Pharmacological and Non-Pharmacological Methods of Labour Pain Relief—Establishment of Effectiveness and Comparison
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Group
2.2. Questionnaire
2.2.1. Demographics and Infant Birth Outcomes
2.2.2. Past Medical History
2.2.3. Methods of Labour Pain Management and Pain Assessment
2.2.4. Statistical Analysis
3. Results
3.1. Pharmacological Methods
3.2. Non-Pharmacological Methods
4. Discussion
4.1. Epidural Analgesia
4.2. Gas for Pain Control
4.3. Water Immersion and Water Birth
4.4. Transcutaneous Electrical Nerve Stimulation (TENS)
4.5. Multiple Management
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| EA | Epidural analgesia |
| G | Gas for pain control |
| HC | Head circumference |
| LPI I | Mean values of labour pain intensity in the first stage of labour |
| LPI II | Mean values of labour pain intensity in the second stage of labour |
| LPI III | Mean values of labour pain intensity in the third stage of labour |
| MLPI | Mean value of labour pain intensity |
| MM | Multiple management |
| N | No pain relief |
| PLPI | Mean prediction of labour pain intensity |
| TENS | Transcutaneous electrical nerve stimulation |
| VAS | Visual analogue scale |
| WB | Water birth |
References
- Karlsdottir, S.I.; Sveinsdottir, H.; Olafsdottir, O.A.; Kristjansdottir, H. Pregnant women’s expectations about pain intensity during childbirth and their attitudes towards pain management: Findings from an Icelandic national study. Sex Reprod. Healthc. 2015, 211–218. [Google Scholar] [CrossRef] [PubMed]
- Serçekuş, P.; Okumuş, H. Fears associated with childbirth among nulliparous women in Turkey. Midwifery 2009, 155–162. [Google Scholar] [CrossRef] [PubMed]
- Gaskin, I.M. Ina May’s Guide to Childbirth: Updated with New Material; Vermilion: London, UK, 2008. [Google Scholar]
- Niven, C.; Gijsbers, K. A study of labour pain using the MCGILL pain questionnaire. Soc. Sci. Med. 1984, 1347–1351. [Google Scholar] [CrossRef]
- Labor, S.; Maguire, S. The Pain of Labour. Rev Pain. 2008, 15–19. [Google Scholar] [CrossRef] [PubMed]
- Koyyalamudi, V.; Sidhu, G.; Cornett, E.M.; Nguyen, V.; Labrie-Brown, C.; Fox, C.J.; Kaye, A.D. New Labor Pain Treatment Options. Curr. Pain Headache Rep. 2016, 20, 11. [Google Scholar] [CrossRef] [PubMed]
- Asadi, N.; Maharlouei, N.; Khalili, A.; Darabi, Y.; Davoodi, S.; Shahraki, H.R.; Hadianfard, M.; Jokar, A.; Vafaei, H.; Kasraeian, M. Effects of LI-4 and SP-6 Acupuncture on Labor Pain, Cortisol Level and Duration of Labor. J. Acupunct. Meridian Stud. 2015, 8, 249–254. [Google Scholar] [CrossRef] [PubMed]
- Bręborowicz, G. Położnictwo i Ginekologia; PZWL: Warszawa, Poland, 2015. [Google Scholar]
- Sulima, M. Alternatywne metody łagodzenia bólu porodowego. Eur. J. Med. Technol. 2013, 1, 32–38. [Google Scholar]
- Lindholm, A.; Hildingsson, I. Women’s preferences and received pain relief in childbirth—A prospective longitudinal study in a northern region of Sweden. Sex Reprod. Healthc. 2015, 6, 74–81. [Google Scholar] [CrossRef] [PubMed]
- Huskisson, E. Measurement of pain. Lancet 1974, 304, 1127–1131. [Google Scholar] [CrossRef]
- Freeman, L.M.; Bloemenkamp, K.W.; Franssen, M.T.; Papatsonis, D.N.; Hajenius, P.J.; van Huizen, M.E.; Bremer, H.A.; van den Akker, E.S.; Woiski, M.D.; Porath, M.M.; et al. Remifentanil patient controlled analgesia versus epidural analgesia in labour A multicentre randomized controlled trial. BMC Pregnancy Childbirth 2012, 63. [Google Scholar] [CrossRef]
- Howell, C.J. Epidural versus non-epidural analgesia for pain relief in labour. Cochrane Database Syst. Rev. 1999, CD000331. [Google Scholar] [CrossRef]
- Howell, C.J.; Kidd, C.; Roberts, W.; Upton, P.; Lucking, L.; Jones, P.W.; Johanson, R.B. Randomised controlled trial of epidural compared with non-epidural analgesia in labour. Br. J. Obstet. Gynaecol. 2001, 108, 27–33. [Google Scholar]
- Impey, L.; MacQuillan, K.; Robson, M. Epidural analgesia need not increase operative delivery rates. Am. J. Obstet. Gynecol. 2000, 182, 358–363. [Google Scholar] [CrossRef]
- Kinsella, S.M. Epidural analgesia for labour and instrumental vaginal delivery: An anaesthetic problem with an obstetric solution? BJOG Int. J. Obstet. Gynaecol. 2001, 108, 1–2. [Google Scholar] [CrossRef]
- Collins, M.R.; Starr, S.A.; Bishop, J.T.; Baysinger, C.L. Nitrous oxide for labor analgesia: Expanding analgesic options for women in the United States. Rev. Obstet. Gynecol. 2012, 126–131. [Google Scholar]
- Richards, W.; Parbrook, G.D.; Wilson, J. Stanislav Klikovich 1853–1910. Anaesthesia 1976, 933–940. [Google Scholar] [CrossRef]
- Likis, F.E.; Andrews, J.C.; Collins, M.R.; Lewis, R.M.; Seroogy, J.J.; Starr, S.A.; Walden, R.R.; McPheeters, M.L. Nitrous oxide for the management of labor pain: A systematic review. Anesth. Analg. 2014, 118, 153–167. [Google Scholar] [CrossRef]
- Certosimo, F.; Walton, M.; Hartzell, D.; Farris, J. Clinical evaluation of the efficacy of three nitrous oxide scavenging units during dental treatment. Gen. Dent. 2002, 430–435. [Google Scholar]
- Reid-Campion, M. Hydrotherapy: Principles and Practice, 2nd ed.; Butterworth Heineman: Oxford, UK, 1997. [Google Scholar]
- Pawelec, M.; Pietras, J.; Wojtysiak, M.; Karmowski, M.; Karmowski, A.; Palczynski, B.; Terpiłowski, Ł. Water birth and water immersion—An important step towards more patient-oriented health care or a new way for obstetrical wards to make profits? Adv. Clin. Exp. Med. 2011, 20, 391–397. [Google Scholar]
- Benfield, R.N.; Hortobágyi, T.; Tanner, C.J.; Swanson, M.; Heitkemper, M.M.; Newton, E.R. The effects of hydrotherapy on anxiety, pain, neuroendocrine responses, and contraction dynamics during labor. Biol. Res. Nurs. 2010, 28–36. [Google Scholar] [CrossRef]
- Poder, T.G.; Larivière, M. Bénéfices et risques de l’accouchement dans l’eau: Une revue systématique. Gynécol. Obs. Fertil. 2014, 706–713. [Google Scholar] [CrossRef] [PubMed]
- Zanetti-Daellenbach, R.A.; Tschudin, S.; Zhong, X.Y.; Holzgreve, W.; Lapaire, O.; Hösli, I. Maternal and neonatal infections and obstetrical outcome in water birth. Eur. J. Obstet. Gynecol. Reprod. Biol. 2007, 37–43. [Google Scholar] [CrossRef] [PubMed]
- Juda, W.; Madej, M.; Zalewski, M.; Jerzy, H.; Zalewski, J. Personal experiences of water birth. Zdr Publ. 2012, 122, 279–284. [Google Scholar] [CrossRef]
- Hodnett, E.D. Pain and women’s satisfaction with the experience of childbirth: A systematic review. Am. J. Obstet. Gynecol. 2002, 160–174. [Google Scholar]
- Spaich, S.; Welzel, G.; Berlit, S.; Temerinac, D.; Tuschy, B.; Sütterlin, M.; Kehl, S. Mode of delivery and its influence on women’s satisfaction with childbirth. Eur. J. Obstet. Gynecol. Reprod. Biol. 2013, 170, 401–406. [Google Scholar] [CrossRef]
- Say, R.E.; Thomson, R. Clinical review decisions—Challenges for doctors. Br. Med. J. 2003, 542–545. [Google Scholar] [CrossRef] [PubMed]
- Goldbort, J.G. Women’s Lived Experience of Their Unexpected Birthing Process. Mcn Am. J. Matern. Nurs. 2009, 57–62. [Google Scholar] [CrossRef] [PubMed]
- Santana, L.S.; Gallo, R.B.S.; Ferreira, C.H.J.; Duarte, G.; Quintana, S.M.; Marcolin, A.C. Transcutaneous electrical nerve stimulation TENS reduces pain and postpones the need for pharmacological analgesia during labour: A randomised trial. J. Physiother. 2015, 29–34. [Google Scholar] [CrossRef] [PubMed]
- Mello Larissa, F.D.; Nóbrega, L.F.; Lemos, A. Transcutaneous electrical stimulation for pain relief during labor: A systematic review and meta-analysis. Braz. J. Phys. Therapy 2011, 15, 175–184. [Google Scholar]
- Smith, C.A.; Collins, C.T.; Cyna, C.M.; Crowther, C. Complementary and alternative therapies for pain management in labour. Cochrane Database Syst. Rev. 2003, 1. [Google Scholar]
- Tournaire, M.; Theau-Yonneau, A. Complementary and alternative approaches to pain relief during labor. Evid.-Based Complement Altern. Med. 2007, 409–417. [Google Scholar] [CrossRef] [PubMed]
- Levett, K.M.; Smith, C.A.; Dahlen, H.G.; Bensoussan, A. Acupuncture and acupressure for pain management in labour and birth: A critical narrative review of current systematic review evidence. Complement Ther. Med. 2014, 22, 523–540. [Google Scholar] [CrossRef] [PubMed]
- Beckmann, M.M.; Stock, O.M. Antenatal perineal massage for reducing perineal trauma. Cochrane Database Syst. Rev. 2013. [Google Scholar] [CrossRef] [PubMed]
- Ginekologicznego, R.Z.E.P.T. Dotyczące Zapobiegania Śródporodowym Urazom Kanału Rodnego oraz Struktur dna Miednicy. Ginekol Pol. 2011, 82, 390–394. [Google Scholar]
- Ahldén, I.; Ahlehagen, S.; Dahlgren, L.; Josefsson, A. Parents’ expectations about participating in antenatal parenthood education classes. J. Perinat. Educ. 2012, 11–17. [Google Scholar] [CrossRef] [PubMed]
- Spinelli, A.; Baglio, G.; Donati, S.; Grandolfo, M.E.; Osborn, J. Do antenatal classes benefit the mother and her baby? J. Matern. Neonatal. Med. 2003, 94–101. [Google Scholar] [CrossRef] [PubMed]
| Epidural Anaesthesia (n = 42) | Gas for Pain Control (n = 40) | TENS (n = 50) | Immersion in Water (n = 40) | Multiple Management (n = 42) | p Value | |
|---|---|---|---|---|---|---|
| Age (years) | 29.95 ± 3.69 | 28.00 ± 3.51 | 29.20 ± 3.83 | 29.40 ± 3.91 | 30.00 ± 3.24 | 0.07 |
| Number of Pregnancies (n) | 1 (1–4) | 2 (1–3) | 1 (1–2) | 1 (1–3) | 1 (1–3) | 0.53 |
| Number of Labour (n) | 1 (1–2) | 1.5 (1–3) | 1 (1–2) | 1 (1–3) | 1 (1–3) | 0.09 |
| Education | 0.31 | |||||
| Primary | 0 | 2 (5) | 2 (4) | 2 (5) | 0 | |
| Secondary | 14 (33.33) | 14 (35) | 10 (20) | 4 (10) | 2 (4.76) | |
| Vocational | 2 (4.76) | 2 (5) | 0 | 4 (10) | 2 (4.76) | |
| Higher | 26 (61.9) | 22 (55) | 38 (76) | 30 (75) | 38 (90.48) | |
| Living and housing condition | <0.01 | |||||
| Weak | 0 | 0 | 0 | 0 | 0 | |
| Average | 4 (9.52) | 4 (10) | 2 (4) | 2 (5) | 0 | |
| Good | 14 (33.33) | 24 (60) | 30 (60) | 12 (30) | 10 (23.8) | |
| Very good | 24 (57.14) | 12 (30) | 18 (36) | 26 (65) | 32 (76.19) | |
| Timing of childbirth (weeks) | 39.19 ± 1.12 | 39.40 ± 0.82 | 39.20 ± 1.15 | 39.45 ± 1.05 | 39.33 ± 0.73 | 0.87 |
| Child’s weight (g) | 3485.24 ± 300.92 | 3574.50 ± 352.11 | 3364.6 ± 437.31 | 3293.5 ± 308.82 | 3324.76 ± 388.31 | 0.54 |
| Child’s height (cm) | 54.95 ± 2.06 | 54.50 ± 5.26 | 54.12 ± 2.80 | 54.00 ± 2.41 | 52.38 ± 7.92 | 0.08 |
| Child’s HC (cm) | 33.35 ± 1.09 | 34.21 ± 1.08 | 34.04 ± 0.89 | 33.28 ± 1.04 | 33.34 ± 1.40 | 0.85 |
| APGAR—1 min | 10 (9-10) | 10 (7-10) | 10 (9-10) | 10 (9-10) | 10 (9-10) | 0.38 |
| APGAR—5 min | 10 (9-10) | 10 (8-10) | 10 (10-10) | 10 (9-10) | 10 (10-10) | 0.56 |
| Primapara (n = 156) | Multipara (n = 102) | p Value | |
|---|---|---|---|
| PLPI | 8.04 ± 1.44 | 8.61 ± 1.88 | <0.01 |
| MLPI | 5.83 ± 1.63 | 6.02 ± 1.83 | 0.50 |
| Difference between PLPI and MLPI | 2.20 ± 2.06 | 2.59 ± 1.71 | 0.14 |
| LPI I | 6.86 ± 2.28 | 6.74 ± 2.24 | 0.66 |
| LPI II | 7.67 ± 2.07 | 8.16 ± 2.00 | 0.03 |
| LPI III | 2.98 ± 2.45 | 3.59 ± 2.43 | 0.01 |
| Epidural Anaesthesia (n = 42) | Gas for Pain Control (n = 40) | TENS (n = 50) | Immersion in Water (n = 40) | Multiple Management (n = 42) | None (n = 44) | p Value | |
|---|---|---|---|---|---|---|---|
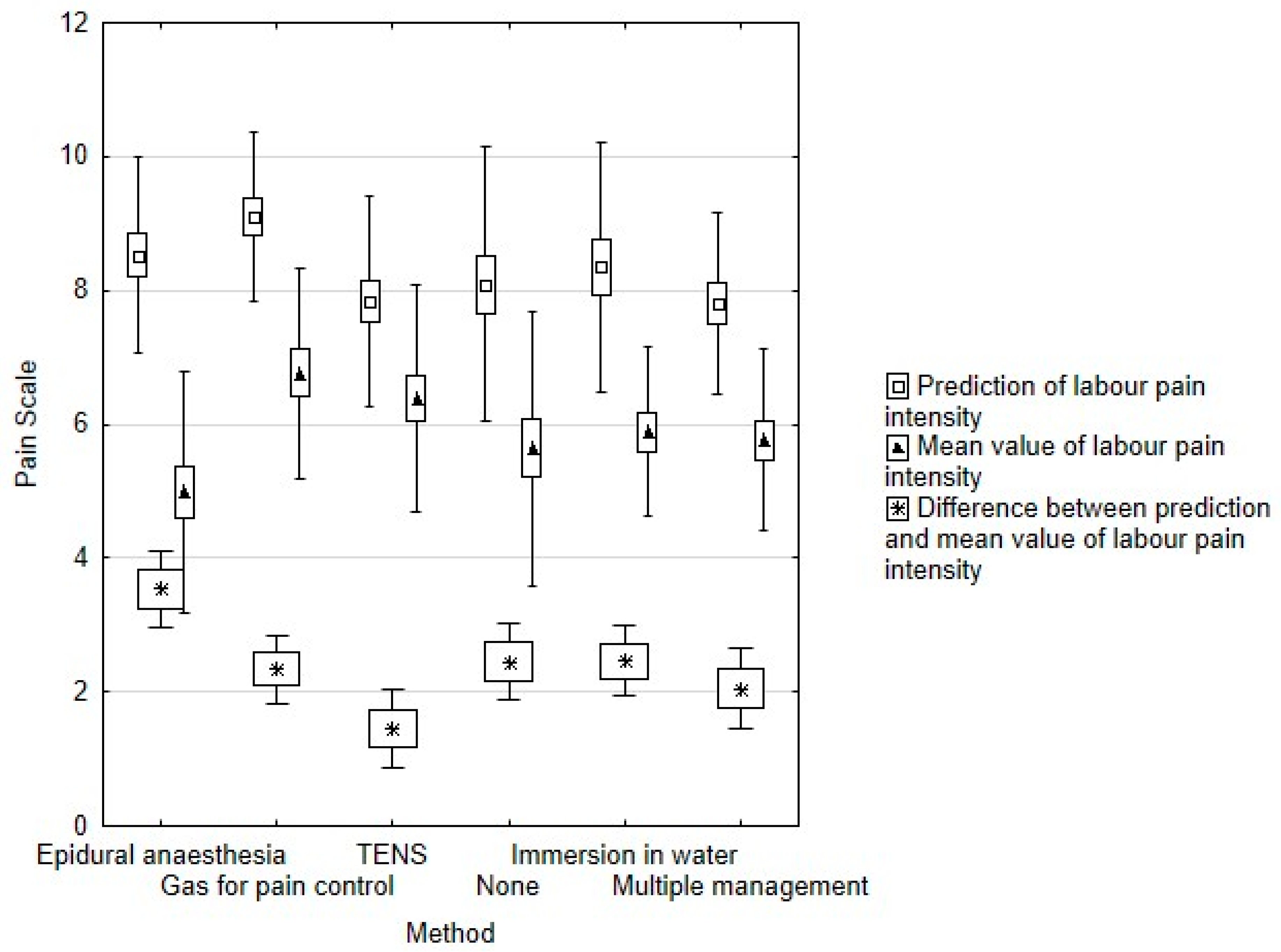
| PLPI | 8.52 ± 1.45 | 9.10 ± 1.24 | 7.84 ± 1.56 | 8.35 ± 1.85 | 7.81 ± 1.35 | 8.09 ± 2.02 | 0.06 |
| MLPI | 4.98 ± 1.79 | 6.77 ± 1.55 | 6.39 ± 1.68 | 5.88 ± 1.25 | 5.76 ± 1.35 | 5.64 ± 2.02 | 0.04 |
| Difference between PLPI and MLPI | 3.54 ± 1.84 | 2.33 ± 1.56 | 1.45 ± 2.05 | 2.47 ± 1.65 | 2.05 ± 1.94 | 2.45 ± 1.92 | 0.02 |
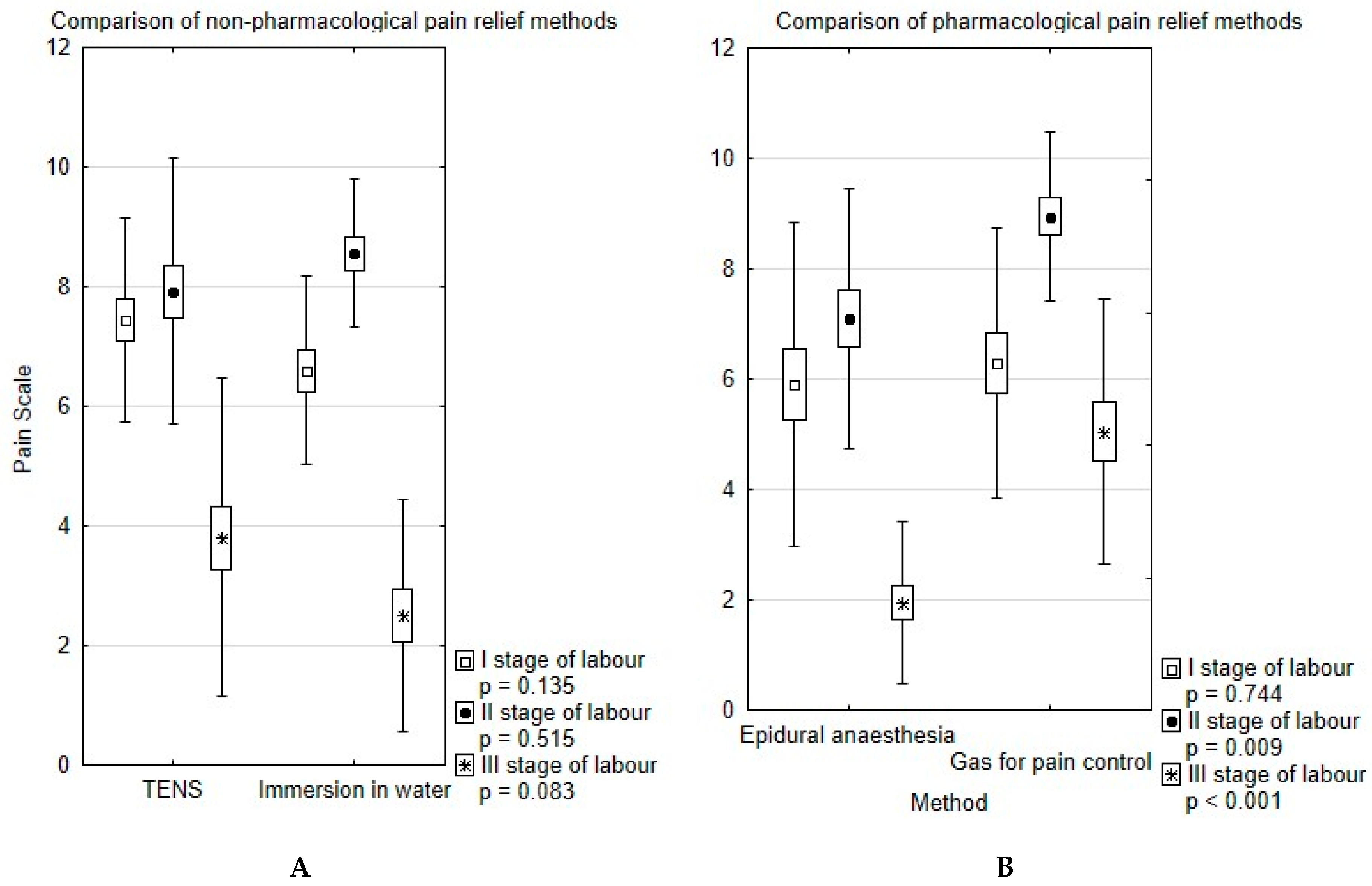
| LPI I | 5.90 ± 2.91 | 6.30 ± 2.42 | 7.44 ± 1.69 | 6.60 ± 1.55 | 7.62 ± 2.20 | 6.86 ± 2.19 | 0.16 |
| LPI II | 7.10 ± 2.34 | 8.95 ± 1.52 | 7.92 ± 2.19 | 8.55 ± 1.22 | 7.23 ± 2.07 | 7.47 ±2.11 | 0.02 |
| LPI III | 1.95 ± 1.45 | 5.05 ± 2.36 | 3.80 ± 2.63 | 2.50 ± 1.91 | 2.43 ± 2.26 | 3.55 ± 2.59 | <0.01 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Czech, I.; Fuchs, P.; Fuchs, A.; Lorek, M.; Tobolska-Lorek, D.; Drosdzol-Cop, A.; Sikora, J. Pharmacological and Non-Pharmacological Methods of Labour Pain Relief—Establishment of Effectiveness and Comparison. Int. J. Environ. Res. Public Health 2018, 15, 2792. https://doi.org/10.3390/ijerph15122792
Czech I, Fuchs P, Fuchs A, Lorek M, Tobolska-Lorek D, Drosdzol-Cop A, Sikora J. Pharmacological and Non-Pharmacological Methods of Labour Pain Relief—Establishment of Effectiveness and Comparison. International Journal of Environmental Research and Public Health. 2018; 15(12):2792. https://doi.org/10.3390/ijerph15122792
Chicago/Turabian StyleCzech, Iwona, Piotr Fuchs, Anna Fuchs, Miłosz Lorek, Dominika Tobolska-Lorek, Agnieszka Drosdzol-Cop, and Jerzy Sikora. 2018. "Pharmacological and Non-Pharmacological Methods of Labour Pain Relief—Establishment of Effectiveness and Comparison" International Journal of Environmental Research and Public Health 15, no. 12: 2792. https://doi.org/10.3390/ijerph15122792
APA StyleCzech, I., Fuchs, P., Fuchs, A., Lorek, M., Tobolska-Lorek, D., Drosdzol-Cop, A., & Sikora, J. (2018). Pharmacological and Non-Pharmacological Methods of Labour Pain Relief—Establishment of Effectiveness and Comparison. International Journal of Environmental Research and Public Health, 15(12), 2792. https://doi.org/10.3390/ijerph15122792






