Physical and Psychological Factors Contributing to Incidental Falls in Older Adults Who Perceive Themselves as Unhealthy: A Cross-Sectional Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Source of Data
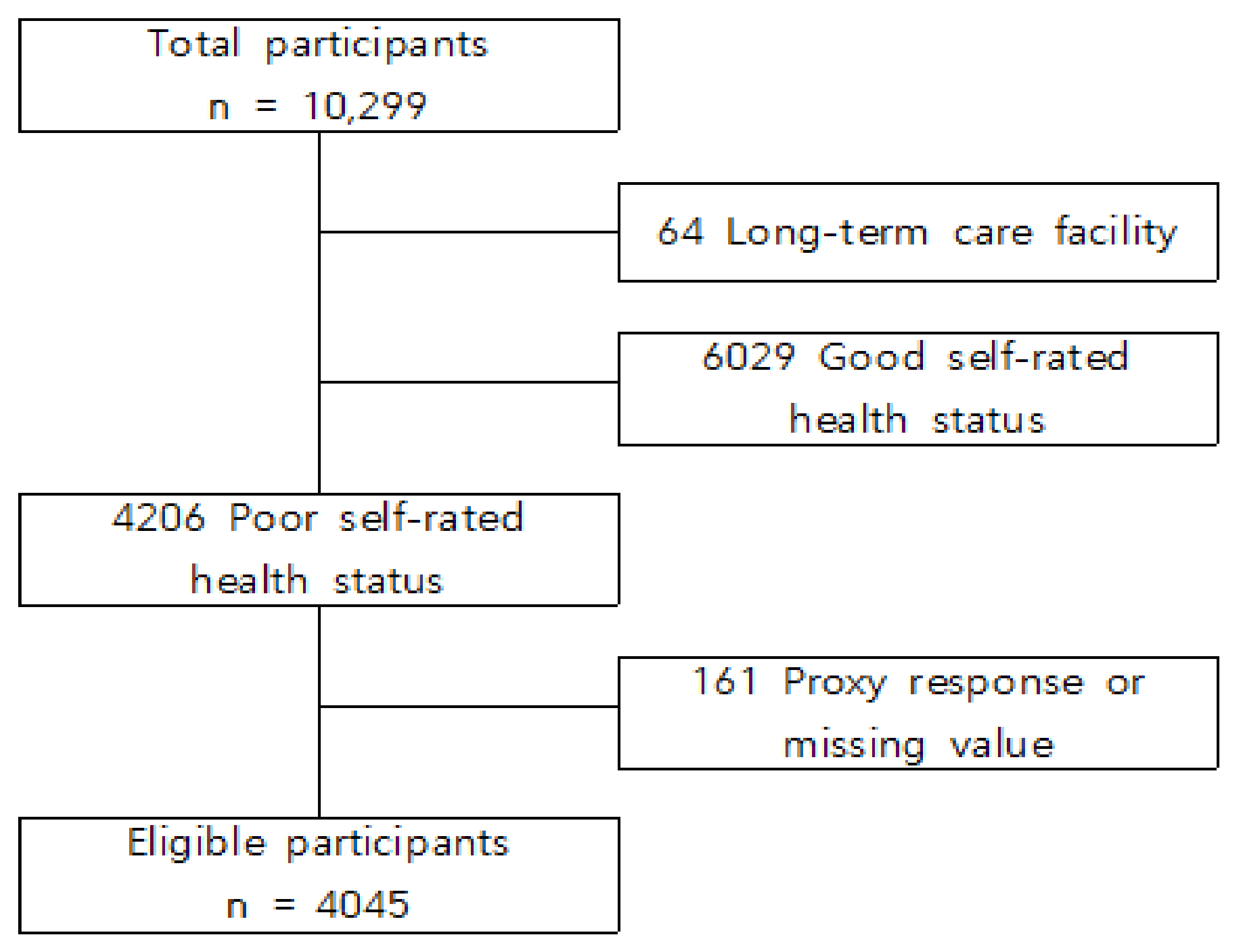
2.2. Study Design and Subjects Selection Criteria
2.3. Key Measurements
2.3.1. Falls
2.3.2. Individual Factors
2.3.3. Physical Factors
2.3.4. Psychological Factor
2.4. Statistical Analysis
3. Results
3.1. Fall Incidence and Average Number of Falls
3.2. Differences in Individual Characteristics between Groups with and without Fall History
3.3. Differences in Physical and Psychological Characteristics between Groups with and without Fall History
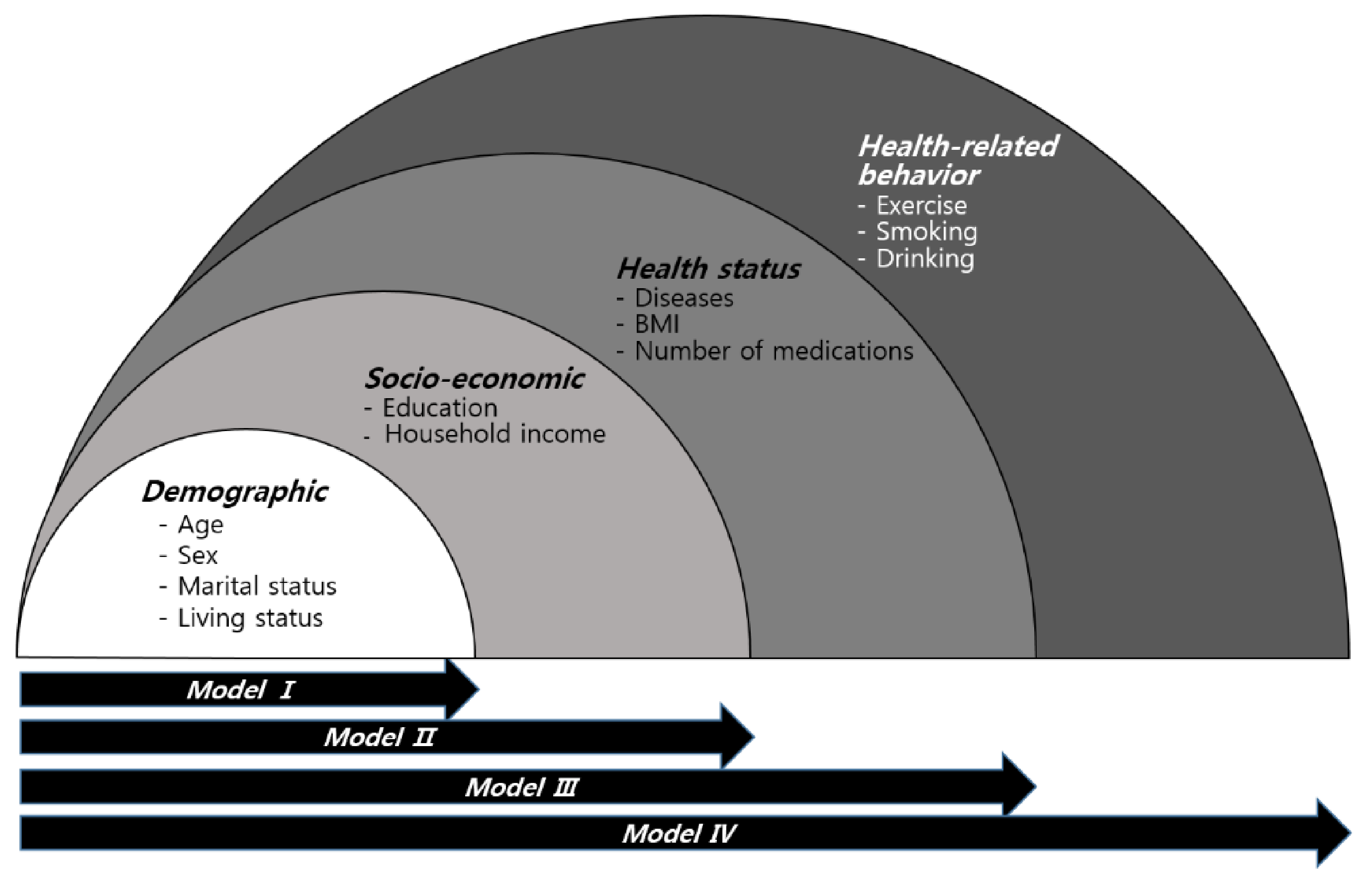
3.4. Multivariable Logistic Regression Analysis of Relevant Factors in Elderly People with Negative SRH Experiencing Falls Using Individual Variables-Adjusted Models
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- United Nations, Department of Economic and Social Affairs, Population Division. World Population Ageing 2009; United Nations, Department of Economic and Social Affairs, Population Division: New York, NY, USA, 2010; p. 73. [Google Scholar]
- Christensen, K.; Doblhammer, G.; Rau, R.; Vaupel, J.W. Ageing population: The challenges ahead. Lancet 2009, 3, 1196–1208. [Google Scholar] [CrossRef]
- Statistics Korea (KOSTAT). 2018 Population and Housing Census; Statistics Korea (KOSTAT): Daejeon, Korea, 2019. [Google Scholar]
- Statistics Korea (KOSTAT). Population Projections for Korea (2017–2067); Statistics Korea (KOSTAT): Daejeon, Korea, 2019. [Google Scholar]
- Bergen, G.; Stevens, M.R.; Burns, E.R. Falls and Fall Injuries Among Adults Aged ≥65 Years—United States, 2014. Morb. Mortal. Wkly. Rep. 2016, 65, 993–998. [Google Scholar] [CrossRef] [PubMed]
- Shumway-Cook, A.; Ciol, M.A.; Hoffman, J.; Dudgeon, B.J.; Yorkston, K.; Chan, L. Falls in the Medicare population: Incidence, associated factors, and impact on health care. Phys. Ther. 2009, 89, 324–332. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.G.; Kim, S.C.; Chang, M.; Nam, E.; Kim, S.G.; Cho, S.I.; Ryu, D.H.; Kam, S.; Choi, B.Y.; Park, S.B.; et al. Complications and Socioeconomic Costs Associated with Falls in the Elderly Population. Ann. Rehabil. Med. 2018, 42, 120–129. [Google Scholar] [CrossRef] [PubMed]
- Mossey, J.M.; Shapiro, E. Self-rated health: A predictor of mortality among the elderly. Am. J. Public Health 1982, 72, 800–808. [Google Scholar] [CrossRef] [PubMed]
- Benyamini, Y.; Idler, E.L. Community Studies Reporting Association between Self-Rated Health and Mortality: Additional Studies, 1995 to 1998. Res. Aging 1999, 21, 392–401. [Google Scholar] [CrossRef]
- Bond, J.; Dickinson, H.O.; Matthews, F.; Jagger, C.; Brayne, C. Self-rated health status as a predictor of death, functional and cognitive impairment: A longitudinal cohort study. Eur. J. Ageing 2006, 3, 193–206. [Google Scholar] [CrossRef]
- Lee, Y. The predictive value of self-assessed general, physical, and mental health on functional decline and mortality in older adults. J. Epidemiol. Community Health 2000, 54, 123–129. [Google Scholar] [CrossRef]
- Singh-Manoux, A.; Guéguen, A.; Martikainen, P.; Ferrie, J.; Marmot, M.; Shipley, M. Self-rated health and mortality: Short- and long-term associations in the Whitehall II study. Psychosom. Med. 2007, 69, 138–143. [Google Scholar] [CrossRef]
- Rohrer, J.E.; Young, R.; Sicola, V.; Houston, M. Overall self-rated health: A new quality indicator for primary care. J. Eval. Clin. Pract. 2007, 13, 150–153. [Google Scholar] [CrossRef]
- de Bruin, A.; Picavet, H.S.; Nossikov, A. Health interview surveys. Towards international harmonization of methods and instruments. WHO Reg. Publ. Eur. Ser. 1996, 58, 1–161. [Google Scholar]
- Fok, S.K.; Chair, S.Y.; Lopez, V. Sense of coherence, coping and quality of life following a critical illness. J. Adv. Nurs. 2005, 49, 173–181. [Google Scholar] [CrossRef]
- Holzhausen, M.; Martus, P. Validation of a new patient-generated questionnaire for quality of life in an urban sample of elder residents. Qual. Life Res. 2013, 22, 131–135. [Google Scholar] [CrossRef]
- Borg, C.; Hallberg, I.R.; Blomqvist, K. Life satisfaction among older people (65+) with reduced self-care capacity: The relationship to social, health and financial aspects. J. Clin. Nurs. 2006, 15, 607–618. [Google Scholar] [CrossRef]
- Gutman, G.M.; Stark, A.; Donald, A.; Beattie, B.L. Contribution of self-reported health ratings to predicting frailty, institutionalization, and death over a 5-year period. Int. Psychogeriatr. 2001, 13, 223–231. [Google Scholar] [CrossRef]
- Ayalon, L. Satisfaction with aging results in reduced risk for falling. Int. Psychogeriatr. 2016, 28, 741–747. [Google Scholar] [CrossRef]
- The Korean Institute for Health and Social Affairs. 2017 National Survey of Older Koreans: Findings and Implications; The Korean Institute for Health and Social Affairs: Seoul, Korea, 2018. [Google Scholar]
- World Health Organization. WHO Guidelines Approved by the Guidelines Review Committee. In Global Recommendations on Physical Activity for Health; World Health Organization: Geneva, Switzerland, 2010. [Google Scholar]
- Allen, J.P.; Wilson, V.B. Assessing Alcohol Problems: A Guide for Clinicians and Researchers, 2nd ed.; NIH Publication: Bethesda, MD, USA, 2003. [Google Scholar]
- Won, C.W.; Yang, K.Y.; Rho, Y.G.; Kim, S.Y.; Lee, E.J.; Yoon, J.L.; Cho, K.H.; Shin, H.C.; Cho, B.R.; Oh, J.R.; et al. The Development of Korean Activities of Daily Living(K-ADL) and Korean Instrumental Activities of Daily Living(K-IADL) Scale. J. Korean Geriatr. Soc. 2002, 6, 107–120. [Google Scholar]
- Dwyer, J. Strategies to Detect and Prevent Malnutrition in the Elderly: The Nutrition Screening Initiative. Nutr. Today 1994, 29, 14–24. [Google Scholar] [CrossRef]
- Cho, M.J.; Bae, J.N.; Suh, G.H.; Hahm, B.J.; Kim, J.K.; Lee, D.W.; Kang, M.H. Validation of Geriatric Depression Scale, Korean Version (GDS) in the Assessment of DSM-III-R Major Depression. J. Korean Neuropsychiatr. Assoc. 1999, 38, 48–63. [Google Scholar]
- Kim, T.; Choi, S.D.; Xiong, S. Epidemiology of fall and its socioeconomic risk factors in community-dwelling Korean elderly, 2020. PLoS ONE 2020, 15, e0234787. [Google Scholar] [CrossRef]
- Ebrahimi, Z.; Wilhelmson, K.; Eklund, K.; Moore, C.D.; Jakobsson, A. Health despite frailty: Exploring influences on frail older adults’ experiences of health. Geriatr. Nurs. 2013, 34, 289–294. [Google Scholar] [CrossRef]
- Young, H.M. Challenges and solutions for care of frail older adults. Online J. Issues Nurs. 2003, 8, 5. [Google Scholar]
- Jylhä, M. What is self-rated health and why does it predict mortality? Towards a unified conceptual model. Soc. Sci. Med. 2009, 69, 307–316. [Google Scholar] [CrossRef]
- Arnberg, F.K.; Lekander, M.; Morey, J.N.; Segerstrom, S.C. Self-rated health and interleukin-6: Longitudinal relationships in older adults. Brain Behav. Immun. 2016, 54, 226–232. [Google Scholar] [CrossRef]
- Christian, L.M.; Glaser, R.; Porter, K.; Malarkey, W.B.; Beversdorf, D.; Kiecolt-Glaser, J.K. Poorer self-rated health is associated with elevated inflammatory markers among older adults. Psychoneuroendocrinology 2011, 36, 1495–1504. [Google Scholar] [CrossRef]
- Tamura, T.; Naito, M.; Maruyama, K.; Tsukamoto, M.; Sasakabe, T.; Okada, R.; Kawai, S.; Hishida, A.; Wakai, K. The association between self-rated health and high-sensitivity C-reactive protein level: A cross-sectional and 5-year longitudinal study. BMC Public Health 2018, 18, 1380. [Google Scholar] [CrossRef]
- Undén, A.L.; Andréasson, A.; Elofsson, S.; Brismar, K.; Mathsson, L.; Rönnelid, J.; Lekander, M. Inflammatory cytokines, behaviour and age as determinants of self-rated health in women. Clin. Sci. 2007, 112, 363–373. [Google Scholar] [CrossRef][Green Version]
- Lekander, M.; Elofsson, S.; Neve, I.M.; Hansson, L.O.; Undén, A.L. Self-rated health is related to levels of circulating cytokines. Psychosom. Med. 2004, 66, 559–563. [Google Scholar] [CrossRef]
- Dantzer, R. Cytokine, sickness behavior, and depression. Neurol. Clin. 2006, 24, 441–460. [Google Scholar] [CrossRef]
- Leshem-Rubinow, E.; Shenhar-Tsarfaty, S.; Milwidsky, A.; Toker, S.; Shapira, I.; Berliner, S.; Benyamini, Y.; Melamed, S.; Rogowski, O. Self-rated health is associated with elevated C-reactive protein even among apparently healthy individuals. Isr. Med. Assoc. J. 2015, 17, 213–218. [Google Scholar]
- Shimada, H.; Suzukawa, M.; Ishizaki, T.; Kobayashi, K.; Kim, H.; Suzuki, T. Relationship between subjective fall risk assessment and falls and fall-related fractures in frail elderly people. BMC Geriatr. 2011, 11, 40. [Google Scholar] [CrossRef] [PubMed]
- Singh, D.K.A.; Shahar, S.; Vanoh, D.; Kamaruzzaman, S.B.; Tan, M.P. Diabetes, arthritis, urinary incontinence, poor self-rated health, higher body mass index and lower handgrip strength are associated with falls among community-dwelling middle-aged and older adults: Pooled analyses from two cross-sectional Malaysian datasets. Geriatr. Gerontol. Int. 2019, 19, 798–803. [Google Scholar] [CrossRef] [PubMed]
- Agmon, M.; Lavie, L.; Doumas, M. The Association between Hearing Loss, Postural Control, and Mobility in Older Adults: A Systematic Review. J. Am. Acad. Audiol. 2017, 28, 575–588. [Google Scholar] [CrossRef] [PubMed]
- Peterka, R.J. Sensorimotor integration in human postural control. J. Neurophysiol. 2002, 88, 1097–1118. [Google Scholar] [CrossRef] [PubMed]
- Lin, F.R.; Ferrucci, L. Hearing loss and falls among older adults in the United States. Arch. Intern. Med. 2012, 172, 369–371. [Google Scholar] [CrossRef]
- Jiam, N.T.; Li, C.; Agrawal, Y. Hearing loss and falls: A systematic review and meta-analysis. Laryngoscope 2016, 126, 2587–2596. [Google Scholar] [CrossRef]
- Lin, F.R.; Niparko, J.K.; Ferrucci, L. Hearing loss prevalence in the United States. Arch. Intern. Med. 2011, 171, 1851–1852. [Google Scholar] [CrossRef]
- Eikema, D.J.; Hatzitaki, V.; Tzovaras, D.; Papaxanthis, C. Age-dependent modulation of sensory reweighting for controlling posture in a dynamic virtual environment. Age 2012, 34, 1381–1392. [Google Scholar] [CrossRef]
- Doumas, M.; Krampe, R.T. Adaptation and reintegration of proprioceptive information in young and older adults’ postural control. J. Neurophysiol. 2010, 104, 1969–1977. [Google Scholar] [CrossRef]
- Mulrow, C.D.; Tuley, M.R.; Aguilar, C. Sustained benefits of hearing aids. J. Speech Lang. Hear. Res. 1992, 35, 1402–1405. [Google Scholar] [CrossRef]
- Mick, P.; Kawachi, I.; Lin, F.R. The association between hearing loss and social isolation in older adults. Otolaryngol. Head Neck Surg. 2014, 150, 378–384. [Google Scholar] [CrossRef]
- Brink, P.; Stones, M. Examination of the relationship among hearing impairment, linguistic communication, mood, and social engagement of residents in complex continuing-care facilities. Gerontologist 2007, 47, 633–641. [Google Scholar] [CrossRef]
- Hornsby, B.W.; Kipp, A.M. Subjective Ratings of Fatigue and Vigor in Adults with Hearing Loss Are Driven by Perceived Hearing Difficulties Not Degree of Hearing Loss. Ear Hear. 2016, 37, e1–e10. [Google Scholar] [CrossRef]
- Gopinath, B.; Schneider, J.; Hickson, L.; McMahon, C.M.; Burlutsky, G.; Leeder, S.R.; Mitchell, P. Hearing handicap, rather than measured hearing impairment, predicts poorer quality of life over 10 years in older adults. Maturitas 2012, 72, 146–151. [Google Scholar] [CrossRef]
- Çinarli, T.; Koç, Z. Fear and Risk of Falling, Activities of Daily Living, and Quality of Life: Assessment When Older Adults Receive Emergency Department Care. Nurs. Res. 2017, 66, 330–335. [Google Scholar] [CrossRef]
- Lord, S.R.; Close, J.C.T. New horizons in falls prevention. Age Ageing 2018, 47, 492–498. [Google Scholar] [CrossRef] [PubMed]
- Iaboni, A.; Flint, A.J. The complex interplay of depression and falls in older adults: A clinical review. Am. J. Geriatr. Psychiatry 2013, 21, 484–492. [Google Scholar] [CrossRef]
- McDermott, L.M.; Ebmeier, K.P. A meta-analysis of depression severity and cognitive function. J. Affect. Disord. 2009, 119, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Wright, S.L.; Kay, R.E.; Avery, E.T.; Giordani, B.; Alexander, N.B. The impact of depression on dual tasking among patients with high fall risk. J. Geriatr. Psychiatry Neurol. 2011, 24, 142–150. [Google Scholar] [CrossRef] [PubMed]
- Woolcott, J.C.; Richardson, K.J.; Wiens, M.O.; Patel, B.; Marin, J.; Khan, K.M.; Marra, C.A. Meta-analysis of the impact of 9 medication classes on falls in elderly persons. Arch. Intern. Med. 2009, 169, 1952–1960. [Google Scholar] [CrossRef] [PubMed]
- Thapa, P.B.; Gideon, P.; Cost, T.W.; Milam, A.B.; Ray, W.A. Antidepressants and the risk of falls among nursing home residents. N. Engl. J. Med. 1998, 339, 875–882. [Google Scholar] [CrossRef]
| Variables | Classification | Without Fall | With Fall | χ2 | p | |
|---|---|---|---|---|---|---|
| (n = 3105) | (n = 940) | |||||
| n (%) or | n (%) or | |||||
| M ± SD * | M ± SD * | |||||
| Demographic | Age | 75.4 ± 6.2 | 76.2 ± 6.2 | 3.29 | 0.001 | |
| Sex | Male | 1047 (33.7) | 233 (24.8) | 26.62 | <0.001 | |
| Female | 2058 (66.3) | 707 (75.2) | ||||
| Marital status | Living with spouse | 1817 (58.5) | 433 (46.1) | 45.35 | <0.001 | |
| Living without spouse | 1288 (41.5) | 507 (53.9) | ||||
| Living status | Alone | 859 (27.7) | 337 (35.8) | 38.92 | <0.001 | |
| Living with spouse | 1456 (46.9) | 341 (36.3) | ||||
| Living with children | 675 (21.7) | 234 (24.9) | ||||
| Others | 115 (3.7) | 28 (3.0) | ||||
| Socioeconomic | Education | 0–6 years | 2228 (71.7) | 687 (73.1) | 3.99 | 0.263 |
| 7–9 years | 422 (13.6) | 127 (13.5) | ||||
| 10–12 years | 341 (11.0) | 104 (11.1) | ||||
| ≥13 years | 114 (3.7) | 22 (2.3) | ||||
| Quantiles of household income | Q1 (lowest) | 827 (26.6) | 312 (33.2) | 22.84 | <0.001 | |
| Q2 | 745 (24.0) | 182 (19.4) | ||||
| Q3 | 636 (20.5) | 180 (19.1) | ||||
| Q4 | 517 (16.7) | 134 (14.3) | ||||
| Q5 (highest) | 380 (12.2) | 132 (14.0) | ||||
| Health status | Disease | Hypertension | 2043 (65.8) | 673 (71.6) | 11.00 | 0.001 |
| Diabetes | 978 (31.5) | 328 (34.9) | 3.81 | 0.051 | ||
| Dementia | 78 (2.5) | 33 (3.5) | 2.70 | 0.101 | ||
| Arthritis | 1495 (48.1) | 517 (55.0) | 13.55 | <0.001 | ||
| BMI ** | Underweight (<18.5) | 164 (5.3) | 55 (5.9) | 1.66 | 0.646 | |
| Normal (≥18.5, <25) | 1992 (64.1) | 583 (62.0) | ||||
| Overweight (≥25) | 949 (30.6) | 302 (32.1) | ||||
| Number of medication(s) | 0 | 157 (5.0) | 29 (3.1) | 258.00 | <0.001 | |
| 1 | 170 (5.5) | 29 (3.1) | ||||
| 2 | 241 (7.8) | 64 (6.8) | ||||
| ≥3 | 2537 (81.7) | 818 (87.0) | ||||
| Health-relatedBehavior | Exercise | None | 1308 (42.1) | 429 (45.6) | 4.63 | 0.099 |
| <150 min. a week | 680 (21.9) | 206 (21.9) | ||||
| ≥150 min. a week | 1117 (36.0) | 305 (32.5) | ||||
| Smoking | Past/Never | 2859 (92.1) | 872 (92.8) | 0.48 | 0.489 | |
| Current | 246 (7.9) | 68 (7.2) | ||||
| Drinking | None | 2558 (82.4) | 794 (84.5) | 3.25 | 0.197 | |
| ≤1 standard drink/day | 243 (7.8) | 72 (7.6) | ||||
| >1 standard drink/day | 304 (9.8) | 74 (7.9) | ||||
| Physical and Psychological Variables | Classification | Without Fall | With Fall | χ2 | p | |
|---|---|---|---|---|---|---|
| (n = 3105) | (n = 940) | |||||
| n (%) | n (%) | |||||
| Physical | Visual discomfort | No | 1760 (56.7) | 488 (51.9) | 6.64 | 0.010 |
| Yes | 1345 (43.3) | 452 (48.1) | ||||
| Hearing discomfort | No | 2375 (76.5) | 656 (69.8) | 17.26 | <0.001 | |
| Yes | 730 (23.5) | 284 (30.2) | ||||
| ADL * limitation | No | 2710 (87.3) | 738 (78.5) | 44.09 | <0.001 | |
| Yes | 395 (12.7) | 202 (21.5) | ||||
| IADL ** limitation | No | 1895 (61.0) | 445 (47.3) | 55.46 | <0.001 | |
| Yes | 1210 (39.0) | 495 (52.7) | ||||
| Nutrition | Good | 1222 (39.4) | 284 (30.2) | 25.81 | <0.001 | |
| Poor | 1883 (60.6) | 656 (69.8) | ||||
| Psychological | Depression | No | 1944 (62.6) | 473 (50.3) | 45.32 | <0.001 |
| Yes | 1161 (37.4) | 467 (49.7) | ||||
| Variables | Model I | Model II | Model III | Model IV |
|---|---|---|---|---|
| OR (95% CI) | OR (95% CI) | OR (95% CI) | OR (95% CI) | |
| Visual discomfort | 1.04 (0.89–1.22) | 1.05 (0.90–1.23) | 1.04 (0.89–1.21) | 1.04 (0.89–1.22) |
| Hearing discomfort | 1.31 (1.10–1.56) * | 1.31 (1.10–1.56) * | 1.30 (1.09–1.55) * | 1.30 (1.09–1.55) * |
| ADL limitation | 1.41 (1.14–1.74) * | 1.39 (1.13–1.72) * | 1.39 (1.13–1.73) * | 1.40 (1.13–1.74) * |
| IADL limitation | 1.33 (1.12–1.58) * | 1.34 (1.13–1.60) * | 1.34 (1.12–1.60) * | 1.34 (1.13–1.61) * |
| Poor nutrition | 1.18 (1.00–1.40) * | 1.19 (1.01–1.41) * | 1.12 (0.94–1.33) | 1.12 (0.94–1.33) |
| Depression | 1.39 (1.19–1.63) * | 1.42 (1.21–1.66) * | 1.43 (1.22–1.68) * | 1.44 (1.23–1.69) * |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Byun, M.; Kim, J.; Kim, J.E. Physical and Psychological Factors Contributing to Incidental Falls in Older Adults Who Perceive Themselves as Unhealthy: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2021, 18, 3738. https://doi.org/10.3390/ijerph18073738
Byun M, Kim J, Kim JE. Physical and Psychological Factors Contributing to Incidental Falls in Older Adults Who Perceive Themselves as Unhealthy: A Cross-Sectional Study. International Journal of Environmental Research and Public Health. 2021; 18(7):3738. https://doi.org/10.3390/ijerph18073738
Chicago/Turabian StyleByun, Mikyong, Jiyeon Kim, and Ji Eun Kim. 2021. "Physical and Psychological Factors Contributing to Incidental Falls in Older Adults Who Perceive Themselves as Unhealthy: A Cross-Sectional Study" International Journal of Environmental Research and Public Health 18, no. 7: 3738. https://doi.org/10.3390/ijerph18073738
APA StyleByun, M., Kim, J., & Kim, J. E. (2021). Physical and Psychological Factors Contributing to Incidental Falls in Older Adults Who Perceive Themselves as Unhealthy: A Cross-Sectional Study. International Journal of Environmental Research and Public Health, 18(7), 3738. https://doi.org/10.3390/ijerph18073738






