Increasing Rural Recruitment and Retention through Rural Exposure during Undergraduate Training: An Integrative Review
Abstract
1. Introduction
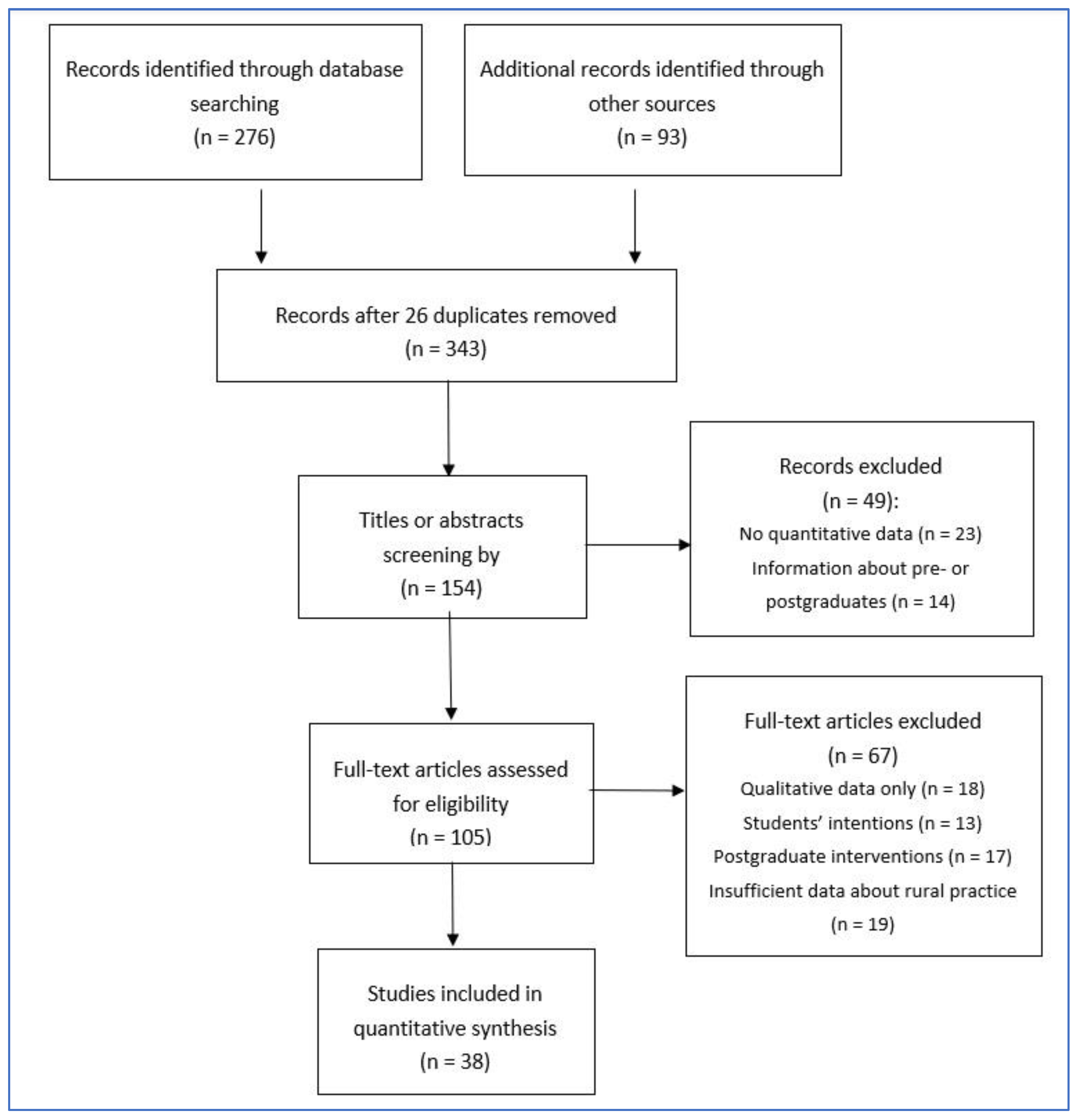
2. Materials and Methods
- Lack of quantitative information on physicians practicing in rural areas after graduation,
- Restriction to student opinions and declarations of intent,
- Provision of purely qualitative information on various aspects of rural tracks,
- Information on the effectiveness of postgraduate interventions,
- Reference to outcomes other than rural practice,
- Mere expressions of opinions and expert perceptions.
3. Results
4. Discussion
5. Limitations
6. Conclusions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Study | Year | Location | Study Type | Intervention Type | Target Group | Students (n) | Outcomes | Findings | Specificity | Quality |
| May et al. [26] | 2018 | New South Wales/Australia | Retrospective cross-sectional cohort study | Extended Rural Clinical School exposure: semester- or year-long rural placement in year 4 and 5 | Domestic medical students graduated between 2012 and 2014 | 171 426 (out of 435 = 98%) | Practice location in under-served district | Rural placement ≥1 year multiplies chance to practice in rural location 3.5 years after graduation by six (OR 6.075, 95%-CI 2.716–13.591) | Fair | + |
| Woolley et al. [28] | 2017 | Philippines | Data-based retrospective cohort control study | 1 month per semester in community placements across years 1–3, followed by 10 months of community placement in year 4 | Medical students at Ateneo de Zamboanga University and University of the Philippines in Manila | 232 graduates in Zamboanga, 121 graduates in Manila. Control cohort: 464 and 264 graduates in medical schools with more conventional curricula | Medical practice in communities <100,000 population; practice in lower-income communities | Practice in smaller communities:
| Fair: Low identification rate of conventionally trained graduates | +– |
| Wheat et al. [25] | 2017 | Alabama/USA | Quasi-experimental nonrandomised control study | Rural Medical School training (as part of the Rural Medical Scholars Programme) | Medical students enrolled between 1997–2002 | 54 rural vs. 182 regional and 649 main campus students | Production of rural physicians | Share of rural practitioners:
| Fair | + |
| Nelson et al. [44] | 2017 | Iowa/USA | Data-based retrospective cohort study | Iowa Family Medicine Training Network | Graduates from Iowa medical schools | 1645 (out of 1676) graduates = 98.2% | Rural location decision and 5-year retention | Likelihood of retention strongly related to undergraduate medical training in Iowa (OR = 6.74. p < 0.001) | Fair | + |
| Wendling et al. [24] | 2016 | Michigan/USA | Retrospective cohort control study | Rural Physician Programme curriculum | Graduates from Michigan University Medical School | 152 rural programme graduates vs. 2230 nonrural graduates | Primary healthcare practice in rural area (acc. to Rural-Urban Commuting Area Code, RUCA) | Rural-programme students more likely than others to practice in
| Fair | + |
| Kondalsamy-Chennakesavan et al. [23] | 2015 | Queensland/Australia | Retrospective comparative cohort study | Undergraduate medical training at Rural Clinical School | Medical students | 754 (out of 1572 = 48%): 236 (31.3%) had a rural background, 276 (36.6%) had attended the University of Queensland (UQRCS). | Current clinical practice in a rural location | Rural clinical practice location: 41.7% (115/276 of Queensland-University attendees) vs. 18.8% (90/478 UQ metropolitan clinical school attendees), p < 0.001. Independent predictors of rural practice: (OR [95%-CI]): Queensland University attendance for 1 year (OR 1.84 [1.21–2.82]) or 2 years (2.71 [1.65–4.45]) Independent predictors of rural practice for interaction between UQRCS attendance and rural background: rural background + UQRCS attendance for 1 year (OR4.44 [2.38–8.29]) or 2 years (7.09 [3.57–14.10])Effects of rural background and UQRCS attendance were duration-dependent. | Fair | + |
| Shires et al. [22] | 2015 | Tasmania/Australia | Comparative data-based cohort study | ≥1 year at Rural Clinical School in smaller city | Medical students in larger cities and at least 1 year in smaller cities | 974 larger-city graduates vs. 202 RCS graduates | Practice location | Rural-clinical-school graduates 5 times as likely to be working in remote areas than control group: 28% vs. 7%, = 59.5, p < 0.0001 (OR 4.9, 95%-CI 3.2–7.6); Monash model: Nine-fold likelihood (OR 9.0, 95%-CI 4.7–17.2) | Fair: not checked for selection bias | + |
| Playford et al. [21] | 2014 | Western Australia | Retrospective control cohort study, logistic regression | ≥1 year at Rural Clinical School (RCS) | Medical students at University of Western Australia | 1017 graduates (out of 1116 = 91%) | Rural vs. urban practice location | Participation in RCSWA strongly associated with greater likelihood of rural practice:
| Fair | + |
| Jamar et al. [33] | 2014 | Southern Australia | Cross-sectional retrospective cohort study based on a 28-question online survey | Rural 5th year during 6-year undergraduate medical program | Former medical students at University of Adelaide | 74 out of 124 (response rate 58.2%) | Practice location in rural area | 20.8%–34.1% of respondents located in a rural area;
| Low | – |
| Woolley et al. [45] | 2014 | Queensland/Australia | Multiple logistic regression analysis using data of a longitudinal cohort study | Medical training at a school in regional area | Medical graduates | 260 (out of 264, response rate 98%) | Practice in a rural town | Prediction by
| Low | +– |
| Gupta et al. [46] | 2014 | Northern Queensland/Australia | Cross-sectional survey via email and telephone communication, and via JCU School of Medicine Facebook | Internship in rural/remote areas | Postgraduate interns across postgraduate years 1 to 7 | 530 (out of 536 = 99%) | Association of later practice location with hometown and internship location | Important association between remoteness area of internship and subsequent rural practice: Likelihood to practice in rural locations: Metropolitan hometown + nonmetropolitan internship > nonmetropolitan hometown + metropolitan internship (OR 6.1 vs. 2.6, p < 0.001) and in inner regional locations (OR 3.1 vs. 1.6, p = 0.003). | High within the selected group | ++ |
| Forster et al. [32] | 2013 | New South Wales/Australia (UNSW) | Cross-sectional retrospective cohort study based on online survey | 1–3 years of undergraduate training at rural clinical school | Medical graduates | 214 (out of 315 = response rate 68%) | Current, preferred current and intended career rural locations | 26% working in rural area Nonrural medicine entry graduates with 3 years at rural campuses more likely to take up rural practice compared to those with 1 year at a rural campus (OR = 8.4, 95%-CI = 2.1–33.5, p = 0.002). OR not significant for 2 vs. 1 year | Low – repeated mix up of current, preferred current and intended rural practice locations | +– |
| Strasser et al. [41] | 2013 | Northern Ontario/Canada | Mixed methods studies to assess socioeconomic impact of medical school through post-graduate tracking | Northern Ontario School of Medicine Comprehensive Community Clerkship | Medical students | 66 | Practice location | 61% of all graduates have chosen predominantly rural family-practice training. 65% of the graduates of the Family Medicine programme practice in Northern Ontario or other rural communities | Low: large overlapping with recruitment strategies | + |
| Eley et al. [31] | 2012 | Queensland/Australia | Longitudinal sequential study via email survey | Undergraduate Rural Clinical School training | Year 4 students | 115 out of 183 = 64% | Practice location | Altogether, 40% working in nonurban locations – high variation (range 0–100%) | Low | +/– |
| Tate and Aoki [20] | 2012 | Manitoba/Canada | Retrospective cross-sectional survey (per mail) | Rural medical education experiences during under- (and postgraduate) medical training | Medical graduates of the University of Manitoba in Winnipeg | 1269 out of 2578 (=49%) | Rural physician practice | Significant association with rural educational exposure during medical school (and residency training) (p = 0.0068): graduates with (partly) undergraduate training in rural settings 1.34 times (95%-CI 1.09 to 1.75) more likely to practise in rural location. Increasing time spent in rural training related to increased likelihood of rural practice | High | + |
| Whitford et al. [43] | 2012 | South Australia | Survey based on indirect, mixed mode of recruitment and a questionnaire (South Australian Allied Health Workforce (SAAHW) survey) | Nonmetropolitan university or college and/or had rural placement | Allied health professionals | 1539 (82% male, 75% in urban practice) (representing 18.3% of potential target group) | Numerous (incl. rural vs. urban placement) | Practice in a rural location influenced by rural experience during training (χ2 [1, n = 1466] = 68.6 [p < 0.001], with an OR = 2.6 [95%-CI = 2.1–3.4]) | Low: factors influencing rural placement represent only a minor part of the survey | + |
| Landry et al. [30] | 2011 | New Brunswick/Québec/Canada | Questionnaire-based survey (reply by telephone or in writing) + multivariate logistic regressions | Exposure to undergraduate medical training in area of interest for, 1, 2, 3, and 4 years; postgraduate exposure | Francophone physicians admitted to Quebec/New Brunswick | 263 (out of 390 = response rate 67%); 174 family and 100 specialty physicians | Current practice in intervention region – recruitment and retention | Undergraduate exposure: Relative likelihood to practise in the area according to years of exposure: Family physicians:
| High | + |
| Quinn et al. [36] | 2011 | Minnesota/USA | Comparative retrospective cohort study | Six-month Rural Track Clerkship | 3rd-year medical students graduated 1997–2009 | 253 | Practice location after graduation | Rural-track participants:
| Low | +/– |
| Rabinowitz et al. [12] | 2011 | Pennsylvania/USA | Case-control study based on longitudinal study | Physician Shortage Area Programme | Jefferson Medical College graduates practising rural family medicine and in Pennsylvania’s rural counties | 2394 | Practice location and specialty | Clearly increased likelihood of Physician shortage are programme graduates to:
| Fair | + |
| Zink et al. [39] | 2010 | Minnesota/USA | Comparative longitudinal survey based on student and practice data | Rural Physician Associate Programme + focus on recruiting students who will be rural family physicians | Medical school graduates | 3365 graduates: 491 intervention group + 2874 control group | Primary care specialisation and rural practice | Students of the two intervention groups most likely to select rural location: 86% vs. 57%; rural practice rate also higher among nonprimary-care specialists graduated from one intervention programme: 43% vs. 15, 11 and 8%. | Fair: Unclear consideration of selection bias | + |
| Straume and Shaw [27] | 2010 | Finnmark/North Norway | Longitudinal survey based on graduates’ data | Intern support project – mandatory internship in a very remote region with group tutorial and day-to-day supervision | Interns | 233 (out of 267, response rate 87.3%), 112 men and 121 women; 18.5% Northern Norway origin, 150 (64.4%) from the South, 40 from abroad | Rural practice in Northern Norway after graduation | Increased likelihood to choose both primary healthcare and a job in remote Northern Norway: 45.9% took first job in Finnmark – highly significant difference (p < 0.001) compared to geographical origin; 89% of graduates from the north took first job there – 8 times as likely compared to those from the south | Fair – large overlapping with origin | + |
| Bustinza et al. [42] | 2009 | Lower St. Lawrence Region, Québec/Canada | Mail-based cross-sectional questionnaire survey and data-based survey (Bas-Saint-Laurent Regional Department of Health and Social Services), Cox proportional hazards model | (Cumulative duration of) Rural rotations in the region | Family physicians practising in the area between 1985 and 2003 | 215 (out of 644 = 33% return rate) | Rural practice and retention | Adjusted probability of physicians remaining in Bas-Saint-Laurent after being exposed to the area through rural rotations had an odds ratio of 2.12 (p = 0.15). | Overlapping/selection bias: probability to remain in the area for physicians originally from the region: 4.5 (p < 0.01). | + |
| Jarman et al. [18] | 2009 | Wisconsin/USA | Retrospective cross-sectional survey based on 51-item online and paper questionnaire on background, interests, location and factors influencing practice choice | Rural clerkship during medical school | Surgery residency programme graduates | 84 (out of 216 = 39%; raw return rate 45%) | Urban or rural surgical practice | Likelihood to choose rural practice positively associated to rural clerkship (79% vs. 37%, p = 0.001) and surgical residency programme committed to rural training (p = 0.046) | Very low: Many confounding qualitative data included in the study | – Very unspecific, rather arbitrary approach |
| Stagg et al. [38] | 2009 | Australia | Retrospective, questionnaire-based survey by telephone or online | Parallel Rural Community Curriculum | Medical graduates | 46 (out of 86 = 53%) | Rural career path | 54% on rural career path
| Fair | – |
| Mathews et al. [17] | 2008 | Memorial University of Newfoundland, Canada | Cross-sectional study based on the Southam Medical database | Medical training at rural medical school | Physicians practising in Canada | 1322 out of 1381 | Medical practice location in rural Newfoundland and Labrador | 167 (12.6%) rural-school graduates working in rural Canada vs. 81 (6.1%) working in rural Newfoundland. Likelihood to practise in rural Canada compared with graduation from urban backgrounds, no residency training at rural medical school or specialists, increased with:
| Weak:Very broad and general intervention, strong selection bias | + |
| Matsumoto et al. [16] | 2008 | Japan | Retrospective cohort study | Medical training at Jichi Medical School | Graduates from Jichi Medical School | 2988 (follow-up rates 98.7%, 98.2%, and 98.0%, respectively; contract fulfilment 100% for all years) | Workforce outcomes during and after contract fulfilment | Likelihood to work in rural areas of rural-training graduates 4.2 times higher than nonrural graduates.After-duty graduates 3.4 times more likely to work in low population density areas, 2.6 times more likely to work in high elderly rate area, and 2.3 times more likely to work in low physician/population ratio areas;Under-duty rural-programme graduates 8.9 times, 6.5 times, and 5.0 times more likely, respectively | Fair | ++ |
| Worley [15] | 2008 | Adelaide-Alice Springs – Darwin/Australia | Longitudinal comparative retrospective study based on postal survey | Flinders Parallel Rural Community Curriculum: 2-year problem-based learning + decentralised placement in rural areas during 3rd year of undergraduate training | Graduates of Flinders University School of Medicine | 13 (out of 28 = response rate 46%) | Workforce outcomes 5 years after graduation | 70% practising in rural communities, compared to 18% of tertiary-hospital-trained students | Very low: tiny sample size, no consideration of other factors such as pre-selection and potential biases | +– |
| Worley et al. [14] | 2008 | Darwin/Australia | Longitudinal retrospective study based on postal survey | Parallel Rural Community Curriculum at Flinders University+ Northern Territory Clinical School | Graduates of rural and urban Flinders University School of Medicine and of Northern Territory Clinical School | 74 (out of 150 = response rate 49%) | Preference for rural vs. urban practice >5 years | Rural training graduates from Flinders 19.1 (95%-CI, 3.4–106.3; p < 0.001) and from Northern Territories 4.3 (95%-CI, 1.2–14.8; p = 0.026) times more likely to choose rural career paths than graduates from urban Flinders Medical Centre, after adjusting for age and rural background | Good | + |
| Daniels et al. [13] | 2007 | New Mexico/USA | Case control study based on a longitudinal data survey and mailed questionnaire | Rural Health Interdisciplinary Programme (elective programme including rural practice) | Graduates from 12 health-professional programmes | 765 (out of 1396: 59% return rate + 55 exclusion for incomplete graduation) | First and any rural employment after graduation | Rural practicum completion associated with rural practice choice (p < 0.01):
| Low: Overlapping of several partly interlinked factors (rural background, proximity to family) | Fair |
| Smucny et al. [12] | 2005 | State University of New York; Upstate Medical University | Mailed, questionnaire-based retrospective survey | Rural Medical Education Program: 36-week clinical experience in rural communities for medical students | Medical students at State University identified acc. to the Physician Masterfiles | 76 (out of 132 = 58%) | Geographic practice location | Practice in rural locations < 50,000 people:
| Fair | + |
| McCready et al. [11] | 2004 | Northwest Ontario/Canada | Retrospective data-based control study (SPSS) using the Canadian Medical Directory | Northwestern Ontario Medical Programme(NOMP) | Former NOMP medical students | 1982 (out of 2335 NOMP participants = 84.9%) | Practice in Northern Ontario | Undergraduate medical students (and postgraduate residents) with NOMP placement 7.11 more likely to practise in North-Western Ontario (p < 0.001, OR 7.11, 95%-CI 5.11–9.90);Single placement (≤1 month): 50/1042 (4.8%) practised in North Western Ontario; longer placement periods usually associated with higher rates of practice (p = 0.003) | Fair | + |
| Alexandersen et al. [37] | 2004 | Tromsø/Norway | Controlled retrospective study based on data from the Norwegian physician registration file | Medical training at Tromsø University vs. Oslo University | Medical students | Intervention group: 318 out of 345 (=92.3%)Control group: 851 out of 992 (=85.8% | Employment in (rural and remote) North Norway | Recruitment/retention rate of intervention group in North Norway: 51.3% compared to 7.5% of North Norwegians trained in Oslo | Low since the intervention is restricted to regional assignment of university places; relevant selection bias | + |
| Phillips et al. [10] | 1999 | Washington/USA | Retrospective cohort study based on data of the Physician Masterfile of the American Medical Association | Family physician curricular pathway | Medical Students at University of Washington | 239 | Family physicians vs. other pathways | Likelihood to practice in very rural areas fivefold compared to earlier graduation cohorts = non-FP pathway.21 graduates from the intervention groups (3.5%) were rural family physician, more than 10 (10.6) times the 2 graduates (0.33%) from 8 years prior to intervention | Week (very low numbers of control group, no confounders or selection effects taken into consideration) | ++ |
| Whiteside and Mathias [35] | 1996 | British Columbia/Canada | Control study based on mailed cross-sectional survey | Rural training programme of the University of British Columbia | Residents graduated from rural training programme (RR) vs. nonprogramme-trained rural family physicians (RP) | 39 RRs (out of 46 = 84.8%) + 35 (out of 46 = 76.1%) | Practice location | 51% located in rural areas, 20.5% in regional settings and 17.9% in metropolitan areas. | Fair | + |
| Rolfe et al. [29] | 1995 | Newcastle/Australia | Cross-sectional survey based on mailed questionnaire | Rural secondment in year 3.Rural general-practice rotation year 5 | Graduates with respective urban practical training | 217 (out of 331 medical doctors = 65.6%) | Rural practice | Rural family practice rotation: Rural vs. urban location: 30% vs. 10% (p = 0.007, RR 3.02, 95%-CI 1.25–7.32)Rural vs. urban 3rd-year secondment: 23% vs. 34% working in rural areas (p = 0.26, RR 0.67, 95%-CI 0.37–1.22) | Fair | + |
| Fryer [8] | 1993 | Colorado/USA | Control study based on retrospective data analysis (AMA Physician File) | Clinical rotation outside metropolitan area;clinical family practice | UCSM graduates | Total 284.Intervention group: 131 with, control: 153 without ≥ 1 clerkship outside metropolitan areas | Practice in rural counties in Colorado and particularly in towns with <5000 inhabitants | Graduates with nonmetropolitan clerkship in rural practice: 13.7% vs. 7.8% of control group.Practice in small town (<5000): 9.9% vs. 4.0% (p = 0.04) | Low | +/– |
| Verby [34] | 1988 | Minnesota/USA | Data-based longitudinal cohort study | Rural Physician Associate Programme of 9–12 months | 3rd year medical students | 327 practising physicians out of 462 RPAP participants | Medical practice location | 57% of former rural-programme students in rural practice, mostly in Minnesota and in communities <10,000 inhabitants, compared to estimated 80% for 1971–1975 | Very low—no other determinant taken into consideration | + |
| Adkins et al. [8] | 1987 | Washington, Alaska, Montana, Idaho/USA | Data-based longitudinal pre-post control study | Cooperative medical education programme | Medical graduates | 1757 pre- and 947 postgraduates: 270 without, 677 with cooperative experience, 299 cooperative-programme students who studied the 1st year elsewhere | Geographic and specialty distribution before and after | Higher likelihood of cooperative-programme graduates to practise in rural settings (23% vs. 12%) (no statistical significance reported) | Fair | + |
References
- WHO. Increasing Access to Health Workers in Remote and Rural Areas through Improved Retention. Global Policy Recommendations; World Health Organization: Geneva, Switzerland, 2010; Available online: http://whqlibdoc.who.int/publications/2010/9789241564014_eng.pdf (accessed on 23 May 2020).
- Herrmann, M.; Hänel, P.; Jansen, E. Landärztliche Ausbildung zur Reduzierung der medizinischen Unterversorgung auf dem Land–Erfahrungen, Chancen, Widrigkeiten [Rural medical training to reduce medical undersupply in rural areas-experiences, chances, adversities]. In Yearbook for Critical Medicine and Health Sciences [Jahrbuch für Kritische Medizin und Gesundheitswissenschaften] 50; Argument Publishing House: Hamburg, Germany, 2014; pp. 144–172. [Google Scholar]
- Woloschuk, W.; Tarrant, M. Does a rural educational experience influence students’ likelihood of rural practice? Impact of student background and gender. Med. Educ. 2002, 36, 241–247. [Google Scholar] [CrossRef]
- Veitch, C.; Underhill, A.; Hays, R.B. The career aspirations and location intentions of James Cook University’s first cohort of medical students: A longitudinal study at course entry and graduation. Rural Remote Health 2006, 6, 537. [Google Scholar] [PubMed]
- Larkins, S.L.; Michielsen, K.; Iputo, J.; Elsanousi, S.; Mammen, M.; Graves, L.; Willems, S.; Cristobal, F.L.; Samson, R.; Ellaway, R.; et al. Impact of selection strategies on representation of underserved populations and intention to practise: International findings. Med. Educ. 2014, 49, 60–72. [Google Scholar] [CrossRef] [PubMed]
- Roseamelia, C.; Greenwald, J.L.; Bush, T.; Pratte, M.; Wilcox, J.; Morley, C. A qualitative study of medical students in a rural track: Views on eventual rural practice. Fam. Med. 2014, 46, 259–266. [Google Scholar]
- Holst, J.; Normann, O.; Herrmann, M. Strengthening training in rural practice in Germany: New approach for undergraduate medical curriculum towards sustaining rural health care. Rural Remote Health 2015, 15, 3563. [Google Scholar] [PubMed]
- Adkins, R.J.; Anderson, G.R.; Cullen, T.J.; Myers, W.W.; Newman, F.S.; Schwarz, M.R. Geographic and specialty distributions of WAMI Program participants and nonparticipants. Acad. Med. 1987, 62, 810–817. [Google Scholar] [CrossRef] [PubMed]
- Fryer, G.; Miyoshi, T.; Stine, C.; Krugman, R. Colorado’s decentralized medical education to increase the number of graduates practicing primary care in rural areas. Acad. Med. 1993, 68, 310–311. [Google Scholar] [CrossRef]
- Phillips, T.J.; A Rosenblatt, R.; Schaad, D.C.; Cullen, T.J. The long-term effect of an innovative family physician curricular pathway on the specialty and location of graduates of the University of Washington. Acad. Med. 1999, 74, 285–288. [Google Scholar] [CrossRef]
- McCready, W.; Jamieson, J.; Tran, M.; Berry, S. The first 25 years of the Northwestern Ontario Medical Programme. Can. J. Rural. Med. 2004, 9, 94–100. [Google Scholar]
- Smucny, J.; Beatty, P.; Grant, W.; Dennison, T.; Wolff, L.T. An Evaluation of the Rural Medical Education Program of the State University of New York Upstate Medical University, 1990–2003. Acad. Med. 2005, 80, 733–738. [Google Scholar] [CrossRef]
- Daniels, Z.M.; Vanleit, B.J.; Skipper, B.J.; Sanders, M.L.; Rhyne, R.L. Factors in Recruiting and Retaining Health Professionals for Rural Practice. J. Rural. Health 2007, 23, 62–71. [Google Scholar] [CrossRef] [PubMed]
- Worley, P.; Martin, A.; Prideaux, D.; Woodman, R.; Worley, E.; Lowe, M. Vocational career paths of graduate entry medical students at Flinders University: A comparison of rural, remote and tertiary tracks. Med. J. Aust. 2008, 188, 177–178. [Google Scholar] [CrossRef] [PubMed]
- Worley, P. Flinders University School of Medicine, Northern Territory, Australia: Achieving Educational Excellence along with a Sustainable Rural Medical Workforce. MEDICC Rev. 2008, 10, 30–34. [Google Scholar] [PubMed]
- Matsumoto, M.; Inoue, K.; Kajii, E. A Contract-Based Training System for Rural Physicians: Follow-Up of Jichi Medical University Graduates (1978–2006). J. Rural. Health 2008, 24, 360–368. [Google Scholar] [CrossRef] [PubMed]
- Mathews, M.; Rourke, J.; Park, A. National and provincial retention of medical graduates of Memorial University of Newfoundland. Can. Med. Assoc. J. 2006, 175, 357–360. [Google Scholar] [CrossRef]
- Jarman, B.T.; Cogbill, T.H.; Mathiason, M.A.; O’Heron, C.T.; Foley, E.F.; Martin, R.F.; Weigelt, J.A.; Brasel, K.J.; Webb, T.P. Factors Correlated With Surgery Resident Choice to Practice General Surgery in a Rural Area. J. Surg. Educ. 2009, 66, 319–324. [Google Scholar] [CrossRef]
- Rabinowitz, H.K.; Diamond, J.J.; Markham, F.W.; Santana, A.J. Increasing the Supply of Rural Family Physicians: Recent Outcomes from Jefferson Medical College’s Physician Shortage Area Program (PSAP). Acad. Med. 2011, 86, 264–269. [Google Scholar] [CrossRef]
- Tate, R.; Aoki, F. Rural practice and the personal and educational characteristics of medical students Survey of 1269 graduates of the University of Manitoba. Can. Fam. Physician 2012, 58, e641–e648. Available online: https://www.cfp.ca/content/cfp/58/11/e641.full.pdf (accessed on 19 May 2020).
- Playford, D.; Nicholson, A.; Riley, G.J.; Puddey, I.B. Longitudinal rural clerkships: Increased likelihood of more remote rural medical practice following graduation. BMC Med. Educ. 2015, 15, 55. [Google Scholar] [CrossRef]
- Shires, L.; Allen, P.; Cheek, C.; Deb, W. Regional universities and rural clinical schools contribute to rural medical workforce, a cohort study of 2002 to 2013 graduates. Rural Remote Health 2015, 15, 3219. [Google Scholar]
- Kondalsamy-Chennakesavan, S.; Eley, D.S.; Ranmuthugala, G.; Chater, A.; Toombs, M.; Darshan, D.; Nicholson, G.C. Determinants of rural practice: Positive interaction between rural background and rural undergraduate training. Med. J. Aust. 2015, 202, 41–45. [Google Scholar] [CrossRef] [PubMed]
- Wendling, A.L.; Phillips, J.; Short, W.; Fahey, C.; Mavis, B. Thirty Years Training Rural Physicians. Acad. Med. 2016, 91, 113–119. [Google Scholar] [CrossRef] [PubMed]
- Wheat, J.R.; Leeper, J.D.; Murphy, S.; Brandon, J.E.; Jackson, J.R. Educating Physicians for Rural America: Validating Successes and Identifying Remaining Challenges with the Rural Medical Scholars Program. J. Rural Health 2017, 34, s65–s74. [Google Scholar] [CrossRef] [PubMed]
- May, J.; Brown, L.J.; Burrows, J. In-Place Training: Optimizing Rural Health Workforce Outcomes through Rural-Based Education in Australia. Educ. Sci. 2018, 8, 20. [Google Scholar] [CrossRef]
- Straume, K.; Shaw, D.M.P. Internship at the ends of the earth—a way to recruit physicians? Rural Remote Health 2010, 10, 1366. [Google Scholar]
- Woolley, T.; Cristobal, F.; Siega-Sur, J.; Ross, S.J.; Neusy, A.-J.; Halili, S.; Reeve, C. Positive implications from socially accountable, community-engaged medical education across two Philippines regions. Rural Remote Health 2018, 18, 4264. [Google Scholar] [CrossRef]
- Rolfe, I.E.; Pearson, S.-A.; O’Connell, D.L.; Dickinson, J.A. Finding solutions to the rural doctor shortage: The roles of selection versus undergraduate medical education at Newcastle. Aust. N. Z. J. Med. 1995, 25, 512–517. [Google Scholar] [CrossRef]
- Landry, M.; Schofield, A.; Bordage, R.; Bélanger, M. Improving the recruitment and retention of doctors by training medical students locally. Med. Educ. 2011, 45, 1121–1129. [Google Scholar] [CrossRef]
- Eley, D.; Synnott, R.; Baker, P.; Chater, A. A decade of Australian Rural Clinical School graduates – where are they and why? Rural. Remote Health 2012, 12, 1937. [Google Scholar] [CrossRef]
- Forster, L.; Assareh, H.; Watts, L.; McLachlan, C.S. Additional years of Australian Rural Clinical School undergraduate training is associated with rural practice. BMC Med. Educ. 2013, 13, 37. [Google Scholar] [CrossRef]
- Jamar, E.; Newbury, J.; Mills, D. Early career location of University of Adelaide rural cohort medical students. Rural Remote Health 2014, 14, 2592. [Google Scholar] [PubMed]
- E Verby, J. The Minnesota Rural Physician Associate Program for medical students. Acad. Med. 1988, 63, 427–437. [Google Scholar] [CrossRef] [PubMed]
- Whiteside, C.; Mathias, R. Training for rural practice. Are graduates of a UBC program well prepared? Can. Fam. Physician. 1996, 42, 1113–1121. [Google Scholar] [PubMed]
- Quinn, K.J.; Kane, K.Y.; Stevermer, J.J.; Webb, W.D.; Porter, J.L.; Williamson, H.A.; Hosokawa, M.C. Influencing Residency Choice and Practice Location Through a Longitudinal Rural Pipeline Program. Acad. Med. 2011, 86, 1397–1406. [Google Scholar] [CrossRef] [PubMed]
- Alexandersen, Ø.; Jørgensen, E.; Østerås, J.; Hasvold, T. Medisinerutdanningen i Tromsø—sikrer den legerekrutteringen til Nord-Norge? [The medical education in Tromsø—does it secure the recruitment of doctors in North Norway?] Tidsskrift for den Norske lægeforening tidsskrift for praktisk medicin, ny række. J. Nor. Dr. Assoc. 2004, 124, 2107–2109. [Google Scholar]
- Stagg, P.; Greenhill, J.; Worley, P. A new model to understand the career choice and practice location decisions of medical graduates. Rural Remote Health 2009, 9, 9. [Google Scholar] [CrossRef]
- Zink, T.M.; Center, B.; Finstad, D.; Boulger, J.G.; Repesh, L.A.; Westra, R.; Christensen, R.; Brooks, K.D. Efforts to Graduate More Primary Care Physicians and Physicians Who Will Practice in Rural Areas: Examining Outcomes From the University of Minnesota–Duluth and the Rural Physician Associate Program. Acad. Med. 2010, 85, 599–604. [Google Scholar] [CrossRef]
- Phillips, R.; Dodoo, M.; Petterson, S.; Xierali, I.; Bazemore, A.; Teevan, B. Specialty and Geographic Distribution of the Physician Workforce: What Influences Medical Student & Resident Choices? Robert Graham Center: Washington, DC, USA,, 2009; Available online: https://www.graham-center.org/dam/rgc/documents/publications-reports/monographs-books/Specialty-geography-compressed.pdf (accessed on 20 May 2020).
- Strasser, R.P.; Hogenbirk, J.C.; Minore, B.; Marsh, D.; Berry, S.; McCready, W.G.; Graves, L. Transforming health professional education through social accountability: Canada’s Northern Ontario School of Medicine. Med. Teach. 2013, 35, 490–496. [Google Scholar] [CrossRef]
- Bustinza, R.; Gagnon, S.; Burigusa, G. Le Programme d’enseignement décentralisé et la rétention des médecins omnipraticiens dans la région du Bas-Saint-Laurent au Québec. Can. Fam. Physician 2009, 55, e29–e34. [Google Scholar]
- Whitford, D.; Smith, T.; Newbury, J. The South Australian Allied Health Workforce survey: Helping to fill the evidence gap in primary health workforce planning. Aust. J. Prim. Health 2012, 18, 234–241. [Google Scholar] [CrossRef]
- Nelson, G.C.; Gruca, T.S. Determinants of the 5-Year Retention and Rural Location of Family Physicians: Results from the Iowa Family Medicine Training Network. Fam. Med. 2017, 49, 473–476. [Google Scholar] [PubMed]
- Woolley, T.; Gupta, T.K.S.; Murray, R.; Hays, R.B. Predictors of rural practice location for James Cook University MBBS graduates at postgraduate year 5. Aust. J. Rural. Health 2014, 22, 165–171. [Google Scholar] [CrossRef] [PubMed]
- Gupta, T.K.S.; Woolley, T.; Murray, R.B.; Hays, R.B.; McCloskey, T. Positive impacts on rural and regional workforce from the first seven cohorts of James Cook University medical graduates. Rural Remote Health 2014, 14, 2657. [Google Scholar] [PubMed]
- Denz-Penhey, H.; Shannon, S.; Murdoch, J.; Newbury, J. Do benefits accrue from longer rotations for students in Rural Clinical Schools? Rural Remote Health 2005, 5, 414. [Google Scholar] [CrossRef][Green Version]
- Pong, R.; Heng, D. The Link between Rural Medical Education and Rural Medical Practice Location: Literature Review and Synthesis; Centre for Rural and Northern Health Research: Greater Sudbury, ON, Canada, 2005. [Google Scholar]
- Somers, G.T.; Spencer, R.J. Nature or nurture: The effect of undergraduate rural clinical rotations on pre-existent rural career choice likelihood as measured by the SOMERS Index. Aust. J. Rural. Health 2012, 20, 80–87. [Google Scholar] [CrossRef]
- Senf, J.H.; Campos-Outcalt, D.; Watkins, A.J.; Bastacky, S.; Killian, C. A systematic analysis of how medical school characteristics relate to graduates’ choices of primary care specialties. Acad. Med. 1997, 72, 524–533. [Google Scholar] [CrossRef]
- Grobler, L.; Marais, B.J.; Mabunda, S.; Marindi, P.; Reuter, H.; Volmink, J. Interventions for increasing the proportion of health professionals practising in rural and other underserved areas. Cochrane Database Syst. Rev. 2009, 1, 005314. [Google Scholar] [CrossRef]
- Dolea, C.; Stormont, L.; Braichet, J.-M. Evaluated strategies to increase attraction and retention of health workers in remote and rural areas. Bull. World Health Organ. 2010, 88, 379–385. [Google Scholar] [CrossRef]
- O’Sullivan, B.; McGrail, M.R.; Russell, D.J.; Chambers, H.; Major, L. A review of characteristics and outcomes of Australia’s undergraduate medical education rural immersion programs. Hum. Resour. Health 2018, 16, 8. [Google Scholar] [CrossRef]
- Curran, V.; Rourke, L.; Snow, P. A framework for enhancing continuing medical education for rural physicians: A summary of the literature. Med Teach. 2010, 32, e501–e508. [Google Scholar] [CrossRef]
- Hsueh, W.; Wilkinson, T.; Bills, J. What evidence-based undergraduate interventions promote rural health? N. Z. Med. J. 2004, 117, U1117. [Google Scholar] [PubMed]
- Hempel, S.; Shekelle, P.; Maggard-Gibbons, M. Rural Healthcare Workforce: A Systematic Review; US Department of Veterans Affairs: Washington, DC, USA, 2015.
- Strasser, R.P.; Neusy, A.-J. Context counts: Training health workers in and for rural and remote areas. Bull. World Health Organ. 2010, 88, 777–782. [Google Scholar] [CrossRef] [PubMed]
- Evans, D.V.; Patterson, D.G.; Andrilla, C.H.A.; Schmitz, D.; Longenecker, R. Do Residencies That Aim to Produce Rural Family Physicians Offer Relevant Training? Fam. Med. 2016, 48, 596–602. [Google Scholar] [PubMed]
- Mateen, F. Future practice location and satisfaction with rural medical education Survey of medical students. Can. Fam. Physician 2016, 52, 1106–1107. [Google Scholar]
- Senf, J.H.; Campos-Outcalt, D.; Kutob, R. Factors related to the choice of family medicine: A reassessment and literature review. J. Am. Board Fam. Pr. 2004, 16, 502–512. [Google Scholar] [CrossRef]
- Laven, G.; Wilkinson, D. Rural doctors and rural backgrounds: How strong is the evidence? A systematic review. Aust. J. Rural. Health 2003, 11, 277–284. [Google Scholar] [CrossRef]
- Walker, J.; E DeWitt, D.; Pallant, J.F.; E Cunningham, C. Rural origin plus a rural clinical school placement is a significant predictor of medical students’ intentions to practice rurally: A multi-university study. Rural Remote Health 2012, 12, 12. [Google Scholar]
- Parlier, A.B.; Galvin, S.; Thach, S.; Kruidenier, D.; Fagan, E. The road to rural primary care: A narrative review of factors that help develop, recruit, and retain rural primary care physicians. Acad. Med. 2017, 93, 130–140. [Google Scholar] [CrossRef]
- Shelker, W.; Zaharic, T.; Sijnja, B.; Glue, P. Influence of rural background and rural medical training on postgraduate medical training and location in New Zealand. N. Z. Med. J. 2014, 127, 12–16. [Google Scholar]
- Rosenblatt, R.A.; Whitcomb, M.E.; Cullen, T.J.; Lishner, D.M.; Hart, L.G. Which Medical Schools Produce Rural Physicians? JAMA 1992, 268, 1559–1565. [Google Scholar] [CrossRef]
- Hunt, D.D.; Norris, T.; Ballweg, R. The University of Washington WAMI Program: 25 years of experience with manpower shortages in rural areas. Aust. J. Rural. Health 1995, 3, 152–158. [Google Scholar] [CrossRef]
- Bianchi, F.; Stobbe, K.; Eva, K. Comparing academic performance of medical students in distributed learning sites: The McMaster experience. Med. Teach. 2008, 30, 67–71. [Google Scholar] [CrossRef] [PubMed]
- Puertas, E.B.; Arósquipa, C.; Gutiérrez, D. Factors that influence a career choice in primary care among medical students from high-, middle-, and low-income countries: A systematic review. Rev. Panam. Salud Pública 2013, 34, 351–358. [Google Scholar] [PubMed]
- Holst, J.; Herrmann, M. Structural Challenges for Improving Rural Medical Training in Germany. J. Health Educ. Res. Dev. 2016, 4, 154. [Google Scholar] [CrossRef]
| Population | Medical students |
| Intervention | All types of rural placements and internships during undergraduate training |
| Comparator | No rural exposure during undergraduate training |
| Outcome | Rural employment after graduation |
© 2020 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Holst, J. Increasing Rural Recruitment and Retention through Rural Exposure during Undergraduate Training: An Integrative Review. Int. J. Environ. Res. Public Health 2020, 17, 6423. https://doi.org/10.3390/ijerph17176423
Holst J. Increasing Rural Recruitment and Retention through Rural Exposure during Undergraduate Training: An Integrative Review. International Journal of Environmental Research and Public Health. 2020; 17(17):6423. https://doi.org/10.3390/ijerph17176423
Chicago/Turabian StyleHolst, Jens. 2020. "Increasing Rural Recruitment and Retention through Rural Exposure during Undergraduate Training: An Integrative Review" International Journal of Environmental Research and Public Health 17, no. 17: 6423. https://doi.org/10.3390/ijerph17176423
APA StyleHolst, J. (2020). Increasing Rural Recruitment and Retention through Rural Exposure during Undergraduate Training: An Integrative Review. International Journal of Environmental Research and Public Health, 17(17), 6423. https://doi.org/10.3390/ijerph17176423





