H-WORK Project: Multilevel Interventions to Promote Mental Health in SMEs and Public Workplaces
Abstract
1. Introduction
2. Materials and Methods
2.1. Conceptual Model
2.1.1. Job Demands–Resources Theory and Positive Psychology
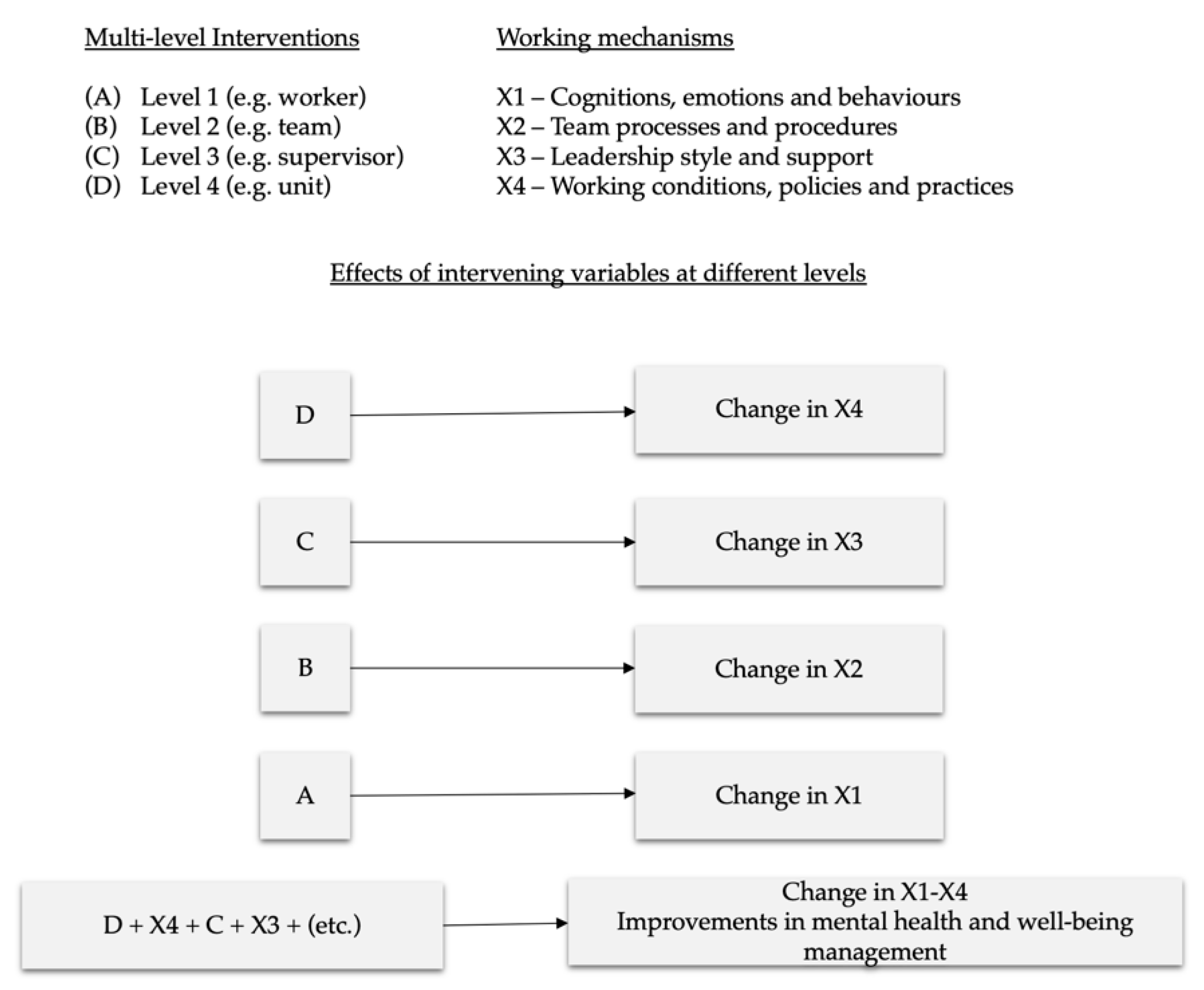
2.1.2. IGLO Model
2.1.3. Participatory Approach
2.1.4. Use of Digital Technologies
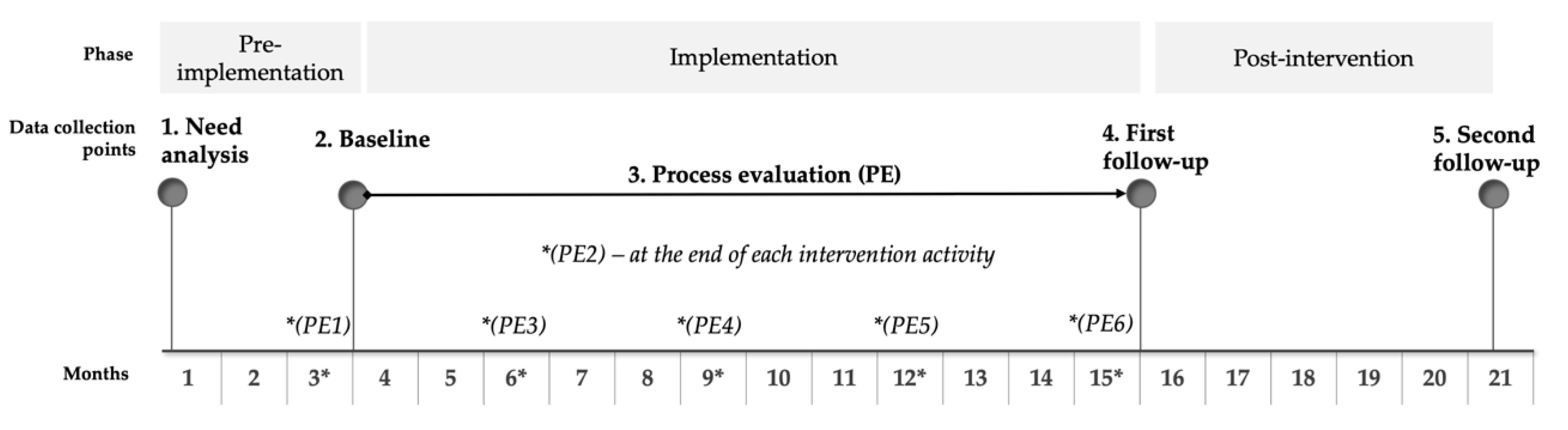
2.2. Study Design Overview
2.2.1. Variables of Study and Statistical Analysis
2.2.2. Population and Sample Size
2.3. The H-WORK Toolkits
2.3.1. The H-WORK Assessment Toolkit (HAT)
2.3.2. The H-WORK Intervention Toolkit (HIT)
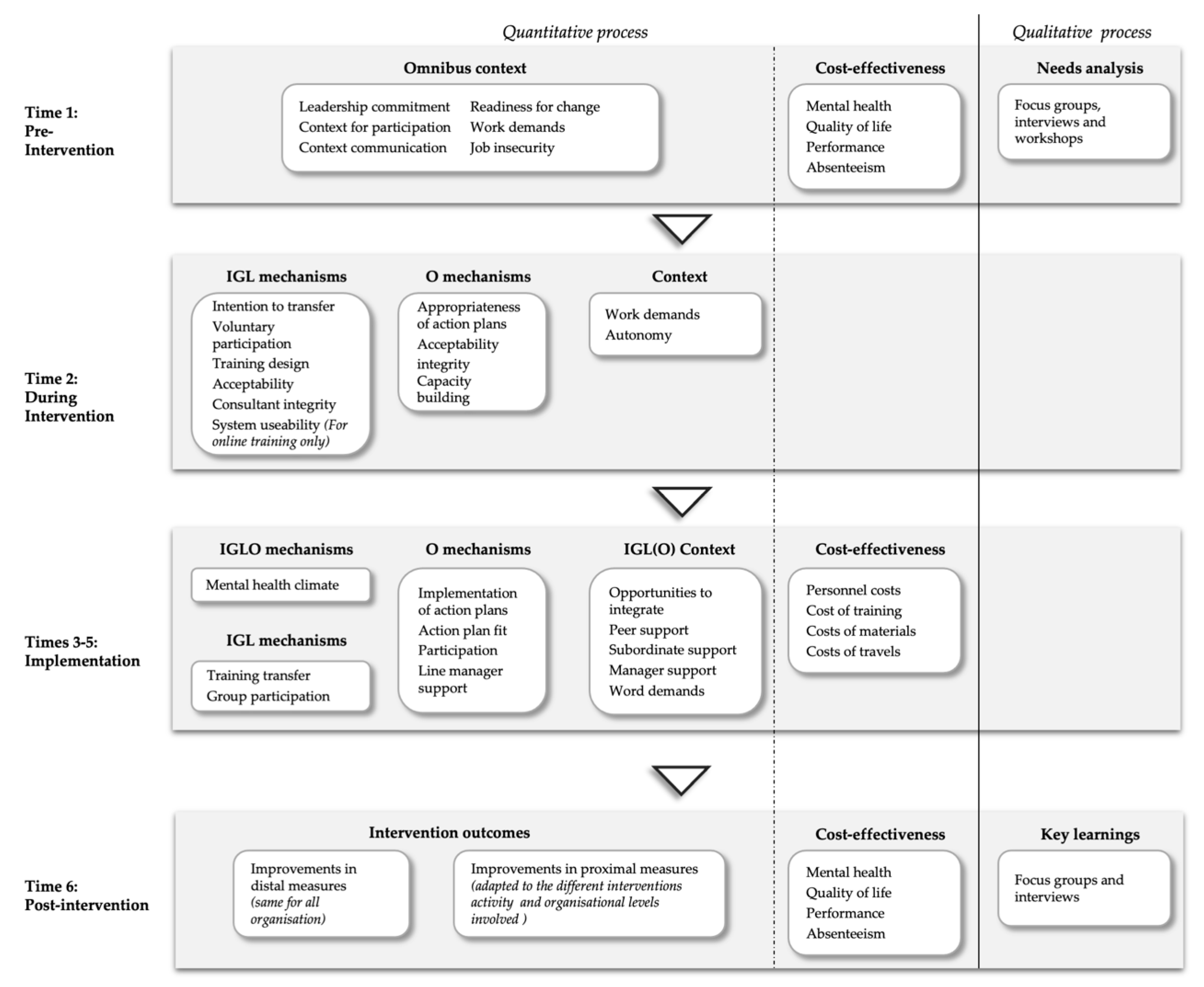
2.3.3. The H-WORK Evaluation Toolkit (HET)
3. Discussion
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- WHO. Mental Health Action Plan 2013–2020. Available online: https://www.who.int/mental_health/publications/action_plan/en/ (accessed on 13 July 2020).
- European Commission. “Together for mental health and well-being”. European Pact for Mental Health and Well-Being. In Proceedings of the EU High-Level Conference, Brussels, Belgium, 12–13 June 2008; Available online: https://ec.europa.eu/health/ph_determinants/life_style/mental/docs/pact_en.pdf (accessed on 15 June 2019).
- European Commission. European Framework for Action on Mental Health and Wellbeing; EU Joint Action on Mental Health and Wellbeing: Brussels, Belgium, 2016; Available online: https://ec.europa.eu/research/participants/data/ref/h2020/other/guides_for_applicants/h2020-SC1-BHC-22-2019-framework-for-action_en.pdf (accessed on 15 June 2019).
- Wittchen, H.U.; Jacobi, F.; Rehm, J.; Gustavsson, A.; Svensson, M.; Jönsson, B.; Olesen, J.; Allgulander, C.; Alonso, J.; Faravelli, C.; et al. The size and burden of mental disorders and other disorders of the brain in Europe 2010. Eur. Neuropsychopharm. 2011, 21, 655–679. [Google Scholar] [CrossRef]
- Leka, S.; Jain, A. EU Compass for Action on Mental Health and Wellbeing—Mental Health in the Workplace in Europe. Available online: https://ec.europa.eu/health/ (accessed on 12 March 2019).
- Eurostat, E.C. Health and Safety at Work in Europe-A Statistical Portrait: Data 1999–2007; European Communities: Luxembourg, 2010; Available online: https://ec.europa.eu/eurostat/documents/ (accessed on 15 June 2019).
- Von Thiele, S.U.; Hasson, H. Employee self-rated productivity and objective organisational production levels: Effects of worksite health interventions involving reduced work hours and physical exercise. J. Occup. Environ. Med. 2011, 53, 838–844. [Google Scholar] [CrossRef]
- Dennerlein, J.T.; Burke, L.; Sabbath, E.L.; Williams, J.A.R.; Peters, S.E.; Wallace, L.; Karapanos, M.; Sorensen, G. An integrative total worker health framework for keeping workers safe and healthy during the COVID-19 pandemic. Hum. Factors. 2020, 62. [Google Scholar] [CrossRef]
- Occupational Safety and Health Administration (OSHA). Guidance on Preparing Workplaces for COVID-19; Department of Labor: Washington, WA, USA, 2020. Available online: https://www.osha.gov/Publications/OSHA3990.pdf (accessed on 4 August 2020).
- Ren, T.; Cao, L.; Chin, T. Crafting jobs for occupational satisfaction and innovation among manufacturing workers facing the COVID-19 crisis. Int. J. Environ. Res. Public Health 2020, 17, 3953. [Google Scholar] [CrossRef] [PubMed]
- Ruhle, S.A.; Breitsohl, H.; Aboagye, E.; Baba, V.; Biron, C.; Correia Leal, C.; Dietz, C.; Ferreira, A.I.; Gerich, J.; Johns, G.; et al. “To work, or not to work, that is the question”—Recent trends and avenues for research on presenteeism. Eur. J. Work Organ. Psychol. 2020, 29, 344–363. [Google Scholar] [CrossRef]
- Alexandrova-Karamanova, A.; Todorova, I.; Montgomery, A.; Panagopoulou, E.; Costa, P.; Baban, A.; Davas, A.; Milosevic, M.; Mijakoski, D. Burnout and health behaviors in health professionals from seven European countries. Int. Arch. Occup. Environ. Health 2016, 89, 1059–1075. [Google Scholar] [CrossRef] [PubMed]
- International Labour Organization (ILO). Safety and Health at the Heart of the Future of Work. Building on 100 Years of Experience; ILO Publications: Geneva, Switzerland, 2019; ISBN 978-92-2-133151-3. [Google Scholar]
- EU-OSHA. Psychosocial Risks in Europe: Prevalence and Strategies for Prevention; Publications Office of the European Union: Luxembourg, 2019; Available online: https://osha.europa.eu/en/tools-andpublications/publications/reports/ (accessed on 15 June 2019).
- Faragher, E.B.; Cass, M.; Cooper, C.L. The relationship between job satisfaction and health: A meta-analysis. In From Stress to Wellbeing Volume 1; Cooper, C.L., Ed.; Palgrave Macmillan: London, UK, 2013; pp. 254–271. [Google Scholar] [CrossRef]
- Kuoppala, J.; Lamminpää, A.; Husman, P. Work health promotion, job well-being, and sickness absences—A systematic review and meta-analysis. J. Occup. Environ. Med. 2008, 50, 1216–1227. [Google Scholar] [CrossRef] [PubMed]
- Nijp, H.H.; Beckers, D.G.J.; Geurts, S.A.E.; Tucker, P.; Kompier, M.A.J. Systematic review on the association between employee worktime control and work-non-work balance, health and well-being, and job-related outcomes. Scand. J. Work Environ. Health 2012, 38, 299–313. [Google Scholar] [CrossRef]
- Carolan, S.; Harris, P.R.; Cavanagh, K. Improving employee well-being and effectiveness: Systematic review and meta-analysis of web-based psychological interventions delivered in the workplace. J. Med. Internet Res. 2017, 19, e271. [Google Scholar] [CrossRef]
- Phillips, E.A.; Gordeev, V.S.; Schreyögg, J. Effectiveness of occupational e-mental health interventions: A systematic review and meta-analysis of randomized controlled trials. Scand. J. Work Environ. Health 2019, 45, 560–576. [Google Scholar] [CrossRef]
- McCoy, K.; Stinson, K.; Scott, K.; Tenney, L.; Newman, L.S. Health promotion in small business: A systematic review of factors influencing adoption and effectiveness of worksite wellness programs. J. Occup. Environ. Med. 2014, 56, 579–587. [Google Scholar] [CrossRef] [PubMed]
- Organisation for Economic Co-operation and Development (OECD). Sick on the Job? Myths and Realities about Mental Health and Work; OECD Publishing: Paris, France, 2012; ISBN 9789264124516. [Google Scholar]
- Michaels, C.N.; Greene, A.M. Worksite wellness: Increasing adoption of workplace health promotion programs. Health Promot. Pract. 2013, 14, 473–479. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, K.; Yarker, J.; Munir, F.; Bültmann, U. IGLOO: An integrated framework for sustainable return to work in workers with common mental disorders. Work Stress 2018, 32, 400–417. [Google Scholar] [CrossRef]
- Havermans, B.M.; Schelvis, R.M.; Boot, C.R.; Brouwers, E.P.; Anema, J.R.; van der Beek, A.J. Process variables in organizational stress management intervention evaluation research: A systematic review. Scand. J. Work Environ. Health 2016, 42, 371–381. [Google Scholar] [CrossRef]
- Biron, C.; Karanika-Murray, M. Process evaluation for organizational stress and well-being interventions: Implications for theory, method, and practice. Int. J. Stress Manag. 2014, 21, 85. [Google Scholar] [CrossRef]
- Nielsen, K.; Randall, R. The importance of employee participation and perceptions of changes in procedures in a teamworking intervention. Work Stress 2012, 26, 91–111. [Google Scholar] [CrossRef] [PubMed]
- Silvaggi, F.; Miraglia, M. Mental health at work: A review of interventions in organizations. E-J. Int. Comp. Labour Stud. 2017, 6, 1–27. [Google Scholar]
- Day, A.; Nielsen, K. What does our organization do to help our well-being? Creating healthy workplaces and workers. In An Introduction of Work and Organizational Psychology; Chmiel, N., Fraccaroli, F., Sverke, M., Eds.; Wiley Blackwell: Hoboken, NJ, USA, 2017; pp. 295–314. [Google Scholar]
- Bakker, A.B.; Demerouti, E. Multiple levels in job demands-resources theory: Implications for employee well-being and performance. In Handbook of Wellbeing; Diener, E., Oishi, S., Tay, L., Eds.; DEF Publishers: Salt Lake City, UT, USA, 2018; pp. 1–13. [Google Scholar]
- Bakker, A.B. Towards a multilevel approach of employee well-being. Eur. J. Work. Organ. Psychol. 2015, 24, 839–843. [Google Scholar] [CrossRef]
- Ilies, R.; Aw, S.S.Y.; Pluut, H. Intraindividual models of employee well-being: What have we learned and where do we go from here? Eur. J. Work. Organ. Psychol. 2015, 24, 827–838. [Google Scholar] [CrossRef]
- Beck, D.; Lenhardt, U. Consideration of psychosocial factors in workplace risk assessments: Findings from a company survey in Germany. Int. Arch. Occ. Environ. Health 2019, 92, 435–451. [Google Scholar] [CrossRef]
- Schuller, K. Interventions as the centerpiece of psychosocial risk assessment—Why so difficult? Int. J. Workplace Health Manag. 2020, 13, 61–80. [Google Scholar] [CrossRef]
- Pollett, H. Mental Health Promotion: A Literature Review; Canadian Mental Health Association: Ottawa, ON, Canada, 2007; Available online: http://www.sfu.ca/~hcscoop/mentalhealth/mentalhealthpapers/Pollet_2007.pdf (accessed on 18 September 2020).
- Jane-Lopis, E.; Barry, M.M.; Hosman, C.; Patel, V. Mental health promotion works: A review. Promot. Educ. 2005, 12, 9–25. [Google Scholar] [CrossRef] [PubMed]
- Bakker, A.B.; Demerouti, E. Job demands-resources theory: Taking stock and looking forward. J. Occup. Health Psychol. 2017, 22, 273–285. [Google Scholar] [CrossRef] [PubMed]
- Van den Broeck, A.; De Cuyper, N.; De Witte, H.; Vansteenkiste, M. Not all job demands are equal: Differentiating job hindrances and job challenges in the Job Demands–Resources model. Eur. J. Work Organ. Psychol. 2010, 19, 735–759. [Google Scholar] [CrossRef]
- Peterson, C.; Park, N.; Sweeney, P.J. Group well-being: Morale from a positive psychology perspective. Appl. Psychol. 2008, 57, 19–36. [Google Scholar] [CrossRef]
- Chen, S.L.; Shih, C.T.; Chi, N.W. A multilevel job demands–resources model of work engagement: Antecedents, consequences, and boundary conditions. Hum. Perform. 2018, 31, 282–304. [Google Scholar] [CrossRef]
- Bakker, A.B.; Derks, D. Positive occupational health psychology. In Occupational Health Psychology; Leka, S., Houdmont, J., Eds.; Wiley: Chichester, UK, 2010; pp. 194–224. [Google Scholar]
- Coo, C.; Salanova, M. Mindfulness can make you happy-and-productive: A mindfulness controlled trial and its effects on happiness, work engagement and performance. J. Happiness Stud. 2018, 19, 1691–1711. [Google Scholar] [CrossRef]
- Meyers, M.C.; van Woerkom, M.; Bakker, A.B. The added value of the positive: A literature review of positive psychology interventions in organizations. Eur. J. Work Organ. Psychol. 2013, 22, 618–632. [Google Scholar] [CrossRef]
- Briñol, P.; Petty, R.E.; Gandarillas, B.; Moreno, L. Are positive interventions always beneficial? Span. J. Psychol. 2020, 23, e23. [Google Scholar] [CrossRef]
- Pawson, R.; Tilley, N. Realistic Evaluation; Sage: London, UK, 1997. [Google Scholar]
- Richardson, K.M.; Rothstein, H.R. Effects of occupational stress management intervention programs: A meta-analysis. J. Occup. Health Psychol. 2008, 13, 69–93. [Google Scholar] [CrossRef]
- Nielsen, K. How can we make organizational intervention works? Employees and line managers as actively crafting interventions. Hum. Relat. 2013, 66, 1029–1050. [Google Scholar] [CrossRef]
- Blume, B.D.; Ford, J.K.; Surface, E.A.; Olenick, J. A dynamic model of training transfer. Hum. Resour. Manag. Rev. 2019, 29, 270–283. [Google Scholar] [CrossRef]
- Bourbonnais, R.; Brisson, C.; Vézina, M. Long-term effects of an intervention on psychosocial work factors among healthcare professionals in a hospital setting. Occup. Environ. Med. 2011, 68, 479–486. [Google Scholar] [CrossRef]
- LaMontagne, A.D.; Keegel, T.; Louie, A.M.; Ostry, A.; Landsbergis, P.A. A systematic review of the job-stress intervention evaluation literature, 1990–2005. Int. J. Occup. Environ. Health 2007, 13, 268–280. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, K.; Nielsen, M.B.; Ogbonnaya, C.; Känsälä, M.; Saari, E.; Isaksson, K. Workplace resources to improve both employee well-being and performance: A systematic review and meta-analysis. Work Stress 2017, 31, 101–120. [Google Scholar] [CrossRef]
- Martin, A.; Karanika-Murray, M.; Biron, C.; Sanderson, K. The psychosocial work environment, employee mental health and organizational interventions: Improving research and practice by taking a multilevel approach. Stress Health 2016, 32, 201–215. [Google Scholar] [CrossRef]
- LaMontagne, A.D.; Martin, A.; Page, K.M.; Reavley, N.J.; Noblet, A.J.; Milner, A.J.; Keegel, T.; Smith, P.M. Workplace mental health: Developing an integrated intervention approach. BMC Psychiatry 2014, 14, 1–11. [Google Scholar] [CrossRef]
- Charns, M.P.; Foster, M.K.; Alligood, E.C.; Benzer, J.K.; Burgess, J.F., Jr.; Li, D.; Mcintosh, N.M.; Burness, A.; Partin, M.R.; Clauser, S.B. Multilevel interventions: Measurement and measures. JNCI Monographs 2012, 44, 67–77. [Google Scholar] [CrossRef]
- Cleary, P.D.; Gross, C.P.; Zaslavsky, A.M.; Taplin, S.H. Multilevel interventions: Study design and analysis issues. JNCI Monographs 2012, 44, 49–55. [Google Scholar] [CrossRef]
- Tetrick, L.E.; Quick, J.C. Prevention at work: Public health in occupational settings. In Handbook of Occupational Health Psychology; Quick, J.C., Tetrick, L.E., Eds.; American Psychological Association: Washington, DC, USA, 2003; pp. 3–17. [Google Scholar]
- Havermans, B.M.; Boot, C.R.L.; Brouwers, E.P.M.; Houtman, I.L.D.; Anema, J.R.; van der Beek, A.J. Process evaluation of a digital platform-based implementation strategy aimed at work stress prevention in a health care organization. J. Occup. Environ. Med. 2018, 60, e484–e491. [Google Scholar] [CrossRef]
- Cirrincione, L.; Plescia, F.; Ledda, C.; Rapisarda, V.; Martorana, D.; Moldovan, R.E.; Theodoridou, K.; Cannizzaro, E. COVID-19 pandemic: Prevention and protection measures to be adopted at the workplace. Sustainability 2020, 12, 3603. [Google Scholar] [CrossRef]
- Luu Duc Huynh, T. Does culture matter social distancing under the COVID-19 pandemic? Saf. Sci. 2020. [Google Scholar] [CrossRef]
- Lai, J.; Ma, S.; Wang, Y.; Cai, Z.; Hu, J.; Wei, N.; Wu, J.; Du, H.; Chen, T.; Li, R.; et al. Factors associated with mental health outcomes among health care workers exposed to Coronavirus Disease 2019. JAMA Netw. Open 2020, 3, e203976. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, K.; Miraglia, M. What works for whom in which circumstances? On the need to move beyond the “what works?” question in organizational intervention research. Hum. Relat. 2017, 70, 40–62. [Google Scholar] [CrossRef]
- Molina-Azorin, J.F.; Bergh, D.D.; Corley, K.G.; Ketchen, D.J., Jr. Mixed methods in the organizational sciences: Taking stock and moving forward. Organ. Res. Methods 2017, 20, 179–192. [Google Scholar] [CrossRef]
- Nielsen, K.; Abildgaard, J.S. Organizational interventions: A research-based framework for the evaluation of both process and effects. Work Stress 2013, 27, 278–297. [Google Scholar] [CrossRef]
- Nielsen, K.; Randall, R.; Christensen, K.B. Does training managers enhance the effects of implementing teamworking? A longitudinal, mixed methods field study. Hum. Relat. 2010, 11, 1719–1741. [Google Scholar] [CrossRef]
- Abildgaard, J.S.; Nielsen, K.; Wåhlin-Jacobsen, C.D.; Maltesen, T.; Christensen, K.B.; Holtermann, A. ‘Same, but different’: A mixed-methods realist evaluation of a cluster-randomized controlled participatory organizational intervention. Hum. Relat. 2020, 73, 1339–1365. [Google Scholar] [CrossRef]
- Lundmark, R.; von Thiele Schwarz, U.; Hasson, H.; Stenling, A.; Tafvelin, S. Making it fit: Associations of line managers’ behaviours with the outcomes of an organizational-level intervention. Stress Health 2018, 34, 163–174. [Google Scholar] [CrossRef]
- Von Thiele Schwarz, U.; Nielsen, K.M.; Stenfors-Hayes, T.; Hasson, H. Using kaizen to improve employee well-being: Results from two organizational intervention studies. Hum. Relat. 2017, 70, 966–993. [Google Scholar] [CrossRef]
- Christensen, M.; Innstrand, S.T.; Saksvik, P.Ø.; Nielsen, K. The line manager’s role in implementing successful organisational interventions. Span. J. Psychol. 2019, 22. [Google Scholar] [CrossRef] [PubMed]
- Sorensen, G.; Sparer, E.; Williams, J.A.R.; Gundersen, D.; Boden, L.I.; Dennerlein, J.T.; Hashimoto, D.; Katz, J.N.; McLellan, D.L.; Okechukwu, C.A.; et al. Measuring best practices for workplace safety, health and wellbeing: The Workplace Integrated Safety and Health Assessment. J. Occup. Environ. Med. 2018, 60, 430–439. [Google Scholar] [CrossRef]
- Dollard, M.F. The PSC-4. A Short PSC Tool. In Psychosocial Safety Climate: A New Work Stress Theory; Dollard, M.F., Dormann, C., Idris, M.A., Eds.; Springer International Publishing: Geneva, Switzerland, 2019; pp. 385–409. ISBN 978-3-030-20319-1. [Google Scholar]
- Hall, G.B.; Dollard, M.F.; Coward, J. Psychosocial Safety Climate: Development of the PSC-12. Int. J. Stress Manag. 2010, 17, 353–383. [Google Scholar] [CrossRef]
- Innstrand, S.T.; Christensen, M. Healthy Universities. The development and implementation of a holistic health promotion intervention programme especially adapted for staff working in the higher educational sector: The ARK study. Glob. Health Promot. 2020, 27, 68–76. [Google Scholar] [CrossRef] [PubMed]
- Schaufeli, W.B. Applying the Job-demands-resources model. Organ. Dyn. 2017, 2, 120–132. [Google Scholar] [CrossRef]
- Van den Heuvel, M.; Demerouti, E.; Peeters, M.C.W. The job crafting intervention: Effects on job resources, self-efficacy, and affective well-being. J. Occup. Organ. Psychol. 2015, 88, 511–532. [Google Scholar] [CrossRef]
- Gilbert, E.; Foulk, T.; Bono, J. Building personal resources through interventions: An integrative review. J. Organ. Behav. 2017, 39, 214–228. [Google Scholar] [CrossRef]
- Muschalla, B. Work-anxiety-coping intervention improves work-coping perception while a recreational intervention leads to deterioration: Results from a randomized controlled trial. Eur. J. Work Organ. Psychol. 2017, 26, 858–869. [Google Scholar] [CrossRef]
- Linden, M.; Muschalla, B.; Hansmeier, T.; Sandner, G. Reduction of sickness absence by an occupational health care management program focusing on self-efficacy and self-management. Work 2013, 47, 485–489. [Google Scholar] [CrossRef]
- Lock, M.; Post, D.; Dollman, J.; Parfitt, G. Efficacy of theory-informed workplace physical activity interventions: A systematic literature review with meta-analyses. Health Psychol. Rev. 2020. [Google Scholar] [CrossRef]
- Babouh, R. Sociomapping of Teams; Dar Ibn Rushd: Praha, Czech Republic, 2012. [Google Scholar]
- Peláez, M.J.; Salanova, M.; Martínez, I.M. Coaching-based leadership intervention program: A controlled trial study. Front. Psychol. 2020, 10, 3066. [Google Scholar] [CrossRef]
- Holman, D.; Axtell, C. Can job redesign interventions influence a broad range of employee outcomes by changing multiple job characteristics? A quasi-experimental study. J. Occup. Health Psychol. 2016, 21, 284–295. [Google Scholar] [CrossRef]
- Hammer, L.B.; Truxillo, D.M.; Bodner, T.; Rineer, J.; Pytlovany, A.C.; Richman, A. Effects of a workplace intervention targeting psychosocial risk factors on safety and health outcomes. Biomed. Res. Int. 2015, 836967, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Pawson, R. The Science of Evaluation: A Realist Manifesto; Sage: London, UK, 2013. [Google Scholar]
- Baldwin, T.T.; Ford, J.K. Transfer of training: A review and directions for future research. Pers. Psychol. 1988, 41, 63–105. [Google Scholar] [CrossRef]
- Blume, T.T.; Ford, J.K.; Baldwin, T.T.; Huang, J.L. Transfer of training: A meta-analytic review. J. Manag. 2010, 36, 1065–1105. [Google Scholar] [CrossRef]
- Nielsen, K.; Noblet, A. Introduction: Organizational interventions: Where we are, where we go from here? In Organizational Interventions for Health and Well-Being: A Handbook for Evidence-Based Practice; Nielsen, K., Noblet, A., Eds.; Routledge: Oxon, UK, 2018; pp. 1–23. [Google Scholar]
- Abildgaard, J.S.; Nielsen, K.; Saksvik, P.O. How to measure the intervention process? An assessment of qualitative and quantitative approaches to data collection in the process evaluation of organizational interventions. Front. Psychol. 2016, 7, 1380. [Google Scholar] [CrossRef]
- Randall, R.; Nielsen, K.; Tvedt, S.D. The development of five scales to measure participants’ appraisal of organizational-level stress management interventions. Work Stress 2009, 23, 1–23. [Google Scholar] [CrossRef]
- Yelon, S.L.; Ford, J.K. Pursuing a multidimensional view of transfer. Perform. Improv. Q. 1999, 12, 58–78. [Google Scholar] [CrossRef]
- Gupta, N.; Wahlin-Jacobsen, C.D.; Abildgaard, J.S.; Henriksen, L.N.; Nielsen, K.; Holtermann, A. Effectiveness of a participatory physical and psychosocial intervention to balance the demands and resources of industrial workers: A cluster-randomized controlled trial. Scand. J. Work Environ. Health 2018, 44, 58–68. [Google Scholar] [CrossRef]
- Vuori, J.; Toppinen-Tanner, S.; Mutanen, P. Effects of resource-building group intervention on career management and mental health in work organizations: Randomized controlled field trial. J. Appl. Psychol. 2012, 97, 273. [Google Scholar] [CrossRef]
- Zhou, L.; Bao, J.; Setiawan, I.M.A.; Saptono, A.; Parmanto, B. The mHealth APP usability questionnaire (MAUQ): Development and validation study. JMIR mHealth uHealth 2019, 7, e11500. [Google Scholar] [CrossRef] [PubMed]
- Van der Klink, J.J.; Blonk, R.W.; Schene, A.H.; van Dijk, F.J. The benefits of interventions for work-related stress. Am. J. Public Health 2001, 91, 270–276. [Google Scholar] [CrossRef] [PubMed]
- Arapovic-Johansson, B.; Wåhlin, C.; Hagberg, J.; Kwak, L.; Björklund, C.; Jensen, I. Participatory work place intervention for stress prevention in primary health care. A randomized controlled trial. Eur. J. Work Organ. Psychol. 2018, 27, 219–234. [Google Scholar] [CrossRef]
- Von Thiele Schwarz, U.; Nielsen, K.; Edwards, K.; Hasson, H.; Ipsen, C.; Savage, C.; Abildgaard, J.S.; Richter, A.; Lornudd, C.; Mazzocato, P.; et al. How to design, implement and evaluate organizational interventions for maximum impact: The Sigtuna Principles. Eur. J. Work Organ. Psychol. 2020, 1–13. [Google Scholar] [CrossRef]
- Nielsen, K.; Randall, R.; Albertsen, K. Participants’ appraisals of process issues and the effects of stress management interventions. J. Organ. Behav. Int. L. Ind. Occup. Organ. Psychol. Behav. 2007, 28, 793–810. [Google Scholar] [CrossRef]
- Tompa, E.; Culyer, A.J.; Dolinschi, R. Economic Evaluation of Interventions for Occupational Health and Safety: Developing Good Practice; Oxford University Press: Oxford, UK, 2008. [Google Scholar]
- Van Dongen, J.M.; van Wier, M.F.; Tompa, E.; Bongers, P.M.; van der Beek, A.J.; van Tulder, M.W.; Bosmans, J.E. Trial-Based Economic Evaluations in Occupational Health. J. Occup Environ. Med. 2014, 56, 563–572. [Google Scholar] [CrossRef] [PubMed]
- Kessler, R.C.; Ames, M.; Hymel, P.A.; Loeppke, R.; McKenas, D.K.; Richling, D.; Stang, P.E.; Üstün, T.B. Using the WHO Health and Work Performance Questionnaire (HPQ) to evaluate the indirect workplace costs of illness. J. Occup. Environ. Health 2004, 46, S23–S37. [Google Scholar]
- Olsson, T.M. Comparing top-down and bottom-up costing approaches for economic evaluation within social welfare. Eur. J. Health Econ. 2011, 12, 445–453. [Google Scholar] [CrossRef]
- Van Lier, L.I.; Bosmans, J.E.; van Hout, H.P.J.; Mokkink, L.B.; van den Hout, W.B.; de Wit, G.A.; Dirksen, C.D.; Nies, H.L.G.R.; Hertogh, C.M.P.M.; van der Roest, H.G. Consensus-based cross-European recommendations for the identification, measurement and valuation of costs in health economic evaluations: A European Delphi study. Eur. J. Health Econ. 2018, 19, 993–1008. [Google Scholar] [CrossRef]
- Nielsen, K.; Randall, R.; Holten, A.-L.; González, E.R. Conducting organizational-level occupational health interventions: What works? Work Stress 2010, 24, 234–259. [Google Scholar] [CrossRef]
- Schneider, A.; Wehler, M.; Wigl, M. Effects of work conditions on provider mental well-being and quality care: A mixed-methods intervention study in the emergency department. BMC Emerg. Med. 2019, 19, 1–12. [Google Scholar] [CrossRef]
- Bowling, N.A.; Beehr, T.A.; Grebner, S. Combating stress in organizations. In International Review of Industrial and Organizational Psychology; Hodgkinson, G.P., Ford, J.K., Eds.; John Wiley & Sons, Ltd.: Chichester, UK, 2012; pp. 65–87. [Google Scholar]
- Daniels, K.; Gedikli, C.; Watson, D.; Semkina, A.; Vaughn, O. Job desing, employment practices and well-being: A systematic review of intervention studies. Ergonomics 2017, 60, 1177–1196. [Google Scholar] [CrossRef]
- Figureoa, C.A.; Aguilera, A. The need for a Mental Health Technology revolution in the COVID-19 pandemic. Front. Psychiat. 2020, 11. [Google Scholar] [CrossRef]
- Blake, H.; Bermingham, F.; Johnson, G.; Tabner, A. Mitigating the psychological impact of COVID-19 on healthcare workers: A digital learning package. Int. J. Environ. Res. Public Health. 2020, 17, 2997. [Google Scholar] [CrossRef] [PubMed]
- Elder, E.G.; Johnston, A.; Wallis, M.; Crilly, J. Work-based strategies/interventions to ameliorate stressors and foster coping for clinical staff working in emergency departments: A scoping review of the literature. Australas. Emerg. Care 2020, 23, 181–192. [Google Scholar] [CrossRef]
- Nielsen, K.; Stage, M.; Abildgaard, J.S.; Brauer, C.V. Participatory intervention from an organizational perspective: Employees as active agents in creating a healthy work environment. In Salutogenic Organizations and Change; Bauer, G.F., Jenny, G.J., Eds.; Springer: Dordrecht, The Netherlands, 2014; pp. 327–350. [Google Scholar]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
De Angelis, M.; Giusino, D.; Nielsen, K.; Aboagye, E.; Christensen, M.; Innstrand, S.T.; Mazzetti, G.; van den Heuvel, M.; Sijbom, R.B.L.; Pelzer, V.; et al. H-WORK Project: Multilevel Interventions to Promote Mental Health in SMEs and Public Workplaces. Int. J. Environ. Res. Public Health 2020, 17, 8035. https://doi.org/10.3390/ijerph17218035
De Angelis M, Giusino D, Nielsen K, Aboagye E, Christensen M, Innstrand ST, Mazzetti G, van den Heuvel M, Sijbom RBL, Pelzer V, et al. H-WORK Project: Multilevel Interventions to Promote Mental Health in SMEs and Public Workplaces. International Journal of Environmental Research and Public Health. 2020; 17(21):8035. https://doi.org/10.3390/ijerph17218035
Chicago/Turabian StyleDe Angelis, Marco, Davide Giusino, Karina Nielsen, Emmanuel Aboagye, Marit Christensen, Siw Tone Innstrand, Greta Mazzetti, Machteld van den Heuvel, Roy B.L. Sijbom, Vince Pelzer, and et al. 2020. "H-WORK Project: Multilevel Interventions to Promote Mental Health in SMEs and Public Workplaces" International Journal of Environmental Research and Public Health 17, no. 21: 8035. https://doi.org/10.3390/ijerph17218035
APA StyleDe Angelis, M., Giusino, D., Nielsen, K., Aboagye, E., Christensen, M., Innstrand, S. T., Mazzetti, G., van den Heuvel, M., Sijbom, R. B. L., Pelzer, V., Chiesa, R., & Pietrantoni, L. (2020). H-WORK Project: Multilevel Interventions to Promote Mental Health in SMEs and Public Workplaces. International Journal of Environmental Research and Public Health, 17(21), 8035. https://doi.org/10.3390/ijerph17218035










