Smartphone Applications for Encouraging Asthma Self-Management in Adolescents: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. Eligibility Criteria and Definitions
2.2. Search Strategy
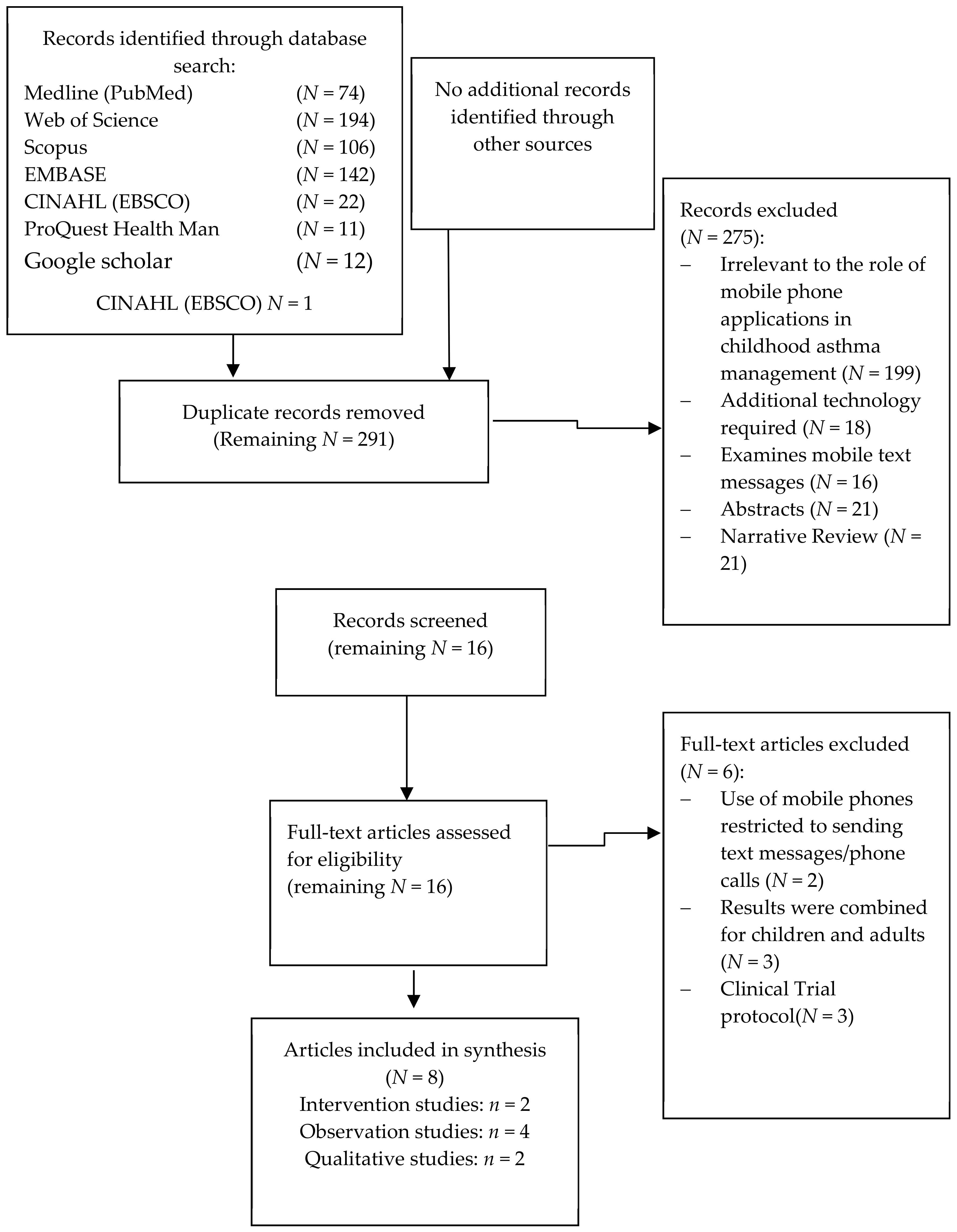
2.3. Study Selection
2.4. Data Extraction
2.5. Quality Assessment
3. Results
3.1. Results from Intervention Studies
3.1.1. Asthma Control
3.1.2. Self-Efficacy
3.1.3. Asthma Medication Adherence
3.1.4. Participant Satisfaction
3.2. Results from Observational Studies
3.3. Results from Qualitative Studies
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Da Costa, T.M.; Salomao, P.L.; Martha, A.S.; Pisa, I.T.; Sigulem, D. The impact of short message service text messages sent as appointment reminders to patients’ cell phones at outpatient clinics in Sao Paulo, Brazil. Int. J. Med. Inform. 2010, 79, 65–70. [Google Scholar] [CrossRef] [PubMed]
- Vervloet, M.; van Dijk, L.; Santen-Reestman, J.; Van Vlijmen, B.; Van Wingerden, P.; Bouvy, M.L.; de Bakker, D.H. SMS reminders improve adherence to oral medication in type 2 diabetes patients who are real time electronically monitored. Int. J. Med. Inform. 2012, 81, 594–604. [Google Scholar] [CrossRef] [PubMed]
- Britto, M.T.; Rohan, J.M.; Dodds, C.M.; Byczkowski, T.L. A randomized trial of user-controlled text messaging to improve asthma outcomes: A pilot study. Clin. Pediatr. 2017, 56, 1336–1344. [Google Scholar] [CrossRef] [PubMed]
- Gustafson, D.; Wise, M.; Bhattacharya, A.; Pulvermacher, A.; Shanovich, K.; Phillips, B.; Lehman, E.; Chinchilli, V.; Hawkins, R.; Kim, J.S. The effects of combining Web-based eHealth with telephone nurse case management for pediatric asthma control: A randomized controlled trial. J. Med. Internet Res. 2012, 14, e101. [Google Scholar] [CrossRef] [PubMed]
- Kuijpers, W.; Groen, W.G.; Aaronson, N.K.; van Harten, W.H. A systematic review of web-based interventions for patient empowerment and physical activity in chronic diseases: Relevance for cancer survivors. J. Med. Internet Res. 2013, 15, e37. [Google Scholar] [CrossRef] [PubMed]
- Badawy, S.M.; Thompson, A.A.; Kuhns, L.M. Medication adherence and technology-based interventions for adolescents with chronic health conditions: A few key considerations. JMIR mHealth uHealth 2017, 5, e202. [Google Scholar] [CrossRef] [PubMed]
- Aussie Teens and Kids Online. Available online: https://www.acma.gov.au/theACMA/engage-blogs/engage-blogs/Research-snapshots/Aussie-teens-and-kids-online (accessed on 5 May 2018).
- Asher, I.; Pearce, N. Global burden of asthma among children. Int. J. Tuberc. Lung Dis. 2014, 18, 1269–1278. [Google Scholar] [CrossRef] [PubMed]
- Pawankar, R.; Canonica, G.; Holgate, S.; Lockey, R.F. World Allergy Organisation (WAO) White Book on Allergy; World Allergy Organization: Milwaukee, WI, USA, 2013. [Google Scholar]
- Taylor, S.J.C.; Pinnock, H.; Epiphaniou, E.; Pearce, G.; Parke, H.L.; Schwappach, A.; Purushotham, N.; Jacob, S.; Griffiths, C.J.; Greenhalgh, T.; et al. A rapid synthesis of the evidence on interventions supporting self-management for people with long-term conditions: PRISMS—Practical systematic Review of Self-Management Support for long-term conditions. Health Serv. Deliv. Res. No. 2.53 2014. [Google Scholar] [CrossRef] [PubMed]
- Mansouri, P.M.; Ghadami, M.M.; Najafi, S.S.M.; Yektatalab, S. The effect of self-management training on self-efficacy of cirrhotic patients referring to transplantation Center of Nemazee Hospital: A randomized controlled clinical trial. Int. J. Community Based Nurs. Midwifery 2017, 5, 256–263. [Google Scholar]
- McClure, N.; Seibert, M.; Johnson, T.; Kannenberg, L.; Brown, T.; Lutenbacher, M. Improving asthma management in the elementary school setting: An education and self-management pilot project. J. Pediatr. Nurs. 2018, 42, 16–20. [Google Scholar] [CrossRef] [PubMed]
- Tinschert, P.; Jakob, R.; Barata, F.; Kramer, J.N.; Kowatsch, T. The potential of mobile apps for improving asthma self-management: A review of publicly available and well-adopted asthma apps. JMIR mHealth uHealth 2017, 5. [Google Scholar] [CrossRef] [PubMed]
- Downs, S.H.; Black, N. The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. J. Epidemiol. Community Health 1998, 52, 377–384. [Google Scholar] [CrossRef] [PubMed]
- Rhee, H.; Allen, J.; Mammen, J.; Swift, M. Mobile phone-based asthma self-management aid for adolescents (mASMAA): A feasibility study. Patient Prefer Adherence 2014, 8, 63–72. [Google Scholar] [CrossRef] [PubMed]
- Mulvaney, S.A.; Ho, Y.X.; Cala, C.M.; Chen, Q.; Nian, H.; Patterson, B.L.; Johnson, K.B. Assessing adolescent asthma symptoms and adherence using mobile phones. J. Med. Internet Res. 2013, 15. [Google Scholar] [CrossRef] [PubMed]
- Peters, D.; Davis, S.; Calvo, R.A.; Sawyer, S.M.; Smith, L.; Foster, J.M. Young people’s preferences for an asthma self-management app highlight psychological needs: A participatory study. J. Med. Internet Res. 2017, 19. [Google Scholar] [CrossRef] [PubMed]
- Pinnock, H.; Slack, R.; Pagliari, C.; Price, D.; Sheikh, A. Understanding the potential role of mobile phone-based monitoring on asthma self-management: Qualitative study. Clin. Exp. Allergy 2007, 37, 794–802. [Google Scholar] [CrossRef] [PubMed]
- Ryan, D.; Cobern, W.; Wheeler, J.; Price, D.; Tarassenko, L. Mobile phone technology in the management of asthma. J. Telemed. Telecare 2005, 11, 43–46. [Google Scholar] [CrossRef] [PubMed]
- Fedele, D.A.; McConville, A.; Thomas, J.G.; McQuaidb, E.L.; Janickea, D.M.; Turner, E.M.; Moon, J.; Abu-Hasan, M. Applying Interactive Mobile health to Asthma Care in Teens (AIM2ACT): Development and design of a randomized controlled trial. Contem. Clin. Trials 2018, 64, 230–237. [Google Scholar] [CrossRef] [PubMed]
- Kosse, R.C.; Bouvy, M.L.; de Vries, T.W.; Kaptein, A.A.; Geers, H.C.; van Dijk, L.; Koster, E.S. mHealth intervention to support asthma self-management in adolescents: The ADAPT study. Patient Preference Adherence 2017, 11, 571. [Google Scholar] [CrossRef] [PubMed]
- Wu, C.T.; Tzeng, Y.F.; Ho, T.W.; Chen, S.W.; Gau, B.S.; Lai, F.; Chiu, H.Y. A Smart Phone Application in Improving Healthy Lifestyles and Health Outcomes for School-Age Children with Asthma. In Proceedings of the 2016 IEEE/ACM International Conference on Advances in Social Networks Analysis and Mining, San Francisco, CA, USA, 18–21 August 2016. [Google Scholar]
- Burbank, A.J.; Lewis, S.D.; Hewes, M.; Schellhase, D.E.; Rettiganti, M.; Hall-Barrow, J. Mobile-based asthma action plans for adolescents. J. Asthma 2015, 52, 583–586. [Google Scholar] [CrossRef] [PubMed]
- Mosnaim, G.; Li, H.; Martin, M.; Richardson, J.; Belice, P.J.; Avery, E.; Silberstein, A.; Leigh, J.; Kenyon, R.; Jones, S.; et al. A tailored mobile health intervention to improve adherence and asthma control in minority adolescents. J. Allergy Clin. Immunol. Pract. 2015, 3, 288–290. [Google Scholar] [CrossRef] [PubMed]
- Carpenter, D.M.; Geryk, L.L.; Sage, A.; Arrindell, C.; Sleath, B.L. Exploring the theoretical pathways through which asthma app features can promote adolescent self-management. Transl. Behave. Med. 2016, 6, 509–518. [Google Scholar] [CrossRef] [PubMed]
- Roberts, C.A.; Geryk, L.L.; Sage, A.J.; Sleath, B.L.; Tate, D.F.; Carpenter, D.M. Adolescent, caregiver, and friend preferences for integrating social support and communication features into an asthma self-management app. J. Asthma 2016, 53, 948–954. [Google Scholar] [CrossRef] [PubMed]
- Schneider, T.; Panzera, A.D.; Couluris, M.; Lindenberger, J.; McDermott, R.; Bryant, C.A. Engaging teens with asthma in designing a patient-centered mobile app to aid disease self-management. Telemed. e-Health 2016, 22, 170–175. [Google Scholar] [CrossRef] [PubMed]
- Odom, L.; Christenbery, T. There is an “app” for that: Designing mobile phone technology to improve asthma action plan use in adolescent patients. J. Am. Assoc. Nurse Pract. 2016, 28, 583–590. [Google Scholar] [CrossRef] [PubMed]
- Koster, E.S.; Philbert, D.; de Vries, T.W.; van Dijk, L.; Bouvy, M.L. “I just forget to take it”: Asthma self-management needs and preferences in adolescents. J. Asthma 2015, 52, 831–837. [Google Scholar] [CrossRef] [PubMed]
- Panzera, A.D.; Schneider, T.K.; Martinasek, M.P.; Lindenberger, J.H.; Couluris, M.; Bryant, C.A.; McDermott, R.J. Adolescent asthma self-management: Patient and parent-caregiver perspectives on using social media to improve care. J. Sch. Health 2013, 83, 921–930. [Google Scholar] [CrossRef] [PubMed]
- Singh, A.; Wilkinson, S.; Braganza, S. Smartphones and pediatric apps to mobilize the medical home. J. Pediatr. 2014, 165, 606–610. [Google Scholar] [CrossRef] [PubMed]
- Huckvale, K.; Morrison, C.; Ouyang, J.; Ghaghda, A.; Car, J. The evolution of mobile apps for asthma: An updated systematic assessment of content and tools. BMC Med. 2015, 13, 58. [Google Scholar] [CrossRef] [PubMed]
- Reddel, H.K.; Sawyer, S.M.; Everett, P.W.; Flood, P.V.; Peters, M.J. Asthma control in Australia: A cross-sectional web-based survey in a nationally representative population. Med. J. Aust. 2015, 202, 492–496. [Google Scholar] [CrossRef] [PubMed]
- Marcano Belisario, J.S.; Huckvale, K.; Greenfield, G.; Car, J.; Gunn, L.H. Smartphone and tablet self management apps for asthma. Cochrane Database System. Rev. 2013, 11. [Google Scholar] [CrossRef] [PubMed]
- Morrison, D.; Wyke, S.; Agur, K.; Cameron, E.J.; Docking, R.I.; MacKenzie, A.M.; McConnachie, A.; Raghuvir, V.; Thomson, N.C.; Mair, F.S. Digital asthma self-management interventions: A systematic review. J. Med. Internet Res. 2014, 16, e51. [Google Scholar] [CrossRef] [PubMed]
- Nickels, A.; Dimov, V. Innovations in technology: Social media and mobile technology in the care of adolescents with asthma. Curr. Allergy Asthma Rep. 2012, 12, 607–612. [Google Scholar] [CrossRef] [PubMed]
| Search No. | Search Terms |
|---|---|
| 1 | Child * OR pediatric OR paediatric OR adolescents OR teen * OR school OR PEDIATRICS/ |
| 2 | smart OR mobile OR phone OR CELL PHONE/ |
| 3 | application OR app * |
| 4 | asthma OR ASTHMA/ |
| 5 | self-manage * OR control OR self-efficacy OR adherence OR medication OR compliance OR observation OR judgement OR “action plan” |
| 6 | 1 AND 2 AND 3 AND 4 AND 5 |
| Author | Study Population; Location | Age Group (Sample Size) | Socially Disadvantaged Groups | Description of the App | Measures and Outcomes |
|---|---|---|---|---|---|
| Burbank et al. [22] | Outpatient paediatric specialty clinic; Arkansas, USA | 12−17 years (N = 20) | - 60% were minorities - 90% had state-issued medical insurance | Asthma Action Plan (AAP). This sends two daily notifications to the participant. The first one prompts for the recording of asthma symptoms and peak flow, and the second one is a medication reminder. It also provides guidance and advice every week via push notification. | - Usage rate of application; - Participant satisfaction; - Asthma control test scores (pre-and post-intervention); - Self-efficacy scores (pre- and post-intervention) |
| Mosnaim et al. [23] | Rush Paediatric Primary Care Centre, Chicago, Illinois, USA | 11−16 years (N = 12) | African-American population (urban minority group). | Mobile Adolescents’ Disease Empowerment and Persistency Technology (M-ADEPT): - Reminders for participants to take their ICS medication - Basketball game (immediate encouragement) for taking inhaled corticosteroid (ICS) - Positive text messages for each puff of ICS taken | ‘Efficacy’ defined as: - asthma control test (ACT) score should be improved by ≥3 points after intervention; - ICS use should be ≥50%. Main measures: - ACT scores (pre- and post- intervention); - ICS adherence. |
| Author | Asthma Control Tests | Self-Efficacy | Asthma Medication Adherence | Participant Satisfaction |
|---|---|---|---|---|
| Burbank et al. [22] | Median ACT scores increased from 20 to 21.5. ACT scores for uncontrolled asthma (N = 9) increased from 16 to 18 (p = 0.03). | Median total self-efficacy increase from 60.5 to 62 for all participants (p = 0.13) | 93% of participants reported their satisfaction. | |
| Mosnaim et al. [23] | 58% of the participants achieved three points in their ACT scores by week eight of the study. Median ACT increased from 18 to 23. | Median ICS adherence increased from 19% to 67 %.Short-acting beta 2-agonist decreased from median of three to zero. |
| Author | Study Population and Location | Age Group (Sample Size) | Other Variables (e.g., Sex, Socially Disadvantaged Groups) | Measures and Outcomes |
|---|---|---|---|---|
| Carpenter et al. [25], Roberts et al. [26] | Adolescents and their caregivers from two paediatric practices located in an urban area of North Carolina, USA | Age 12−16 (N = 20) | - Males = 11 - Females = 9 - White = 9 - Black = 8 - Annual household income: <$25,000 | 1. Participants’ asthma management goals 2. Adolescent technology use 3. Some participants reported the usefulness of each feature in the apps 4. The effect of app features on self-observation, self-judgment and self-reaction |
| Odom and Christenberry [28] | Patients returning for follow-up care at the allergy/immunology practice with a previous diagnosis of asthma, Tennessee, USA | Age 12–19 (N = 12) | - Female: 60% | 1. Ease of use 2. Use without written instructions 3. Expectation of the app features |
| Schneider et al. [27] | Adolescents with daily asthma maintenance medications, Tampa Bay, FL, USA | Age 13–18 (N = 16) | - Not specified | 1. Usefulness of features 2. Additional feature suggestions 3. Interface and app operation feedback |
| Author | Study Population andLocation | Age Group and Sample Size | Other Variables (e.g., Sex, Socially Disadvantaged Groups) | Measures and Outcomes |
|---|---|---|---|---|
| Koster et al. [29] | Two study populations: 1. An online group from the Utrecht Pharmacy Practice Network for Education and Research, the Netherlands in December 2013 2. A face-to-face group from the Department of Paediatrics at the Medical Centre Leeuwarden, the Netherlands in March 2014. | 12−16 years: (N = 21) - Online group (N = 14) - Face-to-face group (N = 7) | Online group: - Males = 8 - Females = 6 Face-to-face group: - Males = 2 - Females = 5 | 1. Adherence: This study clarifies the reasons for not taking medication at the proper times 2. Role of parent(s) 3. The solution that supports medication use 4. The effect of mobile phone applications on medication use |
| Panzera et al. [30] | Teens with asthma and their parent-caregivers who attended pediatric pulmonary clinics, Florida USA | 13–19 years of ages N = 18 | 1. Adherence: This study clarifies the reasons for not taking medication at the proper times 2. Potential role of digital media 3. Potential role of social media |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Alquran, A.; Lambert, K.A.; Farouque, A.; Holland, A.; Davies, J.; Lampugnani, E.R.; Erbas, B. Smartphone Applications for Encouraging Asthma Self-Management in Adolescents: A Systematic Review. Int. J. Environ. Res. Public Health 2018, 15, 2403. https://doi.org/10.3390/ijerph15112403
Alquran A, Lambert KA, Farouque A, Holland A, Davies J, Lampugnani ER, Erbas B. Smartphone Applications for Encouraging Asthma Self-Management in Adolescents: A Systematic Review. International Journal of Environmental Research and Public Health. 2018; 15(11):2403. https://doi.org/10.3390/ijerph15112403
Chicago/Turabian StyleAlquran, Alaa, Katrina A. Lambert, Ambereen Farouque, Anne Holland, Janet Davies, Edwin R. Lampugnani, and Bircan Erbas. 2018. "Smartphone Applications for Encouraging Asthma Self-Management in Adolescents: A Systematic Review" International Journal of Environmental Research and Public Health 15, no. 11: 2403. https://doi.org/10.3390/ijerph15112403
APA StyleAlquran, A., Lambert, K. A., Farouque, A., Holland, A., Davies, J., Lampugnani, E. R., & Erbas, B. (2018). Smartphone Applications for Encouraging Asthma Self-Management in Adolescents: A Systematic Review. International Journal of Environmental Research and Public Health, 15(11), 2403. https://doi.org/10.3390/ijerph15112403





