The Association between Wearing a Mask and COVID-19
Abstract
:1. Introduction
2. Materials and Methods
2.1. Data Collection
2.2. Data Analysis
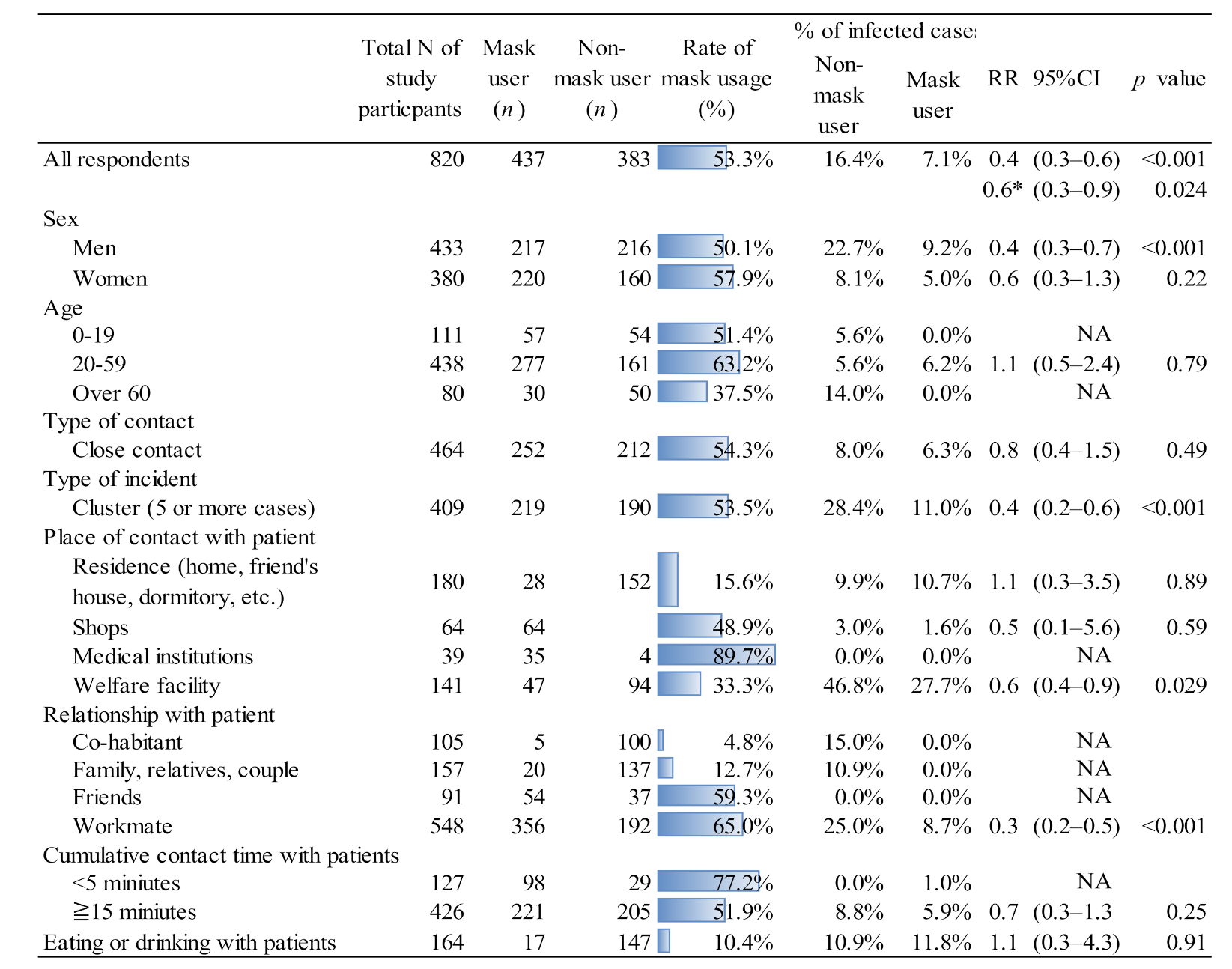
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Greenhalgh, T.; Schmid, M.B.; Czypionka, T.; Bassler, D.; Gruer, L. Face masks for the public during the COVID-19 crisis. BMJ 2020, 369, 1435. [Google Scholar] [CrossRef] [Green Version]
- Feng, C.S.; Xia, N.; Song, W.; Fan, M.; Cowling, B.J. Rational use of face masks in the COVID-19 pandemic. Lancet Respir. Med. 2020, 8, 434–436. [Google Scholar] [CrossRef]
- MacIntyre, C.R.; Chughtai, A.A. A rapid systematic review of the efficacy of face masks and respirators against coronaviruses and other respiratory transmissible viruses for the community, healthcare workers and sick patients. Int. J. Nurs. Stud. 2020, 108, 103629. [Google Scholar] [CrossRef]
- Mitze, T.; Kosfeld, R.; Rode, J.; Walde, K. Face masks considerably reduce COVID-19 cases in Germany. Proc. Natl. Acad. Sci. USA 2020, 117, 32293–32301. [Google Scholar] [CrossRef]
- Bundgaard, H.; Bundgaard, J.S.; Raaschou-Pedersen, D.E.T.; von Buchwald, C.; Todsen, T.; Norsk, J.B.; Pries-Heje, M.M.; Vissing, C.R.; Nielsen, P.B.; Winslow, U.C.; et al. Effectiveness of Adding a Mask Recommendation to Other Public Health Measures to Prevent SARS-CoV-2 Infection in Danish Mask Wearers: A Randomized Controlled Trial. Ann. Intern. Med. 2021, 174, 335–343. [Google Scholar] [CrossRef] [PubMed]
- Cheng, V.C.; Wong, S.C.; Chuang, V.W.; So, S.Y.; Chen, J.H.; Sridhar, S.; To, K.K.; Chan, J.F.; Hung, I.F.; Ho, P.L.; et al. The role of community-wide wearing of face mask for control of coronavirus disease 2019 (COVID-19) epidemic due to SARS-CoV-2. J. Infect. 2020, 81, 107–114. [Google Scholar] [CrossRef] [PubMed]
- Murakami, M.; Yasutaka, T.; Onishi, M.; Naito, W.; Shinohara, N.; Okuda, T.; Fujii, K.; Katayama, K.; Imoto, S. Living with COVID-19: Mass gatherings and minimising risk. QJM 2021, hcab163. [Google Scholar] [CrossRef]
- Manual for Active Epidemiological Surveillance of Patients with Novel Coronavirus Infection (Provisional Version): Addition for the Implementation of Rapid Detection of Clusters (Populations) of Patients. Available online: https://www.niid.go.jp/niid/en/2019-ncov-e/2484-idsc/9472-2019-ncov-02-en.html (accessed on 25 June 2021).
- Standard Disaster Medical Record Report. Available online: https://www.jaam.jp/info/2015/pdf/info-20150602.pdf (accessed on 25 June 2021).
- Schisterman, E.F.; Cole, S.R.; Platt, R.W. Overadjustment bias and unnecessary adjustment in epidemiologic studies. Epidemiology 2009, 20, 488–495. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Carter, R.E.; Lipsitz, S.R.; Tilley, B.C. Quasi-likelihood estimation for relative risk regression models. Biostatistics 2005, 6, 39–44. [Google Scholar] [CrossRef]
- Zou, G. A modified poisson regression approach to prospective studies with binary data. Am. J. Epidemiol. 2004, 159, 702–706. [Google Scholar] [CrossRef]
- Wang, Q.; Yu, C. The role of masks and respirator protection against SARS-CoV-2. Infect. Control. Hosp. Epidemiol. 2020, 41, 746–747. [Google Scholar] [CrossRef] [Green Version]
- Chughtai, A.A.; Seale, H.; Macintyre, C. Effectiveness of Cloth Masks for Protection Against Severe Acute Respiratory Syndrome Coronavirus 2. Emerg. Infect. Dis. 2020, 26, 1–5. [Google Scholar] [CrossRef] [PubMed]
- Guan, W.J.; Ni, Z.Y.; Hu, Y.; Liang, W.H.; Ou, C.Q.; He, J.X.; Liu, L.; Shan, H.; Lei, C.L.; Hui, D.S.; et al. Clinical characteristics of coronavirus disease 2019 in China. N. Engl. J. Med. 2020, 382, 1708–1720. [Google Scholar] [CrossRef]
- Bianchi, I.; Lleo, A.; Gershwin, M.E.; Invernizzi, P. The X chromosome and immune associated genes. J. Autoimmun. 2012, 38, J187–J192. [Google Scholar] [CrossRef]
- Klein, S.L.; Flanagan, K.L. Sex differences in immune responses. Nat. Rev. Immunol. 2016, 16, 626–638. [Google Scholar] [CrossRef]
- Vardavas, C.I.; Nikitara, K. COVID-19 and smoking: A systematic review of the evidence. Tob. Induc. Dis. 2020, 18, 20. [Google Scholar] [CrossRef] [PubMed]
- Avoid the Three Cs. Available online: https://www.mhlw.go.jp/content/3CS.pdf (accessed on 25 June 2021).
- Madewell, Z.J.; Yang, Y.; Longini, I.M.; Halloran, M.E., Jr.; Dean, N.E. Household Transmission of SARS-CoV-2: A Systematic Review and Meta-analysis. JAMA Netw. Open 2020, 3, e2031756. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Li, T.; Barbarino, P.; Gauthier, S.; Brodaty, H.; Molinuevo, J.L.; Xie, H.; Sun, Y.; Yu, E.; Tang, Y.; et al. Dementia care during COVID-19. Lancet 2020, 395, 1190–1191. [Google Scholar] [CrossRef]
- Al-Hanawi, M.K.; Angawi, K.; Alshareef, N.; Qattan, A.M.N.; Helmy, H.Z.; Abudawood, Y.; Alqurashi, M.; Kattan, W.M.; Kadasah, N.A.; Chirwa, G.C.; et al. Knowledge, Attitude and Practice Toward COVID-19 Among the Public in the Kingdom of Saudi Arabia: A Cross-Sectional Study. Front. Public Health 2020, 8, 217. [Google Scholar] [CrossRef]
- Galasso, V.; Pons, V.; Profeta, P.; Becher, M.; Brouard, S.; Foucault, M. Gender differences in COVID-19 attitudes and behavior: Panel evidence from eight countries. Proc. Natl. Acad. Sci. USA 2020, 117, 27285–27291. [Google Scholar] [CrossRef]
- Haischer, M.H.; Beilfuss, R.; Hart, M.R.; Opielinski, L.; Wrucke, D.; Zirgaitis, G.; Uhrich, T.D.; Hunter, S.K. Who is wearing a mask? Gender-, age-, and location-related differences during the COVID-19 pandemic. PLoS ONE 2020, 15, e0240785. [Google Scholar] [CrossRef] [PubMed]
- Lee, L.Y.; Lam, E.P.; Chan, C.K.; Chan, S.Y.; Chiu, M.K.; Chong, W.H.; Chu, K.W.; Hon, M.S.; Kwan, L.K.; Tsang, K.L.; et al. Practice and technique of using face mask amongst adults in the community: A cross-sectional descriptive study. BMC Public Health 2020, 20, 948. [Google Scholar] [CrossRef] [PubMed]
- Al Naam, Y.A.; Elsafi, S.H.; Alkharraz, Z.S.; Alfahad, O.A.; Al-Jubran, K.M.; Al Zahrani, E.M. Community practice of using face masks for the prevention of COVID-19 in Saudi Arabia. PLoS ONE 2021, 16, e0247313. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sugimura, M.; Chimed-Ochir, O.; Yumiya, Y.; Ohge, H.; Shime, N.; Sakaguchi, T.; Tanaka, J.; Takafuta, T.; Mimori, M.; Kuwabara, M.; et al. The Association between Wearing a Mask and COVID-19. Int. J. Environ. Res. Public Health 2021, 18, 9131. https://doi.org/10.3390/ijerph18179131
Sugimura M, Chimed-Ochir O, Yumiya Y, Ohge H, Shime N, Sakaguchi T, Tanaka J, Takafuta T, Mimori M, Kuwabara M, et al. The Association between Wearing a Mask and COVID-19. International Journal of Environmental Research and Public Health. 2021; 18(17):9131. https://doi.org/10.3390/ijerph18179131
Chicago/Turabian StyleSugimura, Mana, Odgerel Chimed-Ochir, Yui Yumiya, Hiroki Ohge, Nobuaki Shime, Takemasa Sakaguchi, Junko Tanaka, Toshiro Takafuta, Michi Mimori, Masao Kuwabara, and et al. 2021. "The Association between Wearing a Mask and COVID-19" International Journal of Environmental Research and Public Health 18, no. 17: 9131. https://doi.org/10.3390/ijerph18179131
APA StyleSugimura, M., Chimed-Ochir, O., Yumiya, Y., Ohge, H., Shime, N., Sakaguchi, T., Tanaka, J., Takafuta, T., Mimori, M., Kuwabara, M., Asahara, T., Kishita, E., & Kubo, T. (2021). The Association between Wearing a Mask and COVID-19. International Journal of Environmental Research and Public Health, 18(17), 9131. https://doi.org/10.3390/ijerph18179131





