The Impact of Parental Stress on Italian Adolescents’ Internalizing Symptoms during the COVID-19 Pandemic: A Longitudinal Study
Abstract
:1. Introduction
1.1. Adolescents’ Internalizing Symptoms during COVID-19 Quarantine
1.2. Parental Stress and Adolescents’ Internalizing Symptoms
1.3. The Mediation Role of Parents’ Expressive Suppression
1.4. The Current Study
2. Materials and Methods
2.1. Participants and Procedures
2.2. Measures
2.2.1. Adolescents’ Anxiety and Depression Symptoms in response to the Quarantine at T1, T2, and T3
2.2.2. Parental Stress at T2
2.2.3. Parents’ Expressive Suppression at T2
2.2.4. Adolescents’ Internalizing Symptoms at T3
2.3. Data Analysis
3. Results
3.1. Attrition Analyses
3.2. Adolescents’ Anxiety and Depression Symptoms
3.3. Descriptive Statistics and Bivariate Correlations
3.4. The Effect of Sociodemographic Variables on Expressive Suppression and Adolescents’ Anxiety and Depression Symptoms
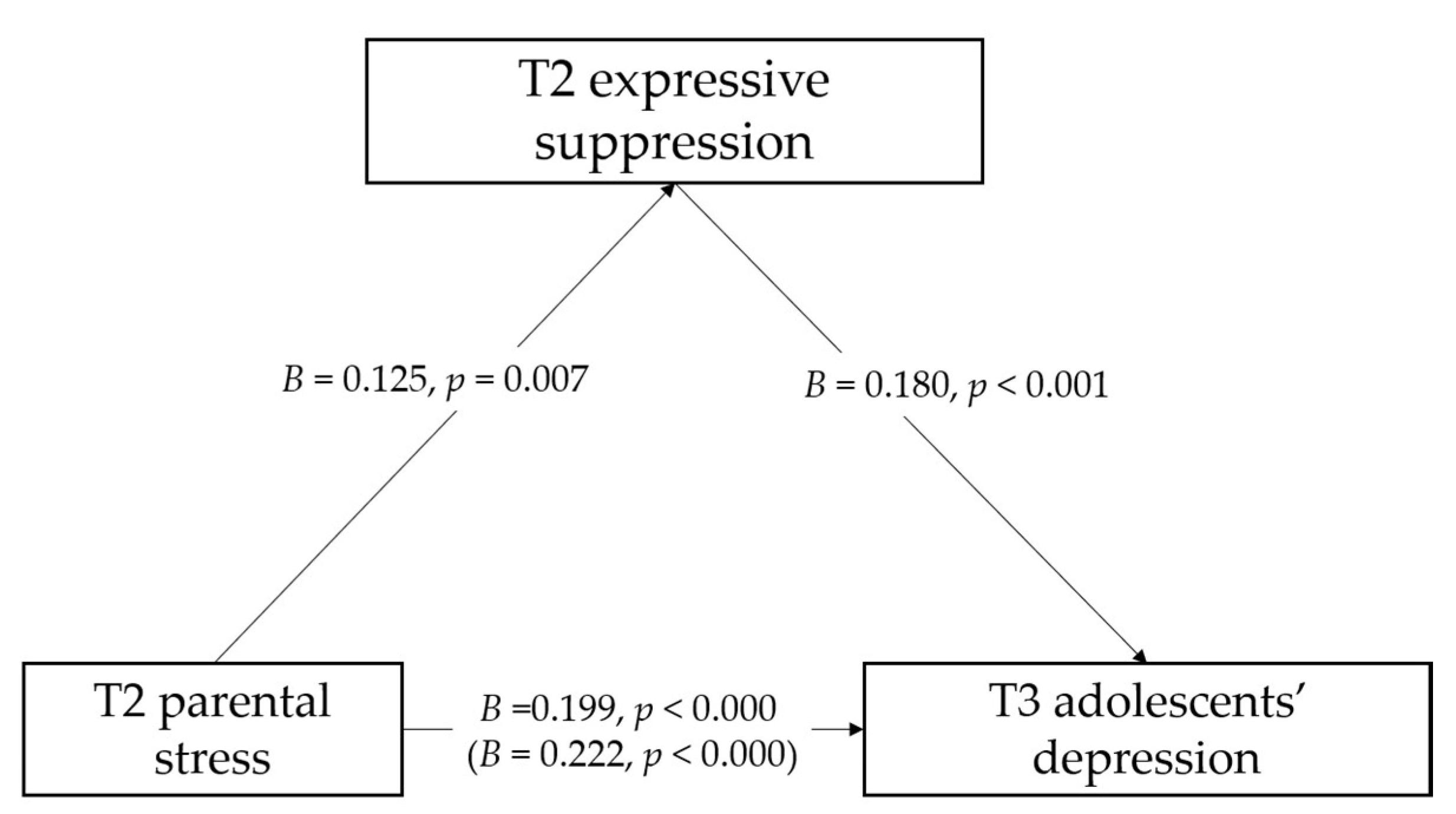
3.5. Mediation Analyses
3.6. Supplementary Analyses
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Orgilés, M.; Morales, A.; Delvecchio, E.; Mazzeschi, C.; Espada, J.P. Immediate psychological effects of the COVID-19 quarantine in youth from Italy and Spain. Front. Psychol. 2020, 11, 579038. [Google Scholar] [CrossRef]
- Brooks, S.K.; Webster, R.K.; Smith, L.E.; Woodland, L.; Wessely, S.; Greenberg, N.; Rubin, G.J. The psychological impact of quarantine and how to reduce it: Rapid review of the evidence. Lancet 2020, 395, 912–920. [Google Scholar] [CrossRef] [Green Version]
- Guessoum, S.B.; Lachal, J.; Radjack, R.; Carretier, E.; Minassian, S.; Benoit, L.; Moro, M.R. Adolescent psychiatric disorders during the COVID-19 pandemic and lockdown. Psychiatry Res. 2020, 291, 113264. [Google Scholar] [CrossRef]
- Li, Y.; Duan, W.; Chen, Z. Latent profiles of the comorbidity of the symptoms for posttraumatic stress disorder and generalized anxiety disorder among children and adolescents who are susceptible to COVID-19. Child. Youth Serv. Rev. 2020, 116, 105235. [Google Scholar] [CrossRef]
- News, U.N. Guterres Calls for ‘Paradigm Shift’ to Recover from COVID Setbacks. Available online: https://news.un.org/en/story/2021/04/1089542 (accessed on 28 May 2021).
- Casey, B.J.; Jones, R.M.; Levita, L.; Libby, V.; Pattwell, S.S.; Ruberry, E.J.; Soliman, F.; Somerville, L.H. The storm and stress of adolescence: Insights from human imaging and mouse genetics. Dev. Psychobiol. 2010, 52, 225–235. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Terranova, A.M.; Boxer, P.; Morris, A.S. Factors influencing the course of posttraumatic stress following a natural disaster: Children’s reactions to Hurricane Katrina. J. Appl. Dev. Psychol. 2009, 30, 344–355. [Google Scholar] [CrossRef]
- Jiao, W.; Wang, L.; Liu, J.; Fang, S.; Jiao, F.; Pettoello-Mantovani, M.; Somekh, E. Behavioral and emotional disorders in children during the COVID-19 epidemic. J. Pediatrics 2020, 221, 264–266. [Google Scholar] [CrossRef]
- Liang, Z.; Delvecchio, E.; Cheng, Y.; Mazzeschi, C. Parent and child’s negative emotions during COVID-19: The moderating role of parental attachment style. Front. Psychol. 2021, 12, 567483. [Google Scholar] [CrossRef] [PubMed]
- Li, H.Y.; Cao, H.; Leung, D.Y.P.; Mak, Y.W. The psychological impacts of a COVID-19 outbreak on college students in China: A longitudinal study. Int. J. Environ. Res. Public Health 2020, 17, 3933. [Google Scholar] [CrossRef]
- De France, K.; Hancock, G.R.; Stack, D.M.; Serbin, L.A.; Hollenstein, T. The mental health implications of COVID-19 for adolescents: Follow-up of a four-wave longitudinal study during the pandemic. Am. Psychol. 2021. [Google Scholar] [CrossRef]
- Fruehwirth, J.C.; Biswas, S.; Perreira, K.M. The Covid-19 pandemic and mental health of first-year college students: Examining the effect of Covid-19 stressors using longitudinal data. PLoS ONE 2021, 16, e0247999. [Google Scholar] [CrossRef]
- Magson, N.R.; Freeman, J.Y.A.; Rapee, R.M.; Richardson, C.E.; Oar, E.L.; Fardouly, J. Risk and protective factors for prospective changes in adolescent mental health during the COVID-19 pandemic. J. Youth Adolesc. 2021, 50, 44–57. [Google Scholar] [CrossRef]
- Wang, C.; Pan, R.; Wan, X.; Tan, Y.; Xu, L.; McIntyre, R.S.; Choo, F.N.; Tran, B.; Ho, R.; Sharma, V.K.; et al. A longitudinal study on the mental health of general population during the COVID-19 epidemic in China. Brain Behav. Immun. 2020, 87, 40–48. [Google Scholar] [CrossRef]
- Fernández-Abascal, E.G.; Martín-Díaz, M.D. Longitudinal study on affect, psychological well-being, depression, mental and physical health, prior to and during the COVID-19 pandemic in Spain. Personal. Individ. Differ. 2021, 172, 110591. [Google Scholar] [CrossRef] [PubMed]
- Rapee, R.M.; Oar, E.L.; Johnco, C.J.; Forbes, M.K.; Fardouly, J.; Magson, N.R.; Richardson, C.E. Adolescent development and risk for the onset of social-emotional disorders: A review and conceptual model. Behav. Res. Ther. 2019, 123, 103501. [Google Scholar] [CrossRef] [PubMed]
- Cohen, S.; Kamarck, T.; Mermelstein, R. A global measure of perceived stress. J. Health Soc. Behav. 1983, 24, 385–396. [Google Scholar] [CrossRef]
- Mondo, M.; Sechi, C.; Cabras, C. Psychometric evaluation of three versions of the Italian Perceived Stress Scale. Curr. Psychol. 2021, 40, 1884–1892. [Google Scholar] [CrossRef]
- Restubog, S.L.D.; Ocampo, A.C.G.; Wang, L. Taking control amidst the chaos: Emotion regulation during the COVID-19 pandemic. J. Vocat. Behav. 2020, 119, 103440. [Google Scholar] [CrossRef]
- Di Giorgio, E.; Di Riso, D.; Mioni, G.; Cellini, N. The interplay between mothers’ and children behavioral and psychological factors during COVID-19: An Italian study. Eur. Child Adolesc. Psychiatry 2020, 1–12. [Google Scholar] [CrossRef]
- Pfefferbaum, B.; North, C.S. Mental health and the Covid-19 pandemic. N. Engl. J. Med. 2020, 383, 510–512. [Google Scholar] [CrossRef] [PubMed]
- Platt, R.; Williams, S.R.; Ginsburg, G.S. Stressful life events and child anxiety: Examining parent and child mediators. Child Psychiatry Hum. Dev. 2016, 47, 23–34. [Google Scholar] [CrossRef] [Green Version]
- Ellis, W.E.; Dumas, T.M.; Forbes, L.M. Physically isolated but socially connected: Psychological adjustment and stress among adolescents during the initial COVID-19 crisis. Can. J. Behav. Sci. 2020, 52, 177–187. [Google Scholar] [CrossRef]
- Holmes, E.A.; O’Connor, R.C.; Perry, V.H.; Tracey, I.; Wessely, S.; Arseneault, L.; Ballard, C.; Christensen, H.; Cohen Silver, R.; Everall, I.; et al. Multidisciplinary research priorities for the COVID-19 pandemic: A call for action for mental health science. Lancet Psychiatry 2020, 7, 547–560. [Google Scholar] [CrossRef]
- Brown, S.M.; Doom, J.R.; Lechuga-Peña, S.; Watamura, S.E.; Koppels, T. Stress and parenting during the global COVID-19 pandemic. Child Abus. Negl. 2020, 110, 104699. [Google Scholar] [CrossRef]
- Tang, S.; Xiang, M.; Cheung, T.; Xiang, Y.-T. Mental health and its correlates among children and adolescents during COVID-19 school closure: The importance of parent-child discussion. J. Affect. Disord. 2021, 279, 353–360. [Google Scholar] [CrossRef] [PubMed]
- Pfefferbaum, B.; Jacobs, A.K.; Houston, J.B.; Griffin, N. Children’s disaster reactions: The influence of family and social factors. Curr. Psychiatry Rep. 2015, 17, 57. [Google Scholar] [CrossRef]
- Cobham, V.E.; McDermott, B.; Haslam, D.; Sanders, M.R. The role of parents, parenting and the family environment in children’s post-disaster mental health. Curr. Psychiatry Rep. 2016, 18, 53. [Google Scholar] [CrossRef] [PubMed]
- Crescentini, C.; Feruglio, S.; Matiz, A.; Paschetto, A.; Vidal, E.; Cogo, P.; Fabbro, F. Stuck outside and inside: An exploratory study on the effects of the COVID-19 outbreak on Italian parents and children’s internalizing symptoms. Front. Psychol. 2020, 11, 586074. [Google Scholar] [CrossRef] [PubMed]
- Lorenzo, N.E.; Zeytinoglu, S.; Morales, S.; Listokin, J.; Almas, A.N.; Degnan, K.A.; Henderson, H.; Chronis-Tuscano, A.; Fox, N.A. Transactional associations between parent and late adolescent internalizing symptoms during the COVID-19 pandemic: The moderating role of avoidant coping. J. Youth Adolesc. 2021, 50, 459–469. [Google Scholar] [CrossRef]
- Orgilés, M.; Espada, J.P.; Delvecchio, E.; Francisco, R.; Mazzeschi, C.; Pedro, M.; Morales, A. Anxiety and depressive symptoms in children and adolescents during covid-19 pandemic: A transcultural approach. Psicothema 2021, 33, 125–130. [Google Scholar] [CrossRef]
- Spinelli, M.; Lionetti, F.; Pastore, M.; Fasolo, M. Parents’ stress and children’s psychological problems in families facing the COVID-19 outbreak in Italy. Front. Psychol. 2020, 11, 1713. [Google Scholar] [CrossRef]
- Luu, T.T. Worker resilience during the COVID-19 crisis: The role of core beliefs challenge, emotion regulation, and family strain. Personal. Individ. Differ. 2021, 179, 110784. [Google Scholar] [CrossRef]
- Gross, J.J.; John, O.P. Individual differences in two emotion regulation processes: Implications for affect, relationships, and well-being. J. Personal. Soc. Psychol. 2003, 85, 348–362. [Google Scholar] [CrossRef]
- Gross, J.J. Emotion regulation: Current status and future prospects. Psychol. Inq. 2015, 26, 1–26. [Google Scholar] [CrossRef]
- Balan, R.; Dobrean, A.; Roman, G.D.; Balazsi, R. Indirect effects of parenting practices on internalizing problems among adolescents: The role of expressive suppression. J. Child Fam. Stud. 2017, 26, 40–47. [Google Scholar] [CrossRef]
- Gross, J.T.; Cassidy, J. Expressive suppression of negative emotions in children and adolescents: Theory, data, and a guide for future research. Dev. Psychol. 2019, 55, 1938–1950. [Google Scholar] [CrossRef]
- Trougakos, J.P.; Chawla, N.; McCarthy, J.M. Working in a pandemic: Exploring the impact of COVID-19 health anxiety on work, family, and health outcomes. J. Appl. Psychol. 2020, 105, 1234–1245. [Google Scholar] [CrossRef]
- Too, L.S.; Butterworth, P. Psychosocial job stressors and mental health: The potential moderating role of emotion regulation. J. Occup. Environ. Med. 2018, 60, e518–e524. [Google Scholar] [CrossRef]
- Moore, S.A.; Zoellner, L.A.; Mollenholt, N. Are expressive suppression and cognitive reappraisal associated with stress-related symptoms? Behav. Res. Ther. 2008, 46, 993–1000. [Google Scholar] [CrossRef] [Green Version]
- Yeung, D.Y.; Wong, S. Effects of cognitive reappraisal and expressive suppression on daily work-related outcomes: Comparison between younger and older Chinese workers. Int. J. Psychol. 2020, 55, 983–994. [Google Scholar] [CrossRef] [PubMed]
- Jiang, H.-J.; Nan, J.; Lv, Z.-Y.; Yang, J. Psychological impacts of the COVID-19 epidemic on Chinese people: Exposure, post-traumatic stress symptom, and emotion regulation. Asian Pac. J. Trop. Med. 2020, 13, 252–259. [Google Scholar] [CrossRef]
- Morris, A.S.; Silk, J.S.; Steinberg, L.; Myers, S.S.; Robinson, L.R. The role of the family context in the development of emotion regulation. Soc. Dev. 2007, 16, 361–388. [Google Scholar] [CrossRef] [Green Version]
- Eisenberg, N. Findings, issues, and new directions for research on emotion socialization. Dev. Psychol. 2020, 56, 664–670. [Google Scholar] [CrossRef] [PubMed]
- Eastabrook, J.M.; Flynn, J.J.; Hollenstein, T. Internalizing symptoms in female adolescents: Associations with emotional awareness and emotion regulation. J. Child Fam. Stud. 2014, 23, 487–496. [Google Scholar] [CrossRef]
- Cai, R.Y.; Richdale, A.L.; Foley, K.-R.; Trollor, J.; Uljarević, M. Brief report: Cross-sectional interactions between expressive suppression and cognitive reappraisal and its relationship with depressive symptoms in autism spectrum disorder. Res. Autism Spectr. Disord. 2018, 45, 1–8. [Google Scholar] [CrossRef]
- Rogers, M.L.; Halberstadt, A.G.; Castro, V.L.; MacCormack, J.K.; Garrett-Peters, P. Maternal emotion socialization differentially predicts third-grade children’s emotion regulation and lability. Emotion 2016, 16, 280–291. [Google Scholar] [CrossRef]
- Perry, N.B.; Dollar, J.M.; Calkins, S.D.; Keane, S.P.; Shanahan, L. Maternal socialization of child emotion and adolescent adjustment: Indirect effects through emotion regulation. Dev. Psychol. 2020, 56, 541–552. [Google Scholar] [CrossRef]
- Stein, A.; Lehtonen, A.; Harvey, A.G.; Nicol-Harper, R.; Craske, M. The influence of postnatal psychiatric disorder on child development. Psychopathology 2009, 42, 11–21. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Spinelli, M.; Lionetti, F.; Setti, A.; Fasolo, M. Parenting stress during the COVID-19 outbreak: Socioeconomic and environmental risk factors and implications for children emotion regulation. Fam. Process. 2021, 60, 639–653. [Google Scholar] [CrossRef] [PubMed]
- Achterberg, M.; Dobbelaar, S.; Boer, O.D.; Crone, E.A. Perceived stress as mediator for longitudinal effects of the COVID-19 lockdown on wellbeing of parents and children. Sci. Rep. 2021, 11, 2971. [Google Scholar] [CrossRef]
- Hollingshead, A.B. Four Factor Index of Social Status; Yale University: New Haven, CT, USA, 1975. [Google Scholar]
- Francisco, R.; Pedro, M.; Delvecchio, E.; Espada, J.P.; Morales, A.; Mazzeschi, C.; Orgilés, M. Psychological symptoms and behavioral changes in children and adolescents during the early phase of COVID-19 quarantine in three European countries. Front. Psychiatry 2020, 11, 570164. [Google Scholar] [CrossRef]
- Liang, Z.; Delvecchio, E.; Buratta, L.; Mazzeschi, C. “Ripple effect”: Psychological responses and coping strategies of Italian children in different COVID-19 severity areas. Rev. De Psicol. Clínica Con Niños Y Adolesc. 2020, 7, 49–58. [Google Scholar] [CrossRef]
- Balzarotti, S.; John, O.P.; Gross, J.J. An Italian adaptation of the Emotion Regulation Questionnaire. Eur. J. Psychol. Assess. 2010, 26, 61–67. [Google Scholar] [CrossRef]
- Reardon, T.; Spence, S.H.; Hesse, J.; Shakir, A.; Creswell, C. Identifying children with anxiety disorders using brief versions of the Spence Children’s Anxiety Scale for children, parents, and teachers. Psychol. Assess. 2018, 30, 1342–1355. [Google Scholar] [CrossRef] [PubMed]
- Ancold, A.; Costello, E.J.; Messer, S.C.; Pickles, A. Development of a short questionnaire for use in epidemiological studies of depression in children and adolescents. Int. J. Methods Psychiatr. Res. 1995, 5, 237–249. [Google Scholar]
- Beasley, T.M.; Schumacker, R.E. Multiple regression approach to analyzing contingency tables: Post hoc and planned comparison procedures. J. Exp. Educ. 1995, 64, 79–93. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences, 2nd ed.; Lawrence Earlbam Associates: Hillsdale, NJ, USA, 1988. [Google Scholar]
- Hayes, A.F. PROCESS: A Versatile Computational Tool for Observed Variable Mediation, Moderation, and Conditional Process Modeling; University of Kansas: Lawrence, KS, USA, 2012. [Google Scholar]
- Hayes, A.F. Beyond Baron and Kenny: Statistical mediation analysis in the new millennium. Commun. Monogr. 2009, 76, 408–420. [Google Scholar] [CrossRef]
- Turner, N.; Joinson, C.; Peters, T.J.; Wiles, N.; Lewis, G. Validity of the Short Mood and Feelings Questionnaire in late adolescence. Psychol. Assess. 2014, 26, 752–762. [Google Scholar] [CrossRef]
- Ellis, W.E.; Zarbatany, L. Understanding processes of peer clique influence in late childhood and early adolescence. Child Dev. Perspect. 2017, 11, 227–232. [Google Scholar] [CrossRef]
- De Figueiredo, C.S.; Sandre, P.C.; Portugal, L.C.L.; Mázala-de-Oliveira, T.; da Silva Chagas, L.; Raony, Í.; Ferreira, E.S.; Giestal-de-Araujo, E.; dos Santos, A.A.; Bomfim, P.O.-S. COVID-19 pandemic impact on children and adolescents’ mental health: Biological, environmental, and social factors. Prog. Neuro. Psychopharmacol. Biol. Psychiatry 2021, 106, 110171. [Google Scholar] [CrossRef]
- Groarke, J.M.; McGlinchey, E.; McKenna-Plumley, P.E.; Berry, E.; Graham-Wisener, L.; Armour, C. Examining temporal interactions between loneliness and depressive symptoms and the mediating role of emotion regulation difficulties among UK residents during the COVID-19 lockdown: Longitudinal results from the COVID-19 psychological wellbeing study. J. Affect. Disord. 2021, 285, 1–9. [Google Scholar] [CrossRef]
- Dvorsky, M.R.; Breaux, R.; Becker, S.P. Finding ordinary magic in extraordinary times: Child and adolescent resilience during the COVID-19 pandemic. Eur. Child Adolesc. Psychiatry 2020, 10.1007/s00787-020-01583-8. [Google Scholar] [CrossRef]
- Hawes, M.T.; Szenczy, A.K.; Olino, T.M.; Nelson, B.D.; Klein, D.N. Trajectories of depression, anxiety and pandemic experiences; A longitudinal study of youth in New York during the Spring-Summer of 2020. Psychiatry Res. 2021, 298, 113778. [Google Scholar] [CrossRef] [PubMed]
- Bartlett, J.D.; Griffin, J.; Thomson, D. Resources for Supporting Children’s Emotional Well-being during the COVID-19 Pandemic. Child Trends. 2020. Available online: https://www.childtrends.org/publications/resources-for-supporting-childrens-emotional-well-being-during-the-covid-19-pandemic (accessed on 28 May 2021).
- Shockley, K.M.; Clark, M.A.; Dodd, H.; King, E.B. Work-family strategies during COVID-19: Examining gender dynamics among dual-earner couples with young children. J. Appl. Psychol. 2021, 106, 15–28. [Google Scholar] [CrossRef]
- Liu, J.J.; Bao, Y.; Huang, X.; Shi, J.; Lu, L. Mental health considerations for children quarantined because of COVID-19. Lancet Child Adolesc. Health 2020, 4, 347–349. [Google Scholar] [CrossRef] [Green Version]
- Saxena, R.; Saxena, S.K. Preparing Children for Pandemics. In Coronavirus Disease 2019 (COVID-19): Epidemiology, Pathogenesis, Diagnosis, and Therapeutics; Saxena, S.K., Ed.; Springer: Singapore, 2020; pp. 187–198. [Google Scholar] [CrossRef]
- Bariola, E.; Gullone, E.; Hughes, E.K. Child and adolescent emotion regulation: The role of parental emotion regulation and expression. Clin. Child Fam. Psychol. Rev. 2011, 14, 198–212. [Google Scholar] [CrossRef]
- Sai, L.; Luo, S.; Ward, A.; Sang, B. Development of the tendency to use emotion regulation strategies and their relation to depressive symptoms in Chinese adolescents. Front. Psychol. 2016, 7, 1222. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Pat-Horenczyk, R.; Cohen, S.; Ziv, Y.; Achituv, M.; Asulin-Peretz, L.; Blanchard, T.R.; Schiff, M.; Brom, D. Emotion regulation in mothers and young children faced with trauma. Infant Ment. Health J. 2015, 36, 337–348. [Google Scholar] [CrossRef] [PubMed]
- Shorer, M.; Leibovich, L. Young children’s emotional stress reactions during the COVID-19 outbreak and their associations with parental emotion regulation and parental playfulness. Early Child Dev. Care 2020, 1–11. [Google Scholar] [CrossRef]
- Cutuli, D. Cognitive reappraisal and expressive suppression strategies role in the emotion regulation: An overview on their modulatory effects and neural correlates. Front. Syst. Neurosci. 2014, 8, 175. [Google Scholar] [CrossRef] [PubMed] [Green Version]

| Variables | Complete Group (n = 288) | Attrition Group (n = 763) | Test a | ||
|---|---|---|---|---|---|
| M | SD | M | SD | ||
| T1 adolescents’ anxiety to quarantine | 2.91 | 2.46 | 2.85 | 2.52 | 0.392 |
| T2 adolescents’ anxiety to quarantine | 3.31 | 2.44 | 2.90 | 2.30 | 1.797 |
| T1 adolescents’ depression to quarantine | 2.18 | 1.73 | 2.08 | 1.67 | 0.829 |
| T2 adolescents’ depression to quarantine | 2.57 | 1.71 | 2.59 | 1.67 | −0.090 |
| T2 parental stress | 19.02 | 7.18 | 18.78 | 7.64 | 0.339 |
| T2 expressive suppression | 13.17 | 5.11 | 12.73 | 4.44 | 0.919 |
| Parents’ age | 46.50 | 4.65 | 46.39 | 5.72 | 0.274 |
| Adolescent’s age | 13.89 | 2.15 | 14.22 | 2.29 | −2.114 * |
| N | % | N | % | ||
| Parents’ gender (female) | 275 | 95.5 | 653 | 85.6 | 19.842 *** |
| Monthly family income (euros) | 3.136 | ||||
| Up to 999 | 4 | 4.5 | 9 | 3.8 | |
| Between 1000 and 1999 | 18 | 20.2 | 65 | 27.1 | |
| Between 2000 and 3999 | 29 | 32.6 | 60 | 25.0 | |
| Between 3000 and 4999 | 27 | 30.3 | 81 | 33.8 | |
| 5000 or more | 11 | 12.4 | 25 | 10.4 | |
| Education level | 1.017 | ||||
| Primary school | 21 | 7.3 | 70 | 9.2 | |
| Secondary school | 133 | 46.2 | 339 | 44.5 | |
| Undergraduate | 94 | 32.6 | 245 | 32.2 | |
| Doctoral or master | 40 | 13.9 | 107 | 14.1 | |
| Mother’s current employment situation | 8.666 | ||||
| Self-employed | 40 | 13.9 | 92 | 12.2 | |
| Part-time | 73 | 25.3 | 178 | 23.5 | |
| Full-time | 59 | 20.5 | 200 | 26.5 | |
| Unemployed | 20 | 6.9 | 45 | 6.0 | |
| Lost job due to COVID-19 | 19 | 6.6 | 27 | 3.6 | |
| Home-working | 54 | 18.8 | 147 | 19.4 | |
| Other | 23 | 8.0 | 67 | 8.9 | |
| Father’s current employment situation | 8.706 | ||||
| Self-employed | 76 | 27.1 | 214 | 28.7 | |
| Part-time | 13 | 4.6 | 45 | 6.0 | |
| Full-time | 133 | 47.5 | 326 | 43.7 | |
| Unemployed | 8 | 2.9 | 25 | 3.4 | |
| Lost job due to COVID-19 | 8 | 2.9 | 16 | 2.1 | |
| Home-working | 42.0 | 15.0 | 103.0 | 13.8 | |
| Other | 0 | 0 | 17.0 | 2.3 | |
| Adolescents’ gender (female) | 130.0 | 45.1 | 386.0 | 50.6 | 2.486 |
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Parent age | – | |||||||||||
| 2. Adolescent age | 0.31 ** | – | ||||||||||
| 3. T1 adolescents’ anxiety to quarantine | 0.06 | −0.04 | – | |||||||||
| 4. T2 adolescents’ anxiety to quarantine | −0.01 | −0.02 | 0.57 ** | – | ||||||||
| 5. T3 adolescents’ anxiety to quarantine | −0.02 | −0.08 | 0.46 ** | 0.56 ** | – | |||||||
| 6. T1 adolescents’ depression to quarantine | 0.04 | −0.03 | 0.61 ** | 0.35 ** | 0.31 ** | – | ||||||
| 7. T2 adolescents’ depression to quarantine | 0.01 | −0.14 * | 0.40 ** | 0.54 ** | 0.34 ** | 0.49 ** | – | |||||
| 8. T3 adolescents’ depression to quarantine | −0.04 | −0.15 * | 0.40 ** | 0.50 ** | 0.62 ** | 0.39 ** | 0.58 ** | – | ||||
| 9. T2 parental stress | −0.07 | −0.05 | 0.27 ** | 0.27 ** | 0.25 ** | 0.19 ** | 0.22 ** | 0.20 ** | – | |||
| 10. T2 expressive suppression | 0.06 | −0.01 | 0.13 * | 0.15 * | 0.18 ** | 0.09 | 0.05 | 0.17 ** | 0.17 ** | – | ||
| 11. T3 adolescents’ anxiety | −0.04 | −0.19 ** | 0.38 ** | 0.28 ** | 0.42 ** | 0.31 *** | 0.20 ** | 0.35 ** | 0.35 ** | 0.23 ** | – | |
| 12. T3 adolescents’ depression | −0.01 | −0.13 * | 0.34 ** | 0.36 ** | 0.51 ** | 0.33 ** | 0.40 ** | 0.60 ** | 0.41 ** | 0.27 ** | 0.67 ** | – |
| M | 46.50 | 13.89 | 2.91 | 3.31 | 2.93 | 2.18 | 2.57 | 2.36 | 19.02 | 13.17 | 6.26 | 5.94 |
| SD | 4.65 | 2.15 | 2.47 | 2.44 | 230 | 1.73 | 1.70 | 1.73 | 7.18 | 5.11 | 3.92 | 5.16 |
| Paths | B | SE | p |
|---|---|---|---|
| DV: T3 Adolescents’ Anxiety (R2 = 0.283) | |||
| T2 parental stress → T3 adolescents’ anxiety | 0.140 | 0.031 | <0.000 |
| T1 adolescents’ anxiety to quarantine → T3 adolescents’ anxiety | 0.365 | 0.120 | 0.003 |
| T2 adolescents’ anxiety to quarantine → T3 adolescents’ anxiety | 0.115 | 0.111 | 0.303 |
| T1 adolescents’ depression to quarantine → T3 adolescents’ anxiety | 0.221 | 0.161 | 0.171 |
| T2 adolescents’ depression to quarantine → T3 adolescents’ anxiety | −0.114 | 0.156 | 0.465 |
| adolescent’s age → T3 adolescents’ anxiety | −0.311 | 0.097 | 0.002 |
| parents’ gender → T3 adolescents’ anxiety | 1.152 | 0.991 | 0.246 |
| mother’s current employment status → T3 adolescents’ anxiety | −0.051 | 0.106 | 0.630 |
| father’s current employment status → T3 adolescents’ anxiety | 0.153 | 0.128 | 0.233 |
| DV: T3 adolescents’ depression (R2 = 0.332) | |||
| T2 parental stress → T3 adolescents’ depression | 0.222 | 0.039 | <0.000 |
| T1 adolescents’ anxiety to quarantine → T3 adolescents’ depression | 0.117 | 0.148 | 0.432 |
| T2 adolescents’ anxiety to quarantine → T3 adolescents’ depression | 0.245 | 0.140 | 0.082 |
| T1 adolescents’ depression to quarantine → T3 adolescents’ depression | 0.336 | 0.201 | 0.096 |
| T2 adolescents’ depression to quarantine → T3 adolescents’ depression | 0.472 | 0.195 | 0.016 |
| adolescent’s age → T3 adolescents’ depression | −0.223 | 0.122 | 0.069 |
| parents’ gender → T3 adolescents’ depression | −0.185 | 1.273 | 0.885 |
| parents’ education level → T3 adolescents’ depression | −0.933 | 0.321 | 0.004 |
| mother’s current employment status → T3 adolescents’ depression | −0.081 | 0.132 | 0.540 |
| Paths | Direct Effects | Indirect Effects | ||||
|---|---|---|---|---|---|---|
| B | SE | p | B | SE | 95% Bootstrapping CI | |
| DV: T3 Adolescents’ Anxiety | ||||||
| T2 parental stress →T2 expressive suppression | 0.127 | 0.046 | 0.007 | |||
| T2 parental stress →T3 adolescents’ anxiety | 0.129 | 0.031 | <0.000 | |||
| T2 expressive suppression → T3 adolescents’ anxiety | 0.087 | 0.041 | 0.034 | |||
| T2 parental stress→ T2 expressive suppression →T3 adolescents’ anxiety | 0.011 | 0.007 | [0.001, 0.032] | |||
| DV: T3 Adolescents’ Depression | ||||||
| T2 parental stress →T2 expressive suppression | 0.125 | 0.046 | 0.007 | |||
| T2 parental stress → T3 adolescents’ depression | 0.199 | 0.038 | <0.000 | |||
| T2 expressive suppression → T3 adolescents’ depression | 0.180 | 0.050 | <0.001 | |||
| T2 parental stress→ T2 expressive suppression →T3 adolescents’ depression | 0.023 | 0.011 | [0.006, 0.050] | |||
| Model Fit Indices | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| AIC | BIC | χ2 | df | CFI | TLI | RMSEA | 90%CI | SRMR | |
| Hypothesized model for depression symptoms | 3343.42 | 3390.82 | 9.01 | 8 | 0.992 | 0.981 | 0.021 | [0.000, 0.075] | 0.023 |
| Competing model for depression symptoms (switch X and M) | 3534.66 | 3582.05 | 51.47 | 8 | 0.743 | 0.390 | 0.139 | [0.104, 0.176] | 0.070 |
| Hypothesized model for anxiety symptoms | 3122.18 | 3169.20 | 9.66 | 8 | 0.983 | 0.959 | 0.027 | [0.000, 0.079] | 0.026 |
| Competing model for anxiety symptoms (switch X and M) | 3311.49 | 3358.51 | 51.24 | 8 | 0.687 | 0.257 | 0.140 | [0.105, 0.178] | 0.070 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liang, Z.; Mazzeschi, C.; Delvecchio, E. The Impact of Parental Stress on Italian Adolescents’ Internalizing Symptoms during the COVID-19 Pandemic: A Longitudinal Study. Int. J. Environ. Res. Public Health 2021, 18, 8074. https://doi.org/10.3390/ijerph18158074
Liang Z, Mazzeschi C, Delvecchio E. The Impact of Parental Stress on Italian Adolescents’ Internalizing Symptoms during the COVID-19 Pandemic: A Longitudinal Study. International Journal of Environmental Research and Public Health. 2021; 18(15):8074. https://doi.org/10.3390/ijerph18158074
Chicago/Turabian StyleLiang, Ziqin, Claudia Mazzeschi, and Elisa Delvecchio. 2021. "The Impact of Parental Stress on Italian Adolescents’ Internalizing Symptoms during the COVID-19 Pandemic: A Longitudinal Study" International Journal of Environmental Research and Public Health 18, no. 15: 8074. https://doi.org/10.3390/ijerph18158074
APA StyleLiang, Z., Mazzeschi, C., & Delvecchio, E. (2021). The Impact of Parental Stress on Italian Adolescents’ Internalizing Symptoms during the COVID-19 Pandemic: A Longitudinal Study. International Journal of Environmental Research and Public Health, 18(15), 8074. https://doi.org/10.3390/ijerph18158074






