Scrutinizing the Profile and Risk Factors of Suicide: A Perspective from a Case–Control Study Focused on a Northern Region of Spain
Abstract
1. Introduction
2. Materials and Methods
2.1. Selection of Cases and Controls
2.2. Data Collection
2.3. Data Analysis
2.4. Ethical Aspects
3. Results
3.1. Social Factors
3.2. Residence Characteristics
3.3. Medico-Legal Features
3.4. Medical History
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Geneva: World Health Organization (WHO). Suicide Wordwide in 2019: Global Health Estimates. Available online: https://www.who.int/publications/i/item/9789240026643 (accessed on 12 June 2022).
- OECD/European Union. Health at a Glance: Europe 2018: State of Health in the EU Cycle; OECD Publishing/European Union: Paris, Brussels, 2018. [Google Scholar] [CrossRef]
- Defunciones Según la Causa de Muerte. Instituto Nacional De Estadística. Available online: https://www.ine.es/jaxiT3/Datos.htm?t=7947#!tabs-grafico (accessed on 15 May 2022).
- De Leo, D. Can we rely on suicide mortality data? Crisis J. Crisis Interv. Suicide Prev. 2015, 36, 1–3. [Google Scholar] [CrossRef] [PubMed]
- Tøllefsen, I.M.; Hem, E.; Ekeberg. The reliability of suicide statistics: A systematic review. BMC Psychiatry 2012, 12, 9. [Google Scholar] [CrossRef] [PubMed]
- Santurtún, A.; Almendra, R.; Silva, G.L.; Fdez-Arroyabe, P.; Santurtún, M.; Santana, P. Suicide and apparent temperature in the two capitals cities in the iberian peninsula. Soc. Sci. Med. 2020, 265, 113411. [Google Scholar] [CrossRef] [PubMed]
- Cornelius, S.; Berry, T.; Goodrich, A.; Shiner, B.; Riblet, N. The Effect of Meteorological, Pollution, and Geographic Exposures on Death by Suicide: A Scoping Review. Int. J. Environ. Res. Public Health 2021, 18, 7809. [Google Scholar] [CrossRef]
- López-Contreras, N.; Rodríguez-Sanz, M.; Novoa, A.; Borrell, C.; Muñiz, J.M.; Gotsens, M. Socioeconomic inequalities in suicide mortality in Barcelona during the economic crisis (2006–2016): A time trend study. BMJ Open 2019, 9, e028267. [Google Scholar] [CrossRef]
- Koirala, S.; Subedi, K.; Subedi, N. Unnatural Deaths among Autopsy Cases Brought at Tertiary Care Hospital of Western Nepal during COVID-19 Pandemic Period: A Descriptive Cross-sectional Study. JNMA J. Nepal Med. Assoc. 2021, 59, 1293–1296. [Google Scholar] [CrossRef]
- Mullins, N.; Kang, J.; Campos, A.I.; Coleman, J.R.; Edwards, A.C.; Galfalvy, H.; Levey, D.F.; Lori, A.; Shabalin, A.; Starnawska, A.; et al. Dissecting the Shared Genetic Architecture of Suicide Attempt, Psychiatric Disorders, and Known Risk Factors. Biol. Psychiatry 2021, 91, 313–327. [Google Scholar] [CrossRef]
- de Mendonça Lima, C.A.; De Leo, D.; Ivbijaro, G.; Svab, I. Suicide prevention in older adults. Asia-Pac. Psychiatry 2021, 13, e12473. [Google Scholar] [CrossRef]
- Rojas, I.; Pemjan, A.; Caprile, M.A.; Gómez, A.; Opazo, R.; Valderrama, S.; Rodríguez, J. Programa nacional de prevención del suicidio—Orientaciones para su Implementación. Ministerio de Salud de Chile. MINSAL. Dep. De Salud Ment. Div. De Prevención Y Control De Enferm. Subsecr. De Salud Pública 2013, 32, 1–83. [Google Scholar]
- Santa Mina, E.E.; Gallop, R.M. Childhood sexual and physical abuse and adult self-harm and suicidal behaviour: A literature review. Can J. Psychiatry 1998, 43, 793–800. [Google Scholar] [CrossRef]
- Molnar, B.E.; Berkman, L.F.; Buka, S. Psychopathology, childhood sexual abuse and other childhood adversities: Relative links to subsequent suicidal behaviour in the US. Psychol. Med. 2001, 31, 965–977. [Google Scholar] [CrossRef]
- Conejero, I.; Olié, E.; Calati, R.; Ducasse, D.; Courtet, P. Psychological Pain, Depression, and Suicide: Recent Evidences and Future Directions. Curr. Psychiatry Rep. 2018, 20, 33. [Google Scholar] [CrossRef] [PubMed]
- Stanley, I.H.; Boffa, J.W.; Rogers, M.L.; Hom, M.A.; Albanese, B.J.; Chu, C.; Capron, D.W.; Schmidt, N.B.; Joiner, T.E. Anxiety sensitivity and suicidal ideation/suicide risk: A meta-analysis. J. Consult. Clin. Psychol. 2018, 86, 946–960. [Google Scholar] [CrossRef]
- Racine, M. Chronic pain and suicide risk: A comprehensive review. Prog. Neuro-Psychopharmacol. Biol. Psychiatry 2018, 87, 269–280. [Google Scholar] [CrossRef] [PubMed]
- Cano-Montalbán, I.; Quevedo-Blasco, R. Sociodemographic Variables Most Associated with Suicidal Behaviour and Suicide Methods in Europe and America. A Systematic Review. Eur. J. Psychol. Appl. Leg. Context 2018, 10, 15–25. [Google Scholar] [CrossRef]
- National Institute of Mental Health. Frequently Asked Questions about Suicide. Available online: https://www.nimh.nih.gov/health/publications/suicide-faq (accessed on 18 June 2022).
- Hu, G.; Wilcox, H.C.; Wissow, L.; Baker, S.P. Mid-life suicide: An increasing problem in U.S. Whites, 1999-2005. Am. J. Prev. Med. 2008, 35, 589–593. [Google Scholar] [CrossRef] [PubMed]
- Stone, D.M.; Holland, K.M.; Bartholow, B.N.; Crosby, A.E.; Davis, S.P.; Wilkins, N. Prevención del Suicidio: Paquete Técnico de Políticas, Programas y Prácticas. Available online: https://www.cdc.gov/suicide/pdf/suicideTechnicalPackage-es.pdf (accessed on 18 June 2022).
- Chan, W.S.; Yip, P.S.; Wong, P.W.; Chen, E.Y. Suicide and unemployment: What are the missing links? Arch. Suicide Res. 2007, 11, 327–335. [Google Scholar] [CrossRef]
- Doupnik, S.K.; Rudd, B.; Schmutte, T.; Worsley, D.; Bowden, C.F.; McCarthy, E.; Eggan, E.; Bridge, J.A.; Marcus, S.C. Association of Suicide Prevention Interventions With Subsequent Suicide Attempts, Linkage to Follow-up Care, and Depression Symptoms for Acute Care Settings. JAMA Psychiatry 2020, 77, 1021–1030. [Google Scholar] [CrossRef]
- Rihmer, Z.; Németh, A.; Kurimay, T.; Perczel-Forintos, D.; Purebl, G.; Döme, P. Recognition, care and prevention of suicidal behaviour in adults. Psychiatr Hung 2017, 32, 4–40. [Google Scholar]
- Ley Orgánica 15/1999, de 13 de Diciembre, de Protección de Datos de Carácter Personal. Available online: https://parlamento-cantabria.es/sites/default/files/dossieres-legislativos/LO%2015_1999%20CON%20MARCADORES.pdf. (accessed on 20 June 2022).
- Denney, J.T. Family and Household Formations and Suicide in the United States. J. Marriage Fam. 2010, 72, 202–213. [Google Scholar] [CrossRef]
- Shaw, R.J.; Cullen, B.; Graham, N.; Lyall, D.M.; Mackay, D.; Okolie, C.; Pearsall, R.; Ward, J.; John, A.; Smith, D.J. Living alone, loneliness and lack of emotional support as predictors of suicide and self-harm: A nine-year follow up of the UK Biobank cohort. J. Affect. Disord. 2020, 279, 316–323. [Google Scholar] [CrossRef] [PubMed]
- Kaufman, J.A.; Salas-Hernández, L.K.; Komro, K.A.; Livingston, M.D. Effects of increased minimum wages by unemployment rate on suicide in the USA. J. Epidemiol. Community Health 2020, 74, 219–224. [Google Scholar] [CrossRef] [PubMed]
- Värnik, P. Suicide in the world. Int. J. Environ. Res. Public Health 2012, 9, 760–771. [Google Scholar] [CrossRef] [PubMed]
- Suescún Arregoces, J.D.; Caballero-Domínguez, C.; Fuentes López, C.; Ceballos Ospino, G. Características sociodemográficas y suicidios consumados en las ciudades de Santa Marta y Bucaramanga (Colombia): Un estudio retrospectivo de género 2010-2014. Cuad. Hispanoam. De Psicol. 2017, 17, 19–28. [Google Scholar] [CrossRef]
- Kposowa, A.J. Marital status and suicide in the National Longitudinal Mortality Study. J. Epidemiol. Community Health 2000, 54, 254–261. [Google Scholar] [CrossRef] [PubMed]
- Suso-Ribera, C.; Mora-Marín, R.; Hernández-Gaspar, C.; Pardo-Guerra, L.; Pardo-Guerra, M.; Belda-Martínez, A.; Palmer-Viciedo, R. El suicidio en Castellón entre 2009 y 2015: ¿ayudan los factores sociodemográficos y psiquiátricos a entender las diferencias entre los ámbitos urbano y rural? Rev. De Psiquiatr. Y Salud Ment. 2017, 11, 4–11. [Google Scholar] [CrossRef]
- Bachmann, S. Epidemiology of Suicide and the Psychiatric Perspective. Int. J. Environ. Res. Public Health 2018, 15, 1425. [Google Scholar] [CrossRef]
- König, D.; Swoboda, P.; Cramer, R.J.; Krall, C.; Postuvan, V.; Kapusta, N.D. Austrian firearm legislation and its effects on suicide and homicide mortality: A natural quasi-experiment amidst the global economic crisis. Eur. Psychiatry 2018, 52, 104–112. [Google Scholar] [CrossRef]
- Lawrence, D.; Kisely, S.; Pais, J. The epidemiology of excess mortality in people with mental illness. Can. J. Psychiatry Rev. Can. De Psychiatr. 2010, 55, 752–760. [Google Scholar] [CrossRef]
- Laursen, T.M.; Plana-Ripoll, O.; Andersen, P.K.; McGrath, J.J.; Toender, A.; Nordentoft, M.; Canudas-Romo, V.; Erlangsen, A. Cause-specific life years lost among persons diagnosed with schizophrenia: Is it getting better or worse? Schizophr. Res. 2019, 206, 284–290. [Google Scholar] [CrossRef]
- Wasserman, D.; Carli, V.; Iosue, M.; Javed, A.; Herrman, H. Suicide prevention in psychiatric patients. Asia-Pac. Psychiatry 2021, 13, e12450. [Google Scholar] [CrossRef] [PubMed]
- Hubers, A.A.M.; Moaddine, S.; Peersmann, S.; Stijnen, T.; Van Duijn, E.; Van Der Mast, R.C.; Dekkers, O.; Giltay, E.J. Suicidal ideation and subsequent completed suicide in both psychiatric and non-psychiatric populations: A meta-analysis. Epidemiol. Psychiatr. Sci. 2016, 27, 186–198. [Google Scholar] [CrossRef] [PubMed]
- Park, C.H.K.; Lee, J.W.; Lee, S.Y.; Moon, J.; Jeon, D.-W.; Shim, S.-H.; Cho, S.-J.; Kim, S.G.; Lee, J.; Paik, J.-W.; et al. Suicide risk factors across suicidal ideators, single suicide attempters, and multiple suicide attempters. J. Psychiatr. Res. 2020, 131, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Shand, F.; Vogl, L.; Robinson, J. Improving patient care after a suicide attempt. Australas. Psychiatry 2018, 26, 145–148. [Google Scholar] [CrossRef] [PubMed]
- Niskanen, L.; Partonen, T.; Auvinen, A.; Haukka, J. Excess mortality in Finnish diabetic subjects due to alcohol, accidents and suicide: A nationwide study. Eur. J. Endocrinol. 2018, 179, 299–306. [Google Scholar] [CrossRef] [PubMed]
- Messaoud, A.; Mensi, R.; Mhalla, A.; Hallara, I.; Neffati, F.; Douki, W.; Najjar, M.; Gaha, L. Dyslipidémie et risque suicidaire chez des patients avec maladies psychiatriques. L’Encéphale 2018, 44, 315–320. [Google Scholar] [CrossRef] [PubMed]
- Crump, C.; Sundquist, K.; Winkleby, M.A. Sociodemographic, psychiatric and somatic risk factors for suicide: A Swedish national cohort study. Psychol. Med. 2013, 44, 279–289. [Google Scholar] [CrossRef]
- Chen, I.-M.; Lin, P.-H.; Wu, V.-C.; Wu, C.-S.; Shan, J.-C.; Chang, S.-S.; Liao, S.-C. Suicide deaths among patients with end-stage renal disease receiving dialysis: A population-based retrospective cohort study of 64,000 patients in Taiwan. J. Affect. Disord. 2018, 227, 7–10. [Google Scholar] [CrossRef]
- Brundin, L.; Erhardt, S.; Bryleva, E.Y.; Achtyes, E.D.; Postolache, T.T. The role of inflammation in suicidal behaviour. Acta Psychiatr. Scand. 2015, 132, 192–203. [Google Scholar] [CrossRef]
- Wisnousky, H.; Lazzara, N.; Ciarletta, M.; Pelton, M.; Chinchilli, V.M.; Ssentongo, A.E.; Ssentongo, P. Rates and risk factors for suicidal ideation, suicide attempts and suicide deaths in persons with HIV: A protocol for a systematic review and meta-analysis. BMJ Open 2021, 11, e037154. [Google Scholar] [CrossRef]
- Oberaigner, W.; Sperner-Unterweger, B.; Fiegl, M.; Geiger-Gritsch, S.; Haring, C. Increased suicide risk in cancer patients in Tyrol/Austria. Gen. Hosp. Psychiatry 2014, 36, 483–487. [Google Scholar] [CrossRef] [PubMed]
- McFarland, D.; Walsh, L.; Napolitano, S.; Morita, J.; Jaiswal, R. Suicide in Patients With Cancer: Identifying the Risk Factors. Oncology 2019, 33, 221–226. [Google Scholar] [PubMed]
- Tang, N.K.Y.; Crane, C. Suicidality in chronic pain: A review of the prevalence, risk factors and psychological links. Psychol. Med. 2006, 36, 575–586. [Google Scholar] [CrossRef] [PubMed]
- Rizk, M.M.; Herzog, S.; Dugad, S.; Stanley, B. Suicide Risk and Addiction: The Impact of Alcohol and Opioid Use Disorders. Curr. Addict. Rep. 2021, 8, 194–207. [Google Scholar] [CrossRef] [PubMed]
- Bohnert, A.S.B.; Ilgen, M.A. Understanding Links among Opioid Use, Overdose, and Suicide. N. Engl. J. Med. 2019, 380, 71–79. [Google Scholar] [CrossRef]
- Ilgen, M.A.; Zivin, K.; McCammon, R.J.; Valenstein, M. Pain and suicidal thoughts, plans and attempts in the United States. Gen. Hosp. Psychiatry 2008, 30, 521–527. [Google Scholar] [CrossRef]
- Alejos, M.; Vázquez-Bourgon, J.; Santurtún, M.; Riancho, J.; Santurtún, A. Do patients diagnosed with a neurological disease present increased risk of suicide? Neurologia 2022. advance online publication. [Google Scholar] [CrossRef]

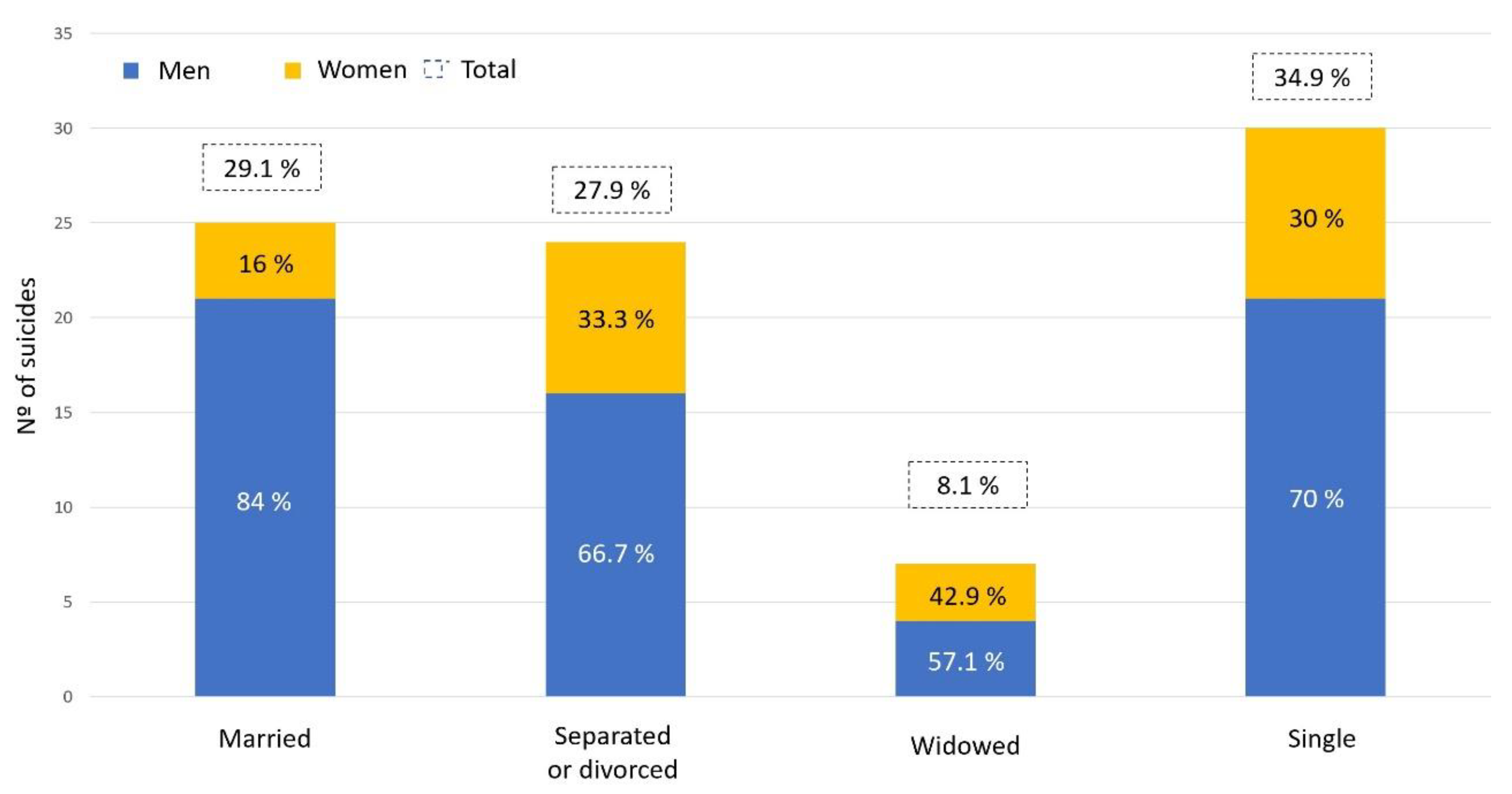
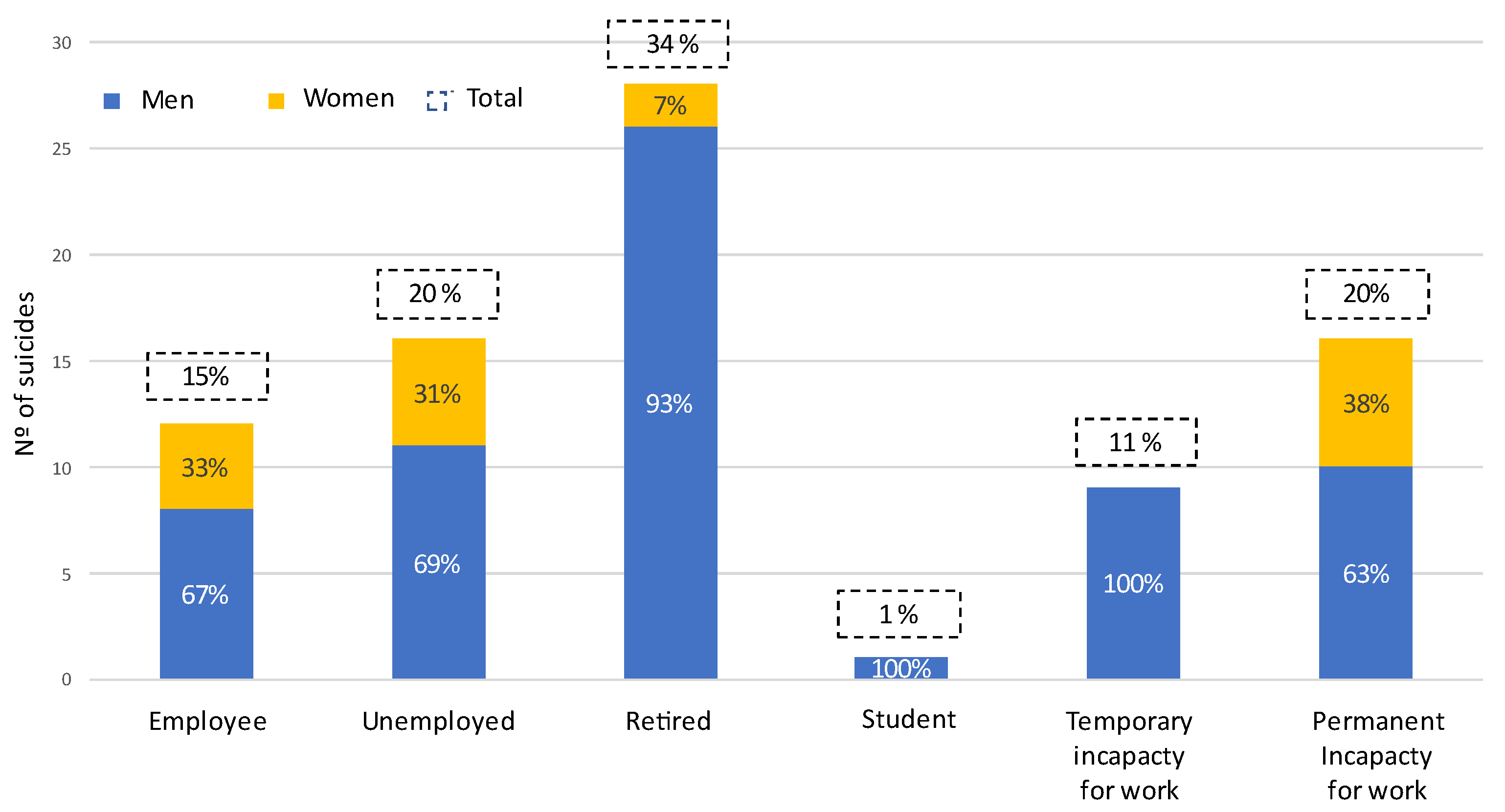
| Variables | Sample (%) | Spanish Population (%) | Z-Score | p | CI 95% |
|---|---|---|---|---|---|
| Divorced | 27.9 | 6.5 | 7.84 | <0.0001 | (0.114–0.315) |
| Married | 29.1 | 52.5 | 4.2 | <0.0001 | (−0.334–−0.130) |
| Spanish nationality | 94.3 | 85.3 | 2.59 | 0.0097 | (0.041–0.132) |
| Living alone | 38.8 | 10.3 | 8.2 | <0.0001 | (0.172–0.398) |
| Urban environment | 63.2 | 64.7 | 0.26 | 0.795 | (−0.104–0.073) |
| Rural environment | 36.8 | 35.3 | 0.26 | 0.795 | (−0.073–0.104) |
| Variables | Cases | Controls | p | OR (IC 95%) | ||
|---|---|---|---|---|---|---|
| n | % | n | % | |||
| Psychiatric diagnosis | 83 | 67% | 59 | 16% | <0.001 | 10.740 (6.738–17.118) |
| High blood pressure | 43 | 35% | 137 | 37% | 0.666 | 0.911 (0.595–1.394) |
| Dyslipidemia | 42 | 34% | 117 | 31% | 0.617 | 1.116 (0.725–1.719) |
| Previous self-harm attempt | 33 | 27% | 6 | 2% | <0.001 | 22.121 (8.997–54.389) |
| Cancer | 20 | 16% | 32 | 9% | 0.018 | 2.043 (1.121–3.724) |
| Diabetes Mellitus | 17 | 14% | 51 | 14% | 1 | 1 (0.554–1.806) |
| Heart Failure | 15 | 12% | 26 | 7% | 0.074 | 1.831 (0.936–3.582) |
| Rheumatological disease | 13 | 10% | 21 | 6% | 0.065 | 1.958 (0.949–4.037) |
| Chronic pain treated with opioids | 12 | 10% | 17 | 5% | 0.036 | 2.237 (1.037–4.827) |
| Chronic pain treated without opioids | 11 | 9% | 23 | 6% | 0.309 | 1.477 (0.698–3.124) |
| COPD | 8 | 6% | 11 | 3% | 0.102 | 2.263 (0.889–5. 762) |
| Renal Insufficiency | 8 | 6% | 11 | 3% | 0.102 | 2.263 (0.889–5.762) |
| Stroke | 8 | 6% | 16 | 4% | 0.334 | 1.534 (0.640–3.678) |
| OSA | 7 | 6% | 27 | 7% | 0.538 | 0.764 (0.324–1.802) |
| Asthma | 6 | 5% | 21 | 6% | 0.732 | 0.850 (0.335–2.156) |
| Neurogenerative disease | 5 | 4% | 10 | 3% | 0.544 | 1.521 (0.510–4.539) |
| Dementia | 3 | 2% | 10 | 3% | 0.871 | 0.898 (0.243–3.315) |
| HIV infection | 3 | 2% | 6 | 2% | 0.697 | 1.512 (0.373–6.140) |
| Parkinson disease | 3 | 2% | 4 | 1% | 0.374 | 2.281 (0.503–10. 335) |
| Fibromyalgia | 2 | 2% | 1 | 0% | 0.156 | 6.082 (0.547–67.659) |
| Spinal cord injury | 2 | 2% | 4 | 1% | 0.643 | 1.508 (0.273–8. 336) |
| Huntington disease | 1 | 1% | 0 | 0% | 0.25 | 0.248 (0.213–0.290) |
| SLE | 0 | 0% | 1 | 0% | 1 | 0.749 (0.712–0.789) |
| Alzheimer disease | 0 | 0% | 3 | 1% | 0.577 | 0.748 (0.711–0.788) |
| MS | 0 | 0% | 2 | 1% | 0.413 | 0.749 (0.712–0.788) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sáenz-Aldea, M.; Zarrabeitia, M.T.; García Blanco, A.; Santurtún, A. Scrutinizing the Profile and Risk Factors of Suicide: A Perspective from a Case–Control Study Focused on a Northern Region of Spain. Int. J. Environ. Res. Public Health 2022, 19, 15867. https://doi.org/10.3390/ijerph192315867
Sáenz-Aldea M, Zarrabeitia MT, García Blanco A, Santurtún A. Scrutinizing the Profile and Risk Factors of Suicide: A Perspective from a Case–Control Study Focused on a Northern Region of Spain. International Journal of Environmental Research and Public Health. 2022; 19(23):15867. https://doi.org/10.3390/ijerph192315867
Chicago/Turabian StyleSáenz-Aldea, María, María T. Zarrabeitia, Ana García Blanco, and Ana Santurtún. 2022. "Scrutinizing the Profile and Risk Factors of Suicide: A Perspective from a Case–Control Study Focused on a Northern Region of Spain" International Journal of Environmental Research and Public Health 19, no. 23: 15867. https://doi.org/10.3390/ijerph192315867
APA StyleSáenz-Aldea, M., Zarrabeitia, M. T., García Blanco, A., & Santurtún, A. (2022). Scrutinizing the Profile and Risk Factors of Suicide: A Perspective from a Case–Control Study Focused on a Northern Region of Spain. International Journal of Environmental Research and Public Health, 19(23), 15867. https://doi.org/10.3390/ijerph192315867







