The Effects of Upper-Body Exoskeletons on Human Metabolic Cost and Thermal Response during Work Tasks—A Systematic Review
Abstract
1. Introduction
- With regard to metabolic aspects, do exoskeletons add physiological strain? Do they increase the metabolic cost of workers during tasks involving the trunk or overhead work?
- With regard to thermal aspects, has the thermal impact already been investigated? If so, do exoskeletons have an impact on the worker’s thermophysiological response? Furthermore, can exoskeletons guarantee thermal comfort for the workers during their activities?
- Describe the state-of-the-art recent studies that have investigated the metabolic cost of upper-body exoskeletons (UBEs) for tasks involving the trunk and overhead work during their use in order to understand if they add a metabolic load;
- Understand if the possible thermal impact of exoskeletons on workers and the aspects related to their thermal comfort have been investigated before.
- A descriptive analysis of their characteristics (Section 3.1.2);
- An assessment of the potential risk of bias for the selected studies included in this review (Section 3.1.3);
- The findings of each selected study, distinguishing the back-support exoskeletons (BSEs) during tasks involving the trunk from the upper-limb support exoskeletons (ULSEs) during overhead tasks (Section 3.1.4).
2. Materials and Methods
2.1. Literature Search Strategy
- For metabolic aspects, 1st group: “exoskeleton”, ”wearable assistive device”, “passive exoskeleton”, “active exoskeleton”, “trunk exoskeleton”, “upper extremity exoskeleton”, “upper limb exoskeleton”, “exosuit”, “lifting”, “overhead work”;
- For metabolic aspects, 2nd group: “oxygen consumption”, “oxygen volume”, “metabolic cost”, “metabolic energy”, “metabolism”;
- For thermal aspects, 1st group: “exoskeleton”, ”wearable assistive device”, “passive exoskeleton”, “active exoskeleton”, “trunk exoskeleton”, “upper extremity exoskeleton”, “upper limb exoskeleton”, “exosuit”;
- For thermal aspects, 2nd group: “thermal comfort”, “comfort”, “human body temperature”, “thermophysiological response”, “thermal stress”, “stress”, “discomfort”, “local temperature”.
2.2. Screening Criteria
2.3. Eligibility Criteria
- For metabolic aspects, studies without metabolic investigations—i.e., measurements of oxygen consumption;
- For thermal aspects, studies without measurements of the core or skin temperatures.
2.4. Data Extraction
- Characteristics of the subjects involved in the study (number of subjects, gender, age, height, weight);
- Intervention measurement details (type of exoskeleton, experimental setup for the trail performed with the exoskeleton);
- Comparison measurement details (experimental setup for the trials performed without the exoskeleton);
- Outcome data when reported. Other outcome parameters provided in the studies were reported for completeness.
2.5. Assessment of Bias
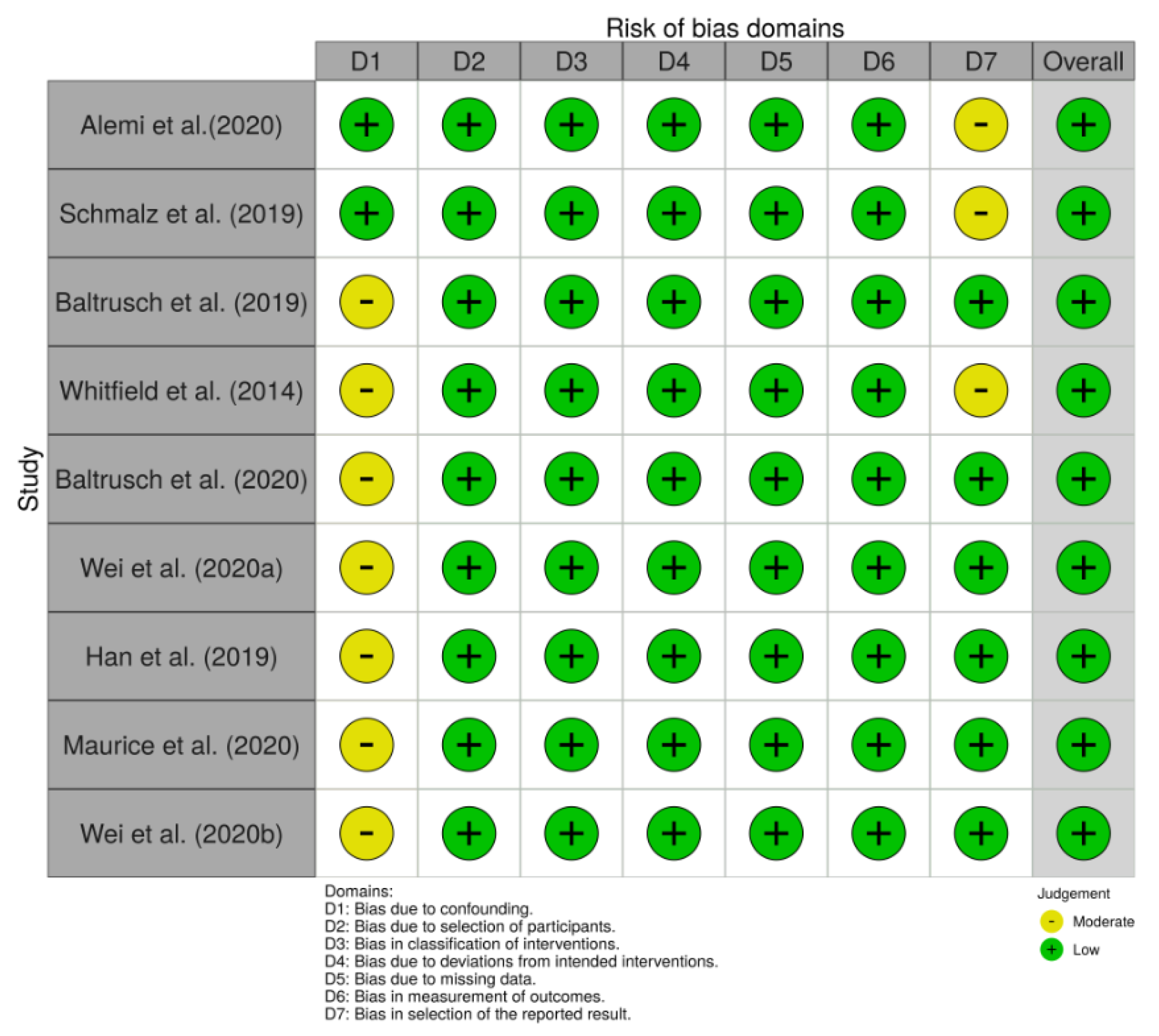
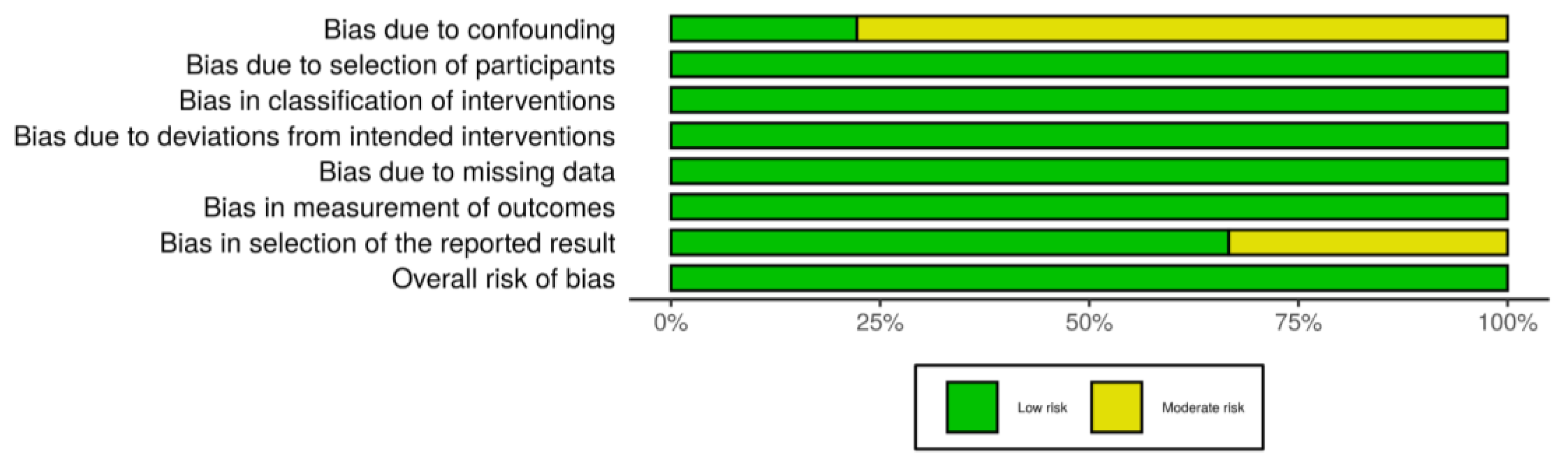
- confounding (D1);
- selection of participants into study (D2);
- classification of interventions (D3);
- deviation from the intended study (D4);
- missing data (D5);
- measurement of outcomes (D6);
- selection of the reported result (D7).
3. Results
3.1. Metabolic Aspects
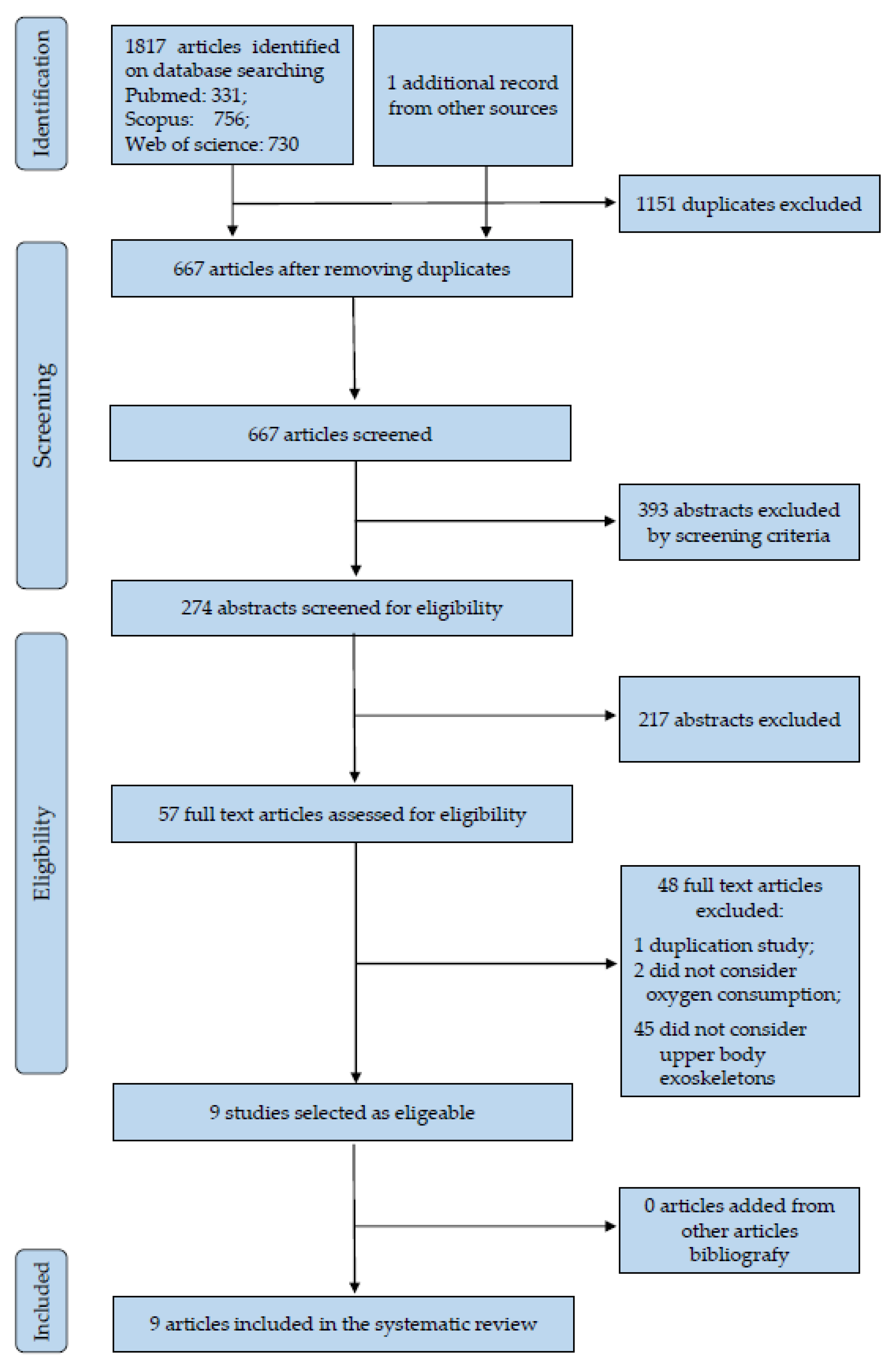
3.1.1. Study Selection
3.1.2. Characteristics of the Studies
3.1.3. Risk of Bias
3.1.4. The Effect of the Upper-Body Exoskeletons on the Metabolic Cost
The Outcome Parameters
The Effects of the BSEs during Tasks Involving the Trunk
The Effects of the ULSEs during Overhead Tasks.
3.2. Thermal Aspects
Study Selection
4. Discussion
Limitation of the Present Systematic Review
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Standard Terminology for Exoskeletons and Exosuits. Available online: https://www.doc88.com/p-4179155217046.html (accessed on 2 March 2020).
- Howard, J.; Murashov, V.V.; Lowe, B.D.; Lu, M.L. Industrial exoskeletons: Need for intervention effectiveness research. Am. J. Ind. Med. 2020, 63, 201–208. [Google Scholar] [CrossRef]
- Voilque, A.; Masood, J.; Fauroux, J.; Sabourin, L.; Guezet, O. Industrial Exoskeleton Technology: Classification, Structural Analysis, and Structural Complexity Indicator. In Proceedings of the 2019 Wearable Robotics Association Conference (WearRAcon), Scottsdale, AZ, USA, 26–28 March 2019; pp. 13–20. [Google Scholar]
- Gopura, R.A.R.C.; Kiguchi, K. Mechanical designs of active upper-limb exoskeleton robots: State-of-the-art and design difficulties. In Proceedings of the 2009 IEEE International Conference on Rehabilitation Robotics, Kyoto, Japan, 23–26 June 2009; pp. 178–187. [Google Scholar]
- De Looze, M.P.; Bosch, T.; Krause, F.; Stadler, K.S.; O’Sullivan, L.W. Exoskeletons for industrial application and their potential effects on physical work load. Ergonomics 2015, 59, 671–681. [Google Scholar] [CrossRef]
- Viteckova, S.; Kutílek, P.; Jirina, M. Wearable lower limb robotics: A review. Biocybern. Biomed. Eng. 2013, 33, 96–105. [Google Scholar] [CrossRef]
- Huo, W.; Mohammed, S.; Moreno, J.C.; Amirat, Y. Lower Limb Wearable Robots for Assistance and Rehabilitation: A State of the Art. IEEE Syst. J. 2014, 10, 1068–1081. [Google Scholar] [CrossRef]
- Gams, A.; Petrič, T.; Debevec, T.; Babic, J. Effects of Robotic Knee Exoskeleton on Human Energy Expenditure. IEEE Trans. Biomed. Eng. 2013, 60, 1636–1644. [Google Scholar] [CrossRef] [PubMed]
- Ranavolo, A.; Mari, S.; Conte, C.; Serrao, M.; Silvetti, A.; Iavicoli, S.; Draicchio, F. A new muscle co-activation index for biomechanical load evaluation in work activities. Ergonomics 2015, 58, 966–979. [Google Scholar] [CrossRef]
- Marras, W.S.; Lavender, S.A.; Ferguson, S.A.; Splittstoesser, R.E.; Yang, G. Quantitative Dynamic Measures of Physical Exposure Predict Low Back Functional Impairment. Spine 2010, 35, 914–923. [Google Scholar] [CrossRef] [PubMed]
- Marras, W.S.; Lavender, S.A.; Ferguson, S.A.; Splittstoesser, R.E.; Yang, G. Quantitative biomechanical workplace exposure measures: Distribution centers. J. Electromyogr. Kinesiol. 2010, 20, 813–822. [Google Scholar] [CrossRef] [PubMed]
- Granata, K.P.; Marras, W.S. Cost–Benefit of Muscle Cocontraction in Protecting Against Spinal Instability. Spine 2000, 25, 1398–1404. [Google Scholar] [CrossRef]
- Ranavolo, A.; Chini, G.; Silvetti, A.; Mari, S.; Serrao, M.; Draicchio, F. Myoelectric manifestation of muscle fatigue in repetitive work detected by means of miniaturized sEMG sensors. Int. J. Occup. Saf. Ergon. 2017, 24, 464–474. [Google Scholar] [CrossRef]
- Cifrek, M.; Medved, V.; Tonković, S.; Ostojić, S. Surface EMG based muscle fatigue evaluation in biomechanics. Clin. Biomech. 2009, 24, 327–340. [Google Scholar] [CrossRef]
- Moreira-Silva, I.; Azevedo, J.; Rodrigues, S.; Seixas, A.; Jorge, M. Predicting musculoskeletal symptoms in workers of a manufacturing company. Int. J. Occup. Saf. Ergon. 2020, 19, 1–9. [Google Scholar] [CrossRef]
- Bureau of Labor Statistic. Nonfatal Occupational Injuries and Illnesses Requiring Days away from Work. 2015. Available online: https://www.bls.gov/news.release/osh2.nr0.htm (accessed on 2 March 2020).
- European Agency for Safety and Health at Work. Work-Related Musculoskeletal Disorders: Prevalence, Costs and Demographics in the EU; Publications Office of the European Union: Luxembourg, 2019; pp. 1–215. [Google Scholar] [CrossRef]
- GBD 2017 Risk Factor Collaborators. Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks for 195 countries and territories, 1990–2017: A systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018, 392, 1923. [Google Scholar]
- Li, R.Y.M.; Ng, D.P.L. Wearable Robotics, Industrial Robots and Construction Worker’s Safety and Health. In Advances in Human Factors in Robots and Unmanned Systems. AHFE 2017. Advances in Intelligent Systems and Computing; Chen, J., Ed.; Springer: Cham, Switzerland, 2018; Volume 595. [Google Scholar]
- Cho, Y.K.; Kim, K.; Ma, S.; Ueda, J. A Robotic Wearable Exoskeleton for Construction Worker’s Safety and Health. Constr. Res. Congr. 2018, 2018, 19–28. [Google Scholar] [CrossRef]
- Zingman, A.; Earnest, G.S.; Lowe, B.D.; Branche, C.M. Exoskeletons in construction: Will They Reduce or Create Hazards? NIOSH Science Blog; 15 June 2015. Available online: https://blogs.cdc.gov/niosh-science-blog/2017/06/15/exoskeletons-in-construction (accessed on 11 February 2020).
- Spada, S.; Ghibaudo, L.; Gilotta, S.; Gastaldi, L.; Cavatorta, M.P. Investigation into the Applicability of a Passive Upper-limb Exoskeleton in Automotive Industry. Procedia Manuf. 2017, 11, 1255–1262. [Google Scholar] [CrossRef]
- Marino, M. Impacts of Using Passive Back Assist and Shoulder Assist Exoskeletons in a Wholesale and Retail Trade Sector Environment. IISE Trans. Occup. Ergon. Hum. Factors 2019, 7, 281–290. [Google Scholar] [CrossRef]
- Yu, H.; Choi, I.S.; Han, K.-L.; Choi, J.Y.; Chung, G.; Suh, J. Development of a Stand-alone Powered Exoskeleton Robot Suit in Steel Manufacturing. ISIJ Int. 2015, 55, 2609–2617. [Google Scholar] [CrossRef]
- European Agency for Safety and Health at Work. The Impact of using Exoskeletons on Occupational Safety and Health. 2019, pp. 1–10. Available online: https://osha.europa.eu/en/publications/impact-using-exoskeletons-occupational-safety-and-health/view (accessed on 31 January 2020).
- Maurice, P.; Čamernik, J.; Gorian, D.; Schirrmeister, B.; Bornmann, J.; Tagliapietra, L.; Latella, C.; Pucci, D.; Fritzsche, L.; Ivaldi, S.; et al. Objective and Subjective Effects of a Passive Exoskeleton on Overhead Work. IEEE Trans. Neural Syst. Rehabilitation Eng. 2020, 28, 152–164. [Google Scholar] [CrossRef]
- Lefeber, N.; Swinnen, E.; Kerckhofs, E. The immediate effects of robot-assistance on energy consumption and cardiorespiratory load during walking compared to walking without robot-assistance: A systematic review. Disabil. Rehabilitation: Assist. Technol. 2016, 12, 657–671. [Google Scholar] [CrossRef]
- Wu, L.; Xie, S.; Zhang, Z.; Meng, W. Energy Efficiency of Gait Rehabilitation Robot: A Review. In Proceedings of the 2019 IEEE/ASME International Conference on Advanced Intelligent Mechatronics (AIM), Honk Kong, China, 8–12 July 2019; Institute of Electrical and Electronics Engineers (IEEE): Honk Kong, China; pp. 465–470. [Google Scholar]
- Parsons, K. Human Thermal Environments; Informa UK Limited: London, UK, 2014. [Google Scholar]
- Occupational Physiology; Informa UK Limited: London, UK, 2016.
- Ergonomics of the Thermal Environment–Determination of Metabolic Rate; International Organization for Standardization: Geneva, Switzerland, 2004; ISO 8996.
- Moher, D.; Liberati, A.; Tetziaff, J.; Altman, D.G.; The PRISMA Group. Linee guida per il reporting di revisioni sistematiche e meta-analisi: Il PRISMA Statement. Evidence 2015, 7, 1–6. [Google Scholar]
- Grant, M.J.; Booth, A. A typology of reviews: An analysis of 14 review types and associated methodologies. Heal. Inf. Libr. J. 2009, 26, 91–108. [Google Scholar] [CrossRef] [PubMed]
- Leonardo, R. PICO: Model for Clinical Questions. Evid. Based Med. Pract. 2018, 3, 1–2. [Google Scholar]
- Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Handb. Syst. Rev. Interv. 2019. [CrossRef]
- McGuinness, L.A. Robvis: An R Package and Web Application for Visualising Risk-of-bias Assessments. Available online: https://github.com/mcguinlu/robvis (accessed on 17 March 2020).
- Sterne, J.A.; A Hernán, M.; Reeves, B.C.; Savović, J.; Berkman, N.D.; Viswanathan, M.; Henry, D.; Altman, D.G.; Ansari, M.T.; Boutron, I.; et al. ROBINS-I: A tool for assessing risk of bias in non-randomised studies of interventions. BMJ 2016, 355, i4919. [Google Scholar] [CrossRef] [PubMed]
- Alemi, M.M.; Madinei, S.; Kim, S.; Srinivasan, D.; Nussbaum, M.A. Effects of Two Passive Back-Support Exoskeletons on Muscle Activity, Energy Expenditure, and Subjective Assessments During Repetitive Lifting. Hum. Factors J. Hum. Factors Ergon. Soc. 2020, 62, 458–474. [Google Scholar] [CrossRef]
- Schmalz, T.; Schändlinger, J.; Schuler, M.; Bornmann, J.; Schirrmeister, B.; Kannenberg, A.; Ernst, M. Biomechanical and Metabolic Effectiveness of an Industrial Exoskeleton for Overhead Work. Int. J. Environ. Res. Public Health 2019, 16, 4792. [Google Scholar] [CrossRef] [PubMed]
- Baltrusch, S.; Van Dieën, J.H.; Bruijn, S.M.; Koopman, A.S.; Van Bennekom, C.A.M.; Houdijk, H. The effect of a passive trunk exoskeleton on metabolic costs during lifting and walking. Ergonomics 2019, 62, 903–916. [Google Scholar] [CrossRef]
- Whitfield, B.H.; Costigan, P.A.; Stevenson, J.M.; Smallman, C.L. Effect of an on-body ergonomic aid on oxygen consumption during a repetitive lifting task. Int. J. Ind. Ergon. 2014, 44, 39–44. [Google Scholar] [CrossRef]
- Baltrusch, S.J.; Van Dieën, J.H.; Koopman, A.S.; Näf, M.B.; Rodriguez-Guerrero, C.; Babič, J.; Houdijk, H. SPEXOR passive spinal exoskeleton decreases metabolic cost during symmetric repetitive lifting. Eur. J. Appl. Physiol. 2019, 120, 401–412. [Google Scholar] [CrossRef]
- Wei, W.; Wang, W.; Qu, Z.; Gu, J.; Lin, X.; Yue, C. The effects of a passive exoskeleton on muscle activity and metabolic cost of energy. Adv. Robot. 2020a, 34, 19–27. [Google Scholar] [CrossRef]
- Han, M.; Li, T.; Wang, S.; Ma, T.; Ai, N. Design of a booster exoskeleton for lumbar spine protection of physical workers. In Proceedings of the 2019 IEEE International Conference on Mechatronics and Automation (ICMA), Tianjin, China, 4–7 August 2019; Institute of Electrical and Electronics Engineers (IEEE): Tianjin, China; pp. 1525–1529. [Google Scholar]
- Wei, W.; Zha, S.; Xia, Y.; Gu, J.; Lin, X. A Hip Active Assisted Exoskeleton That Assists the Semi-Squat Lifting. Appl. Sci. 2020, 10, 2424. [Google Scholar] [CrossRef]
- Brockway, J.M. Derivation of formulae used to calculate energy expenditure in man. Hum. Nutr. Clin. Nutr. 1987, 41, 463–471. [Google Scholar] [PubMed]
- Kipp, S.; Byrnes, W.C.; Kram, R. Calculating metabolic energy expenditure across a wide range of exercise intensities: The equation matters. Appl. Physiol. Nutr. Metab. 2018, 43, 639–642. [Google Scholar] [CrossRef] [PubMed]
- Garby, L.; Astrup, A. The relationship between the respiratory quotient and the energy equivalent of oxygen during simultaneous glucose and lipid oxidation and lipogenesis. Acta Physiol. Scand. 1987, 129, 443–444. [Google Scholar] [CrossRef] [PubMed]
- Ajoudani, A.; Albrecht, P.; Bianchi, M.; Cherubini, A.; Del Ferraro, S.; Fraisse, P.; Fritzsche, L.; Garabini, M.; Ranavolo, A.; Rosen, P.H.; et al. Smart Collaborative Systems for Enabling Flexible and Ergonomic Work Practices [Industry Activities]. IEEE Robot. Autom. Mag. 2020, 27, 169–176. [Google Scholar] [CrossRef]
- Lamers, E.P.; Yang, A.; Zelik, K.E. Feasibility of a Biomechanically-Assistive Garment to Reduce Low Back Loading During Leaning and Lifting. IEEE Trans. Biomed. Eng. 2018, 65, 1674–1680. [Google Scholar] [CrossRef]
- Lotz, C.A.; Agnew, M.J.; Godwin, A.A.; Stevenson, J.M. The effect of an on-body personal lift assist device (PLAD) on fatigue during a repetitive lifting task. J. Electromyogr. Kinesiol. 2009, 19, 331–340. [Google Scholar] [CrossRef]
- Alemi, M.M.; Geissinger, J.; Simon, A.A.; Chang, S.E.; Asbeck, A.T. A passive exoskeleton reduces peak and mean EMG during symmetric and asymmetric lifting. J. Electromyogr. Kinesiol. 2019, 47, 25–34. [Google Scholar] [CrossRef]
- Bosch, T.; Van Eck, J.; Knitel, K.; De Looze, M. The effects of a passive exoskeleton on muscle activity, discomfort and endurance time in forward bending work. Appl. Ergon. 2016, 54, 212–217. [Google Scholar] [CrossRef]
- Frost, D.M.; Abdoli-E, M.; Stevenson, J.M. PLAD (personal lift assistive device) stiffness affects the lumbar flexion/extension moment and the posterior chain EMG during symmetrical lifting tasks. J. Electromyogr. Kinesiol. 2009, 19, e403–e412. [Google Scholar] [CrossRef]
- Muramatsu, Y.; Kobayashi, H.; Sato, Y.; Jiaou, H.; Hashimoto, T.; Kobayashi, H. Quantitative Performance Analysis of Exoskeleton Augmenting Devices—Muscle Suit—for Manual Worker. Int. J. Autom. Technol. 2011, 5, 559–567. [Google Scholar] [CrossRef]
- Imamura, Y.; Tanaka, T.; Suzuki, Y.; Takizawa, K.; Yamanaka, M. Analysis of Trunk Stabilization Effect by Passive Power-Assist Device. J. Robot. Mechatronics 2014, 26, 791–798. [Google Scholar] [CrossRef]
- Graham, R.B.; Agnew, M.J.; Stevenson, J.M. Effectiveness of an on-body lifting aid at reducing low back physical demands during an automotive assembly task: Assessment of EMG response and user acceptability. Appl. Ergon. 2009, 40, 936–942. [Google Scholar] [CrossRef] [PubMed]
- Huysamen, K.; De Looze, M.; Bosch, T.; Ortiz, J.; Toxiri, S.; O’Sullivan, L.W. Assessment of an active industrial exoskeleton to aid dynamic lifting and lowering manual handling tasks. Appl. Ergon. 2018, 68, 125–131. [Google Scholar] [CrossRef]
- Näf, M.B.; Koopman, A.S.; Baltrusch, S.; Rodriguez-Guerrero, C.; VanderBorght, B.; Lefeber, D. Passive Back Support Exoskeleton Improves Range of Motion Using Flexible Beams. Front. Robot. AI 2018, 5, 72. [Google Scholar] [CrossRef]
- Zhang, H.; Kadrolkar, A.; Sup, F.C. Design and Preliminary Evaluation of a Passive Spine Exoskeleton. J. Med. Devices 2015, 10, 011002. [Google Scholar] [CrossRef]
- Weston, E.B.; Alizadeh, M.; Knapik, G.G.; Wang, X.; Marras, W.S. Biomechanical evaluation of exoskeleton use on loading of the lumbar spine. Appl. Ergon. 2018, 68, 101–108. [Google Scholar] [CrossRef]
- Kim, S.; Nussbaum, M.A.; Mokhlespour Esfahani, M.I.; Alemi, M.M.; Alabdulkarim, S.; Rashedi, E. Assessing the influence of a passive, upper extremity exoskeletal vest for tasks requiring arm elevator: Part I–“Expected “effects on discomfort, shoulder muscle activity, and work task performance. Appl. Ergon. 2018, 70, 315–322. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Noguera, F.; Retolaza, I.; Pujana-Arrese, A.; Cenitagoya, A.; Basurko, J.; Landaluze, J. Design of a five actuated DoF upper limb exoskeleton oriented to workplace help. In Proceedings of the 2008 2nd IEEE RAS & EMBS International Conference on Biomedical Robotics and Biomechatronics, Scottsdale, AZ, USA, 19–22 October 2008; Institute of Electrical and Electronics Engineers (IEEE): Scottsdale, AZ, USA, 2008; pp. 169–174. [Google Scholar]
- Hara, H.; Sankai, Y. Development of HAL for Lumbar Support. In Proceedings of the SCIS &ISIS, Okayama, Japan, 8–12 December 2020. [Google Scholar]
- Lee, H.; Lee, B.; Kim, W.; Gil, M.; Han, J.; Han, C. Human-robot cooperative control based on pHRI (Physical Human-Robot Interaction) of exoskeleton robot for a human upper extremity. Int. J. Precis. Eng. Manuf. 2012, 13, 985–992. [Google Scholar] [CrossRef]
- O’Sullivan, L.; Nugent, R.; Van Der Vorm, J. Standards for the Safety of Exoskeletons Used by Industrial Workers Performing Manual Handling Activities: A Contribution from the Robo-Mate Project to their Future Development. Procedia Manuf. 2015, 3, 1418–1425. [Google Scholar] [CrossRef]
- Otten, B.M.; Weidner, R.; Argubi-Wollesen, A. Valuation of a Novel Active Exoskeleton for Tasks at or Above Head Level. IEEE Rob. Autom. Lett. 2018, 3, 2408–2415. [Google Scholar] [CrossRef]
- Pacifico, I.; Scano, A.; Guanziroli, E.; Moise, M.; Morelli, L.; Chiavenna, A.; Romo, D.; Spada, S.; Colombina, G.; Molteni, F.; et al. An Experimental Evaluation of the Proto-MATE: A Novel Ergonomic Upper-Limb Exoskeleton to Reduce Workers’ Physical Strain. IEEE Robot. Autom. Mag. 2020, 27, 54–65. [Google Scholar] [CrossRef]
- Ndahimana, D.; Kim, E.-K. Measurement Methods for Physical Activity and Energy Expenditure: A Review. Clin. Nutr. Res. 2017, 6, 68–80. [Google Scholar] [CrossRef] [PubMed]
- Ranavolo, A.; Varrecchia, T.; Rinaldi, M.; Silvetti, A.; Serrao, M.; Conforto, S.; Draicchio, F. Mechanical lifting energy consumption in work activities designed by means of the “revised NIOSH lifting equation”. Ind. Health 2017, 55, 444–454. [Google Scholar] [CrossRef] [PubMed]
- Ranavolo, A.; Varrecchia, T.; Iavicoli, S.; Marchesi, A.; Rinaldi, M.; Serrao, M.; Conforto, S.; Cesarelli, M.; Draicchio, F. Surface electromyography for risk assessment in work activities designed using the “revised NIOSH lifting equation”. Int. J. Ind. Ergon. 2018, 68, 34–45. [Google Scholar] [CrossRef]
- Ranavolo, A.; Draicchio, F.; Varrecchia, T.; Silvetti, A.; Iavicoli, S. Erratum: Alberto, R. et al., Wearable Monitoring Devices for Biomechanical Risk Assessment at Work: Current Status and Future Challenges—A Systematic Review. Int. J. Environ. Res. Public Health 2018, 15, 2569. [Google Scholar] [CrossRef] [PubMed]
- Alberto, R.; Draicchio, F.; Varrecchia, T.; Silvetti, A.; Iavicoli, S. Wearable Monitoring Devices for Biomechanical Risk Assessment at Work: Current Status and Future Challenges—A Systematic Review. Int. J. Environ. Res. Public Health 2018, 15, 2001. [Google Scholar]
- Varrecchia, T.; De Marchis, C.; Draicchio, F.; Schmid, M.; Conforto, S.; Ranavolo, A. Lifting Activity Assessment Using Kinematic Features and Neural Networks. Appl. Sci. 2020, 10, 1989. [Google Scholar] [CrossRef]
- Varrecchia, T.; De Marchis, C.; Rinaldi, M.; Draicchio, F.; Serrao, M.; Schmid, M.; Conforto, S.; Ranavolo, A. Lifting activity assessment using surface electromyographic features and neural networks. Int. J. Ind. Ergon. 2018, 66, 1–9. [Google Scholar] [CrossRef]
- Del Ferraro, S.; Falcone, T.; Rondinone, B.M.; Molinaro, V. The effect of a power assisted filtering device on the local and whole body thermal response in cold and hot environments. Int. J. Ind. Ergon. 2020, 75, 102895. [Google Scholar] [CrossRef]
- Del Ferraro, S.; Falcone, T.; Tombolini, F.; Rondinone, B.M.; Molinaro, V. Thermophysiological simulations with Newton manikin equipped with a power assisted filtering device in cold environments. J. Therm. Biol. 2018, 78, 320–328. [Google Scholar] [CrossRef] [PubMed]
- Del Ferraro, S.; Tombolini, F.; Plebani, C.; Molinaro, V. Thermophysiological response of Newton manikin equipped with power-assisted filtering device incorporating a full-face mask in hot environment. Int. J. Hyperth. 2017, 33, 717–723. [Google Scholar] [CrossRef] [PubMed]
| Ref. | Population | Intervention (WEC) | Comparison (WOEC) | Outcome | ||||
|---|---|---|---|---|---|---|---|---|
| Author (year) | Subjects Involved in the Study | Task | Exoskeleton Tested | Experimental Setup | Experimental Setup | Metabolic Measured Parameters | Metabolic Results Considered | Other Results Reported |
| Alemi et al. (2020) [38] | 18 young subjects (9 M, 9 F) age: M: 24.4 ± 4.5 y F: 25.1 ± 3.8 y height: M: 176.5 ± 5.5 cm F: 167.4 ± 3.5 cm BM: M: 78.5 ± 7.0 kg F: 67.6 ± 9.4 kg BMI: M: 25.2 ± 2.7 kg/m2 F: 24.1 ± 3.4 kg/m2 | Repetitive lifting | SuitX Laevo V2.5 | Trial: cycle of lifting/lowering a 6.8 kg panel for 5 min; f: 5 lifting/lowering cycles per min. For each exoskeleton, four conditions were tested which combine:
| Trial: cycle of lifting/lowering a panel for 5 min; f: 5 lifting/lowering cycles per min. Four conditions were tested which combine:
| EER, PCEE | sEMG: peak activity of normalized signals from trunk, lower, and upper limb muscles; perceived discomfort and balance; overall usability. | |
| Schmalz et al. (2019) [39] | 12 healthy subjects (6 M, 6 F) age: 24 ± 3 y height: 176 ± 15 cm weight: 73 ± 15 kg Subjects were divided in 2 groups (G1, G2) | Overhead working | PAEXO | Sequence of sessions G1: WE+B+WOE+B+WE. Sequence of sessions G2: WOE+B+WE+B+WOE. Each session WE was a sequence of 2 tasks (T1, T2) of 5 min with a break of 10 min. T1: screwing nuts continuously; T2: drilling using an electric drill. The order of T1 and T2 was chosen randomly. B is of 30 min. G1 performs 2 WE sessions. G2 performs 1 WE session. | Each WOE is a sequence of 2 tasks (T1, T2) of 5 min with a break of 10 min. T1: screwing nuts continuously; T2: drilling using an electric drill. G1 performs 1 WOE session. G2 performs 2 WOE session. | Kinematics: shoulder and elbow angles; sEMG: amplitude and Muscle Fatigue Index from trunk and upper limb muscles. | ||
| Baltrusch et al. (2019) [40] | 13 M subjects for WT 11 M subjects for LT age: 28.9 ± 4.4 y height: 180 ± 4 cm weight: 76.9 ± 12.0 kg | Walking, Repetitive lifting | Laevo HC Laevo LC | WT: 5 min of walking on treadmill with Laevo LC at PWS and PWSX. 2 trials for each subject. LT: cycle of lifting/lowering a 10-kg box; f: 6 lifting/lowering cycles per min. LT was performed for Laevo HC and LC and from 2 heights: ankle and knee height. 4 trials for each subject. 30 s of rest between each trial. | WT: 5 min of walking on treadmill at PWS and PWSX. 2 trials for each subject. LT: cycle of lifting/lowering a 10-kg box; f: 6 lifting/lowering cycles per min. LT was performed from 2 heights: ankle and knee height. 2 trials for each subject. 30 s of rest between each trial. | Kinematics: knee, hip, lumbar flexio-extension and trunk inclination ROM; ROM of the body COM. sEMG: normalized signals from trunk and lower limb muscles. | ||
| Whitfield et al. (2014) [41] | 15 M subjects age: 22.1 ± 2.6 y height: 1.81 ± 0.08 m weight: 81.6±9.2 kg | Repetitive lifting | PLAD | LT: cycle of lifting/lowering a box (average weight 8.9 ± 1.6kg) for 15 min; f: 6 lifting/lowering cycles per min. | LT: cycle of lifting/lowering a 8.9-kg box for 15 min; f: 6 lifting/lowering cycles per min. | Kinematics: maximum knee flexion angles. sEMG: normalized sEMG signals from lower limb muscles. | ||
| Baltrusch et al. (2020) [42] | 11 M employees of KLM age: 47.4 ± 7.1 y height: 175 ± 7.0 cm weight: 84.6 ± 15 kg (finally 10 M were considered because one failed). Enrolled subjects with and without a history of LBP | Symmetric repetitive lifting | SPEXOR | LT: cycle of lifting/lowering a 10-kg box from ankle height to hip height for 5 min; f: 8 lifting/lowering cycles per min. | LT: cycle of lifting/lowering a 10-kg box from ankle height to hip height for 5 min; f: 8 lifting/lowering cycles per min. | Kinematics: knee, hip, trunk and L5-S1 flexion-extension angles; Range of motion of COM; Mechanical work generated at knee, hip, trunk and L5-S1 joint. sEMG: normalized signal from trunk muscles. | ||
| Wei et al. (2020a) [43] | 8 M subjects age: 24.4 ± 2.54 y height: 172.1 ± 5.89 cm weight: 65.25 ± 6.98 kg | Static holding posture | MeBot-EXO (passive device) | SST: forward trunk flexion at an angle of 50–55 degrees and this stooping position is held for 5 min. Each SST was repeated three times. | SST: forward trunk flexion at an angle of 50–55 degrees and this stooping position is held for 5 min. Each SST was repeated three times. | sEMG: RMS of normalized signals from trunk muscles. | ||
| Han et al. (2019) [44] | 3 subjects age: (1) height: (1) weight: (1) | Repetitive lifting | Passive energy-storing booster exoskeleton | LT: 20 cycles of lifting/lowering a 9-kg object. Three LT for each subject. f not considered. | ? | |||
| Maurice et al. (2020) [26] | 12 M subjects age: 23.4 ± 1.2 y height: 179.3 ± 5.9 cm weight: 72.7 ± 5.4 kg | Overhead working | PAEXO | Overhead pointing task: moving the power drill as far as possible from a starting point to a target and remain on the target for 2 s. Session: 5 blocks of 24 pointing movement each with a break of 30 s between blocks. | Overhead pointing task: moving the power drill as far as possible from a starting point to a target and remain on the target for 2 s. Session: 5 blocks of 24 pointing movements, each with a break of 30 s between blocks. | sEMG: RMS of normalized signals from shoulder and trunk muscles. Kinetics: RMS of the CoP displacement and velocity; Duration of movement. Kinematics: temporal profiles and maximum joint angles of the shoulder, elbow, lower back and hip. | ||
| Wei et al. (2020b) [45] | 7 M for the sEMG measurement. 3 M subjects for the metabolic measurement age: 24 ± 3 y height: 170 ± 5 cm weight: 70 ± 5 kg | Repetitive semi-squat lifting | MeBot-EXO (active device) | LT: carrying an 8 kg weight from the ground back and forward to a platform at a height 0.5 m for 5 min. Three LT for each subject. f not declared. | LT: carrying an 8 kg weight from the ground back and forward to a platform at a height 0.5 m for 5 min. Three LT for each subject. f not declared. | ? | EC | Kinematics: temporal profiles of hip (right and left) and back angles. sEMG: RMS of rectified signals from trunk muscles. |
| Outcome Measure | Unit | Description and/or Calculation | Reference |
|---|---|---|---|
| EER | Kcal/min*kg | Energy expenditure rate estimated using the Brockway equation (1987) [46], reported as in [47]. Alemi et al. [38] considered the mean value over the last 2 min of each trial, normalized with respect to the mass. Authors highlighted that this approach accounts for both the participant body mass and the mass of a BSE (if used). | Alemi et al. 2020 [38] |
| PCEE | % | Percentage changes in energy expenditure considering WEC vs. WOEC. | |
| ml/min*kg | Oxygen consumption rate at rest, mean value over the last minute before starting T1 or T2, normalized with respect to the body mass. | Schmalz et al. 2019 [39] | |
| ml/min*kg | Oxygen consumption rate of T1, mean value over the last minute of the task, normalized with respect to the body mass. | ||
| ml/min*kg | Oxygen consumption rate of T2, mean value over the last minute of the task, normalized with respect to the body mass. | ||
| beat/min | Heart rate at rest, mean value over the last minute before starting T1 or T2. | ||
| beat/min | Heart rate of T1, mean value over the last minute of the task. | ||
| beat/min | Heart rate of T2, mean value over the last minute of the task. | ||
| W/kg | Net metabolic cost was calculated by subtracting the resting metabolic cost from the total metabolic rate during lifting from knee height with Laevo LC. The metabolic cost of lifting was estimated using the Garby and Astrup equation [48] for the energetic expenditure, reported as in [47]. Flow rates were averaged over the last 2 min of the trial and were normalized to the body mass. | Baltrush et al. (2019) [40] | |
| % | Percentage of reduction in metabolic cost between WEC and WOEC for lifting from knee height, with the Laevo LC. | ||
| W/kg | Net metabolic cost was calculated by subtracting the resting metabolic cost from the total metabolic rate during lifting from knee height with Laevo HC. The metabolic cost of lifting was estimated using the Garby and Astrup equation [48] for the energetic expenditure, reported as in [47]. Flow rates were averaged over the last 2 min of the trial and were normalized to the body mass. | ||
| % | Percentage of reduction in metabolic cost between WEC and WOEC for lifting from knee height with the Laevo HC. | ||
| W/kg | Net metabolic cost was calculated by subtracting the resting metabolic cost from the total metabolic rate during lifting from ankle height with the Laevo LC. The metabolic cost of lifting was estimated using the Garby and Astrup equation [48] for the energetic expenditure, reported as in [47]. Flow rates were averaged over the last 2 min of the trial and were normalized to the body mass. | ||
| % | Percentage of reduction in metabolic cost between WEC and WOEC for lifting from ankle height with the Laevo LC. | ||
| W/kg | Net metabolic cost was calculated by subtracting the resting metabolic cost from the total metabolic rate during lifting from ankle height with the Laevo HC. The metabolic cost of lifting was estimated using the Garby and Astrup equation [48] for the energetic expenditure, reported as in [47]. Flow rates were averaged over the last 2 min of the trial and were normalized to the body mass. | ||
| % | Percentage of reduction in metabolic cost between WEC and WOEC for lifting from ankle height with the Laevo HC. | ||
| J/m*kg | The metabolic cost of walking with and without Laevo LC at PSW was estimated using the Garby and Astrup equation [48] for the energetic expenditure, reported as in [47]. Flow rates were averaged over the last 2 min of the trial. Metabolic cost was normalized to the body mass and the walking speed. | ||
| J/m*kg | The metabolic cost of walking with and without the Laevo LC at PSWX was estimated using the Garby and Astrup equation [48] for the energetic expenditure, reported as in [47]. Flow rates were averaged over the last 2 min of the trial. Metabolic cost was normalized to the body mass and the walking speed. | ||
| ml/kg*min | Average oxygen consumption, normalized by weight. | Whitfield et al. (2014) [41] | |
| Beat/min | Heart rate. | ||
| W/kg | Net metabolic cost was calculated by subtracting the resting metabolic cost from the total metabolic rate during lifting. The total metabolic cost of lifting from ankle to hip height with SPEXOR was estimated using the Garby and Astrup equation [48] for the energetic expenditure, reported as in [47]. Flow rates were averaged over the last 2 min of the trial and normalized with respect to the body mass. | Baltrush et al. (2020) [42] | |
| % | Percentage of reduction in metabolic cost between WEC and WOEC for lifting. | ||
| Kcal/min*kg | Median metabolic cost of energy (1) during static holding posture normalized by weight. | Wei et al., (2020a) [43] | |
| RR | l/min | Respiratory rate collected before and after wearing the exoskeleton. | Han et al. (2019) [44] |
| beat/min | Average heart rate before wearing the exoskeleton. | ||
| beat/min | Average heart rate after wearing the exoskeleton. | ||
| ml/kg*min | Average oxygen consumption, normalized by weight. | Maurice et al. (2020) [26] | |
| Average heart rate normalized using the maximum and minimum values of the participant in WOEC. | |||
| Kcal/min*Kg | Metabolic rate for 5 min during continuous manual material handling, normalized by weight. | Wei et al. (2020b) [45] | |
| EC | Kcal | Energy consumption for 5 min during continuous manual material handling. |
| Exoskeleton Condition | Control Condition | ||||||
|---|---|---|---|---|---|---|---|
| Ref. | Outcome | Subject | Exoskeleton | Task | M (SD) | Task | M (SD) |
| Alemi et al. (2020) [38] | EER (Kcal/min*Kg) | 18 (9M, 9F) | Laevo | All trials | 0.07 (0.02) (*) | All trials | 0.075 (0.019) |
| SuitX | 0.068 (0.018) (*) | ||||||
| PCEE (%) | Laevo | All trials | −7.5 | ||||
| SuitX | −8 | ||||||
| Laevo | KA | −5.3 | |||||
| KS | −10.8 | ||||||
| SA | −5.5 | ||||||
| SS | −8.9 | ||||||
| SuitX | KA | −6.2 | |||||
| KS | −9.1 | ||||||
| SA | −3.7 | ||||||
| SS | −12.6 | ||||||
| Schmalz et al. (2019) [39] | (ml/min*Kg) | 12 (6M,6F) | Paexo | rest | 4.1 (2) | rest | 3.9 (2) |
(ml/min*Kg) | T1 | 5.2 (2) (*) | T1 | 5.8 (2) | |||
(ml/min*Kg) | T2 | 6.6 (2) (*) | T2 | 7.4 (2) | |||
(beat/min) | rest | 75 (2) | rest | 74 (2) | |||
(beat/min) | T1 | 98 (2) (*) | T1 | 103 (2) | |||
(beat/min) | T2 | 93 (2) (*) | T2 | 99 (2) | |||
| Baltrush et al. (2019) [40] | (W/kg) (%) | 11 M | Laevo LC | LT- knee height | 7 | LT- knee height | 3.09 (0.92) |
(W/kg) (%) | Laevo HC | 2.56 (0.52) (*) 17 (*) | |||||
(W/kg) (%) | Laevo LC | LT- ankle height | 8 | LT-ankle height | 5.06 (1.11) | ||
(W/kg) (%) | Laevo HC | 4.27 (0.6) (*) 16 (*) | |||||
(J/m*kg) | 13 M | Laevo LC | WT-PSW | (1) (increase of 12%) | WT-PSW | (1) | |
(J/m*kg) | Laevo LC | WT-PSWX | (1) (increase of 17%) | WT-PSWX | (1) | ||
| Whitfield et al. (2014) [41] | (ml/kg*min) (beat/min) | 15 M | PLAD | LT | 17.7 (2.6) 116.0 (14.8) | LT | 17.9 (2.4) 117.7 (17.0) |
| Baltrush et al. (2019) [42] | (W/kg) (%) | 10 M | SPEXOR | LT | 4.64 (1.38) (*) 18 | LT | 5.63 (1.26) |
| Wei et al. (2020a) [43] | (Kcal/min*Kg) | 8 M | MeBot-EXO | Static holding posture | (2) (*) | Forward torso flexion | (2) |
| Han et al. (2019) [44] | RR (1/min) | 3 subjects | Passive energy-storing booster exoskeleton | LT | 16 | 25 | |
(beat/min) | 94 (*) (after using exoskeleton) | 114 (*) (before using exoskeleton) | |||||
| Maurice et al. (2020) [26] | (ml/kg*min) | 12 M | PAEXO | Overhead pointing task | (2) (*) by 33% | Overhead pointing task | (2) (*) > |
| (2) (*) by 19% | (2) (*) | ||||||
| Wei et al. (2020b) [45] | 3 M | MeBot-EXO | LT | (2) (*) | LT | (2) (*) | |
| EC | 17.9 (maximum value at the 5th minute) | 22.9 (maximum value at the 5th minute) | |||||
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Del Ferraro, S.; Falcone, T.; Ranavolo, A.; Molinaro, V. The Effects of Upper-Body Exoskeletons on Human Metabolic Cost and Thermal Response during Work Tasks—A Systematic Review. Int. J. Environ. Res. Public Health 2020, 17, 7374. https://doi.org/10.3390/ijerph17207374
Del Ferraro S, Falcone T, Ranavolo A, Molinaro V. The Effects of Upper-Body Exoskeletons on Human Metabolic Cost and Thermal Response during Work Tasks—A Systematic Review. International Journal of Environmental Research and Public Health. 2020; 17(20):7374. https://doi.org/10.3390/ijerph17207374
Chicago/Turabian StyleDel Ferraro, Simona, Tiziana Falcone, Alberto Ranavolo, and Vincenzo Molinaro. 2020. "The Effects of Upper-Body Exoskeletons on Human Metabolic Cost and Thermal Response during Work Tasks—A Systematic Review" International Journal of Environmental Research and Public Health 17, no. 20: 7374. https://doi.org/10.3390/ijerph17207374
APA StyleDel Ferraro, S., Falcone, T., Ranavolo, A., & Molinaro, V. (2020). The Effects of Upper-Body Exoskeletons on Human Metabolic Cost and Thermal Response during Work Tasks—A Systematic Review. International Journal of Environmental Research and Public Health, 17(20), 7374. https://doi.org/10.3390/ijerph17207374





