The Mental Health Outcomes of Drought: A Systematic Review and Causal Process Diagram
Abstract
:1. Introduction
1.1. Climate Change and Drought
1.2. Drought Health Effects
1.3. Characterization of Exposure
1.4. Characterization of Health Outcomes
1.5. Sub-Acute Disasters and Mental Health
1.6. Objectives
- Systematically review the existing literature concerning drought and mental health outcomes.
- Use systematic review results to develop a causal process diagram depicting the pathways linking drought and mental health outcomes.
- Examine risk and protective factors associated with drought exposure and mental health outcomes, including the coping mechanisms used by populations experiencing drought.
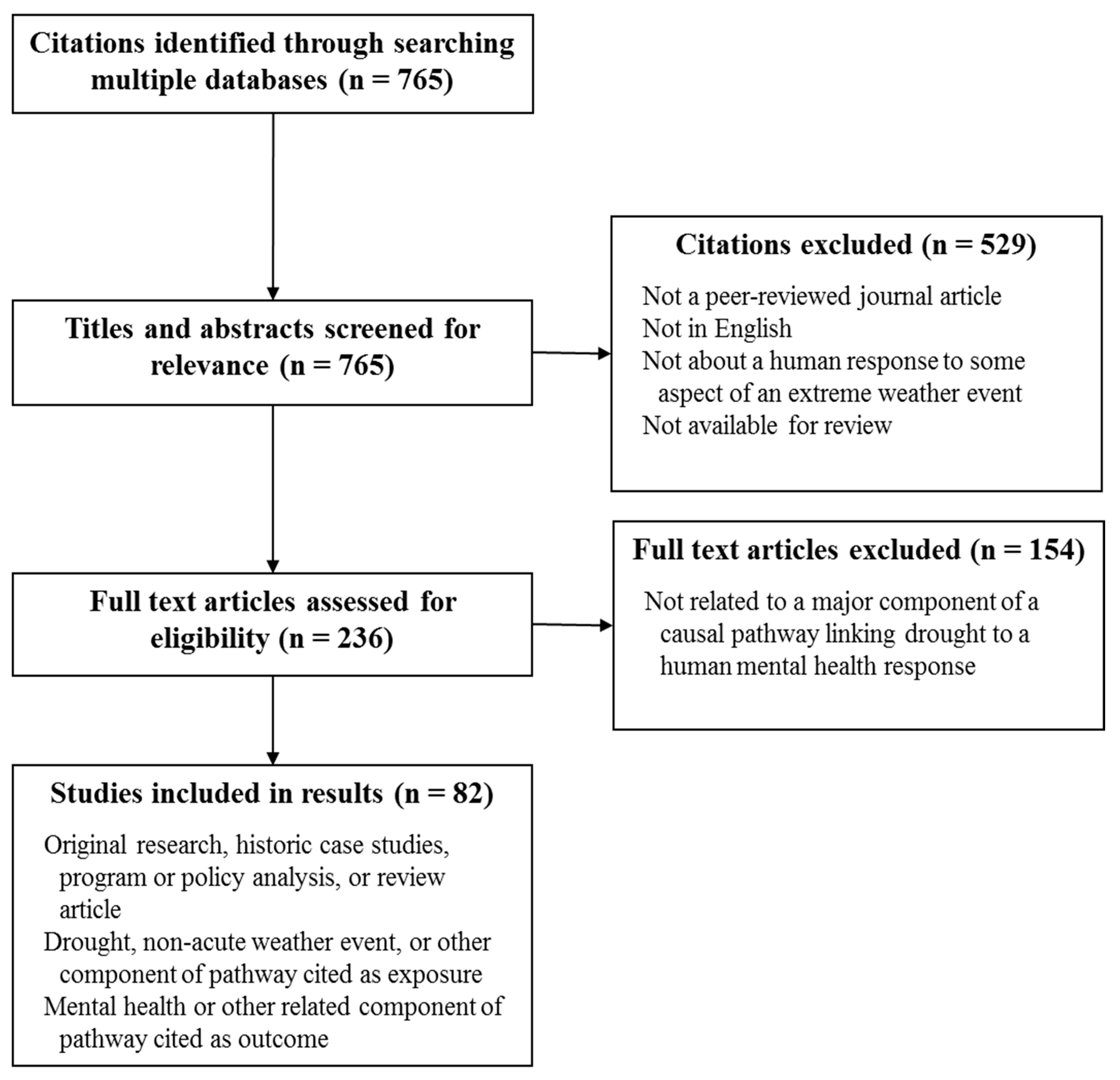
2. Methods
3. Results
3.1. Study Characteristics
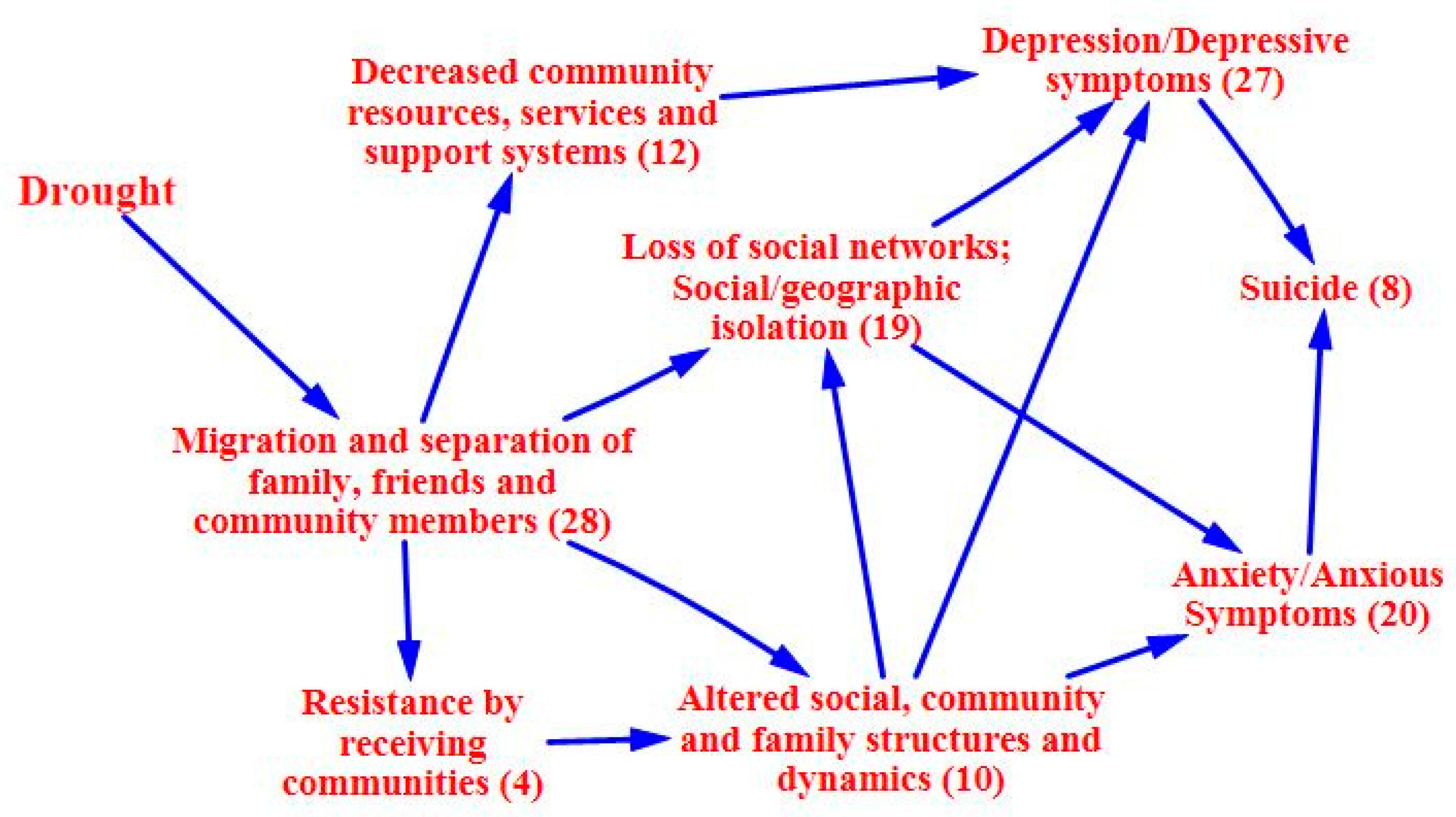
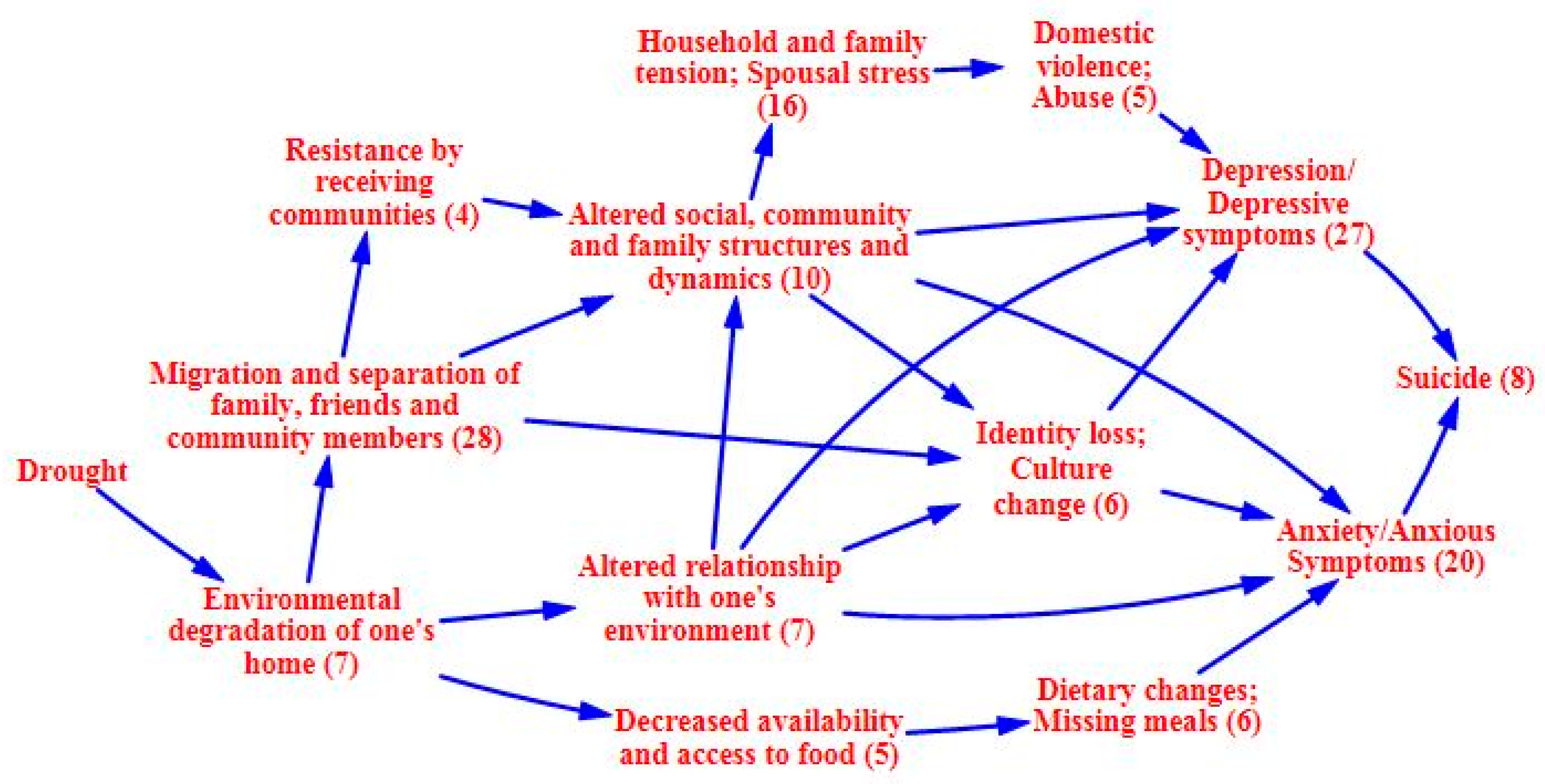
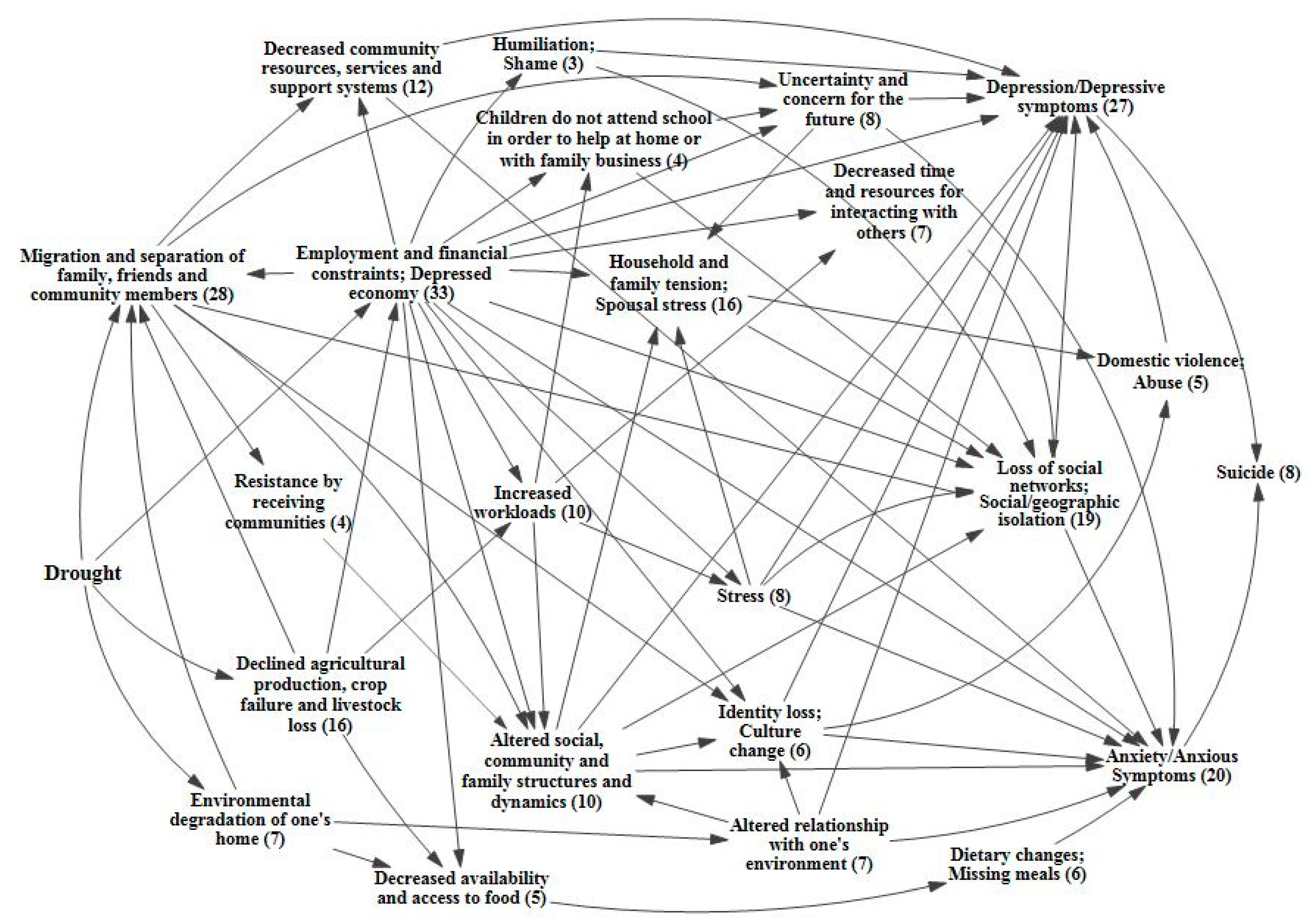
3.2. Causal Process Diagrams
| Characteristic | No. of Eligible Studies | Percent of Total | Percent of Subcategory | |
|---|---|---|---|---|
| Study Type | Original research | 53 | 65% | - |
| Quantitative methods | 24 | - | 45% | |
| Qualitative methods | 21 | - | 40% | |
| Mixed methods | 8 | - | 15% | |
| Historic case studies | 8 | 10% | - | |
| Program/Policy analyses | 5 | 6% | - | |
| Review articles | 16 | 20% | - | |
| Study Location | United States | 7 | 9% | - |
| Other developed countries | 58 | 71% | - | |
| Australia | 52 | - | 90% | |
| Canada | 6 | - | 10% | |
| New Zealand | 1 | - | 2% | |
| United Kingdom | 1 | - | 2% | |
| Developing countries | 10 | 12% | - | |
| Bolivia | 2 | - | 20% | |
| Botswana | 1 | - | 10 % | |
| Brazil | 1 | - | 10% | |
| Ethiopia | 1 | - | 10% | |
| India | 4 | - | 40% | |
| Iran | 1 | - | 10% | |
| Not location specific | 7 | 9% | - | |
| Publication Date | Articles published 2005 or later | 72 | 90% | - |
| Articles published 1996–2004 | 6 | 7% | - | |
| Articles published 1995 or earlier | 4 | 5% | - |
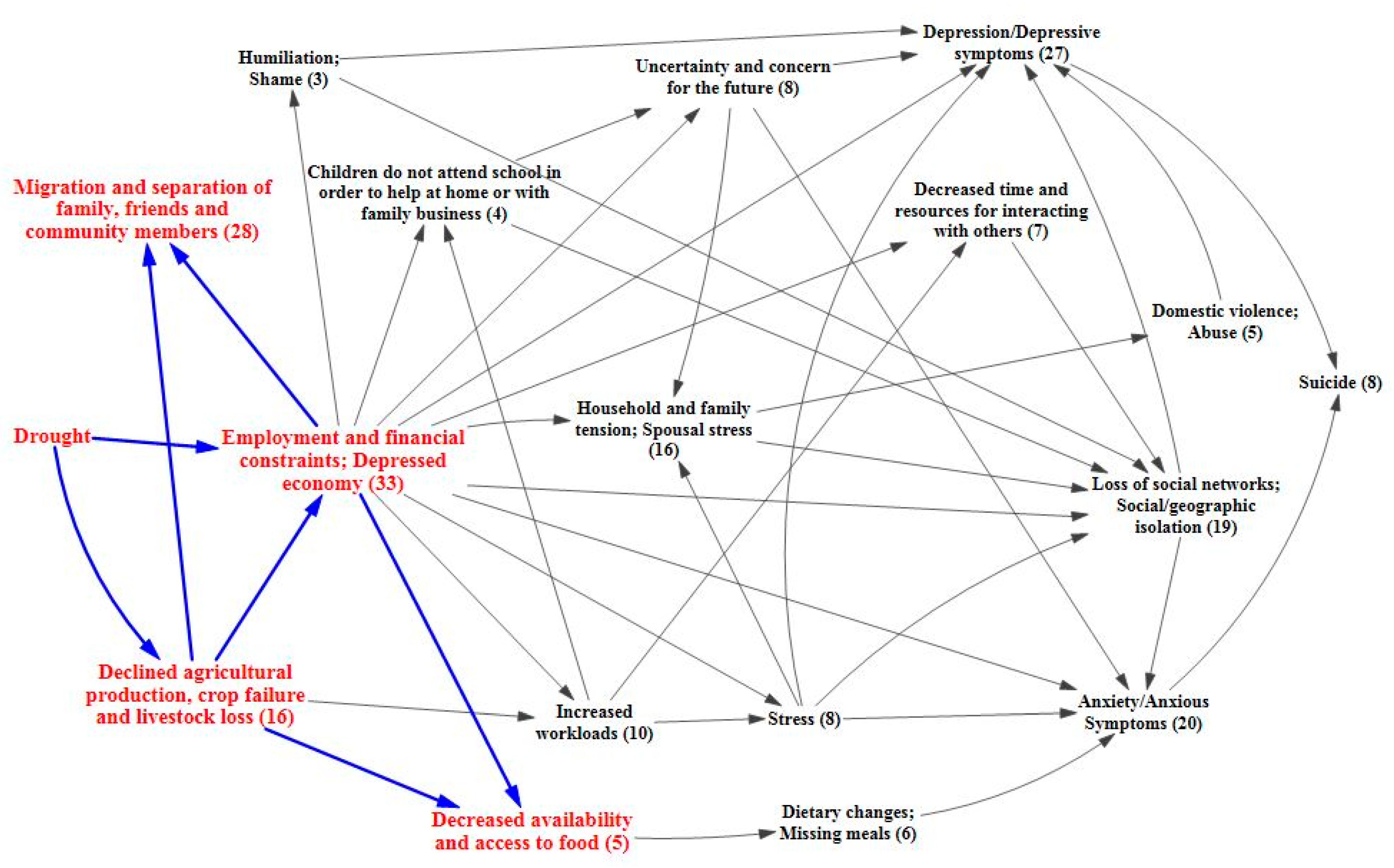
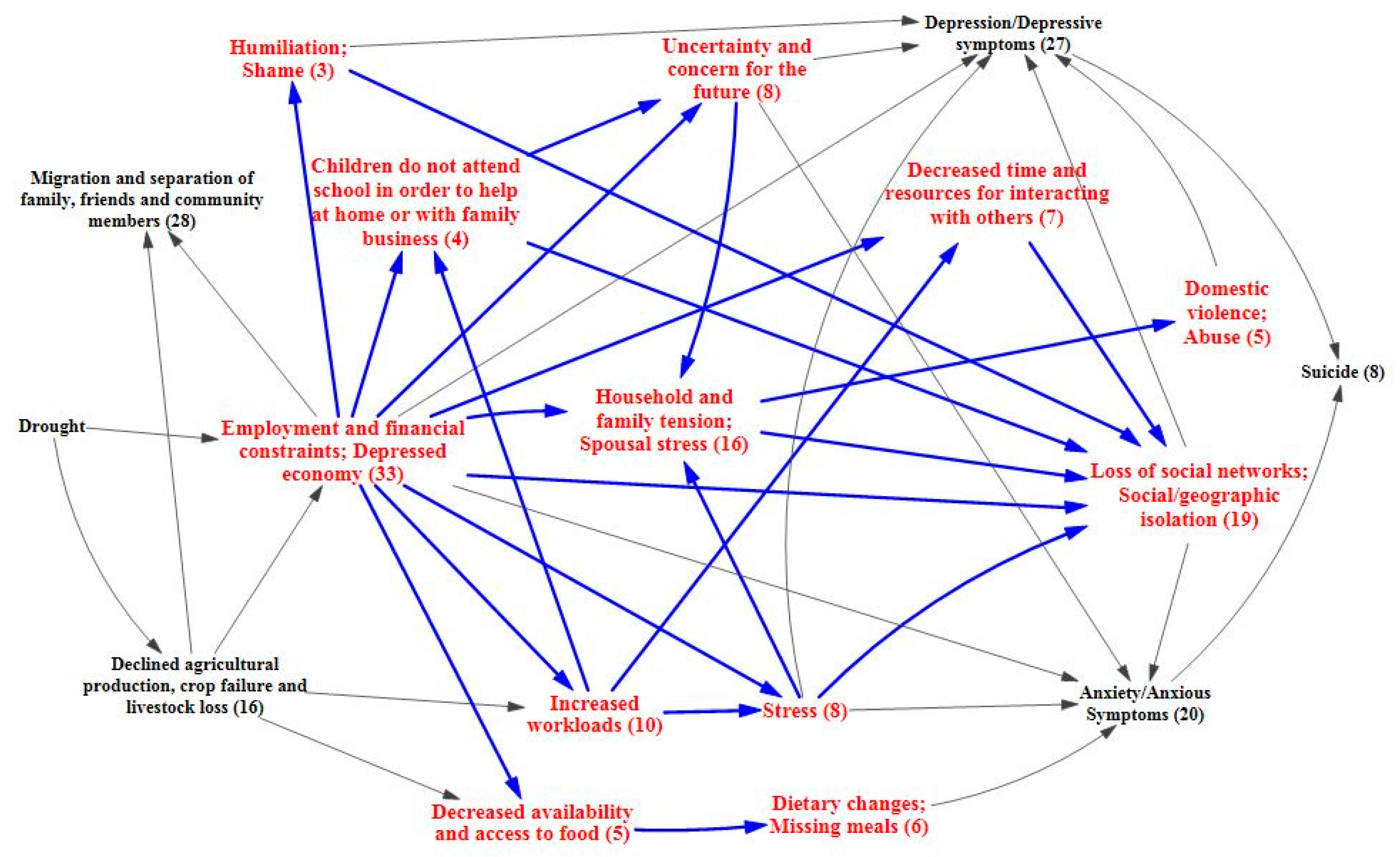
3.3. Vulnerabilities, Protective Factors, and Coping Strategies
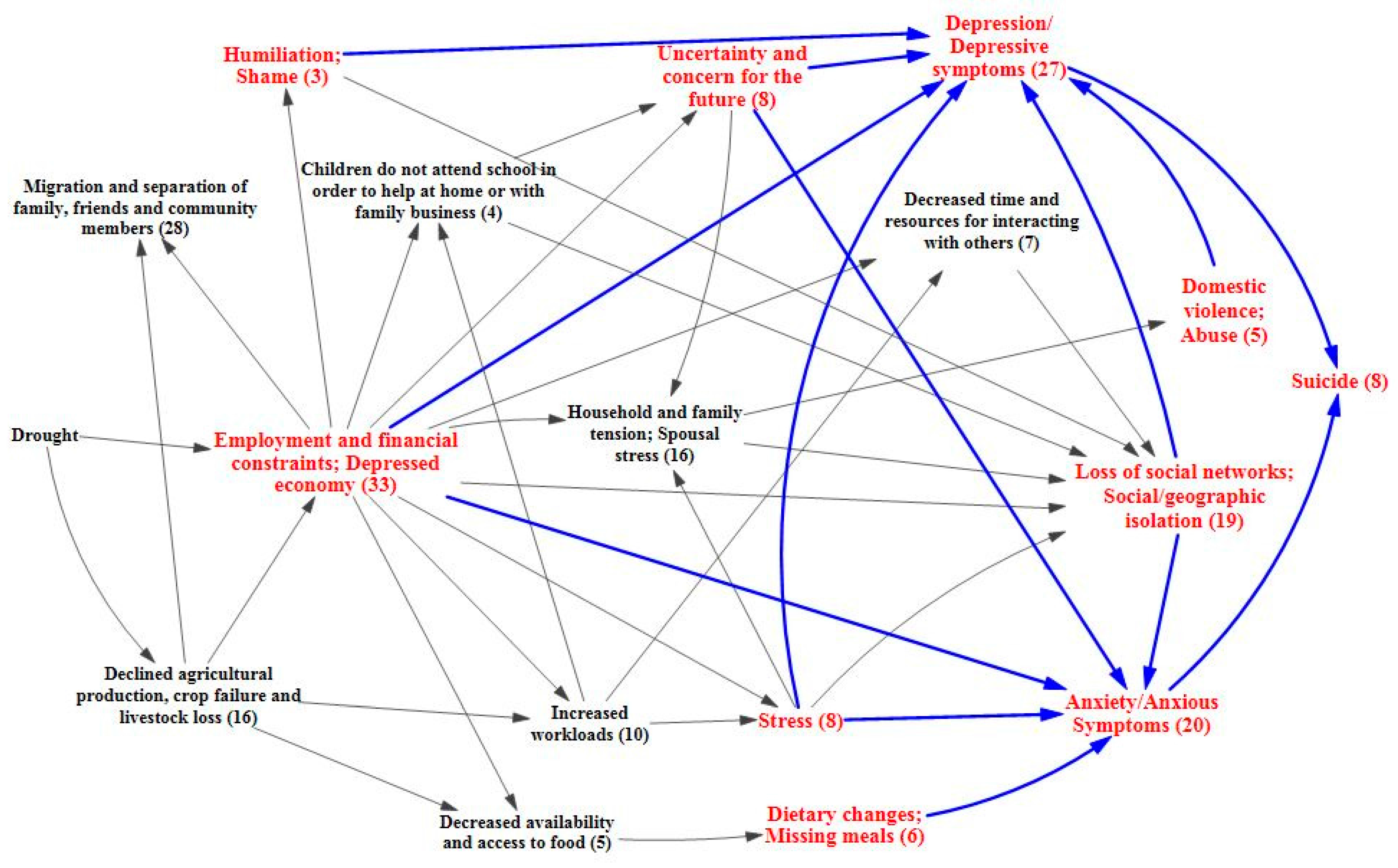
| Vulnerable Characteristics | Protective Factors | Coping Mechanisms |
|---|---|---|
| Rural or remote population (32) Farming or agriculture dependent population (22) Indigenous population (6) Perceived stigma associated with mental health issues (12) Lack of knowledge surrounding mental health issues and availability of services (11) Previous mental health issues or other adverse life events (5) Exposure to an extended period, more intense or severe drought (5) | Social support, social capital and sense of community belonging (15) Shared knowledge and community preparedness regarding availability and access to services (6) Mental health literacy (2) Government assistance and initiatives in place (6) | Employing practical solutions and active methods, including planning for the future (7) Psychological methods, including positive thinking, acceptance and reframing of the problem (4) Utilizing social support and talking about the problem (3) Distracting oneself from the problem; taking a break (2) Turning to religion (3) Alcohol and substance use (8) Denial and avoidance of the problem (3) |
4. Discussion
4.1. Application of the Causal Process Diagram
4.1.1. Prevention Planning
| Broad Category | Component of Diagram/Table | Data | Available from |
|---|---|---|---|
| Distal Exposure | Drought | Palmer drought severity and crop moisture indices for the US | National Weather Service/NOAA Center for Weather and Climate Prediction |
| Drought | GIS and tabular data for drought severity the United States | United States Drought Monitor | |
| Secondary and Intermediate Exposures | Declined crop production, crop failure and livestock loss | Various datasets pertaining to crop production, food prices, and farm economies | United States Department of Agriculture |
| Declined crop production, crop failure and livestock loss | Agricultural data searchable by commodity, location or time period | United States Department of Agriculture | |
| Migration | Changing population counts in rural and urban areas | United States Census | |
| Employment and financial constraints/depressed economy | Unemployment and labor force statistics | Bureau of Labor Statistics | |
| Employment and financial constraints/depressed economy | Poverty data | United States Census | |
| Children do not attend school | School enrollment data | United States Census | |
| Protective Factors and Coping Strategies | Social support | Data on available mental health treatment and levels of emotional support available | Health Indicators Warehouse—Department of Health and Human Services |
| Alcohol and Substance Use | Data on alcohol and illicit drug usage | Health Indicators Warehouse - Department of Health and Human Services | |
| Outcomes | Mental Health | Data on anxiety, depression, conduct and panic disorders | National Health and Nutrition Examination Survey—Centers for Disease Control and Prevention |
| Mental Health | Data on mental health disorders, suicide attempts and deaths | Health Indicators Warehouse—Department of Health and Human Services | |
| Mental Health | Data on depressive disease, anxiety, suicide, domestic violence | Emergency department records | |
| Mental Health | Suicide as cause of death data | National Violent Death Reporting System—Centers for Disease Control and Prevention |
4.1.2. Public Health Programming
4.1.3. Vulnerability and Risk Assessment
4.1.4. Future Research
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Disclaimer
References
- Andreadis, K.M.; Clark, E.A.; Wood, A.W.; Hamlet, A.F.; Lettenmaier, D.P. Twentieth-century drought in the conterminous united states. Am. Meteorol. Soc. 2005, 6, 985–1001. [Google Scholar] [CrossRef]
- The National Drought Mitigation Center. Drought in the Dust Bowl Years. Available online: http://drought.unl.edu/DroughtBasics/DustBowl/DroughtintheDustBowlYears.aspx (accessed on 14 March 2015).
- NOAA Paleoclimatology Program. North American Drought: A Paleo Perspective. Available online: http://www.ncdc.noaa.gov/paleo/drought/drght_home.html (accessed on 14 March 2015).
- National Parks Service. History of Wildland Fire in Yellowstone. Available online: http://www.nps.gov/yell/learn/nature/wildlandfire.htm (accessed on 17 April 2015).
- NOAA National Climatic Data Center. State of the Climate: Drought for Annual 2012. Available online: http://www.ncdc.noaa.gov/sotc/drought/2012/13 (accessed on 14 March 2015).
- Dewey, K. Western Drought Brings Lake Mead to Lowest Level since it was Built. Available online: http://www.climate.gov/news-features/featured-images/western-drought-brings-lake-mead-lowest-level-it-was-built (accessed on 23 March 2015).
- Lindsey, R. California Facing Worst Drought on Record. Available online: http://www.climate.gov/news-features/event-tracker/california-facing-worst-drought-record (accessed on 23 March 2015).
- Lindsey, R. January Precipitation Deficits Keep California Drought Outlook Grim. Available online: http://www.climate.gov/news-features/event-tracker/january-precipitation-deficits-keep-california-drought-outlook-grim (accessed on 23 March 2015).
- NOAA National Climatic Data Center. State of the Climate: Drought for February 2015. Available online: https://www.ncdc.noaa.gov/sotc/drought/201502 (accessed on 14 March 2015).
- Sarvestani, A. Fire forecasting: Texas Watches for Wildfires before They Burn. Available online: http://www.climate.gov/news-features/climate-case-studies/fire-forecasting-texas-watches-wildfires-they-burn (accessed on 23 March 2015).
- Scott, M. Despite Fall Floods, Drought Persists in Southeastern Colorado. Available online: http://www.climate.gov/news-features/event-tracker/despite-fall-floods-drought-persists-southeastern-colorado (accessed on 23 March 2015).
- Governor’s Press Office. Governor Brown Directs First Ever Statewide Mandatory Water Reductions. Available online: https://www.gov.ca.gov/news.php?id=18913 (accessed on 10 April 2015).
- Thomas, R.K.; Melillo, J.M.; Peterson, T.C. Global Climate Change Impacts in the United States; U.S. Global Change Research Program: Washington, DC, USA, 2009.
- Melillo, J.M.; Richmond, T.C.; Gary, W.Y. Climate Change Impacts in the United States: The Third National Climate Assessment; U.S. Global Change Research Program: Washington, DC, USA, 2014.
- Vaughan, D.G.; Comiso, J.C.; Allison, I.; Carrasco, J.; Kaser, G.; Kwok, R.; Mote, P.; Murray, T.; Paul, F.; Ren, J.; et al. Observations: Cryosphere. In Climate Change 2013: The Physical Science Basis. Contribution of Working Group I to the Fifth Assessment Report of the Intergovernmental Panel on Climate Change; Stocker, T.F., Qin, D., Plattner, G.-K., Tignor, M., Allen, S.K., Boschung, J., Nauels, A., Xia, Y., Bex, V., Midgley, P.M., Eds.; Cambridge University Press: Cambridge, UK and New York, NY, USA, 2013; pp. 317–382. [Google Scholar]
- Romero-Lankao, P.; Smith, J.B.; Davidson, D.J.; Diffenbaugh, N.S.; Kinney, P.L.; Kirshen, P.; Kovacs, P.; Villers-Ruiz, L. North America. In Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part B: Regional Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel of Climate Change; Barros, V.R., Field, C.B., Dokken, D.J., Mastrandrea, M.D., Mach, K.J., Bilir, T.E., Chatterjee, M., Ebi, K.L., Estrada, Y.O., Genova, R.C., et al., Eds.; Cambridge University Press: Cambridge, UK and New York, NY, USA, 2014; pp. 1439–1498. [Google Scholar]
- Portier, C.J.; Thigpen, T.K.; Carter, S.R.; Dilworth, C.H.; Grambsch, A.E.; Gohlke, J.; Hess, J.; Howard, S.N.; Luber, G.; Lutz, J.T.; et al. A human health perspective on climate change: A report outlining the research needs on the human health effects of climate change. Environ. Health Pers 2010. [Google Scholar] [CrossRef]
- Kim, K.H.; Kabir, E.; Ara Jahan, S. A review of the consequences of global climate change on human health. J. Environ. Sci. Health 2014, 32, 299–318. [Google Scholar] [CrossRef] [PubMed]
- Olsson, L.; Opondo, M.; Tschakert, P.; Agrawal, A.; Eriksen, S.H.; Ma, S.; Perch, L.N.; Zakieldeen, S.A. Livelihoods and Poverty. In Climate Change 2014: Impacts, Adaptation, and Vulnerability. Part A: Global and Sectoral Aspects. Contribution of Working Group II to the Fifth Assessment Report of the Intergovernmental Panel of Climate Change; Field, C.B., Barros, V.R., Dokken, D.J., Mach, K.J., Mastrandrea, M.D., Bilir, T.E., Chatterjee, M., Ebi, K.L., Estrada, Y.O., Genova, R.C., et al., Eds.; Cambridge University Press: Cambridge, UK and New York, NY, USA, 2014; pp. 793–832. [Google Scholar]
- Pelling, M.; Özerdem, A.; Barakat, S. The macro-economic impact of disasters. Prog. Dev. Stud. 2002, 2, 283–305. [Google Scholar] [CrossRef]
- National Climatic Data Center. Billion-Dollar Weather and Climate Disasters: Table of Events. Avialable online: https://www.ncdc.noaa.gov/billions/events (accessed on 15 April 2015).
- Clayton, S.; Manning, C.M.; Hodge, C. Beyond Storms & Droughts: The Psychological Impacts of Climate Change; American Psychological Association and EcoAmerica: Washington, DC, USA, 2014. [Google Scholar]
- Heim, R.R. A review of twentieth-century drought indices used in the United States. Bull. Am. Meteor. Soc. 2002, 83, 1149–1165. [Google Scholar]
- Coelho, A.E.L.; Adair, J.G.; Mocelllin, J.S.P. Psychological responses to drought in Northeastern Brazil. Interam. J. Psychol. 2004, 38, 95–103. [Google Scholar]
- Sartore, G.; Hoolahan, B.; Tonna, A.; Kelly, B.; Stain, H. Wisdom from the drought: Recommendations from a consultative conference. Aust. J. Rural Health 2005, 13, 315–320. [Google Scholar] [CrossRef] [PubMed]
- O’Brien, L.V.; Berry, H.L.; Coleman, C.; Hanigan, I.C. Drought as a mental health exposure. Environ. Res. 2014, 131, 181–187. [Google Scholar] [CrossRef] [PubMed]
- The National Drought Mitigation Center. Types of Drought. Avialable online: http://drought.unl.edu/DroughtBasics/TypesofDrought.aspx (acessed on 14 March 2015).
- World Health Organization. Mental Health: Strengthening Our Response; World Health Organization: Geneva, Switherland, 2014. [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders; American Psychiatric Association: Arilington, VA, USA, 2013; Use of the Manual. [Google Scholar]
- National Institute of Mental Health. Individual Mental and Behavioral Disorders for Us. Avialable online: http://www.nimh.nih.gov/health/statistics/disability/individual-mental-and-behavioral-disorders-for-us.shtml (accessed on 14 March 2015).
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders; American Psychiatric Association: Arilington, VA, USA, 2013; Depressive disorders. [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders; American Psychiatric Association: Arilington, VA, USA, 2013; Anxiety disorders. [Google Scholar]
- Berry, H.L.; Bowen, K.; Kjellstrom, T. Climate change and mental health: A causal pathways framework. Int. J. Public Health 2010, 55, 123–132. [Google Scholar] [CrossRef] [PubMed]
- Berry, H.L.; Kelly, B.; Hanigan, I.; Coates, J.; McMichael, A.J.; Welsh, J.; Kjellstrom, T. Rural mental health impacts of climate change. In Commissioned Report for the Garnaut Climate Change Review; The Australian National University: Canberra, Ausralia, 2008. [Google Scholar]
- Ahern, M.; Kovats, R.S.; Wilkinson, P.; Few, R.; Matthies, F. Global health impacts of floods: Epidemiologic evidence. Epidemiol. Rev. 2005, 27, 36–46. [Google Scholar] [CrossRef] [PubMed]
- Basu, R. Relation between elevated ambient temperature and mortality: A review of the epidemiologic evidence. Epidemiol. Rev. 2002, 24, 190–202. [Google Scholar] [CrossRef] [PubMed]
- North, C.S.; Hong, B.A.; Suris, A.; Spitznagel, E.L. Distinguishing distress and psychopathology among survivors of the Oakland/Berkeley firestorm. Psychiatry 2008, 71, 35–45. [Google Scholar] [CrossRef] [PubMed]
- Vida, S.; Durocher, M.; Ouarda, T.B.M.J.; Gosselin, P. Relationship between ambient temperature and humidity and visits to mental health emergency departments in Quebec. Psychiatr. Serv. 2012, 63, 1150–1153. [Google Scholar] [CrossRef] [PubMed]
- Khan, K.S.; Kunz, R.; Kleijnen, J.; Antes, G. Five steps to conducting a systematic review. J. Roy. Soc. Med. 2003, 96, 118–121. [Google Scholar] [CrossRef] [PubMed]
- Hosking, J.; Campbell-Lendrum, D. How well does climate change and human health research match the demands of policymakers? A scoping review. Environ. Health Perspect. 2012, 120, 1076–1082. [Google Scholar] [CrossRef] [PubMed]
- Hess, J.J.; Eidson, M.; Tlumak, J.E.; Raab, K.K.; Luber, G. An evidence-based public health approach to climate change adaptation. Environ. Health Perspect. 2014, 122, 1177–1186. [Google Scholar] [CrossRef] [PubMed]
- Joffe, M.; Mindell, J. Complex causal process diagrams for analyzing the health impacts of policy interventions. Am. J. Public Health 2006, 96, 473–479. [Google Scholar] [CrossRef] [PubMed]
- Perry, R.W. Environmental hazards and psychopathology: Linking natural disasters with mental health. Environ. Manag. 1983, 7, 543–551. [Google Scholar] [CrossRef]
- Alston, M. Rural male suicide in Australia. Soc. Sci. Med. 2012, 74, 515–522. [Google Scholar] [CrossRef] [PubMed]
- Alston, M.; Kent, J. The big dry: The link between rural masculinities and poor health outcomes for farming men. J. Sociol. 2008, 44, 133–147. [Google Scholar] [CrossRef]
- Anderson, D. Enduring drought then coping with climate change: Lived experience and local resolve in rural mental health. Rural Soc. 2009, 19, 340–352. [Google Scholar] [CrossRef]
- Berry, H.L.; Hogan, A.; Owen, J.; Rickwood, D.; Fragar, L. Climate change and farmers’ mental health: Risks and responses. Asia. Pac. J. Public Health 2011, 23, 119S–132S. [Google Scholar] [CrossRef] [PubMed]
- Boetto, H.; McKinnon, J. Rural women and climate change: A gender-inclusive perspective. Aust. Soc. Work 2013, 66, 234–247. [Google Scholar] [CrossRef]
- Bourque, F.; Willox, A.C. Climate change: The next challenge for public mental health? Int. Rev. Psychiat. 2014, 26, 415–422. [Google Scholar] [CrossRef] [PubMed]
- Carnie, T.L.; Berry, H.L.; Blinkhorn, S.A.; Hart, C.R. In their own words: Young people’s mental health in drought-affected rural and remote nsw. Aust. J. Rural Health 2011, 19, 244–248. [Google Scholar] [CrossRef] [PubMed]
- Caruana, C. Picking up the pieces: Family functioning in the aftermath of natural disaster. Fam. Matters 2010, 84, 79–88. [Google Scholar]
- Hart, C.R.; Berry, H.L.; Tonna, A.M. Improving the mental health of rural New South Wales communities facing drought and other adversities. Aust. J. Rural Health 2011, 19, 231–238. [Google Scholar] [CrossRef] [PubMed]
- Hossain, D.; Eley, R.; Coutts, J.; Gorman, D. Mental health of farmers in southern Queensland: Issues and support. Aust. J. Rural Health 2008, 16, 343–348. [Google Scholar] [CrossRef] [PubMed]
- Nicholls, N.; Butler, C.D.; Hanigan, I. Inter-annual rainfall variations and suicide in New South Wales, Australia, 1964–2001. Int. J. Biometeorol. 2006, 50, 139–143. [Google Scholar] [CrossRef] [PubMed]
- Rigby, C.W.; Rosen, A.; Berry, H.L.; Hart, C.R. If the land’s sick, we’re sick: * The impact of prolonged drought on the social and emotional well-being of aboriginal communities in rural New South Wales. Aust. J. Rural Health 2011, 19, 249–254. [Google Scholar] [CrossRef] [PubMed]
- Sartore, G.M.; Kelly, B.; Stain, H.; Albrecht, G.; Higginbotham, N. Control, Uncertainty, and Expectations for the Future: A Qualitative Study of the Impact of Drought on Rural Australian Community. Avialiable online: http://www.rrh.org.au/articles/subviewnew.asp?ArticleID=950 (accessed on 19 January 2015).
- Wutich, A. Intrahousehold disparities in women and men’s experiences of water insecurity and emotional distress in urban Bolivia. Med. Anthropol. Quart. 2009, 23, 436–454. [Google Scholar] [CrossRef]
- Babugura, A.A. Vulnerability of children and youth in drought disasters: A case study of Botswana. Child. Youth Environ. 2008, 18, 126–157. [Google Scholar]
- Chur-Hansen, A. Grief and bereavement issues and the loss of a companion animal: People living with a companion animal, owners of livestock, and animal support workers. Clinic. Psychol. 2010, 14, 14–21. [Google Scholar] [CrossRef]
- Dash, J.; Behura, N.K. Crisis management: Lessons from the past—A case study of drought situation in Kalahandi (undivided) of Orissa. Man India 2003, 83, 121–134. [Google Scholar]
- Edwards, A. Influence of drought and depression on a rural community—A case study in Haskell county, Kansas. Soc. Res. Rep. 1939, 7, 1–116. [Google Scholar]
- Edwards, B.; Gray, M.; Hunter, B. The impact of drought on mental health in rural and regional Australia. Soc. Indic. Res. 2014, 121, 177–194. [Google Scholar] [CrossRef]
- Friel, S.; Bowen, K.; Campbell-Lendrum, D.; Frumkin, H.; McMichael, A.J.; Rasanathan, K. Climate change, noncommunicable diseases, and development: The relationships and common policy opportunities. Annu. Rev. Public Health 2011, 32, 133–147. [Google Scholar] [CrossRef] [PubMed]
- Murendo, C.; Keil, A.; Zeller, M. Drought impacts and related risk management by smallholder farmers in developing countries: Evidence from awash river basin, Ethiopia. Risk Manag. 2011, 13, 247–263. [Google Scholar] [CrossRef]
- Ang, H.B.A.; Lamm, F.; Tipples, R. The impact of stressors on the psychological wellbeing of New Zealand farmers and the development of an explanatory conceptual model. Policy Pract. Health Safe. 2008, 6, 79–96. [Google Scholar]
- Dean, J.; Stain, H.J. The impact of drought on the emotional well-being of children and adolescents in rural and remote New South Wales. J. Rural Health 2007, 23, 356–364. [Google Scholar] [CrossRef] [PubMed]
- Keshavarz, M.; Karami, E.; Vanclay, F. The social experience of drought in rural Iran. Land Use Policy 2013, 30, 120–129. [Google Scholar] [CrossRef]
- Huddar, G.; Malakajappa, P.N.S. Agrarian distress and farmers’ suicides in Karnataka: Strategy for prevention. Int. Multidiscipl. Res. J. 2011, 1, 1–5. [Google Scholar]
- Cunsolo, W.A.; Harper, S.L.; Ford, J.D.; Landman, K.; Houle, K.; Edge, V.L. Rigolet Inuit Community Government. “From this place and of this place”: Climate change, sense of place, and health in Nunatsiavut, Canada. Soc. Sci. Med. 2012, 75, 538–547. [Google Scholar] [CrossRef] [PubMed]
- Dean, J.G.; Stain, H.J. Mental health impact for adolescents living with prolonged drought. Aust. J. Rural Health 2010, 18, 32–37. [Google Scholar] [CrossRef] [PubMed]
- Gilbert, G.; McLeman, R. Household access to capital and its effects on drought adaptation and migration: A case study of rural Alberta in the 1930s. Popul. Environ. 2010, 32, 3–26. [Google Scholar] [CrossRef]
- Laforge, J.M.L.; McLeman, R. Social capital and drought-migrant integration in 1930s Saskatchewan. Can. Geogr. 2013, 57, 488–505. [Google Scholar] [CrossRef]
- McLeman, R. Migration out of 1930s rural eastern Oklahoma: Insights for climate change research. Great Plains Quart. 2006, 26, 27–40. [Google Scholar]
- McLeman, R.A.; Ploeger, S.K. Soil and its influence on rural drought migration: Insights from depression-era southwestern Saskatchewan, Canada. Popul. Environ. 2011, 33, 304–332. [Google Scholar] [CrossRef]
- Polain, J.D.; Berry, H.L.; Hoskin, J.O. Rapid change, climate adversity and the next “big dry”: Older farmers’ mental health. Aust. J. Rural Health 2011, 19, 239–243. [Google Scholar] [CrossRef] [PubMed]
- Zamani, G.H.; Gorgievski-Duijvesteijn, M.J.; Zarafshani, K. Coping with drought: Towards a multilevel understanding based on conservation of resources theory. Hum. Ecol. 2006, 34, 677–692. [Google Scholar] [CrossRef]
- Fuller, J.; Edwards, J.; Procter, N.; Moss, J. How definition of mental health problems can influence help seeking in rural and remote communities. Aust. J. Rural Health 2000, 8, 148–153. [Google Scholar] [CrossRef] [PubMed]
- McShane, C.J.; Quirk, F. Mediating and moderating effects of work-home interference upon farm stresses and psychological distress. Aust. J. Rural Health 2009, 17, 244–250. [Google Scholar] [CrossRef] [PubMed]
- Staniford, A.K.; Dollard, M.F.; Guerin, B. Stress and help-seeking for drought-stricken citrus growers in the riverland of south Australia. Aust. J. Rural Health 2009, 17, 147–154. [Google Scholar] [CrossRef] [PubMed]
- Tonna, A.; Kelly, B.; Crockett, J.; Greig, J.; Buss, R.; Roberts, R.; Wright, M. Improving the mental health of drought-affected communities: An Australian model. Rural Soc. 2014, 19, 296–305. [Google Scholar] [CrossRef]
- Parkar, S.R.; Fernandes, J.; Weiss, M.G. Contextualizing mental health: Gendered experiences in a Mumbai slum. Anthropol. Med. 2003, 10, 291–308. [Google Scholar] [CrossRef]
- Mathew, L. Coping with shame of poverty: Analysis of farmers in distress. Psychol. Dev. Soc. 2010, 22, 385–407. [Google Scholar] [CrossRef]
- Novello, D.J.; Stain, H.J.; Lyle, D.; Kelly, B.J. Psychological distress of rural parents: Family influence and the role of isolation. Aust. J. Rural Health 2011, 19, 27–31. [Google Scholar] [CrossRef] [PubMed]
- Cunsolo, W.A.; Harper, S.L.; Ford, J.D.; Edge, V.L.; Landman, K.; Houle, K.; Blake, S.; Wolfrey, C. Climate change and mental health: An exploratory case study from Rigolet, Nunatsiavut, Canada. Clim. Change 2013, 121, 255–270. [Google Scholar] [CrossRef]
- Fragar, L.; Kelly, B.; Peters, M.; Henderson, A.; Tonna, A. Partnerships to promote mental health of NSW farmers: The New South Wales farmers blueprint for mental health. Aust. J. Rural Health 2008, 16, 170–175. [Google Scholar] [CrossRef] [PubMed]
- Williams, R.T. The On-Going Farm Crisis: Extension Leadership in Rural Communities. Available online: http://www.joe.org/joe/1996february/a3.php (accessed on 19 January 2015).
- Hanigan, I.C.; Butler, C.D.; Kokic, P.N.; Hutchinson, M.F. Suicide and drought in New South Wales, Australia, 1970–2007. P. Natl. Acad. Sci. USA 2012, 109, 13950–13955. [Google Scholar] [CrossRef] [PubMed]
- Albrecht, G.; Sartore, G.M.; Connor, L.; Higginbotham, N.; Freeman, S.; Kelly, B.; Stain, H.; Torma, A.; Pollard, G. Solastalgia: The distress caused by environmental change. Aust. Psychiat. 2007, 15, S95–S98. [Google Scholar] [CrossRef] [PubMed]
- Doherty, T.J.; Clayton, S. The psychological impacts of global climate change. Am. Psychol. 2011, 66, 265–276. [Google Scholar] [CrossRef] [PubMed]
- Hoffman, C.S. Drought and depression migration into oregon, 1930 to 1936. Mon. Labor Rev. 1938, 46, 27–35. [Google Scholar]
- Shukla, J. Extreme weather events and mental health: Tackling the psychosocial challenge. ISRN Public Health 2013, 2013, 1–7. [Google Scholar] [CrossRef]
- Albrecht, G. “Solastalgia”. A new concept in health and identity. Philos. Activism Nature 2005, 3, 41–55. [Google Scholar]
- Warren, J.A.; Berner, J.E.; Curtis, T. Climate change and human health: Infrastructure impacts to small remote communities in the north. Int. J. Circumpol. Health 2005, 64, 487–497. [Google Scholar] [CrossRef]
- Wutich, A.; Ragsdale, K. Water insecurity and emotional distress: Coping with supply, access, and seasonal variability of water in a Bolivian squatter settlement. Soc. Sci. Med. 2008, 67, 2116–2125. [Google Scholar] [CrossRef] [PubMed]
- Elliott-Schmidt, R.; Strong, J. The concept of well-being in a rural setting: Understanding health and illness. Aust. J. Rural Health 1997, 5, 59–63. [Google Scholar] [CrossRef] [PubMed]
- Harvey, D.J. Understanding Australian Rural Women’s Ways of Achieving Health and Wellbeing—A Metasynthesis of the Literature. Avialiable online: http://www.rrh.org.au/articles/subviewnew.asp?ArticleID=823 (accessed on 19 January 2015).
- Pierce, D. Factors promoting use of mental health services in a rural area of Australia. J. Comm. Med. Health Educ. 2012, 2. [Google Scholar] [CrossRef]
- Boyd, C.P.; Hayes, L.; Nurse, S.; Aisbett, D.L.; Francis, K.; Newnham, K.; Sewell, J. Preferences and Intention of Rural Adolescents toward Seeking Help for Mental Health Problems. Avialiable online: http://www.rrh.org.au/Articles/subviewnew.asp?ArticleID=1582 (accessed on 19 January 2015).
- Kennedy, A.J.; Maple, M.J.; McKay, K.; Brumby, S.A. Suicide and Accidental Death in Australia's Rural Farming Communities: A Review of the Literature. Avialiable online: http://www.rrh.org.au/articles/showarticlenew.asp?ArticleID=2517 (accessed on 19 January 2015).
- Kelly, B.J.; Lewin, T.J.; Stain, H.J.; Coleman, C.; Fitzgerald, M.; Perkins, D.; Carr, V.J.; Fragar, L.; Fuller, J.; Lyle, D.; et al. Determinants of mental health and well-being within rural and remote communities. Soc. Psych. Psych. Epid. 2011, 46, 1331–1342. [Google Scholar] [CrossRef] [PubMed]
- Gorman, D.; Buikstra, E.; Hegney, D.; Pearce, S.; Rogers-Clark, C.; Weir, J.; McCullagh, B. Rural men and mental health: Their experiences and how they managed. Int. J. Ment. Health Nurs. 2007, 16, 298–306. [Google Scholar] [CrossRef] [PubMed]
- McLaren, S.; Challis, C. Resilience among men farmers: The protective roles of social support and sense of belonging in the depression-suicidal ideation relation. Death Stud. 2009, 33, 262–276. [Google Scholar] [CrossRef] [PubMed]
- Roy, P.; Tremblay, G.; Oliffe, J.L.; Jbilou, J.; Robertson, S. Male farmers with mental health disorders: A scoping review. Aust. J. Rural Health 2013, 21, 3–7. [Google Scholar] [CrossRef] [PubMed]
- Powers, J.R.; Loxton, D.; Baker, J.; Rich, J.L.; Dobson, A.J. Empirical evidence suggests adverse climate events have not affected Australian women’s health and well-being. Aust. NZ. J. Public Health 2012, 36, 452–457. [Google Scholar] [CrossRef] [PubMed]
- Allen, J.; Inder, K.J.; Lewin, T.J.; Attia, J.; Kelly, B.J. Social support and age influence distress outcomes differentially across urban, regional and remote Australia: An exploratory study. BMC Public Health 2012, 12. [Google Scholar] [CrossRef] [PubMed]
- Schulman, M.D.; Armstrong, P.S. Perceived stress, social support and survival: North Carolina farm operators and the farm crisis. J. Soc. Soc. Welfare 1990, 17, 3–22. [Google Scholar]
- Stain, H.J.; Kelly, B.; Lewin, T.J.; Higginbotham, N.; Beard, J.R.; Hourihan, F. Social networks and mental health among a farming population. Soc. Psych. Psych. Epidemiol. 2008, 43, 843–849. [Google Scholar] [CrossRef] [PubMed]
- Caldwell, K.; Boyd, C.P. Coping and Resilience in Farming Families Affected by Drought. Avialiable online: http://www.rrh.org.au/articles/subviewaust.asp?ArticleID=1088 (accessed on 19 January 2015).
- Wilson, R.L. Out back and out-of-whack: Issues Related to the Experience of Early Psychosis in the New England Region, New South Wales, Australia. Avialiable online: http://www.rrh.org.au/articles/subviewnew.asp?articleid=715 (accessed on 19 January 2015).
- Gunn, K.M.; Kettler, L.J.; Skaczowski, G.L.A.; Turnbull, D.A. Farmers’ Stress and Coping in a Time of Drought. Avialiable online: http://www.rrh.org.au/Articles/subviewnew.asp?-ArticleID=2071 (accessed on 19 January 2015).
- Taylor, M.; Barr, M.; Stevens, G.; Bryson-Taylor, D.; Agho, K.; Jacobs, J.; Raphael, B. Psychosocial stress and strategies for managing adversity: Measuring population resilience in New South Wales, Australia. Popul. Health Metr. 2010, 8. [Google Scholar] [CrossRef] [PubMed]
- Rosmann, M.R. Sowing the seeds of hope: Providing regional behavioral health supports to the agricultural population. J. Agr. Safety Health 2005, 11, 431–439. [Google Scholar] [CrossRef]
- Guiney, R. Farming suicides during the victorian drought: 2001–2007. Aust. J. Rural Health 2012, 20, 11–15. [Google Scholar] [CrossRef] [PubMed]
- Leigh, A.; Neill, C. Do gun buybacks save lives? Evidence from panel data. Am. Law Econ. Rev. 2010, 12, 509–557. [Google Scholar] [CrossRef]
- Powers, J.R.; Dobson, A.J.; Berry, H.L.; Graves, A.M.; Hanigan, I.C.; Loxton, D. Lack of association between drought and mental health in a cohort of 45–61 year old rural Australian women. Aust. NZ. J. Publ. Heal. 2015, 39. [Google Scholar] [CrossRef] [PubMed]
- Boxall, A.; Hardy, A.; Beulke, S.; Boucard, T.; Burgin, L.; Falloon, P.D.; Haygarth, P.M.; Hutchinson, T.; Kovats, R.S.; Leonardi, G. Impacts of climate change on indirect human exposure to pathogens and chemicals from agriculture. Environ. Health Perspect. 2008, 117, 508–514. [Google Scholar] [CrossRef] [PubMed]
- Kirkhorn, S.; Schenker, M. Current health effects of agricultural work: Respiratory disease, cancer, reproductive effects, musculoskeletal injuries, and pesticide-related illnesses. J. Agri. Safety Health 2002, 8, 199–214. [Google Scholar] [CrossRef]
- Howitt, R.; Medellín-Azuara, J.; MacEwan, D.; Lund, J.; Sumner, D. Economic Analysis of the 2014 Drought for California Agriculture; University of California: Davis, CA, USA, 2014. [Google Scholar]
- Füssel, H.-M.; Klein, R.J. Climate change vulnerability assessments: An evolution of conceptual thinking. Clim. Change 2006, 75, 301–329. [Google Scholar] [CrossRef]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Vins, H.; Bell, J.; Saha, S.; Hess, J.J. The Mental Health Outcomes of Drought: A Systematic Review and Causal Process Diagram. Int. J. Environ. Res. Public Health 2015, 12, 13251-13275. https://doi.org/10.3390/ijerph121013251
Vins H, Bell J, Saha S, Hess JJ. The Mental Health Outcomes of Drought: A Systematic Review and Causal Process Diagram. International Journal of Environmental Research and Public Health. 2015; 12(10):13251-13275. https://doi.org/10.3390/ijerph121013251
Chicago/Turabian StyleVins, Holly, Jesse Bell, Shubhayu Saha, and Jeremy J. Hess. 2015. "The Mental Health Outcomes of Drought: A Systematic Review and Causal Process Diagram" International Journal of Environmental Research and Public Health 12, no. 10: 13251-13275. https://doi.org/10.3390/ijerph121013251
APA StyleVins, H., Bell, J., Saha, S., & Hess, J. J. (2015). The Mental Health Outcomes of Drought: A Systematic Review and Causal Process Diagram. International Journal of Environmental Research and Public Health, 12(10), 13251-13275. https://doi.org/10.3390/ijerph121013251






