The Association of Interpersonal Relationships and Social Services with the Self-Rated Health of Spanish Homelessness
Abstract
1. Introduction
1.1. Personal Variables and Self-Rated Health
1.2. Interpersonal Relationships, Social Services Support and SRH
1.3. The Present Study
2. Materials and Methods
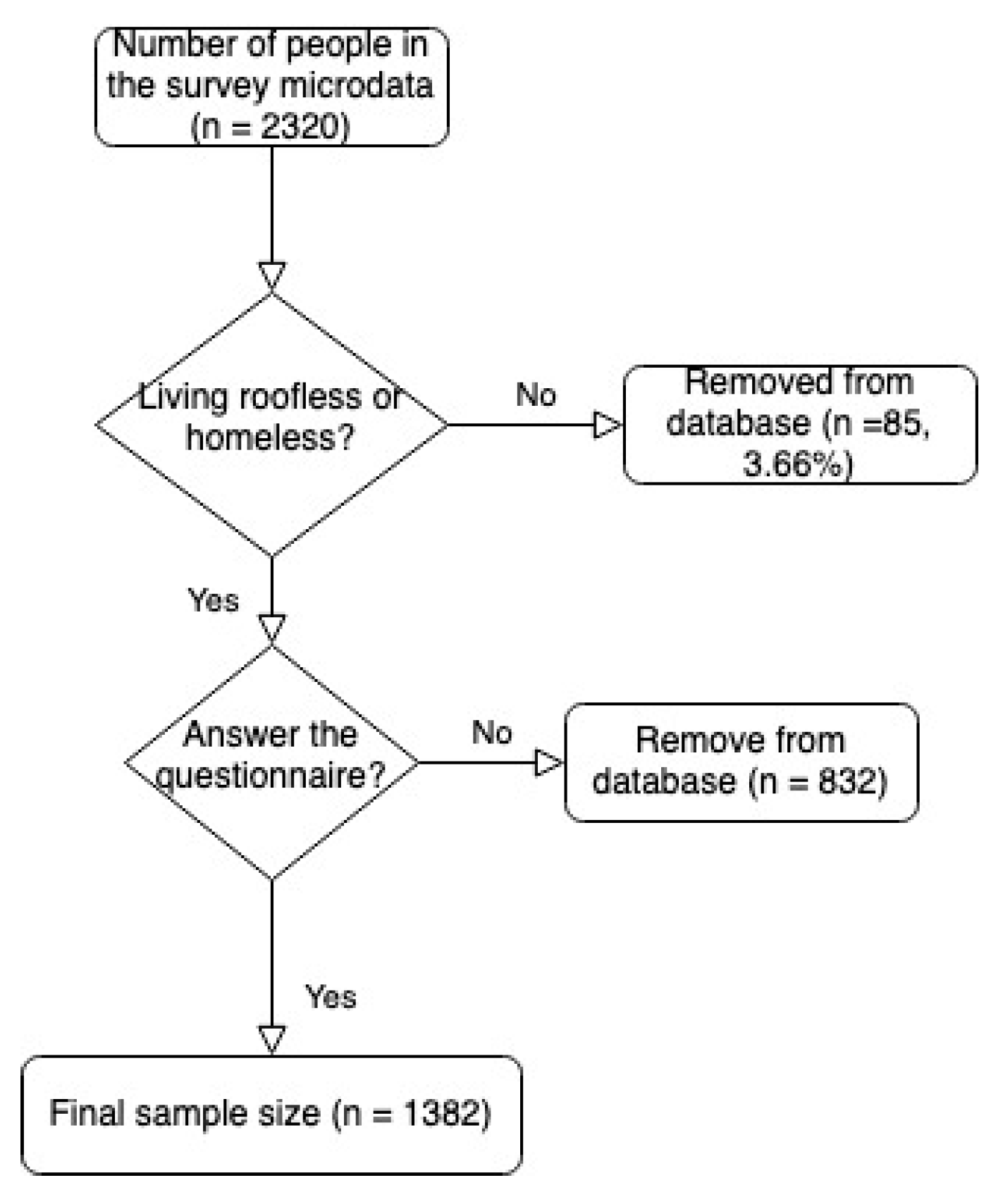
2.1. Participants
2.2. Instrument
- How long have you been living without accommodation that you can consider your home? We refer to the time that you have been homeless, that is, sleeping on the street, in a shelter or from one pension to another (time being homeless). Participants had to write down how many years and months they had been in that situation; if it took less than one year, they had to point the number of months.
- Family and social relationships. This section had two items: (1) In general, do you have a family member with whom you have contact from time to time, either in person and/or through the phone, mail, or internet? The response options were two, Yes or No; and (2) Do you usually spend most of the day alone or do you often spend time together with other people? The response options were also two, I spend most of the day alone, or I spend most of the day with other people.
- Use of services. The question was, “In the last six months of the services or benefits mentioned below, could you say which ones you have used?” The response options were day center, health center or hospital, and mental health center. Each question had two response options: Yes or No.
- Perception of being helped from social services. The question asked, “Please tell me considering your experience if social services have helped you” and had four options: None, Low, Sufficient, or High.
- Health perception. The question was, “In general, how would you say your health is?”, with five answer options: Very good, Good, Regular, Bad, or Very bad.
2.3. Variables
2.4. Statistical Analysis
3. Results
4. Discussion
4.1. Personal Variables and SRH
4.2. Interpersonal Relationships and SRH
4.3. Social Services Support and SRH
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Appendix A
| Categories | Variables | Bad vs. Non-Bad | |
|---|---|---|---|
| β a | O.R. b | ||
| Personal variables | Gender (female) | 0.89 [−0.28, 0.46] | 1.09 |
| Time being homeless c | 0.004 [−0.005, 0.15] | 1.004 | |
| Interpersonal relationships | Family relationships | −0.40 ** [−0.81, −0.009] | 0.67 |
| Spending the day alone | 0.30 [−0.45, 0.65] | 1.35 | |
| Use of social services and perceived help | Use of mental health services | 0.57 ** [0.23, 0.92] | 1.77 ** |
| Use of health care services | 1.05 ** [0.46, 1.58] | 2.86 ** | |
| Use of day center | −1.06 ** [−1.74, −0.38] | 0.35 ** | |
| Perceived help by social services | |||
| Low | −0.52 [−1.08, 0.32] | 0.59 | |
| Sufficient | −0.67 ** [−1.22, 0.12] | 0.51 ** | |
| High | −0.60 ** [−1.16, 0.04] | 0.99 ** | |
| Constant | −1.36 ** [−2.23,−0.54] | 0.25 ** | |
| L2 | 56.40 (0.0000) | ||
| Sample size | 1382 | ||
| Categories | Variables | Good vs. Non-Good | |
|---|---|---|---|
| β a | O.R. b | ||
| Personal variables | Gender (female) | 0.02 [−0.24, 0.28] | 1.02 |
| Time being homeless c | −0.01 ** [−0.02, −0.004] | 0.98 ** | |
| Interpersonal relationships | Family relationships | 0.22 [−0.09, 0.53] | 1.25 |
| Spending the day alone | −0.39 ** [−0.64, −0.15] | 0.67 ** | |
| Use of social services and perceived help | Use of mental health services | −0.62 ** [−0.87, −0.37] | 0.53 ** |
| Use of health care services | −0.92 ** [−1.21, −0.62] | 0.40 ** | |
| Use of day center | 0.46 [−0.07, 0.99] | 1.58 | |
| Perceived help by social services | |||
| Low | 0.001 [−0.43, 0.43] | 1.001 | |
| Sufficient | 0.24 [−0.19, 0.66] | 1.27 | |
| High | 0.27 [−0.16, 0.70] | 1.31 | |
| Constant | 0.60 [−0.06, 1.26] | 1.82 | |
| L2 | 108.91 (0.0000) | ||
| Sample size | 1382 | ||
| Categories | Variables | β a | O.R. b |
|---|---|---|---|
| Personal variables | Gender (female) | 0.05 [−0.24, 0.28] | 1.004 |
| Time being homeless c | 0.01 ** [−0.02, −0.004] | 1.002 ** | |
| Interpersonal Relationships | Family relationships | 0.25 [−0.09, 0.53] | 0.78 |
| Spending the day alone | 0.37 ** [−0.64, −0.15] | 1.44 ** | |
| Use of social services and perceived help | Use of mental health services | 0.63 ** [−0.87, −0.37] | 1.87 ** |
| Use of health care services | 0.93 ** [−1.21, −0.62] | 2.53 ** | |
| Use of day center | −0.62 ** [−0.07, 0.99] | 0.54 ** | |
| Perceived help by social services | |||
| Low | −0.02 [−0.43, 0.43] | 0.85 | |
| Sufficient | −0.37 [−0.19, 0.66] | 0.69 | |
| High | −0.40 [−0.16, 0.70] | 0.68 | |
| L2 | 116.27 (0.0000) | ||
| Sample size | 1382 |
| Categories | Variables | “Regular” vs. “Good” | “Bad” vs. “Good” |
|---|---|---|---|
| β a | β a | ||
| Personal variables | Gender (female) | −0.84 [−0.28, 0.19] | 0.39 [−0.24, 0.32] |
| Time being homeless b | 0.01 ** [0.004, 0.02] | 0.008 [−0.004, 0.02] | |
| Interpersonal Relationships | Family relationships | −0.10 [−0.38, 0.18] | −0.34 ** [−0.66, −0.03] |
| Spending the day alone | 0.31 [0.08, 0.53] | 0.34 ** [0.08, 0.61] | |
| Use of social services and perceived help | Use of mental health services | 0.46 ** [0.23, 0.68] | 0.59 ** [0.32, 0.85] |
| Use of health care services | 0.65 ** [0.39, 0.91] | 0.95 ** [0.60, 1.30] | |
| Use of day center | −0.13 [−0.63, 0.37] | −0.77 ** [−1.31, 0.24] | |
| Perceived help by social services | |||
| Low | 0.16 [−0.23, 0.56] | −0.29 [−0.73, 0.15] | |
| Sufficient | −0.02 [−0.41, 0.36] | −0.46 ** [−0.91, 0.05] | |
| High | −0.07 [−0.47, 0.32] | −0.44 ** [−0.88, 0.002] | |
| Constant | −1.11 ** [−1.73,−0.49] | −0.94 ** [−1.60,−0.28] | |
| Log likelihood | −1236.8535 (0.0000) | ||
| Sample size | 1382 |
References
- Feantsa ETHOS: European Typology on Homelessness and Housing Exclusion. Available online: https://www.feantsa.org/en/toolkit/2005/04/01/ethos-typology-on-homelessness-and-housing-exclusion (accessed on 1 October 2020).
- Amore, K.; Baker, M.; Howden-Chapman, P. The ETHOS Definition and Classification of Homelessness: An Analysis. Eur. J. Homelessness 2011, 5, 19–37. [Google Scholar]
- Edgar, B. The ETHOS Definition and Classification of Homelessness and Housing Exclusion. Eur. J. Homelessness 2012, 6, 219–225. [Google Scholar]
- Calvo, F.; Fitzpatrick, S.; Fàbregas, C.; Carbonell, X.; Turró-Garriga, O. Individuals experiencing chronic homelessness: A 10-year follow-up of a cohort in Spain. Health Soc. Care Community 2020, 28, 1787–1794. [Google Scholar] [CrossRef]
- Nagy-Borsy, E.; Vági, Z.; Skerlecz, P.; Szeitl, B.; Kiss, I.; Rákosy, Z. Health status and health behaviour of the Hungarian homeless people. Arch. Public Health 2021, 79, 15. [Google Scholar] [CrossRef] [PubMed]
- Gil-Salmeron, A.; Smith, L.; Yang, L.; Rieder, A.; Grabovac, I. Differences in health status, health behaviour and healthcare utilisation between Immigrant and native homeless people in Spain: An exploratory study. Health Soc. Care Community 2021, 29, 856–866. [Google Scholar] [CrossRef]
- Government of Spain Estrategia Nacional Integral para Personas Sin Hogar 2015–2020. Available online: www.msssi.gob.es (accessed on 17 October 2017).
- National Statistics Institute. Encuesta Sobre Centros y Servicios de Atención a Personas Sin Hogar. 2017. Available online: https://www.ine.es/dyngs/INEbase/es/operacion.htm?c=Estadistica_C&cid=1254736176925&menu=resultados&idp=1254735976608 (accessed on 25 January 2021).
- National Statistics Institute. Encuesta de Centros y Servicios de Atención a las Personas sin Hogar. Available online: https://www.ine.es/prensa/ecapsh_2018.pdf (accessed on 5 February 2021).
- Muñoz, M.; Sanchez, M.R.; Cabrera, P.J. Informe IX Recuento de Personas Sin Hogar en Madrid; Madrid, Spain. 2019. Available online: https://www.madrid.es/UnidadesDescentralizadas/IntegracionyEmergenciaSocial/SAMUR Social/ficheros/INFORME RECUENTO 2018_FINAL.pdf (accessed on 24 February 2021).
- Foundation Abbé Pierre; FEANTSA. Fourth Overview of Housing Exclusion in Europe; 2019. Available online: https://www.feantsa.org/public/user/Activities/events/OHEEU_2019_ENG_Web.pdf (accessed on 10 February 2021).
- Centro de Documentación y Estudios SiiS.; Fundación Eguía-Careaga. IV Estudio Sobre la Situación de las Personas en Situación de Exclusión Residencial Grave en la CAPV. Available online: https://www.siis.net/documentos/informes/545454.pdf (accessed on 12 January 2021).
- Fajardo-Bullón, F.; Esnaola, I.; Anderson, I.; Benjaminsen, L. Homelessness and self-rated health: Evidence from a national survey of homeless people in Spain. BMC Public Health 2019, 19, 1081. [Google Scholar] [CrossRef]
- Jylhä, M. What is self-rated health and why does it predict mortality? Towards a unified conceptual model. Soc. Sci. Med. 2009, 69, 307–316. [Google Scholar] [CrossRef] [PubMed]
- Castro-Vázquez, A.; Espinosa-Gutierrez, I.; Rodríguez-Contreras, P.; Santos-Iglesias, P. Relación entre el estado de salud percibido e indicadores de salud en la población española. Int. J. Clin. Health Psychol. 2007, 7, 883–898. [Google Scholar]
- Malmusi, D.; Artazcoz, L.; Benach, J.; Borrell, C. Perception or real illness? How chronic conditions contribute to gender inequalities in self-rated health. Eur. J. Public Health 2012, 22, 781–786. [Google Scholar] [CrossRef]
- Dowd, J.B.; Zajacova, A. Does the predictive power of self-rated health for subsequent mortality risk vary by socioeconomic status in the US? Int. J. Epidemiol. 2007, 36, 1214–1221. [Google Scholar] [CrossRef]
- Idler, E.L.; Benyamini, Y. Self-rated health and mortality: A review of twenty-seven community studies. J. Health Soc. Behav. 1997, 38, 21–37. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.; Shinkai, S. A comparison of correlates of self-rated health and functional disability of older persons in the Far East: Japan and Korea. Arch. Gerontol. Geriatr. 2003, 37, 63–76. [Google Scholar] [CrossRef]
- World Health Organization. Health Interview Surveys: Towards International Harmonization of Methods and Instruments; WHO Office for Europe: Copenhagen, Denmark, 1996; ISBN 92-890-1322-2. [Google Scholar]
- Zajacova, A.; Dowd, J.B. Reliability of Self-rated Health in US Adults. Am. J. Epidemiol. 2011, 174, 977–983. [Google Scholar] [CrossRef]
- Clifford, B.; Wilson, A.; Harris, P. Homelessness, health and the policy process: A literature review. Health Policy 2019, 123, 1125–1132. [Google Scholar] [CrossRef]
- Fazel, S.; Geddes, J.R.; Kushel, M. The health of homeless people in high-income countries: Descriptive epidemiology, health consequences, and clinical and policy recommendations. Lancet 2014, 384, 1529–1540. [Google Scholar] [CrossRef]
- Barrow, S.M.; Herman, D.B.; Córdova, P.; Struening, E.L. Mortality among homeless shelter residents in New York City. Am. J. Public Health 1999, 89, 529–534. [Google Scholar] [CrossRef]
- Bambra, C.; Pope, D.; Swami, V.; Stanistreet, D.; Roskam, A.; Kunst, A.; Scott-Samuel, A. Gender, health inequalities and welfare state regimes: A cross-national study of 13 European countries. J. Epidemiol. Community Health 2009, 63, 38–44. [Google Scholar] [CrossRef]
- Zajacova, A.; Huzurbazar, S.; Todd, M. Gender and the structure of self-rated health across the adult life span. Soc. Sci. Med. 2017, 187, 58–66. [Google Scholar] [CrossRef] [PubMed]
- Fajardo-Bullón, F.; Pérez-Mayo, J.; Esnaola, I.; Anderson, I.; Knutagård, M. Influence of psychosocial variables on the health of people living in housing exclusion. Int. J. Environ. Res. Public Health 2020, 17, 8983. [Google Scholar] [CrossRef]
- Hwang, S.; Kirst, M.J.; Chiu, S.; Tolomiczenko, G.; Kiss, A.; Cowan, L.; Levinson, W. Multidimensional social support and the health of homeless individuals. J. Urban Health 2009, 86, 791–803. [Google Scholar] [CrossRef]
- Wolf, J.; Anderson, I.; Van den Dries, L.; Filipovic-Hrast, M. The health of homeless women. In Women’s Homelessness in Europe: A Reader; Mayock, P., Bretherton, J., Eds.; Palgrave M: London, UK, 2016; pp. 155–178. [Google Scholar]
- Peplau, H. The Art and Science of Nursing: Similarities, Differences, and Relations. Nurs. Sci. Q. 1988, 1, 8–15. [Google Scholar] [CrossRef]
- Peplau, H. Interpersonal Relations in Nursing: A Conceptual Frame of Reference for Psychodynamic Nursing; G. P. Putnam’s Sons: New York, NY, USA, 1952. [Google Scholar]
- Forchuk, C.; Reynolds, W.; Sharkey, S.; Martin, M.L.; Jensen, E. Transitional Discharge Based on Therapeutic Relationships: State of the Art. Arch. Psychiatr. Nurs. 2007, 21, 80–86. [Google Scholar] [CrossRef]
- Peplau, H. Interpersonal Relations: A Theoretical Framework for Application in Nursing Practice. Nurs. Sci. Q. 1992, 5, 13–18. [Google Scholar] [CrossRef]
- Peplau, H. Quality of Life: An Interpersonal Perspective. Nurs. Sci. Q. 1994, 7, 10–15. [Google Scholar] [CrossRef] [PubMed]
- Khandor, E.; Mason, K. The Street Health Report; Street Health: Toronto, ON, Canada, 2007. [Google Scholar]
- Berkman, L.F.; Glass, T. Social integration, social networks, social support, and health. In Social Epidemiology; Berkman, L.F., Kawachi, I., Eds.; Oxford University Press: New York, NY, USA, 2000; pp. 137–173. [Google Scholar]
- Noh, S.; Kaspar, V. Perceived Discrimination and Depression: Moderating Effects of Coping, Acculturation, and Ethnic Support. Am. J. Public Health 2003, 93, 232–238. [Google Scholar] [CrossRef]
- Kawachi, I.; Berkman, L.F. Social ties and mental health. J. Urban Health 2001, 78, 458–467. [Google Scholar] [CrossRef]
- Kurtz, P.D.; Lindsey, E.W.; Jarvis, S.; Nackerud, L. How runaway and homeless youth navigate troubled waters: The role of formal and informal helpers. Child Adolesc. Soc. Work J. 2000, 17, 381–402. [Google Scholar] [CrossRef]
- Asante, S.; Castillo, J. Social connectedness, perceived social support, and health among older adults. Innov. Aging 2018, 2, 737. [Google Scholar] [CrossRef]
- Kirst, M.; Zerger, S.; Harris, D.W.; Plenert, E.; Stergiopoulos, V. The promise of recovery: Narratives of hope among homeless individuals with mental illness participating in a Housing First randomised controlled trial in Toronto, Canada. BMJ Open 2014, 4, e004379. [Google Scholar] [CrossRef] [PubMed]
- Lam, J.A.; Rosenheck, R. Social support and service use among homeless persons with serious mental illness. Int. J. Soc. Psychiatry 1999, 45, 13–28. [Google Scholar] [CrossRef]
- Meeks, S.; Murrell, S.A. Service providers in the social networks of clients with severe mental illness. Schizophr. Bull. 1994, 20, 399–406. [Google Scholar] [CrossRef] [PubMed]
- Matulič-Domadzič, V.; Munté-Pascual, A.; De Vicente-Zueras, I.; León-Jiménez, S. “Life Starts for Me Again.” The Social Impact of Psychology on Programs for Homeless People: Solidarity Networks for the Effectiveness of Interventions. Front. Psychol. 2020, 10, 3069. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Moreno, S.; Panadero, S.; Vázquez, J.J. Risk of mental ill-health among homeless women in Madrid (Spain). Arch. Womens. Ment. Health 2020, 23, 657–664. [Google Scholar] [CrossRef]
- Gasior, S.; Forchuk, C.; Regan, S. Youth Homelessness: The Impact of Supportive Relationships on Recovery. Can. J. Nurs. Res. 2018, 50, 28–36. [Google Scholar] [CrossRef] [PubMed]
- Guillén, A.I.; Panadero, S.; Vázquez, J.J. Disability, health, and quality of life among homeless women: A follow-up study. Am. J. Orthopsychiatry 2021, 91, 569–577. [Google Scholar] [CrossRef] [PubMed]
- National Institute for Statistics Draft Survey on Homeless People (SHP-2012). Available online: http://www.ine.es/en/daco/daco42/epsh/epshper_12_en.pdf (accessed on 23 January 2021).
- Calvo, F.; Turró-garriga, O.; Fàbregas, C.; Alfranca, R.; Calvet, A.; Salvans, M. Mortality Risk Factors for Individuals Experiencing Homelessness in Catalonia (Spain): A 10-Year Retrospective Cohort Study. Int. J. Environ. Res. Public Health 2021, 18, 1762. [Google Scholar] [CrossRef] [PubMed]
- Roca, P.; Panadero, S.; Moreno, S.R.; Martín, R.M.; Vázquez, J.J. The revolving door to homelessness. The influence of health, alcohol consumption and stressful life events on the number of episodes of homelessness. An. Psicol. 2019, 35, 175–180. [Google Scholar] [CrossRef]
- Hedeker, D. A mixed-efects multinomial logistic regression model. Stat. Med. 2003, 22, 1433–1446. [Google Scholar] [CrossRef]
- Bayaga, A. Multinomial Logistic Regression: Usage and application in risk analysis. J. Appl. Quant. Methods 2010, 5, 288–297. [Google Scholar]
- Hwang, S.W.; Wilkins, R.; Tjepkema, M.; O’Campo, P.J.; Dunn, J.R. Mortality of Métis and registered Indian adults in Canada: An 11-year follow-up study. BMJ 2009, 339, 1068–1070. [Google Scholar] [CrossRef]
- Anderson, I.; Finnerty, J.; McCall, V. Home, housing and communities: Foundations for inclusive society. Soc. Incl. 2020, 8, 1–4. [Google Scholar] [CrossRef]
- Rolfe, S.; Garnham, L.; Godwin, J.; Anderson, I.; Seaman, P.; Donaldson, C. Housing as a social determinant of health and wellbeing: Developing an empirically-informed realist theoretical framework. BMC Public Health 2020, 20, 1138. [Google Scholar] [CrossRef]
- Henwood, B.F.; Cabassa, L.J.; Craig, C.M.; Padgett, D.K. Permanent supportive housing: Addressing homelessness and health disparities? Am. J. Public Health 2013, 103 (Suppl. 2), S188–S192. [Google Scholar] [CrossRef]
- Anderson, I.; Ytrehus, S. Re-conceptualising approaches to meeting the health needs of homeless people. J. Soc. Policy 2012, 41, 551–568. [Google Scholar] [CrossRef][Green Version]
- Rhoades, H.; Wenzel, S.L.; Henwood, B.F. Changes in Self-Rated Physical Health After Moving Into Permanent Supportive Housing. Am. J. Health Promot. 2019, 33, 1073–1076. [Google Scholar] [CrossRef]
- Winland, D.; Gaetz, S.; Patton, T. Family Matters: Homeless Youth and Eva’s “Family Reconnect” Program; The Canadian Homelessness Research Network Press: Toronto, ON, Canada, 2011. [Google Scholar]
- Fitzpatrick, K.M.; Irwin, J.; Lagory, M.; Ritchey, F. Just thinking about it: Social capital and suicide ideation among homeless persons. J. Health Psychol. 2007, 12, 750–760. [Google Scholar] [CrossRef]
- Nyamathi, A.; Leake, B.; Keenan, C.; Gelberg, L. Type of social support among homeless women: Its impact on psychosocial resources, health and health behaviors, and use of health services. Nurs. Res. 2000, 49, 318–326. [Google Scholar] [CrossRef] [PubMed]
- Omerov, P.; Craftman, Å.G.; Mattsson, E.; Klarare, A. Homeless persons’ experiences of health- and social care: A systematic integrative review. Health Soc. Care Community 2020, 28, 511–521. [Google Scholar] [CrossRef]
- McCay, E.; Quesnel, S.; Langley, J.; Beanlands, H.; Cooper, L.; Blidner, R.; Aiello, A.; Mudachi, N.; Howes, C.; Bach, K. A relationship-based intervention to improve social connectedness in street-involved youth: A pilot study. J. Child Adolesc. Psychiatr. Nurs. 2011, 24, 208–215. [Google Scholar] [CrossRef]
- Morcillo, V.; Lorenzo-Cáceres, A.; Domínguez, P.; Rodríguez, R.; Torijano, M.J. Desigualdades en la salud autopercibida de la población española mayor de 65 años. Gac. Sanit. 2014, 28, 511–521. [Google Scholar] [CrossRef]
- Commission, E. Confronting Homelessness in the European Union. Available online: https://eur-lex.europa.eu/legal-content/EN/TXT/PDF/?uri=CELEX:52013SC0042&from=EN (accessed on 23 April 2021).
- Baptista, I.; Marlier, E. Fighting Homelessness and Housing Exclusion in Europe: A Study of National Policies; European Commission: Brussels, Belgium, 2019; ISBN 9789276087694. [Google Scholar]
- Gordon, A.J.; McGinnis, K.A.; Conigliaro, J.; Rodriguez-Barradas, M.C.; Rabeneck, L.; Justice, A.C. Associations between alcohol use and homelessness with healthcare utilization among human immunodeficiency virus-infected veterans. Med. Care 2006, 44, S37–S43. [Google Scholar] [CrossRef] [PubMed]
| Variable (IV) | N (number of observations) | Percentage |
|---|---|---|
| Gender (female) | 336 | 24.31% |
| Family relationships a | 1170 | 84.66% |
| Spending the day alone a | 392 | 28.36% |
| Use of health care services a | 1036 | 74.96% |
| Use of mental health services a | 403 | 29.16% |
| Use of day centers a | 1307 | 94.57% |
| Perceived level of help from social services | ||
| None | 141 | 10.20% |
| Low | 352 | 25.50% |
| Sufficient | 475 | 34.39% |
| High | 413 | 29.91% |
| Variable(IV) | Mean (years) | S.D. |
| Time being homeless | 4.3602 | 5.9966 |
| Explained variable (DV) | N (number of observations) | Percentage |
| Good health | 796 | 56.70% |
| Regular health | 409 | 29.59% |
| Bad health | 177 | 12.81% |
| Variables (IV) | “Regular” vs. “Good” RR b [IC (95%)] | “Bad” vs. “Good” RR b [IC (95%)] |
|---|---|---|
| Gender (female) | 1.04 [0.79, 1.37] | 1.16 [0.80, 1.68] |
| Time being homeless a | 1.02 ** [1.01, 1.02] | 1.01 ** [1.00, 1.03] |
| Family relationships | 0.85 [0.61, 1.19] | 0.56 ** [0.37, 0.84] |
| Spending the day alone | 1.39 ** [1.07, 1.81] | 1.61 ** [1.13, 2.27] |
| Use of mental health services | 2.05 ** [1.58, 2.66] | 2.57 ** [1.83, 3.62] |
| Use of health care services | 2.29 ** [1.70, 3.09] | 2.97 ** [1.88, 4.68] |
| Use of day center | 1.40 [0.78, 2.52] | 0.57 [0.32, 1.05] |
| Perceived help by social services | ||
| Low | 1.28 [0.80, 2.06] | 0.60 [0.34, 1.05] |
| Sufficient | 1.12 [0.71, 1.78] | 0.52 ** [0.31, 0.89] |
| High | 1.03 [0.64, 1.66] | 0.52 ** [0.30, 0.89] |
| Categories | Variables (IV) | “Regular” vs. “Good” | “Bad” vs. “Good” | ||
|---|---|---|---|---|---|
| β a | R.R. b | β | R.R. | ||
| Personal variables | Gender (female) | −0.06 [−0.35, 0.24] | 0.94 | 0.07 [−0.32, 0.46] | 1.07 |
| Time being homeless c | 0.014 ** [0.00, 0.02] | 1.01 ** | 0.01 ** [0.00, 0.02] | 1.01 ** | |
| Interpersonal relationships | Family relationships | −0.12 [−0.47, 0.23] | 0.89 | −0.45 ** [−0.88, −0.01] | 0.64 ** |
| Spending the day alone | 0.37 ** [0.10, 0.65] | 1.45 ** | 0.45 ** [0.08, 0.82] | 1.57 ** | |
| Use of social services and perceived help | Use of mental health services | 0.55 ** [0.27, 0.83] | 1.73 ** | 0.79 ** [0.43, 1.16] | 2.21 ** |
| Use of health care services | 0.78 ** [0.46, 1.11] | 2.19 ** | 1.30 ** [0.77, 1.83] | 3.67 ** | |
| Use of day center | −0.11 [−0.75, 0.53] | 0.89 | −1.10 ** [−1.82, −0.39] | 0.33 ** | |
| Perceived help by social services | |||||
| Low | 0.23 [−0.27, 0.73] | 1.26 | −0.43 [−1.02, 0.15] | 0.64 | |
| Sufficient | 0.00 [−0.49, 0.49] | 0.99 | −0.68 ** [−1.25, −0.09] | 0.51 ** | |
| High | −0.06 [−0.56, 0.43] | 0.99 | −0.63 ** [−1.22,−0.04] | 0.53 ** | |
| Constant | −1.45 ** [−2.18,−0.72] | 0.25 ** | −1.12 ** [−1.90,−0.35] | 0.30 ** | |
| L2 | 128.59 (0.0000) | ||||
| Sample size | 1382 | ||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Fajardo-Bullón, F.; Pérez-Mayo, J.; Esnaola, I. The Association of Interpersonal Relationships and Social Services with the Self-Rated Health of Spanish Homelessness. Int. J. Environ. Res. Public Health 2021, 18, 9392. https://doi.org/10.3390/ijerph18179392
Fajardo-Bullón F, Pérez-Mayo J, Esnaola I. The Association of Interpersonal Relationships and Social Services with the Self-Rated Health of Spanish Homelessness. International Journal of Environmental Research and Public Health. 2021; 18(17):9392. https://doi.org/10.3390/ijerph18179392
Chicago/Turabian StyleFajardo-Bullón, Fernando, Jesús Pérez-Mayo, and Igor Esnaola. 2021. "The Association of Interpersonal Relationships and Social Services with the Self-Rated Health of Spanish Homelessness" International Journal of Environmental Research and Public Health 18, no. 17: 9392. https://doi.org/10.3390/ijerph18179392
APA StyleFajardo-Bullón, F., Pérez-Mayo, J., & Esnaola, I. (2021). The Association of Interpersonal Relationships and Social Services with the Self-Rated Health of Spanish Homelessness. International Journal of Environmental Research and Public Health, 18(17), 9392. https://doi.org/10.3390/ijerph18179392






