Psychometric and Structural Validity of the Pittsburgh Sleep Quality Index among Filipino Domestic Workers
Abstract
1. Background
2. Methods
2.1. Participants
2.2. Measures
- Objective Sleep:
- Daily Sleep Diary
- Depressive Symptoms
- Anxiety
- Epworth Sleepiness Scale:
- Rumination
- Perceived social support
3. Data Analysis
3.1. Study 1
3.1.1. Reliability Testing
3.1.2. Validity Testing
3.2. Study 2
4. Results
4.1. Study 1
4.1.1. Reliability
4.1.2. Validity
4.2. Study 2
4.2.1. Participants Characteristics
4.2.2. EFA Results
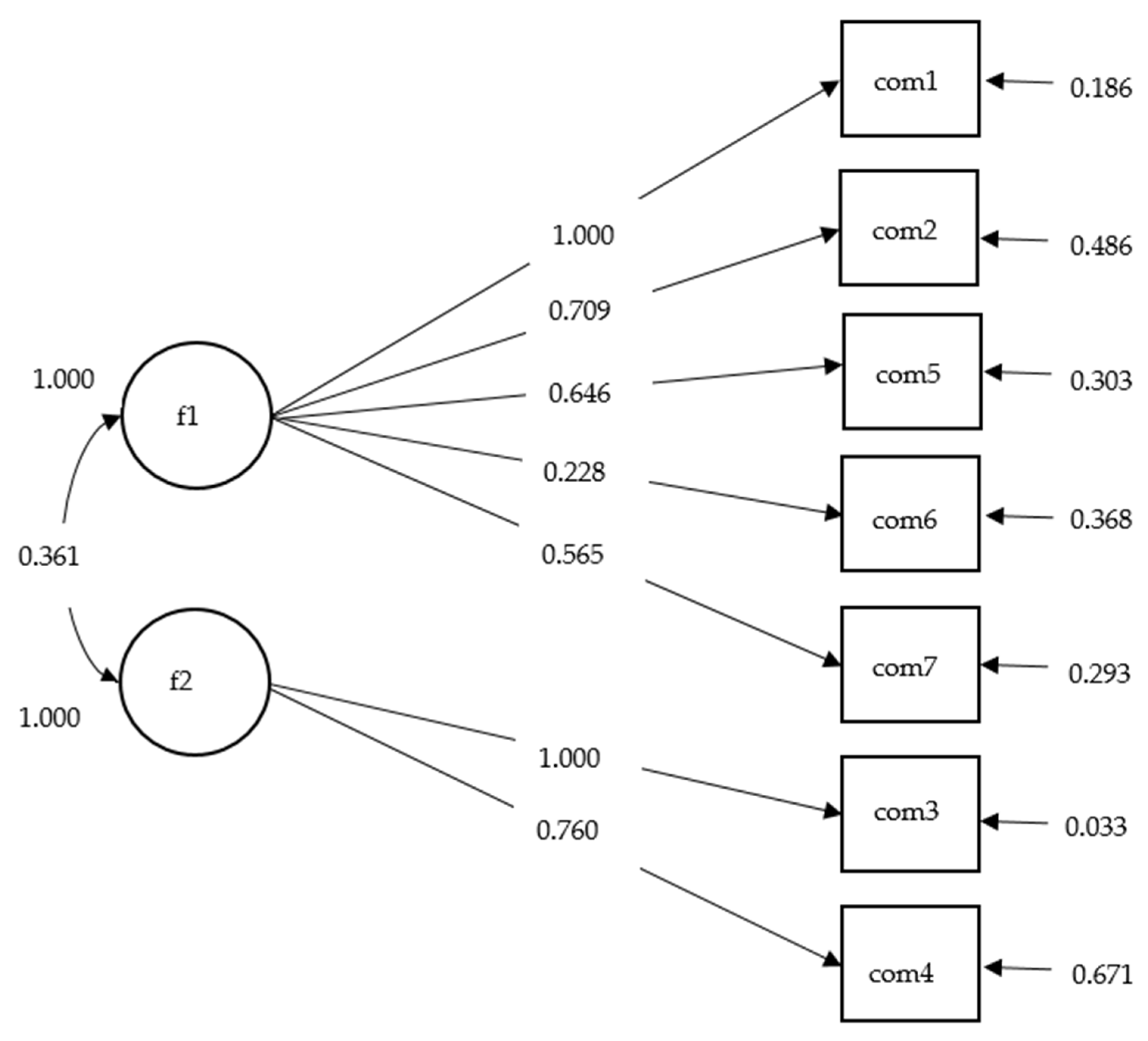
4.2.3. CFA Results
| Study (Year) [Reference] | Population | Sample Size | Type of Structure Model | Results | Added Paths (Modifications) |
|---|---|---|---|---|---|
| Magee et al. (2008) [30] | Australian adults aged 18 to 59 years old | 364 | two-factor | Perceived sleep quality (C1, C2, C5, C6, C7); Sleep efficiency (C3, C4). | |
| Kotronoulas et al. (2011) [28] | Patients with cancer receiving chemotherapy | 209 | two-factor | Quality of nocturnal sleep: C1, C2, C3, C4, C5; Daily disturbances and management of sleep problems: C6, C7. | |
| Guo et al. (2016) [51] | Chinese undergraduate students | 631 | two-factor | Same as Magee et al. (2008). | |
| Qiu et al. (2016) [62] | US pregnant women | 1488 | two-factor | Factor1: C1, C2, C3, C4; Factor2: C5, C7. | C2 and C4, C3 and C4 |
| Becker et al. (2017) [63] | Portuguese community-dwelling older adults | 204 | two-factor | Perceived sleep quality: C1, C2; Sleep efficiency: C3, C4; Daytime function: C5, C7. | |
| Fontes et al. (2017) [60] | Portuguese breast cancer patients | 474 | two-factor | Factor1: C1, C2, C3, C4; Factor2: C5, C6, C7. | |
| Passos et al. (2017) [64] | Brazilian adolescents | 309 | two-factor | Same as Magee et al. (2008) omitting the sleep medication component | |
| Otte et al. (2013) [65] | Non-depressed breast cancer survivors | 1174 | two-factor | Same as Magee et al. (2008). | C1 and C3, C2 and C4, C2 and C6, C2 and C7, C3 and C7. |
| Gelaye et al. (2014) [61] | Undergraduate students in Chile, Ethiopia, and Thailand | 5900 | two-factor | Same as Magee et al. (2008). | |
| Cole et al. (2006) [27] | Community-dwelling adults | 417 | three-factor | Perceived sleep quality: C1, C2, C6, Sleep efficiency (C3, C4); Daily disturbances (C5, C7). | |
| Mariman et al. (2012) [66] | Chronic fatigue syndrome patients | 413 | three-factor | Same as Cole et al. (2006). | |
| Gelaye et al. (2014) [61] | Undergraduate students in Peru | 2581 | three-factor | Sleep quality: C1, C5, C7; Sleep efficiency: C3, C4; Other: C2, C6. | |
| Koh et al. (2015) [29] | Multi-ethnicities population in Singapore | 489 | three-factor | Perceived sleep quality: C1, C2; Sleep efficiency: C3, C4; Daytime function: C5, C6, C7. | |
| Otte et al. (2015) [67] | Women with hot flashes | 890 | three-factor | Same as Cole et al. (2006). | |
| Zhong et al. (2015) [68] | Peruvian Pregnant Women | 642 | three-factor | Perceived sleep quality: C1, C2, C5, C7; Sleep efficiency: C3, C4; Sleep medication: C1, C2, C6. |
| Sleep Patterns | Description | Actigraphy | Daily Sleep Diary |
|---|---|---|---|
| Total sleep time (TST) | The total amount of sleep obtained from falling asleep to final awakening (reported in hours and minutes). | √ | |
| The time in bed (TIB) | It was calculated by the interval period between the time to wake up and the reported bedtime the night before. | √ | |
| Sleep onset latency (SL) | The time between bedtime and sleep onset (reported in minutes). | √ | √ |
| Sleep efficiency (SE) | The result of TST divided by the total time in bed x 100%. | √ | √ |
| Wake after sleep onset (WASO) | The number of minutes scored as awake during the sleep period after initial sleep onset. | √ | |
| Number of wake bouts (WB) | The number of contiguous epochs categorized as wake. | √ | |
| Fragmentation index (FI) | The sum of the ‘mobile time (%)’ and the ‘immobile bouts <= 1 min (%)’. | √ | |
| Sleep quality (SQ) | Item from PSQI, ‘During the past month, how would you rate your sleep quality overall?’ | √ |
| Items | Mean | Standard Deviation | Item-To-Total Correlation b | Alpha if Item Deleted | ICC | 95% CI of ICC |
|---|---|---|---|---|---|---|
| Component 1: Subjective sleep quality | 1.13 | 0.63 | 0.66 ** | 0.55 | 0.44 ** | (−0.07, 0.91) |
| Component 2: Sleep latency | 1.46 | 0.86 | 0.66 ** | 0.56 | 0.58 ** | (0.05, 1.13) |
| Component 3: Sleep duration | 1.37 | 0.90 | 0.63 **,a | 0.58 | 0.58 ** | (0.09, 1.08) |
| Component 4: Habitual sleep efficiency | 0.45 | 0.74 | 0.43 **,a | 0.64 | 0.35 ** | (−0.27, 0.99) |
| Component 5: Sleep disturbances | 1.51 | 0.61 | 0.52 ** | 0.59 | 0.43 ** | (−0.25, 1.10) |
| Component 6: Use of sleeping medicine | 0.27 | 0.62 | 0.37 **,a | 0.64 | 0.30 ** | (−0.18, 0.73) |
| Component 7: Daytime dysfunction | 0.88 | 0.70 | 0.59 ** | 0.57 | 0.42 ** | (−0.21, 1.03) |
| PSQI-Global (0-21) | 7.09 | 2.86 | 0.63 ** | (0.01, 1.24) |
| PSQI Items | PHQ-9 a | GAD-7 a | ESS a | RRS a | MSPSS | Height a | |||
|---|---|---|---|---|---|---|---|---|---|
| Total a | Family a | Friends a | Other a | ||||||
| Component 1 | 0.27 ** | 0.26 ** | −0.06 | 0.21 * | −0.23 ** | −0.25 ** | −0.17 | −0.16 | 0.09 |
| Component 2 | 0.13 | 0.06 | 0.07 | 0.20 * | −0.21 * | −0.27 ** | −0.13 | −0.12 | 0.09 |
| Component 3 | 0.13 | 0.10 | 0.05 | 0.10 | −0.17 | −0.18 * | −0.17 | −0.07 | 0.003 |
| Component 4 | −0.06 | −0.03 | 0.07 | 0.12 | −0.04 | −0.13 | 0.03 | 0.07 | 0.22 * |
| Component 5 | 0.38 ** | 0.3 1** | 0.11 | 0.38 ** | .06 | 0.10 | 0.03 | 0.05 | 0.03 |
| Component 6 | 0.23 ** | 0.23 ** | 0.24 ** | 0.19 * | −0.05 | −0.03 | −0.01 | −0.09 | 0.10 |
| Component 7 | 0.47 ** | 0.29 ** | 0.19 * | 0.38 ** | −0.11 | −0.11 | −0.19 | −0.10 | 0.12 |
| PSQI-Global | 0.36 ** | 0.28 ** | 0.17 | 0.39 ** | −0.18 * | −0.21 * | −0.15 | −0.07 | 0.18 * |
| Follow-Up PSQI Items | Sleep Diary (n = 58) | Actigraphic Variables (n = 61) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| TIB b | SL a | TST b | SQ a | SE a | TST a | SL a | SE a | WASO a | WB b | FI b | |
| Component 1 | −0.27 * | 0.31 * | −0.27 * | 0.61 ** | 0.19 | −0.11 | 0.14 | −0.07 | 0.04 | −0.10 | 0.15 |
| Component 2 | −0.19 | 0.62 ** | −0.23 | 0.44 ** | 0.34** | −0.09 | 0.16 | −0.16 | 0.17 | −0.07 | 0.15 |
| Component 3 | −0.80 ** | 0.25 | −0.79 ** | 0.36 ** | 0.16 | −0.65 ** | −0.09 | 0.13 | −0.24 | −0.43 ** | −0.06 |
| Component 4 | −0.29 *,a | 0.15 | −0.31 **,a | 0.30 * | 0.19 | 0.02 | −0.01 | 0.02 | −0.05 | −0.09 a | 0.09 a |
| Component 5 | −0.10 | 0.28 * | −0.06 | 0.46 ** | 0.12 | −0.04 | −0.09 | 0.07 | 0.04 | −0.09 | 0.03 |
| Component 6 | / | / | / | / | / | 0.15 | 0.12 | −0.18 | 0.22 | 0.09 a | 0.18 a |
| Component 7 | −0.13 | 0.30 * | −0.09 ** | 0.44 ** | −0.10 | −0.11 | 0.14 | −0.07 | 0.01 | −0.02 | 0.02 |
| PSQI-Global | −0.48 ** | 0.48 ** | −0.48 ** | 0.65 ** | 0.25 | −0.23 | 0.03 | 0.02 | −0.03 | −0.21 | 0.14 |
| Selected Variables | Total Sample (n = 1363) | Sample for EFA (n = 681) | Sample for CFA (n = 682) |
|---|---|---|---|
| Age (years, mean SD) | 40.99 8.92 | 40.79 8.87 | 41.19 8.97 |
| Age group | |||
| 18–30 | 188 (13.79) | 92 (13.51) | 96 (14.08) |
| 31–40 | 491 (36.02) | 256 (37.59) | 235 (34.46) |
| 41–50 | 482 (35.36) | 233 (34.21) | 249 (36.51) |
| 51 | 202 (14.82) | 100 (14.68) | 102 (14.96) |
| Time working as a domestic worker in Macao (years) | 6.07 8.60 | 6.16 8.86 | 5.97 8.34 |
| Marital status | |||
| Single, never married | 347 (25.46) | 175 (25.70) | 172 (25.22) |
| Married | 603 (44.24) | 302 (44.35) | 301 (44.13) |
| Partnered but not married | 97 (7.12) | 46 (6.75) | 51 (7.48) |
| Separated | 214 (15.70) | 100 (14.68) | 114 (16.72) |
| Legally separated | 9 (0.66) | 6 (.88) | 3 (0.44) |
| Widowed | 93 (6.82) | 52 (7.64) | 41 (6.01) |
| Education level | |||
| Elementary | 24 (1.76) | 11 (1.62) | 13 (1.91) |
| High school | 489 (35.88) | 244 (35.83) | 245 (35.92) |
| Technical/vocational | 147 (10.79) | 72 (10.57) | 75 (11.00) |
| 2-year associate degree | 209 (15.33) | 107 (15.71) | 102 (14.96) |
| Some college | 225 (16.51) | 116 (17.03) | 109 (15.98) |
| Bachelor’s degree | 265 (19.44) | 130 (19.09) | 135 (19.79) |
| Master’s degree or higher | 4 (0.29) | 1 (0.15) | 3 (0.44) |
| Type of Visa | |||
| Working Visa | 1358 (99.63) | 678 (99.56) | 680 (99.71) |
| Temporary permanent resident | 3 (0.22) | 2 (0.29) | 1 (0.15) |
| Permanent resident | 2 (0.15) | 1 (0.15) | 1 (0.15) |
| Language speaking level (Cantonese) | 1.64 1.76 | 1.63 1.76 | 1.64 1.75 |
| Language understanding level (Cantonese) | 1.72 1.88 | 1.72 1.91 | 1.71 1.85 |
| Live-in / live-out | |||
| Live-in | 672 (49.30) | 333 (48.90) | 339 (49.71) |
| Live-out | 691 (50.70) | 348 (51.50) | 343 (50.29) |
| Monthly salary (USD) | 436.93 101.31 | 436.72 108.46 | 437.14 93.70 |
| Working hours per week | 65.60 21.99 | 66.55 22.51 | 64.66 21.44 |
| Numbers of days off per month | 3.71 1.77 | 3.71 1.13 | 3.71 1.23 |
| PSQI Items | Factor 1 | Factor 2 |
|---|---|---|
| Component 1: Subjective sleep quality | 0.62 | 0.16 |
| Component 2: Sleep latency | 0.48 | 0.11 |
| Component 3: Sleep duration | 0.13 | 0.77 |
| Component 4: Habitual sleep efficiency | 0.00 | 0.77 |
| Component 5: Sleep disturbances | 0.58 | 0.03 |
| Component 6: Use of sleeping medicine | 0.38 | 0.08 |
| Component 7: Daytime dysfunction | 0.60 | 0.05 |
| % Variance explained | 33.99% | 22.25% |
| Models | df | CFI | TLI | RMSEA | SRMR | ||
|---|---|---|---|---|---|---|---|
| The second random sample | One-factor | 466.20 ** | 14 | 0.55 | 0.33 | 0.22 | 0.12 |
| Two-factor a | 50.75 ** | 13 | 0.96 | 0.94 | 0.065 | 0.039 | |
| Two-factor b | 457.24 ** | 13 | 0.56 | 0.29 | 0.22 | 0.11 | |
| Two-factor c | 464.13 ** | 13 | 0.55 | 0.28 | 0.23 | 0.11 | |
| Three-factor a | 83.29 ** | 12 | 0.93 | 0.88 | 0.050 | 0.093 | |
| Three-factor b | 72.42 ** | 12 | 0.94 | 0.90 | 0.048 | 0.086 | |
| Three-factor c | 83.78 ** | 12 | 0.93 | 0.88 | 0.084 | 0.05 |
| PSQI Items | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 |
|---|---|---|---|---|---|---|---|---|---|
| 1.Component 1: Subjective sleep quality | 1 | ||||||||
| 2. Component 2: Sleep latency | 0.41 ** | 1 | |||||||
| 3. Component 3: Sleep duration | 0.23 ** | 0.14 ** | 1 | ||||||
| 4. Component 4: Habitual sleep efficiency | 0.08 ** | 0.04 | 0.60 ** | 1 | |||||
| 5. Component 5: Sleep disturbances | 0.39 ** | 0.38 ** | 0.13 ** | 0.01 | 1 | ||||
| 6. Component 6: Use of sleeping medicine | 0.16 ** | 0.04 | 0.09 ** | 0.09 ** | 0.24 ** | 1 | |||
| 7. Component 7: Daytime dysfunction | 0.39 ** | 0.28 ** | 0.16 ** | 0.06 * | 0.38 ** | 0.26 ** | 1 | ||
| 8. PSQI factor 1 | 0.73 ** | 0.75 ** | NA | NA | 0.71 ** | 0.24 ** | 0.68 ** | 1 | |
| 9. PSQI factor 2 | NA | NA | 0.91 ** | 0.85 ** | NA | NA | NA | NA | 1 |
| Mean | 0.79 | 1.29 | 1.29 | 0.83 | 1.28 | 0.27 | 0.54 | 3.89 | 2.12 |
| Standard deviation | 0.63 | 0.83 | 1.00 | 1.13 | 0.67 | 0.65 | 0.67 | 2.04 | 1.96 |
| Median | 1 | 1 | 1 | 0 | 1 | 0 | 0 | 4 | 1 |
| IQR | 0–1 | 1–2 | 1–2 | 0–1 | 1–2 | 0–0 | 0–1 | 2–5 | 1–3 |
4.2.4. Basic Psychometric Properties of PSQI
5. Discussion
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Declarations
Abbreviations
References
- Skouteris, H.; Wertheim, E.H.; Germano, C.; Paxton, S.J.; Milgrom, J. Assessing sleep during pregnancy: A study across two time points examining the Pittsburgh Sleep Quality Index and associations with depressive symptoms. Womens Health Issues 2009, 19, 45–51. [Google Scholar] [CrossRef]
- Shekleton, J.A.; Rogers, N.L.; Rajaratnam, S.M. Searching for the daytime impairments of primary insomnia. Sleep Med. Rev. 2010, 14, 47–60. [Google Scholar] [CrossRef]
- Skouteris, H.; Germano, C.; Wertheim, E.H.; Paxton, S.J.; Milgrom, J. Sleep quality and depression during pregnancy: A prospective study. J. Sleep Res. 2008, 17, 217–220. [Google Scholar] [CrossRef]
- Broström, A.; Wahlin, Å.; Alehagen, U.; Ulander, M.; Johansson, P. Sex-specific associations between self-reported sleep duration, depression, anxiety, fatigue and daytime sleepiness in an older community-dwelling population. Scand. J. Caring Sci. 2018, 32, 290–298. [Google Scholar] [CrossRef]
- Edinger, J.D.; Means, M.K.; Carney, C.E.; Krystal, A.D. Psychomotor performance defcits and their relation to prior nights’ sleep among individuals with primary insomnia. Sleep 2008, 31, 599–607. [Google Scholar] [CrossRef]
- Walker, M.P.; Stickgold, R. Sleep-dependent learning and memory consolidation. Neuron 2004, 44, 121–133. [Google Scholar] [CrossRef]
- Kessler, R.C.; Berglund, P.A.; Coulouvrat, C.; Hajak, G.; Roth, T.; Shahly, V.; Shillington, A.C.; Stephenson, J.J.; Walsh, J.K. Insomnia and the performance of US workers: Results from the America insomnia survey. Sleep 2011, 34, 1161–1171. [Google Scholar] [CrossRef] [PubMed]
- Burnham, L.; Theodore, N. Home Economics: The Invisible and Unregulated World of Domestic Work. Available online: https://idwfed.org/en/resources/home-economics-the-invisible-and-unregulated-world-of-domestic-work/@@display-file/attachment_1 (accessed on 1 January 2020).
- Hall, B.J.; Garabiles, M.R.; Latkin, C.A. Work life, relationship, and policy determinants of health and well-being among filipino domestic workers in China: A qualitative study. BMC Public Health 2019, 19, 229. [Google Scholar] [CrossRef]
- Vargas, M.C.; Garabiles, M.R.; Hall, B.J. Narrative identities of overseas filipino domestic worker community in Macao (SAR) China. J. Community Psychol. 2020, 48, 977–993. [Google Scholar] [CrossRef] [PubMed]
- Hall, B.J.; Yip, P.S.Y.; Garabiles, M.R.; Lao, C.K.; Chan, E.W.W.; Marx, B.P. Psychometric validation of the PTSD checklist-5 among female Filipino migrant workers. Eur. J. Psychotraumatol. 2019, 10, 1571378. [Google Scholar] [CrossRef] [PubMed]
- Sandberg, J.C.; Grzywacz, J.G.; Talton, J.W.; Quandt, S.A.; Chen, H.; Chatterjee, A.B.; Arcury, T.A. A cross-sectional exploration of excessive daytime sleepiness, depression, and musculoskeletal pain among migrant farmworkers. J. Agromed. 2012, 17, 70–80. [Google Scholar] [CrossRef]
- Lies, J.; Drummond, S. Prevalence Study of Sleep Disturbance, Mental Health, and Psychosocial Concerns among Asylum Seekers and Refugees; Journal of Sleep Research, 2017; Wiley: Hoboken, NJ, USA, 2017; pp. 45–46. [Google Scholar]
- The Commission on Filipinos Overseas 2015 CFO Statistics on Philippine International Migration. Available online: http://www.cfo.gov.ph/images/pdf/2017/2015compendiumstats-insidepages (accessed on 29 June 2017).
- Riley, K.; Nazareno, J.; Malish, S. 24-hour care: Work and sleep conditions of migrant Filipino live-in caregivers in Los Angeles. Am. J. Ind. Med. 2016, 59, 1120–1129. [Google Scholar] [CrossRef]
- Hovey, J.D.; Magaña, C. Acculturative stress, anxiety, and depression among Mexican immigrant farmworkers in the Midwest United States. J. Immigr. Health 2000, 2, 119–131. [Google Scholar] [CrossRef]
- Tang, J.; Liu, J.; Wu, D.; Deng, X.; Yuan, F. Correlation analysis between sleep quality and anxiety and depression among migrant workers in Shenzhen. Chin. J. Soc. Med. 2010, 27, 362–364. [Google Scholar]
- Garabiles, M.R.; Ofreneo, M.A.P.; Hall, B.J. Towards a model of resilience for transnational families of Filipina domestic workers. PLoS ONE 2017, 12, e0183703. [Google Scholar] [CrossRef]
- Garabiles, M.R.; Lao, C.K.; Yip, P.; Chan, E.W.W.; Mordeno, I.; Hall, B.J. Psychometric validation of PHQ-9 and GAD-7 in filipino migrant domestic workers in Macao (SAR), China. J. Pers. Assess 2019, 1–12. [Google Scholar] [CrossRef]
- Yi, G.; Huang, L.; Lam, A.I.F.; Latkin, C.; Hall, B.J. Spatial and sociodemographic correlates of gambling participation and disorder among female Filipino migrant workers in Macao, People’s Republic of China. Addict. Behav. 2019, 97, 49–55. [Google Scholar] [CrossRef] [PubMed]
- Hall, B.J.; Pangan, C.A.C.; Chan, E.W.W.; Huang, R.L. The effect of discrimination on depression and anxiety symptoms and the buffering role of social capital among female domestic workers in Macao, China. Psychiat. Res. 2019, 271, 200–207. [Google Scholar] [CrossRef]
- Holroyd, E.A.; Molassiotis, A.; Taylor-Pilliae, R.E. Filipino domestic workers in Hong Kong: Health related behaviors, health locus of control and social support. Women Health 2001, 33, 181–205. [Google Scholar] [CrossRef]
- Buysse, D.J.; Reynolds, C.F.; Monk, T.H.; Berman, S.R.; Kupfer, D.J. The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28, 193–213. [Google Scholar] [CrossRef]
- Ait-Aoudia, M.; Levy, P.P.; Bui, E.; Insana, S.; de Fouchier, C.; Germain, A.; Jehel, L. Validation of the French version of the Pittsburgh Sleep Quality Index addendum for posttraumatic stress disorder. Eur. J. Psychotraumatol. 2013, 4, 19298. [Google Scholar] [CrossRef]
- Manzar, M.D.; Moiz, J.A.; Zannat, W.; Spence, D.W.; Pandi-Perumal, S.R.; Hussain, M.E. Validity of the Pittsburgh Sleep Quality Index in Indian University students. Oman Med. J. 2015, 30, 193–202. [Google Scholar] [CrossRef]
- Nakajima, S.; Okajima, I.; Sasai, T.; Kobayashi, M.; Furudate, N.; Drake, C.L.; Roth, T.; Inoue, Y. Validation of the Japanese version of the ford insomnia response to stress test and the association of sleep reactivity with trait anxiety and insomnia. Sleep Med. 2014, 15, 196–202. [Google Scholar] [CrossRef]
- Cole, J.C.; Motivala, S.J.; Buysse, D.J.; Oxman, M.N.; Levin, M.J.; Irwin, M.R. Validation of a 3-factor scoring model for the Pittsburgh Sleep Quality Index in older adults. Sleep 2006, 29, 112–116. [Google Scholar] [CrossRef]
- Kotronoulas, G.C.; Papadopoulou, C.N.; Papapetrou, A.; Patiraki, E. Psychometric evaluation and feasibility of the Greek Pittsburgh Sleep Quality Index (GR-PSQI) in patients with cancer receiving chemotherapy. Support. Care Cancer 2011, 19, 1831–1840. [Google Scholar] [CrossRef]
- Koh, H.W.; Lim, R.B.; Chia, K.S.; Lim, W.Y. The Pittsburgh Sleep Quality Index in a multi-ethnic Asian population contains a three-factor structure. Sleep Breath. Schlaf Atm. 2015, 19, 1147–1154. [Google Scholar] [CrossRef]
- Magee, C.A.; Caputi, P.; Iverson, D.C.; Huang, X.F. An investigation of the dimensionality of the Pittsburgh Sleep Quality Index in Australian adults. Sleep Biol. Rhythm. 2008, 6, 222–227. [Google Scholar] [CrossRef]
- Garabiles, M.R.; Lao, C.K.; Xiong, Y.; Hall, B.J. Exploring comorbidity between anxiety and depression among migrant Filipino domestic workers: A network approach. J. Affect. Disord. 2019, 250, 85–93. [Google Scholar] [CrossRef]
- Garabiles, M.R.; Lao, K.L.; Wang, S.Y.; Hall, B.J. The network structure of posttraumatic stress disorder among Filipina migrant domestic workers: Comorbidity with depression. Eur. J. Psychotraumatol. 2020, 10, 1571378. [Google Scholar]
- Hall, B.J.; Yang, X.; Huang, L.; Yi, G.; Chan, E.W.W.; Tucker, J.D.; Latkin, C.A. Barriers and facilitators of rapid HIV and syphilis testing uptake among Filipino transnational migrants in China. AIDS Behav. 2020, 24, 418–427. [Google Scholar] [CrossRef]
- Pfizer Screener Overview. Available online: http://www.phqscreeners.com (accessed on 1 February 2016).
- World Health Organization. Process of Translation and Adaptation of Instruments. Available online: http://www.who.int/substance_abuse/research_tools/translation/en (accessed on 1 February 2016).
- Shin, M.; Swan, P.; Chow, C.M. The validity of actiwatch2 and senseWear armband compared against polysomnography at different ambient temperature conditions. Sleep Sci. 2015, 8, 9–15. [Google Scholar] [CrossRef] [PubMed]
- Kroenke, K.; Spitzer, R.L.; Williams, J.B. The PHQ-9: Validity of a brief depression severity measure. J. Gen. Intern. Med. 2001, 16, 606–613. [Google Scholar] [CrossRef] [PubMed]
- Mendoza, N.B.; Mordeno, I.G.; Latkin, C.A.; Hall, B.J. Evidence of the paradoxical effect of social network support: A study among Filipino domestic workers in China. Psychiatry Res. 2017, 255, 263–271. [Google Scholar] [CrossRef]
- Mordeno, I.G.; Carpio, J.G.E.; Mendoza, N.B.; Hall, B.J. The latent structure of major depressive symptoms and its relationship with somatic disorder symptoms among Filipino female domestic workers in China. Psychiatry Res. 2018, 270, 587–594. [Google Scholar] [CrossRef]
- Spitzer, R.L.; Kroenke, K.; Williams, J.B.; Löwe, B. A brief measure for assessing generalized anxiety disorder: The GAD-7. Arch. Intern. Med. 2006, 166, 1092–1097. [Google Scholar] [CrossRef]
- Johns, M.W. A new method for measuring daytime sleepiness: The epworth sleepiness scale. Sleep 1991, 14, 540–545. [Google Scholar] [CrossRef]
- Johns, M.W. A new perspective on sleepiness. Sleep Biol. Rhythm. 2010, 8, 170–179. [Google Scholar] [CrossRef]
- Treynor, W.; Gonzalez, R.; Nolen-Hoeksema, S. Rumination reconsidered: A psychometric analysis. Cogn. Ther. Res. 2003, 27, 247–259. [Google Scholar] [CrossRef]
- Zimet, G.D.; Dahlem, N.W.; Zimet, S.G.; Farley, G.K. The multidimensional scale of perceived social support. J. Personal. Assess. 1988, 52, 30–41. [Google Scholar] [CrossRef]
- Scheffer, J. Dealing with missing data. In Research Letters in the Information and Mathematical Sciences; Massey University: Auckland, New Zealand, 2002; Volume 3, pp. 153–160. [Google Scholar]
- Griethuijsen, R.A.L.F.; Michiel, W.; Helen, H.; Perry, J.; Nigel, C.; Mansour, N.; Ayse, S.; BouJaoude, S. Global patterns in students’ views of science and interest in science. Res. Sci. Educ. 2015, 45, 581–603. [Google Scholar] [CrossRef]
- DeVellis, R.F. Scale Development: Theory and Applications; Sage Publications: New York, NY, USA, 2016; Volume 26. [Google Scholar]
- Weir, J.P. Quantifying test-retest reliability using the intraclass correlation coefficient and the SEM. J. Strength Cond. Res. 2005, 19, 231–240. [Google Scholar]
- Kaneita, Y.; Ohida, T.; Uchiyama, M.; Takemura, S.; Kawahara, K.; Yokoyama, E.; Miyake, T.; Harano, S.; Suzuki, K.; Fujita, T. The relationship between depression and sleep disturbances: A Japanese nationwide general population survey. J. Clin. Psychiatry 2006, 67, 196–203. [Google Scholar] [CrossRef] [PubMed]
- Rosa, R.R.; Bonnet, M.H.; Kramer, M. The relationship of sleep and anxiety in anxious subjects. Biol. Psychol. 1983, 16, 119–126. [Google Scholar] [CrossRef]
- Guo, S.; Sun, W.; Liu, C.; Wu, S. Structural validity of the Pittsburgh Sleep Quality Index in Chinese undergraduate students. Front. Psychol. 2016, 7, 1126. [Google Scholar] [CrossRef]
- Tsai, P.-S.; Wang, S.-Y.; Wang, M.-Y.; Su, C.-T.; Yang, T.-T.; Huang, C.-J.; Fang, S.-C. Psychometric evaluation of the Chinese version of the Pittsburgh Sleep Quality Index (CPSQI) in primary insomnia and control subjects. Qual. Life Res. 2005, 14, 1943–1952. [Google Scholar] [CrossRef]
- Bush, A.L.; Armento, M.E.; Weiss, B.J.; Rhoades, H.M.; Novy, D.M.; Wilson, N.L.; Kunik, M.E.; Stanley, M.A. The Pittsburgh Sleep Quality Index in older primary care patients with generalized anxiety disorder: Psychometrics and outcomes following cognitive behavioral therapy. Psychiatry Res. 2012, 199, 24–30. [Google Scholar] [CrossRef] [PubMed]
- Beavers, A.S.; Lounsbury, J.W.; Richards, J.K.; Huck, S.W.; Skolits, G.J.; Esquivel, S.L. Practical considerations for using exploratory factor analysis in educational research. Pract. Assess. Res. Eval. 2013, 18, 6. [Google Scholar]
- Kaiser, H.F. The application of electronic computers to factor analysis. Educ. Psychol. Meas. 1960, 20, 141–151. [Google Scholar] [CrossRef]
- Suh, Y. The performance of maximum likelihood and weighted least square mean and variance adjusted estimators in testing differential item functioning with nonnormal trait distributions. Struct. Equ. Model. A Multidiscip. J. 2015, 22, 568–580. [Google Scholar] [CrossRef]
- Hu, L.T.; Bentler, P.M. Fit indices in covariance structure modeling: Sensitivity to underparameterized model misspecification. Psychol. Methods 1998, 3, 424–453. [Google Scholar] [CrossRef]
- Wood, P. Confirmatory Factor Analysis for Applied Research; Taylor & Francis: Abingdon, UK, 2008. [Google Scholar]
- Muthén, L.K.; Muthén, B.O. Mplus: Statistical Analysis with Latent Variables: User’s Guide; Muthén & Muthén: Los Angeles, CA, USA, 2005. [Google Scholar]
- Fontes, F.; Goncalves, M.; Maia, S.; Pereira, S.; Severo, M.; Lunet, N. Reliability and validity of the Pittsburgh Sleep Quality Index in breast cancer patients. Support. Care Cancer 2017, 25, 3059–3066. [Google Scholar] [CrossRef] [PubMed]
- Gelaye, B.; Lohsoonthorn, V.; Lertmeharit, S.; Pensuksan, W.C.; Sanchez, S.E.; Lemma, S.; Berhane, Y.; Zhu, X.; Velez, J.C.; Barbosa, C.; et al. Construct validity and factor structure of the pittsburgh Sleep Quality Index and epworth sleepiness scale in a multi-national study of African, South East Asian and South American college students. PLoS ONE 2014, 9, e116383. [Google Scholar] [CrossRef] [PubMed]
- Qiu, C.; Gelaye, B.; Zhong, Q.Y.; Enquobahrie, D.A.; Frederick, I.O.; Williams, M.A. Construct validity and factor structure of the Pittsburgh Sleep Quality Index among pregnant women in a Pacific-Northwest cohort. Sleep Breath. 2016, 20, 293–301. [Google Scholar] [CrossRef]
- Becker, N.B.; de Neves Jesus, S. Adaptation of a 3-factor model for the Pittsburgh Sleep Quality Index in Portuguese older adults. Psychiatry Res. 2017, 251, 298–303. [Google Scholar] [CrossRef] [PubMed]
- Passos, M.H.; Silva, H.A.; Pitangui, A.C.; Oliveira, V.M.; Lima, A.S.; Araujo, R.C. Reliability and validity of the Brazilian version of the Pittsburgh Sleep Quality Index in adolescents. J. Pediatr. 2017, 93, 200–206. [Google Scholar] [CrossRef]
- Otte, J.L.; Rand, K.L.; Carpenter, J.S.; Russell, K.M.; Champion, V.L. Factor analysis of the Pittsburgh Sleep Quality Index in breast cancer survivors. J. Pain Symptom Manag. 2013, 45, 620–627. [Google Scholar] [CrossRef] [PubMed]
- Mariman, A.; Vogelaers, D.; Hanoulle, I.; Delesie, L.; Tobback, E.; Pevernagie, D. Validation of the three-factor model of the PSQI in a large sample of chronic fatigue syndrome (CFS) patients. J. Psychosom. Res. 2012, 72, 111–113. [Google Scholar] [CrossRef]
- Otte, J.L.; Rand, K.L.; Landis, C.A.; Paudel, M.L.; Newton, K.M.; Woods, N.; Carpenter, J.S. Confirmatory factor analysis of the Pittsburgh Sleep Quality Index in women with hot flashes. Menopause (New York, N.Y.) 2015, 22, 1190–1196. [Google Scholar] [CrossRef] [PubMed]
- Zhong, Q.Y.; Gelaye, B.; Sanchez, S.E.; Williams, M.A. Psychometric properties of the Pittsburgh Sleep Quality Index (PSQI) in a cohort of peruvian pregnant women. J. Clin. Sleep Med. 2015, 11, 869–877. [Google Scholar] [CrossRef]
- Schmitt, N. Uses and abuses of coefficient alpha. Psychol. Assess. 1996, 8, 350–353. [Google Scholar] [CrossRef]
- Takacs, J.; Bodizs, R.; Ujma, P.P.; Horvath, K.; Rajna, P.; Harmat, L. Reliability and validity of the Hungarian version of the Pittsburgh Sleep Quality Index (PSQI-HUN): Comparing psychiatric patients with control subjects. Sleep Breath. 2016, 20, 1045–1051. [Google Scholar] [CrossRef] [PubMed]
- Guastella, A.J.; Moulds, M.L. The impact of rumination on sleep quality following a stressful life event. Pers. Individ. Differ. 2007, 42, 1151–1162. [Google Scholar] [CrossRef]
- Dietch, J.R.; Taylor, D.J.; Sethi, K.; Kelly, K.; Bramoweth, A.D.; Roane, B.M. Psychometric evaluation of the PSQI in U.S. College Students. J. Clin. Sleep Med. 2016, 12, 1121–1129. [Google Scholar] [CrossRef]
- Backhaus, J.; Junghanns, K.; Broocks, A.; Riemann, D.; Hohagen, F. Test–retest reliability and validity of the Pittsburgh Sleep Quality Index in primary insomnia. J. Psychosom. Res. 2002, 53, 737–740. [Google Scholar] [CrossRef]
- Grandner, M.A.; Kripke, D.F.; Yoon, I.Y.; Youngstedt, S.D. Criterion validity of the Pittsburgh Sleep Quality Index: Investigation in a non-clinical sample. Sleep Boil. Rhythm. 2006, 4, 129–139. [Google Scholar] [CrossRef] [PubMed]
- Aloba, O.O.; Adewuya, A.O.; Ola, B.A.; Mapayi, B.M. Validity of the Pittsburgh Sleep Quality Index (PSQI) among Nigerian university students. Sleep Med. 2007, 8, 266–270. [Google Scholar] [CrossRef] [PubMed]
- Zheng, W.; Luo, X.N.; Li, H.Y.; Ke, X.Y.; Dai, Q.; Zhang, C.J.; Ng, C.H.; Ungvari, G.S.; Xiang, Y.T.; Ning, Y.P. Association of sleep duration with sleep disturbances, quality of life, and sociodemographic factors in general hospital outpatients. Perspect. Psychiatr. Care 2018, 54, 422–427. [Google Scholar] [CrossRef]
- Wang, S.; Wu, Y.; Ungvari, G.S.; Ng, C.H.; Forester, B.P.; Gatchel, J.R.; Chiu, H.F.K.; Kou, C.; Fu, Y.; Qi, Y.; et al. Sleep duration and its association with demographics, lifestyle factors, poor mental health and chronic diseases in older Chinese adults. Psychiatry Res. 2017, 257, 212–218. [Google Scholar] [CrossRef]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Xiong, P.; Spira, A.P.; Hall, B.J. Psychometric and Structural Validity of the Pittsburgh Sleep Quality Index among Filipino Domestic Workers. Int. J. Environ. Res. Public Health 2020, 17, 5219. https://doi.org/10.3390/ijerph17145219
Xiong P, Spira AP, Hall BJ. Psychometric and Structural Validity of the Pittsburgh Sleep Quality Index among Filipino Domestic Workers. International Journal of Environmental Research and Public Health. 2020; 17(14):5219. https://doi.org/10.3390/ijerph17145219
Chicago/Turabian StyleXiong, Peng, Adam P. Spira, and Brian J. Hall. 2020. "Psychometric and Structural Validity of the Pittsburgh Sleep Quality Index among Filipino Domestic Workers" International Journal of Environmental Research and Public Health 17, no. 14: 5219. https://doi.org/10.3390/ijerph17145219
APA StyleXiong, P., Spira, A. P., & Hall, B. J. (2020). Psychometric and Structural Validity of the Pittsburgh Sleep Quality Index among Filipino Domestic Workers. International Journal of Environmental Research and Public Health, 17(14), 5219. https://doi.org/10.3390/ijerph17145219






