Impact of the Emergency Procedure Zone on Emergency Care
Abstract
1. Introduction
2. Methods
2.1. Emergency Department
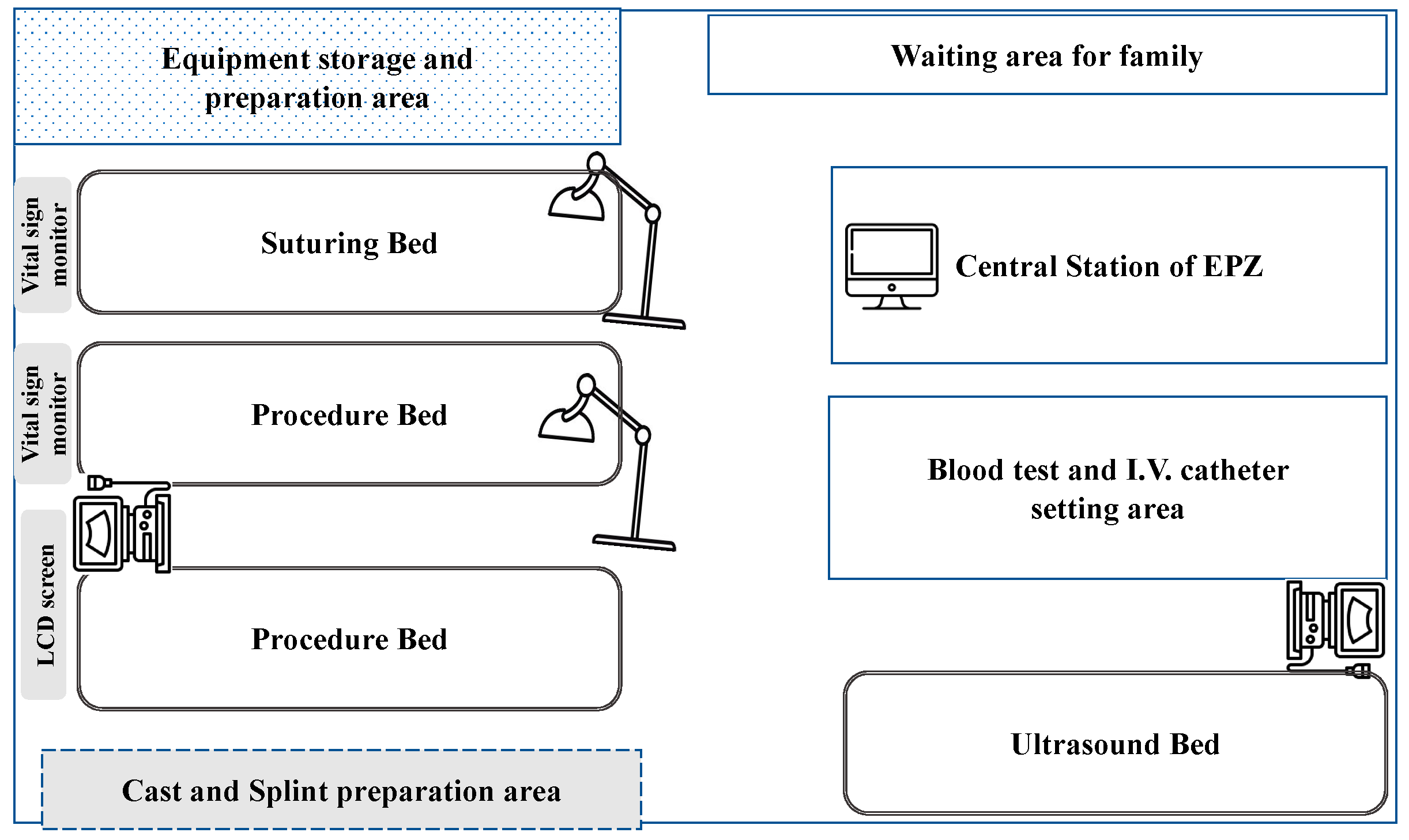
2.2. Emergency Procedure Zone
2.3. Data Collection
2.4. Data Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| CVC | central venous catheter |
| ED | emergency department |
| EPZ | emergency procedure zone |
| FAST | focused abdominal sonography for trauma |
| LOS-ED | length of stay in the emergency department |
| POCUS | point-of-care ultrasound |
References
- Rabin, E.; Kocher, K.; McClelland, M.; Pines, J.; Hwang, U.; Rathlev, N.; Asplin, B.; Trueger, N.S.; Weber, E. Solutions to emergency department “boarding” and crowding are underused and may need to be legislated. Health Aff. 2012, 31, 1757–1766. [Google Scholar] [CrossRef] [PubMed]
- Government Accountability Office; Hospital Emergency Departments. Crowding Continues to Occur, and Some Patients Wait Longer than Recommended Time Frames; GAO: Washington, DC, USA, 2009. [Google Scholar]
- Asplin, B.R.; Magid, D.J.; Rhodes, K.V.; Solberg, L.I.; Lurie, N.; Camargo, C.A., Jr. A conceptual model of emergency department crowding. Ann. Emerg. Med. 2003, 42, 173–180. [Google Scholar] [CrossRef] [PubMed]
- Kenny, J.F.; Chang, B.C.; Hemmert, K.C. Factors affecting emergency department crowding. Emerg. Med. Clin. N. Am. 2020, 38, 573–587. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.-H.; Kao, C.-Y.; Huang, C.-Y. Managing emergency department overcrowding via ambulance diversion: A discrete event simulation model. J. Formos. Med. Assoc. 2015, 114, 64–71. [Google Scholar] [CrossRef] [PubMed]
- Kao, C.Y.; Yang, J.C.; Lin, C.H. The Impact of Ambulance and Patient Diversion on Crowdedness of Multiple Emergency Departments in a Region. PLoS ONE 2015, 10, e0144227. [Google Scholar] [CrossRef] [PubMed]
- Lucas, R.; Farley, H.; Twanmoh, J.; Urumov, A.; Olsen, N.; Evans, B.; Kabiri, H. Emergency department patient flow: The influence of hospital census variables on emergency department length of stay. Acad. Emerg. Med. 2009, 16, 597–602. [Google Scholar] [CrossRef] [PubMed]
- Hsieh, C.-C.; Lee, C.-C.; Hsu, H.-C.; Shih, H.-I.; Lu, C.-H.; Lin, C.-H. Impact of delayed admission to intensive care units on patients with acute respiratory failure. Am. J. Emerg. Med. 2017, 35, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Jarvis, P.; Davies, T.; Mitchell, K.; Taylor, I.; Baker, M. Does rapid assessment shorten the amount of time patients spend in the emergency department? Br. J. Hosp. Med. 2014, 75, 648–651. [Google Scholar] [CrossRef] [PubMed]
- Chaisirin, W.; Wongkrajang, P.; Praphruetkit, N.; Nakornchai, T.; Riyapan, S.; Ruangsomboon, O.; Laiwejpithaya, S.; Rattanathummawat, K.; Pavichai, R.; Chakorn, T.; et al. Role of Point-of-Care Testing in Reducing Time to Treatment Decision-Making in Urgency Patients: A Randomized Controlled Trial. West J. Emerg. Med. 2020, 21, 404–410. [Google Scholar] [CrossRef] [PubMed]
- Jarvis, P.R.E. Improving emergency department patient flow. Clin. Exp. Emerg. Med. 2016, 3, 63–68. [Google Scholar] [CrossRef] [PubMed]
- Langlands, B. Design Distinctions for Exam, Procedure and Operating Rooms: Planning Advice Based on the FGI Guidelines’ Requirements Helps to Ensure Optimally Designed Spaces. Health Facilities Management. 8 October 2019. Available online: https://www.hfmmagazine.com/articles/3764-design-distinctions-for-exam-procedure-and-operating-rooms (accessed on 1 January 2023).
- Beeson, M.S.; Ankel, F.; Bhat, R.; Broder, J.S.; Dimeo, S.P.; Gorgas, D.L.; Jones, J.S.; Patel, V.; Schiller, E.; Ufberg, J.W.; et al. The 2019 Model of the Clinical Practice of Emergency Medicine. J. Emerg. Med. 2020, 59, 96–120. [Google Scholar] [CrossRef] [PubMed]
- Kuo, Y.-S.; Lu, C.-H.; Chiu, P.-W.; Chang, H.-C.; Lin, Y.-Y.; Huang, S.-P.; Wang, P.-Y.; Chen, C.-J.; Lin, I.-C.; Tang, J.-S.; et al. Challenges of Using Instant Communication Technology in the Emergency Department during the COVID-19 Pandemic: A Focus Group Study. Int. J. Environ. Res. Public Health 2021, 18, 12463. [Google Scholar] [CrossRef] [PubMed]
- Yoo, J.; Kang, S.Y.; Jo, I.J.; Kim, T.; Lee, G.; Park, J.E.; Hwang, S.Y.; Cha, W.C.; Shin, T.G.; Yoon, H. The Use of Point-of-care Ultrasound in Emergency Medical Centers in Korea: A National Cross-sectional Survey. J. Korean Med. Sci. 2021, 36, e141. [Google Scholar] [CrossRef] [PubMed]
- Adhikari, S.; Amini, R.; Stolz, L.; Blaivas, M. Impact of point-of-care ultrasound on quality of care in clinical practice. Rep. Med. Imaging 2014, 2014, 81–93. [Google Scholar] [CrossRef]
- Fleshner, M.; Fox, S.; Robertson, T.; Fujita, A.W.; Bhamidipati, D.; Bui, T. Impact of Point-of-Care Ultrasound in Medical Decision Making: Informing the Development of an Internal Medicine Global Health POCUS Curriculum. POCUS J. 2022, 7, 144–153. [Google Scholar] [CrossRef] [PubMed]
- Considine, J.; Kropman, M.; E Stergiou, H. Effect of clinician designation on emergency department fast track performance. Emerg. Med. J. 2010, 27, 838–842. [Google Scholar] [CrossRef] [PubMed]
- Taylor, J.K.; Gaillemin, O.S.; Pearl, A.J.; Murphy, S.; Fox, J. Embedding comprehensive geriatric assessment in the emergency assessment unit: The impact of the COPE zone. Clin. Med. 2016, 16, 19–24. [Google Scholar] [CrossRef] [PubMed]
- Emergency Department Design Guidelines Australasian College for Emergency Medicine (ACEM) Ver.No3. Available online: https://acem.org.au/getmedia/faf63c3b-c896-4a7e-aa1f-226b49d62f94/Emergency_Department_Design_Guidelines (accessed on 1 May 2023).
| Pre-EPZ N = 137,141 n (%) | Post-EPZ N = 118,386 n (%) | p Value | ||
|---|---|---|---|---|
| Age | Adults (≥18 years) | 113,900 (83.1) | 102,539 (86.6) | <0.001 |
| Children (<18 years) | 23,241 (16.9) | 15,847 (13.4) | ||
| Gender | Male | 68,424 (49.9) | 58,583 (49.5) | 0.039 |
| Female | 68,717 (50.1) | 59,803 (50.5) | ||
| Mechanism | Trauma | 41,503 (30.3) | 27,984 (23.6) | <0.001 |
| Non-trauma | 95,638 (69.7) | 90,402 (76.4) | ||
| Triage acuity level | 1 | 5755 (4.2) | 5593 (4.7) | <0.001 |
| 2 | 20,727 (15.1) | 21,020 (17.8) | ||
| 3 | 103,450 (75.4) | 87,902 (74.3) | ||
| 4 | 6661 (4.9) | 2863 (2.4) | ||
| 5 | 548 (0.4) | 1008 (0.9) | ||
| Disposition | Direct discharge from the emergency department | 96,814 (70.6) | 96,215 (81.3) | <0.001 |
| Mean daily patient volume | 249.8 (0.1) | 216.8 (0.1) | <0.001 | |
| Pre-EPZ N = 137,141 n (%) | Post-EPZ N = 118,386 n (%) | p Value | ||
|---|---|---|---|---|
| Procedure | Suture | 6533 (4.76) | 4797 (4.05) | <0.001 |
| CVC insertion | 612 (0.45) | 1572 (1.33) | <0.001 | |
| Chest tube or pigtail placement | 292 (0.21) | 348 (0.29) | <0.001 | |
| Thoracentesis | 543 (0.40) | 524 (0.44) | 0.073 | |
| Abdominocentesis | 396 (0.29) | 281 (0.24) | 0.013 | |
| Arthrocentesis | 42 (0.03) | 129 (0.11) | <0.001 | |
| Lumbar puncture | 150 (0.11) | 408 (0.34) | <0.001 | |
| Incision and drainage | 26 (0.02) | 123 (0.10) | <0.001 | |
| Reduction | 199 (0.15) | 183 (0.15) | 0.571 | |
| Splint | 378 (0.28) | 253 (0.21) | 0.002 | |
| Ultrasound | Total of ultrasound scans | 10,060 (7.34) | 12,053 (10.18) | <0.001 |
| Ultrasound performed in the emergency department (ED) | 2026 (1.48) | 5370 (4.54) | <0.001 | |
| Focused abdominal sonography for trauma (FAST) in the ED | 1426 (1.04) | 2704 (2.28) | <0.001 | |
| Non-FAST in the ED | 600 (0.44) | 2666 (2.25) | <0.001 | |
| Ultrasound performed in the radiology or cardiology department | 8034 (5.86) | 6683 (5.65) | 0.022 |
| Pre-EPZ N = 96,814 n (%) | Post-EPZ N = 96,215 n (%) | p Value | ||
|---|---|---|---|---|
| Procedure | Suture | 5507 (5.69) | 3938 (4.09) | <0.001 |
| CVC insertion | 18 (0.02) | 67 (0.07) | <0.001 | |
| Chest tube or pigtail placement | 10 (0.01) | 8 (0.01) | 0.824 | |
| Thoracentesis | 157 (0.16) | 153 (0.16) | 0.908 | |
| Abdominocentesis | 210 (0.22) | 146 (0.15) | <0.001 | |
| Arthrocentesis | 17 (0.02) | 64 (0.07) | <0.001 | |
| Lumbar puncture | 33 (0.03) | 133 (0.14) | <0.001 | |
| Incision and drainage | 12 (0.01) | 86 (0.09) | <0.001 | |
| Reduction | 157 (0.16) | 144 (0.15) | 0.523 | |
| Splint | 269 (0.28) | 189 (0.20) | 0.003 | |
| Ultrasound | Overall | 3814 (3.94) | 5487 (5.7) | <0.001 |
| Ultrasound performed in emergency department (ED) | 1257 (1.30) | 3339 (3.47) | <0.001 | |
| Focused abdominal sonography for trauma (FAST) in the ED | 902 (0.93) | 1731 (1.80) | <0.001 | |
| Non-FAST in the ED | 355 (0.37) | 1608 (1.67) | <0.001 | |
| Ultrasound performed in the radiology or cardiology department | 2557 (2.64) | 2148 (2.23) | <0.001 | |
| Pre-EPZ Median (IQR) (min) | Post-EPZ Median (IQR) (min) | p Value | |
|---|---|---|---|
| The LOS-ED for all patients | 110 (53–127) | 102 (33–208) | <0.001 |
| The LOS-ED for patients who underwent procedures | |||
| Suture | 72 (43–141) | 105 (64–186) | <0.001 |
| CVC | 1154 (308–1658) | 1198 (476–2076) | 0.687 |
| Chest tube or pigtail placement | 1425 (236–2684) | 288 (213–479) | 0.083 |
| Thoracentesis | 379 (224.3–1103.5) | 481 (285.3–1275.8) | 0.018 |
| Abdominocentesis | 229 (136–384) | 265 (149–410) | 0.276 |
| Arthrocentesis | 258 (151–662) | 241 (154–581) | 0.672 |
| Lumbar puncture | 1222 (469.3–1636.8) | 1271 (720.8–2270.5) | 0.304 |
| I&D | 333.5 (181–2332.5) | 109 (54–227) | 0.002 |
| Reduction | 107 (62.8–183.3) | 150 (80.0–220.0) | 0.007 |
| Splint | 156 (111.8–231.3) | 189 (119.0–272.5) | 0.007 |
| The LOS-ED for patients who underwent ultrasound scans | |||
| Overall | 365 (166–926) | 270 (143–551) | <0.001 |
| Ultrasound performed in the emergency department (ED) | 124 (68–280) | 180 (109–305) | <0.001 |
| Focused abdominal sonography for trauma (FAST) in the ED | 112 (63–238) | 158 (93–277.8) | <0.001 |
| Non-FAST in the ED | 166 (86–335) | 204 (129–339) | <0.001 |
| Ultrasound performed in the radiology or cardiology department | 562 (297–1203) | 535 (309–1254) | 0.470 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Lin, I.-C.; Chiu, P.-W.; Lin, C.-H. Impact of the Emergency Procedure Zone on Emergency Care. Medicina 2023, 59, 901. https://doi.org/10.3390/medicina59050901
Lin I-C, Chiu P-W, Lin C-H. Impact of the Emergency Procedure Zone on Emergency Care. Medicina. 2023; 59(5):901. https://doi.org/10.3390/medicina59050901
Chicago/Turabian StyleLin, I-Chen, Po-Wei Chiu, and Chih-Hao Lin. 2023. "Impact of the Emergency Procedure Zone on Emergency Care" Medicina 59, no. 5: 901. https://doi.org/10.3390/medicina59050901
APA StyleLin, I.-C., Chiu, P.-W., & Lin, C.-H. (2023). Impact of the Emergency Procedure Zone on Emergency Care. Medicina, 59(5), 901. https://doi.org/10.3390/medicina59050901







