Is There a Relationship between Voice Quality and Obstructive Sleep Apnea Severity and Cumulative Percentage of Time Spent at Saturations below Ninety Percent: Voice Analysis in Obstructive Sleep Apnea Patients
Abstract
1. Introduction
2. Materials and Methods
2.1. Voice Analysis
2.2. Statistical Method
3. Results
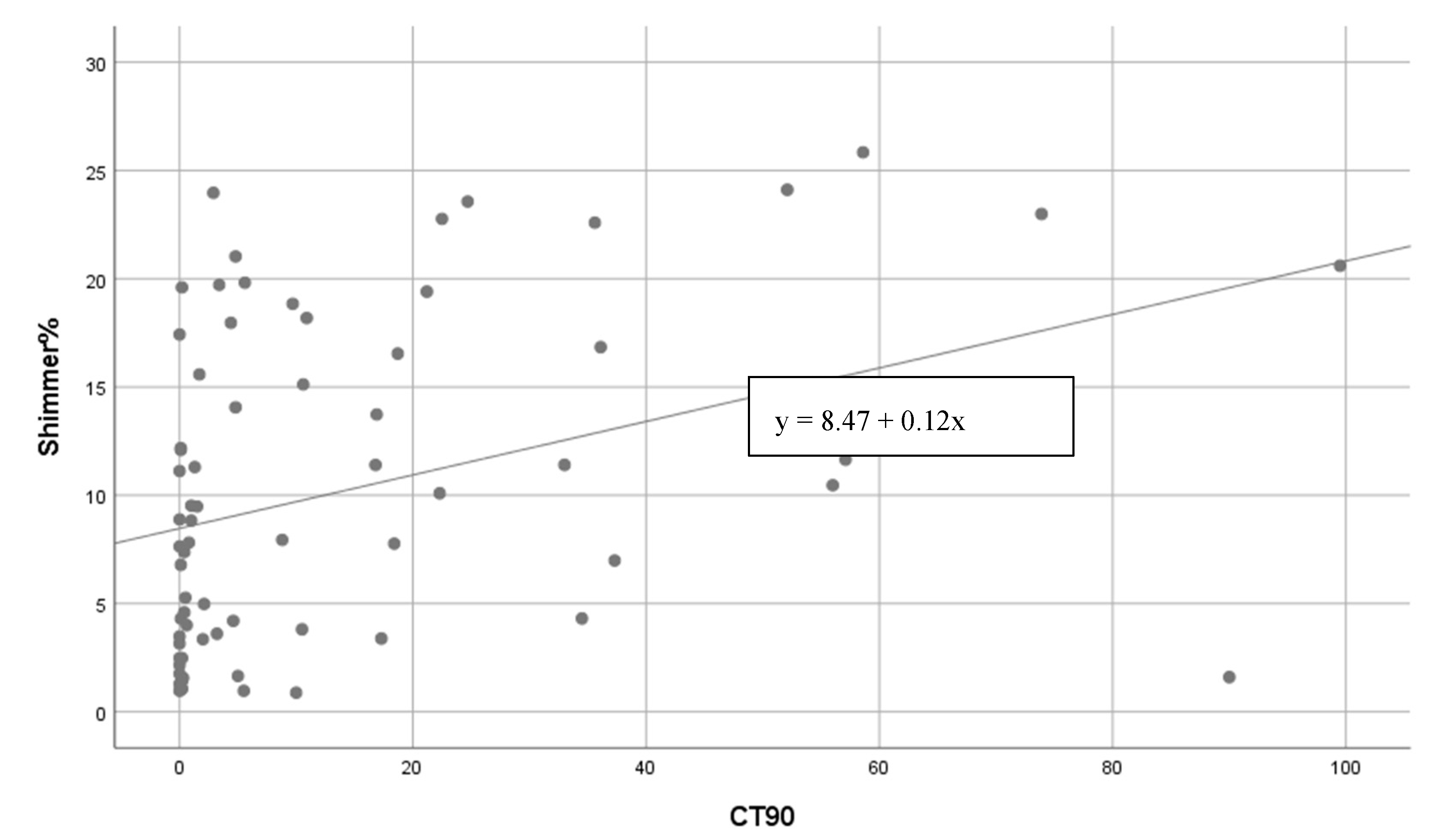
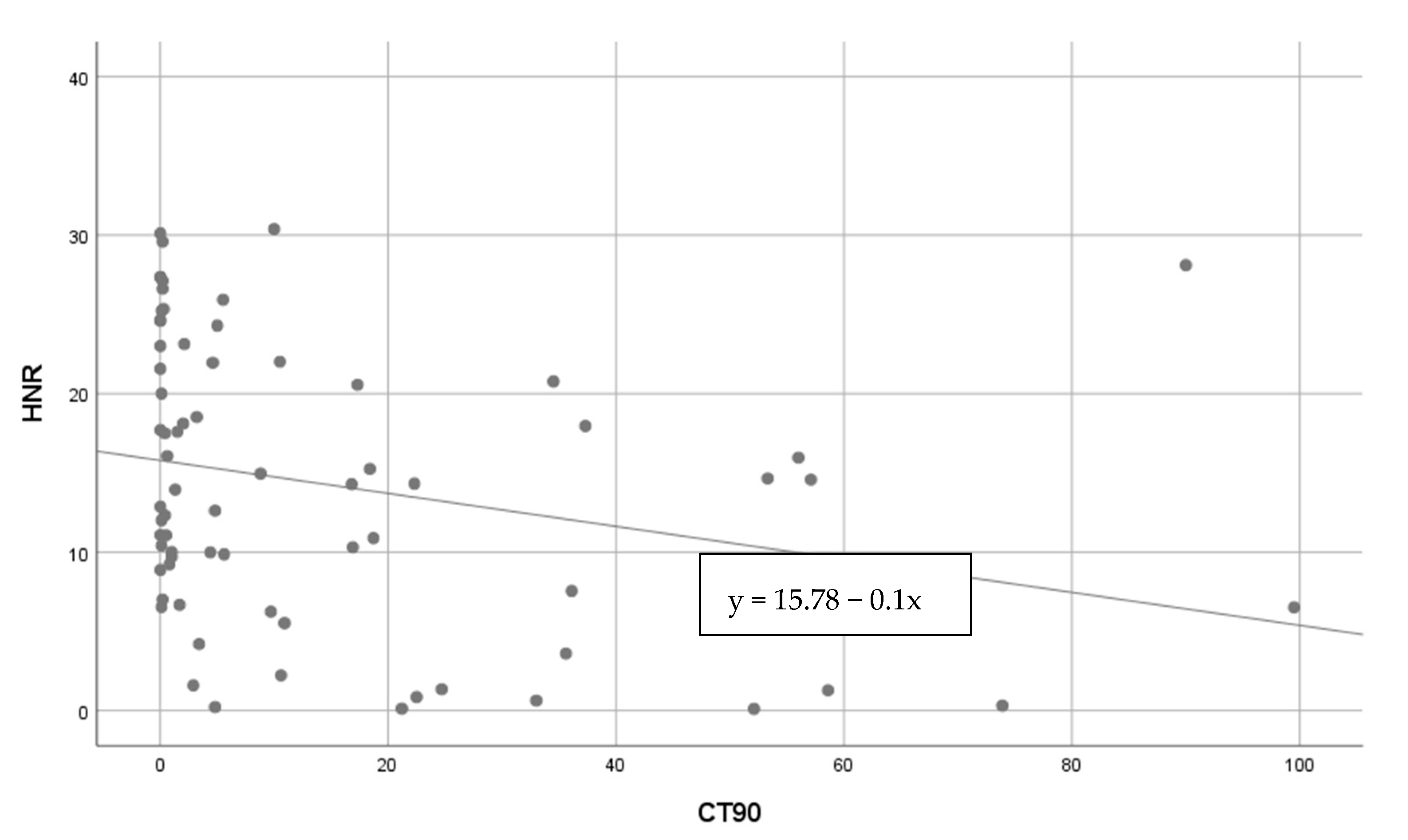
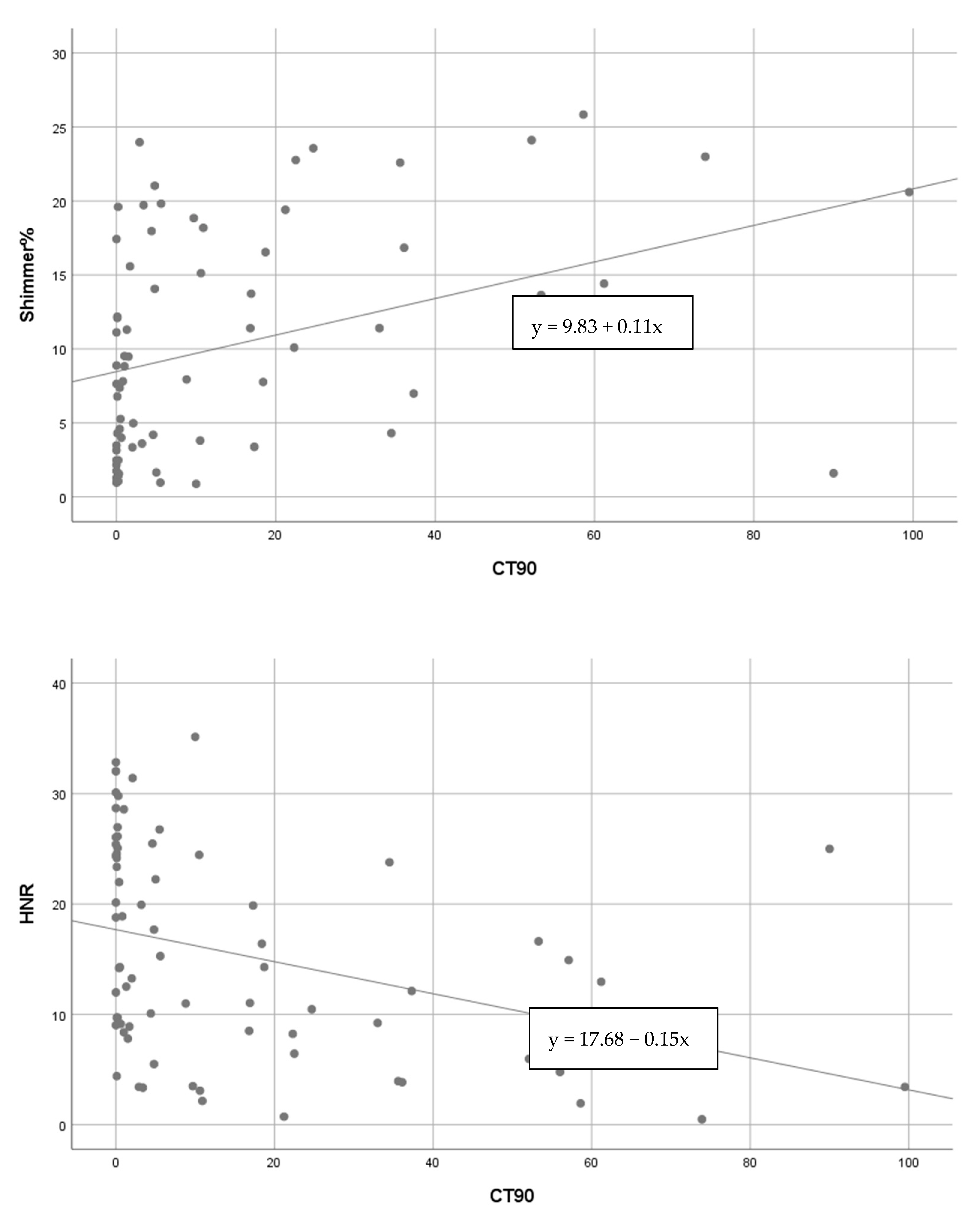
3.1. Voice Analysis
Aerodynamic Voice Analysis
3.2. Acoustic Voice Analysis
3.2.1. Vowel Sound /α:/
3.2.2. Vowel Sound /i:/
3.3. VHI-10 Questionnaire for Subjective Voice Analysis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Olson, L.G.; King, M.T.; Hensley, M.J.; Saunders, N.A. A community study of snoring and sleep-disordered breathing prevalence. Am. J. Respir. Crit. Care Med. 1995, 152, 711–716. [Google Scholar] [CrossRef] [PubMed]
- Young, T.; Skatrud, J.; Peppard, P.E. Risk factors for obstructive sleep apnea in adults. JAMA 2004, 291, 2013–2016. [Google Scholar] [CrossRef] [PubMed]
- Colten, H.R.; Altevogt, B.M. Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem; National Academies Press: Washington, DC, USA, 2006; pp. 65–66. [Google Scholar] [CrossRef]
- Edwards, B.A.; Eckert, D.J.; McSharry, D.G.; Sands, S.A.; Desai, A.; Kehlmann, G.; Bakker, J.P.; Genta, P.R.; Owens, R.L.; White, D.P.; et al. Clinical predictors of the respiratory arousal threshold in patients with obstructive sleep apnea. Am. J. Respir. Crit. Care Med. 2014, 190, 1293–1300. [Google Scholar] [CrossRef] [PubMed]
- Antonaglia, C.; Passuti, G.; Giudici, F.; Salton, F.; Ruaro, B.; Radovanovic, D.; Confalonieri, M. Low arousal threshold: A common pathophysiological trait in patients with obstructive sleep apnea syndrome and asthma. Sleep Breath 2022. [Google Scholar] [CrossRef] [PubMed]
- Yamaguchi, Y.; Shiota, S.; Kusunoki, Y.; Hamaya, H.; Ishii, M.; Kodama, Y.; Akishita, M.; Kida, K.; Takahashi, K.; Nagase, T.; et al. Polysomnographic features of low arousal threshold in overlap syndrome involving obstructive sleep apnea and chronic obstructive pulmonary disease. Sleep Breath 2019, 23, 1095–1100. [Google Scholar] [CrossRef]
- Chaudhary, B.; Dasti, S.; Park, Y.; Brown, T.; Davis, H.; Akhtar, B. Hour-to-hour variability of oxygen saturation in sleep apnea. Chest 1998, 113, 719–722. [Google Scholar] [CrossRef]
- Hoshino, T.; Sasanabe, R.; Murotani, K.; Arimoto, M.; Inagawa, S.; Tanigawa, T.; Uchida, Y.; Ogawa, T.; Ueda, H.; Shiomi, T. Polysomnographic parameters during non-rapid eye movement sleep predict continuous positive airway pressure adherence. Nagoya J. Med. Sci. 2016, 78, 195–203. [Google Scholar]
- Sabato, R.; Guido, P.; Salerno, F.G.; Resta, O.; Spanevello, A.; Barbaro, M.P. Airway inflammation in patients affected by obstructive sleep apnea. Monaldi. Arch. Chest Dis. 2006, 65, 102–105. [Google Scholar] [CrossRef]
- Remmers, J.E.; de Groot, W.J.; Sauerland, E.K.; Anch, A.M. Pathogenesis of upper airway occlusion during sleep. J. Appl. Physiol. 1978, 44, 931–938. [Google Scholar] [CrossRef]
- Robb, M.P.; Yates, J.; Morgan, E.J. Vocal tract resonance characteristics of adults with obstructive sleep apnea. Acta Otolaryngol. 1997, 117, 760–763. [Google Scholar] [CrossRef]
- Behrman, A.; Shikowitz, M.J.; Dailey, S. The effect of upper airway surgery on voice. Otolaryngol. Head Neck Surg. 2002, 127, 36–42. [Google Scholar] [CrossRef] [PubMed]
- Lan, Z.; Itoi, A.; Takashima, M.; Oda, M.; Tomoda, K. Difference of pharyngeal morphology and mechanical property between OSAHS patients and normal subjects. Auris Nasus Larynx 2006, 33, 433–439. [Google Scholar] [CrossRef] [PubMed]
- Han, D.; Xu, W.; Hu, R.; Zhang, L. Voice function following Han’s uvulopalatopharyngoplasty. J. Laryngol. Otol. 2012, 126, 47–51. [Google Scholar] [CrossRef]
- Sarıca, S.; Bilal, N.; Sağıroğlu, S.; Oğuzhan, O.; Altınışık, M.; Kılıç, M.A. Comparing Voice Frequency and Perturbation Parameters Using Different Analysis Programs. ENT-HNS J. 2017, 25, 13–20. [Google Scholar] [CrossRef][Green Version]
- Jacobson, B.H.; Johnson, A.; Grywalski, C.; Silbergleit, A.; Jacobson, G.P.; Benninger, M.S.; Newman, C.W. The Voice Handicap Index (VHI) development and validation. Am. J. Speech. Lang. Pathol. 1997, 6, 66–70. [Google Scholar] [CrossRef]
- Kiliç, M.A.; Okur, E.; Yildirim, I.; Oğüt, F.; Denizoğlu, I.; Kizilay, A.; Oğuz, H.; Kandoğan, T.; Doğan, M.; Akdoğan, O.; et al. Reliability and validity of the Turkish version of the Voice Handicap Index. Kulak. Burun. Bogaz. Ihtis. Derg. 2008, 18, 139–147. [Google Scholar] [PubMed]
- Berry, R.B.; Quan, S.F.; Abreu, A.R.; Bibbs, M.L.; DelRosso, L.; Harding, S.M.; Mao, M.M.; Plante, D.T.; Presman, M.R.; Troester, M.M.; et al. The AASM Manual for the Scoring of Sleep and Associated Events: Rules, Terminology and Technical Specifications, Version 2.6; American Academy of Sleep Medicine: Darien, IL, USA, 2020; Available online: http://www.aasmnet.org/scoringmanual/ (accessed on 13 January 2020).
- Deyoung, P.N.; Bakker, J.P.; Sands, S.; Batool-Anwar, S.; Connolly, J.G.; Butler, J.P.; Malhotra, A. Acoustic pharyngometry measurement of minimal cross-sectional airway area is a significant independent predictor of moderate-to-severe obstructive sleep apnea. J. Clin. Sleep Med. 2013, 9, 1161–1164. [Google Scholar] [CrossRef]
- Espinoza-Cuadros, F.; Fernández-Pozo, R.; Toledano, D.T.; Alcázar-Ramírez, J.D.; López-Gonzalo, E.; Hernández-Gómez, L.A. Speech signal and facial ımage processing for obstructive sleep apnea assessment. Comput. Math. Methods Med. 2015, 2015, 489761. [Google Scholar] [CrossRef]
- Karakurt, S.E.; Karakuş, M.F.; Eravcı, F.C.; Kum, N.; Özcan, M.; Özcan, K.M. Evaluation of the Relationship Between the Required Pressure Level in Continuous Positive Airway Pressure Treatment and Voice in Patients With Obstructive Sleep Apnea Syndrome. J. Voice 2021, 35, 609–613. [Google Scholar] [CrossRef]
- Verdolini, K.M.; Titze, I.R.; Druker, D.G. Changes in phonation threshold pressure with induced conditions of hydration. J. Voice 1990, 4, 142–151. [Google Scholar] [CrossRef]
- Finkelhor, B.K.; Titze, I.R.; Durham, P.L. The effects of viscosity changes in the vocal folds on the range of oscillation. J. Voice 1988, 1, 320–335. [Google Scholar] [CrossRef]
- Tao, C.; Jiang, J.J.; Zhang, Y. A fluid-saturated poroelastic model of the vocal folds with hydrated tissue. J. Biomech 2009, 42, 774–780. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Jiang, J.; Verdolini, K.; Aquino, B.; Ng, J.; Hanson, D. Effects of dehydration on phonation in excised canine larynges. Ann. Otol. Rhinol. Laryngol. 2000, 109, 568–575. [Google Scholar] [CrossRef] [PubMed]
- Hamdan, A.L.; Al-Barazi, R.; Kanaan, A.; Al-Tamimi, W.; Sinno, S.; Husari, A. The effect of snoring on voice: A controlled study of 30 subjects. Ear. Nose Throat. J. 2012, 91, 28–33. [Google Scholar] [CrossRef] [PubMed]
- Bertino, G.; Matti, E.; Migliazzi, S.; Pagella, F.; Tinelli, C.; Benazzo, M. Acoustic changes in voice after surgery for snoring: Preliminary results. Acta. Otorhinolaryngol. Ital. 2006, 26, 110–114. [Google Scholar] [PubMed]
- Rubinstein, I.; Slutsky, A.S.; Zamel, N.; Hoffstein, V. Paradoxical glottic narrowing in patients with severe obstructive sleep apnea. J. Clin. Inv. 1988, 81, 1051–10555. [Google Scholar] [CrossRef] [PubMed]
- Titze, I.R. On the relation between subglottal pressure and fundamental frequency in phonation. J. Acoust. Soc. Am. 1989, 85, 901–906. [Google Scholar] [CrossRef]
- Fiz, J.A.; Morera, J.; Abad, J.; Belsunces, A.; Haro, M.; Jane, R.; Caminal, P.; Rodenstein, D. Acoustic analysis of vowel emission in obstructive sleep apnea. Chest 1993, 104, 1093–1096. [Google Scholar] [CrossRef]
- Atan, D.; Ozcan, K.M.; Ikincioğulları, A.; Köseoğlu, S.; Çetin, M.A.; Ensari, S.; Dere, H. The effect of obstructive sleep apnea syndrome and continuous positive airway pressure treatment on voice performance. Sleep Breath. 2015, 19, 777–782. [Google Scholar] [CrossRef]
- Wei, M.; Du, J.; Wang, X.; Lu, H.; Wang, W.; Lin, P. Voice disorders in severe obstructive sleep apnea patients and comparison of two acoustic analysis software programs: MDVP and Praat. Sleep Breath. 2021, 25, 433–439. [Google Scholar] [CrossRef]
- Desjardins, M.; Halstead, L.; Cooke, M.; Bonilha, H.S. A systematic review of voice therapy: What “effectiveness” really ımplies. J. Voice 2017, 31, 392. [Google Scholar] [CrossRef] [PubMed]
- Chhetri, S.S.; Gautam, R. Acoustic analysis before and after voice therapy for laryngeal pathology. Kathmandu Univ. Med. J. 2015, 13, 323–327. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Awan, S.N.; Frenkel, M.L. Improvements in estimating the harmonics- to-noise ratio of the voice. J. Voice 1994, 8, 255–262. [Google Scholar] [CrossRef]
- Hillenbrand, J. A methodological study of perturbed and additive noise in synthetically generated voice signals. J. Speech Hear. Res. 1987, 30, 448–461. [Google Scholar] [CrossRef] [PubMed]
- de Krom, G. A cepstrum-based technique for determining a harmonics-to-noise ratio in speech signals. J. Speech Hear. Res. 1993, 36, 254–266. [Google Scholar] [CrossRef] [PubMed]
- Martin, D.; Fitch, J.; Wolfe, V. Pathologic voice type and the acoustic predictions of severity. J. Speech Hear. Res. 1995, 38, 765–771. [Google Scholar] [CrossRef]
- Eskenazi, L.; Childers, D.G.; Hicks, D.M. Acoustic correlates of vocal quality. J. Speech Hear. Res. 1990, 33, 298–306. [Google Scholar] [CrossRef]
- de Krom, G. Some spectral correlates of pathological breathy and rough voice quality for different types of vowel fragments. J. Speech Hear. Res. 1995, 38, 794–811. [Google Scholar] [CrossRef]
- Ferrand, C.T. Harmonics-to-noise ratio: An index of vocal aging. J. Voice 2002, 16, 480–487. [Google Scholar] [CrossRef]
- Mahato, N.B.; Regmi, D.; Bista, M.; Sherpa, P. Acoustic Analysis of Voice in School Teachers. JNMA J. Nepal. Med. Assoc. 2018, 56, 658–661. [Google Scholar] [CrossRef]
- Benavides, A.M.; Pozo, R.F.; Toledano, D.T.; Murilloa, J.L.B.; Gonzaloa, E.L.; Gomez, L.H. Analysis of voice features related to obstructive sleep apnea and their application in diagnosis support. Comput. Speech Lang. 2014, 28, 434–452. [Google Scholar] [CrossRef]
- Pozo, R.F.; Murillo, J.L.B.; Gomez, L.H.; Gonzalo, E.L.; Ramırez, J.A.; Toledano, D.T. Assessment of severe apnoea through voice analysis, automatic speech, and speaker recognition techniques. Eurasip. J. Adv. Signal. Process. 2009, 2009, 982531. [Google Scholar] [CrossRef]
- Karlsen, T.; Sandvik, L.; Heimdal, J.H.; Aarstad, H.J. Acoustic voice analysis and maximum phonation time in relation to voice handicap ındex score and larynx disease. J. Voice 2020, 34, 161.e27–161.e35. [Google Scholar] [CrossRef] [PubMed]
- Greene, J.S.; Zipfel, T.E.; Harlor, M. The effect of uvulopalatopharyngoplasty on the nasality of voice. J. Voice 2004, 18, 423–430. [Google Scholar] [CrossRef]
- Eun, Y.G.; Shin, S.Y.; Kim, S.W. Effects of uvulopalatopharyngoplasty with or without radiofrequency tongue base reduction on voice in patients with obstructive sleep apnea. Laryngoscope 2013, 123, 1806–1810. [Google Scholar] [CrossRef]
- Gelfer, M.P.; Pazera, J.F. Maximum duration of sustained /s/ and /z/ and the s/z ratio with controlled intensity. J. Voice 2006, 20, 369–379. [Google Scholar] [CrossRef]
- Eckel, F.C.; Boone, D.R. The s/z ratio as an indicator of laryngeal pathology. J. Speech Hear. Disord. 1981, 46, 147–149. [Google Scholar] [CrossRef]
- Hufnagle, J.; Hufnagle, K.K. s/z ratio in dysphonic children with and without vocal cord nodules. Lang. Speech Hear. Serv. Sch. 1988, 19, 418–422. [Google Scholar] [CrossRef]
- Adams, S.G.; Irish, J.C.; Durkin, L.C.; Wong, D.L.; Brown, D.H. Evaluation of vocal function in unilateral vocal fold paralysis following thyroplastic surgery. J. Otolaryngol. 1996, 25, 165–170. [Google Scholar]
- Wheeler, K.M.; Collins, S.P.; Sapienza, C.M. The relationship between VHI scores and specific acoustic measures of mildly disordered voice production. J. Voice 2006, 20, 308–317. [Google Scholar] [CrossRef]
- Hsiung, M.W.; Pai, L.; Wang, H.W. Correlation between voice handicap index and voice laboratory measurements in dysphonic patients. Eur. Arch. Otorhinolaryngol. 2002, 259, 97–99. [Google Scholar] [CrossRef] [PubMed]
- Bostanci, A.; Turhan, M.; Bozkurt, S. Factors influencing sleep time with oxygen saturation below 90% in sleep-disordered breathing. Laryngoscope 2015, 125, 1008–1012. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.B.; Zen, H.Q.; Lin, Q.C.; Chen, G.P.; Chen, L.D.; Chen, H. TST, as a polysomnographic variable, is superior to the apnea hypopnea index for evaluating intermittent hypoxia in severe obstructive sleep apnea. Eur. Arch. Otorhinolaryngol. 2014, 271, 2745–2750. [Google Scholar] [CrossRef] [PubMed]
| Vowel Sound /α:/ | Mean f0 (Hz) | Mean Jitter% | Mean Shimmer% | Mean HNR (dB) | ||||
|---|---|---|---|---|---|---|---|---|
| Min | Max | Min | Max | Min | Max | Min | Max | |
| 1st group | 179 | 0.23 * p ≤ 0.00 | 4.58 * p ≤ 0.00, **** p ≤ 0.032 | 20.66 * p ≤ 0.00 | ||||
| 79 | 308 | 0.09 | 0.44 | 0.97 | 17.43 | 8.87 | 30.11 | |
| 2nd group | 140 | 0.22 ** p ≤ 0.00 | 9.35 ** p ≤ 0.002 | 14.60 ** p ≤ 0.018 | ||||
| 76 | 289 | 0.13 | 0.39 | 1.6 | 20.60 | 6.51 | 28.11 | |
| 3rd group | 156 | 0.86 *** p ≤ 0.002 | 10.28 *** p ≤ 0.007 | 14.60 *** p ≤ 0.018 | ||||
| 76 | 245 | 0.16 | 4.76 | 0.88 | 23.97 | 0.31 | 30.39 | |
| 4th group | 134 | 3.24 | 17.06 | 7.04 | ||||
| 81 | 320 | 0.26 | 9.85 | 10.09 | 25.84 | 0.10 | 15.96 | |
| Vowel Sound /i:/ | Mean f0 (Hz) | Mean Jitter% | Mean Shimmer% | Mean HNR (dB) | ||||
|---|---|---|---|---|---|---|---|---|
| Min | Max | Min | Max | Min | Max | Min | Max | |
| 1 st Group | 4.58 * p ≤ 0.028, *** p ≤ 0.015 | 0.25 * p ≤ 0.04 | 5.08 * p ≤ 0.00, **** p ≤ 0.041 | 22.76 * p ≤ 0.00, *** p ≤ 0.032 | ||||
| 100 | 322 | 0.10 | 0.74 | 0.60 | 21.06 | 8.37 | 32.82 | |
| 2 nd Group | 137 | 0.46 ** p ≤ 0.013 | 11.09 | 15.07 | ||||
| 79 | 296 | 0.18 | 1.70 | 0.79 | 24.54 | 3.42 | 32.03 | |
| 3 rd Group | 161 | 1.18 | 12.10 | 15.61 | ||||
| 79 | 275 | 0.12 | 5.52 | 0.91 | 24.77 | 0.49 | 35.12 | |
| 4 th Group | 131 | 2.08 | 17.55 | 8.59 | ||||
| 86 | 238 | 0.11 | 8.66 | 6.63 | 26.40 | 0.73 | 17.68 | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yaslıkaya, S.; Geçkil, A.A.; Birişik, Z. Is There a Relationship between Voice Quality and Obstructive Sleep Apnea Severity and Cumulative Percentage of Time Spent at Saturations below Ninety Percent: Voice Analysis in Obstructive Sleep Apnea Patients. Medicina 2022, 58, 1336. https://doi.org/10.3390/medicina58101336
Yaslıkaya S, Geçkil AA, Birişik Z. Is There a Relationship between Voice Quality and Obstructive Sleep Apnea Severity and Cumulative Percentage of Time Spent at Saturations below Ninety Percent: Voice Analysis in Obstructive Sleep Apnea Patients. Medicina. 2022; 58(10):1336. https://doi.org/10.3390/medicina58101336
Chicago/Turabian StyleYaslıkaya, Serhat, Ayşegül Altıntop Geçkil, and Zehra Birişik. 2022. "Is There a Relationship between Voice Quality and Obstructive Sleep Apnea Severity and Cumulative Percentage of Time Spent at Saturations below Ninety Percent: Voice Analysis in Obstructive Sleep Apnea Patients" Medicina 58, no. 10: 1336. https://doi.org/10.3390/medicina58101336
APA StyleYaslıkaya, S., Geçkil, A. A., & Birişik, Z. (2022). Is There a Relationship between Voice Quality and Obstructive Sleep Apnea Severity and Cumulative Percentage of Time Spent at Saturations below Ninety Percent: Voice Analysis in Obstructive Sleep Apnea Patients. Medicina, 58(10), 1336. https://doi.org/10.3390/medicina58101336






