Dental Criteria Could Alert for Malnutrition Risk and Inappropriate Choice of Food Texture in Older Subjects with Dementia: An Analytical Cross-Sectional Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Design
2.2. Sample
2.3. Procedure
2.4. Measures
2.5. Data Analyses
2.5.1. Hypotheses
2.5.2. Statistical Analyses
3. Results
3.1. Characteristics of the Participants
3.2. Anthropometric Measurements of Malnutrition in the Study Group
3.3. Variables Associated with Malnutrition as Measured by MUAC
3.4. Variables Associated with Type of Oral Feeding
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ADL | Activity of Daily Living index |
| MMSE | Mini Mental State Examination |
| MNA | Mini Nutritional Assessment index |
| MUAC | Mid-Upper Arm Circumference |
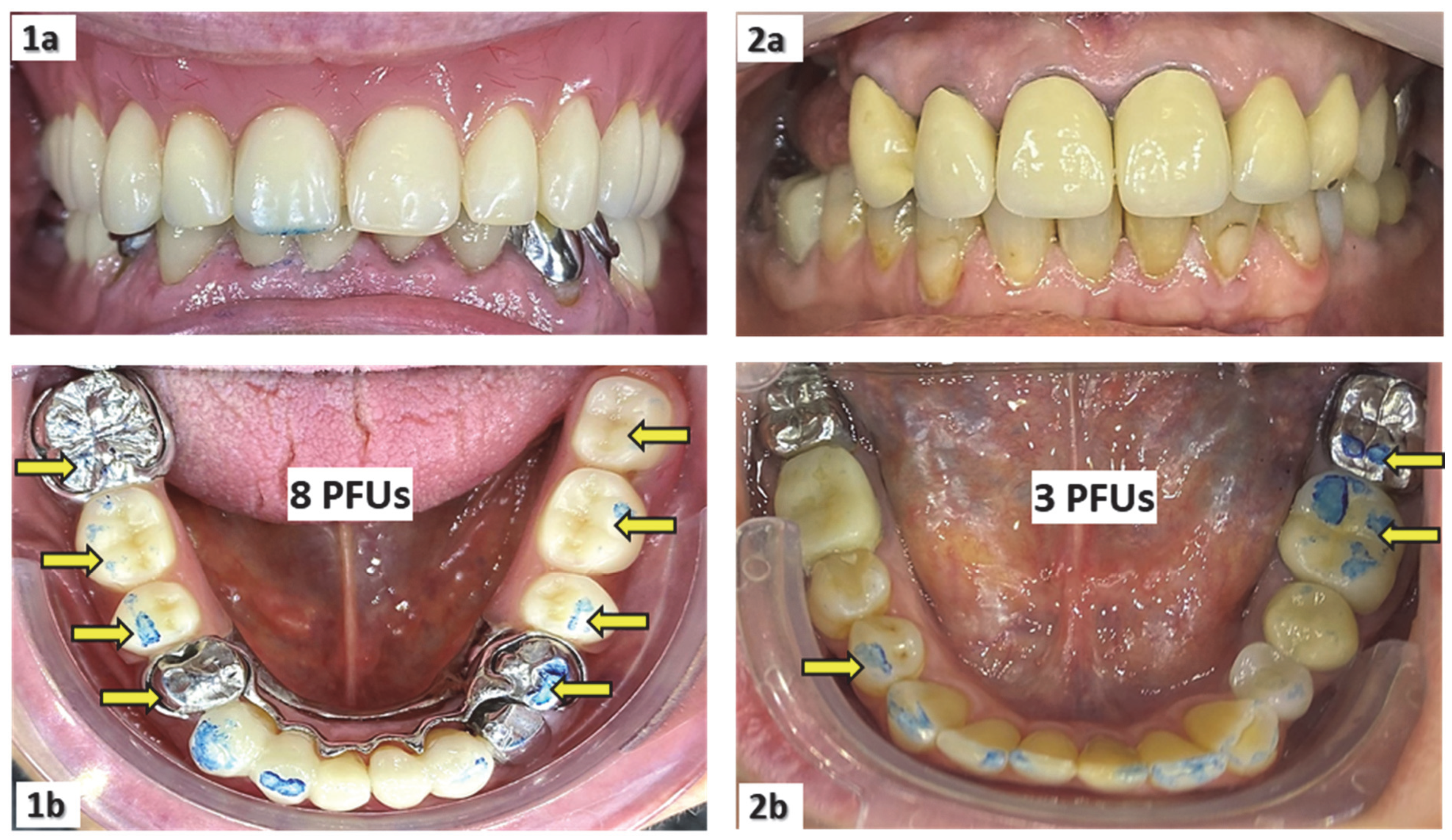
| PFUs | Posterior Functional dental Units |
References
- Prince, M.; Bryce, R.; Albanese, E.; Wimo, A.; Ribeiro, W.; Ferri, C.P. The global prevalence of dementia: A systematic review and metaanalysis. Alzheimers Dement. J. Alzheimers Assoc. 2013, 9, 63–75. [Google Scholar] [CrossRef] [PubMed]
- Wimo, A.; Jönsson, L.; Bond, J.; Prince, M.; Winblad, B. Alzheimer disease international the worldwide economic impact of dementia 2010. Alzheimers Dement. J. Alzheimers Assoc. 2013, 9, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Vellas, B.; Villars, H.; Abellan, G.; Soto, M.E.; Rolland, Y.; Guigoz, Y.; Morley, J.E.; Chumlea, W.; Salva, A.; Rubenstein, L.Z.; et al. Overview of the MNA—Its history and challenges. J. Nutr. Health Aging 2006, 10, 456–463; discussion 463–465. [Google Scholar] [PubMed]
- Gillette-Guyonnet, S.; Nourhashemi, F.; Andrieu, S.; de Glisezinski, I.; Ousset, P.J.; Riviere, D.; Albarede, J.L.; Vellas, B. Weight loss in Alzheimer disease. Am. J. Clin. Nutr. 2000, 71, 637S–642S. [Google Scholar] [CrossRef] [PubMed]
- White, H.; Pieper, C.; Schmader, K.; Fillenbaum, G. Weight change in Alzheimer’s disease. J. Am. Geriatr. Soc. 1996, 44, 265–272. [Google Scholar] [CrossRef]
- Fjellström, C.; Starkenberg, A.; Wesslén, A.; Licentiate, M.S.; Tysén Bäckström, A.-C.; Faxén-Irving, G. OmegAD Study group to be a good food provider: An exploratory study among spouses of persons with Alzheimer’s disease. Am. J. Alzheimers Dis. Other Demen. 2010, 25, 521–526. [Google Scholar] [CrossRef]
- Young, K.W.; Greenwood, C.E. Shift in diurnal feeding patterns in nursing home residents with Alzheimer’s disease. J. Gerontol. A Biol. Sci. Med. Sci. 2001, 56, M700–M706. [Google Scholar] [CrossRef]
- Konishi, M.; Kakimoto, N. Relationship between oral and nutritional status of older residents with severe dementia in an aged care nursing home. Gerodontology 2021, 38, 179–184. [Google Scholar] [CrossRef]
- Van de Rijt, L.J.M.; Feast, A.R.; Vickerstaff, V.; Sampson, E.L.; Lobbezoo, F. Oral function and its association with nutrition and quality of life in nursing home residents with and without dementia: A cross-sectional study. Gerodontology 2021, 38, 404–413. [Google Scholar] [CrossRef]
- Akın, S.; Mucuk, S.; Öztürk, A.; Mazıcıoğlu, M.; Göçer, Ş.; Arguvanlı, S.; Şafak, E.D. Muscle function-dependent sarcopenia and cut-off values of possible predictors in community-dwelling turkish elderly: Calf circumference, midarm muscle circumference and walking speed. Eur. J. Clin. Nutr. 2015, 69, 1087–1090. [Google Scholar] [CrossRef]
- Hu, F.-J.; Liu, H.; Liu, X.-L.; Jia, S.-L.; Hou, L.-S.; Xia, X.; Dong, B.-R. Mid-upper arm circumference as an alternative screening instrument to appendicular skeletal muscle mass index for diagnosing sarcopenia. Clin. Interv. Aging 2021, 16, 1095–1104. [Google Scholar] [CrossRef] [PubMed]
- Norazman, C.W.; Adznam, S.N.; Jamaluddin, R. Malnutrition as key predictor of physical frailty among malaysian older adults. Nutrients 2020, 12, E1713. [Google Scholar] [CrossRef]
- Selvaraj, K.; Jayalakshmy, R.; Yousuf, A.; Singh, A.K.; Ramaswamy, G.; Palanivel, C. Can mid-upper arm circumference and calf circumference be the proxy measures to detect undernutrition among elderly? Findings of a community-based survey in rural puducherry, India. J. Fam. Med. Prim. Care 2017, 6, 356–359. [Google Scholar] [CrossRef] [PubMed]
- Shi, J.; Yang, Z.; Niu, Y.; Zhang, W.; Li, X.; Zhang, H.; Lin, N.; Gu, H.; Wen, J.; Ning, G.; et al. Large mid-upper arm circumference is associated with metabolic syndrome in middle-aged and elderly individuals: A community-based study. BMC Endocr. Disord. 2020, 20, 78. [Google Scholar] [CrossRef] [PubMed]
- Başıbüyük, G.Ö.; Ayremlou, P.; Saeidlou, S.N.; Ay, F.; Dalkıran, A.; Simzari, W.; Vitályos, G.Á.; Bektaş, Y. A comparison of the different anthropometric indices for assessing malnutrition among older people in turkey: A large population-based screening. J. Health Popul. Nutr. 2021, 40, 13. [Google Scholar] [CrossRef]
- Bonaccorsi, G.; Santomauro, F.; Lorini, C.; Indiani, L.; Pellegrino, E.; Pasquini, G.; Molino-Lova, R.; Epifani, F.; Macchi, C. Mugello study working group risk of malnutrition in a sample of nonagenarians: Specific versus classic bioelectrical impedance vector analysis. Nutrition 2016, 32, 368–374. [Google Scholar] [CrossRef]
- Pohlhausen, S.; Uhlig, K.; Kiesswetter, E.; Diekmann, R.; Heseker, H.; Volkert, D.; Stehle, P.; Lesser, S. Energy and protein intake, anthropometrics, and disease burden in elderly home-care receivers—A cross-sectional study in germany (ErnSIPP Study). J. Nutr. Health Aging 2016, 20, 361–368. [Google Scholar] [CrossRef]
- Suzana, S.; Siti Saifa, H. Validation of nutritional screening tools against anthropometric and functional assessments among elderly people in Selangor. Malays. J. Nutr. 2007, 13, 29–44. [Google Scholar]
- Gottschall, C.; Tarnowski, M.; Machado, P.; Raupp, D.; Marcadenti, A.; Rabito, E.I.; Silva, F.M. Predictive and concurrent validity of the malnutrition universal screening tool using mid-upper arm circumference instead of body mass index. J. Hum. Nutr. Diet. 2019, 32, 775–780. [Google Scholar] [CrossRef]
- Yilmaz, M.; Atilla, F.D.; Sahin, F.; Saydam, G. The effect of malnutrition on mortality in hospitalized patients with hematologic malignancy. Support. Care Cancer 2020, 28, 1441–1448. [Google Scholar] [CrossRef]
- Aukner, C.; Eide, H.D.; Iversen, P.O. Nutritional status among older residents with dementia in open versus special care units in municipal nursing homes: An observational study. BMC Geriatr. 2013, 13, 26. [Google Scholar] [CrossRef] [PubMed]
- Pilleron, S.; Jésus, P.; Desport, J.-C.; Mbelesso, P.; Ndamba-Bandzouzi, B.; Clément, J.-P.; Dartigues, J.-F.; Preux, P.-M.; Guerchet, M.; EPIDEMCA Group; et al. Association between Mild cognitive impairment and dementia and undernutrition among elderly people in Central Africa: Some results from the EPIDEMCA (Epidemiology of Dementia in Central Africa) programme. Br. J. Nutr. 2015, 114, 306–315. [Google Scholar] [CrossRef] [PubMed]
- Peyron, M.A.; Woda, A.; Bourdiol, P.; Hennequin, M. Age-related changes in mastication. J. Oral Rehabil. 2017, 44, 299–312. [Google Scholar] [CrossRef] [PubMed]
- Decerle, N.; Nicolas, E.; Hennequin, M. Chewing deficiencies in adults with multiple untreated carious lesions. Caries Res. 2013, 47, 330–337. [Google Scholar] [CrossRef] [PubMed]
- Godlewski, A.E.; Veyrune, J.L.; Nicolas, E.; Ciangura, C.A.; Chaussain, C.C.; Czernichow, S.; Basdevant, A.; Hennequin, M. Effect of dental status on changes in mastication in patients with obesity following bariatric surgery. PLoS ONE 2011, 6, e22324. [Google Scholar] [CrossRef]
- El Osta, N.; Hennequin, M.; Tubert-Jeannin, S.; Abboud Naaman, N.B.; El Osta, L.; Geahchan, N. The pertinence of oral health indicators in nutritional studies in the elderly. Clin. Nutr. 2014, 33, 316–321. [Google Scholar] [CrossRef]
- Hennequin, M.; Mazille, M.-N.; Cousson, P.-Y.; Nicolas, E. Increasing the Number of inter-arch contacts improves mastication in adults with down syndrome: A prospective controlled trial. Physiol. Behav. 2015, 145, 14–21. [Google Scholar] [CrossRef]
- El Osta, N.; El Osta, L.; Lassauzay, C.; Ghosn, M.; Tubert-Jeannin, S.; Hennequin, M. Oral health and chemotherapy act as cofactors in malnutrition in the elderly with other cancers than head and neck malignancies. Clin. Oral Investig. 2019, 23, 235–243. [Google Scholar] [CrossRef]
- Chahine, L.M.; Bijlsma, A.; Hospers, A.P.N.; Chemali, Z. Dementia and depression among nursing home residents in Lebanon: A pilot study. Int. J. Geriatr. Psychiatry 2007, 22, 283–285. [Google Scholar] [CrossRef]
- El-Hayeck, R.; Baddoura, R.; Wehbé, A.; Bassil, N.; Koussa, S.; Abou Khaled, K.; Richa, S.; Khoury, R.; Alameddine, A.; Sellal, F. An arabic version of the mini-mental state examination for the Lebanese population: Reliability, validity, and normative data. J. Alzheimers Dis. JAD 2019, 71, 525–540. [Google Scholar] [CrossRef]
- Guyonnet, S.; Rolland, Y. Screening for malnutrition in older people. Clin. Geriatr. Med. 2015, 31, 429–437. [Google Scholar] [CrossRef] [PubMed]
- Keller, U. Nutritional laboratory markers in malnutrition. J. Clin. Med. 2019, 8, E775. [Google Scholar] [CrossRef] [PubMed]
- Nasser, R.; Doumit, J. Validity and reliability of the arabic version of activities of daily living (ADL). BMC Geriatr. 2009, 9, 11. [Google Scholar] [CrossRef] [PubMed]
- Bonnefoy, M.; Jauffret, M.; Kostka, T.; Jusot, J.F. Usefulness of calf circumference measurement in assessing the nutritional state of hospitalized elderly people. Gerontology 2002, 48, 162–169. [Google Scholar] [CrossRef] [PubMed]
- Veyrune, J.-L.; Miller, C.C.; Czernichow, S.; Ciangura, C.A.; Nicolas, E.; Hennequin, M. Impact of morbid obesity on chewing ability. Obes. Surg. 2008, 18, 1467–1472. [Google Scholar] [CrossRef]
- Saleh, J.; Figueiredo, M.A.Z.; Cherubini, K.; Salum, F.G. Salivary hypofunction: An update on aetiology, diagnosis and therapeutics. Arch. Oral Biol. 2015, 60, 242–255. [Google Scholar] [CrossRef]
- Viljakainen, S.; Nykänen, I.; Ahonen, R.; Komulainen, K.; Suominen, A.L.; Hartikainen, S.; Tiihonen, M. Xerostomia among older home care clients. Community Dent. Oral Epidemiol. 2016, 44, 232–238. [Google Scholar] [CrossRef]
- Silness, J.; Loe, H. Periodontal disease in pregnancy. II. Correlation between oral hygiene and periodontal condition. Acta Odontol. Scand. 1964, 22, 121–135. [Google Scholar] [CrossRef]
- Peltola, P.; Vehkalahti, M.M.; Simoila, R. Effects of 11-month interventions on oral cleanliness among the long-term hospitalised elderly. Gerodontology 2007, 24, 14–21. [Google Scholar] [CrossRef]
- Tabachnick, B.G.; Fidell, L.S. Using Multivariate Statistics, 6th ed.; Pearson: Boston, UK, 2012; ISBN 978-0-205-84957-4. [Google Scholar]
- Bourdiol, P.; Hennequin, M.; Peyron, M.-A.; Woda, A. Masticatory adaptation to occlusal changes. Front. Physiol. 2020, 11, 263. [Google Scholar] [CrossRef]
- Woda, A.; Mishellany, A.; Peyron, M.-A. The regulation of masticatory function and food bolus formation. J. Oral Rehabil. 2006, 33, 840–849. [Google Scholar] [CrossRef] [PubMed]
- Séoud, J.; Nehmé, C.; Atallah, R.; Zablit, C.; Yérétzian, J.; Lévesque, L.; Giroux, F.; Ducharme, F. The health of family caregivers of older impaired persons in Lebanon: An interview survey. Int. J. Nurs. Stud. 2007, 44, 259–272. [Google Scholar] [CrossRef] [PubMed]
- Faxén-Irving, G.; Fereshtehnejad, S.-M.; Falahati, F.; Cedergren, L.; Göranzon, H.; Wallman, K.; García-Ptacek, S.; Eriksdotter, M.; Religa, D. Body mass index in different dementia disorders: Results from the Swedish dementia quality registry (SveDem). Dement. Geriatr. Cogn. Disord. Extra 2014, 4, 65–75. [Google Scholar] [CrossRef] [PubMed]
- Catteau, C.; Mishellany, A.; Faulks, D.; Lassauzay, C.; Hennequin, M. Oral health status of persons with disabilities attending special establishments. First results of the national health education programme “Oral Health and Autonomy”. Bull. Groupèment Int. Rech. Sci. Stomatol. Odontol. 2011, 50, 15–18. [Google Scholar]
- Elsig, F.; Schimmel, M.; Duvernay, E.; Giannelli, S.V.; Graf, C.E.; Carlier, S.; Herrmann, F.R.; Michel, J.-P.; Gold, G.; Zekry, D.; et al. Tooth loss, chewing efficiency and cognitive impairment in geriatric patients. Gerodontology 2015, 32, 149–156. [Google Scholar] [CrossRef] [PubMed]
- Hoeksema, A.R.; Peters, L.L.; Raghoebar, G.M.; Meijer, H.J.A.; Vissink, A.; Visser, A. Oral health status and need for oral care of care-dependent indwelling elderly: From admission to death. Clin. Oral Investig. 2017, 21, 2189–2196. [Google Scholar] [CrossRef] [PubMed]
- Chebib, N.; Cuvelier, C.; Malézieux-Picard, A.; Parent, T.; Roux, X.; Fassier, T.; Müller, F.; Prendki, V. Pneumonia prevention in the elderly patients: The other sides. Aging Clin. Exp. Res. 2021, 33, 1091–1100. [Google Scholar] [CrossRef] [PubMed]
- Cockburn, N.; Pradhan, A.; Taing, M.W.; Kisely, S.; Ford, P.J. Oral health impacts of medications used to treat mental illness. J. Affect. Disord. 2017, 223, 184–193. [Google Scholar] [CrossRef] [PubMed]
- King, S.; Chow, C.K.; Eberhard, J. Oral health and cardiometabolic disease: Understanding the relationship. Intern. Med. J. 2022, 52, 198–205. [Google Scholar] [CrossRef]
- Adams, R. Qualified nurses lack adequate knowledge related to oral health, resulting in inadequate oral care of patients on medical wards. J. Adv. Nurs. 1996, 24, 552–560. [Google Scholar] [CrossRef]
- Logan, H.L.; Ettinger, R.; McLeran, H.; Casko, R.; Dal Secco, D. Common misconceptions about oral health in the older adult: Nursing practices. Spec. Care Dent. 1991, 11, 243–247. [Google Scholar] [CrossRef] [PubMed]
- Yi Mohammadi, J.J.; Franks, K.; Hines, S. Effectiveness of professional oral health care intervention on the oral health of residents with dementia in residential aged care facilities: A systematic review protocol. JBI Database Syst. Rev. Implement. Rep. 2015, 13, 110–122. [Google Scholar] [CrossRef] [PubMed]
- Cousson, P.Y.; Bessadet, M.; Nicolas, E.; Veyrune, J.-L.; Lesourd, B.; Lassauzay, C. Nutritional status, dietary intake and oral quality of life in elderly complete denture wearers. Gerodontology 2012, 29, e685–e692. [Google Scholar] [CrossRef] [PubMed]
| Severity of Dementia | |||||
|---|---|---|---|---|---|
| Moderate (n = 35) | Severe (n = 68) | Total | p-Value | ||
| Sociodemographic characteristics | Age (years) | 84.69 ± 8.64 | 83.49 ± 8.83 | 83.90 ± 8.74 | 0.515 |
| Gender | 0.388 | ||||
| Men | 11 (31.4%) | 16 (23.5%) | 27 (26.2%) | ||
| Women | 24 (68.6%) | 52 (76.5%) | 76 (73.8%) | ||
| Marital status | 0.201 | ||||
| Single | 6 (17.1%) | 15 (22.1%) | 21 (20.4%) | ||
| Married | 5 (14.3%) | 13 (19.1%) | 18 (17.5%) | ||
| Divorced/widowed | 24 (68.6%) | 40 (58.8%) | 64 (62.2%) | ||
| Duration of stay in institution | 0.487 | ||||
| <1 year | 9 (25.7%) | 22 (32.4%) | 31 (30.1%) | ||
| >1 year | 26 (74.3%) | 46 (67.6%) | 72 (69.9%) | ||
| Nutritional status | MUAC < 21 cm | 5 (14.3%) | 20 (29.4%) | 25 (24.3%) | 0.090 |
| Albumin < 35 g/L | 7 (20.0%) | 28 (41.2%) | 35 (34.0%) | 0.032 | |
| Feeding routes and food texture | Feeding route | 0.092 | |||
| Oral | 35 (100.0%) | 61 (89.7%) | 96 (93.2%) | ||
| Enteral | 0 (0.0%) | 7 (10.3%) | 7 (6.8%) | ||
| Food texture * | 0.015 | ||||
| Normal texture | 30 (85.7%) | 38 (62.3%) | 68 (70.8%) | ||
| Modified texture | 5 (14.3%) | 23 (37.7%) | 28 (29.2%) | ||
| Dietary supplement intake | 2 (5.7%) | 8 (11.8%) | 10 (9.7%) | 0.488 | |
| General health status | Drug intake number per day | 7.34 ± 3.82 | 7.65 ± 3.86 | 7.54 ± 3.83 | 0.705 |
| Number of chronic diseases | 2.51 ± 1.31 | 2.12 ± 1.63 | 2.25 ± 1.53 | 0.215 | |
| ADL score | 2.39 ± 2.12 | 1.1 ± 1.56 | 1.53 ± 1.86 | <0.001 | |
| Oral health status | FU ≤ 4 | 23 (65.7%) | 43 (63.2%) | 66 (64.1%) | 0.804 |
| Dry mouth | 24 (68.6%) | 55 (80.9%) | 79 (76.7%) | 0.162 | |
| Poor oral hygiene | 19 (54.3%) | 47 (69.1%) | 66 (64.1%) | 0.137 | |
| MUAC <21 cm (n = 25) | MUAC ≥21 cm (n = 78) | p-Value | ||
|---|---|---|---|---|
| Sociodemographic characteristics | Age (years) | 84.40 ± 9.17 | 83.56 ± 8.74 | 0.682 |
| Gender | ||||
| Men | 5 (18.5%) | 22 (81.5%) | 0.417 | |
| Women | 20 (26.3%) | 56 (73.7%) | ||
| Marital status | ||||
| Married | 3 (16.7%) | 15 (83.3%) | 0.551 | |
| Others | 22 (25.9%) | 63 (74.1%) | ||
| Duration of the stay | ||||
| <1 year | 11 (35.5%) | 20 (64.5%) | 0.082 | |
| >1 year | 14 (19.4%) | 58 (80.6%) | ||
| Feeding habits | Feeding route | |||
| Oral | 22 (22.9%) | 74 (77.1%) | 0.256 | |
| Enteral | 3 (42.9%) | 4 (57.1%) | ||
| Food texture * | ||||
| Normal texture | 9 (13.2%) | 59 (86.8%) | 0.001 | |
| Modified texture | 13 (46.4%) | 15 (53.6%) | ||
| Dietary supplement intake | ||||
| Yes | 4 (40.0%) | 6 (60.0%) | 0.251 | |
| No | 21 (22.6%) | 72 (77.4%) | ||
| Nutritional status | Albumin level | |||
| <35 g/L | 19 (76.0%) | 16 (20.5%) | <0.001 | |
| >35 g/L | 6 (24.0%) | 62 (79.5%) | ||
| Oral health status | PFUs | |||
| ≤4 | 21 (31.8%) | 45 (68.2%) | 0.017 | |
| >4 | 4 (10.8%) | 33 (89.2%) | ||
| Dry mouth | ||||
| No | 2 (8.3%) | 22 (91.7%) | 0.038 | |
| Yes | 23 (29.1%) | 56 (70.9%) | ||
| General health status | Drugs intake number | 6.96 ± 3.43 | 7.73 ± 3.95 | 0.384 |
| Number of chronic diseases | 2.00 ± 1.29 | 2.33 ± 1.60 | 0.346 | |
| ADL score | 0.46 ± 0.88 | 1.88 ± 1.97 | 0.001 |
| B | S.E. | Wald | Sig. | OR | 95% C.I. for OR | ||
|---|---|---|---|---|---|---|---|
| Lower | Upper | ||||||
| Albumin level < 35 g/L | 2.526 | 0.684 | 13.625 | 0.000 | 12.503 | 3.270 | 47.811 |
| Duration of stay ≤ 1 year | 1.643 | 0.750 | 4.792 | 0.029 | 5.169 | 1.188 | 22.495 |
| Modified food texture | 1.446 | 0.687 | 4.434 | 0.035 | 4.247 | 1.105 | 16.316 |
| PFUs ≤ 4 | 2.015 | 0.941 | 4.589 | 0.032 | 7.504 | 1.187 | 47.438 |
| Clinical sign of dry mouth | 1.352 | 0.960 | 1.986 | 0.159 | 3.867 | 0.589 | 25.368 |
| Constant | −10.507 | 2.812 | 13.960 | 0.000 | 0.000 | ||
| Type of Oral Feeding | ||||
|---|---|---|---|---|
| Normal Texture (n = 68) | Modified Texture (n = 28) | p-Value | ||
| Sociodemographic characteristics | Men | 20 (29.4%) | 5 (17.9%) | 0.241 |
| Age | 83.75 ± 8.77 | 83.32 ± 9.33 | 0.831 | |
| Duration of stay > 1 year | 49 (72.1%) | 21 (75.0%) | 0.768 | |
| Nutritional status | MUAC < 21 cm | 9 (13.2%) | 13 (46.4%) | 0.001 |
| Albumin < 35 g/L | 14 (20.6%) | 15 (53.6%) | 0.001 | |
| Feeding habits | Dietary supplement intake | 3 (4.4%) | 6 (21.4%) | 0.017 |
| General health status | Number of chronic diseases | 2.38 ± 1.56 | 2.07 ± 1.36 | 0.359 |
| Drug intake number/day | 7.82 ± 3.87 | 7.57 ± 3.12 | 0.760 | |
| ADL | 2.17 ± 1.94 | 0.34 ± 0.87 | <0.001 | |
| Severe dementia | 36 (52.9%) | 23 (82.1%) | 0.008 | |
| Oral health status | Number PFUs ≤ 4 | 41 (60.3%) | 19 (67.9%) | 0.487 |
| Dry mouth | 49 (72.1%) | 23 (82.1%) | 0.300 | |
| Bad oral hygiene | 43 (63.2%) | 17 (60.7%) | 0.817 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
El Osta, N.; Wehbe, A.; Sleiman, N.; Drancourt, N.; El Osta, L.; Hennequin, M. Dental Criteria Could Alert for Malnutrition Risk and Inappropriate Choice of Food Texture in Older Subjects with Dementia: An Analytical Cross-Sectional Study. Int. J. Environ. Res. Public Health 2022, 19, 15086. https://doi.org/10.3390/ijerph192215086
El Osta N, Wehbe A, Sleiman N, Drancourt N, El Osta L, Hennequin M. Dental Criteria Could Alert for Malnutrition Risk and Inappropriate Choice of Food Texture in Older Subjects with Dementia: An Analytical Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2022; 19(22):15086. https://doi.org/10.3390/ijerph192215086
Chicago/Turabian StyleEl Osta, Nada, Amine Wehbe, Nelly Sleiman, Noemie Drancourt, Lana El Osta, and Martine Hennequin. 2022. "Dental Criteria Could Alert for Malnutrition Risk and Inappropriate Choice of Food Texture in Older Subjects with Dementia: An Analytical Cross-Sectional Study" International Journal of Environmental Research and Public Health 19, no. 22: 15086. https://doi.org/10.3390/ijerph192215086
APA StyleEl Osta, N., Wehbe, A., Sleiman, N., Drancourt, N., El Osta, L., & Hennequin, M. (2022). Dental Criteria Could Alert for Malnutrition Risk and Inappropriate Choice of Food Texture in Older Subjects with Dementia: An Analytical Cross-Sectional Study. International Journal of Environmental Research and Public Health, 19(22), 15086. https://doi.org/10.3390/ijerph192215086






