Psychosocial and Diet-Related Lifestyle Clusters in Overweight and Obesity
Abstract
1. Introduction
2. Materials and Methods
2.1. Participants and Procedure
2.2. Study Variables and Measures
2.3. Statistical Analyses
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Perdue, T.O.; Schreier, A.; Swans, M.; Neil, J.; Carels, R. Evolving self view and body image concerns in female postoperative bariatric surgery patients. J. Clin. Nurs. 2018, 27, 4018–4027. [Google Scholar] [CrossRef]
- Gagnon-Girouard, M.P.; Bégin, C.; Provencher, V.; Tremblay, A.; Boivin, S.; Lemieux, S. Subtyping weight-preoccupied overweight/obese women along restraint and negative affect. Appetite 2010, 55, 742–745. [Google Scholar] [CrossRef] [PubMed]
- Green, M.A.; Strong, M.; Razak, F.; Subramanian, S.V.; Relton, C.; Bissell, P. Who are the obese? A cluster analysis exploring subgroups of the obese. J. Public Health 2015, 38, 258–264. [Google Scholar] [CrossRef]
- Olson, R.; Thompson, S.V.; Wipfli, B.; Hanson, G.; Elliot, D.L.; Anger, W.K.; Bodner, T.; Hammer, L.B.; Hohn, E.; Perrin, N.A. Sleep, dietary, and exercise behavioral clusters among truck drivers with obesity: Implications for interventions. J. Occup. Environ. Med. 2016, 58, 314–321. [Google Scholar] [CrossRef] [PubMed]
- Claes, L.; Vandereycken, W.; Vandeputte, A.; Braet, C. Personality subtypes in female pre-bariatric obese patients: Do they differ in eating disorder symptoms, psychological complaints and coping behaviour? Eur. Eat. Disord. Rev. 2013, 21, 72–77. [Google Scholar] [CrossRef]
- Gullo, S.; Lo Coco, G.; Salerno, L.; La Pietra, F.; Bruno, V. A study of personality subtypes in obese patients seeking treatment. Res. Psychother. Psychopathol. Process. Outcome 2013, 16, 85–92. [Google Scholar] [CrossRef][Green Version]
- Müller, A.; Claes, L.; Wilderjan, T.F.; de Zwaan, M. Temperament subtypes in treatment seeking obese individuals: A latent profile analysis. Eur. Eat. Disord. Rev. 2014, 22, 260–266. [Google Scholar] [CrossRef]
- Pérez Martínez, E.; Tirado, S.; Mateu, M.; van der Hofstad, C.J.; Rodríguez-Marín, J. Psychopathology in a sample of candidate patients for bariatric surgery. Int. J. Psychiatry Clin. Pract. 2013, 17, 197–205. [Google Scholar] [CrossRef]
- Claes, L.; Boekaerts, E.; Verschueren, M.; Boukaert, W.; Luyckx, K. Identity statuses in prebariatric patients with obesity: Associations with eating disorder symptoms, psychological complaints, and coping behaviour? Eur. Eat. Disord. Rev. 2019, 27, 410–420. [Google Scholar] [CrossRef]
- Jansen, A.; Havermans, R.; Nederkoor, C.; Roefs, A. Jolly fat or sad fat? Subtyping non-eating disordered overweight and obesity along an affect dimension. Appetite 2008, 51, 635–640. [Google Scholar] [CrossRef]
- Caroleo, M.; Primerano, A.; Rania, M.; Aloi, M.; Pugliese, V.; Magliocco, F.; Filippo, A.; Sinopoli, F.; Ricchio, M.; Segura-Garcia, C. A real world study on the genetic, cognitive and psychopathological differences of obese patients clustered according to eating behaviours. Eur. Psychiatry 2018, 48, 58–64. [Google Scholar] [CrossRef]
- Calugi, S.; Grave, R. Psychological features in obesity: A network analysis. Int. J. Eat. Disord. 2020, 53, 248–255. [Google Scholar] [CrossRef] [PubMed]
- Godoy-Izquierdo, D.; González-Hernández, J.; Rodríguez-Tadeo, A.; Lara, R.; Ogallar, A.; Navarrón, E.; Ramírez, M.J.; López-Mora, C.; Arbinaga, F. Body satisfaction, weight stigma, positivity, and happiness among Spanish adults with overweight and obesity. Int. J. Environ. Res. Public Health 2020, 17, 4186. [Google Scholar] [CrossRef]
- Bibiloni, M.; Coll, J.; Pich, J.; Pons, A.; Tur, J. Body image satisfaction and weight concerns among a Mediterranean adult population. BMC Public Health 2017, 17, 39. [Google Scholar] [CrossRef] [PubMed]
- Chao, H. Body image change in obese and overweight persons enrolled in weight loss intervention programs: A systematic review and meta-analysis. PLoS ONE 2015, 10, e0124036. [Google Scholar] [CrossRef]
- Godoy-Izquierdo, D.; González, J.; Rodríguez, A.; Ramírez, M.; Navarrón, E.; Lara, R.; Jiménez, M. «Oberexia»: The desire to be fat (ter) in adults with excess weight. Cuad. De Psicol. Del Deporte 2019, 19, 186–197. [Google Scholar] [CrossRef][Green Version]
- Godoy-Izquierdo, D.; Gonzalez, J.; Lara, R.; Rodríguez-Tadeo, A.; Ramirez, M.J.; Navarrón, E.; Ogallar-Blanco, A.; López-Mora, C.; Arbinaga, F.; Arbinaga, F. Considering BMI, body image and desired weight change for suitable obesity management options. Span. J. Psychol. 2020, 23, e35. [Google Scholar] [CrossRef]
- Ibáñez-Zamacona, M.; Poveda, A.; Rebato, E. Body image in relation to nutritional status in adults from the Basque Country, Spain. J. Biosoc. Sci. 2020, 52, 272–285. [Google Scholar] [CrossRef] [PubMed]
- Latner, J.; Wilson, R. Obesity and body image in adulthood. In Body Image: A Handbook of Science, Practice, and Prevention; Cash, T., Smolak, L., Eds.; Guilford Press: New York, NY, USA, 2011; pp. 189–197. [Google Scholar]
- Silva, D.; Ferriani, L.; Viana, M. Depression, anthropometric parameters, and body image in adults: A systematic review. Rev. Da Assoc. Médica Bras. 2019, 65, 731–738. [Google Scholar] [CrossRef]
- Varela, C.; Montecinos, C.; García, C. Estudio transcultural de los diferentes componentes de la insatisfacción corporal en muestras comunitarias de España y Chile. Nutr. Hosp. 2019, 36, 691–697. [Google Scholar] [CrossRef] [PubMed]
- Weinberger, N.; Kersting, A.; Riedel-Heller, S.; Luck-Sikorski, C. Body dissatisfaction in individuals with obesity compared to normal-weight individuals: A systematic review and meta-analysis. Obes. Facts 2016, 9, 424–441. [Google Scholar] [CrossRef] [PubMed]
- Magallares, A.; Bolaños-Rios, P.; Ruiz-Prieto, I.; de Valle, P.B.; Irles, J.A.; Jáuregui-Lobera, I. The mediational effect of weight self-stigma in the relationship between blatant and subtle discrimination and depression and anxiety. Span. J. Psychol. 2017, 20, 1–7. [Google Scholar] [CrossRef]
- Pearl, R.L.; Puhl, R.M. Weight bias internalization and health: A systematic review. Obes. Rev. 2018, 19, 1141–1163. [Google Scholar] [CrossRef]
- Rubino, F.; Puhl, R.M.; Cummings, D.E.; Eckel, R.H.; Ryan, D.H.; Mechanick, J.I.; Apovian, C.M. Joint international consensus statement for ending stigma of obesity. Nat. Med. 2020, 32127716. [Google Scholar] [CrossRef]
- Spahlholz, J.; Baer, N.; König, H.H.; Riedel-Heller, S.G.; Luck-Sikorski, C. Obesity and discrimination–a systematic review and meta-analysis of observational studies. Obes. Rev. 2016, 17, 43–55. [Google Scholar] [CrossRef]
- Wu, Y.K.; Berry, D.C. Impact of weight stigma on physiological and psychological health outcomes for overweight and obese adults: A systematic review. J. Adv. Nurs. 2018, 74, 1030–1042. [Google Scholar] [CrossRef]
- Blanchflower, D.G.; Oswald, A.J.; van Landeghem, B. Imitative Obesity and Relative Utility. Discussion Paper No. 4010; Institut zur Zukunft der Arbeit: Bonn, Germany, 2009. [Google Scholar]
- Böckerman, P.; Johansson, E.; Saarni, S.I.; Saarni, S.E. The negative association of obesity with subjective well-being: Is it all about health? J. Happiness Stud. 2014, 15, 857–867. [Google Scholar] [CrossRef]
- Godoy-Izquierdo, D.; Ogallar, A.; Lara, R.; Rodríguez-Tadeo, A.; Arbinaga, F. Association of a Mediterranean diet and fruit and vegetable consumption with subjective well-being among adults with overweight and obesity. Nutrients 2021, 13, 1342. [Google Scholar] [CrossRef]
- Katsaiti, M.S. Obesity and happiness. Appl. Econ. 2012, 44, 4101–4114. [Google Scholar] [CrossRef]
- Kuroki, M. Life satisfaction, overweightness and obesity. Int. J. Wellbeing 2016, 6, 93–110. [Google Scholar] [CrossRef]
- Latif, E. Obesity and happiness: Does gender matter? Econ. Bus. Lett. 2014, 3, 59–67. [Google Scholar] [CrossRef]
- Magallares, A.; de Valle, P.B.; Irles, J.A.; Jauregui-Lobera, I. Overt and subtle discrimination, subjective well-being and physical health-related quality of life in an obese sample. Span. J. Psychol. 2014, 17, 1–8. [Google Scholar] [CrossRef]
- Magallares, A.; Morales, J.F.; Rubio, M.A. Group identification, discrimination and psychological health in an obese sample. Int. J. Psychol. Psychol. Ther. 2014, 14, 421–431. [Google Scholar]
- Oswald, A.; Powdthavee, N. Obesity, Unhappiness, and the Challenge of Affluence: Theory and Evidence. IZA Discussion Paper No. 2717. 2007. Available online: https://ssrn.com/abstract=981703 (accessed on 1 June 2018).
- Robertson, S.; Davies, M.; Winefield, H. Why weight for happiness? Correlates of BMI and SWB in Australia. Obes. Res. Clin. Pract. 2015, 9, 609–612. [Google Scholar] [CrossRef]
- Ul-Haq, Z.; Mackay, D.; Martin, D.; Smith, D.; Gill, J.; Nicholl, B.; Cullen, B.; Evans, J.; Roberts, B.; Deary, I.J.; et al. Heaviness, health and happiness: A cross-sectional study of 163066 UK Biobank participants. J. Epidemiol. Community Health 2014, 68, 340–348. [Google Scholar] [CrossRef] [PubMed]
- Wadsworth, T.; Pendergast, P.M. Obesity (sometimes) matters: The importance of context in the relationship between obesity and life satisfaction. J. Health Soc. Behav. 2014, 55, 196–214. [Google Scholar] [CrossRef] [PubMed]
- Caprara, G.; Eisenberg, N.; Alessandri, G. Positivity: The dispositional basis of happiness. J. Happiness Stud. 2017, 18, 353–371. [Google Scholar] [CrossRef]
- Caprara, G.; Alessandri, G.; Caprara, M. Associations of positive orientation with health and psychosocial adaptation: A review of findings and perspectives. Asian J. Soc. Psychol. 2019, 22, 126–132. [Google Scholar] [CrossRef]
- de Oliveira, M.C.; Anderson, C.A.; Dearborn, J.L.; Ferranti, E.P.; Mozaffarian, D.; Rao, G.; Wylie-Rosett, J.; Lichtenstein, A.H. Dietary diversity: Implications for obesity prevention in adult populations: A science advisory from the American Heart Association. Circulation 2018, 138, E160–E168. [Google Scholar] [CrossRef]
- Alissa, E.M.; Ferns, G.A. Dietary fruits and vegetables and cardiovascular diseases risk. Crit. Rev. Food Sci. Nutr. 2017, 57, 1950–1962. [Google Scholar] [CrossRef]
- Aune, D.; Giovannucci, E.; Boffetta, P.; Fadnes, L.T.; Keum, N.; Norat, T.; Greenwood, D.C.; Riboli, E.; Vatten, L.J.; Tonstad, S. Fruit and vegetable intake and the risk of cardiovascular disease, total cancer and all-cause mortality—A systematic review and dose-response meta-analysis of prospective studies. Int. J. Epidemiol. 2017, 46, 1029–1056. [Google Scholar] [CrossRef] [PubMed]
- Carlos, S.; La Fuente-Arrillaga, D.; Bes-Rastrollo, M.; Razquin, C.; Rico-Campà, A.; Martínez-González, M.A.; Ruiz-Canela, M. Mediterranean diet and health outcomes in the SUN cohort. Nutrients 2018, 10, 439. [Google Scholar] [CrossRef]
- Castro-Barquero, S.; Lamuela-Raventos, R.M.; Domenech, M.; Estruch, R. Relationship between Mediterranean dietary polyphenol intake and obesity. Nutrients 2018, 10, 1523. [Google Scholar] [CrossRef]
- Kwan, H.Y.; Chao, X.; Su, T.; Fu, X.; Tse, A.K.; Fong, W.F.; Fong, W.F. The anticancer and antiobesity effects of Mediterranean diet. Crit. Rev. Food Sci. Nutr. 2017, 57, 82–94. [Google Scholar] [CrossRef] [PubMed]
- Nour, M.; Lutze, S.A.; Grech, A.; Allman-Farinelli, M. The relationship between vegetable intake and weight outcomes: A systematic review of cohort studies. Nutrients 2018, 10, 1626. [Google Scholar] [CrossRef]
- Onvani, S.; Haghighatdoost, F.; Surkan, P.J.; Larijani, B.; Azadbakht, L. Adherence to the Healthy Eating Index and Alternative Healthy Eating Index dietary patterns and mortality from all causes, cardiovascular disease and cancer: A meta-analysis of observational studies. J. Hum. Nutr. Diet. 2017, 30, 216–226. [Google Scholar] [CrossRef]
- Schwingshackl, L.; Schwedhelm, C.; Hoffmann, G.; Lampousi, A.M.; Knüppel, S.; Iqbal, K.; Bechthold, A.; Schlesinger, S.; Boeing, H. Food groups and risk of all-cause mortality: A systematic review and meta-analysis of prospective studies. Am. J. Clin. Nutr. 2017, 105, 1462–1473. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Rodriguez, E.; Aparicio, A.; Aranceta-Bartrina, J.; Gil, A.; Gonzalez-Gross, M.; Serra-Majem, L.; Varela-Moreiras, G.; Ortega, R.M. Low adherence to dietary guidelines in Spain, especially in the overweight/obese population: The ANIBES Study. J. Am. Coll. Nutr. 2017, 36, 240–247. [Google Scholar] [CrossRef]
- Benhammou, S.; Heras-Gonzalez, L.; Ibanez-Peinado, D.; Barcelo, C.; Hamdan, M.; Rivas, A.; Mariscal-Arcas, M.; Olea-Serrano, F.; Monteagudo, C. Comparison of Mediterranean diet compliance between European and non-European populations in the Mediterranean basin. Appetite 2016, 107, 521–526. [Google Scholar] [CrossRef] [PubMed]
- Blas, A.; Garrido, A.; Unver, O.; Willaarts, B. A comparison of the Mediterranean diet and current food consumption patterns in Spain from a nutritional and water perspective. Sci. Total. Environ. 2019, 664, 1020–1029. [Google Scholar] [CrossRef]
- Gomez-Donoso, C.; Martinez-Gonzalez, M.A.; Martinez, J.A.; Sayon-Orea, C.; de la Fuente-Arrillaga, C.; Bes-Rastrollo, M. Adherence to dietary guidelines for the Spanish population and risk of overweight/obesity in the SUN cohort. PLoS ONE 2019, 14, e0226565. [Google Scholar] [CrossRef]
- Olmedo-Requena, R.; González-Donquiles, C.; Dávila-Batista, V.; Romaguera, D.; Castelló, A.; Molina de la Torre, A.J.; Martín, V. Agreement among Mediterranean diet pattern adherence indexes: MCC-Spain study. Nutrients 2019, 11, 488. [Google Scholar] [CrossRef] [PubMed]
- Lecube, A.; Sanchez, E.; Monereo, S.; Medina-Gomez, G.; Bellido, D.; Garcia-Almeida, J.M.; De Icaya, P.M.; Malagón, M.M.; Goday, A.; Tinahones, F.J.; et al. Factors accounting for obesity and its perception among the adult Spanish population: Data from 1000 computer-assisted telephone interviews. Obes. Facts 2020, 13, 322–332. [Google Scholar] [CrossRef] [PubMed]
- Hulley, S.B.; Cummings, S.R.; Browner, W.S.; Grady, D.; Newman, T.B. Designing Clinical Research: An Epidemiologic Approach, 4th ed.; Lippincott Williams Wilkins: Philadelphia, PA, USA, 2013; Appendix 6C; p. 79. [Google Scholar]
- Lecube, A.; Monereo, S.; Rubio, M.A.; Martínez-de-Icaya, P.; Martí, A.; Salvador, J.; Masmiquel, L.; Goday, A.; Bellido, D.; Lurbe, E.; et al. Prevención, Diagnóstico y Tratamiento de la Obesidad. Posicionamiento SEEDO 2016; Sociedad Española para el Estudio de la Obesidad: Madrid, Spain, 2016. [Google Scholar]
- World Health Organization. Global Action Plan. on Physical Activity 2018–2030: More Active People for a Healthier World; WHO: Geneva, Switzerland, 2019. [Google Scholar]
- Grogan, S. Body Image: Understanding Body Dissatisfaction in Men, Women, and Children, 3rd ed.; Routledge: New York, NY, USA, 2017. [Google Scholar]
- Gómez, S.; Baile, J. Propiedades psicométricas de una adaptación española de la escala de Interiorización de prejuicios sobre la obesidad (WBIS). Nutr. Hosp. 2015, 32, 1510–1515. [Google Scholar] [CrossRef]
- Durso, L.; Latner, J. Understanding self-directed stigma: Development of the Weight Bias Internalization Scale. Obesity 2008, 16, S80–S86. [Google Scholar] [CrossRef] [PubMed]
- Heikamp, T.; Alessandri, G.; Laguna, M.; Petrovic, V.; Caprara, M.; Trommsdorff, G. Cross-cultural validation of the Positivity Scale in five European countries. Pers. Individ. Differ. 2014, 71, 140–145. [Google Scholar] [CrossRef]
- Caprara, G.; Alessandri, G.; Eisenberg, N.; Kupfer, A.; Steca, P.; Caprara, M.; Trommsdorff, G.; Abela, J. The positivity Scale. Psychol. Assess. 2012, 24, 701–712. [Google Scholar] [CrossRef] [PubMed]
- Godoy-Izquierdo, D.; Lara, R.; Vázquez, M.; Araque, F.; Godoy, J. Correlates of happiness among older Spanish institutionalised and non-institutionalised adults. J. Happiness Stud. 2012, 14, 389–414. [Google Scholar] [CrossRef]
- Pavot, W. The cornerstone of research on subjective well-being: Valid assessment methodology. In Handbook of Well-Being; Diener, E., Oishi, S., Tay, L., Eds.; DEF Publishers: Salt Lake City, UT, USA, 2018. [Google Scholar]
- Diener, E.; Suh, E.; Lucas, R.; Smith, H. Subjective well-being: Three decades of progress. Psychol. Bull. 1999, 125, 276–302. [Google Scholar] [CrossRef]
- Schröder, H.; Fitó, M.; Estruch, R.; Martínez-González, M.A.; Corella, D.; Salas-Salvadó, J.; Lamuela-Raventós, R.; Ros, E.; Salaverría, I.; Fiol, M.; et al. A short screener is valid for assessing Mediterranean diet adherence among older Spanish men and women. J. Nutr. 2011, 141, 1140–1145. [Google Scholar] [CrossRef]
- Estruch, R.; Ros, E.; Salas-Salvadó, J.; Covas, M.I.; Corella, D.; Arós, F.; Gómez-Gracia, E.; Ruiz-Gutierrez, V.; Fiol, M.; Lapetra, J.; et al. PREDIMED Study Investigators. Primary prevention of cardiovascular disease with a Mediterranean Diet supplemented with extra-virgin olive oil or nuts. N. Engl. J. Med. 2018, 378, e34. [Google Scholar] [CrossRef]
- García-Conesa, M.T.; Philippou, E.; Pafilas, C.; Massaro, M.; Quarta, S.; Andrade, V.; Jorge, R.; Chervenkov, M.; Ivanova, T.; Dimitrova, D.; et al. Exploring the validity of the 14-item Mediterranean diet adherence screener (MEDAS): A cross-national study in seven European countries around the Mediterranean region. Nutrients 2020, 12, 2960. [Google Scholar] [CrossRef]
- Hernandez-Ruiz, A.; García-Villanova, B.; Guerra-Hernández, E.; Amiano, P.; Azpiri, M.; Molina-Montes, E. Description of indexes based on the adherence to the Mediterranean dietary pattern: A review. Nutr. Hosp. 2015, 32, 1872–1884. [Google Scholar] [CrossRef] [PubMed]
- Galilea-Zabalza, I.; Buil-Cosiales, P.; Salas-Salvador, J.; Toledo, E.; Ortega-Azorín, C.; Díez-Espino, J.; Vázquez-Ruiz, Z.; Zomeño, M.D.; Vioque, J.; Martínez, J.A.; et al. Mediterranean diet and quality of life: Baseline cross-sectional analysis of the PREDIMED-PLUS trial. PLoS ONE 2018, 13, e0198974. [Google Scholar] [CrossRef] [PubMed]
- Martínez-González, M.A.; Gea, A.; Ruiz-Canela, M. The Mediterranean diet and cardiovascular health: A critical review. Circ. Res. 2019, 124, 779–798. [Google Scholar] [CrossRef] [PubMed]
- Davis, C.; Bryan, J.; Hodgson, J.; Murphy, K. Definition of the Mediterranean diet; a literature review. Nutrients 2015, 7, 9139–9153. [Google Scholar] [CrossRef]
- Martínez-González, M.A.; Hershey, M.S.; Zazpe, I.; Trichopoulou, A. Transferability of the Mediterranean diet to non-Mediterranean countries. What is and what is not the Mediterranean diet. Nutrients 2017, 9, 1226. [Google Scholar] [CrossRef]
- US Department of Agriculture; US Department of Health and Human Services. Dietary Guidelines for Americans, 2015–2020; US Government Printing Office: Washington, DC, USA, 2015.
- Wallace, T.C.; Bailey, R.L.; Blumberg, J.B.; Burton-Freeman, B.; Chen, C.O.; Crowe-White, K.M.; Drewnowski, A.; Hooshmand, S.; Johnson, E.; Lewis, R.; et al. Fruits, vegetables, and health: A comprehensive narrative, umbrella review of the science and recommendations for enhanced public policy to improve intake. Crit. Rev. Food Sci. Nutr. 2020, 60, 2174–2211. [Google Scholar] [CrossRef]
- Tylka, T.L.; Annunziato, R.A.; Burgard, D.; Daníelsdóttir, S.; Shuman, E.; Davis, C.; Calogero, R.M. The weight-inclusive versus weight-normative approach to health: Evaluating the evidence for prioritizing well-being over weight loss. J. Obes. 2014, 18, 983495. [Google Scholar] [CrossRef]
- World Health Organization. Obesidad y Sobrepeso [Obesity and Overweight]; WHO: Geneva, Switzerland, 2017. [Google Scholar]
- Gracia-Arnaiz, M.; Kraemer, F.B.; Demonte, F.C. Acting against obesity: A cross-cultural analysis of prevention models in Spain, Argentina and Brazil. Crit. Rev. Food Sci. Nutr. 2020, 1–12. [Google Scholar] [CrossRef]
- Taylor, M.M. The obesity epidemic: Individual accountability and the social determinants of health. In The Obesity Epidemic; Palgrave Pivot: Cham, Switzerland, 2018. [Google Scholar] [CrossRef]
- Grosso, G.; Galvano, F. Mediterranean diet adherence in children and adolescents in southern European countries. NFS J. 2016, 3, 13–19. [Google Scholar] [CrossRef]
- Hilpert, M.; Brockmeier, K.; Dordel, S.; Koch, B.; Weiß, V.; Ferrari, N.; Tokarski, W.; Graf, C. Sociocultural influence on obesity and lifestyle in children: A study of daily activities, leisure time behavior, motor skills, and weight status. Obes. Facts 2017, 10, 168–178. [Google Scholar] [CrossRef] [PubMed]
- Ponce-Blandón, J.A.; Pabón-Carrasco, M.; Romero-Castillo, R.; Romero-Martín, M.; Jiménez-Picón, N.; Lomas-Campos, M. Effects of advertising on food consumption preferences in children. Nutrients 2020, 12, 3337. [Google Scholar] [CrossRef]
- Leis, R.; Jurado-Castro, J.M.; Llorente-Cantarero, F.J.; Anguita-Ruiz, A.; Iris-Rupérez, A.; Bedoya-Carpente, J.J.; Vázquez-Cobela, R.; Aguilera, C.M.; Bueno, G.; Gil-Campos, M. Cluster analysis of physical activity patterns, and relationship with sedentary behavior and healthy lifestyles in prepubertal children: Genobox Cohort. Nutrients 2020, 12, 1288. [Google Scholar] [CrossRef] [PubMed]
- Medina, F.X.; Solé-Sedeno, J.M.; Bach-Faig, A.; Aguilar-Martínez, A. Obesity, Mediterranean diet, and public health: A vision of obesity in the Mediterranean context from a sociocultural perspective. Int. J. Environ. Res. Public Health 2021, 18, 3715. [Google Scholar] [CrossRef]
- Trainer, S.; Brewis, A.; Hruschka, D.; Williams, D. Translating obesity: Navigating the front lines of the “war on fat”. Am. J. Hum. Biol. 2015, 27, 61–68. [Google Scholar] [CrossRef] [PubMed]
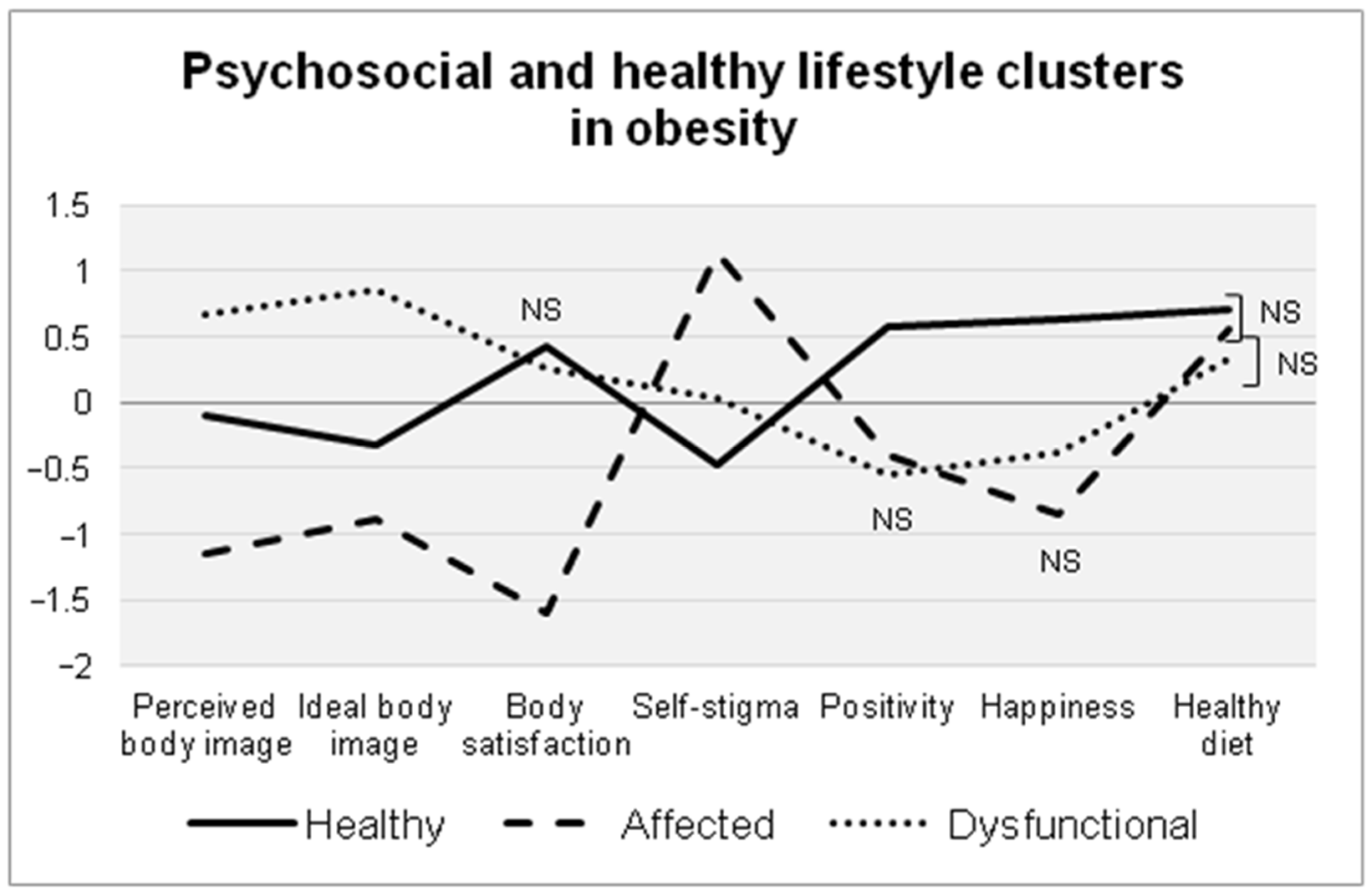
| Configurational Variables | Healthy N = 46% | Affected N = 18% | Dysfunctional N = 36% | F | p | |||
|---|---|---|---|---|---|---|---|---|
| M | SD | M | SD | M | SD | |||
| Perceived body image | −0.09 | 0.62 | −1.14 | 0.48 | 0.68 | 1.04 | 33.092 | 0.000 ** |
| Ideal body image | −0.33 | 0.83 | −0.88 | 0.64 | 0.86 | 0.66 | 41.895 | 0.000 ** |
| Body satisfaction | 0.42 | 0.58 | −1.59 | 0.82 | 0.25 | 0.69 | 62.701 | 0.000 ** |
| Self-stigma | −0.48 | 0.62 | 1.15 | 1.00 | 0.04 | 0.93 | 25.637 | 0.000 ** |
| Positivity | 0.58 | 0.65 | −0.40 | 1.10 | −0.54 | 0.93 | 20.046 | 0.000 ** |
| Happiness | 0.63 | 0.62 | −0.84 | 1.07 | −0.38 | 0.86 | 27.933 | 0.000 ** |
| Healthy diet | 0.70 | 0.47 | 0.56 | 0.51 | 0.33 | 0.48 | 5.808 | 0.004 ** |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Godoy-Izquierdo, D.; Lara, R.; Ogallar, A.; Rodríguez-Tadeo, A.; Ramírez, M.J.; Navarrón, E.; Arbinaga, F. Psychosocial and Diet-Related Lifestyle Clusters in Overweight and Obesity. Int. J. Environ. Res. Public Health 2021, 18, 6461. https://doi.org/10.3390/ijerph18126461
Godoy-Izquierdo D, Lara R, Ogallar A, Rodríguez-Tadeo A, Ramírez MJ, Navarrón E, Arbinaga F. Psychosocial and Diet-Related Lifestyle Clusters in Overweight and Obesity. International Journal of Environmental Research and Public Health. 2021; 18(12):6461. https://doi.org/10.3390/ijerph18126461
Chicago/Turabian StyleGodoy-Izquierdo, Débora, Raquel Lara, Adelaida Ogallar, Alejandra Rodríguez-Tadeo, María J. Ramírez, Estefanía Navarrón, and Félix Arbinaga. 2021. "Psychosocial and Diet-Related Lifestyle Clusters in Overweight and Obesity" International Journal of Environmental Research and Public Health 18, no. 12: 6461. https://doi.org/10.3390/ijerph18126461
APA StyleGodoy-Izquierdo, D., Lara, R., Ogallar, A., Rodríguez-Tadeo, A., Ramírez, M. J., Navarrón, E., & Arbinaga, F. (2021). Psychosocial and Diet-Related Lifestyle Clusters in Overweight and Obesity. International Journal of Environmental Research and Public Health, 18(12), 6461. https://doi.org/10.3390/ijerph18126461







