Analysis of the Local Health-Enhancing Physical Activity Policies on the French Riviera
Abstract
1. Introduction
2. Materials and Methods
2.1. Description of the CAPLA-Santé Tool
2.2. Participants
2.3. Data Collection and Analysis
3. Results
3.1. Participants
3.2. Data Collection and Analysis
3.2.1. Section 1: Overview of HEPA Stakeholders in the Local Government Area
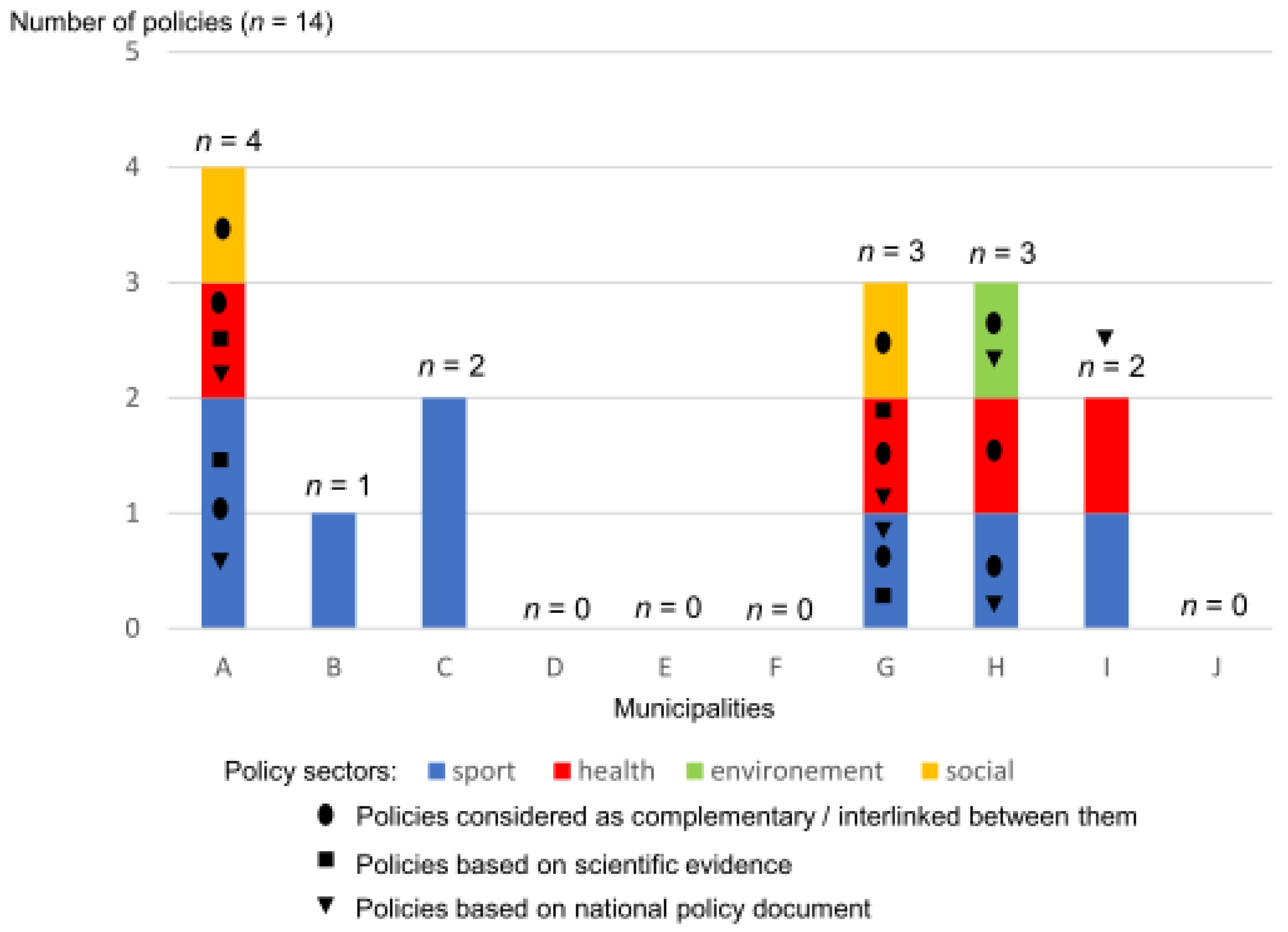
3.2.2. Section 2: Policy Documents
3.2.3. Section 3: Policy Contents
3.2.4. Section 4: Funding and Political Engagement
3.2.5. Section 5: Studies and Measures Relating to Physical Activity in the Local Government Area
3.2.6. Section 6: Progress Achieved and Future Challenges
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lee, I.-M.; Shiroma, E.J.; Lobelo, F.; Puska, P.; Blair, S.N.; Katzmarzyk, P.T.; Group, L.P.A.S.W. Effect of physical inactivity on major non-communicable diseases worldwide: An analysis of burden of disease and life expectancy. Lancet 2012, 380, 219–229. [Google Scholar] [CrossRef]
- Reiner, M.; Niermann, C.; Jekauc, D.; Woll, A. Long-term health benefits of physical activity-a systematic review of longitudinal studies. BMC Public Health 2013, 13, 813. [Google Scholar] [CrossRef] [PubMed]
- International Society for Physical Activity and Health. The Toronto Charter for Physical Activity: A Global Call for Action. J. Phys. Act. Health 2010, 7, 370–385. [Google Scholar] [CrossRef] [PubMed]
- International Society for Physical Activity and Health. The Bangkok Declaration on Physical Activity for Global Health and Sustainable Development. Br. J. Sports Med. 2017, 51, 1389–1391. [Google Scholar] [CrossRef] [PubMed]
- Bauman, A.E.; Reis, R.S.; Sallis, J.F.; Wells, J.C.; Loos, R.J.F.; Martin, B.W. Correlates of physical activity: Why are some people physically active and others not? Lancet 2012, 380, 258–271. [Google Scholar] [CrossRef]
- Reis, R.S.; Salvo, D.; Ogilvie, D.; Lambert, E.V.; Goenka, S.; Brownson, R.C. Scaling up physical activity interventions worldwide: Stepping up to larger and smarter approaches to get people moving. Lancet 2016, 388, 1337–1348. [Google Scholar] [CrossRef]
- Golden, S.D.; McLeroy, K.R.; Green, L.W.; Earp, J.A.L.; Lieberman, L.D. Upending the Social Ecological Model to Guide Health Promotion Efforts Toward Policy and Environmental Change. Health Educ. Behav. 2015, 42, 8S–14S. [Google Scholar] [CrossRef]
- Ding, D.; Ramirez Varela, A.; Bauman, A.E.; Ekelund, U.; Lee, I.M.; Heath, G.; Katzmarzyk, P.T.; Reis, R.; Pratt, M. Towards better evidence-informed global action: Lessons learnt from the Lancet series and recent developments in physical activity and public health. Br. J. Sports Med. 2020, 54, 462–468. [Google Scholar] [CrossRef]
- Pratt, M.; Perez, L.G.; Goenka, S.; Brownson, R.C.; Bauman, A.; Sarmiento, O.L.; Hallal, P.C. Can Population Levels of Physical Activity Be Increased? Global Evidence and Experience. Prog. Cardiovasc. Dis. 2015, 57, 356–367. [Google Scholar] [CrossRef]
- Wilkinson, R. The Solid Fact-promoting Physical Activity and Active Living in Urban Environments-the Role of Local Governments: WHO Regional Publications, European Series No. 89; World Health Organization: Geneva, Switzerland, 2006; ISBN 9289021810. [Google Scholar]
- World Health Organization. More Active People for a Healthier World: Global Action Plan on Physical Activity 2018–2030; World Health Organization: Geneva, Switzerland, 2018; ISBN 9789241514187. [Google Scholar]
- World Health Organization. Physical Activity Strategy for the WHO European Region 2016–2025; World Health Organization: Geneva, Switzerland, 2016. [Google Scholar]
- Noël Racine, A.; Garbarino, J.M.; Corrion, K.; D’Arripe-Longueville, F.; Massiera, B.; Vuillemin, A. Perceptions of barriers and levers of health-enhancing physical activity policies in mid-size French municipalities. Health Res. Policy Syst. 2020, 18, 1–10. [Google Scholar] [CrossRef]
- Guthold, R.; Stevens, G.A.; Riley, L.M.; Bull, F.C. Worldwide trends in insufficient physical activity from 2001 to 2016: A pooled analysis of 358 population-based surveys with 1·9 million participants. Lancet. Glob. Health 2018, 6, e1077–e1086. [Google Scholar] [CrossRef]
- World Health Organization. France-Physical Activity Factsheet (2018); World Health Organization: Geneva, Switzerland, 2018. [Google Scholar]
- World Health Organization. Global Recommendations on Physical Activity for Health; World Health Organization: Geneva, Switzerland, 2010. [Google Scholar]
- Prévot-Ledrich, J.; Van Hoye, A.; Lombrail, P.; Lecomte, F.; Vuillemin, A. Panorama des politiques publiques françaises de promotion de l’activité physique bénéfique pour la santé. Sante Publique 2016, 28, S25–S31. [Google Scholar] [CrossRef] [PubMed]
- Daugbjerg, S.B.; Kahlmeier, S.; Racioppi, F.; Martin-Diener, E.; Martin, B.; Oja, P.; Bull, F. Promotion of physical activity in the European region: Content analysis of 27 national policy documents. J. Phys. Act. Health 2009, 6, 805–817. [Google Scholar] [CrossRef] [PubMed]
- Van Hoye, A.; Vandoorne, C.; Absil, G.; Lecomte, F.; Fallon, C.; Lombrail, P.; Vuillemin, A. Health enhancing physical activity in all policies? Comparison of national public actors between France and Belgium. Health Policy 2019, 123, 327–332. [Google Scholar] [CrossRef]
- Kohl, H.W.; Craig, C.L.; Lambert, E.V.; Inoue, S.; Alkandari, J.R.; Leetongin, G.; Kahlmeier, S.; Andersen, L.B.; Bauman, A.E.; Blair, S.N.; et al. The pandemic of physical inactivity: Global action for public health. Lancet 2012, 380, 294–305. [Google Scholar] [CrossRef]
- Rütten, A.; Abu-Omar, K.; Gelius, P.; Schow, D. Physical inactivity as a policy problem: Applying a concept from policy analysis to a public health issue. Health Res. Policy Syst. 2013, 11, 9. [Google Scholar] [CrossRef]
- Vuori, I.; Lankenau, B.; Pratt, M. Physical activity policy and program development: The experience in Finland. Public Health Rep. 2004, 119, 331–345. [Google Scholar] [CrossRef]
- Guglielmin, M.; Muntaner, C.; O’Campo, P.; Shankardass, K. A scoping review of the implementation of health in all policies at the local level. Health Policy 2018, 122, 284–292. [Google Scholar] [CrossRef]
- World Health Organization. Healthy Cities Promoting Health and Equity-Evidence for Local Policy and Practice; World Health Organization Europe: Copenhagen, Denmark, 2014. [Google Scholar]
- Spitters, H.P.E.M.; Lau, C.J.; Sandu, P.; Quanjel, M.; Dulf, D.; Glumer, C.; van Oers, H.A.M.; van de Goor, I.A.M. Unravelling networks in local public health policymaking in three European countries-a systems analysis. Health Res. Policy Syst. 2017, 15, 5. [Google Scholar] [CrossRef]
- Bull, F. Translating science to inform global policy on physical activity. J. Sport Health Sci. 2018, 7, 3–4. [Google Scholar] [CrossRef]
- Noël Racine, A.; Van Hoye, A.; Boyd, A.; Jackson, F.; Garbarino, J.M.; Massiera, B.; Kahlmeier, S.; Sandu, P.; Vuillemin, A. A scoping review of published research on local government policies promoting health-enhancing physical activity. Int. J. Sport Policy Polit. 2020, 12, 747–763. [Google Scholar] [CrossRef]
- Bull, F.C.; Milton, K.; Kahlmeier, S. National policy on physical activity: The development of a policy audit tool. J. Phys. Act. Health 2014, 11, 233–240. [Google Scholar] [CrossRef] [PubMed]
- Noël Racine, A.; Van Hoye, A.; Baron, A.; Lecomte, F.; Garbarino, J.M.; Massiera, B.; Honta, M.; Vuillemin, A. Development of a Local Health-Enhancing Physical Activity Policy Analysis Tool in France: CAPLA-Santé. Health Promot. Pract. 2020. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Health-Enhancing Physical Activity (HEPA) Policy Audit Tool (PAT)-Version 2 (2015); World Health Organization: Geneva, Switzerland, 2015. [Google Scholar]
- Institut National de la Statistique et des Etudes Economiques. Available online: https://www.insee.fr/fr/accueil (accessed on 9 October 2019).
- Observatoire Régional de la Santé Provence-Alpes-Côte d’Azur. SIRSéPACA. Available online: http://www.sirsepaca.org (accessed on 11 May 2020).
- King, A.; John, W. Kingdon, Agendas, Alternatives, and Public Policies, Boston: Little, Brown, 1984, xi + 240 pp., $9.95. J. Public Policy 1985, 5, 281–283. [Google Scholar] [CrossRef]
- McKay, H.; Naylor, P.J.; Lau, E.; Gray, S.M.; Wolfenden, L.; Milat, A.; Bauman, A.; Race, D.; Nettlefold, L.; Sims-Gould, J. Implementation and scale-up of physical activity and behavioural nutrition interventions: An evaluation roadmap. Int. J. Behav. Nutr. Phys. Act. 2019, 16, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Woods, C.B.; Mutrie, N. Putting physical activity on the policy agenda. Quest 2012, 64, 92–104. [Google Scholar] [CrossRef]
- Giles-Corti, B.; Vernez-Moudon, A.; Reis, R.; Turrell, G.; Dannenberg, A.L.; Badland, H.; Foster, S.; Lowe, M.; Sallis, J.F.; Stevenson, M.; et al. City planning and population health: A global challenge. Lancet 2016, 388, 2912–2924. [Google Scholar] [CrossRef]
- Coghill, C.L.; Valaitis, R.K.; Eyles, J.D. Built environment interventions aimed at improving physical activity levels in rural Ontario health units: A descriptive qualitative study Health policies, systems and management. BMC Public Health 2015, 15. [Google Scholar] [CrossRef]
- Lemon, S.C.; Goins, K.V.; Schneider, K.L.; Brownson, R.C.; Valko, C.A.; Evenson, K.R.; Eyler, A.A.; Heinrich, K.M.; Lyn, R.; Litt, J.; et al. Municipal officials’ participation in built environment policy development in the United States. Am. J. Health Promot. 2015, 30, 42–49. [Google Scholar] [CrossRef]
- Thomas, M.M.; Hodge, W.; Smith, B.J. Building capacity in local government for integrated planning to increase physical activity: Evaluation of the VicHealth MetroACTIVE program. Health Promot. Int. 2009, 24. [Google Scholar] [CrossRef]
- Brownson, R.C.; Jones, E. Bridging the gap: Translating research into policy and practice. Prev. Med. 2009, 49, 313–315. [Google Scholar] [CrossRef] [PubMed]
- Rivière, F. Contribution to the Surveillance and Measurement of Physical Activity and Sedentary Behaviors. Ph.D. Thesis, Université de Lorraine, Nancy, France, 13 December 2017. [Google Scholar]
- Althoff, T.; Sosič, R.; Hicks, J.L.; King, A.C.; Delp, S.L.; Leskovec, J. Large-scale physical activity data reveal worldwide activity inequality. Nature 2017, 547, 336–339. [Google Scholar] [CrossRef] [PubMed]
- Lavrakas, P. Encyclopedia of Survey Research Methods; SAGE Publications: Thousand Oaks, CA, USA, 2008. [Google Scholar]
| Municipality | Inhabitants (n) * | Median Income (€) ** | People Affected by a Chronic Illness (n) *** | Key Informant Position | Sector Position |
|---|---|---|---|---|---|
| A | 74,875 | 22,392 | 12,441 | HD | social |
| Head of HEPA † project Project officer | sport health | ||||
| B | 49,322 | 22,046 | 8012 | HD | social |
| HD | sport | ||||
| C | 28,919 | 22,858 | 4592 | HD | social |
| HD | sport | ||||
| D | 50,937 | 20,704 | 7607 | HD | sport and social |
| E | 41,571 | 20,010 | 7250 | HD | sport |
| HD | health | ||||
| F | 35,296 | 23,152 | 6913 | HD | sport |
| HD | health | ||||
| G | 64,903 | 18,656 | 11,305 | HD | sport |
| HD | health | ||||
| H | 74,285 | 18,962 | 14,369 | HD HD | sport social |
| I | 25,047 | 20,940 | 4656 | HD | social |
| HD | sport | ||||
| J | 23,347 | 21,778 | 3342 | HD | social |
| HD | sport | ||||
| HD | health |
| Municipality | Sectors and Public Agencies (n) Engaged in HEPA Promotion | Non-Governmental Stakeholders (n) Engaged in HEPA Promotion | Leadership Identified | Coordinator Identified | Connections with HEPA Network |
|---|---|---|---|---|---|
| A | sport (n = 2), health (n = 1), multisectoral (n = 1) | insurance and private sport (n = 2), sport (n = 1), health (n = 1) | municipality | sports department | yes |
| B | sport (n = 3), multisectoral (n = 2) health (n = 1), education (n = 1) | sport (n = 1), health (n = 1) | municipality | - | yes |
| C | sport (n = 2), health (n = 1), social (n = 1), multisectoral (n = 1) | sport (n = 3), health (n = 2), insurance and private sport (n = 2) | municipality | - | yes |
| D | health (n = 3), education (n 2), sport (n = 1), | sport (n = 1) | - | - | - |
| E | sport (n = 2), health (n = 1) | sport (n = 1), health (n = 1) | - | - | - |
| F | multisectoral (n = 1) | sport (n = 1), health (n = 1), insurance (n = 1) | - | - | none |
| G | health (n = 3), sport (n = 2), education (n = 1); multisectoral (n = 1) | health (n = 2), private sport (n = 1), sport (n = 1) | municipality | social services department | yes |
| H | sport (n =1), health (n = 1), education (n = 1) | sport (n = 1), health (n = 1) | municipality | Health services | yes |
| I | health (n = 2), sport (n = 1), | sport (n =1), health (n = 1), education (n = 1) | municipality | - | - |
| J | sport (n = 1), education (n = 1) | sport (n = 1), education (n = 1) | - | - | - |
| Municipality | Policy Settings | Target Audiences | Communication Strategies or Actions | Concrete Actions |
|---|---|---|---|---|
| A | sports and leisure urban environment health and social care centers | general population seniors inactive and people suffering from chronic diseases | website social networks local newspapers events awareness of healthcare professional | PA * program fitness trails |
| B | sports and leisure | sedentary people | website events | PA program |
| C | sports and leisure | seniors | website social networks local newspapers | PA program |
| D | no data | no data | no data | no data |
| E | no data | no data | no data | no data |
| F | no data | no data | website social networks | events promoting PA for heath |
| H | sports and leisure tourism urban environment | general population inactive people pre-school and children | website social networks events | outdoor fitness and trail network HEPA events |
| I | sports and leisure primary school priority neighborhoods for urban policy | seniors children | website social networks | PA programs |
| J | no data | no data | no data | no data |
| Municipality | Keys Moments | Strengths | Weaknesses | Progress | Challenges |
|---|---|---|---|---|---|
| A | national legislation of physical activity prescription; local conference on the topic | local stakeholder network; geographic situation; sportsfacilities; presence of PA and health professionals | limited resources; lack of cycle path network | implementation of HEPA actions | formalize global HEPA action; develop HEPA events; identify recurring funding to sustain HEPA policies |
| B | pilot implementation of PA program | local stakeholder network; quality and number of PA facilities | lack of intersectoral coordination; geographic difficulties in accessing PA facilities | sustainment of a PA pilot program for seniors to a regular program | improve stakeholder coordination; identify recurring findings to sustain HEPA policies; develop public space to practice PA |
| C | mayor’s willingness to promote PA | local stakeholder network; geographic situation | few PA programs available for sedentary and inactive people; lack of resources; overuse of PA facilities | implementation of HEPA actions | develop human resources with PA and health training; identify recurring funding to sustain HEPA policies |
| D | no data | local stakeholder network | unwillingness to develop policy; difficulties moving in the city without a car; lack of resources | no data | build willingness to develop a policy; develop a global intersectoral HEPA policy |
| E | no data | knowledge of the territory | lack of resources | no data | develop active mobility; develop a HEPA plan |
| F | no data | local stakeholder network; quality and number of sports facilities; knowledge of the local context | unwillingness to develop policy; lack of knowledge in PA and health, lack of intersectoral collaboration | no data | formalize a HEPA policy; develop a campaign to sensitize residents |
| G | -national policy to promote PA | local stakeholder network; culture of sport; global vision of health | lack of resources and PA facilities | implementation of HEPA actions | develop a global HEPA project from children to older people |
| H | -mandate of the mayor; national HEPA campaign | local stakeholder network, geographic situation; willingness of the mayor; PA facilities | overcrowed PA facilities | implementation of HEPA actions | target more inactive people; develop more cyclable paths |
| I | -national policy to promote PA | geographic situation; PA facilities; good communication | lack of resources | implementation of HEPA actions | target more inactive people; develop a global intersectoral HEPA policy with dedicated human resources |
| J | no data | local network of stakeholders | lack of PA facilities and lack of public open space | no data | build willingness to develop a policy; develop a global HEPA policy with the metropolis |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Racine, A.N.; Garbarino, J.-M.; Massiera, B.; Vuillemin, A. Analysis of the Local Health-Enhancing Physical Activity Policies on the French Riviera. Int. J. Environ. Res. Public Health 2021, 18, 156. https://doi.org/10.3390/ijerph18010156
Racine AN, Garbarino J-M, Massiera B, Vuillemin A. Analysis of the Local Health-Enhancing Physical Activity Policies on the French Riviera. International Journal of Environmental Research and Public Health. 2021; 18(1):156. https://doi.org/10.3390/ijerph18010156
Chicago/Turabian StyleRacine, Antoine Noël, Jean-Marie Garbarino, Bernard Massiera, and Anne Vuillemin. 2021. "Analysis of the Local Health-Enhancing Physical Activity Policies on the French Riviera" International Journal of Environmental Research and Public Health 18, no. 1: 156. https://doi.org/10.3390/ijerph18010156
APA StyleRacine, A. N., Garbarino, J.-M., Massiera, B., & Vuillemin, A. (2021). Analysis of the Local Health-Enhancing Physical Activity Policies on the French Riviera. International Journal of Environmental Research and Public Health, 18(1), 156. https://doi.org/10.3390/ijerph18010156






