The Difficult Balance between Ensuring the Right of Nursing Home Residents to Communication and Their Safety
Abstract
1. Introduction
2. Protecting the Right of Elderly People to Social Contact
- (a)
- Residents of facilities for which the implementation of preventive measures, including “physical distancing and restrictions on social contact, has caused a reduction in interaction between individuals and in social-emotional connections, which, in a population of frail, cognitively unstable individuals, may result in further psycho-emotional degradation. This, in turn, may increase the risk of deterioration of organic diseases.”
- (b)
- Family members of residents who “have had to cope with being distant from their loved one and with the consequent difficulty in providing emotional support and assistance.”
- Perform rapid antigen tests on visitors authorized by the facility manager.
- Perform molecular tests to screen new resident admissions and facility staff.
- Suspend visitor access to residential and nursing homes when a COVID-19 case or cluster has been identified, with the opportunity to “visit patients in isolation or quarantine, in cases authorized by the facility managers” and “increasing the options for distanced interaction using various methods and ensuring family members are provided constant information on the residents’ health condition.”
- Suspend new admissions in residential and nursing homes when cases have been identified among the residents.
- Organize visitation in the event of end-of-life situations of patients affected by COVID-19.
- Organizational and infection prevention measures.
3. Managing Distanced Interaction
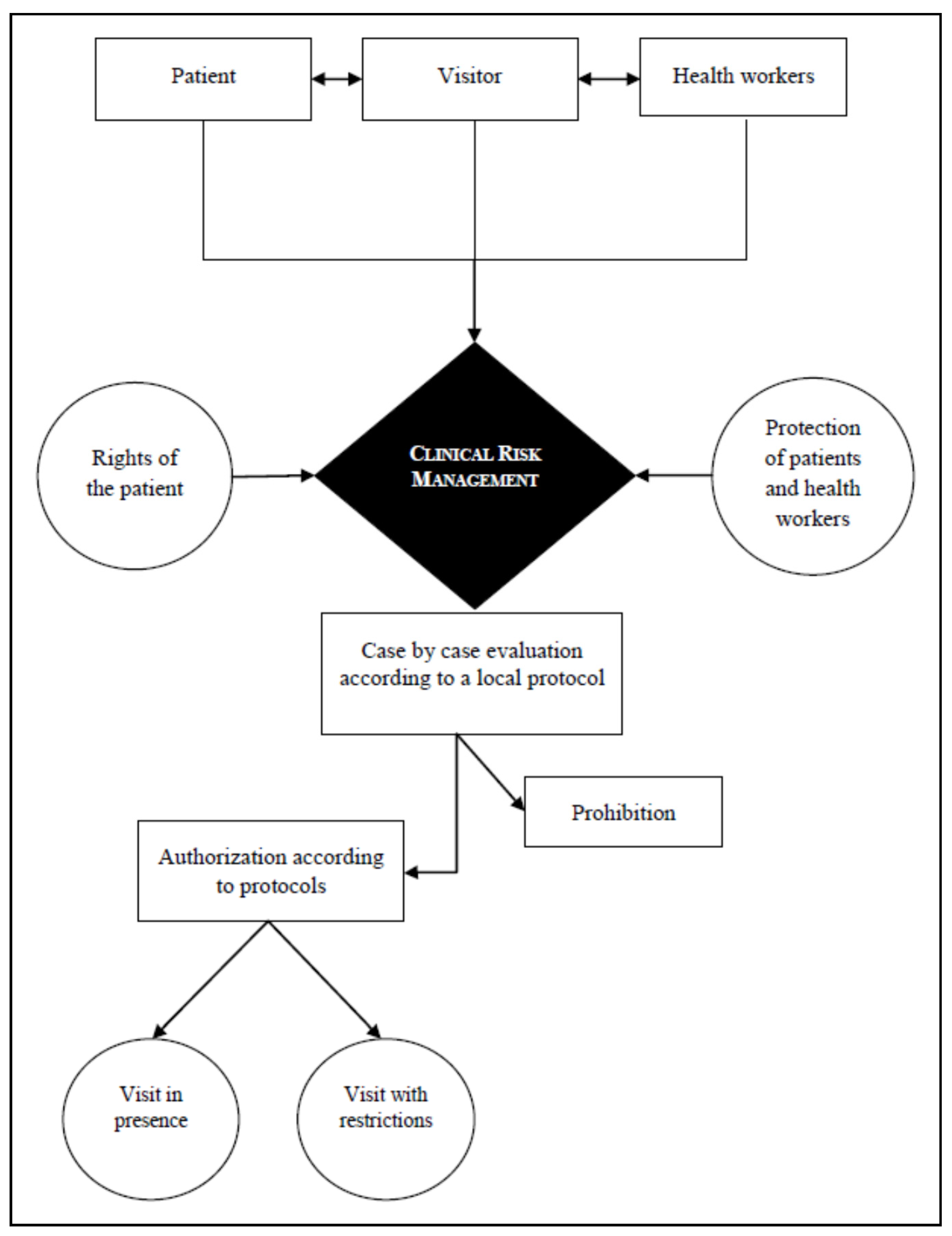
4. Clinical Risk Management
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Miller, I.F.; Becker, A.D.; Grenfell, B.T.; Metcalf, C.J.E. Disease and healthcare burden of COVID-19 in the United States. Nat. Med. 2020, 26, 1212–1217. [Google Scholar] [CrossRef]
- Cimerman, S.; Chebabo, A.; Cunha, C.A.D.; Rodríguez-Morales, A.J. Deep impact of COVID-19 in the healthcare of Latin America: The case of Brazil. Braz. J. Infect. Dis. 2020, 24, 93–95. [Google Scholar] [CrossRef]
- Grech, V. Malta’s healthcare escalation for COVID-19. J. Vis. Commun. Med. 2020, 43, 153–161. [Google Scholar] [CrossRef]
- Bolcato, M.; Russo, M.; Rodriguez, D.; Aprile, A. Patient blood management implementation in light of new Italian laws on patient’s safety. Transfus. Apher. Sci. 2020, 59, 102811. [Google Scholar] [CrossRef]
- Bolcato, M.; Rodriguez, D.; Aprile, A. Risk Management in the New Frontier of Professional Liability for Nosocomial Infection: Review of the Literature on Mycobacterium Chimaera. Int. J. Environ. Res. Public Health 2020, 17, 7328. [Google Scholar] [CrossRef]
- Scopetti, M.; Santurro, A.; Tartaglia, R.; Frati, P.; Fineschi, V. Expanding frontiers of risk management: Care safety in nursing home during COVID-19 pandemic. Int. J. Qual. Health Care 2020. Epub ahead of print. [Google Scholar] [CrossRef]
- Stall, N.M.; Farquharson, C.; Fan-Lun, C.; Wiesenfeld, L.; Loftus, C.A.; Kain, D.; Johnstone, J.; McCreight, L.; Goldman, R.D.; Mahtani, R. A Hospital Partnership with a Nursing Home Experiencing a COVID-19 Outbreak: Description of a Multiphase Emergency Response in Toronto, Canada. J. Am. Geriatr. Soc. 2020, 68, 1376–1381. [Google Scholar] [CrossRef]
- Rubin, R. The Challenge of Preventing COVID-19 Spread in Correctional Facilities. JAMA 2020, 323, 1760–1761. [Google Scholar] [CrossRef]
- Ouslander, J.G.; Grabowski, D.C. COVID-19 in Nursing Homes: Calming the Perfect Storm. J. Am. Geriatr. Soc. 2020, 68, 2153–2162. [Google Scholar] [CrossRef]
- Heudorf, U.; Müller, M.; Schmehl, C.; Gasteyer, S.; Steul, K. COVID-19 in long-term care facilities in Frankfurt am Main, Germany: Incidence, case reports, and lessons learned. GMS Hyg. Infect. Control 2020, 15, Doc26. [Google Scholar] [CrossRef]
- Davidson, P.M.; Szanton, S.L. Nursing homes and COVID-19: We can and should do better. J. Clin. Nurs. 2020, 29, 2758–2759. [Google Scholar] [CrossRef]
- McMichael, T.M.; Currie, D.W.; Clark, S.; Pogosjans, S.; Kay, M.; Schwartz, N.G.; Lewis, J.; Baer, A.; Kawakami, V.; Lukoff, M.D.; et al. Epidemiology of Covid-19 in a Long-Term Care Facility in King County, Washington. N. Engl. J. Med. 2020, 382, 2005–2011. [Google Scholar] [CrossRef]
- Grabowski, D.C.; Mor, V. Nursing Home Care in Crisis in the Wake of COVID-19. JAMA 2020, 324, 23–24. [Google Scholar] [CrossRef]
- Fisman, D.N.; Bogoch, I.; Lapointe-Shaw, L.; McCready, J.; Tuite, A.R. Risk Factors Associated With Mortality Among Residents With Coronavirus Disease 2019 (COVID-19) in Long-term Care Facilities in Ontario, Canada. JAMA Netw. Open 2020, 3, e2015957. [Google Scholar] [CrossRef]
- Stall, N.M.; Jones, A.; Brown, K.A.; Rochon, P.A.; Costa, A.P. For-profit long-term care homes and the risk of COVID-19 outbreaks and resident deaths. CMAJ 2020, 192, E946–E955. [Google Scholar] [CrossRef]
- Trabucchi, M.; De Leo, D. Nursing homes or besieged castles: COVID-19 in northern Italy. Lancet Psychiatry 2020, 7, 387–388. [Google Scholar] [CrossRef]
- Arons, M.M.; Hatfield, K.M.; Reddy, S.C.; Kimball, A.; James, A.; Jacobs, J.R.; Taylor, J.; Spicer, K.; Bardossy, A.C.; Oakley, L.P.; et al. Presymptomatic SARS-CoV-2 Infections and Transmission in a Skilled Nursing Facility. N. Engl. J. Med. 2020, 382, 2081–2090. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; He, W.; Yu, X.; Hu, D.; Bao, M.; Liu, H.; Zhou, J.; Jiang, H. Coronavirus disease 2019 in elderly patients: Characteristics and prognostic factors based on 4-week follow-up. J. Infect. 2020, 80, 639–645. [Google Scholar] [CrossRef]
- Niu, S.; Tian, S.; Lou, J.; Kang, X.; Zhang, L.; Lian, H.; Zhang, J. Clinical characteristics of older patients infected with COVID-19: A descriptive study. Arch. Gerontol. Geriatr. 2020, 89, 104058. [Google Scholar] [CrossRef]
- Applegate, W.B.; Ouslander, J.G. COVID-19 Presents High Risk to Older Persons. J. Am. Geriatr. Soc. 2020, 68, 681. [Google Scholar] [CrossRef]
- Davies, N.G.; Klepac, P.; Liu, Y.; Prem, K.; Jit, M.; CMMID COVID-19 Working Group; Eggo, R.M. Age-dependent effects in the transmission and control of COVID-19 epidemics. Nat. Med. 2020, 26, 1205–1211. [Google Scholar] [CrossRef]
- McGarry, B.E.; Grabowski, D.C.; Barnett, M.L. Severe Staffing and Personal Protective Equipment Shortages Faced By Nursing Homes during The COVID-19 Pandemic. Health Aff. 2020, 39, 1812–1821. [Google Scholar] [CrossRef]
- Bolcato, M.; Trabucco Aurilio, M.; Aprile, A.; Di Mizio, G.; Della Pietra, B.; Feola, A. Take-Home Messages from the COVID-19 Pandemic: Strengths and Pitfalls of the Italian National Health Service from a Medico-Legal Point of View. Healthcare 2020, 9, 17. [Google Scholar] [CrossRef]
- Nienhaus, A.; Hod, R. COVID-19 among Health Workers in Germany and Malaysia. Int. J. Environ. Res. Public Health 2020, 17, 4881. [Google Scholar] [CrossRef]
- Coppeta, L.; Somma, G.; Ippoliti, L.; Ferrari, C.; D’Alessandro, I.; Pietroiusti, A.; Trabucco Aurilio, M. Contact Screening for Healthcare Workers Exposed to Patients with COVID-19. Int. J. Environ. Res. Public Health 2020, 17, 9082. [Google Scholar] [CrossRef]
- Abbasi, J. Social Isolation-the Other COVID-19 Threat in Nursing Homes. JAMA 2020, 324, 619–620. [Google Scholar] [CrossRef]
- Bergman, C.; Stall, N.M.; Haimowitz, D.; Aronson, L.; Lynn, J.; Steinberg, K.; Wasserman, M. Recommendations for Welcoming Back Nursing Home Visitors During the COVID-19 Pandemic: Results of a Delphi Panel. J. Am. Med. Dir. Assoc. 2020, 21, 1759–1766. [Google Scholar] [CrossRef]
- Monin, J.K.; Ali, T.; Syed, S.; Piechota, A.; Lepore, M.; Mourgues, C.; Gaugler, J.E.; Marottoli, R.; David, D. Family Communication in Long-Term Care During a Pandemic: Lessons for Enhancing Emotional Experiences. Am. J. Geriatr. Psychiatry 2020, 28, 1299–1307. [Google Scholar] [CrossRef]
- Hado, E.; Friss Feinberg, L. Amid the COVID-19 Pandemic, Meaningful Communication between Family Caregivers and Residents of Long-Term Care Facilities is Imperative. J. Aging Soc. Policy 2020, 32, 410–415. [Google Scholar] [CrossRef]
- Schlaudecker, J.D. Essential Family Caregivers in Long-Term Care during the COVID-19 Pandemic. J. Am. Med. Dir. Assoc. 2020, 21, 983. [Google Scholar] [CrossRef]
- Benatti, S.V. Love in the Time of Corona. Ann. Intern. Med. 2020, 172, 628. [Google Scholar] [CrossRef]
- Decreto del Presidente del Consiglio dei Ministri dell’8 marzo 2020. Ulteriori disposizioni attuative del decreto-legge 23 febbraio 2020, n. 6, recante misure urgenti in materia di contenimento e gestione dell’emergenza epidemiologica da COVID-19. (20A01522) (GU Serie Generale n. 59 del 08-03-2020). Available online: https://www.gazzettaufficiale.it/eli/id/2020/03/08/20A01522/sg (accessed on 7 February 2021).
- Ulteriori disposizioni attuative del decreto-legge 25 marzo 2020, n. 19, convertito, con modificazioni, dalla legge 25 maggio 2020, n. 35, recante «Misure urgenti per fronteggiare l’emergenza epidemiologica da COVID-19», e del decreto-legge 16 maggio 2020, n. 33, convertito, con modificazioni, dalla legge 14 luglio 2020, n. 74, recante «Ulteriori misure urgenti per fronteggiare l’emergenza epidemiologica da COVID-19». (20A06109) (GU Serie Generale n.275 del 04-11-2020-Suppl. Ordinario n. 41). Available online: https://www.gazzettaufficiale.it/eli/id/2020/11/04/20A06109/sg (accessed on 7 February 2021).
- Indicazioni ad Interim per la Prevenzione e il Controllo Dell’infezione da SARS-CoV-2 in Strutture Residenziali Sociosanitarie e Socioassistenziali. Available online: https://www.iss.it/documents/20126/0/Rapporto+ISS+COVID-19+n.+4-2020_Rev.+2+%281%29.pdf/54f1745b-adef-935d-9b2a-09e875b14481?t=1599145436882 (accessed on 7 February 2021).
- World Health Organization. Infection Prevention and Control during Health Care when Coronavirus Disease (COVID-19) is Suspected or Confirmed. Interim guidance 29 June 2020. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-IPC-2020.4 (accessed on 7 February 2021).
- Covid-19, Indicazioni per L'assistenza a Domicilio e per L'accesso dei Visitatori nelle Strutture Residenziali Sociosanitarie. Available online: http://www.salute.gov.it/portale/nuovocoronavirus/dettaglioNotizieNuovoCoronavirus.jsp?lingua=italiano&id=5201 (accessed on 7 February 2021).
- European Centre for Disease Prevention and Control. Surveillance of COVID-19 in Long-Term Care Facilities in the EU/EEA, 19 May 2020. Stockholm: ECDC. Available online: https://www.ecdc.europa.eu/sites/default/files/documents/covid-19-long-term-care-facilities-surveillance-guidance.pdf (accessed on 7 February 2021).
- European Centre for Disease Prevention and Control. Guidance for Discharge and Ending Isolation in the Context of Widespread Community Transmission of COVID-19–First Update, 8 April 2020, Stockholm: ECDC. Available online: https://www.ecdc.europa.eu/sites/default/files/documents/covid-19-guidance-discharge-and-ending-isolation-first%20update.pdf (accessed on 7 February 2021).
- ISS Survey Nazionale sul Contagio COVID-19 nelle Strutture Residenziali e Sociosanitarie REPORT FINALE 05.05.2020. Available online: https://www.epicentro.iss.it/coronavirus/pdf/sars-cov-2-survey-rsa-rapporto-finale.pdf (accessed on 7 February 2021).
- Amnesty International. Italy: Violations of the Human Rights of Older Residents of Care Homes during COVID-19 Pandemic. Available online: https://www.amnesty.org/en/latest/news/2020/12/italyviolations-of-the-h-uman-rights-of-older-residents-of-care-homes-during-covid-19-pandemic/ (accessed on 7 February 2021).
- Gerst-Emerson, K.; Jayawardhana, J. Loneliness as a public health issue: The impact of loneliness on health care utilization among older adults. Am. J. Public Health 2015, 105, 1013–1019. [Google Scholar] [CrossRef]
- Zhong, B.L.; Chen, S.L.; Conwell, Y. Effects of Transient Versus Chronic Loneliness on Cognitive Function in Older Adults: Findings From the Chinese Longitudinal Healthy Longevity Survey. Am. J. Geriatr. Psychiatry 2016, 24, 389–398. [Google Scholar] [CrossRef] [PubMed]
- Lim, K.K.; Chan, A. Association of loneliness and healthcare utilization among older adults in Singapore. Geriatr. Gerontol. Int. 2017, 17, 1789–1798. [Google Scholar] [CrossRef] [PubMed]
- Santini, Z.I.; Jose, P.E.; York Cornwell, E.; Koyanagi, A.; Nielsen, L.; Hinrichsen, C.; Meilstrup, C.; Madsen, K.R.; Koushede, V. Social disconnectedness, perceived isolation, and symptoms of depression and anxiety among older Americans (NSHAP): A longitudinal mediation analysis. Lancet Public Health 2020, 5, e62–e70. [Google Scholar] [CrossRef]
- Armitage, R.; Nellums, L.B. COVID-19 and the consequences of isolating the elderly. Lancet Public Health 2020, 5, e256. [Google Scholar] [CrossRef]
- O’Caoimh, R.; O’Donovan, M.R.; Monahan, M.P.; O’Connor, C.D.; Buckley, C.; Kilty, C.; Fitzgerald, S.; Hartigan, I.; Cornally, N. Psychosocial Impact of COVID-19 Nursing Home Restrictions on Visitors of Residents With Cognitive Impairment: A Cross-Sectional Study as Part of the Engaging Remotely in Care (ERiC) Project. Front. Psychiatry 2020, 11, 585373. [Google Scholar] [CrossRef]
- Nguyen, M.; Pachana, N.A.; Beattie, E.; Fielding, E.; Ramis, M.A. Effectiveness of interventions to improve family-staff relationships in the care of people with dementia in residential aged care: A systematic review protocol. JBI Database Syst. Rev. Implement Rep. 2015, 13, 52–63. [Google Scholar] [CrossRef] [PubMed]
- Cluver, L.; Lachman, J.M.; Sherr, L.; Wessels, I.; Krug, E.; Rakotomalala, S.; Blight, S.; Hillis, S.; Bachman, G.; Green, O.; et al. Parenting in a time of COVID-19. Lancet 2020, 395, e64. [Google Scholar] [CrossRef]
- Plagg, B.; Engl, A.; Piccoliori, G.; Eisendle, K. Prolonged social isolation of the elderly during COVID-19: Between benefit and damage. Arch. Gerontol Geriatr. 2020, 89, 104086. [Google Scholar] [CrossRef]
- McMichael, T.M.; Clark, S.; Pogosjans, S.; Kay, M.; Lewis, J.; Baer, A.; Kawakami, V.; Lukoff, M.D.; Ferro, J.; Brostrom-Smith, C.; et al. COVID-19 in a Long-Term Care Facility-King County, Washington, February 27–March 9, 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 339–342. [Google Scholar] [CrossRef] [PubMed]
- Verbeek, H.; Gerritsen, D.L.; Backhaus, R.; de Boer, B.S.; Koopmans, R.T.C.M.; Hamers, J.P.H. Allowing Visitors Back in the Nursing Home during the COVID-19 Crisis: A Dutch National Study Into First Experiences and Impact on Well-Being. J. Am. Med. Dir. Assoc. 2020, 21, 900–904. [Google Scholar] [CrossRef]
- Hart, J.L.; Turnbull, A.E.; Oppenheim, I.M.; Courtright, K.R. Family-Centered Care during the COVID-19 Era. J. Pain Symptom Manag. 2020, 60, e93–e97. [Google Scholar] [CrossRef]
- Simard, J.; Volicer, L. Loneliness and Isolation in Long-term Care and the COVID-19 Pandemic. J. Am. Med. Dir. Assoc. 2020, 21, 966–967. [Google Scholar] [CrossRef] [PubMed]
- Banskota, S.; Healy, M.; Goldberg, E.M. 15 Smartphone Apps for Older Adults to Use While in Isolation during the COVID-19 Pandemic. West. J. Emerg. Med. 2020, 21, 514–525. [Google Scholar] [CrossRef] [PubMed]
- Levin, T.T.; Moreno, B.; Silvester, W.; Kissane, D.W. End-of-life communication in the intensive care unit. Gen. Hosp. Psychiatry 2010, 32, 433–442. [Google Scholar] [CrossRef]
- Lind, R.; Lorem, G.F.; Nortvedt, P.; Hevrøy, O. Family members’ experiences of “wait and see” as a communication strategy in end-of-life decisions. Intensive Care Med. 2011, 37, 1143–1150. [Google Scholar] [CrossRef] [PubMed]
- Lind, R. Sense of responsibility in ICU end-of-life decision-making: Relatives’ experiences. Nurs. Ethics 2019, 26, 270–279. [Google Scholar] [CrossRef] [PubMed]
- Mistraletti, G.; Gristina, G.; Mascarin, S.; Iacobone, E.; Giubbilo, I.; Bonfanti, S.; Fiocca, F.; Fullin, G.; Fuselli, E.; Bocci, M.G.; et al. How to communicate with families living in complete isolation. BMJ Supportive Palliat. Care 2020. [Google Scholar] [CrossRef]
- Stall, N.M.; Johnstone, J.; McGeer, A.J.; Dhuper, M.; Dunning, J.; Sinha, S.K. Finding the Right Balance: An Evidence-Informed Guidance Document to Support the Re-Opening of Canadian Nursing Homes to Family Caregivers and Visitors during the Coronavirus Disease 2019 Pandemic. J. Am. Med. Dir. Assoc. 2020, 21, 1365–1370. [Google Scholar] [CrossRef]
- Bethell, J.; Aelick, K.; Babineau, J.; Bretzlaff, M.; Edwards, C.; Gibson, J.L.; Hewitt Colborne, D.; Iaboni, A.; Lender, D.; Schon, D.; et al. Social Connection in Long-Term Care Homes: A Scoping Review of Published Research on the Mental Health Impacts and Potential Strategies During COVID-19. J. Am. Med. Dir. Assoc. 2021, 22, 228–237. [Google Scholar] [CrossRef] [PubMed]
- Kemp, C.L. #MoreThanAVisitor: Families as “Essential” Care Partners during COVID-19. Gerontologist 2021, 61, 145–151. [Google Scholar] [CrossRef] [PubMed]
- Bolcato, M.; Fassina, G.; Rodriguez, D.; Russo, M.; Aprile, A. The contribution of legal medicine in clinical risk management. BMC Health Serv. Res. 2019, 19, 85. [Google Scholar] [CrossRef]
- Albolino, S.; Bellandi, T.; Cappelletti, S.; Di Paolo, M.; Fineschi, V.; Frati, P.; Offidani, C.; Tanzini, M.; Tartaglia, R.; Turillazzi, E. New Rules on Patient’s Safety and Professional Liability for the Italian Health Service. Curr. Pharm. Biotechnol. 2019, 20, 615–624. [Google Scholar] [CrossRef]
- Bolcato, M.; Fassina, G.; Sanavio, M.; Aprile, A. Seventeen-year Medical Professional Liability Experience in a Level III University Hospital. Curr. Pharm. Biotechnol. 2020. [Google Scholar] [CrossRef] [PubMed]
- Kimball, A.; Hatfield, K.M.; Arons, M.; James, A.; Taylor, J.; Spicer, K.; Bardossy, A.C.; Oakley, L.P.; Tanwar, S.; Chisty, Z.; et al. Asymptomatic and Presymptomatic SARS-CoV-2 Infections in Residents of a Long-Term Care Skilled Nursing Facility-King County, Washington, March 2020. MMWR Morb. Mortal. Wkly. Rep. 2020, 69, 377–381. [Google Scholar] [CrossRef]
- Gatto, V.; Scopetti, M.; La Russa, R.; Santurro, A.; Cipolloni, L.; Viola, R.V.; Di Sanzo, M.; Frati, P.; Fineschi, V. Advanced loss eventuality assessment and technical estimates: An integrated approach for management of healthcare-associated infections. Curr. Pharm. Biotechnol. 2019, 20, 625–634. [Google Scholar] [CrossRef]
- Bolcato, M.; Russo, M.; Trentino, K.; Isbister, J.; Rodriguez, D.; Aprile, A. Patient blood management: The best approach to transfusion medicine risk management. Transfus. Apher. Sci. 2020, 59, 102779. [Google Scholar] [CrossRef]
- Giraldi, G.; Montesano, M.; Napoli, C.; Frati, P.; La Russa, R.; Santurro, A.; Scopetti, M.; Orsi, G.B. Healthcare associated infections due to multidrug-resistant organisms: A surveillance study on extra hospital stay and direct costs. Curr. Pharm. Biotechnol. 2019, 20, 643–652. [Google Scholar] [CrossRef]
- Giannouli, V.; Mistraletti, G.; Umbrello, M. ICU experience for patients’ relatives: Is information all that matters? Discussion on “A family information brochure and dedicated website to improve the ICU experience for patients’ relatives: An Italian multicenter before-and-after study”. Intensive Care Med. 2017, 43, 722–723. [Google Scholar] [CrossRef] [PubMed]
- Cox, C.E.; Jensen, H.I. The unmet need of information access for family members of ICU patients. Intensive Care Med. 2017, 43, 240–242. [Google Scholar] [CrossRef]
- McGaughey, J.; Harrison, S. Developing an information booklet to meet the needs of intensive care patients and relatives. Intensive Crit. Care Nurs. 1994, 10, 271–277. [Google Scholar] [CrossRef]
- Gallienne-Bouygues, S.; Soltner, C.; Lassalle, V.; Beydon, L. Information booklets to patients’ family and relatives. Survey of practice in a sample of 59 intensive care units, in France. Ann. Fr. Anesth Reanim. 2006, 25, 1105–1106. [Google Scholar] [CrossRef] [PubMed]
- Wammes, J.D.; Kolk, M.D.; van den Besselaar, J.H.; MacNeil-Vroomen, J.L.; Buurman-van, B.M.; van Rijn, M. Evaluating Perspectives of Relatives of Nursing Home Residents on the Nursing Home Visiting Restrictions During the COVID-19 Crisis: A Dutch Cross-Sectional Survey Study. J. Am. Med. Dir. Assoc. 2020, 21, 1746–1750. [Google Scholar] [CrossRef] [PubMed]
- Sizoo, E.M.; Monnier, A.A.; Bloemen, M.; Hertogh, C.M.P.M.; Smalbrugge, M. Dilemmas With Restrictive Visiting Policies in Dutch Nursing Homes During the COVID-19 Pandemic: A Qualitative Analysis of an Open-Ended Questionnaire With Elderly Care Physicians. J. Am. Med. Dir. Assoc. 2020, 21, 1774–1781. [Google Scholar] [CrossRef]
- Chaet, D.; Clearfield, R.; Sabin, J.E.; Skimming, K.; Council on Ethical and Judicial Affairs American Medical Association. Ethical practice in Telehealth and Telemedicine. J. Gen. Intern. Med. 2017, 32, 1136–1140. [Google Scholar] [CrossRef] [PubMed]
- Ferorelli, D.; Nardelli, L.; Spagnolo, L.; Corradi, S.; Silvestre, M.; Misceo, F.; Marrone, M.; Zotti, F.; Mandarelli, G.; Solarino, B.; et al. Medical Legal Aspects of Telemedicine in Italy: Application Fields, Professional Liability and Focus on Care Services During the COVID-19 Health Emergency. J. Prim. Care Community Health 2020, 11, 2150132720985055. [Google Scholar] [CrossRef]
|
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Bolcato, M.; Trabucco Aurilio, M.; Di Mizio, G.; Piccioni, A.; Feola, A.; Bonsignore, A.; Tettamanti, C.; Ciliberti, R.; Rodriguez, D.; Aprile, A. The Difficult Balance between Ensuring the Right of Nursing Home Residents to Communication and Their Safety. Int. J. Environ. Res. Public Health 2021, 18, 2484. https://doi.org/10.3390/ijerph18052484
Bolcato M, Trabucco Aurilio M, Di Mizio G, Piccioni A, Feola A, Bonsignore A, Tettamanti C, Ciliberti R, Rodriguez D, Aprile A. The Difficult Balance between Ensuring the Right of Nursing Home Residents to Communication and Their Safety. International Journal of Environmental Research and Public Health. 2021; 18(5):2484. https://doi.org/10.3390/ijerph18052484
Chicago/Turabian StyleBolcato, Matteo, Marco Trabucco Aurilio, Giulio Di Mizio, Andrea Piccioni, Alessandro Feola, Alessandro Bonsignore, Camilla Tettamanti, Rosagemma Ciliberti, Daniele Rodriguez, and Anna Aprile. 2021. "The Difficult Balance between Ensuring the Right of Nursing Home Residents to Communication and Their Safety" International Journal of Environmental Research and Public Health 18, no. 5: 2484. https://doi.org/10.3390/ijerph18052484
APA StyleBolcato, M., Trabucco Aurilio, M., Di Mizio, G., Piccioni, A., Feola, A., Bonsignore, A., Tettamanti, C., Ciliberti, R., Rodriguez, D., & Aprile, A. (2021). The Difficult Balance between Ensuring the Right of Nursing Home Residents to Communication and Their Safety. International Journal of Environmental Research and Public Health, 18(5), 2484. https://doi.org/10.3390/ijerph18052484












