Frailty and Different Exercise Interventions to Improve Gait Speed in Older Adults after Acute Coronary Syndrome
Abstract
:1. Introduction
2. Materials and Methods
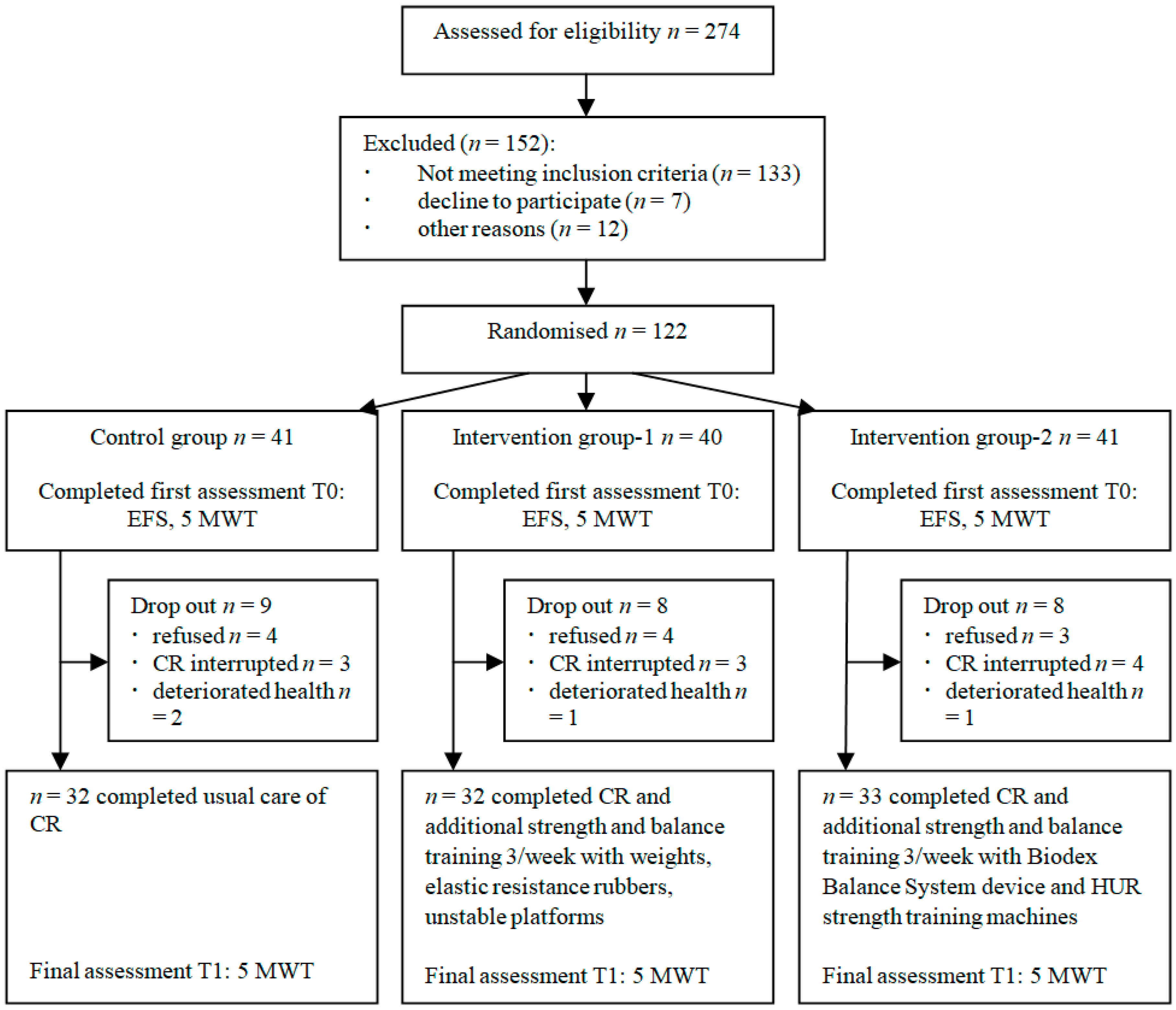
2.1. Study Design and Participants
2.2. Study Assessment
2.3. Study Interventions
2.4. Statistical Analysis
3. Results
3.1. Frailty Prevalence
3.2. Effectiveness of Cardiac Rehabilitation on Gait Speed
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Timmis, A.; Townsend, N.; Gale, C.P.; Torbica, A.; Lettino, M.; Petersen, S.E.; Mossialos, E.A.; Maggioni, A.P.; Kazakiewicz, D.; May, H.T.; et al. European Society of Cardiology: Cardiovascular Disease Statistics 2019. Eur. Heart J. 2020, 41, 12–85. [Google Scholar] [CrossRef] [PubMed]
- Piepoli, M.F.; Hoes, A.W.; Agewall, S.; Albus, C.; Brotons, C.; Catapano, A.L.; Cooney, M.; Corrà, U.; Cosyns, B.; Deaton, C.; et al. 2016 European Guidelines on cardiovascular disease prevention in clinical practice: The Sixth Joint Task Force of the European Society of Cardiology and Other Societies on Cardiovascular Disease Prevention in Clinical Practice (constituted by representatives of 10 societies and by invited experts)Developed with the special contribution of the European Association for Cardiovascular Prevention & Rehabilitation (EACPR). Eur. Heart J. 2016, 37, 2315–2381. [Google Scholar] [CrossRef] [PubMed]
- Thiele, H.; Barbato, E.; Barthelemy, O.; Bauersachs, J.; Bhatt, D.L. 2020 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Rev. Esp. Cardiol. (Engl. Ed.) 2021, 74, 544. [Google Scholar] [CrossRef]
- Thomas, R.J.; Balady, G.; Banka, G.; Beckie, T.M.; Chiu, J.; Gokak, S.; Ho, P.M.; Keteyian, S.J.; King, M.; Lui, K.; et al. 2018 ACC/AHA Clinical Performance and Quality Measures for Cardiac Rehabilitation: A Report of the American College of Cardiology/American Heart Association Task Force on Performance Measures. J. Am. Coll. Cardiol. 2018, 71, 1814–1837. [Google Scholar] [CrossRef]
- Ambrosetti, M.; Abreu, A.; Corrà, U.; Davos, C.H.; Hansen, D.; Frederix, I.; Iliou, M.C.; E Pedretti, R.F.; Schmid, J.-P.; Vigorito, C.; et al. Secondary prevention through comprehensive cardiovascular rehabilitation: From knowledge to implementation. 2020 update. A position paper from the Secondary Prevention and Rehabilitation Section of the European Association of Preventive Cardiology. Eur. J. Prev. Cardiol. 2021, 28, 460–495. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- United Nations, Department of Economic and Social Affairs, Population Division. World Population Prospects Highlights, 2019 Revision. Available online: https://population.un.org/wpp/Publications/Files/WPP2019_Highlights.pdf (accessed on 13 September 2021).
- World Health Organization. WHO Clinical Consortium on Healthy Ageing: Topic Focus: Frailty and Intrinsic Capacity: Report of Consortium Meeting, 1–2 December 2016 in Geneva, Switzerland. 2017. Available online: https://apps.who.int/iris/handle/10665/272437 (accessed on 1 December 2021).
- Wolfe, R.R. Optimal nutrition, exercise, and hormonal therapy promote muscle anabolism in the elderly. J. Am. Coll. Surg. 2006, 202, 176–180. [Google Scholar] [CrossRef]
- Harada, H.; Kai, H.; Niiyama, H.; Nishiyama, Y.; Katoh, A.; Yoshida, N.; Fukumoto, Y.; Ikeda, H. Effectiveness of cardiac rehabilitation for prevention and treatment of sarcopenia in patients with cardiovascular disease-a retrospective cross-sectional analysis. J. Nutr. Health Aging. 2017, 21, 449–456. [Google Scholar] [CrossRef]
- Kamiya, K.; Hamazaki, N.; Matsuzawa, R.; Nozaki, K.; Tanaka, S.; Ichinosawa, Y.; Maekawa, E.; Noda, C.; Yamaoka-Tojo, M.; Matsunaga, A.; et al. Sarcopenia: Prevalence and prognostic implications in elderly patients with cardiovascular disease. JCSM Clin. Rep. 2017, 2. [Google Scholar] [CrossRef] [Green Version]
- Cadore, E.L.; Rodríguez-Mañas, L.; Sinclair, A.; Izquierdo, M. Effects of Different Exercise Interventions on Risk of Falls, Gait Ability, and Balance in Physically Frail Older Adults: A Systematic Review. Rejuvenation Res. 2013, 16, 105–114. [Google Scholar] [CrossRef] [Green Version]
- Lohman, M.C.; Mezuk, B.; Dumenci, L. Depression and frailty: Concurrent risks for adverse health outcomes. Aging Ment. Health 2017, 21, 399–408. [Google Scholar] [CrossRef]
- Shamliyan, T.; Talley, K.M.C.; Ramakrishnan, R.; Kane, R.L. Association of frailty with survival: A systematic literature review. Ageing Res. Rev. 2013, 12, 719–736. [Google Scholar] [CrossRef] [PubMed]
- O’Caoimh, R.; Galluzzo, L.; Rodríguez-Laso, Á.; Ranhoff, A.H.; Lamprini-Koula, M.; Ciutan, M.; van der Heyden, J.; López-Samaniego, L.; Carcaillon-Bentata, L.; Kennelly, S.; et al. Prevalence of frailty at population level in European ADVANTAGE Joint Action Member States: A systematic review and meta-analysis. Ann. Ist. Super Sanita 2018, 54, 226–238. [Google Scholar] [CrossRef] [PubMed]
- Beigienė, A.; Petruševičienė, D.; Barasaitė, V.; Kubilius, R.; Macijauskienė, J. Cardiac Rehabilitation and Complementary Physical Training in Elderly Patients after Acute Coronary Syndrome: A Pilot Study. Medicina 2021, 57, 529. [Google Scholar] [CrossRef] [PubMed]
- University of Alberta Faculty of Medicine & Dentistry. Edmonton Frail Scale. Tool Kit. Version 1.7. Available online: https://articulateusercontent.com/rise/courses/2-ONUZ_z1z4FRSEF3_L1YDtd7RdarwMf/2BmfnjfGbam9JF6f-EFS%2520Tool%2520Kit%25201.7.pdf (accessed on 13 September 2021).
- Graham, M.M.; Galbraith, P.D.; O’Neill, D.; Rolfson, D.B.; Dando, C.; Norris, C.M. Frailty and Outcome in Elderly Patients With Acute Coronary Syndrome. Can. J. Cardiol. 2013, 29, 1610–1615. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- He, Y.; Li, L.W.; Hao, Y.; Sim, E.Y.; Ng, K.L.; Lee, R.; Lim, M.S.; Poopalalingam, R.; Abdullah, H.R. Assessment of predictive validity and feasibility of Edmonton Frail Scale in identifying postoperative complications among elderly patients: A prospective observational study. Sci. Rep. 2020, 10, 14682. [Google Scholar] [CrossRef]
- Cesari, M.; Kritchevsky, S.B.; Penninx, B.W.H.J.; Nicklas, B.J.; Simonsick, E.M.; Newman, A.B.; Tylavsky, F.A.; Brach, J.S.; Satterfield, S.; Bauer, D.C.; et al. Prognostic Value of Usual Gait Speed in Well-Functioning Older People—Results from the Health, Aging and Body Composition Study: USUAL GAIT SPEED IN OLDER PERSONS. J. Am. Geriatr. Soc. 2005, 53, 1675–1680. [Google Scholar] [CrossRef] [Green Version]
- JCS Joint Working Group. Guidelines for Rehabilitation in Patients With Cardiovascular Disease (JCS 2012):–Digest Version–. Circ. J. 2014, 78, 2022–2093. [Google Scholar] [CrossRef] [Green Version]
- Rolfson, D.B.; Majumdar, S.R.; Tsuyuki, R.T.; Tahir, A.; Rockwood, K. Validity and reliability of the Edmonton Frail Scale. Age Ageing 2006, 35, 526–529. [Google Scholar] [CrossRef] [Green Version]
- Giallauria, F.; Di Lorenzo, A.; Venturini, E.; Pacileo, M.; D’Andrea, A.; Garofalo, U.; De Lucia, F.; Testa, C.; Cuomo, G.; Iannuzzo, G.; et al. Frailty in Acute and Chronic Coronary Syndrome Patients Entering Cardiac Rehabilitation. JCM 2021, 10, 1696. [Google Scholar] [CrossRef]
- Abbasi, M.; Rolfson, D.; Khera, A.S.; Dabravolskaj, J.; Dent, E.; Xia, L. Identification and management of frailty in the primary care setting. CMAJ 2018, 190, E1134–E1140, Erratum in: CMAJ 2019, 191, E54. [Google Scholar] [CrossRef] [Green Version]
- Dent, E.; Kowal, P.; Hoogendijk, E.O. Frailty measurement in research and clinical practice: A review. Eur. J. Intern. Med. 2016, 31, 3–10. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Rolfson, D. Successful Aging and Frailty: A Systematic Review. Geriatrics 2018, 3, 79. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Collard, R.M.; Boter, H.; Schoevers, R.A.; Oude Voshaar, R.C. Prevalence of Frailty in Community-Dwelling Older Persons: A Systematic Review. J. Am. Geriatr. Soc. 2012, 60, 1487–1492. [Google Scholar] [CrossRef] [PubMed]
- O’Caoimh, R.; Sezgin, D.; O’Donovan, M.R.; Molloy, D.W.; Clegg, A.; Rockwood, K.; Liew, A. Prevalence of frailty in 62 countries across the world: A systematic review and meta-analysis of population-level studies. Age Ageing 2021, 50, 96–104. [Google Scholar] [CrossRef]
- Bieniek, J.; Wilczyński, K.; Szewieczek, J. Fried frailty phenotype assessment components as applied to geriatric inpatients. Clin. Interv. Aging. 2016, 11, 453–459. [Google Scholar] [CrossRef] [Green Version]
- Soler, V.; Sourdet, S.; Balardy, L.; Abellan Van Kan, G.; Brechemier, D.; Bugat, M.E.R.; Tavassoli, N.; Cassagne, M.; Malecaze, F.; Nourhashemi, F.; et al. Visual impairment screening at the Geriatric Frailty Clinic for Assessment of Frailty and Prevention of Disability at the Gérontopôle. J. Nutr. Health Aging 2016, 20, 870–877. [Google Scholar] [CrossRef]
- Dapp, U.; Minder, C.E.; Anders, J.; Golgert, S.; von Renteln-Kruse, W. Long-term prediction of changes in health status, frailty, nursing care and mortality in community-dwelling senior citizens-results from the longitudinal urban cohort ageing study (LUCAS). BMC Geriatr. 2014, 14, 141. [Google Scholar] [CrossRef] [Green Version]
- Mulasso, A.; Roppolo, M.; Gobbens, R.; Mosso, C.; Rabaglietti, E. A comparison between uni- and multidimensional frailty measures: Prevalence, functional status, and relationships with disability. CIA 2015, 1669. [Google Scholar] [CrossRef] [Green Version]
- Xue, Q.-L. The Frailty Syndrome: Definition and Natural History. Clin. Geriatr. Med. 2011, 27, 1–15. [Google Scholar] [CrossRef] [Green Version]
- Shimada, H.; Doi, T.; Lee, S.; Tsutsumimoto, K.; Bae, S.; Makino, K.; Nakakubo, S.; Arai, H. Identification of Disability Risk in Addition to Slow Walking Speed in Older Adults. Gerontology 2021, 14, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Afilalo, J.; Eisenberg, M.J.; Morin, J.-F.; Bergman, H.; Monette, J.; Noiseux, N.; Perrault, L.P.; Alexander, K.P.; Langlois, Y.; Dendukuri, N.; et al. Gait Speed as an Incremental Predictor of Mortality and Major Morbidity in Elderly Patients Undergoing Cardiac Surgery. J. Am. Coll. Cardiol. 2010, 56, 1668–1676. [Google Scholar] [CrossRef] [Green Version]
- Afilalo, J.; Kim, S.; O’Brien, S.; Brennan, J.M.; Edwards, F.H.; Mack, M.J.; McClurken, J.B.; Cleveland, J.C.; Smith, P.K.; Shahian, D.M.; et al. Gait Speed and Operative Mortality in Older Adults Following Cardiac Surgery. JAMA Cardiol. 2016, 1, 314. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Afilalo, J. Evaluating and Treating Frailty in Cardiac Rehabilitation. Clin. Geriatr. Med. 2019, 35, 445–457. [Google Scholar] [CrossRef] [PubMed]
- Braun, T.; Grüneberg, C.; Süßmilch, K.; Wiessmeier, M.; Schwenk, I.; Eggert, S.; Machleit-Ebner, A.; Harras, I.; Thiel, C. An augmented prescribed exercise program (APEP) to improve mobility of older acute medical patients–a randomized, controlled pilot and feasibility trial. BMC Geriatr. 2019, 19, 240. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Nagai, K.; Miyamato, T.; Okamae, A.; Tamaki, A.; Fujioka, H.; Wada, Y.; Uchiyama, Y.; Shinmura, K.; Domen, K. Physical activity combined with resistance training reduces symptoms of frailty in older adults: A randomized controlled trial. Arch. Gerontol. Geriatr. 2018, 76, 41–47. [Google Scholar] [CrossRef]
- Veronese, N. (Ed.) Frailty and Cardiovascular Diseases: Research into an Elderly Population; Springer International Publishing: Cham, Switzerland, 2020; Volume 1216. [Google Scholar] [CrossRef]
- Khadanga, S.; Savage, P.D.; Ades, P.A. Resistance Training for Older Adults in Cardiac Rehabilitation. Clin. Geriatr. Med. 2019, 35, 459–468. [Google Scholar] [CrossRef]
- Giné-Garriga, M.; Roqué-Fíguls, M.; Coll-Planas, L.; Sitjà-Rabert, M.; Salvà, A. Physical Exercise Interventions for Improving Performance-Based Measures of Physical Function in Community-Dwelling, Frail Older Adults: A Systematic Review and Meta-Analysis. Arch. Phys. Med. Rehabil. 2014, 95, 753–769.e3. [Google Scholar] [CrossRef]
- de Labra, C.; Guimaraes-Pinheiro, C.; Maseda, A.; Lorenzo, T.; Millán-Calenti, J.C. Effects of physical exercise interventions in frail older adults: A systematic review of randomized controlled trials. BMC Geriatr. 2015, 15, 154. [Google Scholar] [CrossRef] [Green Version]
- Kim, H.; Suzuki, T.; Kim, M.; Kojima, N.; Ota, N.; Shimotoyodome, A.; Hase, T.; Hosoi, E.; Yoshida, H. Effects of Exercise and Milk Fat Globule Membrane (MFGM) Supplementation on Body Composition, Physical Function, and Hematological Parameters in Community-Dwelling Frail Japanese Women: A Randomized Double Blind, Placebo-Controlled, Follow-Up Trial. PLoS ONE 2015, 10, e0116256. [Google Scholar] [CrossRef] [Green Version]
- Coelho-Júnior, H.J.; Uchida, M.C. Effects of Low-Speed and High-Speed Resistance Training Programs on Frailty Status, Physical Performance, Cognitive Function, and Blood Pressure in Prefrail and Frail Older Adults. Front. Med. 2021, 8, 702436. [Google Scholar] [CrossRef]
| Characteristic | All (n = 97) | IG-1 (n = 32) | IG-2 (n = 33) | CG (n = 32) | p Value * |
|---|---|---|---|---|---|
| Age, years | 73.1 ± 5.3 | 72.6 ± 4.6 | 70.6 ± 4.3 | 74.6 ± 6.3 | 0.008 |
| Sex, n (%) | |||||
| Female | 26 (26.8) | 8 (25) | 11 (33.3) | 7 (21.9) | 0.558 |
| Male | 71 (73.2) | 24 (75) | 22 (66.7) | 25 (78.1) | |
| Height, m | 1.7 ± 0.1 | 1.7 ± 0.1 | 1.7 ± 0.1 | 1.7 ± 0.1 | 0.234 |
| Weight, kg | 80.1 ± 13.7 | 80.8 ± 12.3 | 83.8 ± 15.8 | 77.8 ± 12.3 | 0.220 |
| Body mass index, kg/m2 | 27.9 ± 3.9 | 28.5 ± 3.4 | 28.4 ± 4.2 | 26.9 ± 4 | 0.176 |
| Current smokers, n (%) | 11 (11.3) | 4 (12.5) | 3 (9.1) | 4 (12.5) | 0.882 |
| LV ejection fraction, % | 47.7 ± 5.3 | 48.8 ± 5.1 | 46.8 ± 4.6 | 47.5 ± 56 | 0.311 |
| CR duration, days | 18.9 ± 1.7 | 19.6 ± 0.8 | 18.8 ± 1.6 | 18.3 ± 2.3 | 0.008 |
| Comorbidities, n (%) | |||||
| Diabetes | 15 (15.5) | 7 (21.9) | 2 (6.1) | 6 (18.8) | 0.174 |
| Atrial fibrillation | 18 (18.6) | 6 (18.8) | 7 (21.2) | 5 (15.6) | 0.845 |
| Degenerative joint disease | 6 (6.2) | 1 (3.1) | 4 (12.1) | 1 (3.1) | 0.219 |
| Cancer | 8 (8.2) | 3 (9.4) | 3 (9.1) | 2 (6.3) | 0.881 |
| Treatment, n (%) | |||||
| Coronary artery by-pass graft | 58 (59.8) | 25 (78.1) | 17 (51.5) | 16 (50) | 0.035 |
| PTCA | 39 (40.2) | 7 (21.9) | 16 (48.5) | 16 (50) | |
| Medication, n (%) | |||||
| ACE inhibitor | 78 (80.4) | 22 (68.8) | 27 (81.8) | 29 (90.6) | 0.085 |
| Diuretic | 70 (72.2) | 26 (81.3) | 24 (72.7) | 20 (62.5) | 0.246 |
| Statin | 93 (95.9) | 30 (93.8) | 32 (97) | 31 (96.9) | 0.761 |
| Frailty Assessment | All (n = 97) | IG-1 (n = 32) | IG-2 (n = 33) | CG (n = 32) | p Value * |
|---|---|---|---|---|---|
| Total EFS score (0–17), median (IQR) | 5 (4–6) | 5 (4–6.8) | 5 (3–7) | 5 (4–6) | 0.880 |
| Frailty classification by EFS, n (%) | |||||
| Fit (0–3) | 20 (20.6) | 4 (12.5) | 9 (27.3) | 7 (21.9) | 0.643 |
| Vulnerable (4–5) | 41 (42.3) | 16 (50) | 12 (36.4) | 13 (40.6) | |
| Frailty (≥6) | 36 (37.1) | 12 (37.5) | 12 (36.4) | 12 (37.5) | |
| EFS items | |||||
| Cognition, n (%) | |||||
| Clock drawing test faultless | 30 (30.9) | 8 (25) | 11 (33.3) | 11 (34.4) | 0.672 |
| Clock drawing test with minor and major errors | 67 (69.1) | 24 (75) | 22 (66.7) | 21 (65.6) | 0.210 |
| One and more hospitalizations in the past year, n (%) | 87 (89.7) | 28 (87.5) | 31 (93.9) | 28 (87.5) | 0.902 |
| General health status, n (%) | |||||
| Excellent, very good, good | 22 (22.7) | 7 (21.9) | 9 (27.3) | 6 (18.8) | 0.708 |
| Fair, poor | 75 (77.3) | 25 (78.1) | 24 (72.7) | 26 (81.3) | 0.470 |
| Functional independence, n (%) | |||||
| Independent | 76 (78.4) | 27 (84.4) | 27 (81.8) | 22 (68.8) | 0.265 |
| Require help in two and more activities | 21 (21.6) | 5 (15.6) | 6 (18.2) | 10 (31.3) | 0.944 |
| Social support, n (%) | |||||
| Always | 91 (93.6) | 31 (96.9) | 31 (93.9) | 29 (90.6) | 0.957 |
| Sometimes, never | 6 (6.2) | 1 (3.1) | 2 (6.1) | 3 (9.4) | NA |
| Medication use, n (%) | |||||
| Amount ≥ 5 | 80 (82.5) | 27 (84.4) | 28 (84.8) | 25 (78.1) | 0.916 |
| Forgetfulness | 14 (14.4) | 5 (15.6) | 3 (9.1) | 6 (18.8) | NA |
| Nutrition–weight loss, n (%) | 22 (22.7) | 8 (25) | 8 (24.2) | 6 (18.8) | 0.808 |
| Mood–sad, depressed, n (%) | 30 (30.9) | 11 (34.4) | 10 (30.3) | 9 (28.1) | 0.860 |
| Urinary incontinence, n (%) | 7(7.2) | 3 (9.4) | 2 (6.1) | 2 (6.3) | NA |
| Functional performance by the TUG test, n (%) | |||||
| 0–10 s | 68 (70.1) | 23 (71.9) | 23 (69.7) | 22 (68.8) | 0.962 |
| 11–20 s | 29 (29.9) | 9 (28.1) | 10 (30.3) | 10 (31.3) | 0.607 |
| Parameter | IG-1 (n = 28) | IG-2 (n = 24) | CG (n = 25) | p * | ||||
|---|---|---|---|---|---|---|---|---|
| T0 | T1 | T0 | T1 | T0 | T1 | Within groups | Among groups | |
| Gait speed, m/s | 1.23 (1.02–1.45) | 1.41 (1.18–1.61) | 1.37 (0.92–1.59) | 1.56 (1.3–1.66) | 1.35 (0.94–1.56) | 1.53 (1–1.68) | <0.05 | 0.100 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Beigienė, A.; Petruševičienė, D.; Barasaitė, V.; Kubilius, R.; Macijauskienė, J. Frailty and Different Exercise Interventions to Improve Gait Speed in Older Adults after Acute Coronary Syndrome. Medicina 2021, 57, 1344. https://doi.org/10.3390/medicina57121344
Beigienė A, Petruševičienė D, Barasaitė V, Kubilius R, Macijauskienė J. Frailty and Different Exercise Interventions to Improve Gait Speed in Older Adults after Acute Coronary Syndrome. Medicina. 2021; 57(12):1344. https://doi.org/10.3390/medicina57121344
Chicago/Turabian StyleBeigienė, Aurelija, Daiva Petruševičienė, Vitalija Barasaitė, Raimondas Kubilius, and Jūratė Macijauskienė. 2021. "Frailty and Different Exercise Interventions to Improve Gait Speed in Older Adults after Acute Coronary Syndrome" Medicina 57, no. 12: 1344. https://doi.org/10.3390/medicina57121344
APA StyleBeigienė, A., Petruševičienė, D., Barasaitė, V., Kubilius, R., & Macijauskienė, J. (2021). Frailty and Different Exercise Interventions to Improve Gait Speed in Older Adults after Acute Coronary Syndrome. Medicina, 57(12), 1344. https://doi.org/10.3390/medicina57121344






