Assessment of Nursing Care and Teaching: A Qualitative Approach
Abstract
1. Introduction
2. Materials and Methods
2.1. Research Team and Reflexivity
2.2. Study Design
2.3. Data Collection
2.4. Data Analysis
2.5. Ethical Considerations
3. Results
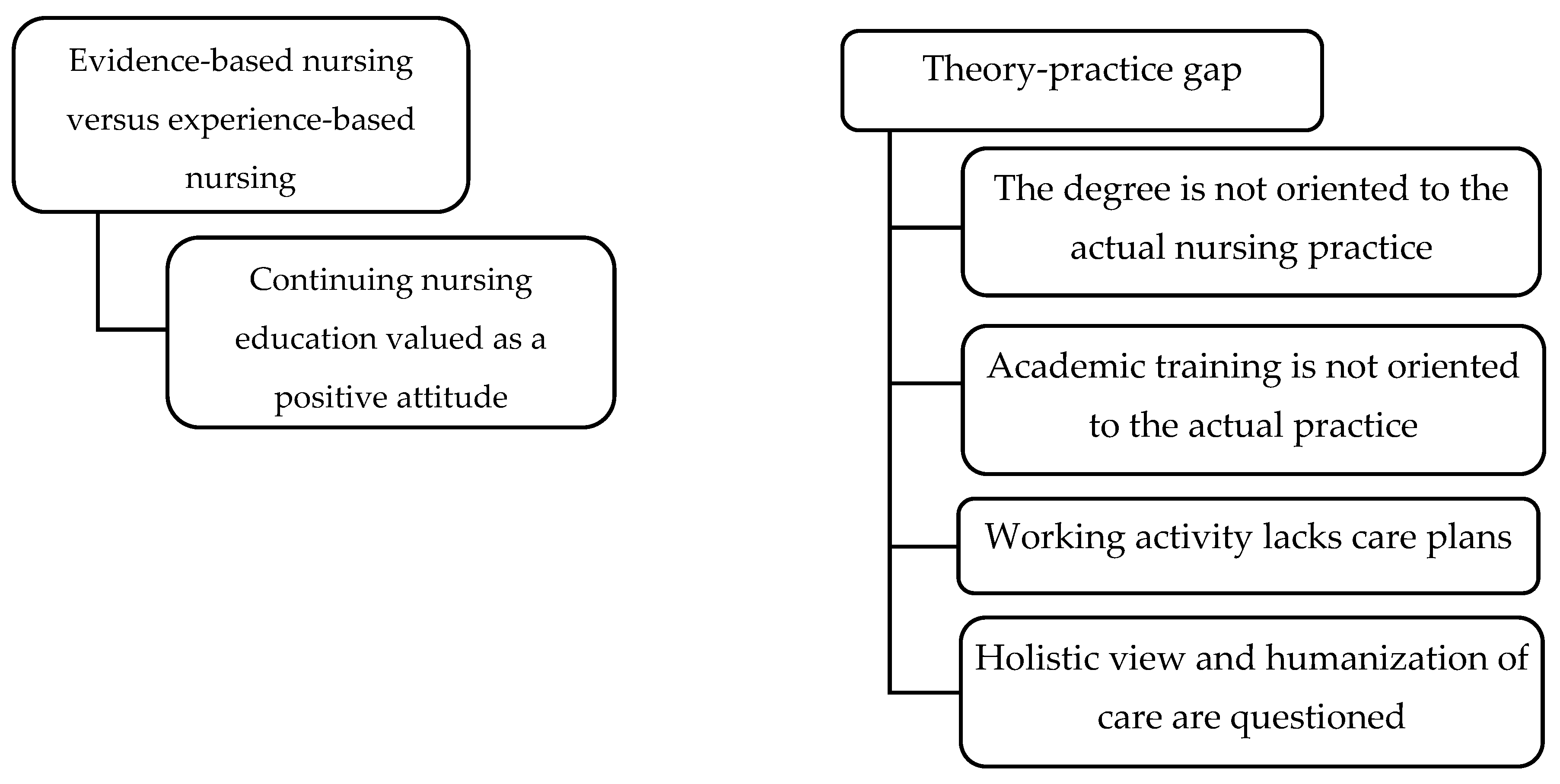
3.1. EBN vs. Experience-Based Nursing
“In the operating room, for example, I did. Clinical practice guidelines were available whenever I wanted to read them, there was no problem. However, in other units, it is complicated, especially in primary care. In primary care, there is just no guidance practically.”(E12)
“One of my biggest weaknesses in working as a nurse is not being able to explain why some things are done, grounding certain things… I mean… evidence-based nursing practice. When it comes to protocols, there were a lot of them, but none of them were followed.”(E2)
Continuing Nursing Education Valued as a Positive Attitude
“If the workers are recently graduated or just young, they are more likely to have been trained in information searching, papers, etc.[…] And then you find people who, although there are protocols of action or clinical practice guidelines, they just don’t follow them because, according to them, it’s how they’re used to working, they do it that way and they think it’s better.”(E5)
“I think so, there are many contradictions […] and here they are telling you one thing and there you come across another. Then, you get confused, because you don’t know what’s well done and what’s not.”(GF2-P11)
3.2. Theory-Practice Gap
3.2.1. The Degree Is Not Oriented to Actual Nursing Practice
“Then, reality is other and, OK, they explain a theory to you, but then, when you get to the practice, everything is totally different, so…”(E5)
“That’s fine, but then there are also services […] whose way to work is unknown to me, I just don’t know what I’m going to find there, and there are others that I do know, […] and I think the snag is in the course itself, if the course approaches disorders in a certain way, that is finally the idea that you build in your head…”(GF2-P10)
“I believe that the global vision of what a nursing degree is, which is to train general nurses, and not researchers or specialist nurses, has been somewhat lost. […] Because they are very basic things, but things that cannot be taught only in one or two short placements, but in every course.”(GF1-P1)
3.2.2. Academic Training Is Not Oriented to Actual Practice
“But, for example, they teach us intubation… We don’t do intubation; it’s good to know in case that, by any chance, it must be done because there is no one else to do it. But there are also many techniques that you do in the hospital and which you haven’t been taught in university, techniques you eventually learn in the placements.”(E7)
“I want to point out that, we work on a lot of topics during the lectures, topics which then don’t fit in so well with actual practice. The lectures then should be more focused on how to use some devices in order to prevent those typical situations in which we say: I’ve never seen this and I don’t know how to do it.”(GF1-P6)
“It’s true that the problem is that there are courses that are six-monthly, or perhaps four-monthly, and maybe they should be annual.”(E5)
“I understand that there are courses that have to be there, because they have to, but these don’t contribute much, and they are given a lot of importance. There are very important courses that have lost importance […]”(E1)
“Yes, indeed. Nurses who both work and teach transmit knowledge that is much more adapted to reality, you don’t feel that they have the head in the clouds.”(GF1-P5)
“In addition, you can see that there are teachers who haven’t worked in hospitals for many years and you say “that’s impossible…!” […] And you realize it’s impossible. And you make comments like: Yes, that would happen in the ‘90s. And you are like… The difference lies in experience, uh? But… tell me that as an anecdote, it’s not done anymore. […] And besides, some courses are quite old-fashioned, so you say: This was done in the past… but not anymore.”(E3)
3.2.3. Working Activity Lacks Care Plans
“Yes, with regard to the Nursing Care Plan (NCP) that we studied… here you can study them, and I think they’re useful, but… I think they can’t be implemented because it takes a lot of time to carry them out too.”(E3)
“I want to point out that we really worked on the NCP in lectures, which then don’t fit in so well with actual practice. Yes, they have to teach you how to make an NCP, but here in lectures you should be more focused on other topics, because then you start working […] and you say: I’ve never seen this in my life and I do not know how to do it.”(GF1-P6)
3.2.4. Holistic View and Humanization of Care Are Questioned
“It’s the nursing concept I like, but not the one I see, because… it’s true that at university the subject of humanization often arises, and we deal with people and humanize and humanize and humanize and humanize… And that’s from the day you start until the day you leave. And I think it’s very important. But it’s not what you see at the hospital. […] “Patient from room No. X” or… “The man in that room”. People don’t seem to have names.”(E3)
“I think the same, it also depends on the nurse. However, in one service, for example, what caught my attention was that the nurse introduced me to all the patients one by one on the first day, and that was interesting.”(GF2-P10)
4. Discussion
Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- European Higher Education Area. Available online: http://www.eees.es/pdf/Bolonia_ES.pdf (accessed on 8 January 2019).
- Tuning Educational Structures in Europe II. Universities’ Contribution to the Bologna Process. Available online: http://tuningacademy.org/wp-content/uploads/2014/02/TuningEUI_Final-Report_SP.pdf (accessed on 8 January 2019).
- European Association for Quality Assurance in Higher Education, European Students’ Union, European University Association & European Association of Institutions in Higher Education. Available online: https://enqa.eu/wp-content/uploads/2015/11/ESG_2015.pdf (accessed on 8 January 2019).
- Carr, W. Theories of Theory and Practice. J. Philos. Educ. 1986, 20, 177–186. [Google Scholar] [CrossRef]
- Cody, W. Critical Thinking and Nursing Science: Judgment, or Vision? Nurs. Sci. Q. 2002, 15, 184–189. [Google Scholar] [CrossRef] [PubMed]
- Lafuente, J.V.; Escanero, J.F.; Manso, J.M.; Mora, S.; Miranda, T.; Castillo, M.; Díaz-Veliz, G.; Gargiulo, P.; Bianchi, R.; Gorena, D.; et al. El diseño curricular por competencias en educación médica: Impacto en la formación profesional. Educ. Med. 2007, 10, 86–92. [Google Scholar] [CrossRef]
- Upton, D.J. How can we achieve evidence-based practice if we have a theory-practice gap in nursing today? J. Adv. Nurs. 1999, 29, 549–555. [Google Scholar] [CrossRef] [PubMed]
- Matesanz, M.A. Pasado, presente y futuro de la Enfermería: Una aptitud constante. Rev. Admin. Sanit Siglo Xxi 2009, 7, 243–260. [Google Scholar]
- Stavrou, A.; Challoumas, D.; Dimitrakakis, G. Archibald Cochrane (1909–1988): The father of evidence-based medicine. Interact. Cardiovasc. Thorac. Surg. 2014, 18, 121–124. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Shah, H.M.; Chung, K.C. Archie Cochrane and his vision for evidence-based medicine. Plast Reconstr. Surg. 2009, 124, 982–988. [Google Scholar] [CrossRef] [PubMed]
- Fineout-Overholt, E.; Melnyk, B.M.; Schultz, A. Transforming health care from the inside out: Advancing evidence-based practice in the 21st century. J. Prof. Nurs. 2005, 21, 335–344. [Google Scholar] [CrossRef]
- Tong, A.; Sainsbury, P.; Craig, J. Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. Int. J. Qual. Health C 2007, 19, 349–357. [Google Scholar] [CrossRef]
- Creswell, J. Qualitative Inquiry and Research Design: Choosing Among Five Approaches, 3rd ed.; Sage: Los Angeles, CA, USA, 2013; pp. 105–131. [Google Scholar]
- Ward, G.; Dixon, H. The research masters experience: The impact of efficacy and outcome expectations on enrolment and completion. J. Furth. High. Educ. 2014, 38, 163–181. [Google Scholar] [CrossRef]
- Morse, J.M. Data were saturated. Qual. Health Res. 2015, 25, 587–588. [Google Scholar] [CrossRef] [PubMed]
- McLenan, S.R.; Diebold, M.; Rich, L.E.; Elger, B.S. Nurses´s perspectives regarding the disclosure of errors to patients: A qualitative study. Int. J. Nurs. Stud. 2016, 54, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qual. Res. Psychol. 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Flemming, K. Asking answerable questions. Evid. Based Nurs. 1998, 1, 36–37. [Google Scholar] [CrossRef]
- Sackett, D.L.; Rosenberg, W.M.; Gray, J.A.; Haynes, R.B.; Richardson, W.S. Evidence based medicine: What it is and what it isn’t. BMJ 1996, 312, 71–72. [Google Scholar] [CrossRef] [PubMed]
- Martínez, J. Barreras e instrumentos facilitadores de la enfermería basada en la evidencia. Enfer Clin. 2003, 13, 303–308. [Google Scholar] [CrossRef]
- Dalheim, A.; Harthug, S.; Nilsen, R.M.; Nortvedt, M.W. Factors influencing the development of evidence-based practice among nurses: A self-report survey. BMC Health Serv. Res. 2012, 12, 367. [Google Scholar] [CrossRef] [PubMed]
- Milner, F.M.; Estabrooks, C.A.; Humphrey, C. Clinical nurse educators as agents for change: Increasing research utilization. Int. J. Nurs. Stud. 2005, 42, 899–914. [Google Scholar] [CrossRef]
- Zabalegui, A.; Cabrera, E. New nursing education in Spain. Nurs. Educ. Today 2009, 31, 500–504. [Google Scholar] [CrossRef]
- Granollers, R.; Montanuy, T.; Estany, P.; Roca, B.; Ortega, B. Do nurses utilize the scientific method? Rev. Enferm. 2006, 29, 29–32. [Google Scholar]
- Cachón-Pérez, J.M.; Alvarez-López, C.; Palacios-Ceña, D. The meaning of standardized language NANDA-NIC-NOC intensive care nurses in Madrid: A phenomenological approach. Enferm. Intensiva 2012, 23, 68–76. [Google Scholar] [PubMed]
- Fernández, M.A.C. Lenguajes estandarizados de enfermería. Evidentia 2007, 4. Available online: http://www.index-f.com/evidentia/n17/r376articulo.php (accessed on 25 January 2019).
- Boletín Oficial del Estado. Real Decreto 1093/2010, de 3 de Septiembre, por el que se Aprueba el Conjunto Mínimo de Datos de los Informes Clínicos en el Sistema Nacional de Salud. Available online: https://www.boe.es/boe/dias/2010/09/16/pdfs/BOE-A-2010-14199.pdf (accessed on 15 February 2019).
- Santos, S. Factores Determinantes del uso de Modelos Teóricos en la Práctica Enfermera. Ph.D. Thesis, Universitat Jaume I, Castellón de la Plana, Spain, May 2014. [Google Scholar]
- Wennberg, J.E. Unwanted variations in the rules of practice. JAMA 1991, 265, 1306–1307. [Google Scholar] [CrossRef] [PubMed]
- Marión, J.; Peiró, S.; Márquez, S.; Meneu, R. Variaciones en la práctica médica: Importancia, causas e implicaciones. Med. Clin. 1998, 110, 382–390. [Google Scholar]
- Fernández-de-Maya, J.; Richard-Martínez, M. Variabilidad de la práctica clínica. Situación actual y retos para enfermería. Enferm. Clin. 2010, 20, 114–118. [Google Scholar]
- Ajani, K.; Moez, S. Gap between knowledge and practice in nursing. Procedia Soc. Behav. Sci. 2011, 15, 3927–3931. [Google Scholar] [CrossRef]
- Cook, S. Mind the theory/practice gap in nursing. J. Adv. Nurs. 1991, 16, 1462–1469. [Google Scholar] [CrossRef]
- Landers, M. The theory/practice gap in nursing: The views of the students. Irel. J. Nurs. Midwifery 2002, 1, 142–147. [Google Scholar]
- El Hussein, M.T.; Osuji, J. Bridging the theory-practice dichotomy in nursing: The role of nurse educators. J. Nurs. Educ. Pract. 2017, 7, 20–25. [Google Scholar] [CrossRef]
- Rolfe, G. Closing the theory-practice gap: A model of nursing praxis. J. Clin. Nurs. 1993, 3, 173–177. [Google Scholar] [CrossRef]
- Alexander, J.G.; McDaniel, G.S.; Baldwin, M.S.; Money, B.J. Promoting, applying and evaluating problem-based learning in the undergraduate nursing curriculum. Nurs. Educ. Perspect. 2002, 23, 248–253. [Google Scholar] [PubMed]
- Gallagher, P. How the metaphor of a gap between theory and practice has influenced nursing education. Nurs. Educ. Today 2004, 24, 263–268. [Google Scholar] [CrossRef] [PubMed]
- Higginson, R. The theory-practice gap still exists in nursing. BJN 2004, 13, 68. [Google Scholar] [CrossRef] [PubMed]
- Maben, J.; Latter, S.; Macleod, J. The theory-practice gap: Impact of professional-bureaucratic work conflict on newly qualified nurses. J. Adv. Nurs. 2006, 55, 465–477. [Google Scholar] [CrossRef] [PubMed]
- Martin, G.; Mitchell, G. A study of critical incident analysis as a route to the identification of change necessary in clinical practice: Addressing the theory-practice gap. Nurs. Educ. Pract. 2001, 1, 27–34. [Google Scholar] [CrossRef] [PubMed]
- Bennett, L.L.; Grimsley, A.; Grimsley, L.; Rodd, J. The Gap between Nursing Education and Clinical Skills. ABNF J. 2017, 28, 96–102. [Google Scholar]
- Saifan, A.; AbuRuz, M.E.; Masa’deh, R. Theory Practice Gaps in Nursing Education: A Qualitative Perspective. J. Soc. Sci. 2015, 11, 20–29. [Google Scholar] [CrossRef]
- Arreciado, A.; Isla, M.P. Theory and practice in the construction of professional identity in nursing students: A qualitative study. Nurs. Educ. Today 2015, 35, 859–863. [Google Scholar] [CrossRef]
- Brasell, B.R.; Vallance, E. Clinical practice/education exchange: Bridging the theory-practice gap. Nurs. Prax N. Z. 2002, 18, 17–26. [Google Scholar]
- Edwards, S. Nursing knowledge: Defining new boundaries. Nurs. Stand. 2002, 17, 40–44. [Google Scholar] [CrossRef]
- Landers, M. The theory-practice gap in nursing: The role of the nurse teacher. J. Adv. Nurs. 2000, 32, 1550–1556. [Google Scholar] [CrossRef] [PubMed]
- Riksaasen, I.K. The theory-practice relationship: Reflective skills and theoretical knowledge as key factors in bridging the gap between theory and practice in initial nursing education. J. Adv. Nurs. 2012, 68, 868–877. [Google Scholar]
- Medina, J.L. The Desire to Provide Care and the Will to Do So; The Teaching of Nursing, Publicacions i Edicions Universitat de Barcelona: Barcelona, Spain, 2005; pp. 102–141. [Google Scholar]
- Estrada-Masllorens, J.M.; Galimany-Masclans, J.; Constantí-Balasch, M. Enseñanza universitaria de enfermería: De la diplomatura al grado. FEM 2016, 19, 71–76. [Google Scholar] [CrossRef]
- Pérez, N.; Amezcua, M. Entre la disociación y la armonía: La compleja relación entre teoría y práctica enfermera. Index Enferm. 2017, 26, 245–247. [Google Scholar]
- American Holistic Nurses Association. Holistic Nursing: Scope and Standards of Practice. Available online: http://samples.jbpub.com/9781449651756/45632_CH02_Pass1.pdf (accessed on 15 January 2019).
- Marriner, T.A.; Raile, A.M. Modelos y Teorías en Enfermería, 7th ed.; Elsevier: Madrid, Spain, 2011; pp. 242–265. [Google Scholar]
- Peplau, H. Relaciones Interpersonales en Enfermería. Un marco de Referencia Conceptual en Enfermería Psicodinámica; Salvat: Barcelona, España, 1990; pp. 125–136. [Google Scholar]
- Watson, J. Nursing: Human Science and Human Care; Appleton Century Croft: Appleton, WI, USA, 1985; pp. 86–102. [Google Scholar]
- Arredondo-González, C.P.; Siles-González, J. Tecnología y Humanización de los Cuidados. Una mirada desde la Teoría de las Relaciones Interpersonales. Index Enferm. 2009, 18, 32–36. [Google Scholar]
- Standards and Guidelines for Quality Assurance in the European Higher Education Area. ESG 2015. Available online: https://enqa.eu/wp-content/uploads/2015/11/ESG_2015.pdf (accessed on 30 July 2019).
| Personal Interviews | Focus Groups | ||||||
|---|---|---|---|---|---|---|---|
| Interview Code | Age | Sex | Work Experience in Months | Graduation Year | Focus Group Code | Age | Sex |
| E1 | 26 | Woman | 3 | 2017 | GF1-P1 | 40 | Woman |
| E2 | 23 | Woman | 4 | 2016 | GF1-P2 | 21 | Man |
| E3 | 25 | Woman | 7.5 | 2016 | GF1-P3 | 21 | Man |
| E4 | 23 | Woman | 3 | 2016 | GF1-P4 | 23 | Woman |
| E5 | 23 | Man | 3 | 2016 | GF1-P5 | 22 | Woman |
| E6 | 25 | Woman | 3 | 2015 | GF1-P6 | 24 | Woman |
| E7 | 23 | Woman | 9 | 2016 | GF2-P7 | 21 | Man |
| E8 | 28 | Woman | 6 | 2017 | GF2-P8 | 23 | Man |
| E9 | 25 | Woman | 6 | 2016 | GF2-P9 | 51 | Man |
| E10 | 28 | Man | 9 | 2017 | GF2-P10 | 21 | Man |
| E11 | 25 | Man | 12 | 2015 | GF2-11 | 21 | Woman |
| E12 | 51 | Man | 12 | 2015 | GF2-P12 | 22 | Man |
| Pre-Established Categories | Primary Questions |
|---|---|
| Clinical training | Which rotating internship was your favorite? Can you explain why?What nursing techniques did you practice? Could you practice them all?Were you involved in any difficult emotional situation that a patient/family member was going through? Can you explain how you felt and how you helped them? |
| Theoretical/Academic training | Are you satisfied with what you learned at a theoretical level during the degree? Can you explain your experience?Which courses do you think are most important? Can you explain why?Would you make any change to the academic curriculum? |
| Working situation | How do you evaluate your transition from study to work?What kind of difficulties have you experienced working as a nurse?Which circumstances cause you stress in your day-to-day work? |
| Themes | Subthemes | Codes |
|---|---|---|
| Evidence-based nursing vs. experience-based nursing | Retrained vs. non-retrained nursing professionals | EBN in daily work, retrained nurses and stagnant nurses, no widespread use of guidelines and protocols, professionals working according to their experience, differences among EBN training professionals. |
| Theory-practice gap | The degree is not oriented to the actual nursing practice | Course not adapted to the actual healthcare situation, number of credits not adequate to the relevance of a course, reorganization of courses, contents not adapted to reality. |
| Academic training not oriented to the actual practice | Adaptation of theory to actual healthcare situation, difference between theory and healthcare practice, reorganization of clinical placements, reorganization of courses. | |
| Working without care plans | Care plans not used in actual practice, too much attention to care plans in class. | |
| Holistic vision and humanization of care into question | Dehumanization at work, forgetting the holistic vision of the person, greater importance to techniques than to humanization and holistic vision. |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Martínez-Linares, J.M.; Martínez-Yébenes, R.; Andújar-Afán, F.A.; López-Entrambasaguas, O.M. Assessment of Nursing Care and Teaching: A Qualitative Approach. Int. J. Environ. Res. Public Health 2019, 16, 2774. https://doi.org/10.3390/ijerph16152774
Martínez-Linares JM, Martínez-Yébenes R, Andújar-Afán FA, López-Entrambasaguas OM. Assessment of Nursing Care and Teaching: A Qualitative Approach. International Journal of Environmental Research and Public Health. 2019; 16(15):2774. https://doi.org/10.3390/ijerph16152774
Chicago/Turabian StyleMartínez-Linares, Jose Manuel, Rocío Martínez-Yébenes, Francisco Antonio Andújar-Afán, and Olga María López-Entrambasaguas. 2019. "Assessment of Nursing Care and Teaching: A Qualitative Approach" International Journal of Environmental Research and Public Health 16, no. 15: 2774. https://doi.org/10.3390/ijerph16152774
APA StyleMartínez-Linares, J. M., Martínez-Yébenes, R., Andújar-Afán, F. A., & López-Entrambasaguas, O. M. (2019). Assessment of Nursing Care and Teaching: A Qualitative Approach. International Journal of Environmental Research and Public Health, 16(15), 2774. https://doi.org/10.3390/ijerph16152774





