Supporting the Sharing of Mental Health Challenges in the Workplace: Findings from Comparative Case Study Research at Two Mental Health Services
Abstract
:1. Introduction
2. Materials and Methods
- MH professionals identifying with LE, publicly or privately (MHPLE);
- MH professionals not identifying with LE (MHP);
- staff in designated LE roles (Peer Workers);
- staff in supervisory roles (Supervisors) from the above groups.
3. Results
3.1. Participant Characteristics
3.2. Contextual Factors Supporting Revelation of Mental Health (MH) Challenges
3.2.1. Perceived Organizational Support
“I was looking at peer work roles and, in the end, decided against it because I wasn’t really comfortable with the level of disclosure that is implicit in the peer role. I was really reluctant to have that on my resume.”(Finley, MHPLE, Organization B)
3.2.2. Perceived Supervisor Support
“My supervisor […] creates a safe space for me to be able to explore those issues […] so that, […] I’m able to […] develop my relationship with LE and sharing in a way that supports the work and our consumers, as well.”(Yarden, MHPLE, Organization B)
3.2.3. Individual Differences
“By being myself fully, I felt it might allow space for other people to feel they can be themselves fully, […] feeling permission to be themselves and to be their authentic selves…. can create… contribute to the change that is maybe needed.”(Tanveer, MHPLE, Organization B)
“The older you get, and the more senior you get in your position, the more people value what you say […]. When you […] do disclose something, that it carries a lot of weight. And so, it’s important to be very careful about how you do that and judicious.”(Quinn, MHPLE, Organization A)
3.3. Identity Management Behaviours in the Workplace
“I think, it is good to share so they can see someone that’s going to work and seeming, relatively, fine… and, having that diagnosis. It’s part of breaking down the stigma.”(Neeru, Peer worker, Organization A)
3.4. Sharing Lived Experience
3.5. Team Culture and Type of Sharing
“We are a multi-disciplinary team but there’s no hierarchy at all. It’s a very flat structure. [...] there’s no person or professional on the team is more or less than anyone else. [...] and I’ve only received encouragement to […] discuss issues, and consumers, and struggles with the team.”(Halcyon, Peer worker, Organization B)
“Most people are okay with looking at… at naming their strengths and weaknesses and working together around that… which is quite challenging, really. […] It’s hard but we’re getting really good at it. It’s a great environment now, and necessary for the work. Like, we’ve got a great healthy team… really supportive team.”(Blake, Peer worker, Organization B)
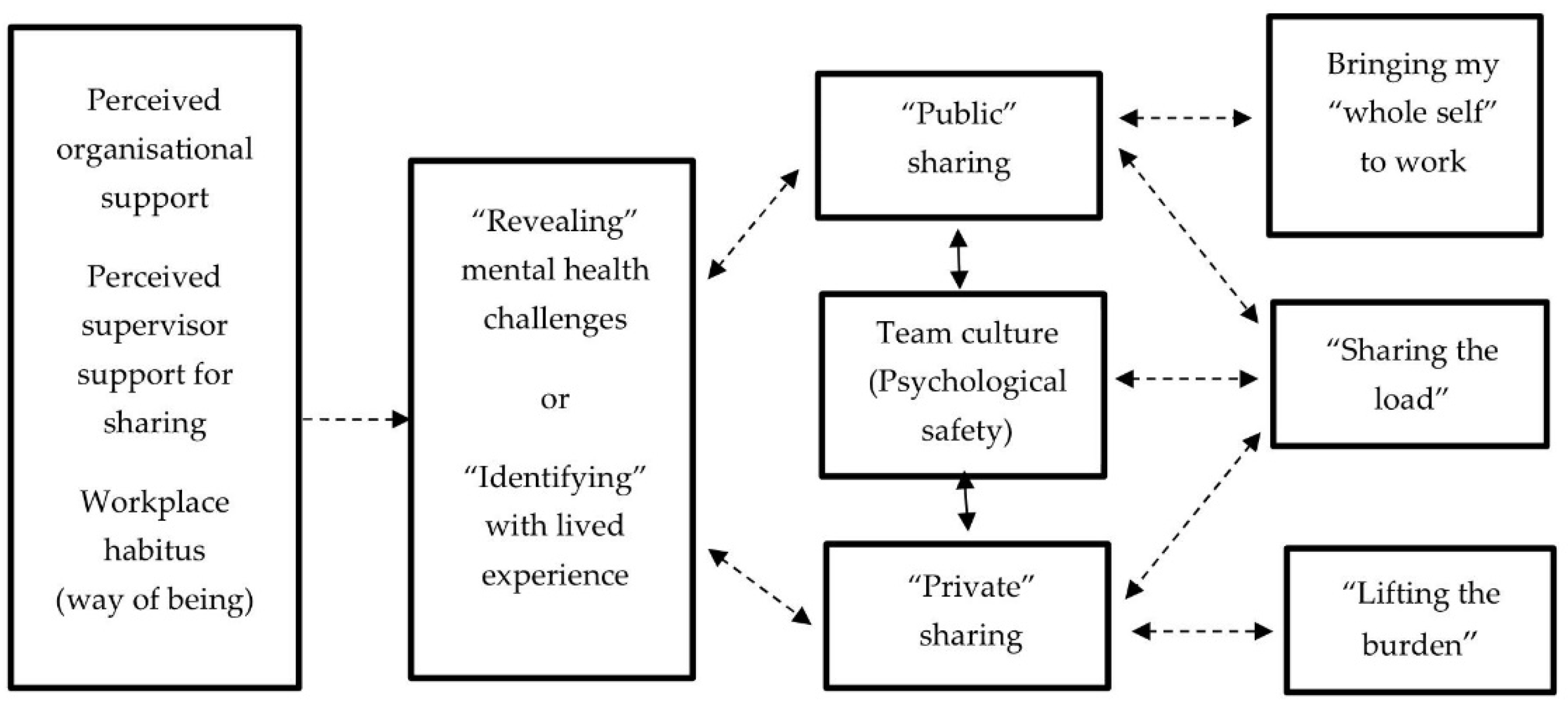
3.6. Consequences of Revealing and Sharing Lived Experience (LE)
3.6.1. Lifting the Burden
3.6.2. Sharing the Load
“So, the ones that you care about, and they care about you, you actually would go out of your way to help them […]. If you’re closer to someone they naturally volunteer to help you more and you feel more supported. If you don’t have that, it’s just stressful.”(Melissa, MHPLE, Organization A)
3.6.3. Bringing My Whole Self to Work
“I guess, what’s developed from that is a feeling of real satisfaction within my role because I feel like I can bring all of myself to this work. It’s not like I have to put on a professional façade and feel like I have a whole lot of experience that might be informing the way I do my work but that I need to keep a secret.”(Yarden, MHPLE, Organization B)
3.6.4. Once Bitten, Twice Shy
4. Discussion
- planned and unplanned, individual and team “check-ins”;
- mutual sharing and support by colleagues and supervisors;
- opportunities for individual and team reflection.
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Quinn, D.M.; Weisz, B.M.; Lawner, E.K. Impact of active concealment of stigmatized identities on physical and psychological quality of life. Soc. Sci. Med. 2017, 192, 14–17. [Google Scholar] [CrossRef]
- Camacho, G.; Reinka, M.A.; Quinn, D.M. Disclosure and concealment of stigmatized identities. Curr. Opin. Psychol. 2020, 31, 28–32. [Google Scholar] [CrossRef]
- Jones, K.P.; King, E.B. Managing Concealable Stigmas at Work: A Review and Multilevel Model. J. Manag. 2014, 40, 1466–1494. [Google Scholar] [CrossRef]
- Jones, A.M. Disclosure of Mental Illness in the Workplace: A Literature Review. Am. J. Psychiatr. Rehabil. 2011, 14, 212–229. [Google Scholar] [CrossRef]
- Brouwers, E.P.M.; Joosen, M.C.W.; Van Zelst, C.; Van Weeghel, J. To Disclose or Not to Disclose: A Multi-stakeholder Focus Group Study on Mental Health Issues in the Work Environment. J. Occup. Rehabil. 2020, 30, 84–92. [Google Scholar] [CrossRef] [Green Version]
- Brohan, E.; Henderson, C.; Wheat, K.; Malcolm, E.; Clement, S.; Barley, E.A.; Slade, M.; Thornicroft, G. Systematic review of beliefs, behaviours and influencing factors associated with disclosure of a mental health problem in the workplace. BMC Psychiatry 2012, 12, 11. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hastuti, R.; Timming, A.R. An inter-disciplinary review of the literature on mental illness disclosure in the workplace: Implications for human resource management. Int. J. Hum. Resour. Manag. 2021, 32, 3302–3338. [Google Scholar] [CrossRef]
- Edmondson, A.C. The Fearless Organization: Creating Psychological Safety in the Workplace for Learning, Innovation, and Growth; Wiley: Hoboken, NJ, USA, 2018. [Google Scholar]
- Harris, J.I.; Leskela, J.; Hoffman-Konn, L. Provider lived experience and stigma. Am. J. Orthopsychiatry 2016, 86, 604–609. [Google Scholar] [CrossRef] [PubMed]
- Henderson, C.; Noblett, J.; Parke, H.; Clement, S.; Caffrey, A.; Gale-Grant, O.; Schulze, B.; Druss, B.; Thornicroft, G. Mental health-related stigma in health care and mental health-care settings. Lancet Psychiatry 2014, 1, 467–482. [Google Scholar] [CrossRef]
- Carrara, B.S.; Ventura, C.A.A.; Bobbili, S.J.; Jacobina, O.M.P.; Khenti, A.; Mendes, I.A.C. Stigma in health professionals towards people with mental illness: An integrative review. Arch. Psychiatr. Nurs. 2019, 33, 311–318. [Google Scholar] [CrossRef]
- Hansson, L.; Jormfeldt, H.; Svedberg, P.; Svensson, B. Mental health professionals & rsquo; attitudes towards people with mental illness: Do they differ from attitudes held by people with mental illness? Int. J. Soc. Psychiatry 2013, 59, 48–54. [Google Scholar] [PubMed]
- King, A.J.; Brophy, L.; Fortune, T.L.; Byrne, L. Factors Affecting Mental Health Professionals’ Sharing of Their Lived Experience in the Workplace: A Scoping Review. Psychiatr. Serv. 2020, 71, 1047–1064. [Google Scholar] [CrossRef]
- Hudson, E.; Arnaert, A.; Lavoie-Tremblay, M. Healthcare professional disclosure of mental illness in the workplace: A rapid scoping review. J. Ment. Health 2021, 1–13. [Google Scholar] [CrossRef]
- Nairz-Wirth, E.; Feldmann, K. Professional Habitus and Fields. In Pierre Bourdieu in Studies of Organization and Management: Societal Change and Transforming Fields; Robinson, S., Ernst, J., Larsen, K., Thomassen, O.J., Eds.; Taylor & Francis Group: Abingdon, UK, 2021; pp. 157–175. [Google Scholar]
- Morgan, P.J.; Lawson, J. Developing guidelines for sharing lived experience of staff in health and social care. Ment. Health Soc. Incl. 2015, 19, 78–86. [Google Scholar] [CrossRef]
- Yin, R.K. Case Study Research: Design and Methods, 5th ed.; SAGE Publications: Thousand Oaks, CA, USA, 2014. [Google Scholar]
- Thomas, G.; Myers, K. The Anatomy of the Case Study; SAGE Publications: London, UK, 2015. [Google Scholar]
- Miles, M.B.; Huberman, A.M.; Saldaña, J. Qualitative Data Analysis: A Methods Sourcebook, 4th ed.; SAGE Publications: Thousand Oaks, CA, USA, 2020. [Google Scholar]
- Etherington, K.; Bridges, N. Narrative case study research: On endings and six session reviews. Couns. Psychother. Res. 2011, 11, 11–22. [Google Scholar] [CrossRef]
- Bazeley, P. Qualitative Data Analysis: Practical Strategies; Sage: London, UK, 2013. [Google Scholar]
- Saldaña, J. The Coding Manual for Qualitative Researchers, 3rd ed.; SAGE: London, UK, 2016. [Google Scholar]
- Timmermans, S.; Tavory, I. Theory Construction in Qualitative Research: From Grounded Theory to Abductive Analysis. Sociol. Theory 2012, 30, 167–186. [Google Scholar] [CrossRef]
- Etherington, K. Ethical research in reflexive relationships. Qual. Inq. 2007, 13, 599–616. [Google Scholar] [CrossRef]
- Bourdieu, P. The Weight of the World; Polity Press: London, UK, 1999. [Google Scholar]
- Byrne, L.; Roennfeldt, H.; Davidson, L.; Miller, R.; Bellamy, C. To disclose or not to disclose? Peer workers impact on a culture of safe disclosure for mental health professionals with lived experience. Psychol. Serv. 2021, 1–10. [Google Scholar] [CrossRef]
- Bearse, J.L.; McMinn, M.R.; Seegobin, W.; Free, K. Barriers to Psychologists Seeking Mental Health Care. Prof. Psychol. Res. Pract. 2013, 44, 150–157. [Google Scholar] [CrossRef] [Green Version]
- Edwards, J.L.; Crisp, D.A. Seeking help for psychological distress: Barriers for mental health professionals. Aust. J. Psychol. 2017, 69, 218–225. [Google Scholar] [CrossRef]
- Hassan, T.M.; Tran, T.; Mazhar, M.N.; Doan, N.; Munshi, T.; Bajaj, N.; Groll, D.; Galbraith, N. Attitudes of Canadian psychiatry residents if mentally ill: Awareness, barriers to disclosure, and help-seeking preferences. Can. Med. Educ. J. 2016, 7, e14–e24. [Google Scholar] [CrossRef] [PubMed]
- Tay, S.; Alcock, K.; Scior, K. Mental health problems among clinical psychologists: Stigma and its impact on disclosure and help-seeking. J. Clin. Psychol. 2018, 74, 1545–1555. [Google Scholar] [CrossRef] [PubMed]
- When Mental Health Professionals Reveal Their Mental Illnesses at Work. 2017. Available online: http://tucollaborative.org/wp-content/uploads/Full-Disclosure-When-Mental-Health-Professionals-Reveal-Their-Mental-Illness-at-Work.pdf (accessed on 31 October 2019).
- Creating Welcoming Work Environments: Recommendations for Fully Embracing a Supporting Clinical Staff with Mental Illnesses. 2016. Available online: http://tucollaborative.org/wp-content/uploads/2017/03/Creating-Welcoming-Mental-Health-Work-Environments.pdf (accessed on 31 October 2019).
- Harris, J.I.; Leskela, J.; Lakhan, S.; Usset, T.; Devries, M.; Mittal, D.; Boyd, J. Developing Organizational Interventions to Address Stigma Among Mental Health Providers: A Pilot Study. Community Ment. Health J. 2019, 55, 924–931. [Google Scholar] [CrossRef] [PubMed]
| MHPLE | MHP | Peer Workers | Supervisors 1 | |
|---|---|---|---|---|
| Organization A | 10 | 1 | 4 | 8 |
| Organization B | 11 | 4 | 3 | 6 |
| Discipline | No. of Participants |
|---|---|
| Social Work | 10 |
| Non-clinical, MH related 1 | 9 |
| Nursing | 5 |
| Psychology | 5 |
| Other clinical 2 | 5 |
| Peer Support | 5 |
| Occupational Therapy | 2 |
| Psychiatry | 2 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
King, A.J.; Fortune, T.L.; Byrne, L.; Brophy, L.M. Supporting the Sharing of Mental Health Challenges in the Workplace: Findings from Comparative Case Study Research at Two Mental Health Services. Int. J. Environ. Res. Public Health 2021, 18, 12831. https://doi.org/10.3390/ijerph182312831
King AJ, Fortune TL, Byrne L, Brophy LM. Supporting the Sharing of Mental Health Challenges in the Workplace: Findings from Comparative Case Study Research at Two Mental Health Services. International Journal of Environmental Research and Public Health. 2021; 18(23):12831. https://doi.org/10.3390/ijerph182312831
Chicago/Turabian StyleKing, Alicia Jean, Tracy Lee Fortune, Louise Byrne, and Lisa Mary Brophy. 2021. "Supporting the Sharing of Mental Health Challenges in the Workplace: Findings from Comparative Case Study Research at Two Mental Health Services" International Journal of Environmental Research and Public Health 18, no. 23: 12831. https://doi.org/10.3390/ijerph182312831
APA StyleKing, A. J., Fortune, T. L., Byrne, L., & Brophy, L. M. (2021). Supporting the Sharing of Mental Health Challenges in the Workplace: Findings from Comparative Case Study Research at Two Mental Health Services. International Journal of Environmental Research and Public Health, 18(23), 12831. https://doi.org/10.3390/ijerph182312831







