Developing an Awareness Campaign to Reduce Second Hand Smoke Among Disadvantaged Families—A Participatory M-Health Approach
Abstract
1. Introduction
2. Materials and Methods
2.1. Phase 1: Semi-Structured Interviews
2.2. Phase 2: Focus Group Discussions
2.3. Phase 3: Quantitative Assessment
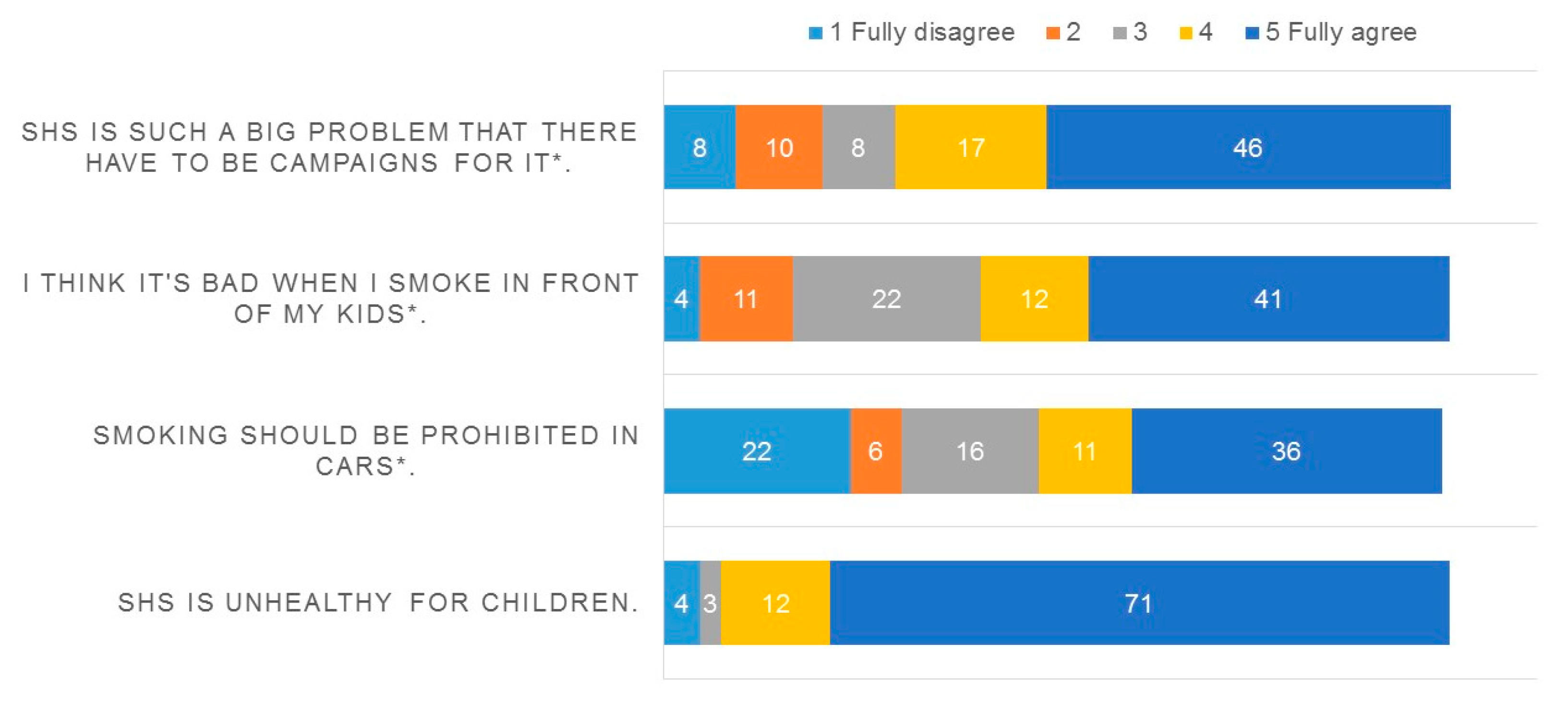
- Attitude towards SHS (4 items)
- Evaluation of each of the illustrations:
- ◦
- First impression (1 item)
- ◦
- Appeal (1 item)
- ◦
- Quality (5 items)
- ◦
- Intention to share in social media (4 items)
- Overall evaluation of the campaign:
- ◦
- Suitability for social media (3 items)
- ◦
- Content (3 items)
- ◦
- Effectiveness (4 items)
2.4. Statistical Analyses
3. Results
3.1. Phase 1: Semi-Structured Interviews
3.2. Phase 2: Focus Group Discussions
3.3. Phase 3: Quantitative Assessment
3.4. Evaluation of the Individual Campaign Illustrations
3.5. Overall Evaluation of the Campaign
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgements
Conflicts of Interest
References
- WHO Global Report: Mortality Attributable to Tobacco. Available online: http://www.who.int/tobacco/publications/surveillance/rep_mortality_attributable/en/ (accessed on 5 September 2018).
- Rockville. The Health Consequences of Smoking—50 Years of Progress. A Report of the Surgeon General; U.S. Department of Health and Human Servives: Atlanta, GA, USA, 2014.
- Tabakrauchbelastung von Kindern in Bayern: Ansatzpunkte für Gesundheitsförderungsstrategien auf Gemeindeebene. Available online: https://www.lgl.bayern.de/gesundheit/arbeitsplatz_umwelt/projekte_a_z/doc/gme_tabakrauchbelastung_kinder_abschlussbericht.pdf (accessed on 14 August 2018).
- King, B.A.; Patel, R.; Babb, S.D.; Hartman, A.M.; Freeman, A. National and state prevalence of smoke-free rules in homes with and without children and smokers: Two decades of progress. Prev. Med. 2016, 82, 51–58. [Google Scholar] [CrossRef] [PubMed]
- Mbulo, L.; Palipudi, K.M.; Andes, L.; Morton, J.; Bashir, R.; Fouad, H.; Ramanandraibe, N.; Caixeta, R.; Dias, R.C.; Wijnhoven, T.M.; et al. Secondhand smoke exposure at home among one billion children in 21 countries: Findings from the global adult tobacco survey (gats). Tob. Control 2016, 25, e95–e100. [Google Scholar] [CrossRef] [PubMed]
- Müller, S.; Kraus, L.; Piontek, D.; Pabst, A. Changes in exposure to secondhand smoke and smoking behavior. SUCHT 2010, 56, 373–384. [Google Scholar] [CrossRef]
- Boeckmann, M.; Kotz, D.; Shahab, L.; Brown, J.; Kastaun, S. German public support for tobacco control policy measures: Results from the German study on tobacco use (DEBRA), a representative national survey. Int. J. Environ. Res. Public Health 2018, 15, 696. [Google Scholar] [CrossRef] [PubMed]
- Kuntz, B.; Lampert, T. Smoking and passive smoke exposure among adolescents in Germany. Dtsch Ärztebl Int. 2016, 113, 23–30. [Google Scholar] [CrossRef] [PubMed]
- Klingshirn, H.; Hendrowarsito, L.; Fromme, H.; Bolte, G.; Studiengruppe, G.M.E. Die Bedeutung des Migrationshintergrundes fur die Tabakrauchbelastung von Kindern. Eine Querschnittstudie im Rahmen der Gesundheits-Monitoring-Einheiten (GME) in Bayern. Gesundheitswesen 2014, 76, e14–e22. (In German) [Google Scholar] [PubMed]
- Jones, L.L.; Atkinson, O.; Longman, J.; Coleman, T.; McNeill, A.; Lewis, S.A. The motivators and barriers to a smoke-free home among disadvantaged caregivers: Identifying the positive levers for change. Nicotine Tob. Res. 2011, 13, 479–486. [Google Scholar] [CrossRef] [PubMed]
- Rowa-Dewar, N.; Amos, A. Disadvantaged parents’ engagement with a national secondhand smoke in the home mass media campaign: A qualitative study. Int. J. Environ. Res. Public Health 2016, 13, 901. [Google Scholar] [CrossRef] [PubMed]
- Mai, Y.; Leonardo, S.; Soulakova, J.N. Smoke-free homes among single-parent families: Differences associated with parental race/ethnicity and smoking behaviors. Prev. Med. Rep. 2018, 9, 18–23. [Google Scholar] [CrossRef] [PubMed]
- Cheah, Y.K.; Teh, C.H.; Lim, H.K. Factors associated with second-hand smoke awareness in Malaysia. Proc. Singap. Healthc. 2017, 27, 148–156. [Google Scholar] [CrossRef]
- Schaeffer, D.; Berens, E.M.; Vogt, D. Health literacy in the German population. Dtsch. Ärztebl. Int. 2017, 114, 53–60. [Google Scholar] [PubMed]
- Passey, M.E.; Longman, J.M.; Robinson, J.; Wiggers, J.; Jones, L.L. Smoke-free homes: What are the barriers, motivators and enablers? A qualitative systematic review and thematic synthesis. BMJ Open 2016, 6, e010260. [Google Scholar] [CrossRef] [PubMed]
- Savas, L.S.; Mullen, P.D.; Hovell, M.F.; Escoffrey, C.; Fernandez, M.E.; Jones, J.A.; Cavazos, J.; Gutierrez Monroy, J.A.A.; Kegler, M.C. A qualitative study among Mexican Americans to understand factors influencing the adoption and enforcement of home smoking bans. Nicotine Tob. Res. 2017, 19, 1465–1472. [Google Scholar] [CrossRef] [PubMed]
- Kuntz, B.; Lampert, T. Social disparities in parental smoking and young children’s exposure to secondhand smoke at home: A time-trend analysis of repeated cross-sectional data from the German KiGGS study between 2003–2006 and 2009–2012. BMC Public Health 2016, 16, 485. [Google Scholar] [CrossRef] [PubMed]
- Rosen, L.J.; Myers, V.; Winickoff, J.P.; Kott, J. Effectiveness of interventions to reduce tobacco smoke pollution in homes: A systematic review and meta-analysis. Int. J. Environ. Res. Public Health 2015, 12, 16043–16059. [Google Scholar] [CrossRef] [PubMed]
- Rosen, L.J.; Myers, V.; Hovell, M.; Zucker, D.; Ben Noach, M. Meta-analysis of parental protection of children from tobacco smoke exposure. Pediatrics 2014, 133, 698–714. [Google Scholar] [CrossRef] [PubMed]
- Family and Carer Smoking Control Programmes for Reducing Children’s Exposure to Environmental Tobacco Smoke. Available online: https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD001746.pub3/abstract (accessed on 1 March 2014).
- Tobacco Advisory Group of the Royal College of Physicians. Passive Smoking in Children: A Report; Royal College of Physicians: London, UK, 2010. [Google Scholar]
- Israel, B.A.; Schulz, A.J.; Parker, E.A.; Becker, A.B. Review of community-based research: Assessing partnership approaches to improve public health. Annu. Rev. Public Health 1998, 19, 173–202. [Google Scholar] [CrossRef] [PubMed]
- Weiner, J.; McDonald, J.A. Three models of community-based participatory research. LDI Issue Briefs 2013, 18, 1–8. [Google Scholar] [PubMed]
- Nastasi, B.K.; Hitchcock, J.; Sarkar, S.; Burkholder, G.; Varjas, K.; Jayasena, A. Mixed methods in intervention research: Theory to adaptation. J. Mixed Methods Res. 2007, 1, 164–182. [Google Scholar] [CrossRef]
- Neuhauser, L.; Kreps, G. The advent of e-health. How interactive media are transforming health communication. M&K 2003, 51, 541–556. [Google Scholar]
- Wayne, N.; Ritvo, P. Smartphone-enabled health coach intervention for people with diabetes from a modest socioeconomic strata community: Single-arm longitudinal feasibility study. J. Med. Int. Res. 2014, 16, e149. [Google Scholar] [CrossRef] [PubMed]
- Bock, B.C.; Rosen, R.K.; Barnett, N.P.; Thind, H.; Walaska, K.; Foster, R.; Deutsch, C.; Traficante, R. Translating behavioral interventions onto mhealth platforms: Developing text message interventions for smoking and alcohol. JMIR Mhealth Uhealth 2015, 3, e22. [Google Scholar] [CrossRef] [PubMed]
- Sukalla, F.; Karnowski, V.; Radon, K.; Barth, S.; Gerlich, J.; Weinmann, T. Transdisziplinarität und partizipativität beI der entwicklung einer kampagne zur reduktion der passivrauchbelastung beI kindern. In Gesundheitskommunikation als Transdisziplinäres Forschungsfeld, 1st ed.; Lampert, C., Grimm, M.M.A., Eds.; Nomos Verlagsgesellschaft mbH & Co. KG: Baden-Baden, Germany, 2017; pp. 187–198. [Google Scholar]
- Thomas, S.; Heinrich, S.; Kuhnlein, A.; Radon, K. The association between socioeconomic status and exposure to mobile telecommunication networks in children and adolescents. Bioelectromagnetics 2010, 31, 20–27. [Google Scholar] [PubMed]
- Mayring, P. Qualitative Inhaltsanalyse. Grundlagen und Techniken; Beltz: Weinheim, Deutschland, 2003. [Google Scholar]
- Witte, K. Putting the fear back into fear appeals: The extended parallel process model. Commun. Monogr. 1992, 59, 329–349. [Google Scholar] [CrossRef]
- Ajzen, I.; Albarracín, D. Predicting and changing behavior: A reasoned action approach. In Prediction and Change of Health Behavior: Applying the Reasoned Action Approach; Lawrence Erlbaum Associates Publishers: Mahwah, NJ, USA, 2007; pp. 3–21. [Google Scholar]
- Rosenstock, I.M. Why people use health services. Milbank Q. 2005, 8. [Google Scholar] [CrossRef]
- Mayring, P. Qualitative Inhaltsanalyse; Beltz: Weinheim, Deutschland, 2010. [Google Scholar]
- Berens, E.M.; Riedel, J.; Reder, M.; Razum, O.; Kolip, P.; Spallek, J. Postalische Befragung von Frauen mit türkischem Migrationshintergrund-Identifizierung, Stichprobenbereinigung und Response im Rahmen der Inema-Studie. Gesundheitswesen 2017, 79, 1000–1003. (In German) [Google Scholar] [CrossRef] [PubMed]
- Reiss, K.; Makarova, N.; Spallek, J.; Zeeb, H.; Razum, O. Identifizierung und Rekrutierung von Menschen mit Migrationshintergrund fur epidemiologische Studien in Deutschland. Gesundheitswesen 2013, 75, e49–e58. (In German) [Google Scholar] [CrossRef] [PubMed]
- Leviton, L.C. Generalizing about public health interventions: A mixed-methods approach to external validity. Annu. Rev. Public Health 2017, 38, 371–391. [Google Scholar] [CrossRef] [PubMed]
- Hamill, S.; Turk, T.; Murukutla, N.; Ghamrawy, M.; Mullin, S. I ‘like’ mpower: Using facebook, online ads and new media to mobilise tobacco control communities in low-income and middle-income countries. Tob. Control 2015, 24, 306–312. [Google Scholar] [CrossRef] [PubMed]
- Derrick, J.L.; Eliseo-Arras, R.K.; Hanny, C.; Britton, M.; Haddad, S. Comparison of internet and mailing methods to recruit couples into research on unaided smoking cessation. Addict. Behav. 2017, 75, 12–16. [Google Scholar] [CrossRef] [PubMed]
- Zentrum für Interdisziplinäre Suchtforschung der Universität Hamburg. MIRAS-Miteinander Rauchbelastung senken. Available online: http://www.zis-hamburg.de/projekte/projektdetails/MIRAS-Miteinander-Rauchbelastung-senken (accessed on 6 September 2018).

| Illustration 1: Asthma (%) | Illustration 2: Cool Like My Mom (%) | Illustration 3: Otitis Media (%) | Illustration 4: Bad Smell (%) | ||
|---|---|---|---|---|---|
| First impression | pANOVA | ||||
| 1 very poor | 44.6 | 31.4 | 33.9 | 26.4 | |
| 2 | 3.3 | 9.9 | 1.7 | 8.3 | |
| 3 | 8.3 | 11.6 | 11.6 | 10.7 | |
| 4 | 9.1 | 7.4 | 9.1 | 12.4 | |
| 5 very good | 16.5 | 17.4 | 18.2 | 15.7 | |
| Mean (SD) | 2.38 (1.67) | 2.61 (1.62) | 2.68 (1.70) | 2.76 (1.60) | 0.28 |
| Do you feel personally addressed by the message? | |||||
| 1 no, not at all | 29.8 | 18.2 | 24.8 | 19.0 | |
| 2 | 5.8 | 5.8 | 6.6 | 9.9 | |
| 3 | 14.9 | 16.5 | 16.5 | 13.2 | |
| 4 | 10.7 | 10.7 | 12.4 | 12.4 | |
| 5 yes, very much | 21.5 | 26.4 | 14.9 | 18.2 | |
| Mean (SD) | 2.86 (1.64) | 3.28 (1.57) | 2.81 (1.53) | 3.01 (1.54) | 0.08 |
| Illustration 1: Asthma | Illustration 2: Cool Like My Mom | Illustration 3: Otitis Media | Illustration 4: Bad Smell | ||
|---|---|---|---|---|---|
| Mean (Standard deviation) | pANOVA | ||||
| Incomprehensible (1)/comprehensible (5) | 4.64 (0.84) | 4.49 (0.90) | 4.30 (1.16) | 4.40 (1.05) | 0.01 * |
| Not interesting (1)/interesting (5) | 4.20 (0.94) | 3.96 (1.20) | 4.12 (1.05) | 4.06 (1.16) | 0.21 |
| Implausible (1)/plausible (5) | 4.18 (1.13) | 4.11 (1.12) | 3.93 (1.22) | 4.07 (1.30) | 0.02 * |
| Unimportant (1)/important (5) | 4.58 (0.92) | 4.41 (0.98) | 4.69 (0.65) | 4.33 (0.97) | <0.01 ** |
| Inappropriate (1)/appropriate (5) | 4.21 (1.12) | 4.10 (1.07) | 3.97 (1.36) | 3.90 (1.36) | 0.06 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Weinmann, T.; Radon, K.; Sukalla, F.; Gerlich, J.; Barth, S.; Nowak, D.; Karnowski, V. Developing an Awareness Campaign to Reduce Second Hand Smoke Among Disadvantaged Families—A Participatory M-Health Approach. Int. J. Environ. Res. Public Health 2018, 15, 1945. https://doi.org/10.3390/ijerph15091945
Weinmann T, Radon K, Sukalla F, Gerlich J, Barth S, Nowak D, Karnowski V. Developing an Awareness Campaign to Reduce Second Hand Smoke Among Disadvantaged Families—A Participatory M-Health Approach. International Journal of Environmental Research and Public Health. 2018; 15(9):1945. https://doi.org/10.3390/ijerph15091945
Chicago/Turabian StyleWeinmann, Tobias, Katja Radon, Freya Sukalla, Jessica Gerlich, Swaantje Barth, Dennis Nowak, and Veronika Karnowski. 2018. "Developing an Awareness Campaign to Reduce Second Hand Smoke Among Disadvantaged Families—A Participatory M-Health Approach" International Journal of Environmental Research and Public Health 15, no. 9: 1945. https://doi.org/10.3390/ijerph15091945
APA StyleWeinmann, T., Radon, K., Sukalla, F., Gerlich, J., Barth, S., Nowak, D., & Karnowski, V. (2018). Developing an Awareness Campaign to Reduce Second Hand Smoke Among Disadvantaged Families—A Participatory M-Health Approach. International Journal of Environmental Research and Public Health, 15(9), 1945. https://doi.org/10.3390/ijerph15091945





