Data-Powered Positive Deviance during the SARS-CoV-2 Pandemic—An Ecological Pilot Study of German Districts
Abstract
:Key Summary Points
- We used the mixed-methods framework DPPD (a novel approach, using quantitative and qualitative methodologies) to examine successful districts in controlling the SARS-CoV-2 transmission in Germany.
- We identified the positively deviant districts regarding their ability to reduce the R0.
- These districts were from two separate timeframes, the lockdown period in Spring 2020 and the 2020 summer vacation, and we conducted interviews with political representatives of some of these districts to find successful strategies for pandemic response.
- The essential components for controlling the R0 were: fast-paced response, preparedness, situational analyses, containment, social network effects, communication and community compliance.
- This method has potentials for low- and middle-income countries, thanks to its usage of freely available datasets.
1. Introduction
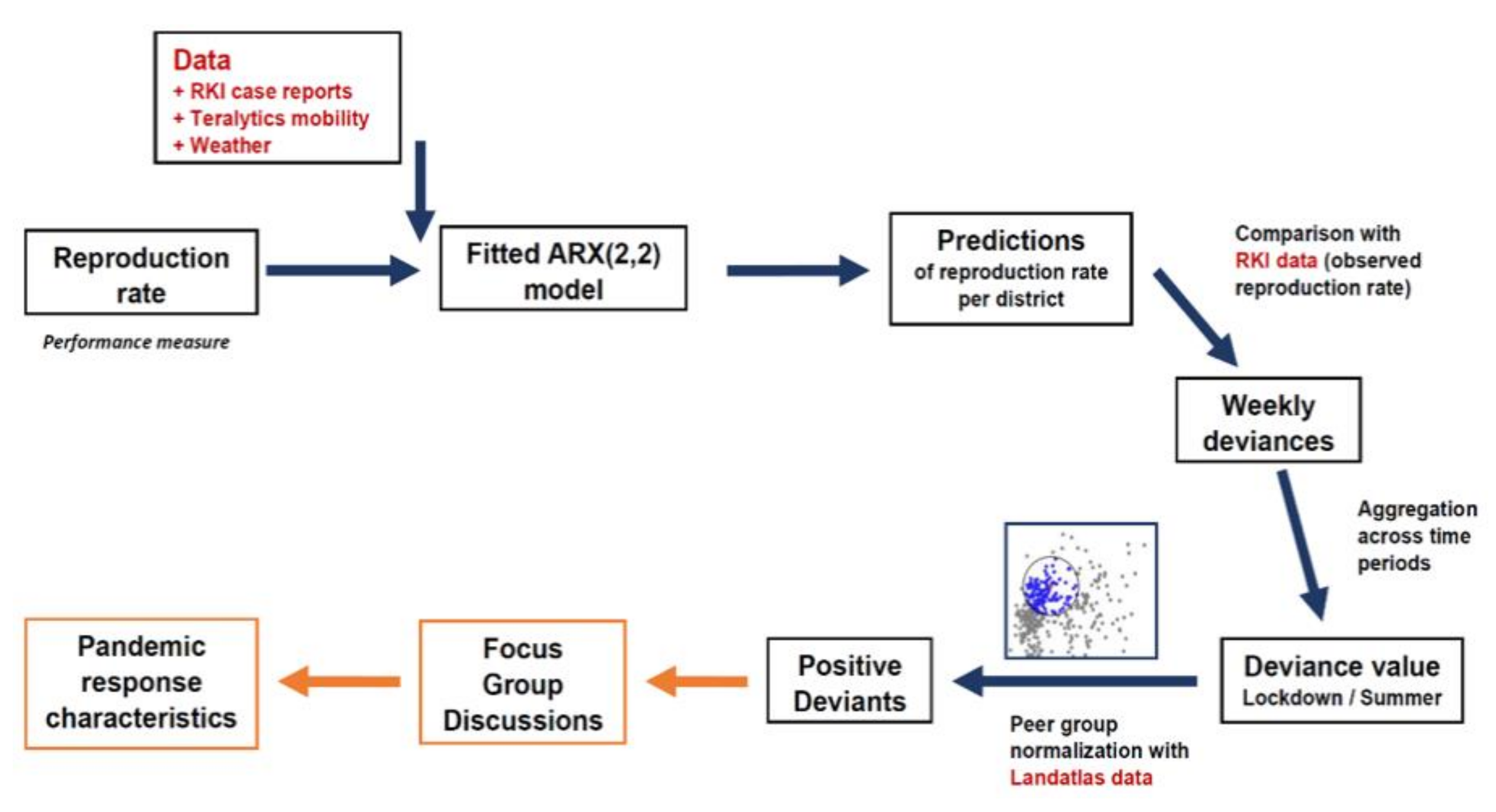
Data-Powered Positive Deviance
2. Materials and Method
2.1. Study Setting and Design
2.2. Data Sources, Measurements, and Variables
2.2.1. First Data Source: Robert Koch Institute (RKI)
2.2.2. Second Data Source: Teralytics
2.2.3. Third Data Source: German Weather Service (DWD)
2.2.4. Fourth Data Source: Landatlas
2.3. Statistical Analysis
2.3.1. Performance Model
2.3.2. Estimating Model Parameters
2.3.3. Calculation of Weekly Deviances
2.3.4. Aggregation of Weekly Deviances
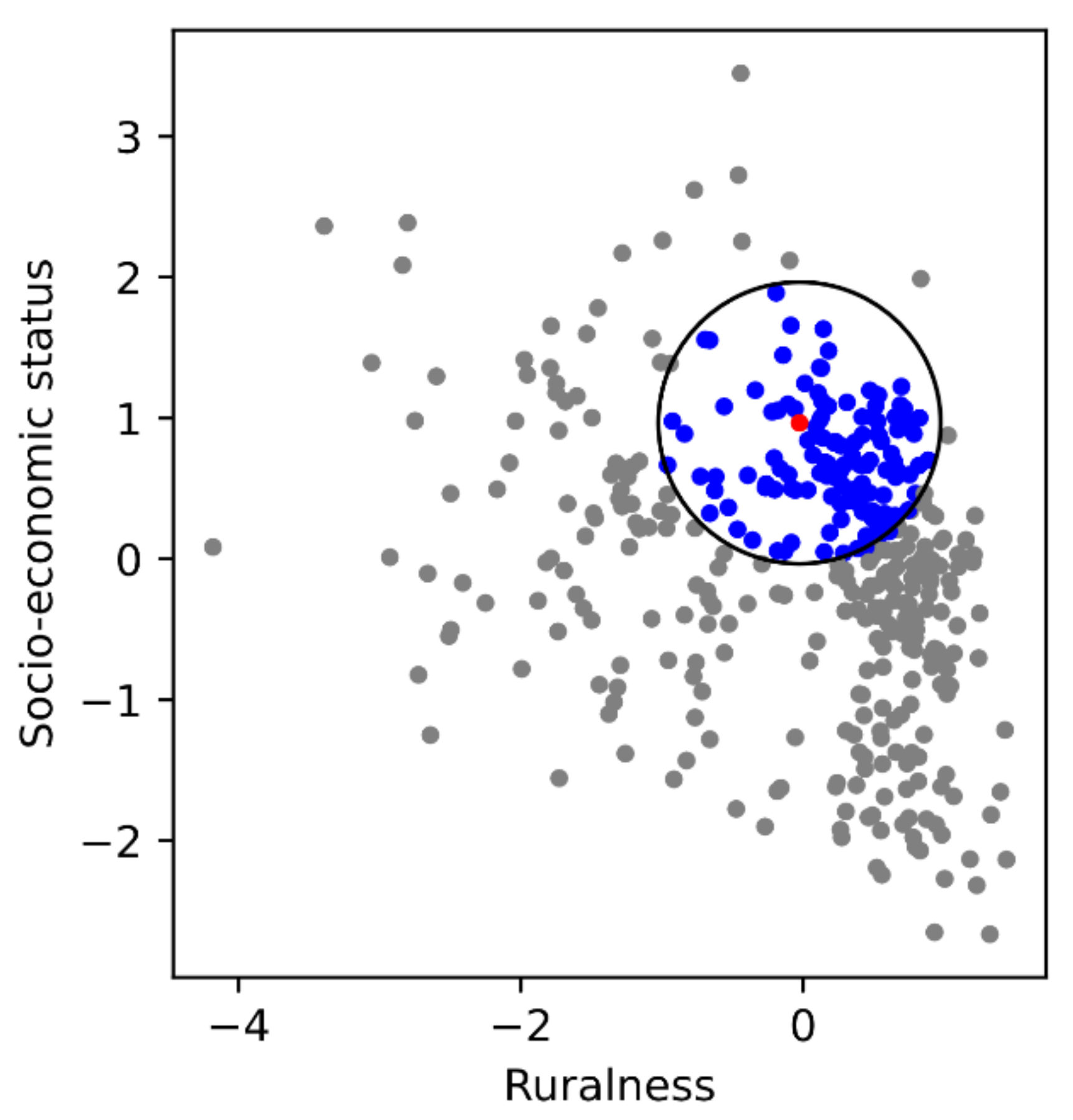
2.3.5. Peer Group Normalization
2.3.6. Ranking of Districts
2.4. Focus Group Discussions with PD Candidates
3. Results
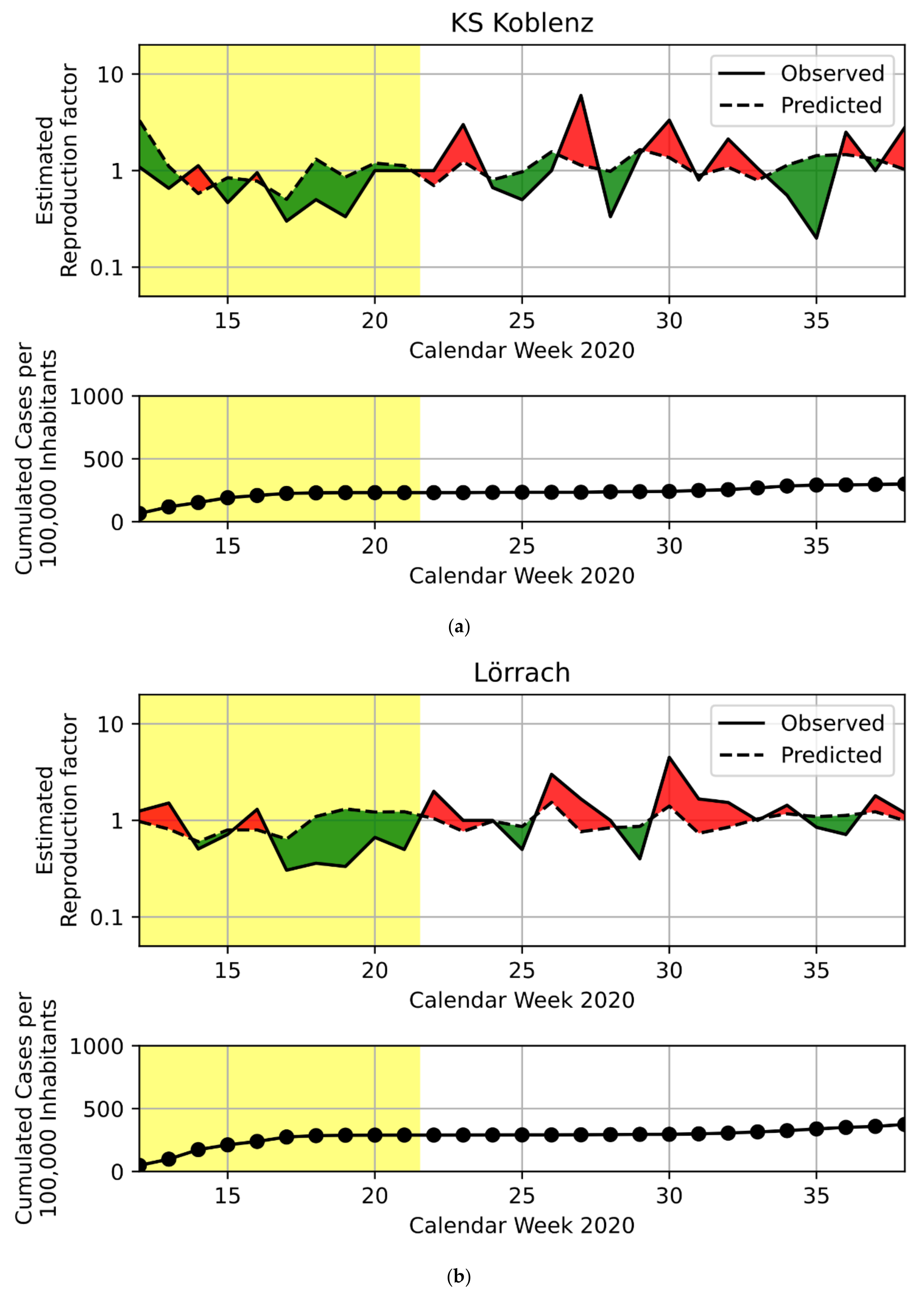
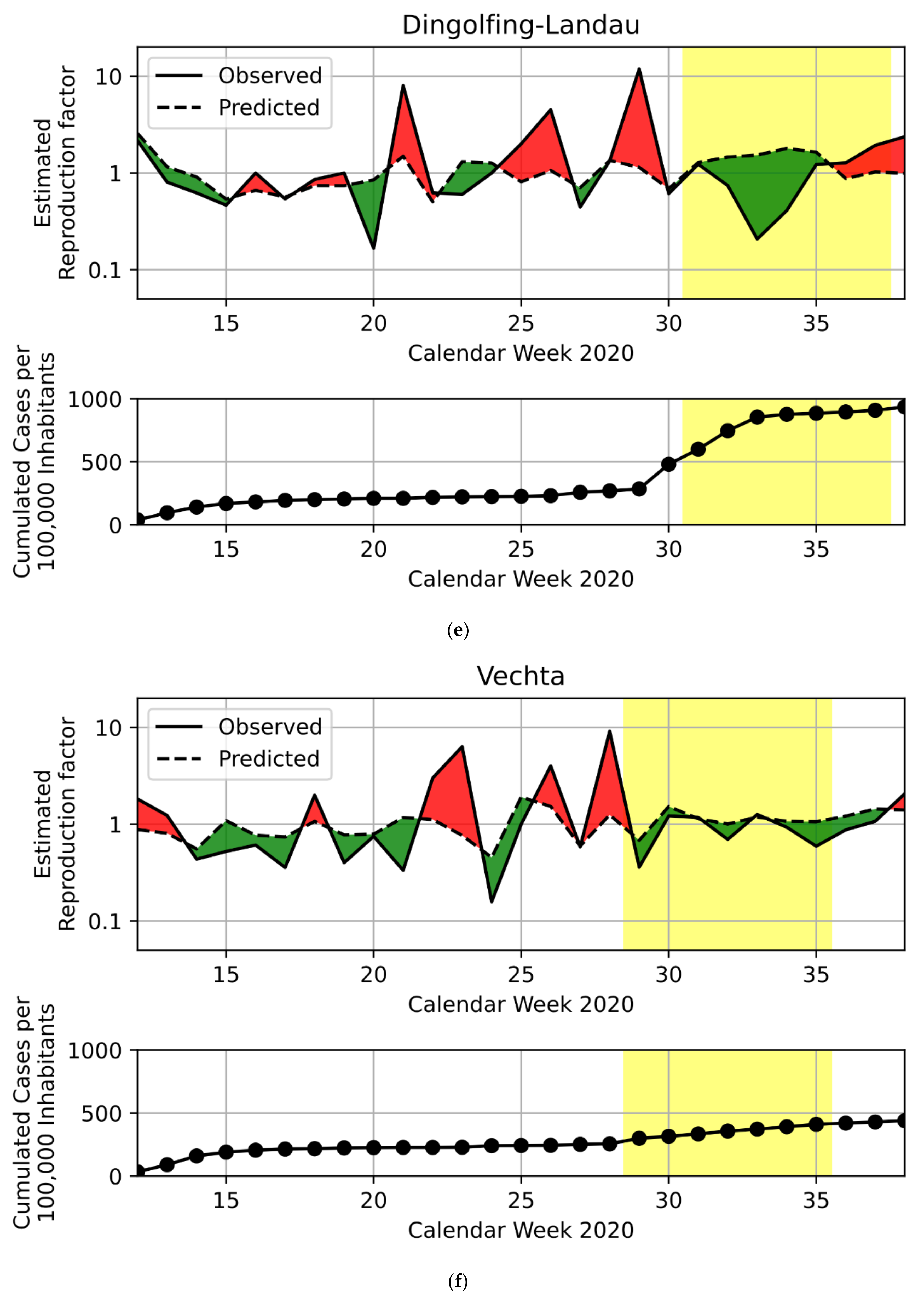
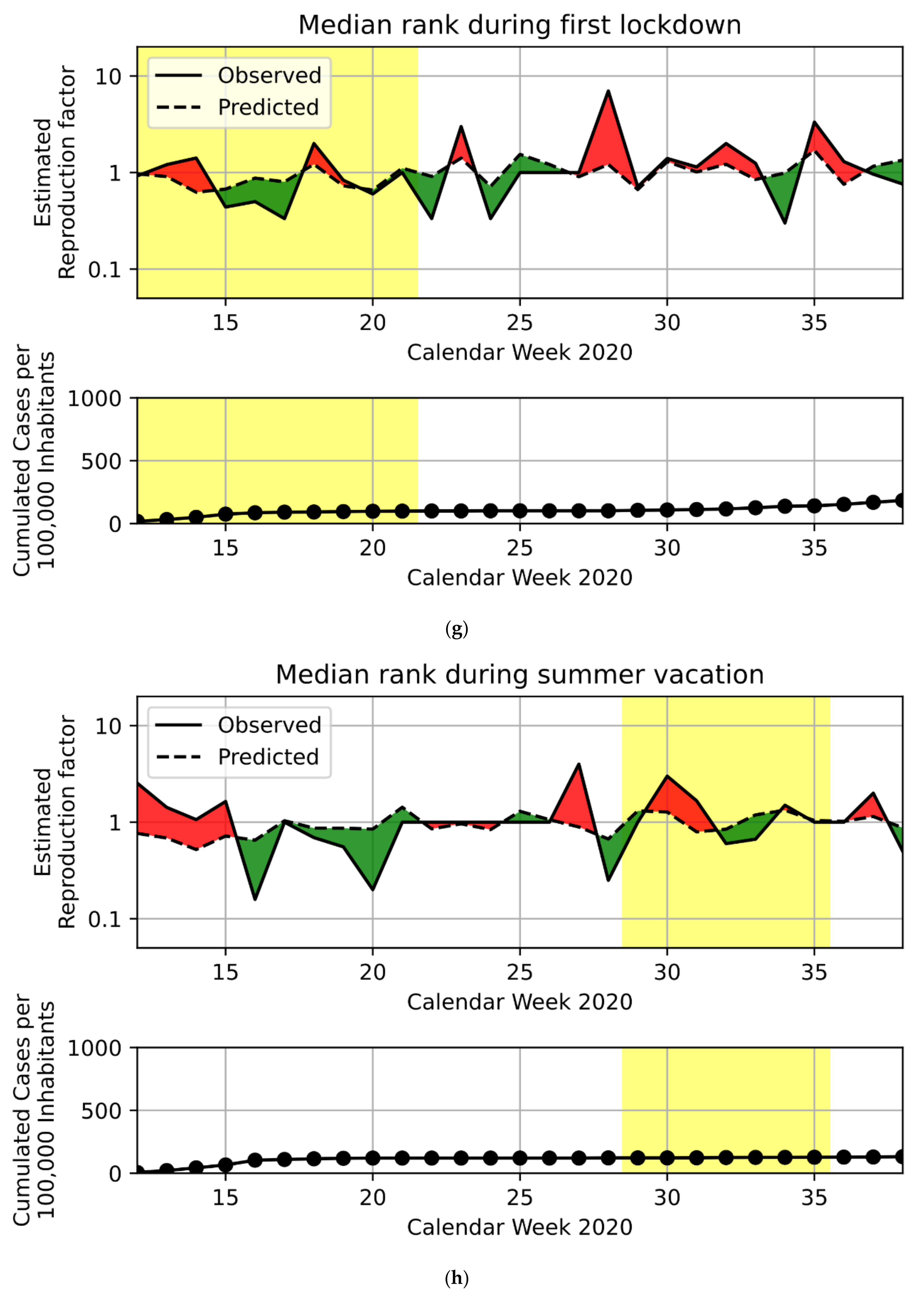
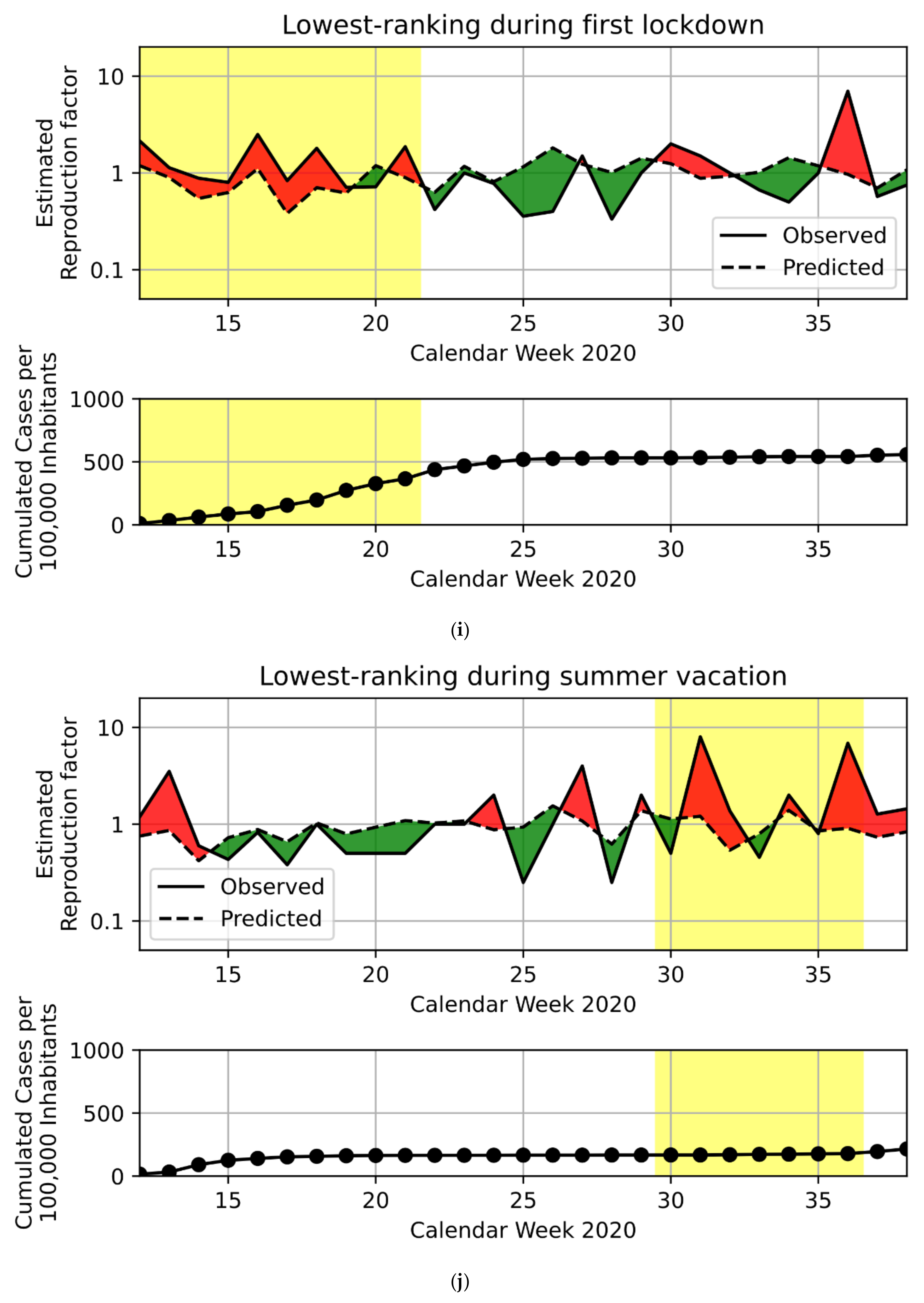
3.1. Regression Model
3.2. PD Candidates
3.3. Focus Group Discussion
3.3.1. Theme 1: Characteristics of Local Administrations’ Fast-Paced SARS-CoV-2 Emergency Response
Action Bias
“But that is precisely the point, acting flexibly and pragmatically, looking ahead and staying ahead of the situation, as you say in crisis response circles. I believe this to be a very important thing. Instead of doing the usual bureaucratic waiting and seeing what happens and what we guidelines we get.”
“I believe it is important to always think proactively, and not first wait until you get some guidelines from [federal or provincial institutions], but instead react to the local situation on a daily basis.”
“The [citizen] doesn’t ask, whose responsibility is this, he asks how he can be helped.”
“[Some task] was basically not the health department’s job, but we just did it, because we saw that it needed to be done.”
Agility in Public Administration
“If you had asked me two years ago whether I can imagine a health department as an agile organisation, I would have said ‘What? No way’. And now, after this year, yes, I have never seen a more agile organisation than a health department.”
“Then naturally, you need people who are highly committed, who stay with it and no one says ‘It’s the weekend now’.”
Fill Regulatory Gaps/Courage to Deviate
“Wherever possible we wanted to act ourselves and shape the response, and simply act. Of course, we got quite a lot of, let’s say, scepticism or first astonishment. But in the end, they [the decision makers higher up in the hierarchy], noticed that we always fared well with our strategy, and actually were always acting proactively, which turned essentially always turned out well.”
“We were always [operating] on a daily basis, as soon as we noticed that the Robert Koch Institute changed its guidelines, we immediately implemented them, and everything for which there was no guideline, we just amended it reasonably.”
“There was no [pandemic response] blueprint in Germany. We had to develop it ourselves in the shortest possible time. We developed it using our experience with normal containment plus the special [characteristics of] the situation.”
Cross-Organizational Collaboration
“It is absolutely imperative that ‘silos’ that normally operate entirely side by side, in this kind of situation work hand in hand, and coordinate with each other very closely.”
“[…] and having, as is the purpose of a crisis management group, relatively short communication lines. Thus, the reported situation as we appraised it was known to everyone.”
3.3.2. Theme 2: Preparedness
Risk Consciousness and Early Initiation of Measures
“We saw what happened in China. We saw what happened in Italy, and it was absolutely clear: This will come to us—and when it happened, we acted very quickly and resolutely implemented measures which we deemed reasonable under medical aspects for containing a pandemic.”
“We have to generate a road map and we have to be ready to go, when the first case happens in our district, we have to have created administrative structures.”
Emergency Infrastructure and Procurement
“In total, we built three facilities […] with almost 340 beds. Also, nurses would have been available, and we would have ensured 24-h operation. We were prepared.”
3.3.3. Theme 3. Situational Analysis and Reporting
Data Flow
“We from the emergency services contacted [local policy makers] and said: We now need a team for continuous situation monitoring, i.e., we used the emergency services for this; all reports coming in from the city need to go into one central department, and the politically responsible need to examine them and generate a [response].”
Analyses and Projections
“We have a daily data analysis. In this data analysis, in a very detailed form, we started very early, but extended it further in the context of the outbreak, in order to assess very precisely whether we have infections into sensitive areas like schools, day cares, and care facilities.”
Information Technology (IT) System in Health Departments
“A special software was introduced, which is still in use today, to handle and track the cases. However, we were also able to assign big IT-based teams with special software, where we could monitor everything, and also send out our directives.”
3.3.4. Theme 4. Containment
Strive to Remain in Control
“Therefore, we acted quickly and created the fever walk-in clinic […] to stay ahead of the situation and keep the infections as low as possible, identify early on who is infected, identify contacts and isolate accordingly.”
“We always had the aspiration to keep the situation under control, and I believe we also had the situation under control during times when we had a higher infection occurrence, and we were working every day of the week.”
Shut Down and Isolate Early and Comprehensively
“We started very early on to shut down public life through [a far-reaching policy instrument].”
“We were always very courageous in our decision. We did not isolate individual [school] classes, but also said: the institution gets shut down. No one had a whole lot of experience, but we acted aggressively—always stay ahead of the situation.”
Large Scale Testing
“This was always our strategy: testing, testing—targeted of course, but also a lot.”
3.3.5. Theme 5. Communication
Reliable and Trustworthy Public Communication
“Every crisis needs a face. […] Daily video messages, two to three minutes: What is happening here? Why are we doing this? Why are we ahead of the situation? What are the rules?”
“But many neglected the media situation, that needed to be handled comprehensively. Early on this took almost as much time as the medical situation.”
Consistent Health Messages Dissemination across All Channels
“[It is important] to speak with one voice. We often noticed that, whenever there were small differences in wording between [different communication channels], people were very preoccupied with this, so we learned to coordinate our publications very well.”
3.3.6. Theme 6. Utilization of Social Capital
Personal Networks of Decision Makers
“And again, one thing was helpful, […] having a [senior health dept. official] who knows the district and knows everyone here. Compared to a someone where this is not so, this is an important factor, I think.”
Role of Social Cohesion
“We have about 23,000 members of carnival associations. We then started an appeal, since one knows one another, one is in exchange with one another. Many associations sewed face masks, which in part came to us, and in part were distributed within those associations.”
“On one hand, we’re a district with international players […]. On the other hand, we have connections like in a small village—one does know one another. And this is totally helpful for contact tracing, even though they are actually global players. […] One knows one another and can utilize personal, informal channels.”
3.3.7. Theme 7. Community Compliance
Early Preparedness Measures Reinforce Risk Consciousness among the Population
“We noticed that we didn‘t need a lot of [built emergency infrastructure], like overflow hospitals. But it was covered in the media, which of course created some sensibility in the population.”
Proximity of a Major Outbreak Increases Compliance
“I think there was generally high sensibility in the population here. That must be said very clearly. We think that the [distancing, hygiene and mask] rules had a higher significance due to [the local, publicised outbreak], compared to regions where it was a lot easy-going after the first wave.”
4. Discussion
4.1. Pandemic Response Characteristics of the PD Candidates
4.2. Methodological Strengths and Weaknesses
4.3. Application of Our Approach in the Global South
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
Appendix B
| Predictor Variable | Standardized β-Weights |
|---|---|
| Log-R0 t-1 | −0.293 |
| Log-R0 t-2 | −0.081 |
| Internal travel per capita week t | −0.337 |
| Internal travel per capita week t-1 | 0.35 |
| Incoming travel per capita week t | −0.668 |
| Incoming travel per capita week t-1 | 0.694 |
| Incoming infection load per capita week t | 0.247 |
| Incoming infection load per capita week t-1 | −0.267 |
| Average temperature week t | 0.08 |
| Average temperature week t-1 | 0.067 |
| Average humidity week t | 0.018 |
| Average humidity week t-1 | 0.016 |
| Average precipitation week t | −0.012 |
| Average precipitation week t-1 | 0.043 |
| Average daily sunshine week t | 0.036 |
| Average daily sunshine week t-1 | −0.106 |
References
- World Health Organization (WHO). Coronavirus Disease (COVID-19): Vaccines; World Health Organization: Geneva, Switzerland, 2020; Available online: https://www.who.int/news-room/q-a-detail/coronavirus-disease-(covid-19)-vaccines?topicsurvey=v8kj13)&gclid=CjwKCAjwhOyJBhA4EiwAEcJdcQrTM687xOYEe9jqrUZ2RaXdlbhLg_Q3PpHuOGlngdxk3rIs1ee_UBoCJa8QAvD_BwE (accessed on 1 August 2021).
- Kucharski, A.J.; Russell, T.W.; Diamond, C.; Liu, Y.; Edmunds, J.; Funk, S.; Eggo, R.M. Early dynamics of transmission and control of COVID-19: A mathematical modelling study. Lancet Infect. Dis. 2020, 20, 553–558, on behalf of the Centre for Mathematical Modelling of Infectious Diseases COVID-19 working Group. [Google Scholar] [CrossRef] [Green Version]
- Riou, J.; Althaus, C. Pattern of early human-to-human transmission of Wuhan 2019 novel coronavirus (2019-nCoV), December 2019 to January 2020. Eurosurveillance 2020, 25, 2000058. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Morgenstern, C.; Kelly, J.; Lowe, R.; Jit, M.; CMMID COVID-19 Working Group. The impact of non-pharmaceutical interventions on SARS-CoV-2 transmission across 130 countries and territories. BMC Med. 2021, 19, 40. [Google Scholar] [CrossRef] [PubMed]
- United Nations. Low-Income Countries Have Received Just 0.2 Per Cent of All COVID-19 Shots Given. 2021. Available online: https://news.un.org/en/story/2021/04/1089392 (accessed on 1 May 2021).
- Xio, Y.; Torok, M.E. Taking the right measures to control COVID-19. Lancet 2020, 20, 523–524. [Google Scholar] [CrossRef] [Green Version]
- The German Agency for International Cooperation (GIZ). DPPD COVID-19. 2021. Available online: https://github.com/gizdatalab/DPPD_Covid (accessed on 3 July 2021).
- Albanna, B.; Heeks, R. Positive deviance, big data, and development: A systematic literature review. Electron. J. Inf. Syst. Dev. Ctries. 2019, 85, e12063. [Google Scholar] [CrossRef] [Green Version]
- Sternin, J. Positive deviance: A new paradigm for addressing today’s problems today. J. Corp. Citizsh. 2002, 5, 57–63. [Google Scholar]
- Pulse Lab Jakarta. Identifying Potential Positive Deviants (PDs) Across Rice Producing Areas in Indonesia: An Application of Big Data Analytics and Approaches. 2020. Available online: https://medium.com/@dppd/identifying-potential-positive-deviants-pds-across-rice-producing-areas-in-indonesia-an-27a113b3f410 (accessed on 13 June 2021).
- Data Powered Positive Deviance DPPD. Positividade* and Data against COVID-19: Description of a Python-Based Model Prototype Initiated during the #WirVsVirus Hackathon. 2020. Available online: https://medium.com/@dppd/positividade-and-data-against-covid-19-111f4d25bde2 (accessed on 13 June 2021).
- Robert Koch Institut. Table Showing Current Covid-19 Infections Per Day (Time Series) (In German). 2021. Available online: https://npgeo-corona-npgeo-de.hub.arcgis.com/datasets/dd4580c810204019a7b8eb3e0b329dd6_0/explore (accessed on 3 November 2020).
- Bommer, C.; Vollmer, S. Average Detection Rate of SARS-CoV-2 Infections Is Estimated Around Six Percent; University of Goettingen: Göttingen, Germany, 2020. [Google Scholar]
- Schlosser, F.; Maier, B.F.; Jack, O.; Hinrichs, D.; Zachariae, A.; Brockmann, D. COVID-19 lockdown induces disease-mitigating structural changes in mobility networks. Proc. Natl. Acad. Sci. USA 2020, 117, 32883–32890. Available online: https://www.pnas.org/content/early/2020/12/02/2012326117 (accessed on 8 July 2021). [CrossRef]
- Thünen-Institut für Ländliche Räume—Braunschweig. Land Atlas. 2021. Available online: www.landatlas.de (accessed on 15 July 2021).
- Pearson, K. On lines and planes of closest fit to systems of points in space. London Edinburgh Dublin Philos. Mag. J. Sci. 2010, 2, 559–572. [Google Scholar] [CrossRef] [Green Version]
- Brockwell, P.J.; Davis, R.A. Introduction to Time Series and Forecasting; Springer: Berlin/Heidelberg, Germany, 2016; ISBN 978-3-319-29854-2. [Google Scholar]
- Huber, P.J. Robust Statistics; John Wiley & Sons, Inc.: Hoboken, NJ, USA, 2004. [Google Scholar]
- Food Service Portal—Germany. How the Federal States are Opening Up Gastronomy (German Article). 2020. Available online: https://www.food-service.de/praxis/gesetze/re-start—coronakrise-wie-die-einzelnen-bundeslaender-die-gastronomie-hochfahren-45240 (accessed on 1 June 2021).
- Jay, J.; Bor, J.; Nsoesie, E.; Lipson, S.K.; Jones, D.K.; Galea, S.; Raifman, J. Neighborhood income and physical distancing during the COVID-19 pandemic in the US. MedRxiv 2020, 4, 1294–1302. [Google Scholar]
- Bradley, E.H.; Curry, L.A.; Ramanadhan, S.; Rowe, L.; Nembhard, I.M.; Krumholz, H.M. Research in action: Using positive deviance to improve quality of health care. Implement. Sci. 2009, 4, 25. [Google Scholar] [CrossRef] [Green Version]
- Günther, T.; Czech-Sioli, M.; Indenbirken, D.; Robitaille, A.; Tenhaken, P.; Exner, M.; Ottinger, M.; Fischer, N.; Grundhoff, A.; Brinkmann, M.M. SARS-CoV-2 outbreak investigation in a German meat processing plant. EMBO Mol. Med. 2020, 12, e13296. [Google Scholar] [CrossRef]
- Tagesschau. The Corona Situation at a Glance (in German). 2021. Available online: https://www.tagesschau.de/inland/schlachthof-lohne-101.html (accessed on 11 August 2021).
- Bedford, J.; Enria, D.; Giesecke, J.; Heymann, D.L.; Ihekweazu, C.; Kobinger, G.; Lane, H.C.; Memish, Z.A.; Oh, M.; Sall, A.A.; et al. Living with the COVID-19 pandemic: Act now with the tools we have. Lancet 2020, 396, 1314–1316. [Google Scholar] [CrossRef]
- Bahá’í World News Service. Radio Broadcasts in Uganda Comfort and Inspire Amidst Crisis. 2021. Available online: https://news.bahai.org/story/1409/ (accessed on 15 July 2021).
- Jewett, R.L.; Mah, S.M.; Howell, N.; Larsen, M.M. Social Cohesion and Community Resilience During COVID-19 and Pandemics: A Rapid Scoping Review to Inform the United Nations Research Roadmap for COVID-19 Recovery. Int. J. Health Serv. 2021, 51, 325–336. [Google Scholar] [CrossRef]
- Dayrit, M.; Mendoza, R.U. Social Cohesion vs COVID-19. SSRN Electron. J. 2020, 25, 191–203. [Google Scholar] [CrossRef]
- Makridis, C.A.; Wu, C. How social capital helps communities weather the COVID-19 pandemic. PLoS ONE 2021, 16, e0245135. [Google Scholar] [CrossRef]
- Heydari, S.T.; Zarei, L.; Sadati, A.K.; Moradi, N.; Akbari, M.; Mehralian, G.; Lankarani, K.B. The effect of risk communication on preventive and protective Behaviours during the COVID-19 outbreak: Mediating role of risk perception. BMC Public Health 2021, 21. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Risk Communication and Community Engagement Readiness and Response to Coronavirus Disease (COVID-19): Interim Guidance; WHO: Geneva, Switzerland, 2020; Available online: https://www.who.int/publications/i/item/risk-communication-and-community-engagement-readiness-and-initial-response-for-novel-coronaviruses (accessed on 19 March 2020).
- Wilkinson, A.; Fairhead, J. Comparison of social resistance to Ebola response in Sierra Leone and Guinea suggests explanations lie in political configurations not culture. Crit. Public Health 2017, 27, 14–27. [Google Scholar] [CrossRef]
- Vinck, P.; Pham, P.N.; Bindu, K.K.; Bedford, J.; Nilles, E.J. Institutional trust and misinformation in the response to the 2018–19 Ebola outbreak in North Kivu, DR Congo: A population-based survey. Lancet Infect. Dis. 2019, 19, 529–536. [Google Scholar] [CrossRef] [Green Version]
- Trapido, J. Ebola: Public trust, intermediaries, and rumour in the DR Congo. Lancet Infect. Dis. 2019, 19, 457–458. [Google Scholar] [CrossRef] [Green Version]
- Terpstra, T.; Enader, A.; Gutteling, J.; Kuhlicke, C. Communicating Disaster Risk. In Public Perception of Risk (Chapter 4); The Joint Research Centre (JPR): Ispra, Italy, 2017; pp. 393–440. [Google Scholar]
- Ransome, Y.; Ojikutu, B.O.; Buchanan, M.; Johnston, D.; Kawachi, I. Neighborhood Social Cohesion and Inequalities in COVID-19 Diagnosis Rates by Area-Level Black/African American Racial Composition. J. Urban Health 2021, 98, 222–232. [Google Scholar] [CrossRef]
- Chuang, Y.-C.; Huang, Y.-L.; Tseng, K.-C.; Yen, C.-H.; Yang, L.-H. Social capital and health-protective behavior intentions in an influenza pandemic. PLoS ONE 2015, 10, e0122970. [Google Scholar]
- Brayne, C. Mitigation of disasters through community cohesion. Lancet Planetry Health 2017, 1, e86–e87. [Google Scholar] [CrossRef]
- Mendez-Brito, A.; El-Bcheraoui, C.; Pozo-Martin, F. Systematic review of empirical studies comparing the effectiveness of non-pharmaceutical interventions against COVID-19. J. Infect. 2021, in press. [Google Scholar] [CrossRef]
- Alzunitan, M.; Edmond, M.; Alsuhaibani, M.; Samuelson, R.; Schweizer, M.; Marra, A. Positive deviance in infection prevention and control: A systematic literature review. Infect. Control Hosp. Epidemiol. 2020, 1–8. [Google Scholar] [CrossRef]
- Gladwin, C.; Peterson, J.; Mwale, A. The quality of science in participatory research: A case study from Eastern Zambia. World Dev. 2002, 30, 523–543. [Google Scholar] [CrossRef]
- Robert Koch Institut. Epidemiologisches Bulletin; Robert Koch Institut: Berlin, Germany, 2020; Available online: https://www.rki.de/DE/Content/Infekt/EpidBull/Archiv/2020/Ausgaben/49_20.pdf?__blob=publicationFile (accessed on 8 July 2021).
- Inglesby, T.V. Public Health Measures and the Reproduction Number of SARS-CoV-2. JAMA 2020, 323, 2186–2187. [Google Scholar] [CrossRef] [PubMed]
- Ives, A.R.; Bozzuto, C. Estimating and explaining the spread of COVID-19 at the county level in the USA. Commun. Biol. 2021, 4, 6. [Google Scholar] [CrossRef]
- United Nations. Better Data. Better Lives; United Nations: New York, NY, USA, 2015; Available online: https://www.un.org/en/desa/better-data-saves-lives (accessed on 8 July 2021).
- Thabane, L.; Mbuagbaw, L.; Zhang, S.; Samaan, Z.; Marcucci, M.; Ye, C.; Thabane, M.; Giangregorio, L.; Dennis, B.; Kosa, D.; et al. A tutorial on sensitivity analyses in clinical trials: The what, why, when and how. BMC Med. Res. Methodol. 2013, 13, 92. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Lima, R.; Sampaio, R. What is uncertainty quantification? J. Braz. Soc. Mech. Sci. Eng. 2018, 40, 155. [Google Scholar] [CrossRef]
- van de Schoot, R.; Depaoli, S.; King, R.; Kramer, B.; Märtens, K.; Tadesse, M.G.; Vannucci, M.; Gelman, A.; Veen, D.; Willemsen, J.; et al. Bayesian statistics and modelling. Nat. Rev. Methods Primers 2021, 1, 1. [Google Scholar] [CrossRef]

| Data Source (DS) | Data Type | Variables Used |
|---|---|---|
| 1. RKI 1 | SARS-CoV-2 case reports | Weekly reproduction factor (log scale). |
| 2. Teralytics | Mobility data | Weekly number of trips both starting and ending in the respective district, i.e., internal trips and roundtrips. Weekly number of incoming trips to the respective district. Weekly incoming infection load, i.e., incoming trips multiplied by new cases per capita of the origin districts. All mobility features were standardized relative to population size in 2019. |
| 3. DWD 2 | Weather data | Weekly average temperature. Weekly average humidity. Weekly average precipitation per day. Weekly average hours of sunshine per day. |
| 4. Landatlas study, Thünen-Institute | Structural data | Ruralness Index. Socioeconomic Status Index. |
| Variable | Mean | SD | Min. | PR-25 | PR-50 | PR-75 | Max. |
|---|---|---|---|---|---|---|---|
| Log of R-factor | −0.02 | 0.78 | −4.33 | −0.53 | 0 | 0.45 | 3.37 |
| R-factor | 1.35 | 1.48 | 0.01 | 0.59 | 1 | 1.57 | 29 |
| Internal trips per inhabitant | 9.98 | 2.98 | 3.62 | 8.01 | 9.57 | 11.34 | 33.11 |
| Incoming trips per inhabitant | 4.28 | 1.78 | 0.7 | 2.98 | 3.99 | 5.37 | 12.62 |
| Incoming infection load (10−5 per inhabitant) | 42 | 53.6 | 0.48 | 11.06 | 24.77 | 53.12 | 898.93 |
| Average temperature (°C) | 14.78 | 4.9 | 0.16 | 11.64 | 15.51 | 18.18 | 25.41 |
| Average humidity (%) | 66.42 | 9.11 | 20.11 | 60.43 | 67.23 | 73.13 | 90.57 |
| Average daily precipitation (cm) | 1.58 | 1.98 | 0 | 0.11 | 0.87 | 2.36 | 21.72 |
| Average daily sunshine (minutes) | 473.67 | 145.73 | 34.03 | 354.92 | 474.22 | 594.8 | 801.24 |
| Standardized socio-economic status index | 0 | 1 | −2.66 | −0.55 | 0.06 | 0.65 | 3.45 |
| Standardized ruralness index | 0 | 1 | −4.18 | −0.6 | 0.39 | 0.72 | 1.44 |
| District | PD Timeframe | Province | Ranking during First Lockdown | Ranking during Summer Vacation | Rur. | SES | Pop. | Pop.-Dens. |
|---|---|---|---|---|---|---|---|---|
| City of Koblenz | First Lockdown | Rhineland-Palatinate | 1 | 68 | −1.16 | 0.69 | 114052 | 1084 |
| Lörrach | First Lockdown | Baden-Wuerttemberg | 2 | 254 | −0.03 | 0.97 | 228736 | 284 |
| City of Würzburg | First Lockdown | Bavaria | 3 | 392 | −1.29 | 0.49 | 127934 | 1460 |
| Gütersloh | Summer Vacation | North Rine-Westphalia | 310 | 1 | 0.03 | 0.84 | 364938 | 377 |
| Dingolfing-Landau | Summer Vacation | Bavaria | 291 | 2 | 0.83 | 1.99 | 96683 | 110 |
| Vechta | Summer Vacation | Lower Saxony | 49 | 3 | 0.8 | 0.47 | 142814 | 175 |
| Theme | Characteristics |
|---|---|
| 1. Characteristics of local administrations’ fast-paced SARS-CoV-2 emergency response | 1.1. Action bias |
| 1.2. Agility in public administration | |
| 1.3. Fill regulatory gaps/Courage to deviate | |
| 1.4. Cross-organizational collaboration | |
| 2. Preparedness | 2.1. Risk consciousness and early initiation of measures |
| 2.2. Emergency infrastructure and procurement | |
| 3. Situational analysis and reporting | 3.1. Data Flow |
| 3.2. Analyses and Projections | |
| 3.3. IT System in health departments | |
| 4. Containment | 4.1. Strive to remain in control |
| 4.2. Shut down and isolate early and comprehensively | |
| 4.3. Large scale testing | |
| 5. Communication | 5.1. Reliable and trustworthy public communication |
| 5.2. Consistent health messages across all channels | |
| 6. Utilization of social capital | 6.1. Personal networks (of decision makers) |
| 6.2. Role of social cohesion | |
| 7. Community compliance | 7.1. Early preparedness measures reinforce risk consciousness among the population |
| 7.2. Proximity of major outbreak increases compliance |
| Variable | Suggested Data Source | URL |
|---|---|---|
| SARS-CoV-2 case numbers | WHO Coronavirus Dashboard | https://covid19.who.int/table (accessed on 12 July 2021) |
| SARS-CoV-2 R0 | WHO Coronavirus Dashboard | https://covid19.who.int/table (accessed on 12 July 2021) |
| Individual data mobility | Google Mobility | https://www.google.com/covid19/mobility/ (accessed on 12 July 2021) |
| Ruralness per country | World Bank—Rural access index | https://datacatalog.worldbank.org/dataset/rural-access-index-rai (accessed on 12 July 2021) |
| Socio-economic status * | World Bank ^ | https://data.worldbank.org/country (accessed on 12 July 2021) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Driesen, J.; El-Khatib, Z.; Wulkow, N.; Joblin, M.; Vasileva, I.; Glücker, A.; Kruspel, V.; Vogel, C. Data-Powered Positive Deviance during the SARS-CoV-2 Pandemic—An Ecological Pilot Study of German Districts. Int. J. Environ. Res. Public Health 2021, 18, 9765. https://doi.org/10.3390/ijerph18189765
Driesen J, El-Khatib Z, Wulkow N, Joblin M, Vasileva I, Glücker A, Kruspel V, Vogel C. Data-Powered Positive Deviance during the SARS-CoV-2 Pandemic—An Ecological Pilot Study of German Districts. International Journal of Environmental Research and Public Health. 2021; 18(18):9765. https://doi.org/10.3390/ijerph18189765
Chicago/Turabian StyleDriesen, Joshua, Ziad El-Khatib, Niklas Wulkow, Mitchell Joblin, Iskriyana Vasileva, Andreas Glücker, Valentin Kruspel, and Catherine Vogel. 2021. "Data-Powered Positive Deviance during the SARS-CoV-2 Pandemic—An Ecological Pilot Study of German Districts" International Journal of Environmental Research and Public Health 18, no. 18: 9765. https://doi.org/10.3390/ijerph18189765
APA StyleDriesen, J., El-Khatib, Z., Wulkow, N., Joblin, M., Vasileva, I., Glücker, A., Kruspel, V., & Vogel, C. (2021). Data-Powered Positive Deviance during the SARS-CoV-2 Pandemic—An Ecological Pilot Study of German Districts. International Journal of Environmental Research and Public Health, 18(18), 9765. https://doi.org/10.3390/ijerph18189765







