Clinical Outcomes of Enamel Matrix Derivate Used in Surgical and Non-Surgical Treatment of Peri-Implantitis: A Systematic Review of Clinical Studies
Abstract
1. Introduction
2. Materials and Methods
2.1. Eligibility Criteria
- -
- Participants: patient diagnosed with peri-implantitis or peri-implant mucositis;
- -
- Interventions: surgical treatment of peri-implantitis or peri-implant mucositis using enamel matrix derivate;
- -
- Comparison: non-surgical treatment of peri-implantitis or peri-implant mucositis using enamel matrix derivate;
- -
- Outcome: changes in periodontal parameters recorded: probing depth (PD), clinical attachment loss (CAL), bleeding on probing (BOP), and radiographic bone level (RBL);
- -
- Study design: clinical trials; prospective, retrospective studies; cohort studies, case-control studies; and case series.
2.2. Search Process
2.3. Data Extraction
2.4. Risk of Bias Assessment
2.5. Statistical Analysis
3. Results
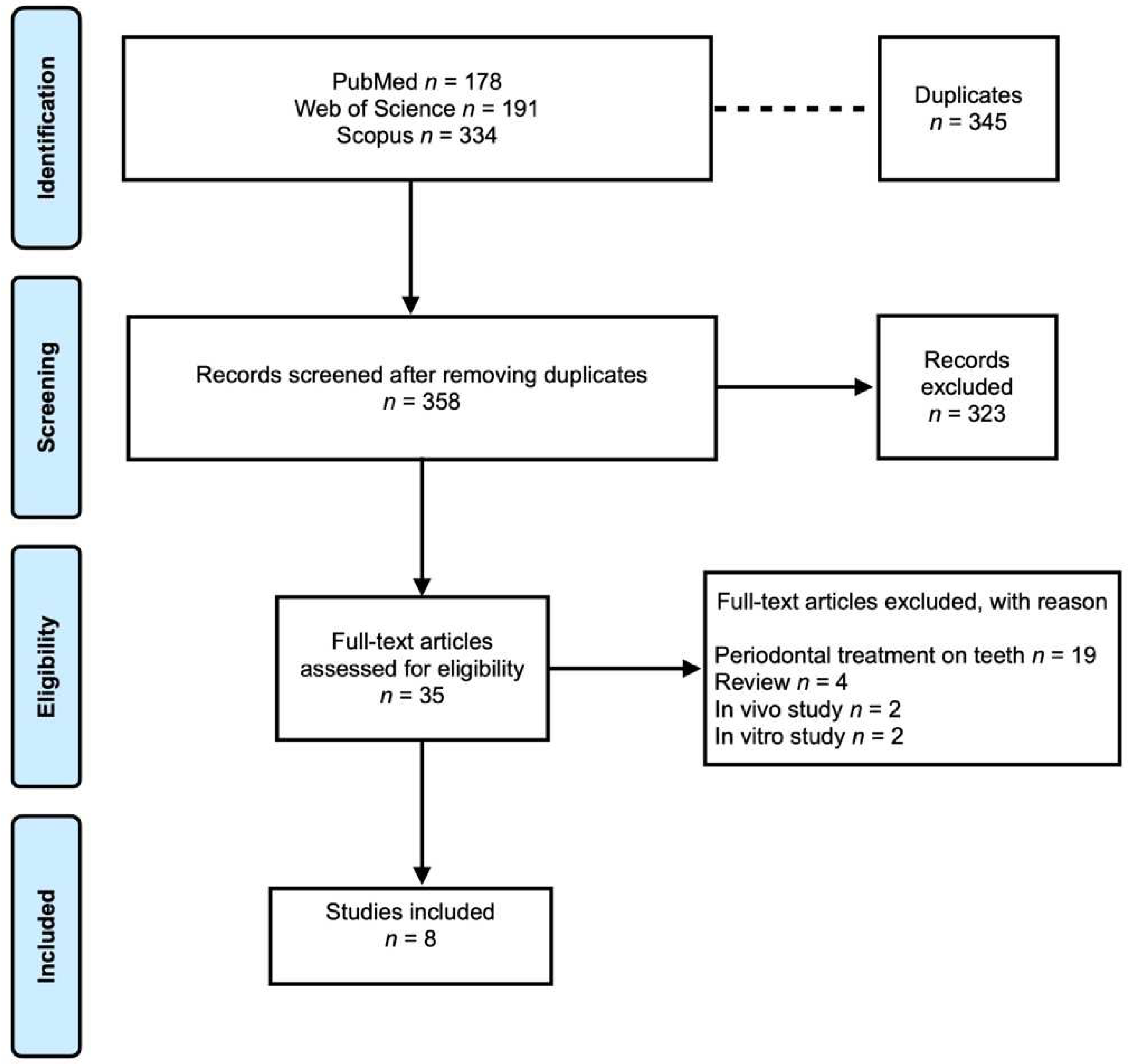
3.1. Study Selection
3.2. Study Characteristics
3.2.1. Description of the Included Studies
3.2.2. Characteristics of Studies Included
Non-Surgical Treatment
Surgical Treatment
| Author. Year. Country | Study Type | Participant’s Characteristics | Type of Intervention | Periodontal Parameters | Follow-up | Outcomes |
|---|---|---|---|---|---|---|
| Non-surgical treatment | ||||||
| Faramarzi. 2015. Iran [19] | Double-blind, three arm parallel RCT | MSM: n = 23 EMD: n = 20 Control: n = 21 Diagnosis: peri-implant mucositis (n = NA) | Mechanical debridement + MSM Mechanical debridement + EMD Mechanical debridement alone | PD BOP | 2 weeks 3 months | PD reduction BOP reduction |
| Kashefimehr. 2017. Iran [20] | Double-blind RCT | Test: n = 20 Control: n = 21 Diagnosis: peri-implant mucositis (n = NA) | Test: mechanical debridement + EMD Control: mechanical debridement alone | PD BOP | 3 months | PD reduction BOP reduction |
| Surgical treatment | ||||||
| Froum. 2012. USA [24] | Prospective cohort | n = 38 Diagnosis: peri-implantitis (n = 51) | OFD with surface decontamination + EMD + PDGF + an organic bovine/mineralized freeze-dried bone + SCTG/collagen matrix | PD BOP RBL | 3 to 7.5 years | PD reduction BOP reduction Bone-level gain |
| Froum. 2015. USA [23] | Prospective cohort | n = 100 Diagnosis: peri-implantitis (n = 170) | OFD with surface decontamination + EMD + PDGF + an organic bovine/mineralized freeze-dried bone + SCTG/collagen matrix | PD BOP RBL | 2 to 10 years | PD reduction BOP reduction Bone level gain |
| Isehed. 2016. Sweden [22] | Double-blind RCT | Test: n = 15 Control: n = 14 Diagnosis: peri-implantitis (n = 29) | Test: OFD + EMD Control: OFD alone | PD BOP RBL | 3, 6, 12 months | PD reduction BOP reduction Bone level gain |
| Isehed. 2018. Sweden [21] | RCT | Test: n = 13 Control: n = 12 Diagnosis: peri-implantitis (n = 25) | Test: OFD + EMD Control: OFD alone | BOP RBL | 1 year 3 years 5 years | BOP reduction Bone level gain |
| Mercado. 2018. Australia [25] | Prospective cohort | n = 30 Diagnosis: peri-implantitis (n = 30) | OFD + EMD + deproteinized bovine bone mineral with 10% collagen + doxycycline +/− CTG | PD BOP RBL | 1, 2, 3 years | PD reduction BOP reduction Bone level reduction |
| Pilenza. 2022. Switzerland [26] | Retrospective case series | n = 11 Diagnosis: peri-implantitis (n = 20) | OFD + EMD + hydroxyapatite + collagen membrane | PPD BOP RBL | 1 year | PPD reduction |
3.3. Risk of Bias Assessment
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Monje, A.; Amerio, E.; Cha, J.K.; Kotsakis, G.; Pons, R.; Renvert, S.; Sanz-Martin, I.; Schwarz, F.; Sculean, A.; Stavropoulos, A.; et al. Strategies for implant surface decontamination in peri-implantitis therapy. Int. J. Oral Implantol. 2022, 15, 213–248. [Google Scholar]
- Figuero, E.; Graziani, F.; Sanz, I.; Herrera, D.; Sanz, M. Management of peri-implant mucositis and peri-implantitis. Periodontol. 2000 2014, 66, 255–273. [Google Scholar] [CrossRef]
- Algraffee, H.; Borumandi, F.; Cascarini, L. Peri-implantitis. Br. J. Oral Maxillofac. Surg. 2012, 50, 689–694. [Google Scholar] [CrossRef]
- John, V.; Shin, D.; Marlow, A.; Hamada, Y. Peri-Implant Bone Loss and Peri-Implantitis: A Report of Three Cases and Review of the Literature. Case Rep. Dent. 2016, 2016, 2491714. [Google Scholar] [CrossRef] [PubMed]
- Mancini, L.; Romandini, M.; Fratini, A.; Americo, L.M.; Panda, S.; Marchetti, E. Biomaterials for Periodontal and Peri-Implant Regeneration. Materials 2021, 14, 3319. [Google Scholar] [CrossRef] [PubMed]
- Barootchi, S.; Wang, H.-L. Peri-implant diseases: Current understanding and management. Int. J. Oral Implantol. 2021, 14, 263–282. [Google Scholar]
- Salvi, G.E.; Roccuzzo, A.; De Ry, S.P.; Roccuzzo, M. Non-Surgical Management of Peri-implant Diseases. Forum Implantol. 2021, 17, 57–69. [Google Scholar]
- Schwarz, F.; Derks, J.; Monje, A.; Wang, H.-L. Peri-implantitis. J. Periodontol. 2018, 89 (Suppl. S1), S267–S290. [Google Scholar] [CrossRef]
- Maney, P.; Schiavo, J.H.; Mascarenhas, F.; Dragonas, P. Risk Factors for Peri-implantitis. Curr. Oral Health Rep. 2020, 7, 234–248. [Google Scholar] [CrossRef]
- Geisinger, M.L.; Calvert Grosso, K.; Kaur, M.; Abou-Arraj, R.V.; Basma, H.; Ogdon, D.; Geurs, N.C. Clinical Decision Making for Primary Peri-Implantitis Prevention: Practical Applications. Clin. Adv. Periodontics 2021, 11, 43–53. [Google Scholar] [CrossRef]
- Ramanauskaite, A.; Obreja, K.; Schwarz, F. Surgical Management of Peri-implantitis. Curr. Oral Health Rep. 2020, 7, 283–303. [Google Scholar] [CrossRef]
- Park, J.-B. Clinical Application of Enamel Matrix Derivative for Periodontal Regeneration and Treatment of Peri-Implantitis. In Periodontology and Dental Implantology; Manakil, J., Ed.; IntechOpen: Rijeka, Croatia, 2018. [Google Scholar]
- Alberti, A.; Francetti, L.; Taschieri, S.; Corbella, S. The Applications of Enamel Matrix Derivative in Implant Dentistry: A Narrative Review. Materials 2021, 14, 3045. [Google Scholar] [CrossRef]
- Ortiz-vigón, A.; Regidor, E. Innovations in the Surgical Reconstructive Treatment of Peri-Implant- Innovations in the Surgical Reconstructive Treatment of Peri-Implant- Related Intrabony Defects. Available online: https://blog.iti.org/clinical-insights/peri-implant-related-intrabony-defects/ (accessed on 5 July 2022).
- Higgins, J.P.T.; Green, S. Guide to the Contents of a Cochrane Protocol and Review. In Cochrane Handbook for Systematic Reviews of Interventions; John Wiley & Sons, Ltd.: Hoboken, NJ, USA, 2008; pp. 51–79. ISBN 9780470712184. [Google Scholar]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Med. 2009, 6, e1000097. [Google Scholar] [CrossRef] [PubMed]
- Higgins, J.P.T.; Altman, D.G.; Gotzsche, P.C.; Juni, P.; Moher, D.; Oxman, A.D.; Savovic, J.; Schulz, K.F.; Weeks, L.; Sterne, J.A.C. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 2011, 343, d5928. [Google Scholar] [CrossRef] [PubMed]
- Sterne, J.A.; Hernán, M.A.; Reeves, B.C.; Savović, J.; Berkman, N.D.; Viswanathan, M.; Henry, D.; Altman, D.G.; Ansari, M.T.; Boutron, I.; et al. ROBINS-I: A tool for assessing risk of bias in non-randomised studies of interventions. BMJ 2016, 355, i4919. [Google Scholar] [CrossRef] [PubMed]
- Faramarzi, M.; Goharfar, Z.; Pourabbas, R.; Kashefimehr, A.; Shirmohmmadi, A. Microbiological and clinical effects of enamel matrix derivative and sustained-release micro-spherical minocycline application as an adjunct to non-surgical therapy in peri-implant mucosal inflammation. J. Korean Assoc. Oral Maxillofac. Surg. 2015, 41, 181–189. [Google Scholar] [CrossRef]
- Kashefimehr, A.; Pourabbas, R.; Faramarzi, M.; Zarandi, A.; Moradi, A.; Tenenbaum, H.C.; Azarpazhooh, A. Effects of enamel matrix derivative on non-surgical management of peri-implant mucositis: A double-blind randomized clinical trial. Clin. Oral Investig. 2017, 21, 2379–2388. [Google Scholar] [CrossRef]
- Isehed, C.; Svenson, B.; Lundberg, P.; Holmlund, A. Surgical treatment of peri-implantitis using enamel matrix derivative, an RCT: 3- and 5-year follow-up. J. Clin. Periodontol. 2018, 45, 744–753. [Google Scholar] [CrossRef]
- Isehed, C.; Holmlund, A.; Renvert, S.; Svenson, B.; Johansson, I.; Lundberg, P. Effectiveness of enamel matrix derivative on the clinical and microbiological outcomes following surgical regenerative treatment of peri-implantitis. A randomized controlled trial. J. Clin. Periodontol. 2016, 43, 863–873. [Google Scholar] [CrossRef]
- Froum, S.J.; Froum, S.H.; Rosen, P.S. A Regenerative Approach to the Successful Treatment of Peri-implantitis: A Consecutive Series of 170 Implants in 100 Patients with 2- to 10-Year Follow-up. Int. J. Periodontics Restor. Dent. 2015, 35, 857–863. [Google Scholar] [CrossRef]
- Froum, S.J.; Froum, S.H.; Rosen, P.S. Successful management of peri-implantitis with a regenerative approach: A consecutive series of 51 treated implants with 3- to 7.5-year follow-up. Int. J. Periodontics Restor. Dent. 2012, 32, 11–20. [Google Scholar]
- Mercado, F.; Hamlet, S.; Ivanovski, S. Regenerative surgical therapy for peri-implantitis using deproteinized bovine bone mineral with 10% collagen, enamel matrix derivative and Doxycycline-A prospective 3-year cohort study. Clin. Oral Implant. Res. 2018, 29, 583–591. [Google Scholar] [CrossRef] [PubMed]
- Pilenza, D.; Filippi, A.; Walter, C.; Zitzmann, N.U.; Bornstein, M.M.; Kühl, S. Surgical therapy of peri-implantitis with adjunctive hydroxyapatite and enamel matrix derivative: A 1-year retrospective case series. Swiss Dent. J. 2022, 132, 238–246. [Google Scholar] [PubMed]
- Berglundh, T.; Armitage, G.; Araujo, M.G.; Avila-Ortiz, G.; Blanco, J.; Camargo, P.M.; Chen, S.; Cochran, D.; Derks, J.; Figuero, E.; et al. Peri-implant diseases and conditions: Consensus report of workgroup 4 of the 2017 World Workshop on the Classification of Periodontal and Peri-Implant Diseases and Conditions. J. Clin. Periodontol. 2018, 45 (Suppl. S2), S286–S291. [Google Scholar] [CrossRef] [PubMed]
- Bompard, X. Enamel Matrix Derivative in the Treatment of Peri-Implant Diseases—A Systematic Review. Available online: https://bdigital.ufp.pt/handle/10284/9386 (accessed on 5 July 2022).
- Ramanauskaite, A.; Fretwurst, T.; Schwarz, F. Efficacy of alternative or adjunctive measures to conventional non-surgical and surgical treatment of peri-implant mucositis and peri-implantitis: A systematic review and meta-analysis. Int. J. Implant Dent. 2021, 7, 112. [Google Scholar] [CrossRef]
- Hu, M.-L.; Zheng, G.; Lin, H.; Li, N.; Zhao, P.-F.; Han, J.-M. Network meta-analysis of the treatment efficacy of different lasers for peri-implantitis. Lasers Med. Sci. 2021, 36, 619–629. [Google Scholar] [CrossRef]
- Zhao, R.; Liu, S.; Liu, Y.; Cui, S. Adjunctive Use of Active Compounds such as Chlorhexidine in the Nonsurgical Treatment of Peri-Implant Mucositis for Oral Health: A Systematic Review and Meta-Analysis. Oxid. Med. Cell. Longev. 2022, 2022, 2312784. [Google Scholar] [CrossRef]
- Toledano-Osorio, M.; Vallecillo, C.; Toledano, R.; Aguilera, F.S.; Osorio, M.T.; Muñoz-Soto, E.; García-Godoy, F.; Vallecillo-Rivas, M. A Systematic Review and Meta-Analysis of Systemic Antibiotic Therapy in the Treatment of Peri-Implantitis. Int. J. Environ. Res. Public Health 2022, 19, 6502. [Google Scholar] [CrossRef]
- Tomasi, C.; Regidor, E.; Ortiz-Vigón, A.; Derks, J. Efficacy of reconstructive surgical therapy at peri-implantitis-related bone defects. A systematic review and meta-analysis. J. Clin. Periodontol. 2019, 46 (Suppl. S2), 340–356. [Google Scholar] [CrossRef]
| Author | Adequate Sequence Generation | Allocation Concealment | Blinding of Participants and Personnel | Blinding of Outcome Assessment | Incomplete Outcome Data Addressed | Selective Outcome Reporting | Other Bias | Estimated Potential ROB |
|---|---|---|---|---|---|---|---|---|
| Faramarzi [19] | Low | Unclear | Low | Low | Unclear | Low | Low | Unclear |
| Kashefimehr [20] | Unclear | High | High | Unclear | Unclear | Low | Low | High |
| Isehed [21] | High | Low | Low | Low | Low | Low | Low | High |
| Isehed [22] | High | Low | Low | Low | Low | Low | Low | High |
| Author | Confounding | Selection of Participants | Classification of Interventions | Deviations from Intended Interventions | Missing Data | Measurements of Outcome | Selection of the Reported Result | Estimated Potential ROB |
|---|---|---|---|---|---|---|---|---|
| Froum [21] | Moderate | Critical | Moderate | Low | Low | Low | Moderate | Critical |
| Froum [22] | Moderate | Moderate | Moderate | Low | Low | Low | Moderate | Moderate |
| Mercado [25] | Low | Low | Low | Low | Low | Low | Low | Low |
| Pilenza [26] | Low | Low | Low | Low | Low | Low | Low | Low |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Moldovan, R.; Mester, A.; Piciu, A.; Bran, S.; Onisor, F. Clinical Outcomes of Enamel Matrix Derivate Used in Surgical and Non-Surgical Treatment of Peri-Implantitis: A Systematic Review of Clinical Studies. Medicina 2022, 58, 1819. https://doi.org/10.3390/medicina58121819
Moldovan R, Mester A, Piciu A, Bran S, Onisor F. Clinical Outcomes of Enamel Matrix Derivate Used in Surgical and Non-Surgical Treatment of Peri-Implantitis: A Systematic Review of Clinical Studies. Medicina. 2022; 58(12):1819. https://doi.org/10.3390/medicina58121819
Chicago/Turabian StyleMoldovan, Raluca, Alexandru Mester, Andra Piciu, Simion Bran, and Florin Onisor. 2022. "Clinical Outcomes of Enamel Matrix Derivate Used in Surgical and Non-Surgical Treatment of Peri-Implantitis: A Systematic Review of Clinical Studies" Medicina 58, no. 12: 1819. https://doi.org/10.3390/medicina58121819
APA StyleMoldovan, R., Mester, A., Piciu, A., Bran, S., & Onisor, F. (2022). Clinical Outcomes of Enamel Matrix Derivate Used in Surgical and Non-Surgical Treatment of Peri-Implantitis: A Systematic Review of Clinical Studies. Medicina, 58(12), 1819. https://doi.org/10.3390/medicina58121819






