Association between Moving to a High-Volume Hospital in the Capital Area and the Mortality among Patients with Cancer: A Large Population-Based Cohort Study
Abstract
1. Introduction
2. Methods
2.1. Data and Participants
2.2. Variables
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Jung, K.-W.; Won, Y.-J.; Oh, C.-M.; Kong, H.-J.; Lee, D.H.; Lee, K.H. Cancer statistics in Korea: Incidence, mortality, survival, and prevalence in 2014. Cancer Res. Treat. Off. J. Korean Cancer Assoc. 2017, 49, 292. [Google Scholar] [CrossRef] [PubMed]
- Lee, K.-S.; Chang, H.-S.; Lee, S.-M.; Park, E.-C. Economic burden of cancer in Korea during 2000–2010. Cancer Res. Treat. Off. J. Korean Cancer Assoc. 2015, 47, 387. [Google Scholar] [CrossRef] [PubMed]
- Quality: Korea 2012—Raising Standards. Available online: https://www.oecd.org/publications/oecd-reviews-of-health-care-quality-korea-9789264173446-en.htm (accessed on 5 April 2021).
- Lee, J.Y.; Jo, M.-W.; Yoo, W.-S.; Kim, H.J.; Eun, S.J. Evidence of a broken healthcare delivery system in Korea: Unnecessary hospital outpatient utilization among patients with a single chronic disease without complications. J. Korean Med. Sci. 2014, 29, 1590–1596. [Google Scholar] [CrossRef] [PubMed]
- Choi, J.K.; Kim, S.H.; Park, M.B. Effects of high-speed rail on health-care service utilization. J. Transp. Health 2019, 12, 13–20. [Google Scholar] [CrossRef]
- Tullock, G. Public decisions as public goods. J. Political Econ. 1971, 79, 913–918. [Google Scholar] [CrossRef]
- Borders, T.F.; Rohrer, J.E. Rural residence and migration for specialty physician care. Health Care Manag. Rev. 2001, 26, 40–49. [Google Scholar] [CrossRef]
- Birkmeyer, J.D.; Siewers, A.E.; Finlayson, E.V.; Stukel, T.A.; Lucas, F.L.; Batista, I.; Welch, H.G.; Wennberg, D.E. Hospital volume and surgical mortality in the United States. N. Engl. J. Med. 2002, 346, 1128–1137. [Google Scholar] [CrossRef] [PubMed]
- Dudley, R.A.; Johansen, K.L.; Brand, R.; Rennie, D.J.; Milstein, A. Selective referral to high-volume hospitals: Estimating potentially avoidable deaths. JAMA 2000, 283, 1159–1166. [Google Scholar] [CrossRef]
- Jeon, B.-Y.; Choi, S.-M.; Kim, C.-Y. Socioeconomic equity in regional distribution of health care resources in Korea. Health Policy Manag. 2012, 22, 85–108. [Google Scholar] [CrossRef]
- Ward, E.; Halpern, M.; Schrag, N.; Cokkinides, V.; DeSantis, C.; Bandi, P.; Siegel, R.; Stewart, A.; Jemal, A. Association of insurance with cancer care utilization and outcomes. CA Cancer J. Clin. 2008, 58, 9–31. [Google Scholar] [CrossRef] [PubMed]
- Roetzheim, R.G.; Gonzalez, E.C.; Ferrante, J.M.; Pal, N.; Van Durme, D.J.; Krischer, J.P. Effects of health insurance and race on breast carcinoma treatments and outcomes. Cancer Interdiscip. Int. J. Am. Cancer Soc. 2000, 89, 2202–2213. [Google Scholar] [CrossRef]
- Bradley, C.J.; Given, C.W.; Roberts, C. Disparities in cancer diagnosis and survival. Cancer 2001, 91, 178–188. [Google Scholar] [CrossRef]
- Bradley, C.J.; Gardiner, J.; Given, C.W.; Roberts, C. Cancer, Medicaid enrollment, and survival disparities. Cancer Interdiscip. Int. J. Am. Cancer Soc. 2005, 103, 1712–1718. [Google Scholar] [CrossRef]
- Clegg, L.X.; Li, F.P.; Hankey, B.F.; Chu, K.; Edwards, B.K. Cancer survival among US whites and minorities: A SEER (Surveillance, Epidemiology, and End Results) Program population-based study. Arch. Intern. Med. 2002, 162, 1985–1993. [Google Scholar] [CrossRef] [PubMed]
- Eley, J.W.; Hill, H.A.; Chen, V.W.; Austin, D.F.; Wesley, M.N.; Muss, H.B.; Greenberg, R.S.; Coates, R.J.; Correa, P.; Redmond, C.K. Racial differences in survival from breast cancer: Results of the National Cancer Institute Black/White Cancer Survival Study. JAMA 1994, 272, 947–954. [Google Scholar] [CrossRef] [PubMed]
- Li, C.I.; Malone, K.E.; Daling, J.R. Differences in breast cancer stage, treatment, and survival by race and ethnicity. Arch. Intern. Med. 2003, 163, 49–56. [Google Scholar] [CrossRef] [PubMed]
- Ward, E.; Jemal, A.; Cokkinides, V.; Singh, G.K.; Cardinez, C.; Ghafoor, A.; Thun, M. Cancer disparities by race/ethnicity and socioeconomic status. CA Cancer J. Clin. 2004, 54, 78–93. [Google Scholar] [CrossRef] [PubMed]
- Rinaldo, L.; Brinjikji, W.; McCutcheon, B.A.; Bydon, M.; Cloft, H.; Kallmes, D.F.; Rabinstein, A.A. Hospital transfer associated with increased mortality after endovascular revascularization for acute ischemic stroke. J. Neurointerv. Surg. 2017, 9, 1166–1172. [Google Scholar] [CrossRef]
- Rinaldo, L.; Brinjikji, W.; Rabinstein, A.A. Transfer to high-volume centers associated with reduced mortality after endovascular treatment of acute stroke. Stroke 2017, 48, 1316–1321. [Google Scholar] [CrossRef]
- Byers, T.; Mouchawar, J.; Marks, J.; Cady, B.; Lins, N.; Swanson, G.M.; Bal, D.G.; Eyre, H.; Incidence, A.R.i.C.; Committee, M. The American Cancer Society challenge goals: How far can cancer rates decline in the US by the year 2015? Cancer 1999, 86, 715–727. [Google Scholar] [CrossRef]
- Liu, M.; Zhang, Q.; Lu, M.; Kwon, C.S.; Quan, H. Rural and Urban Disparity in Health Services Utilization in China. Med. Care 2007, 45, 767–774. [Google Scholar] [CrossRef] [PubMed]
- Cook, M.B.; McGlynn, K.A.; Devesa, S.S.; Freedman, N.D.; Anderson, W.F. Sex disparities in cancer mortality and survival. Cancer Epidemiol. Prev. Biomark. 2011, 20, 1629–1637. [Google Scholar] [CrossRef] [PubMed]
- Cook, M.B.; Dawsey, S.M.; Freedman, N.D.; Inskip, P.D.; Wichner, S.M.; Quraishi, S.M.; Devesa, S.S.; McGlynn, K.A. Sex disparities in cancer incidence by period and age. Cancer Epidemiol. Prev. Biomark. 2009, 18, 1174–1182. [Google Scholar] [CrossRef] [PubMed]
- Jiang, M.; Kim, E. Impact of high-speed railroad on regional income inequalities in China and Korea. Int. J. Urban Sci. 2016, 20, 393–406. [Google Scholar] [CrossRef]
- Alter, D.A.; Naylor, C.D.; Austin, P.; Tu, J.V. Effects of socioeconomic status on access to invasive cardiac procedures and on mortality after acute myocardial infarction. N. Engl. J. Med. 1999, 341, 1359–1367. [Google Scholar] [CrossRef] [PubMed]
- Brawley, O.W.; Freeman, H.P. Race and outcomes: Is this the end of the beginning for minority health research? J. Natl. Cancer Inst. 1999, 91, 1908–1909. [Google Scholar] [CrossRef][Green Version]
- Dignam, J.J. Differences in breast cancer prognosis among African-American and Caucasian women. CA Cancer J. Clin. 2000, 50, 50–64. [Google Scholar] [CrossRef]
- McCollum, A.D.; Catalano, P.J.; Haller, D.G.; Mayer, R.J.; Macdonald, J.S.; Benson, A.B., III; Fuchs, C.S. Outcomes and toxicity in african-american and caucasian patients in a randomized adjuvant chemotherapy trial for colon cancer. J. Natl. Cancer Inst. 2002, 94, 1160–1167. [Google Scholar] [CrossRef]
- Kwon, S. Thirty years of national health insurance in South Korea: Lessons for achieving universal health care coverage. Health Policy Plan. 2009, 24, 63–71. [Google Scholar] [CrossRef]
- Jang, S.Y.; Seon, J.Y.; Oh, I.H. Influencing Factors of Transportation Costs Regarding Healthcare Service Utilization in Korea. J. Korean Med. Sci. 2020, 35, e290. [Google Scholar] [CrossRef]
- Yoon, T.H.; Lee, S.Y.; Kim, C.W.; Kim, S.Y.; Jeong, B.G.; Park, H.K. Inequalities in medical care utilization by South Korean cancer patients according to income: A retrospective cohort study. Int. J. Health Serv. 2011, 41, 51–66. [Google Scholar] [CrossRef] [PubMed]
- Numico, G.; Zanelli, C.; Ippoliti, R.; Rossi, M.; Traverso, E.; Antonuzzo, A.; Bellini, R. The hospital care of patients with cancer: A retrospective analysis of the characteristics of their hospital stay in comparison with other medical conditions. Eur. J. Cancer 2020, 139, 99–106. [Google Scholar] [CrossRef]
- Birkmeyer, J.D.; Stukel, T.A.; Siewers, A.E.; Goodney, P.P.; Wennberg, D.E.; Lucas, F.L. Surgeon volume and operative mortality in the United States. N. Engl. J. Med. 2003, 349, 2117–2127. [Google Scholar] [CrossRef] [PubMed]
- Gruen, R.L.; Pitt, V.; Green, S.; Parkhill, A.; Campbell, D.; Jolley, D. The effect of provider case volume on cancer mortality: Systematic review and meta-analysis. CA Cancer J. Clin. 2009, 59, 192–211. [Google Scholar] [CrossRef] [PubMed]
- Yun, Y.H.; Kim, Y.A.; Min, Y.H.; Park, S.; Won, Y.J.; Kim, D.Y.; Choi, I.J.; Kim, Y.W.; Park, S.J.; Kim, J.H.; et al. The influence of hospital volume and surgical treatment delay on long-term survival after cancer surgery. Ann. Oncol. 2012, 23, 2731–2737. [Google Scholar] [CrossRef]
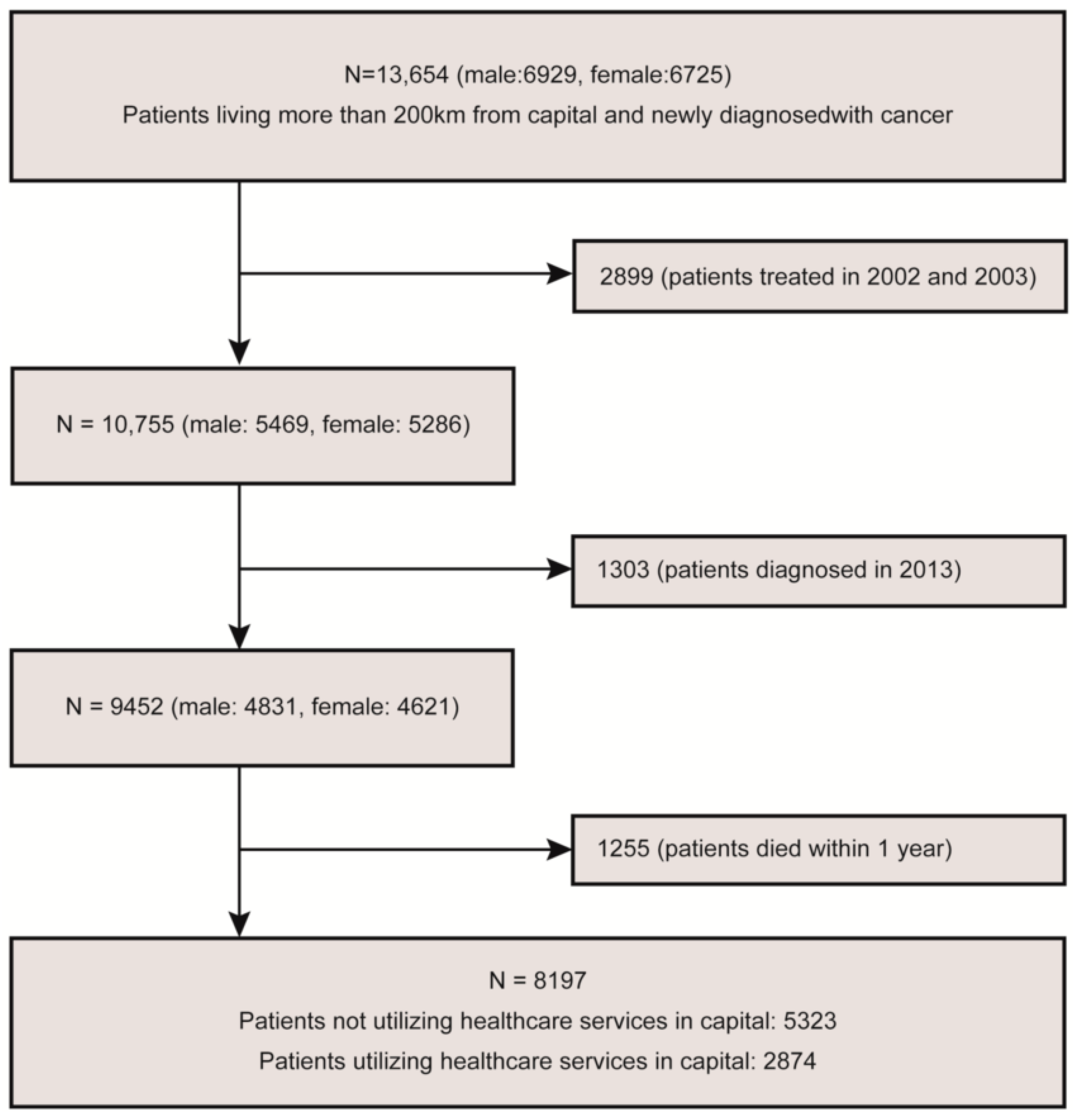
| Total | Patients Not Utilizing Healthcare Services in Capital | Patients Utilizing Healthcare Services in Capital | p-Value | ||||
|---|---|---|---|---|---|---|---|
| n | % | n | % | ||||
| Total | 8197 | 5323 | (64.9) | 2874 | (35.1) | ||
| Sex | Male | 3939 | 2445 | (62.1) | 1494 | (37.9) | <0.0001 |
| Female | 4258 | 2878 | (67.6) | 1380 | (32.4) | ||
| Age Group (Years) | ≤39 | 908 | 576 | (63.4) | 332 | (36.6) | <0.0001 |
| 40‒49 | 1379 | 882 | (64.0) | 497 | (36.0) | ||
| 50‒59 | 2099 | 1282 | (61.1) | 817 | (38.9) | ||
| 60‒69 | 2075 | 1329 | (64.0) | 746 | (36.0) | ||
| ≥70 | 1736 | 1254 | (72.2) | 482 | (27.8) | ||
| Income Level | 1 grade (lowest) | 1413 | 1057 | (74.8) | 356 | (25.2) | <0.0001 |
| 2 grade | 1045 | 738 | (70.6) | 307 | (29.4) | ||
| 3 grade | 1392 | 930 | (66.8) | 462 | (33.2) | ||
| 4 grade | 1754 | 1123 | (64.0) | 631 | (36.0) | ||
| 5 grade (highest) | 2593 | 1475 | (56.9) | 1118 | (43.1) | ||
| Type of Social Security | Medical aids | 442 | 368 | (83.3) | 74 | (16.7) | <0.0001 |
| Industrial worker | 4969 | 3174 | (63.9) | 1795 | (36.1) | ||
| Self-employed | 2786 | 1781 | (63.9) | 1005 | (36.1) | ||
| Disability | Not disabled | 7318 | 4719 | (64.5) | 2599 | (35.5) | 0.013 |
| Disabled | 879 | 604 | (68.7) | 275 | (31.3) | ||
| Chemotherapy | No | 916 | 686 | (74.9) | 230 | (25.1) | <0.0001 |
| Yes | 7281 | 4637 | (63.7) | 2644 | (36.3) | ||
| Death | No | 7363 | 4829 | (65.6) | 2534 | (34.4) | < 0.0001 |
| Yes | 834 | 494 | (59.2) | 340 | (40.8) | ||
| Total | Survival | Death | p-Value | |||
|---|---|---|---|---|---|---|
| n | % | n | % | |||
| Digestive Organs | 3304 | 2856 | (86.4) | 448 | (13.6) | |
| Not Utilizing in Capital | 1977 | 1719 | (86.9) | 258 | (13.1) | 0.2967 |
| Utilizing in Capital | 1327 | 1137 | (85.7) | 190 | (14.3) | |
| Thyroid and Other Endocrine Gland | 1489 | 1483 | (99.6) | 6 | (0.4) | |
| Not Utilizing in Capital | 1106 | 1104 | (99.8) | 2 | (0.2) | 0.0215 |
| Utilizing in Capital | 383 | 379 | (99.0) | 4 | (1.0) | |
| Breast | 694 | 656 | (94.5) | 38 | (5.5) | |
| Not Utilizing in Capital | 471 | 448 | (95.1) | 23 | (4.9) | 0.3189 |
| Utilizing in Capital | 223 | 208 | (93.3) | 15 | (6.7) | |
| Respiratory and Intrathoracic Organs | 670 | 534 | (79.7) | 136 | (20.3) | |
| Not Utilizing in Capital | 429 | 345 | (80.4) | 84 | (19.6) | 0.5375 |
| Utilizing in Capital | 241 | 189 | (78.4) | 52 | (21.6) | |
| Female Genital Organs | 454 | 428 | (94.3) | 26 | (5.7) | |
| Not Utilizing in Capital | 314 | 303 | (96.5) | 11 | (3.5) | 0.0023 |
| Utilizing in Capital | 140 | 125 | (89.3) | 15 | (10.7) | |
| Patients not Utilized in Capital | Patients Utilized in Capital | p-Value | |||
|---|---|---|---|---|---|
| Mean | SD | Mean | SD | ||
| Outpatient Visit (no.) | 15.09 | 14.61 | 17.53 (14.02) | 16.90 | <0.0001 |
| Inpatient Visit (no.) | 3.78 | 5.35 | 5.19 (4.37) | 7.94 | <0.0001 |
| Length of Stay (days) | 30.88 | 44.99 | 29.32 (22.17) | 38.65 | 0.2980 |
| Univariate Model | Multivariate Model | ||||||||
|---|---|---|---|---|---|---|---|---|---|
| HR | 95% CI | HR | 95% CI | ||||||
| Sex (ref: Male) | Female | 0.42 *** | 0.36 | −0.48 | 0.69 *** | 0.58 | −0.81 | ||
| Age Group (ref: ≤39) | 40–49 | 1.62 * | 1.07 | −2.44 | 1.67 * | 1.07 | −2.61 | ||
| 50–59 | 2.59 *** | 1.78 | −3.78 | 2.09 *** | 1.39 | −3.14 | |||
| 60–69 | 4.01 *** | 2.78 | −5.78 | 3.16 *** | 2.12 | −4.72 | |||
| ≥70 | 4.93 *** | 3.42 | −7.11 | 4.33 *** | 2.87 | −6.55 | |||
| Income level (ref: 1 Quintile) | 2 quintile | 0.96 | 0.74 | −1.24 | 0.89 | 0.66 | −1.21 | ||
| 3 quintile | 1.13 | 0.90 | −1.43 | 1.06 | 0.81 | −1.39 | |||
| 4 quintile | 1.20 | 0.97 | −1.49 | 1.14 | 0.88 | −1.47 | |||
| 5 quintile | 0.93 | 0.75 | −1.15 | 0.89 | 0.69 | −1.14 | |||
| Type of Social Security (ref: Medical Aid) | IW | 1.32 | 0.92 | −1.91 | 1.13 | 0.72 | −1.78 | ||
| SE | 1.37 | 0.94 | −1.99 | 1.13 | 0.71 | −1.78 | |||
| Disability (ref: Normal) | Handicapped | 1.52 *** | 1.25 | −1.84 | 1.27 * | 1.02 | −1.57 | ||
| Outpatient Visit(no.) | continuous | 1.02 *** | 1.02 | −1.02 | 1.00 | 1.00 | −1.00 | ||
| Inpatient visit(no.) | continuous | 1.03 *** | 1.03 | −1.04 | 1.02 *** | 1.01 | −1.03 | ||
| Length of Stay(days) | continuous | 1.01 *** | 1.01 | −1.01 | 1.01 *** | 1.00 | −1.01 | ||
| Chemotherapy (ref: No) | Yes | 18.60 *** | 7.73 | −44.77 | 16.07 ** | 2.26 | −114.34 | ||
| Utilized in Capital (ref: No) | Yes | 1.23 *** | 1.07 | −1.42 | 1.29 ** | 1.10 | −1.51 | ||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Choi, J.-k.; Kim, S.-H.; Park, M.-B. Association between Moving to a High-Volume Hospital in the Capital Area and the Mortality among Patients with Cancer: A Large Population-Based Cohort Study. Int. J. Environ. Res. Public Health 2021, 18, 3812. https://doi.org/10.3390/ijerph18073812
Choi J-k, Kim S-H, Park M-B. Association between Moving to a High-Volume Hospital in the Capital Area and the Mortality among Patients with Cancer: A Large Population-Based Cohort Study. International Journal of Environmental Research and Public Health. 2021; 18(7):3812. https://doi.org/10.3390/ijerph18073812
Chicago/Turabian StyleChoi, Jung-kyu, Se-Hyung Kim, and Myung-Bae Park. 2021. "Association between Moving to a High-Volume Hospital in the Capital Area and the Mortality among Patients with Cancer: A Large Population-Based Cohort Study" International Journal of Environmental Research and Public Health 18, no. 7: 3812. https://doi.org/10.3390/ijerph18073812
APA StyleChoi, J.-k., Kim, S.-H., & Park, M.-B. (2021). Association between Moving to a High-Volume Hospital in the Capital Area and the Mortality among Patients with Cancer: A Large Population-Based Cohort Study. International Journal of Environmental Research and Public Health, 18(7), 3812. https://doi.org/10.3390/ijerph18073812







