Exploration of Superspreading Events in 2015 MERS-CoV Outbreak in Korea by Branching Process Models
Abstract
1. Introduction
2. MERS-CoV Data
2.1. Data Sources
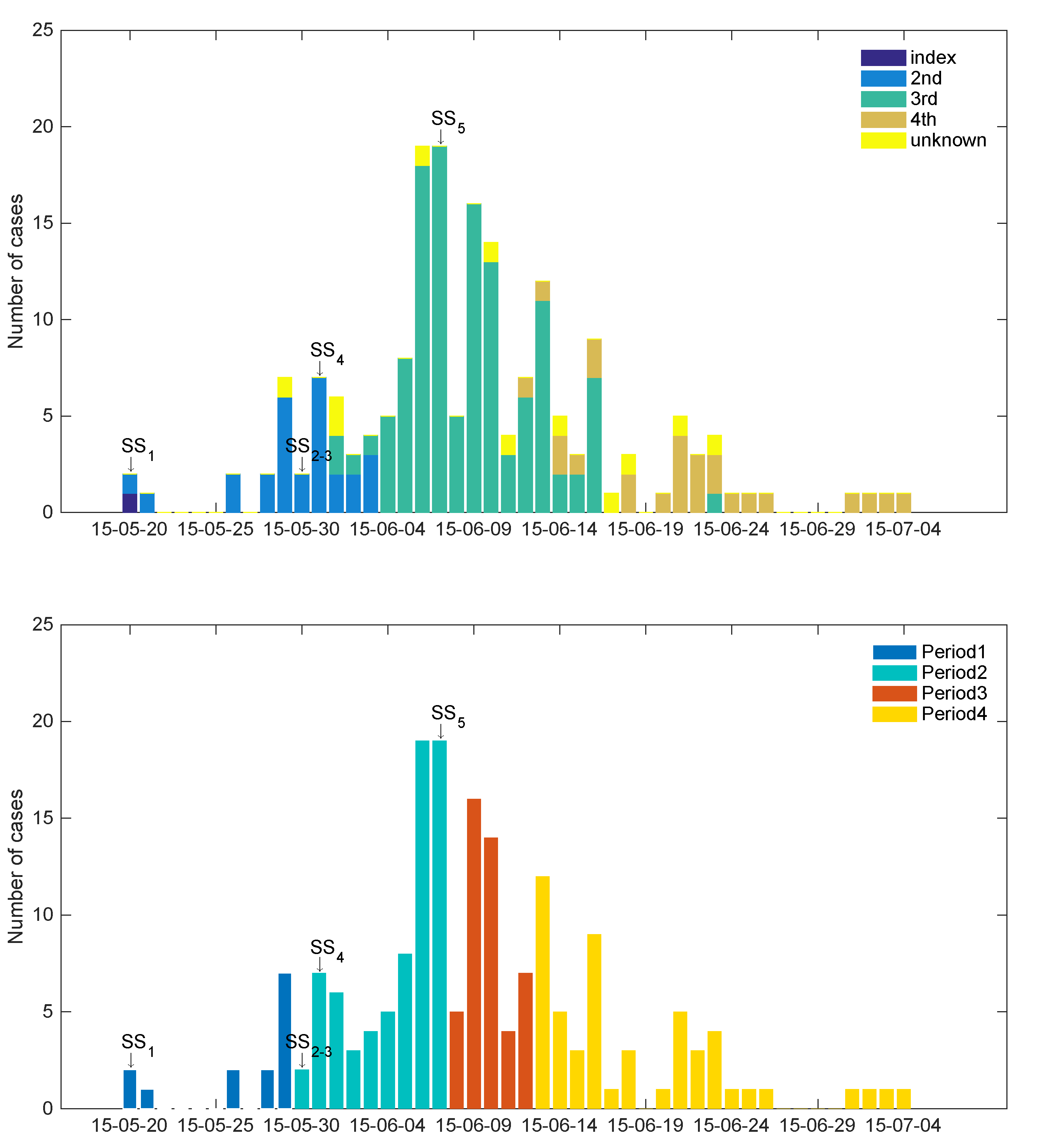
2.2. Superspreading Events
2.3. Nosocomial Infections
3. Branching Process Models
- Branching process model 1 (BP1)
- Branching process model 2 (BP2)
- Lloyd-Smith (LS) branching process model
4. Numerical Results
4.1. Parameter Estimation
4.2. The Effect of Control Measures
5. Discussion
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| BP | Branching process |
| LS | Lloyd-Smith et al. |
| MERS-CoV | Middle East respiratory syndrome coronavirus |
| SARS | Severe acute respiratory syndrome |
| SSE | Superspreading event |
References
- World Health Organization. Q&A on Coronaviruses (COVID-19). Available online: https://www.who.int/news-room/q-a-detail/q-a-coronaviruses#:~:text (accessed on 31 July 2020).
- Korea Centers for Disease Control and Prevention. 2020 COVIID-19 outbreak in the Republic of Korea. Available online: http://ncov.mohw.go.kr (accessed on 31 July 2020).
- Korea Centers for Disease Control and Prevention. Middle East Respiratory Syndrome coronavirus outbreak in the Republic of Korea, 2015. Osong Public Health Res. Perspect. 2015, 6, 269–278. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Middle East Respiratory Syndrome coronavirus (MERS-CoV): Summary of Current Situation, Literature Update and Risk Assessment. WHO/MERS/RA/151. 2015. Available online: http://www.who.int/csr/disease/coronavirus_infections/risk-assessment-7july2015/en/ (accessed on 1 December 2017).
- Galvani, A.P.; May, R.M. Epidemiology: Dimensions of superspreading. Nature 2005, 438, 293–295. [Google Scholar] [CrossRef] [PubMed]
- Stein, R.A. Super-spreaders in infectious diseases. Int. J. Infect. Dis. 2011, 15, e510–e513. [Google Scholar] [CrossRef] [PubMed]
- Lau, M.S.; Dalziel, B.D.; Funk, S.; McClelland, A.; Tiffany, A.; Riley, S.; Metcalf, C.J.; Grenfell, B.T. Spatial and temporal dynamics of superspreading events in the 2014–2015 West Africa Ebola epidemic. Proc. Natl. Acad. Sci. USA 2017, 114, 2337–2342. [Google Scholar] [CrossRef] [PubMed]
- Chowell, G.; Abdirizak, F.; Lee, S.; Lee, J.; Jung, E.; Nishiura, H.; Viboud, C. Transmission characteristics of MERS and SARS in the healthcare setting: A comparative study. BMC Med. 2015, 13, 210. [Google Scholar] [CrossRef] [PubMed]
- James, A.; Pitchford, J.W.; Plank, M.J. An event-based model of superspreading in epidemics. Proc. R. Soc. Lond. B Biol. Sci. 2007, 274, 741–747. [Google Scholar] [CrossRef] [PubMed]
- Chun, B.C. Understanding and Modeling the Super-spreading Events of the Middle East Respiratory Syndrome Outbreak in Korea. Infect. Chemother. 2015, 48, 147–149. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Lee, S.; Chu, C.; Choe, S.; Hong, S.; Shin, Y. The Characteristics of Middle Eastern Respiratory Syndrome Coronavirus Transmission Dynamics in South Korea. Osong Public Health Res. Perspect. 2016, 7, 49–55. [Google Scholar] [CrossRef]
- Park, J.W.; Lee, K.J.; Lee, K.H.; Lee, S.H.; Cho, J.R.; Mo, J.W.; Choi, S.Y.; Kwon, G.Y.; Shin, J.Y.; Hong, J.Y.; et al. Hospital outbreaks of middle east respiratory syndrome, Daejeon, South Korea, 2015. Emerg. Infect. Dis. 2017, 23, 898. [Google Scholar] [CrossRef]
- Cho, S.Y.; Kang, J.M.; Ha, Y.E.; Park, G.E.; Lee, J.Y.; Ko, J.H.; Lee, J.Y.; Kim, J.M.; Kang, C.I.; Jo, I.J.; et al. MERS-CoV outbreak following a single patient exposure in an emergency room in South Korea: An epidemiological outbreak study. Lancet 2016, 388, 994–1001. [Google Scholar] [CrossRef]
- Xiao, S.; Li, Y.; Sung, M.; Wei, J.; Yang, Z. A study of the probable transmission routes of MERS-CoV during the first hospital outbreak in the Republic of Korea. Indoor Air 2018, 28, 51–63. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.S.; Pebody, R.; Charlett, A.; De Angelis, D.; Birrell, P.; Kang, H.; Choi, Y.H. Estimating and modelling the transmissibility of Middle East Respiratory Syndrome CoronaVirus during the 2015 outbreak in the Republic of Korea. Influenza Other Respir. Viruses 2017, 11, 434–444. [Google Scholar] [CrossRef] [PubMed]
- Chowell, G.; Blumberg, S.; Simonsen, L.; Miller, M.A.; Viboud, C. Synthesizing data and models for the spread of MERS-CoV, 2013: Key role of index cases and hospital transmission. Epidemics 2014, 9, 40–51. [Google Scholar] [CrossRef] [PubMed]
- Poletto, C.; Colizza, V.; Boëlle, P.Y. Quantifying spatiotemporal heterogeneity of MERS-CoV transmission in the Middle East region: A combined modelling approach. Epidemics 2016, 15, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Xia, Z.Q.; Zhang, J.; Xue, Y.K.; Sun, G.Q.; Jin, Z. Modeling the Transmission of Middle East Respirator Syndrome Corona Virus in the Republic of Korea. PLoS ONE 2015, 10, e0144778. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.; Ryu, H.; Lee, S. Agent-based modeling for supersupreading events: A case study of MERS-CoV transmission dynamics in the Republic of Korea. Int. J. Environ. Res. Public Health 2018, 15, 2369. [Google Scholar] [CrossRef] [PubMed]
- Lloyd-Smith, J.O.; Schreiber, S.J.; Kopp, P.E.; Getz, W.M. Superspreading and the effect of individual variation on disease emergence. Nature 2005, 438, 355–359. [Google Scholar] [CrossRef]
- KBS Digital News Division. Current State of MERS Infection [Internet]. Available online: http://dj.kbs.co.kr/resources/2015-06-08/ (accessed on 30 May 2016).
- Nishiura, H.; Endo, A.; Saitoh, M.; Kinoshita, R.; Ueno, R.; Nakaoka, S.; Miyamatsu, Y.; Dong, Y.; Chowell, G.; Mizumoto, K. Identifying determinants of heterogeneous transmission dynamics of the Middle East respiratory syndrome (MERS) outbreak in the Republic of Korea, 2015: A retrospective epidemiological analysis. BMJ Open 2016, 6, e009936. [Google Scholar] [CrossRef]
- Kim, S.W.; Park, J.W.; Jung, H.D.; Yang, J.S.; Park, Y.S.; Lee, C.; Kim, K.M.; Lee, K.J.; Kwon, D.; Hur, Y.J.; et al. Risk factors for transmission of Middle East respiratory syndrome coronavirus infection during the 2015 outbreak in South Korea. Clin. Infect. Dis. 2017, 64, 551–557. [Google Scholar] [CrossRef]
- Gyeong-gi News Paper. Pyeongtaek Good Morning Hospital Emergency Medical Center ‘The best grade’. Available online: http://www.kgnews.co.kr/news/articleView.html?idxno=506694 (accessed on 6 March 2018).
- Rapportian. Why did “ MERS Patient No. 14” stay at Samsung Medical Center for Three Days? Available online: http://www.rapportian.com/news/articleView.html?idxno=22749 (accessed on 6 March 2018).
- Medipana. Cancel 6 Non-Standardized Emergency Medical Institutions… Seoul National University Emergency Room is #1 in Complexity. Available online: http://www.medipana.com/news/news_viewer.asp?NewsNum=164380&MainKind =C&NewsKind=100&vCount=12&vKind=1 (accessed on 6 March 2018).
- Saha, K.; Paul, S. Bias corrected maximum likelihood estimator of the negative binomial dispersion parameter. Biometrics 2005, 61, 179–185. [Google Scholar] [CrossRef]
- Anscombe, F.J. Sampling theory of the negative binomial and logarithmic series distributions. Biometrika 1950, 37, 358–382. [Google Scholar] [CrossRef] [PubMed]
- Breban, R.; Riou, J.; Fontanet, A. Interhuman transmissibility of Middle East respiratory syndrome coronavirus: Estimation of pandemic risk. Lancet 2013, 82, 694–699. [Google Scholar] [CrossRef]
- Cauchemez, S.; Fraser, C.; Van Kerkhove, M.D.; Donnelly, C.A.; Riley, S.; Rambaut, A.; Ferguson, N.M.; Rambaut, A.; Enouf, V.; van der Werf, P. Middle East respiratory syndrome coronavirus: Quantification of the extent of the epidemic, surveillance biases, and transmissibility. Lancet Infect. Dis. 2014, 14, 50–56. [Google Scholar] [CrossRef]









| # 1 | # 14 | # 15 | # 16 | # 76 | |
|---|---|---|---|---|---|
| Age (years) | 68 | 35 | 35 | 41 | 75 |
| Gender | Male | Male | Male | Male | Female |
| Number of secondary infections | 28 | 79 | 6 | 23 | 11 |
| Number of contacts | 626 | 594 | 304 | 277 | 805 |
| Exposed hospitals | — | A | A | A | B |
| Number of hospitals visited | 5 | 3 | 3 | 4 | 3 |
| Duration of exposure | April 29–May 2 | May 15–17 | May 15–17 | May 15–17 | May 27–28 |
| Underlying disease | Hypertension | — | Liver failure | Pancreatitis | Multiple myeloma |
| Parameter | N | Mean (95% CI) | k (95% CI) | Pr (Extinct) |
|---|---|---|---|---|
| Value | 167 | 0.96 (0.6915, 1.2285) | 0.063 (0.0451, 0.0809) | 0.99 |
| Value | 186 | 1.0 (0.7720, 1.3480) | 0.12 (0.1008, 0.1392) | 0.98 |
| BP1 | BP2 | LS | MERS-CoV Data | |
|---|---|---|---|---|
| Outbreak size | 41.19 | 59.22 | 140.06 | 186 |
| Generations | 8.47 | 7.25 | 4.37 | 4 |
| Number of secondary infections of the index case | 12 | 14 | 102 | 79 |
| Peak size | 4.06 | 5.77 | 17.13 | 19 |
| Peak generation | 4.41 | 4.02 | 2.67 | 3 |
| Extinction probability | 0.99 | 1 | 0.99 | — |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Choe, S.; Kim, H.-S.; Lee, S. Exploration of Superspreading Events in 2015 MERS-CoV Outbreak in Korea by Branching Process Models. Int. J. Environ. Res. Public Health 2020, 17, 6137. https://doi.org/10.3390/ijerph17176137
Choe S, Kim H-S, Lee S. Exploration of Superspreading Events in 2015 MERS-CoV Outbreak in Korea by Branching Process Models. International Journal of Environmental Research and Public Health. 2020; 17(17):6137. https://doi.org/10.3390/ijerph17176137
Chicago/Turabian StyleChoe, Seoyun, Hee-Sung Kim, and Sunmi Lee. 2020. "Exploration of Superspreading Events in 2015 MERS-CoV Outbreak in Korea by Branching Process Models" International Journal of Environmental Research and Public Health 17, no. 17: 6137. https://doi.org/10.3390/ijerph17176137
APA StyleChoe, S., Kim, H.-S., & Lee, S. (2020). Exploration of Superspreading Events in 2015 MERS-CoV Outbreak in Korea by Branching Process Models. International Journal of Environmental Research and Public Health, 17(17), 6137. https://doi.org/10.3390/ijerph17176137






