Association between Resting Heart Rate and Colorectal Cancer: Results from a Case-Controlled Study
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Population and Data Collection
2.2. Ethical Approval
2.3. Definition of CRC
2.4. Covariates
2.5. Statistical Analysis
3. Results
3.1. Clinical Characteristics of Non-PS-Matched and PS-Matched CRC Patient Cohorts
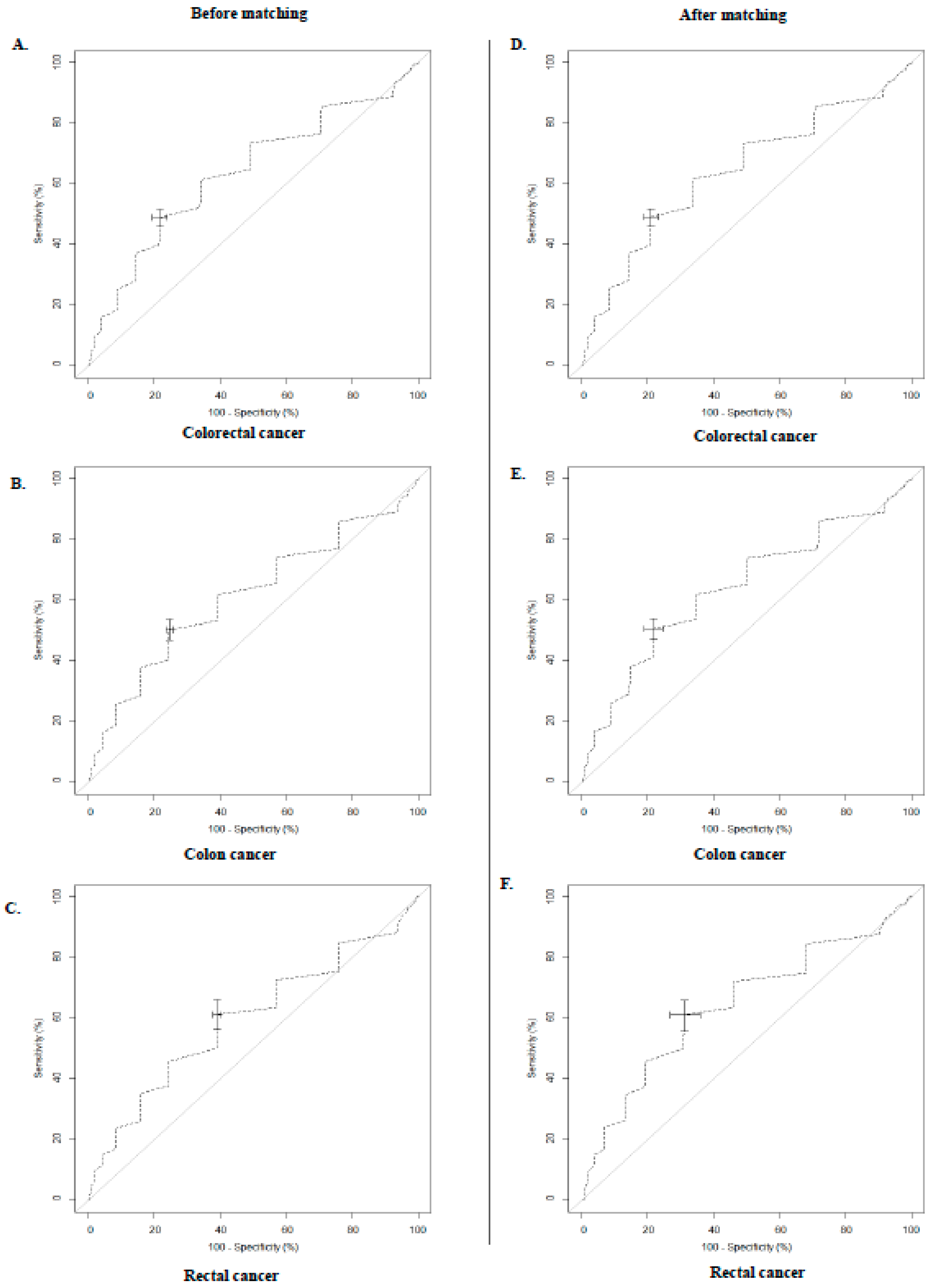
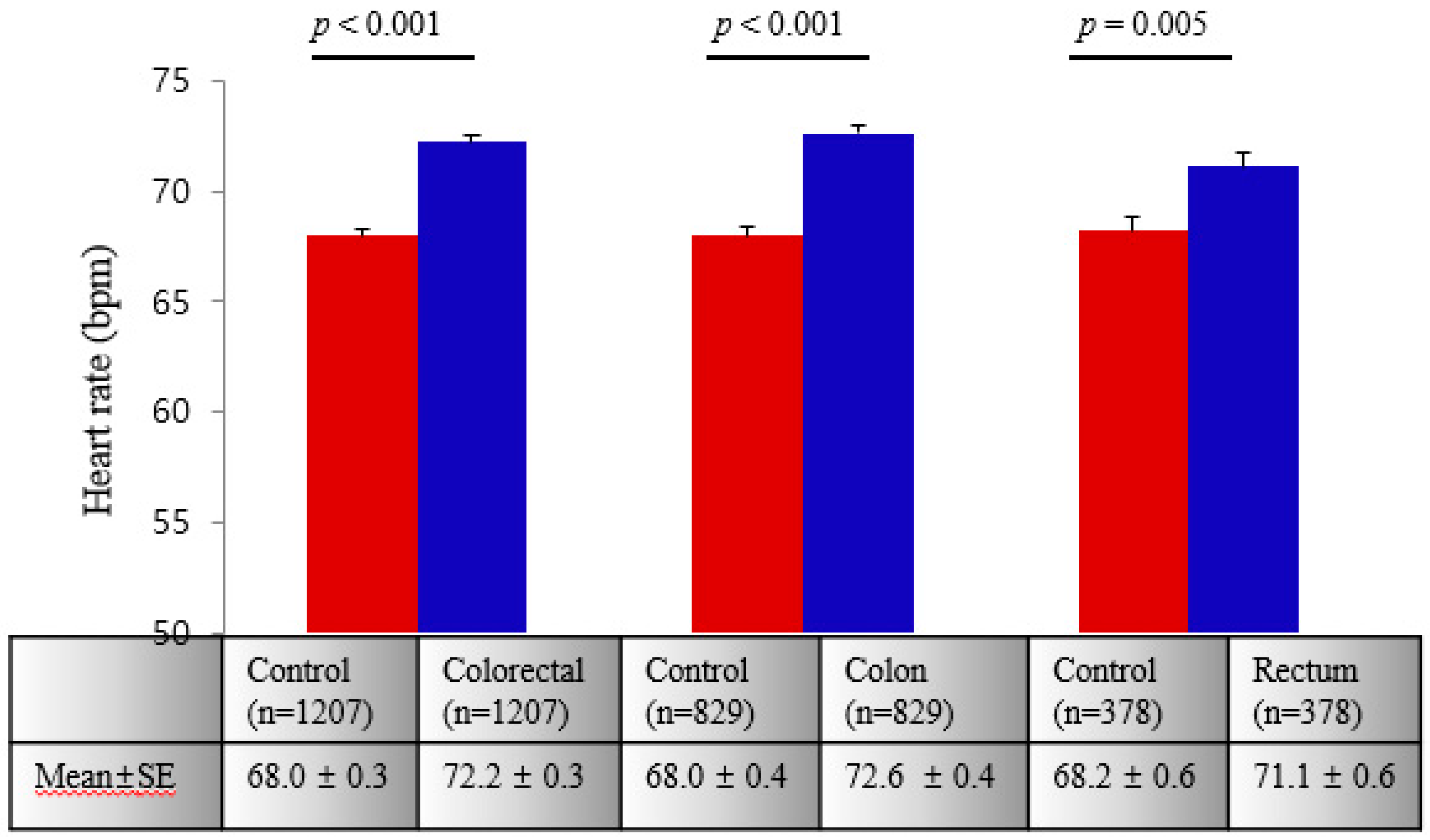
3.2. Associations between RHR and CRC
4. Discussion
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Appendix A
References
- Bray, F.; Ferlay, J.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: Globocan estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2018, 68, 394–424. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Larsen, V.; Morton, V.; Norat, T.; Moreira, A.; Potts, J.F.; Reeves, T.; Bakolis, I. Dietary patterns derived from principal component analysis (PCA) and risk of colorectal cancer: A systematic review and meta-analysis. Eur. J. Clin. Nutr. 2019, 73, 366–386. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.J.; Lee, D.H.; Han, K.D.; Shin, C.M.; Kim, N. Abdominal obesity, glucose intolerance and decreased high-density lipoprotein cholesterol as components of the metabolic syndrome are associated with the development of colorectal cancer. Eur. J. Epidemiol. 2018, 33, 1077–1085. [Google Scholar] [CrossRef] [PubMed]
- Grassi, G.; Vailati, S.; Bertinieri, G.; Seravalle, G.; Stella, M.L.; Dell’Oro, R.; Mancia, G. Heart rate as marker of sympathetic activity. J. Hypertens. 1998, 16, 1635–1639. [Google Scholar] [CrossRef] [PubMed]
- Kovar, D.; Cannon, C.P.; Bentley, J.H.; Charlesworth, A.; Rogers, W.J. Does initial and delayed heart rate predict mortality in patients with acute coronary syndromes? Clin. Cardiol. 2004, 27, 80–86. [Google Scholar] [CrossRef] [PubMed]
- Woodward, M.; Webster, R.; Murakami, Y.; Barzi, F.; Lam, T.H.; Fang, X.; Suh, I.; Batty, G.D.; Huxley, R.; Rodgers, A. The association between resting heart rate, cardiovascular disease and mortality: Evidence from 112,680 men and women in 12 cohorts. Eur. J. Prev. Cardiol. 2014, 21, 719–726. [Google Scholar] [CrossRef] [PubMed]
- Bohm, M.; Swedberg, K.; Komajda, M.; Borer, J.S.; Ford, I.; Dubost-Brama, A.; Lerebours, G.; Tavazzi, L. Heart rate as a risk factor in chronic heart failure (shift): The association between heart rate and outcomes in a randomised placebo-controlled trial. Lancet 2010, 376, 886–894. [Google Scholar] [CrossRef]
- Ho, J.E.; Bittner, V.; Demicco, D.A.; Breazna, A.; Deedwania, P.C.; Waters, D.D. Usefulness of heart rate at rest as a predictor of mortality, hospitalization for heart failure, myocardial infarction, and stroke in patients with stable coronary heart disease (data from the treating to new targets [TNT] trial). Am. J. Cardiol. 2010, 105, 905–911. [Google Scholar] [CrossRef]
- Tverdal, A.; Hjellvik, V.; Selmer, R. Heart rate and mortality from cardiovascular causes: A 12 year follow-up study of 379,843 men and women aged 40-45 years. Eur. Heart J. 2008, 29, 2772–2781. [Google Scholar] [CrossRef]
- Palatini, P.; Julius, S. Association of tachycardia with morbidity and mortality: Pathophysiological considerations. J. Hum. Hypertens. 1997, 11 Suppl 1, S19–S27. [Google Scholar]
- Fox, K.; Borer, J.S.; Camm, A.J.; Danchin, N.; Ferrari, R.; Lopez Sendon, J.L.; Steg, P.G.; Tardif, J.C.; Tavazzi, L.; Tendera, M. Resting heart rate in cardiovascular disease. J. Am. Coll. Cardiol. 2007, 50, 823–830. [Google Scholar] [CrossRef] [PubMed]
- Palatini, P.; Julius, S. Elevated heart rate: A major risk factor for cardiovascular disease. Clin. Exp. Hypertens. 2004, 26, 637–644. [Google Scholar] [CrossRef] [PubMed]
- Alhalabi, L.; Singleton, M.J.; Oseni, A.O.; Shah, A.J.; Zhang, Z.M.; Soliman, E.Z. Relation of higher resting heart rate to risk of cardiovascular versus noncardiovascular death. Am. J. Cardiol. 2017, 119, 1003–1007. [Google Scholar] [CrossRef]
- Greenland, P.; Daviglus, M.L.; Dyer, A.R.; Liu, K.; Huang, C.F.; Goldberger, J.J.; Stamler, J. Resting heart rate is a risk factor for cardiovascular and noncardiovascular mortality: The chicago heart association detection project in industry. Am. J. Epidemiol. 1999, 149, 853–862. [Google Scholar] [CrossRef] [PubMed]
- Seviiri, M.; Lynch, B.M.; Hodge, A.M.; Yang, Y.; Liew, D.; English, D.R.; Giles, G.G.; Milne, R.L.; Dugue, P.A. Resting heart rate, temporal changes in resting heart rate, and overall and cause-specific mortality. Heart 2018, 104, 1076–1085. [Google Scholar] [CrossRef]
- Jouven, X.; Escolano, S.; Celermajer, D.; Empana, J.P.; Bingham, A.; Hermine, O.; Desnos, M.; Perier, M.C.; Marijon, E.; Ducimetiere, P. Heart rate and risk of cancer death in healthy men. PLoS ONE 2011, 6, e21310. [Google Scholar] [CrossRef]
- Cole, S.W.; Sood, A.K. Molecular pathways: Beta-adrenergic signaling in cancer. Clin. Cancer Res. 2012, 18, 1201–1206. [Google Scholar] [CrossRef]
- Masur, K.; Niggemann, B.; Zanker, K.S.; Entschladen, F. Norepinephrine-induced migration of SW 480 colon carcinoma cells is inhibited by β-blockers. Cancer Res. 2001, 61, 2866–2869. [Google Scholar]
- Guo, K.; Ma, Q.; Wang, L.; Hu, H.; Li, J.; Zhang, D.; Zhang, M. Norepinephrine-induced invasion by pancreatic cancer cells is inhibited by propranolol. Oncol. Rep. 2009, 22, 825–830. [Google Scholar]
- van Kruijsdijk, R.C.; van der Graaf, Y.; Bemelmans, R.H.; Nathoe, H.M.; Peeters, P.H.; Visseren, F.L. The relation between resting heart rate and cancer incidence, cancer mortality and all-cause mortality in patients with manifest vascular disease. Cancer Epidemiol. 2014, 38, 715–721. [Google Scholar] [CrossRef]
- Anker, M.S.; Ebner, N.; Hildebrandt, B.; Springer, J.; Sinn, M.; Riess, H.; Anker, S.D.; Landmesser, U.; Haverkamp, W.; von Haehling, S. Resting heart rate is an independent predictor of death in patients with colorectal, pancreatic, and non-small cell lung cancer: Results of a prospective cardiovascular long-term study. Eur. J. Heart Fail. 2016, 18, 1524–1534. [Google Scholar] [CrossRef] [PubMed]
- Jansen, L.; Weberpals, J.; Kuiper, J.G.; Vissers, P.A.J.; Wolkewitz, M.; Hoffmeister, M.; Brenner, H. Pre- and post-diagnostic beta-blocker use and prognosis after colorectal cancer: Results from a population-based study. Int. J. Cancer Res. 2017, 141, 62–71. [Google Scholar] [CrossRef] [PubMed]
- Hicks, B.M.; Murray, L.J.; Powe, D.G.; Hughes, C.M.; Cardwell, C.R. Beta-blocker usage and colorectal cancer mortality: A nested case-control study in the UK clinical practice research datalink cohort. Ann. Oncol. 2013, 24, 3100–3106. [Google Scholar] [CrossRef] [PubMed]
- Jansen, L.; Hoffmeister, M.; Arndt, V.; Chang-Claude, J.; Brenner, H. Stage-specific associations between beta blocker use and prognosis after colorectal cancer. Cancer 2014, 120, 1178–1186. [Google Scholar] [CrossRef] [PubMed]
- Park, J.; Kim, J.H.; Park, Y.; Park, S.J.; Cheon, J.H.; Kim, W.H.; Park, J.S.; Jeon, J.Y.; Kim, T.I. Resting heart rate is an independent predictor of advanced colorectal adenoma recurrence. PLoS ONE 2018, 13, e0193753. [Google Scholar] [CrossRef] [PubMed]
- Kweon, S.; Kim, Y.; Jang, M.J.; Kim, Y.; Kim, K.; Choi, S.; Chun, C.; Khang, Y.H.; Oh, K. Data resource profile: The korea national health and nutrition examination survey (knhanes). Int. J. Epidemiol. 2014, 43, 69–77. [Google Scholar] [CrossRef]
- Korea Centers for Disease Control and Prevention. The Korea National Health and Nutrition Examination Survey. Available online: https://knhanes.cdc.go.kr/knhanes/main.do (accessed on 5 April 2019).
- Hari, D.M.; Leung, A.M.; Lee, J.H.; Sim, M.S.; Vuong, B.; Chiu, C.G.; Bilchik, A.J. AJCC cancer staging manual 7th edition criteria for colon cancer: Do the complex modifications improve prognostic assessment? J. Am. Coll. Surg. 2013, 217, 181–190. [Google Scholar] [CrossRef]
- World Health Organization. The Asia-Pacific Perspective: Redefining Obesity and Its Treatment; Health Communications Australia: Sydney, Australia, 2000. [Google Scholar]
- Fitzgerald, P.J. Is norepinephrine an etiological factor in some types of cancer? Int. J. Cancer 2009, 124, 257–263. [Google Scholar] [CrossRef]
- Zhong, S.; Yu, D.; Zhang, X.; Chen, X.; Yang, S.; Tang, J.; Zhao, J.; Wang, S. Beta-blocker use and mortality in cancer patients: Systematic review and meta-analysis of observational studies. Eur. J. Cancer Prev. 2016, 25, 440–448. [Google Scholar] [CrossRef]
- Komninou, D.; Ayonote, A.; Richie, J.P., Jr.; Rigas, B. Insulin resistance and its contribution to colon carcinogenesis. Exp Biol Med 2003, 228, 396–405. [Google Scholar] [CrossRef]
- Zeman, R.J.; Ludemann, R.; Easton, T.G.; Etlinger, J.D. Slow to fast alterations in skeletal muscle fibers caused by clenbuterol, a beta 2-receptor agonist. Am. J. Physiol. 1988, 254, E726–E732. [Google Scholar] [CrossRef] [PubMed]
- Jamerson, K.A.; Smith, S.D.; Amerena, J.V.; Grant, E.; Julius, S. Vasoconstriction with norepinephrine causes less forearm insulin resistance than a reflex sympathetic vasoconstriction. Hypertension 1994, 23, 1006–1011. [Google Scholar] [CrossRef] [PubMed]
- Abbruzzese, C.; Diodoro, M.G.; Sperduti, I.; Mileo, A.M.; Pattaro, G.; De Salvo, L.; Cosimelli, M.; Perrotti, N.; Paggi, M.G. Detection of phosphorylated insulin receptor in colorectal adenoma and adenocarcinoma: Implications for prognosis and clinical outcome. J. Cell. Physiol. 2015, 230, 562–567. [Google Scholar] [CrossRef] [PubMed]
- van der Sijp, M.P.; Bastiaannet, E.; Mesker, W.E.; van der Geest, L.G.; Breugom, A.J.; Steup, W.H.; Marinelli, A.W.; Tseng, L.N.; Tollenaar, R.A.; van de Velde, C.J.; et al. Differences between colon and rectal cancer in complications, short-term survival and recurrences. Int. J. Colorectal Dis. 2016, 31, 1683–1691. [Google Scholar] [CrossRef] [PubMed]
- Wei, E.K.; Giovannucci, E.; Wu, K.; Rosner, B.; Fuchs, C.S.; Willett, W.C.; Colditz, G.A. Comparison of risk factors for colon and rectal cancer. Int. J. Cancer 2004, 108, 433–442. [Google Scholar] [CrossRef] [PubMed]
- Paschke, S.; Jafarov, S.; Staib, L.; Kreuser, E.D.; Maulbecker-Armstrong, C.; Roitman, M.; Holm, T.; Harris, C.C.; Link, K.H.; Kornmann, M. Are colon and rectal cancer two different tumor entities? A proposal to abandon the term colorectal cancer. Int. J. Mol. 2018, 19, 2577. [Google Scholar] [CrossRef] [PubMed]
- Kobayashi, H. Effect of measurement duration on accuracy of pulse-counting. Ergonomics 2013, 56, 1940–1944. [Google Scholar] [CrossRef]

| Variable | Control | Cases | p | ||||
|---|---|---|---|---|---|---|---|
| Colorectal | Colon | Rectum | †P | ‡P | §P | ||
| N | 5909 | 1241 | 854 | 387 | |||
| Age (years) | 47.3 ± 15.5 | 62.6 ± 11.8 | 63.4 ± 11.5 | 61.0 ± 12.4 | * | * | * |
| Gender | * | * | * | ||||
| Male | 2836 (48.0) | 712 (57.4) | 464 (54.3) | 248 (64.1) | |||
| Female | 3073 (52.0) | 529 (42.6) | 390 (45.7) | 139 (35.9) | |||
| SBP (mmHg) | 116.5 ± 15.6 | 126.0 ± 15.1 | 126.2 ± 15.1 | 125.4 ± 15.0 | * | * | * |
| DBP (mmHg) | 75.2 ± 10.2 | 77.2 ± 10.3 | 77.1 ± 10.3 | 77.5 ± 10.2 | * | * | * |
| RHR (bpm) | 68.7 ± 9.0 | 72.7 ± 11.3 | 72.8 ± 11.3 | 72.3 ± 11.3 | * | * | * |
| Weight status | * | * | NS | ||||
| Underweight | 2386 (40.4) | 555 (44.7) | 380 (44.5) | 175 (45.2) | |||
| Normal | 1442 (24.4) | 308 (24.8) | 217 (25.4) | 91 (23.5) | |||
| Overweight | 1844 (31.2) | 310 (25.0) | 210 (24.6) | 100 (25.8) | |||
| Obese | 237 (4.0) | 68 (5.5) | 47 (5.5) | 21 (5.4) | |||
| WBC (103 cells) | 6.2 ± 1.3 | 6.4 ± 1.5 | 6.6 ± 1.5 | 6.1 ± 1.4 | * | * | NS |
| Glucose (mg/dL) | 98.9 ± 21.1 | 109.4 ± 31.2 | 110.3 ± 32.5 | 107.5 ± 28.2 | * | * | * |
| TC (mg/dL) | 188.1 ± 33.7 | 176.1 ± 36.7 | 173.3 ± 35.7 | 182.1 ± 38.2 | * | * | * |
| HTN, n (%) | 913 (15.4) | 518 (41.7) | 374 (43.8) | 144 (37.2) | * | * | * |
| DM, n (%) | 371 (6.3) | 225 (18.1) | 161 (18.8) | 64 (16.5) | * | * | * |
| Dyslipidemia, n (%) | 405 (6.8) | 200 (16.1) | 147 (17.2) | 53 (13.7) | * | * | * |
| Alcohol | * | * | * | ||||
| Never | 602 (10.2) | 688 (55.4) | 492 (57.6) | 196 (50.7) | |||
| Ex | 804 (13.6) | 330 (26.6) | 187 (21.9) | 143 (37.0) | |||
| Current | 4503 (76.2) | 223 (18.0) | 175 (20.5) | 48 (12.4) | |||
| Smoking | * | * | * | ||||
| Never | 3383 (57.3) | 764 (61.5) | 552 (64.6) | 212 (54.8) | |||
| Ex | 1183 (20.0) | 362 (29.2) | 222 (26.0) | 140 (36.2) | |||
| Current | 1343 (22.7) | 115 (9.3) | 80 (9.4) | 35 (9.0) | |||
| TNM stage | |||||||
| 0 | - | 326 (26.3) | 187 (21.9) | 139 (35.9) | |||
| I | - | 365 (29.4) | 270 (31.6) | 95 (24.6) | |||
| II | - | 359 (28.9) | 257 (30.1) | 102 (26.4) | |||
| III | - | 191 (15.4) | 140 (16.4) | 51 (13.2) | |||
| Variable | Control | Colorectal | p | Control | Colon | p | Control | Rectum | p |
|---|---|---|---|---|---|---|---|---|---|
| N | 1207 | 1207 | 829 | 829 | 378 | 378 | |||
| Age (years) | 62.0 ± 11.4 | 62.0 ± 11.4 | NS | 62.7 ± 11.1 | 62.7 ± 11.1 | NS | 60.4 ± 12.0 | 60.4 ± 12.0 | NS |
| Gender | NS | NS | NS | ||||||
| Male | 695 (57.6) | 695 (57.6) | 452 (54.5) | 452 (54.5) | 243 (64.3) | 243 (64.3) | |||
| Female | 512 (42.4) | 512 (42.4) | 377 (45.5) | 377 (45.5) | 135 (35.7) | 135 (35.7) | |||
| SBP (mmHg) | 123.6 ± 16.1 | 125.6 ± 15.0 | * | 123.4 ± 16.3 | 126.1 ± 15.0 | * | 124.2 ± 15.9 | 125.4 ± 15.0 | NS |
| DBP (mmHg) | 75.6 ± 10.3 | 77.3 ± 10.3 | * | 75.4 ± 10.2 | 77.2 ± 10.3 | * | 76.3 ± 10.4 | 77.5 ± 10.2 | NS |
| RHR (bpm) | 67.6 ± 9.2 | 72.7 ± 11.3 | * | 67.8 ± 9.2 | 72.9 ± 11.4 | * | 67.1 ± 9.1 | 72.2 ± 11.3 | * |
| Weight status | * | * | * | ||||||
| Underweight | 28 (2.3) | 64 (5.3) | 18 (2.2) | 45 (5.4) | 10 (2.6) | 19 (5.0) | |||
| Normal | 423 (35.1) | 543 (45.0) | 302 (36.4) | 372 (44.9) | 121 (32.0) | 171 (45.2) | |||
| Overweight | 338 (28.0) | 302 (25.0) | 226 (27.3) | 211 (25.5) | 112 (29.6) | 91 (24.1) | |||
| Obese | 418 (34.3) | 298 (24.7) | 283 (34.1) | 201 (24.3) | 135 (35.7) | 97 (25.7) | |||
| WBC (103 cells) | 6.2 ± 1.3 | 6.4 ± 1.5 | * | 6.1 ± 1.3 | 6.6 ± 1.5 | * | 6.2 ± 1.3 | 6.1 ± 1.4 | NS |
| Glucose (mg/dL) | 103.6 ± 22.0 | 109.3 ± 31.1 | * | 102.9 ± 20.7 | 110.2 ± 32.3 | * | 105.2 ± 24.6 | 107.5 ± 28.1 | NS |
| TC (mg/dL) | 191.2 ± 34.7 | 177.0 ± 36.4 | * | 192.0 ± 34.7 | 174.4 ± 35.3 | * | 189.5 ± 34.6 | 182.6 ± 38.2 | * |
| HTN, n (%) | 381 (31.6) | 497 (41.18) | * | 278 (33.5) | 357 (43.1) | * | 103 (27.2) | 140 (37.0) | * |
| DM, n (%) | 148 (12.3) | 216 (17.90) | * | 102 (12.3) | 157 (18.9) | * | 46 (12.2) | 59 (15.6) | NS |
| Dyslipidemia,n (%) | 130 (10.77) | 193 (16.0) | * | 100 (12.1) | 141 (17.0) | * | 30 (7.9) | 52 (13.8) | * |
| Alcohol | * | * | * | ||||||
| Never | 189 (15.7) | 659 (54.6) | 149 (18.0) | 470 (56.7) | 40 (10.6) | 189 (50.0) | |||
| Ex | 220 (18.2) | 325 (26.9) | 151 (18.2) | 184 (22.2) | 69 (18.2) | 141 (37.3) | |||
| Current | 798 (66.1) | 223 (18.5) | 529 (63.8) | 175 (21.1) | 269 (71.2) | 48 (12.7) | |||
| Smoking | * | * | * | ||||||
| Never | 591 (49.0) | 740 (61.3) | 430 (51.9) | 533 (64.3) | 161 (42.6) | 207 (54.8) | |||
| Ex | 351 (29.1) | 352 (29.2) | 237 (28.6) | 216 (26.1) | 114 (30.2) | 136 (36.0) | |||
| Current | 265 (21.9) | 115 (9.5) | 162 (19.5) | 80 (9.6) | 103 (27.3) | 35 (9.2) | |||
| TNM stage | |||||||||
| 0 | - | 320 (26.5) | - | 184 (22.2) | - | 136 (36.0) | |||
| I | - | 353 (29.3) | - | 260 (31.4) | - | 93 (24.6) | |||
| II | - | 345 (28.6) | - | 246 (29.7) | - | 99 (26.2) | |||
| III | - | 189 (15.7) | - | 139 (16.8) | - | 50 (13.2) |
| Model | Colorectal Cancer | Colon Cancer | Rectal Cancer | |||
|---|---|---|---|---|---|---|
| OR (95% CIs) | p | OR (95% CIs) | p | OR (95% CIs) | p | |
| Before PS matching | ||||||
| Univariable * | 1.043 (1.036–1.049) | <0.001 | 1.045 (1.037–1.053) | <0.001 | 1.040 (1.030–1.051) | <0.001 |
| Multivariable † | 1.043 (1.034–1.051) | <0.001 | 1.046 (1.037–1.055) | <0.001 | 1.040 (1.027–1.052) | <0.001 |
| After PS matching | ||||||
| Univariable ** | 1.051 (1.042–1.060) | <0.001 | 1.050 (1.039–1.061) | <0.001 | 1.053 (1.036–1.070) | <0.001 |
| Multivariable ‡ | 1.044 (1.032–1.057) | <0.001 | 1.046 (1.032–1.061) | <0.001 | 1.035 (1.008–1.063) | <0.001 |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Kwon, Y.-J.; Lee, H.S.; Cho, M.R.; Kim, S.N.; Jeon, J.Y.; Kim, N.K.; Lee, J.-W. Association between Resting Heart Rate and Colorectal Cancer: Results from a Case-Controlled Study. Int. J. Environ. Res. Public Health 2019, 16, 2883. https://doi.org/10.3390/ijerph16162883
Kwon Y-J, Lee HS, Cho MR, Kim SN, Jeon JY, Kim NK, Lee J-W. Association between Resting Heart Rate and Colorectal Cancer: Results from a Case-Controlled Study. International Journal of Environmental Research and Public Health. 2019; 16(16):2883. https://doi.org/10.3390/ijerph16162883
Chicago/Turabian StyleKwon, Yu-Jin, Hye Sun Lee, Mi Ra Cho, Si Nae Kim, Justin Y. Jeon, Nam Kyu Kim, and Ji-Won Lee. 2019. "Association between Resting Heart Rate and Colorectal Cancer: Results from a Case-Controlled Study" International Journal of Environmental Research and Public Health 16, no. 16: 2883. https://doi.org/10.3390/ijerph16162883
APA StyleKwon, Y.-J., Lee, H. S., Cho, M. R., Kim, S. N., Jeon, J. Y., Kim, N. K., & Lee, J.-W. (2019). Association between Resting Heart Rate and Colorectal Cancer: Results from a Case-Controlled Study. International Journal of Environmental Research and Public Health, 16(16), 2883. https://doi.org/10.3390/ijerph16162883






