-Vargas, A.I.; Buchan, J.; Pajares, B.; Alba, E.; Trinidad-Fernández, M.; Ruiz-Medina, S.; García-Almeida, J.M.; Ríos-López, M.J.; Roldán-Jiménez, C. Energy System Assessment in Survivors of Breast Cancer. Phys. Ther. 2020, 100, 438–446. [Google Scholar] [CrossRef] [PubMed]
- Escriche-Escuder, A.; Trinidad-Fernández, M.; Pajares, B.; Iglesias-Campos, M.; Alba, E.; Cuesta-Vargas, A.I.; Roldán-Jiménez, C. Ultrasound Use in Metastatic Breast Cancer to Measure Body Composition Changes Following an Exercise Intervention. Sci. Rep. 2021, 11, 8858. [Google Scholar] [CrossRef] [PubMed]
- Cuesta-Vargas, A.I.; Gabel, P.C. Cross-Cultural Adaptation, Reliability and Validity of the Spanish Version of the Upper Limb Functional Index. Health Qual. Life Outcomes 2013, 11, 126. [Google Scholar] [CrossRef] [PubMed]
- Kaiser, H.F. An Index of Factorial Simplicity. Psychometrika 1974, 39, 31–36. [Google Scholar] [CrossRef]
- Bartlett, M.G.; Bartlett, M.; Bartlett, M.S.; Bartlett, M.S.; Bartlett, M.S. A Note on the Multiplying Factors for Various Chi Square Approximations. J. R. Stat. Soc. Ser. B Methodol. 1954, 16, 296–298. [Google Scholar]
- Costello, A.B.; Osborne, J.W. Best Practices in Exploratory Factor Analysis: Four Recommendations for Getting the Most From Your Analysis. Pract. Assess. Res. Eval. 2005, 10, 7. [Google Scholar]
- Hair, J.F. Análisis Multivariante; Pearson Educación: London, UK, 1999; ISBN 978-84-8322-035-1. [Google Scholar]
- Terwee, C.B.; Bot, S.D.M.; de Boer, M.R.; van der Windt, D.A.W.M.; Knol, D.L.; Dekker, J.; Bouter, L.M.; de Vet, H.C.W. Quality Criteria Were Proposed for Measurement Properties of Health Status Questionnaires. J Clin. Epidemiol. 2007, 60, 34–42. [Google Scholar] [CrossRef]
- Cronbach, L.J. Coefficient Alpha and the Internal Structure of Tests. Psychometrika 1951, 16, 297–334. [Google Scholar] [CrossRef]
- Schermelleh-Engel, K.; Moosbrugger, H.; Müller, H. Evaluating the Fit of Structural Equation Models: Tests of Significance and Descriptive Goodness-of-Fit Measures. Methods Psychol. Res. Online 2003, 8, 23–74. [Google Scholar]
- Hu, L.; Bentler, P.M. Cutoff Criteria for Fit Indexes in Covariance Structure Analysis: Conventional Criteria versus New Alternatives. Struct. Equ. Model. A Multidiscip. J. 1999, 6, 1–55. [Google Scholar] [CrossRef]
- IBM SPSS Statistics. Available online: http://www-01.ibm.com/software/analytics/spss/products/statistics/ (accessed on 10 October 2022).
- Jöreskog, K.G.; Sörbom, D. LISREL 10 for Windows [Computer Software]; Scientific Software International, Inc.: Skokie, IL, USA, 2018. [Google Scholar]
- Davis, L.E.; Bubis, L.D.; Mahar, A.L.; Li, Q.; Sussman, J.; Moody, L.; Barbera, L.; Holloway, C.M.; Coburn, N.G. Patient-Reported Symptoms after Breast Cancer Diagnosis and Treatment: A Retrospective Cohort Study. Eur. J. Cancer 2018, 101, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Bravini, E.; Franchignoni, F.; Giordano, A.; Sartorio, F.; Ferriero, G.; Vercelli, S.; Foti, C. Classical Test Theory and Rasch Analysis Validation of the Upper Limb Functional Index in Subjects with Upper Limb Musculoskeletal Disorders. Arch. Phys. Med. Rehabil. 2015, 96, 98–104. [Google Scholar] [CrossRef]
- Gabel, C.P.; Yelland, M.; Melloh, M.; Burkett, B. A Modified QuickDASH-9 Provides a Valid Outcome Instrument for Upper Limb Function. BMC Musculoskelet. Disord. 2009, 10, 161. [Google Scholar] [CrossRef] [PubMed]
- Tonga, E.; Durutürk, N.; Gabel, P.C.; Tekindal, A. Cross-Cultural Adaptation, Reliability and Validity of the Turkish Version of the Upper Limb Functional Index (ULFI). J. Hand Ther. 2015, 28, 279–284, quiz 285. [Google Scholar] [CrossRef]
- Arooj, A.; Amjad, F.; Tanveer, F.; Arslan, A.U.; Ahmad, A.; Gilani, S.A. Translation, Cross-Cultural Adaptation and Psychometric Properties of Urdu Version of Upper Limb Functional Index; a Validity and Reliability Study. BMC Musculoskelet. Disord. 2022, 23, 691. [Google Scholar] [CrossRef] [PubMed]
- Luque-Suarez, A.; Rondon-Ramos, A.; Fernandez-Sanchez, M.; Roach, K.E.; Morales-Asencio, J.M. Spanish Version of SPADI (Shoulder Pain and Disability Index) in Musculoskeletal Shoulder Pain: A New 10-Items Version after Confirmatory Factor Analysis. Health Qual. Life Outcomes 2016, 14, 32. [Google Scholar] [CrossRef]
- Hidding, J.T.; Beurskens, C.H.G.; van der Wees, P.J.; van Laarhoven, H.W.M.; Nijhuis-van der Sanden, M.W.G.N. Treatment Related Impairments in Arm and Shoulder in Patients with Breast Cancer: A Systematic Review. PLoS ONE 2014, 9, e96748. [Google Scholar] [CrossRef]
- Larsson, I.L.; Jönsson, C.; Olsson, A.C.; Gard, G.; Johansson, K. Women’s Experience of Physical Activity Following Breast Cancer Treatment. Scand. J. Caring Sci. 2008, 22, 422–429. [Google Scholar] [CrossRef]
- Gencay Can, A.; Can, S.S.; Ekşioğlu, E.; Çakcı, F.A. Is Kinesiophobia Associated with Lymphedema, Upper Extremity Function, and Psychological Morbidity in Breast Cancer Survivors? Turk. J. Phys. Med. Rehabil. 2019, 65, 139–146. [Google Scholar] [CrossRef] [PubMed]
- De Groef, A.; Meeus, M.; De Vrieze, T.; Vos, L.; Van Kampen, M.; Christiaens, M.-R.; Neven, P.; Geraerts, I.; Devoogdt, N. Pain Characteristics as Important Contributing Factors to Upper Limb Dysfunctions in Breast Cancer Survivors at Long Term. Musculoskelet. Sci. Pract. 2017, 29, 52–59. [Google Scholar] [CrossRef] [PubMed]
- Smoot, B.; Paul, S.M.; Aouizerat, B.E.; Dunn, L.; Elboim, C.; Schmidt, B.; Hamolsky, D.; Levine, J.D.; Abrams, G.; Mastick, J.; et al. Predictors of Altered Upper Extremity Function During the First Year After Breast Cancer Treatment. Am. J. Phys. Med. Rehabil. 2016, 95, 639–655. [Google Scholar] [CrossRef] [PubMed]
- Stubblefield, M.D.; McNeely, M.L.; Alfano, C.M.; Mayer, D.K. A Prospective Surveillance Model for Physical Rehabilitation of Women with Breast Cancer: Chemotherapy-Induced Peripheral Neuropathy. Cancer 2012, 118, 2250–2260. [Google Scholar] [CrossRef]
- Shamley, D.; Robb, K. An Early Warning Surveillance Programme for Detecting Upper Limb Deterioration after Treatment for Breast Cancer: A Novel Technology Supported System. BMC Cancer 2015, 15, 635. [Google Scholar] [CrossRef]
- Hamasaki, T.; Demers, L.; Filiatrault, J.; Aubin, G. A Cross-Cultural Adaptation of the Upper Limb Functional Index in French Canadian. J. Hand Ther. 2014, 27, 247–252, quiz 253. [Google Scholar] [CrossRef]
- Sartorio, F.; Moroso, M.; Vercelli, S.; Bravini, E.; Medina, M.E.; Spalek, R.; Ferriero, G. Cross-cultural adaptation, and validity of the italian version of the Upper Limb Functional Index (ULFI-I). G. Ital. Med. Lav. Ergon. 2015, 37, 115–119. [Google Scholar]
| Mean (SD) | Min–Max | |
|---|---|---|
| Age (years) | 51.64 (9.10) | 32.0–69.0 |
| BMI (Kg/m2) | 27.97 (5.39) | 17.60–43.50 |
| Years from diagnosis | 2.43 (2.16) | 0–13 |
| Surgical intervention | Percentage (n) | |
| Lumpectomy | 11% (23) | |
| Lumpectomy and sentinel lymph node | 38% (83) | |
| Lumpectomy and axillary dissection | 24% (52) | |
| Mastectomy | 27% (58) | |
| Cancer treatment | ||
| Chemotherapy | 88.5% (191) | |
| Radiotherapy | 90.6% (195) | |
| Hormone therapy | 82.2% (190) | |
| Monoclonal antibody | 29.3% (63) | |
| Current treatment | ||
| None | 23% (49) | |
| Radiotherapy | 6% (13) | |
| Monoclonal antibody | 6% (13) | |
| Hormone therapy | 65% (140) |
| Item Number | Item Description | Item Average Score (SD) | Inter-Item Correlation | Communalities | |
|---|---|---|---|---|---|
| 25 Item (Original Version) | 14 Item (Short Version) | ||||
| 1 | Stays at home most of the time | 0.18 (0.34) | 0.516 | 0.247 | |
| 2 | Changes positions frequently | 0.38 (0.43) | 0.621 | 0.357 | 0.483 |
| 3 | Avoids heavy jobs | 0.59 (0.45) | 0.541 | 0.271 | |
| 4 | Rests more often | 0.52 (0.45) | 0.647 | 0.388 | 0.375 |
| 5 | Gets others to do things | 0.29 (0.37) | 0.506 | 0.237 | |
| 6 | Pain is constant | 0.26 (0.38) | 0.702 | 0.456 | 0.535 |
| 7 | Lifting and carrying | 0.47 (0.44) | 0.703 | 0.458 | 0.471 |
| 8 | Appetite affected | 0.18 (0.35) | 0.399 | 0.147 | |
| 9 | Walking/normal recreation/sport | 0.35 (0.41) | 0.584 | 0.316 | 0.321 |
| 10 | Home/family duties and chores | 0.33 (0.40) | 0.771 | 0.551 | 0.733 |
| 11 | Sleeps less well | 0.46 (0.45) | 0.480 | 0.214 | |
| 12 | Assistance with personal care and hygiene | 0.02 (0.14) | 0.352 | 0.115 | |
| 13 | Regular daily activities, work/social | 0.31 (0.41) | 0.659 | 0.402 | 0.391 |
| 14 | More irritable/bad tempered | 0.29 (0.40) | 0.482 | 0.215 | |
| 15 | Feeling weaker or stiffer | 0.38 (0.42) | 0.729 | 0.493 | 0.553 |
| 16 | Transport independence | 0.08 (0.22) | 0.398 | 0.147 | |
| 17 | Arm in shirt sleeve/dressing | 0.15 (0.30) | 0.531 | 0.261 | |
| 18 | Writing/using keyboard or mouse | 0.06 (0.21) | 0.491 | 0.223 | |
| 19 | Doing things at/above shoulder height | 0.22 (0.34) | 0.618 | 0.354 | 0.486 |
| 20 | Eating and using utensils | 0.05 (0.18) | 0.434 | 0.175 | |
| 21 | Holding or moving dense objects | 0.21 (0.36) | 0.657 | 0.400 | 0.408 |
| 22 | Drops things, causing minor accidents | 0.16 (0.32) | 0.572 | 0.303 | 0.299 |
| 23 | Uses other arm more often | 0.48 (0.46) | 0.588 | 0.321 | 0.323 |
| 24 | Difficult button key coins taps | 0.23 (0.37) | 0.629 | 0.357 | 0.337 |
| 25 | Difficult opening, holding, pushing or pressing | 0.42 (0.42) | 0.698 | 0.452 | 0.468 |
| Psychometric Properties | ULFI | 25-Item Model (Original Version) | 14-Item Model (Short Version) |
|---|---|---|---|
| AFE | KMO | 0.889 | 0.920 |
| Barlett’s test | |||
| Chi-squared | 2087.167 | 1171.591 | |
| Df; p | 300; <0.000 | 91; <0.000 | |
| CFA | CFI | 0.802 | 0.905 |
| RMSEA | 0.075 | 0.069 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martín-Martín, J.; Pajares-Hachero, B.; Alba-Conejo, E.; Ribelles, N.; Cuesta-Vargas, A.I.; Roldán-Jiménez, C. Validation of the Upper Limb Functional Index on Breast Cancer Survivor. Int. J. Environ. Res. Public Health 2023, 20, 4997. https://doi.org/10.3390/ijerph20064997
Martín-Martín J, Pajares-Hachero B, Alba-Conejo E, Ribelles N, Cuesta-Vargas AI, Roldán-Jiménez C. Validation of the Upper Limb Functional Index on Breast Cancer Survivor. International Journal of Environmental Research and Public Health. 2023; 20(6):4997. https://doi.org/10.3390/ijerph20064997
Chicago/Turabian StyleMartín-Martín, Jaime, Bella Pajares-Hachero, Emilio Alba-Conejo, Nuria Ribelles, Antonio I. Cuesta-Vargas, and Cristina Roldán-Jiménez. 2023. "Validation of the Upper Limb Functional Index on Breast Cancer Survivor" International Journal of Environmental Research and Public Health 20, no. 6: 4997. https://doi.org/10.3390/ijerph20064997
APA StyleMartín-Martín, J., Pajares-Hachero, B., Alba-Conejo, E., Ribelles, N., Cuesta-Vargas, A. I., & Roldán-Jiménez, C. (2023). Validation of the Upper Limb Functional Index on Breast Cancer Survivor. International Journal of Environmental Research and Public Health, 20(6), 4997. https://doi.org/10.3390/ijerph20064997








